预约演示
更新于:2026-06-06
Autologous CD19-directed CAR-T cells(University of Sao Paulo)
更新于:2026-06-06
概要
基本信息
非在研机构- |
权益机构- |
最高研发阶段临床1/2期 |
首次获批日期- |
最高研发阶段(中国)- |
特殊审评- |
登录后查看时间轴
关联
1
项与 Autologous CD19-directed CAR-T cells(University of Sao Paulo) 相关的临床试验NCT06101381
CD19-directed CAR-T Cell Therapy for Refractory or Relapsed Acute Lymphoblastic Leukemia or Non-Hodgkin Lymphoma: a Multicenter Phase I/II Trial.
The goal of this prospective, multicentric, single-arm, phase I/II clinical trial is to evaluate the safety and efficacy of a novel CD19-directed CAR-T cell locally produced in an academic institution in Brazil in patients with refractory or relapsed acute lymphoblastic leukemia or non-Hodgkin lymphoma.
Participants will receive a single intravenous infusion of an autologous academic anti-CD19 CAR-T cell and will be followed for 5 years.
Participants will receive a single intravenous infusion of an autologous academic anti-CD19 CAR-T cell and will be followed for 5 years.
开始日期2024-03-21 |
申办/合作机构 |
100 项与 Autologous CD19-directed CAR-T cells(University of Sao Paulo) 相关的临床结果
登录后查看更多信息
100 项与 Autologous CD19-directed CAR-T cells(University of Sao Paulo) 相关的转化医学
登录后查看更多信息
100 项与 Autologous CD19-directed CAR-T cells(University of Sao Paulo) 相关的专利(医药)
登录后查看更多信息
5
项与 Autologous CD19-directed CAR-T cells(University of Sao Paulo) 相关的文献(医药)2023-09-04·Cureus
Myelodysplastic Syndrome After Anti-CD19 Chimeric Antigen Receptor T-cell Therapy: A Case Series
作者: Ravi, Soumiya ; Dhaliwal, Armaan
The utility of CD19-targeted chimeric antigen receptor T-cell (CAR-T cell) therapy in the management of refractory/relapsed B-cell malignancies has increased tremendously in recent times. In addition to cytokine release syndrome (CRS), neurotoxicity, and infections, CAR-T cell patients develop cytopenias, with about 15% of the patients continuing to have severe cytopenias up to three months after treatment. Retrospective reviews have reported the development of myelodysplastic syndrome (MDS) in patients undergoing CAR-T cell therapy. Here, we describe four cases of MDS and/or clonal cytopenias of undetermined significance (CCUS), developing after CAR-T cell therapy. A retrospective review of four patients with relapsed/refractory B-cell lymphomas treated with CD19-directed autologous CAR-T cell was conducted at our institution. The median age was 72.5 years (range 63-76). Three of the four patients had double-hit diffuse large B-cell lymphoma (DLBCL). The median number of lines of therapy before CAR-T cell was three. Only one patient had a prior autologous stem cell transplant (ASCT). The median time to diagnosis of MDS/CCUS from CAR-T cell therapy was three months. Two cases of CCUS diagnosed were at one- and two-month post-CAR-T cell, and two cases of MDS were diagnosed at 10 and 26 months. None of the patients had dysplastic clones before the initiation of CAR-T cell therapy. Only one patient was found to have CCUS-developed CRS post-CAR-T cell requiring treatment with tocilizumab and steroids. Three patients showed complete response, with one showing a very good partial response. All the patients were in remission with no additional therapies post-CAR-T cell. One patient died secondary to COVID-19-related complications. Four patients with prolonged cytopenias were found to have either MDS or CCUS after CAR-T cell therapy. Two CCUS cases underwent bone marrow evaluation early in the course of cytopenias and may develop into MDS, acute myeloid leukemia (AML), or myeloproliferative neoplasm over time. Our retrospective case series review, compared to previous studies, constitutes of patients with no prior clonal hematopoiesis-related cytogenetic abnormalities, fewer lines of therapy, and only one patient with previous hematopoietic stem cell transplantation (HSCT). Based on the upcoming data and our review, a bone marrow biopsy with next-generation sequencing (NGS) is imperative in patients with prolonged cytopenias after CAR-T cell therapy. A diagnosis of CCUS/MDS in these cases can help guide treatment.
