预约演示
更新于:2026-06-06
Arcitumomab technetium-99m
更新于:2026-06-06
概要
基本信息
在研机构- |
非在研机构 |
权益机构- |
最高研发阶段撤市 |
首次获批日期 欧盟 (1996-10-04), |
最高研发阶段(中国)- |
特殊审评孤儿药 (美国) |
登录后查看时间轴
结构/序列
使用我们的ADC技术数据为新药研发加速。
登录
或

Sequence Code 143480H

Sequence Code 143724L

关联
100 项与 Arcitumomab technetium-99m 相关的临床结果
登录后查看更多信息
100 项与 Arcitumomab technetium-99m 相关的转化医学
登录后查看更多信息
100 项与 Arcitumomab technetium-99m 相关的专利(医药)
登录后查看更多信息
13
项与 Arcitumomab technetium-99m 相关的文献(医药)2004-05-01·Clinical nuclear medicine3区 · 医学
Bilateral Ovarian Metastases From Colon Carcinoma Visualized on F-18 FDG PET Scan
3区 · 医学
Article
作者: David L. Lilien ; Travis Henley ; Madhusudhan P. Reddy ; Mohan R. Ramaswamy
Ovarian metastases (Krukenberg tumor) from primary colorectal carcinoma are relatively uncommon despite the fact that the colon is the most frequent location for gastrointestinal primaries. There are a number of diagnostic and management issues that appear to impact on survival, including timing of definitive diagnosis of Krukenberg tumors such as before, after, or at the same time as diagnosis of the gastrointestinal primary tumor, menopausal status, concurrent pregnancy, role of debulking, and prophylactic oophorectomy. We present a case of bilateral ovarian metastases visualized on fluorine-18-2-fluro-2-deoxy-D-glucose-positron emission tomography (F-18 FDG PET) and CEA Scan using Tc-99m arcitumomab after right hemicolectomy for cecal carcinoma. PET is a useful modality to evaluate for metastases.
2001-11-25·Colorectal disease : the official journal of the Association of Coloproctology of Great Britain and Ireland3区 · 医学
Immunoscintigraphy and intra‐operative radioimmunodetection in the treatment of colorectal carcinoma
3区 · 医学
Article
作者: P. Hladik ; J. Bedrna ; K. Smejkal ; L. Strnad ; Z. Voboril ; D. Simkovic ; J. Vizda
Purpose:
Intra‐operative radioimmunodetection of malignant involved lymph nodes follows the pre‐operative immunoscintigraphy in the treatment of patients with colorectal carcinoma. The aims of this clinical study were to determine the sensitivity of the method, to compare the results in study when using Oncoscint and CEA‐Scan and to evaluate the importance of the method of surgery and postoperative adjuvant therapy.
Patients and methods:
121 patients with colorectal tumours (106 primary and 15 recurrent) were operated on using radioimmunoguided surgery (RIGS). The study compared results of pre‐operative immunoscintigraphy, intra‐operative radioimmunodetection and postoperative histological examination. Histological investigation used classical H&E staining. In histologically negative and RIGS positive cases the immunohistochemical investigation was supplemented. Two radiopharmaceuticals were used Oncoscint CR 103 (MAb B72.3, Satumomab Pendetide), labelled with 111In in 56 patients and CEA‐Scan (IMMU 4‐Fab′ fragments MAb against CEA, Arcitumomab), labelled with 99mTc in 65 patients.
Results:
The relationship between RIGS positive results and histological examination was statistically assessed after 38 operations and the most acceptable RIGS evaluating index was determined. All subsequent results were evaluated by this index. Immunoscintigraphy of tumour was positive in 112 cases (92.6%). Fifty‐five RIGS positive cases of malignant infiltrated lymph nodes were confirmed by 43 histologically positive examinations (78%). In this group 9 cases were discovered only by immunohistochemistry. Sixty‐six remaining RIGS negative results were confirmed in 62 (94%) cases by negative histology.
