预约演示
更新于:2026-05-02
ODN2395
更新于:2026-05-02
概要
基本信息
在研机构- |
权益机构- |
最高研发阶段无进展临床前 |
首次获批日期- |
最高研发阶段(中国)- |
特殊审评- |
结构/序列
使用我们的RNA技术数据为新药研发加速。
登录
或
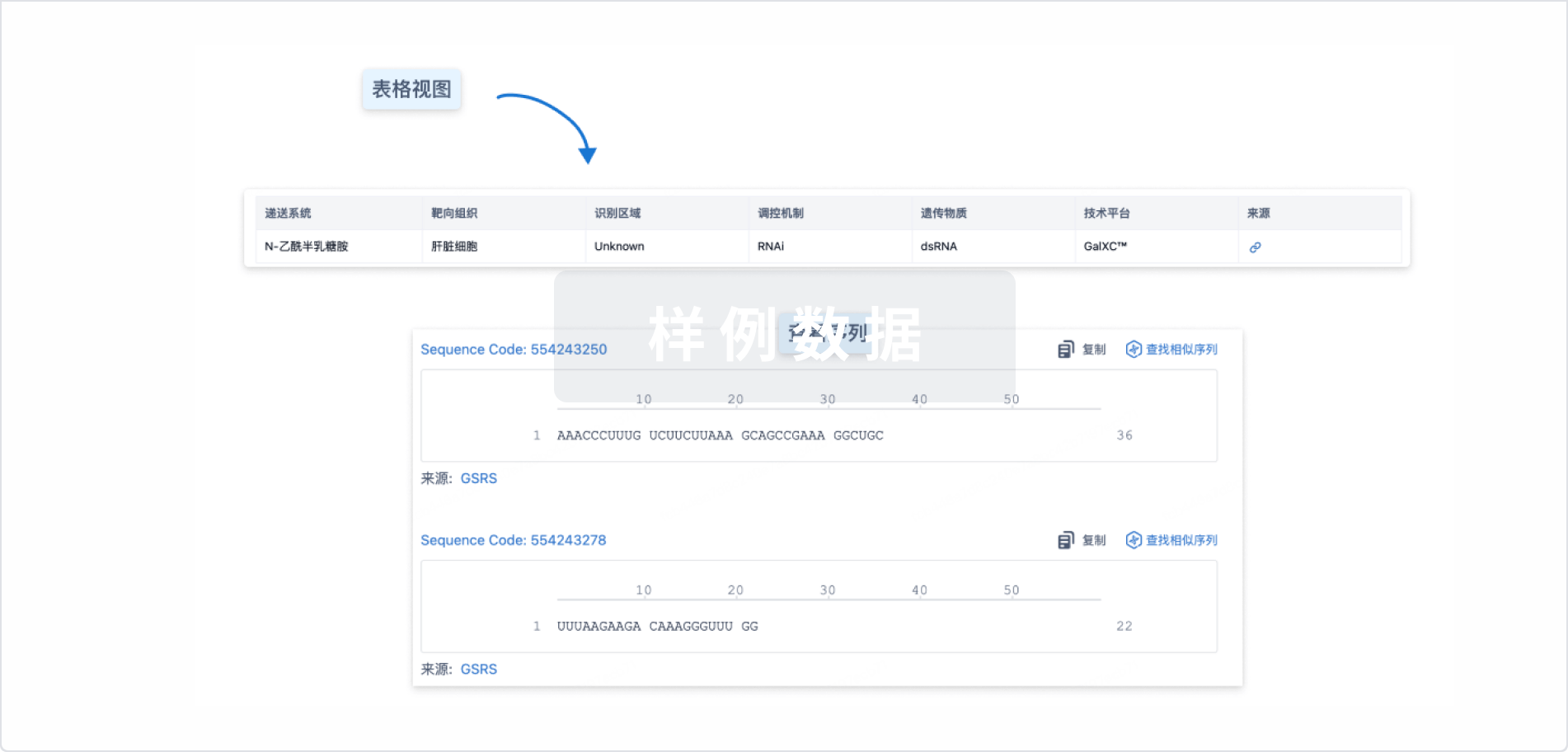
Sequence Code 29244644