2023-08-01·Current rheumatology reviews
Autologous CD19-Targeted Chimeric Antigen Receptor (CAR)T-Cells as
the Future of Systemic Lupus Erythematosus Treatment
Article
作者: Surya Rini, Sandra ; Kambayana, Gede
Abstract::
Systemic lupus erythematosus (SLE) is a chronic autoimmune illness with an unclear eti-ology and a range of clinical manifestations. The therapeutic results of current conventional treat-ments are frequently unsatisfactory. Many B-cell-directed immunotherapies have recently been dis-covered, as B cells play a key role in the pathogenesis of SLE. However, large-scale rituximab trials found that the antibody against CD20 was no better than a placebo. Autologous CAR T-cell therapy has garnered considerable interest and is considered a potential treatment option for SLE. CD19+CD20- B cells are thought to play an essential role in the onset and progression of SLE. CD19-targeted CAR T-cells destroy B cells without requiring an accessory cell type, thereby de-creasing B cells more efficiently. Preclinical trials of CAR T-cells in mice have shown promising results against SLE. The review aimed to shed light on autologous CD19-targeted CAR T-cells as a potential treatment for SLE.
2019-05-02·JCI insight1区 · 医学
Safety and tolerability of conditioning chemotherapy followed by CD19-targeted CAR T cells for relapsed/refractory CLL
1区 · 医学
ArticleOA
作者: Hsu, Meier ; Palomba, M. Lia ; Wang, Yongzeng ; Wang, Xiuyan ; Halton, Elizabeth ; Purdon, Terence J. ; Rivière, Isabelle ; Sénéchal, Brigitte ; Bernal, Yvette ; Brentjens, Renier J. ; van Leeuwen, Dayenne G. ; Geyer, Mark B. ; Sadelain, Michel ; Park, Jae H. ; Devlin, Sean M.
BACKGROUND:
Subgroups of patients with relapsed or refractory (R/R) chronic lymphocytic leukemia (CLL) exhibit suboptimal outcomes after standard therapies, including oral kinase inhibitors. We and others have previously reported on the safety and efficacy of autologous CD19-targeted CAR T cells for these patients. Here, we report safety and long-term follow-up of CAR T cell therapy with or without conditioning chemotherapy for patients with R/R CLL and indolent B cell non-Hodgkin lymphoma (B-NHL).
METHODS:
We conducted a phase I clinical trial investigating CD19-targeted CAR T cells incorporating a CD28 costimulatory domain (19–28z). Seventeen of twenty patients received conditioning chemotherapy prior to CAR T cell infusion. Five patients with CLL received ibrutinib at the time of autologous T cell collection and/or CAR T cell administration.
RESULTS:
This analysis included 16 patients with R/R CLL and 4 patients with R/R indolent B-NHL. Cytokine release syndrome (CRS) was observed in all 20 patients, but grade 3 and 4 CRS and neurological events were uncommon (10% for each). Ex vivo expansion of T cells and proportions of CAR T cells with the CD62L
+
CD127
+
immunophenotype were significantly greater (
P
= 0.047; CD8 subset,
P
= 0.0061, CD4 subset) in patients on ibrutinib at leukapheresis. Three of twelve evaluable CLL patients receiving conditioning chemotherapy achieved complete response (CR) (2 had minimal residual disease–negative CR). All patients achieving CR remained progression free at median follow-up of 53 months.