Conclusions:
Both immunoscintigraphy and RIGS enable one to make a more accurate diagnosis. While treating the primary disease the use of RIGS may help in assessment of necessary extent of operation performance and in staging of the disease by revealing occult lymph nodes involved. Pre‐operative immunoscintigraphy seems to be a useful diagnostic method for detection of tumour recurrence. When comparing two radiopharmaceuticals used, CEA‐Scan seems to be more suitable for diagnostic studies, but using the Oncoscint for tumour recurrence detection had some specific benefit, too.
2000-06-01·Journal of nuclear medicine : official publication, Society of Nuclear Medicine
Safety and efficacy of arcitumomab imaging in colorectal cancer after repeated administration.
Article
作者: Petrelli, N ; Goldenberg, D M ; Serafini, A ; Wegener, W A
METHODS:
Human antimouse antibody (HAMA) response, adverse events, clinical laboratory values, and diagnostic imaging results were evaluated in 44 patients (24 men, 20 women; age range, 2878 y) after repeated arcitumomab administration (44 second and 3 third injections). Most patients initially had Dukes' class B or C colorectal cancer and had known or occult disease recurrence and elevated serum carcinoembryonic antigen levels at the time of the repeated injection.
RESULTS:
At the repeated injection, in no patient did elevated HAMA titers develop, hematology and serum chemistry changes were clinically insignificant, and only 1 adverse event (eosinophilia) was judged at least possibly related to arcitumomab. Arcitumomab imaging results at the second injection were comparable with those obtained in phase III trials after a single injection of arcitumomab, having a 78% per-lesion concordance with CT in the abdomen and pelvis and a 73% sensitivity and 94% specificity based on 9 patients with cancer confirmed surgically at 11 anatomic sites and excluded at 16 sites.
