预约演示
更新于:2026-03-11
Recombinant epidermal growth factor gel(Guilin Pavay Gene Pharmaceutical)
重组人表皮生长因子(桂林华诺威基因药业有限公司)
更新于:2026-03-11
概要
基本信息
原研机构 |
在研机构 |
非在研机构- |
权益机构- |
最高研发阶段批准上市 |
最高研发阶段(中国)批准上市 |
特殊审评- |
登录后查看时间轴
关联
100 项与 重组人表皮生长因子(桂林华诺威基因药业有限公司) 相关的临床结果
登录后查看更多信息
100 项与 重组人表皮生长因子(桂林华诺威基因药业有限公司) 相关的转化医学
登录后查看更多信息
100 项与 重组人表皮生长因子(桂林华诺威基因药业有限公司) 相关的专利(医药)
登录后查看更多信息
10
项与 重组人表皮生长因子(桂林华诺威基因药业有限公司) 相关的文献(医药)2026-01-01·Nursing in Critical Care
Individualised Wound Treatment Strategies for Skin Lesions Caused by Calcium Gluconate Extravasation in Neonates: A Case Report
Article
作者: Li, Jiarong ; Chen, Xushu ; Li, Xiaowen ; Liu, Chunhua ; Yan, Jing ; Hu, Yanling ; Liu, Yan
ABSTRACT:
Extravasation of calcium gluconate solution is a rare yet serious complication in neonatal intensive care units (NICUs), capable of causing significant skin necrosis, ulceration and long‐term functional impairment. This study reports a case of such injury and describes an effective, individualised strategy for wound management. An 18‐day‐old, 4200 g male infant, diagnosed with hypocalcaemia (serum calcium: 1.6 mmol/L) at a hospital in China, experienced calcium gluconate extravasation following peripheral intravenous supplementation. This complication resulted in localised skin swelling, ulceration and necrosis. After eight days of unsuccessful conventional management, the infant was transferred to a tertiary maternity and children's hospital in Sichuan, China. We implemented a structured treatment protocol involving combined debridement to excise necrotic tissue and calcium deposits. The wound was then managed with a tailored regimen: Lipido‐colloid dressings with silver ions were applied to control infection, alongside recombinant human epidermal growth factor gel to stimulate cellular regeneration. A moist wound environment was maintained using alginate hydrogel and foam dressings. The silver‐containing dressings were discontinued after 10 days upon resolution of erythema and cessation of exudate. The infant was discharged after a 32‐day course with satisfactory wound epithelialisation and full preservation of joint mobility. One‐year follow‐up confirmed normal limb function and the absence of scar contracture. A structured, individualised wound management strategy was effective in treating skin injuries resulting from calcium gluconate extravasation. The combination of surgical debridement, advanced wound dressings and adjunctive growth factor therapy facilitated tissue regeneration, promoted healing and supported functional recovery. An integrated protocol of surgical debridement, advanced wound dressings, and adjunctive growth factor therapy effectively fostered tissue regeneration, accelerated healing, and underpinned functional recovery.
2025-12-01·Biochemistry and Biophysics Reports
Chinese traditional medicine complex hemorrhoidal analgesic cream promotes wound healing in diabetic rats after anal fistula surgery via Keap1/Nrf2 signaling pathway
Article
作者: Liu, Delong ; Liu, Jian ; Yin, Zhitao ; Tian, Xiaojun ; Wang, Chunxiao ; Yuan, Hexue
This study to elucidate how hemorrhoidal analgesic cream (HAC), grounded in the traditional Chinese medicine (TCM) 'elevation and causation' theory, promotes postoperative wound healing after anal fistula surgery in diabetic rats by modulating the Keap1/Nrf2 signaling pathway. We used high-sugar and high-fat chow combined with streptozotocin (STZ) to induce diabetic rats to establish a postoperative wound model of anal fistula. The rats were divided into a blank control group, model group, wound-only group, experimental group (HAC treatment), and positive control group (recombinant human epidermal growth factor gel). HAC's impact on wound healing was evaluated by glycated hemoglobin (HbA1c), serum inflammatory factors (TNF-α, IL-6), oxidative stress markers (SOD, MDA), and Nrf2 pathway proteins and mRNA. The results showed that the wound healing rate was significantly increased in the HAC group (92.85 ± 3.41 %, P < 0.01), the levels of HbA1c were decreased (P < 0.05), the levels of TNF-α, IL-6, and MDA were decreased (P < 0.01), the activity of SOD was increased (P < 0.05), and the Keap1/Nrf2 signaling pathway was activated. The study demonstrated that HAC could reduce oxidative stress and inflammatory responses by regulating the Keap1/Nrf2 signaling pathway, which validates its scientific value in promoting wound healing after diabetes mellitus (DM) fistula surgery.
2025-03-01·OPHTHALMIC PLASTIC AND RECONSTRUCTIVE SURGERY
Experimental Study of Ultra-Pulsed CO2 Fractional Laser Combined With Recombinant Human Epidermal Growth Factor Gel in the Treatment of Eyelid Keloid
Article
作者: Qu, Yixin ; Li, Xingyi ; Lin, Xianchai ; Mao, Zhen ; Huang, Danping ; Chen, Rongxin ; Gao, Wuyou
Purpose::
Keloid (KD) and hypertrophic scars are prevalent and result from excessive growth of dermal tissue after skin damage. This review focused on the clinical application of the ultra-pulsed CO2 fractional laser combined with recombinant human epidermal growth factor (rHEGF) gel in patients with eyelid KD.
Methods::
Patients (N = 98) with KD who underwent surgery were randomly divided into a study group (ultra-pulsed CO2 fractional laser combined with rHEGF gel therapy, N = 49) and a control group (ultra-pulsed CO2 fractional laser therapy, N = 49). Besides, 5 cases dropped out of the study, including 2 cases in the study group and 3 cases in the control group. Finally, 47 cases of the study group and 46 cases of the study group were included in the analysis. The clinical baseline data such as sex, age, body mass index, scar area, etiology, Vancouver Scar Scale score, Patient and Observer Scar Assessment Scale score, four-item itch questionnaire score, serum interleukin-6 (IL-6), IL-10, and tumor necrosis factor-α level expression were recorded in the study group (N = 47) and the control group (N = 46).
Results::
There was no significant difference in gender, age, body mass index, scar area, etiology, Vancouver Scar Scale score, Patient and Observer Scar Assessment Scale score, 4-item itch questionnaire score, IL-6, IL-10, and tumor necrosis factor-α levels between the patients treated with ultra-pulse CO2 fractional laser + rHEGF gel and those only treated with ultra-pulse CO2 fractional laser (p > 0.05). Vancouver Scar Scale scores, Patient and Observer Scar Assessment Scale scores, and four-item itch questionnaire scores of patients with eyelid KD decreased to a greater extent than those treated with ultra-pulsed CO2 fractional laser combined with rHEGF gel (p <0.01). Compared with ultra-pulsed CO2 fractional laser treatment, ultra-pulsed CO2 fractional laser combined with rHEGF gel was more efficacious in treating patients with eyelid KD, with a lower incidence of adverse effects and a 1-year recurrence rate.
Conclusions::
Ultra-pulsed CO2 fractional laser combined with rHEGF gel can significantly improve the scar status and scar itching in patients with eyelid KD, with an obvious therapeutic effect, a low incidence of adverse effects, a 1-year recurrence rate, and high safety, which is worthy of popularization and application.
100 项与 重组人表皮生长因子(桂林华诺威基因药业有限公司) 相关的药物交易
登录后查看更多信息
外链
| KEGG | Wiki | ATC | Drug Bank |
|---|---|---|---|
| - | - | - |
研发状态
10 条最早获批的记录, 后查看更多信息
登录
| 适应症 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|
| 烧伤 | 中国 | 2002-12-23 | |
| 皮肤溃疡 | 中国 | 2002-12-23 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
No Data | |||||||
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或