关联
100 项与 ODN2395 相关的临床结果
登录后查看更多信息
100 项与 ODN2395 相关的转化医学
登录后查看更多信息
100 项与 ODN2395 相关的专利(医药)
登录后查看更多信息
17
项与 ODN2395 相关的文献(医药)2025-01-21·CLINICAL AND EXPERIMENTAL IMMUNOLOGY
A novel mouse model of myositis-associated interstitial lung disease was established by using TLR9 agonist combined with muscle homogenate
Article
作者: Li, Feifei ; Zhao, Peipei ; Bai, Ling ; Ma, Wenlan ; Zhang, Cen ; Zhang, Sigong ; Zhu, Jiarui
Abstract:
Our group previously demonstrated that NETs were involved in interstitial lung diseases (ILD) among patients with idiopathic inflammatory myopathies (IIM) and the experimental autoimmune myositis (EAM) mouse model and that NETs activated lung fibroblasts through the TLR9-miR7-Smad2 axis. This study aimed to establish a novel mouse model of myositis-associated interstitial lung disease (MAILD) by using a TLR9 agonist (ODN2395). ODN2395 and muscle homogenate were used to induce MAILD in BALB/c mice. MAILD was evaluated using histopathology, immunohistochemistry, serum NETs determination, and myositis-specific antibody profile. Furthermore, TLR9 and IRF3 were examined in a lung biopsy tissue from a dermatomyositis patient with ILD. MAILD mice developed inflammatory myopathy with positive expression of myositis-specific antibodies. ILD occurred in all mice of the MAILD group. ODN2395 at doses of 5 μg, 10 μg, or 20 μg induced ILD, with increasing severity as the dose increased, but 20 μg ODN2395 was not recommended due to non-specific damage to the lungs. ILD could occur as early as one week after immunization and was most pronounced by the fourth/fifth week. MAILD process was accompanied by NETs infiltration and TLR9 activation. TLR9 activation was demonstrated in the patient with DM-ILD. Serum levels of Cit-H3 were elevated in the MAILD group. Skeletal muscle homogenate and ODN2395 induced neutrophils to form NETs in vitro. Combined with muscle homogenate, ODN2395 induced a novel MAILD mouse model with NETs infiltration and TLR9 activation, which are similar to pathogenesis of IIM-ILD, suggesting that MAILD model could replace EAM model in IIM-ILD research.
2024-11-01·JOURNAL OF THROMBOSIS AND HAEMOSTASIS
CpG oligonucleotides induce acute murine thrombocytopenia dependent on toll-like receptor 9 and spleen tyrosine kinase pathways
Article
作者: Henry, Scott ; Semple, John W ; Italiano, Joseph E ; Marcoux, Geneviève ; Shen, Lijiang ; Rebetz, Johan ; Johansson, Karl ; Narayanan, Padma ; Shannon, Oonagh ; Maouia, Amal
BACKGROUND:
CpG oligonucleotides (ODNs) are synthetic single-stranded DNA sequences that act as immunostimulants. They have been increasingly used to treat several cancers; however, thrombocytopenia is a potential recognized side effect of some sequences.
OBJECTIVES:
We tested the ability of 2 CpG ODNs (ODN 2395 and ISIS 120704) to induce thrombocytopenia when administered to BALB/c mice and determined mechanisms associated with thrombocytopenia.
METHODS:
BALB/c mice were prebled and then injected with titrated doses of CpG ODNs, and platelet counts were determined. The mice were treated with intravenous immunoglobulin (IVIg) or various inhibitors and antagonists of toll-like receptor 9 (TLR9) and spleen tyrosine kinase (Syk) to determine their effects on thrombocytopenia.
RESULTS:
Compared with saline-treated mice or mice treated with 2'-O-methoxyethyl-modified antisense ODN, both ODN 2395 and ISIS 120704 induced acute dose-dependent thrombocytopenia within 3 and 24 hours, respectively. The thrombocytopenia was associated with significant increases in plasma monocyte chemoattractant protein 1. IVIg administration significantly rescued the CpG ODN-induced thrombocytopenia, as did treatment with either a Syk inhibitor or TLR9 antagonists. In vitro, CpG ODN could activate human platelets and this correlated significantly with enhanced IVIg- and Syk-dependent phagocytosis by THP-1 monocytes.
CONCLUSION:
These results suggest that CpG ODNs induce acute inflammatory-associated (IVIg-sensitive) thrombocytopenia that can be alleviated by Syk- or TLR9-blockade, and an IVIg- and Syk-dependent platelet clearance pathway appears primarily responsible for the thrombocytopenia.
2022-07-01·Vaccine
Development and immunogenicity evaluation of porcine deltacoronavirus inactivated vaccine with different adjuvants in mice
Article
作者: Lu, Si-Jia ; Xiang, Yu-Qiang ; Ma, Meng-Yao ; Zhao, Fu-Jie ; Zheng, Lan-Lan ; Hu, Hui ; Wang, Nian-Xiang ; Liu, Lin-Tao ; Wang, Zi ; Jia, Xin-Hao
Porcine deltacoronavirus (PDCoV) is a novel coronavirus that causes diarrhea in pigs of various ages, especially in suckling piglets, and there are no effective measures to prevent and control PDCoV currently. In this study, two adjuvants Al(OH)3 and ODN2395 working through different mechanisms were used to prepare inactivated PDCoV vaccines, and the immune effects of PDCoV inactivated vaccines were assessed in mice. From the results, we found that both PDCoV/Al(OH)3 vaccine and PDCoV/2395 vaccine could induce IgG and neutralizing antibodies with high levels in mice. At the same time, cytokines of IFN-γ, IL-4 and chemokine ligand of CXCL13 in serum were significantly increased after immunization, and reached the highest levels in PDCoV/2395 vaccine group, which suggested that PDCoV/2395 could promote the production of both Th1 and Th2 polarized cytokines. In addition, histopathological observations showed that vaccination helped mice resist PDCoV infection. These results indicated that both the two inactivated vaccines have good immune effects. Moreover, the PDCoV/2395 vaccine worked better than the PDCoV/Al(OH)3 vaccine for PDCoV/2395 having the good ability to induce both humoral and cellular immunogenicity. The PDCoV/2395 inactivated vaccine developed in this study might be an effective tool for the prevention of PDCoV infection.
100 项与 ODN2395 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 肝癌 | 临床前 | 美国 | 2021-04-10 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
No Data | |||||||
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或

药物交易
使用我们的药物交易数据加速您的研究。
登录
或

核心专利
使用我们的核心专利数据促进您的研究。
登录
或

临床分析
紧跟全球注册中心的最新临床试验。
登录
或

批准
利用最新的监管批准信息加速您的研究。
登录
或

特殊审评
只需点击几下即可了解关键药物信息。
登录
或

生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