CONCLUSION:
These data indicate that at least 2 injections of arcitumomab can be given safely to patients with colorectal cancer, without increased immunogenicity and with imaging efficacy equivalent to the first administration.
2
项与 Arcitumomab technetium-99m 相关的新闻(医药)2026-01-12
BiotechJK是一个非营利性技术组织,成立于2016年,创始人为吴文哲,初心是为了解决生物制药相关技术问题,关注行业发展动态。
当下生物制药行业主题较多,但缺乏针对技术问题的深入探讨。BiotechJK在线上建立微信群讨论交流的基础上,定期组织线下技术交流活动。
交流活动汇聚广大英才,针对工作的痛点,明晰法规内的模糊条款,讨论并梳理出业内认可的共识性意见,在其基础上能梳理出行业内的指导性文件,并成立相关资料库,服务生物制药行业。
使 命
技术降低成本,科技改变生活
愿 景
行业技术标杆,标准引领全球
提 倡
创新、合作、共享、互赢
如有不同观点,可以在下方评论区发表见解
02
———
Fab的表达
在基因工程抗体中,Fab类抗体有许多优势,如相对分子质量小、组织分布特异性强和免疫原性低等,使Fab类抗体成为近几十年来的研究热点。在已上市应用于临床的Fab片段药物及诸多临床前研究中,制备Fab的常用方法是酶消化法;在Fab的诸多表达系统,如细菌、酵母、哺乳动物细胞、昆虫和植物表达系统中,应用最为广泛的是大肠杆菌(E.coli)表达系统。
2.1 Fab的酶法生成制备
酶解法是通过特定的蛋白酶对全长的抗体分子进行水解从而获得期望的片段抗体。该方法制备片段抗体的特点是生产成本低、转化率高、工艺简便、便捷快速。目前,用于酶切抗体的酶主要包括木瓜蛋白酶、胃蛋白酶和无花果蛋白酶,其中木瓜蛋白酶消化IgG抗体是用于获得Fab最传统的方法。FDA批准并应用于临床的多数Fab类药物均是通过木瓜蛋白酶消化IgG所获得的。比如阿昔单抗(abciximab)、阿西莫单抗(arcitumomab)、响尾蛇多价免疫Fab和地高辛免疫Fab。基因工程抗体的出现使抗体生产得到了革新,但酶切法制备Fab类抗体因其独特的优越性并不会被基因工程抗体取代,尤其是非重组Fab类抗体片段的生成。
酶解法依据其使用的方法,通常可分为游离酶切和固定化酶切。游离酶切反应在溶液中完成,通过优化酶解条件可提高酶解效率;固定化酶切是通过吸附、包埋、交联和结合等方法将酶固定在一定的载体上并在有限的范围内进行催化反应。与游离酶切相比,固定化酶切可更好地控制消化过程,并有效地将酶解产物和酶分开。固定化酶切的切割程度可通过控制消化时间或过柱流速来调节;无酶抗体结合物的产生;可快速清除酶解产物中的酶,无须离子交换法来分离抗体片段;增加酶对热稳定性和自溶稳定性,有利于固定化酶的长时间维护等,使其在很多应用中逐渐取代了游离酶切。
2.2 Fab的大肠杆菌表达
大肠杆菌因其具有成本低、生长速度快、转化效率高、可在短时间内获得目标蛋白并对其进行纯化和分析,且最终蛋白产量较高等优势,可作为生成Fab的独特系统。重组Fab向E.coli 周质空间分泌需要一段15~30个氨基酸的信号肽引导。在Fab周质分泌表达中,常用的信号肽是主要外膜蛋白A(OmpA)和果胶裂解酶B(pelB)。此外,也可用相关软件从基因组中快速预测更适合目的Fab周质表达的信号肽。