CONCLUSION:
Conditioning chemotherapy and 19–28z CAR T cells were acceptably tolerated across investigated dose levels in heavily pretreated patients with R/R CLL and indolent B-NHL, and a subgroup of patients achieved durable CR. Ibrutinib therapy may modulate autologous T cell phenotype.
TRIAL REGISTRATION:
ClinicalTrials.gov NCT00466531.
FUNDING:
Juno Therapeutics and NIH/National Cancer Institute Cancer Center Support Grant (P30-CA08748).
100 项与 Autologous CD19-directed CAR-T cells(University of Sao Paulo) 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 急性白血病 | 临床2期 | 巴西 | 2024-03-21 | |
| 弥漫性大B细胞淋巴瘤 | 临床2期 | 巴西 | 2024-03-21 | |
| 滤泡性淋巴瘤 | 临床2期 | 巴西 | 2024-03-21 | |
| 高级别B细胞淋巴瘤 | 临床2期 | 巴西 | 2024-03-21 | |
| 难治性 B 细胞急性淋巴细胞白血病 | 临床2期 | 巴西 | 2024-03-21 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
No Data | |||||||
登录后查看更多信息
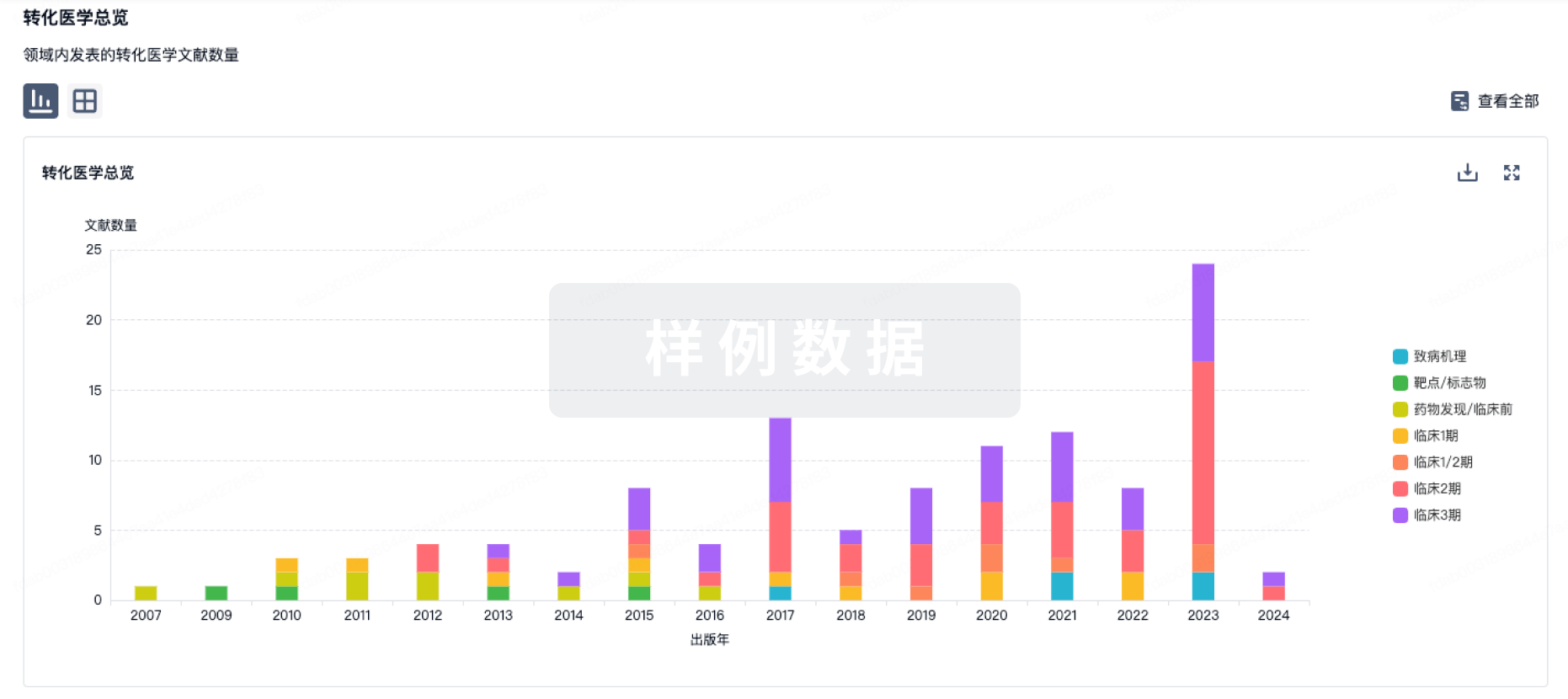
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