药物交易
使用我们的药物交易数据加速您的研究。
登录
或

核心专利
使用我们的核心专利数据促进您的研究。
登录
或

临床分析
紧跟全球注册中心的最新临床试验。
登录
或

批准
利用最新的监管批准信息加速您的研究。
登录
或

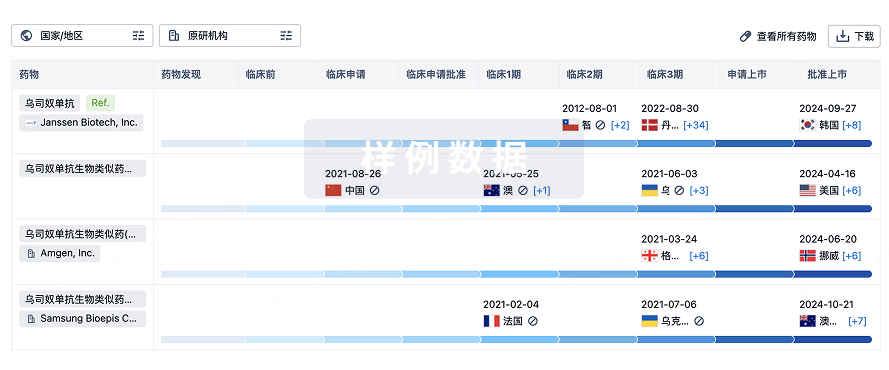
生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
特殊审评
只需点击几下即可了解关键药物信息。
登录
或

生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