除了在Fab片段前引入信号肽序列外,还可以通过改造宿主菌实现Fab的可溶性表达。有研究发现,大肠杆菌硫氧还原蛋白酶和谷胱甘肽还原酶缺陷株(trxB,gor)无硫氧还蛋白和谷胱甘肽还原酶活性,可提供一个有利于Fab正确折叠的氧化性胞质环境,功能性Fab在大肠杆菌trxB/gor突变株中可高产率表达。如Novagen公司的FA113菌株和Origami系列菌株皆为此类型突变菌,有利于Fab中二硫键的形成,且增加其可溶性,活性更高。
此外,特定培养条件可促使周质Fab在上清中的累积,其原因可能是诱导表达后周质中Fab积聚促使菌体裂解,也可能是特定的培养条件增加了大肠杆菌外膜的溶解性。上清液中的高浓度Fab是周质中Fab渗透到胞外的,因此从上清中纯化所得的Fab比从周质和裂解产物中纯化所得的Fab纯度更高。通常,不同的宿主菌、培养基、摇菌速率和通氧量,Fab的总产率及胞外渗透率有明显的不同。在分批补料葡萄糖培养基中,Fab表达总量及胞外产率最高,且与250r/min摇速的2%~17%胞外渗透率相比,150r/min的胞外渗透率高至75%;在含甘油的自诱导培养基中,250r/min条件下Fab的总产率是150r/min的5~9倍,且胞外Fab比率从10%增加至20%~90%;低通氧量会促进Fab的胞外分泌。这些发现对Fab的小规模生产有实际意义,且Fab胞外分泌对培养条件的依赖为Fab表达的控制和定位提供了有效途径。
2.3 Fab的其他表达系统
由于原核表达缺少真核转录后的蛋白修饰过程,酵母、昆虫和植物细胞表达系统的转录后加工修饰体系与哺乳动物细胞不完全相同,且表达的蛋白在糖链的结构和组分上与哺乳动物表达系统表达的蛋白有所差异。杆状病毒昆虫表达系统可有效表达Fab抗体片段,由于昆虫系统的糖基化方式与人类不同,临床治疗性抗体表达通常不建议采用此类方法。
无细胞系统也可产生功能性Fab抗体片段。无细胞蛋白质合成系统是一种以外源mRNA或DNA为模板的体外翻译系统,通过向细胞抽提物的酶系中补充底物和能源物质来合成蛋白质。与传统的体内重组表达系统相比,体外无细胞合成系统更简便、更快、更易操控,且可提供一个合适、可控且稳定的氧化还原电势辅助功能性Fab的表达。但该系统最具挑战的是轻、重链二硫键的形成及Fab的折叠;后者可通过使用谷胱甘肽氧化还原缓冲液、纯化氧化还原酶及添加分子伴侣等解决。无细胞系统表达Fab具有可扩展性和提升空间,可使得Fab产率优化,这将会是一个有前景的Fab生成方法。
抗体片段Fab在细胞质中合成并运输到周质腔,因此蛋白翻译后的折叠、转运过程及宿主细胞本身均会对其产生影响。不同抗体片段在表达过程中同时也受到抗体序列影响,这可能与其主要影响目标蛋白的合成和折叠有关。通常,新生多肽有两种去向;折叠与聚集,往往低温有利于蛋白折叠的进行。在培养基中加入0.4mol/L蔗糖后,在非常低的异丙基-β-D-硫代半乳糖苷(0.02~0.03mmol/L)诱导时可以增加抗体的表达量。
当在一种表达系统中效果欠佳时,可考虑采用以下方法: ① 尝试使用不同的载体系统、标签和融合蛋白;② 将此表达系统导入不同的宿主菌中表达;③ 如果目的基因的编码序列含大肠杆菌的稀有密码子较多,可同时表达氨基酸的tRNA基因;④ 共表达分子伴侣或折叠酶,有时可提高抗体的可溶表达。
03
———
F(ab')2 的制备表达
与单价抗原结合活性片段Fab相比,F(ab')2 是双价抗原结合活性片段,表观亲和力比Fab高;因其分子量较全长IgG分子减少了1/3(约100kDa),而对肿瘤的穿透能力较强,免疫原性降低,同时在肿瘤部位滞留时间较长,在实验动物体内的半衰期也比Fab长;由于片段抗体F(ab')2 缺乏恒定区,减少了与表达Fc受体的细胞发生非特异性结合的机会,因此在免疫诊断、医学影像和临床治疗方面有着重要的应用价值。