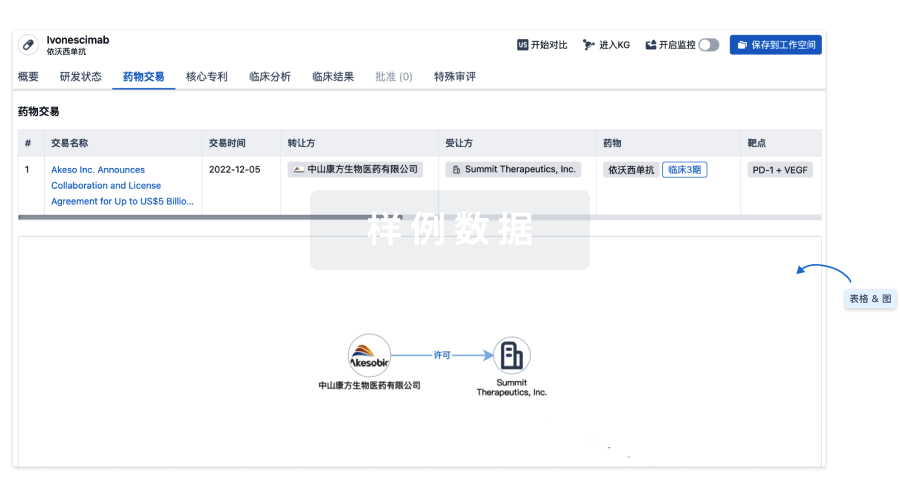
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
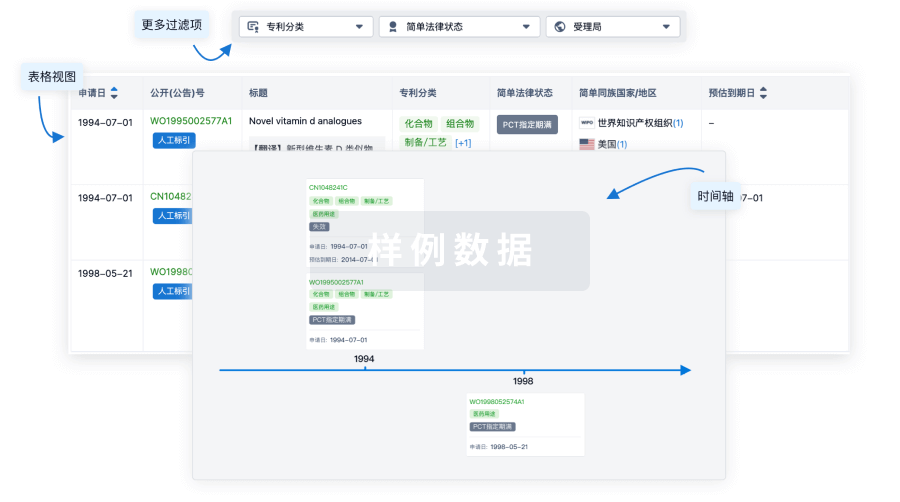
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
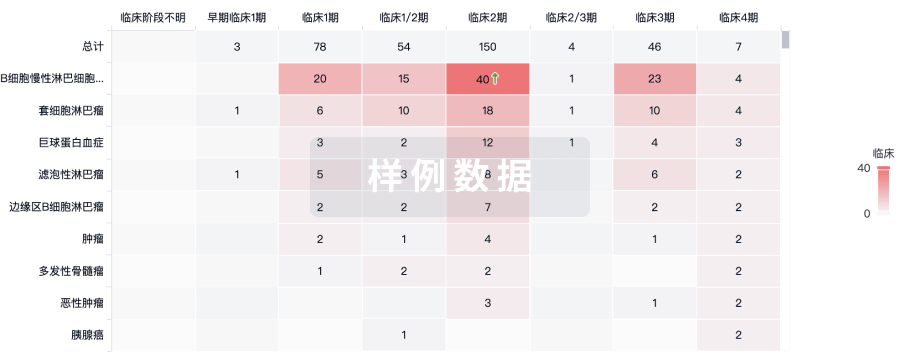
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
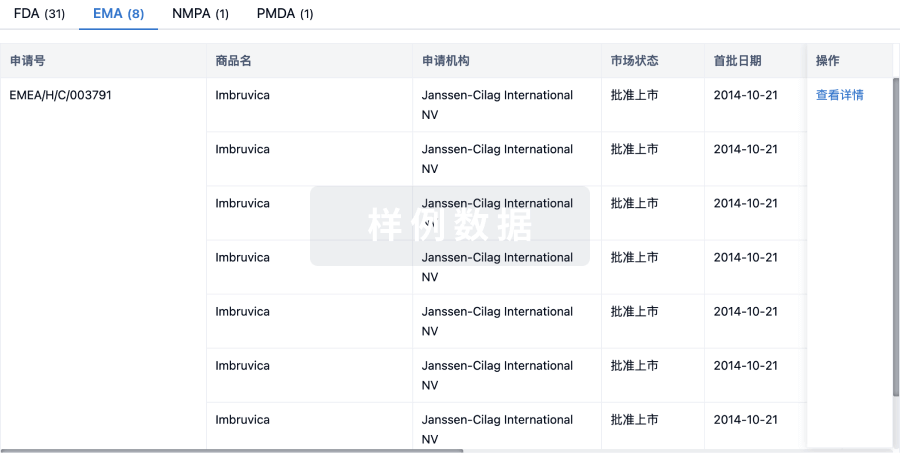
批准
利用最新的监管批准信息加速您的研究。
登录
或
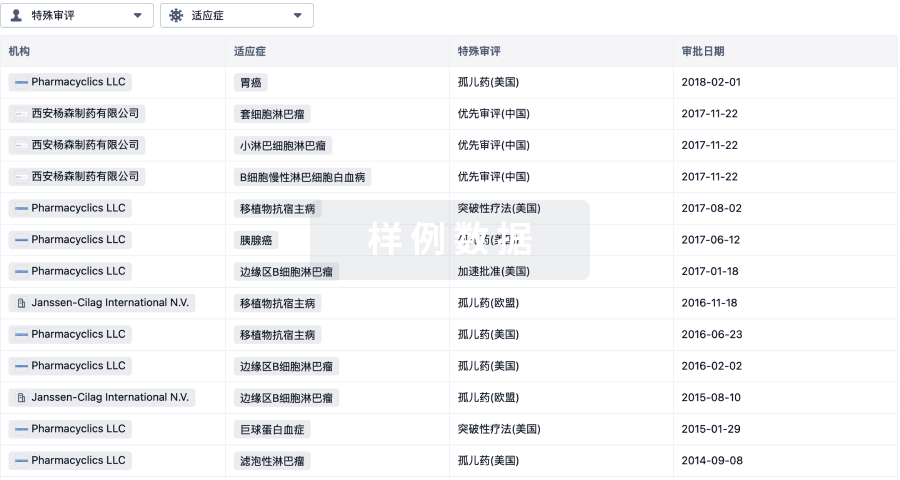
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