F(ab')2 片段可用胃蛋白酶酶解的方法制备,但其效率较低。随着分子生物学技术迅速发展,适合于双特异性抗体的构建模式同样适用于F(ab')2 双价片段抗体的表达制备。此外,还有如下方法,① 抗体片段的化学偶联;② 用短肽接头构建双价抗体片段;③ 亮氨酸拉链聚合;④ 表达免疫球蛋白的绞链区等。
抗体片段的化学偶联制备是指应用化学试剂[如邻苯二马来酰亚胺(O -PDM)、二硫代硝基苯甲酸(DTNB)和N-琥珀酰-3-(2-吡啶二巯基)丙酸盐(SPDP)等化学偶联剂],通过氧化还原反应将表达纯化的抗体片段Fab通过二硫键或硫醚键连成一个双价F(ab')2 分子。Carter等报道用大肠杆菌(E. coli)表达人源化HuMab4D5-8抗体Fab片段,之后用化学偶联法获得双价的F(ab')2 分子,产量可达2g/L,这一方法虽然引入外源性的化学偶联剂,但70%的产物以双价的抗体片段形式存在。
采用短肽接头构建双价抗体片段是将2个Fab的重链基因串联之后与相应轻链基因在宿主细胞中共表达,产生线型的F(ab')2,即L-F(ab')2。在L-F(ab')2 中,位于C末端的抗原结合位点与抗原的结合受到空间位阻的影响较大,表观亲和力介于F(ab')2和Fab之间。通常,可用5肽RTVAA、7肽RTVAAPS、10肽RTVAAPSVFI(缺乏柔韧性)或者(Gly4Ser)3 将Fab的重链基因串联后,和表达的轻链体外蛋白复性而获得L-F(ab')2,这一过程也可用来F(ab')2 体外的组装。
采用亮氨酸拉链聚合构建双价抗体片段可通过修饰Fos或Jun型亮氨酸拉链,在其两端分别加上一个Cys,然后将Fos或Jun的N末端与Fab的C 末端相融合而形成F(ab')2。二聚化结构域(dimerization domain)能促使蛋白质亚基之间装配成功能性二聚体。有报道显示,通过表达具有亮氨酸拉链聚合序列Fab段,之后将分别制备的针对不同靶点的Fab段体外混合,可生成双特异性二聚体形式的F(ab')2 片段,通常也可通过引入互补的杵臼结构(knobs into holes)修饰CH3界面来提高二聚化形成。研究显示,通过亮氨酸拉链连接抗体片段Fab其效率较高。
表达免疫球蛋白的绞链区构建双价抗体片段即通过在重链的Fd的羧基端加上小肽(CPP)3 的编码序列,模拟天然免疫球蛋白的绞链区来制备双价抗体片段F(ab')2。由于天然免疫球蛋白重链CH1的C 末端和CH2的N 末端交界处有1~2个Cys残基,它们可以两两氧化生成二硫键将2条重链紧密地共价结合在一起。这样,在重链Fd的3'端连接上小肽(CPP)3 的编码序列,富含Cys而且相邻的两个Cys之间由Pro隔开,使这部分肽链充分伸展但不能自由旋转和弯曲,不易形成链内二硫键,并且使Cys残基不易被其他氨基酸残基所遮掩,活性基团(—SH)充分暴露。片段抗体在表达过程中提高了重链间二硫键的形成的概率,提高了表达产物中F(ab')2 的含量。早在2002年,我国协和医科大学也报道了通过在CH1基因的末端添加一段二聚化结构的编码序列的方法,实现了从细菌周质腔隙中提取可溶性抗CD20嵌合F(ab')2 抗体分子;该分子具有天然三维立体结构,不需要进行变性复性,经蛋白G和Sephacyl S200 -HR分子筛两步分离纯化,纯度可达90%以上。
美妥昔单抗是鼠源F(ab')2 片段抗体,通过胃蛋白酶酶解的方法制备。将其与放射性元素131I标记,所制备的“利卡汀”用于原发肝癌的免疫靶向治疗。“利卡汀”可特异性地与肝癌细胞膜上的HAb18G/CD147抗原结合,将其荷载的放射性碘输送到肿瘤部位,从而产生抗肿瘤作用。该片段抗体F(ab')2 在临床应用中显示了良好的前景,同时也是全球第一个运用单抗进行核素标记实施靶向治疗原发性肝癌的分子靶向药物。一项纳入106例肝癌患者的多中心Ⅱ期临床研究结果显示,经过1~2个疗程“利卡汀”治疗后,患者21个月生存率为44.54%。其中73例患者完成了2个疗程的治疗,6例(8.22%)部分缓解(PR),14例(19.18%)完全缓解(CR),43例(58.90%)稳定(SD)。一项纳入60例经过肝移植手术后的Ⅲ期/Ⅳ期肝癌患者的利卡汀临床试验研究显示,患者一年内复发率显著降低,降低了30.4%,生存率提高了20.6%。同时“利卡汀”联合经导管肝动脉栓塞化疗术(transcatheter arterial chemoembolization,TACE)治疗原发性肝癌具有更显著的疗效,一项纳入148名肝癌患者的临床试验结果显示,与单独TACE治疗相比,利卡汀联合TACE治疗可有效延长患者的总体中位生存期。
关注更多内容请加入公众号 BiotechJK,欢迎志同道合的人一起加入
为您分享行业最新动态 共同讨论生物制药相关专业知识
公众号有相关专业讨论群(BiotechJK、BiotechJK2)
微信加我(wuwz92)审核入群,交流或商务合作
请备注:姓名 公司 职能/意向
吴文哲
2023-02-28
点击上方的 行舟Drug ▲ 添加关注浅析抗体偶联核素类产品药学研发和评价关注点来源《中国新药杂志》2023年第32卷第2期作者王雪,李倩,韦薇国家药品监督管理局药品审评中心摘要抗体偶联核素药物(antibody radionuclide conjugates,ARC)采用的放射性核素与抗体通过连接臂和螯合剂偶联,可以发挥体内诊断或治疗等不同功能。目前,ARC作为放射性核素偶联药物(radionuclide drug conjugates,RDC)重要的产品类型,正在开展临床试验的候选药物数量较多。但是,国内工业界在开发临床应用级ARC产品时面临诸多挑战。因此,本文总结了ARC产品的相关法规及最新研究进展,从生产工艺、质量研究与控制、稳定性等方面对此类产品的药学研究与评价的关注点展开讨论,以期促进此类产品的临床转化与应用。关键词抗体偶联核素; 药学研发; 药学评价; 关注点_正文_抗体偶联药物(antibody drug conjugates,ADC)已成为国内外研究较为充分、商业化较为成功的药物类型之一。随着核医疗与核技术的创新和迭代,另一种类似的偶联药物设计—放射性核素偶联药物(radionuclide drug conjugates,RDC)近年来也迎来了研发热潮[1]。RDC在药物结构组成上与ADC类似,主要由介导靶向定位作用的抗体或小分子(ligand)、连接臂(linker)、螯合物(chelator)和细胞毒性基团/显像核素(放射性同位素,radioisotope)构成[2]。稍有区别的是,RDC的有效载荷为功能性的放射性同位素,因此其连接臂上需连接能装载同位素的特定官能团结构的螯合剂。根据靶向配体的不同类型,RDC又可细分为: 抗体偶联核素药物(antibody radionuclide conjugates,ARC)、多肽偶联核素药物(peptide radionuclide conjugates,PRC)和小分子偶联核素药物(small molecular radionuclide conjugates,SMRC)。RDC突出特点还在于更换使用的放射性核素种类,可以发挥诊断或治疗的不同功能,从而实现“可视即可治”的诊疗一体化功能[3]。在临床研究与基础科研领域,用于显像诊断的核素包括2类: 其一是以18F,68Ga,89Zr,64Cu等为代表的释放正电子(β+)的核素,利用正电子发射断层扫描(positron emission tomography,PET)即可获得全身各方位的断层扫描图像; 其二是以99mTc,111In等为代表的释放单光子的核素,利用单光子发射计算机断层扫描(single-photon emission computed tomography,SPECT)亦可实现可视化成像。这些技术也可以扩展到结合了PET(或SPECT)和计算机断层扫描(computed tomography,CT)的混合成像系统,形成由伽马射线和X射线(PET/CT)绘制的2个图像,从而实现更高的诊断效率和准确性。用于治疗的核素主要包括2类: 其一是以225Ac,223Ra,213Bi,211At等为代表的释放α粒子(其本质为2个质子与2个中子的He原子核),其二是以188Re,177Lu,131I,90Y,89Sr等为代表的释放β射线(负电子)的核素。主要的作用机制是通过产生电离辐射导致细胞DNA损伤,最终造成靶细胞死亡。放射性核素靶向治疗是以肿瘤特异性高表达的分子为靶点,利用高亲和力特异性结合的靶向分子(如抗体分子或多肽分子等)将放射性核素精准递送到肿瘤部位,利用核素衰变产生的射线发挥杀伤作用,对肿瘤进行特异性、靶向性内照射治疗。放射性核素靶向药物通过核射线不仅杀伤肿瘤组织表层或浅层的肿瘤组织及细胞,同时利用核射线的穿透力杀伤实体瘤内部的肿瘤细胞,即“交叉火力”效应。与单纯的生物药物和化学药物相比,放射性药物具有更强的杀伤力。另外,对于通过影像学诊断和外科手术无法及时诊断的小体积肿瘤病灶或转移灶,体内放射靶向治疗将发挥其独特的疗效。本文结合国内外ARC类产品的最新研发进展,探讨此类产品的药学研究内容与评价关注点,以期促进国内同类产品的注册申报与临床转化。1国内外上市及研究现状核素类药物在临床上的使用最早是从1913年的Ra元素开始的,而正式获批的药物则是在1951年,美国FDA首次批准Na131I用于甲状腺疾病的治疗,首个单光子诊断药物是于1991年上市的99mTc标记的心肌灌注,此后又相继出现了68Ga,201Tl,111In广泛用于心脏、脑、肾脏、骨、肺脏等多种疾病的诊断。随着PET/CT的出现,1994年美国FDA批准的18F-FDG引领了整个核医学的进步,2013年拜耳的α治疗药物223RaCl2获批上市用于治疗前列腺癌骨转移,核药领域不断发展[4]。如今RDC领域的研发也进入了快车道,国际范围内研发比较成熟的靶点包括用于神经内分泌瘤诊疗的生长抑素受体SSTR,以及用于前列腺癌诊疗的前列腺特异性膜抗原PSMA,目前均有相应的诊疗产品上市,但多以小分子/多肽偶联核素产品为主,ARC作为RDC药物重要的产品类型,获批上市的较少。1996年美国FDA批准的CEA-Scan是首个获批上市的诊断用ARC药物,用于经组织学证实的结肠癌或直肠癌患者的复发和/或转移的影像学检查; 2002年上市靶向CD20的Zevalin(90Y-ibritumomab tiuxetan)是第一个获批的治疗用ARC药物,用于非霍奇金淋巴瘤的治疗[5]。截至2022年10月20日,如表1所示(数据来自医药魔方数据库)国际上已经批准上市的ARC药物较少,且多为2010年前上市的产品。随着近些年生物技术的发展,此类产品的质量研究更加透彻,风险控制也更加完善。文章内容由凡默谷小编查阅文献选取,排版与编辑为原创。如转载,请尊重劳动成果,注明【来源:凡默谷公众号】。2ARC产品的药学研究与评价现状2.1 国内外对放射性药物的相关法规及指导原则美国无放射性药物的专属法律法规,但《联邦法规》和《美国药典》等主要的药品法规中,均考虑了放射性药物注册申报的特殊文件要求,建立了多项技术指导原则[6-8],对诊断用药和治疗用药的考量重点、PET药物申请和cGMP要求等,提供了详细的参考指引。美国FDA还设立了专门的放射性药物审批部门负责放射性药物的注册审批。欧盟目前已颁布的《放射性药物研究指南》[9]和《基于单克隆抗体的放射性药物指导原则》[10],规定了放射性药物上市许可或授权药品变更申请申报资料的具体要求,《欧洲药典》中也有针对一些放射性核素的专论。欧盟视放射性药物为一般性药物管理,并未设置专门的审批机构。我国现行版的《药品注册管理办法》部分考虑了放射性药物的特殊性,药学研究参照化学药物相应要求进行。目前《中华人民共和国药典》2020年版四部中已纳入通则1401(放射性药品检定法)、指导原则9501(正电子类放射性药品质量控制指导原则)和9502(锝[99mTc]放射性药品质量控制指导原则)。2.2 ARC类产品的药学研发及评价的挑战ARC类产品药学研究和评价主要依据上述国内和国外的法规、技术要求、指导原则等。相对于工艺研究和质量控制研究成熟的抗体药物或放射性药物,ARC类产品的药学开发与评价存在着诸多挑战。如原材料方面,核素属放射性药物,引入化学计量低、有特定的物理半衰期、放射性活度随时间的延长而减少等特点。生产工艺方面,核素物理半衰期短,原液和制剂通常采用连续生产; 产能放大受限,一般每批要仅供较少人数(几人份至几十人份)使用。质量研究方面,除考虑抗体相关的质量研究内容,还需关注放射性药物的特殊性,如纯度(放化纯、化学纯度、放核纯)、放射性核素对抗体的影响、标准品的选择合理性等。上述问题均对ARC产品的药学研究与评价提出了挑战。3ARC类产品的药学研究内容与评价考虑3.1 抗体部分药学研究与评价关注点ARC类产品的靶向配体即抗体部分,可参考“人用单克隆抗体质量控制技术指导原则”及“人用重组单克隆抗体制品总论”、“人用重组DNA蛋白制品总论”、ICH Q6B等相关技术要求。原则上,抗体中间体的质量研究要求和抗体药物的要求基本一致。此外,还需对可能影响偶联工艺的质量属性进行充分研究和适当控制。其质量关注点在于效价、鉴别、抗体含量、纯度、杂质、细菌内毒素、无菌检查等。3.2 核素部分药学研究与评价关注点核素是ARC类产品的有效载荷,它是ARC药物发挥作用的关键因素。由于ARC通常为非终端灭菌产品,制备过程应关注微生物安全性。放射性药物中放射性核素的半衰期通常很短,伴随放射性衰变,放射性药物的组分随时间改变,故质量研究中需关注其放射性核素特征、效价(放射性核素浓度)、纯度(放射性核素纯度、放射化学纯度、比活度、化学成分以及金属离子、还原物质等化学杂质)、体外化学稳定性等。3.3 连接臂和螯合剂部分药学研究与评价关注点ARC药物的抗体和放射性核素之间由连接臂(linker)和螯合物(chelator)两部分组成,连接臂和螯合剂作为将抗体与核素连接起来的桥梁,可以作为一个整体来考虑。连接臂和螯合剂对于ARC的稳定性、有效载荷有显著影响,从而影响药物疗效和安全性。连接臂和螯合剂通常为化学小分子结构,一方面通过反应性官能团共价结合链接抗体,一方面通过络合基团螯合核素,其制备和质量控制可按化学药的起始物料要求进行研究和评价。需关注连接臂、螯合剂起始物料核素、螯合剂与最终制剂制备工艺可能引入的毒性溶剂/试剂、催化剂、元素杂质、遗传毒性杂质等的残留,并按照相关技术要求对临床样品进行控制。3.4 ARC部分药学研究与评价关注点ARC类产品由于其核素物理半衰期短,原液和制剂通常采用连续生产,且对于非终端灭菌产品,应充分关注无菌生产工艺。制剂处方中,对于常规辅料或其他类型辅料包括新型辅料,关注重点是其与药物本身的相容性,应有足够的理由和安全性数据支持。若制剂处方中包含稳定剂,除安全性数据支持外,还需开展对ARC与受体结合的干扰性研究等。虽然放射性射线主要使细胞DNA变性,而蛋白质对其相对不敏感,但仍需关注含有抗体的中间体偶联核素后对抗体的影响,重点关注对抗体的高级结构修饰、生物学活性的影响。另外,质量研究还需关注偶联引起的关键质量属性,如抗体含量、放射化学纯度、放射性活度以及游离核素/游离螯合剂链接的核素等与产品质量密切相关的指标。另外,抗体偶联核素的比例为此类产品的关键质量属性,对ARC的有效性和产品批间一致性有较大影响,但由于ARC产品具有放射性,对方法学有限制,鼓励研发者开发合适的方法来研究实际抗体偶联核素的比例,对该质量属性进行控制。质量标准制定时应充分考虑放射性物质的特性,如放射性核素的特性和纯度、放射化学特性和纯度、比活度、放射性浓度(放射性活度·mL-1)以及标定日期等。其他质量标准检测项可根据药典、ICH Q6B以及早期开发的产品性质和特性的数据进行设定,并且关注质量标准中无菌、支原体等微生物安全性检测项目的检测方法、取样时间的合理性。3.5 稳定性及包材药学研究与评价由于生产过程时间短、有效期短,从产品完成包装、运输到最终人体使用前均储存在铅罐中保存等特点,ARC类药物稳定性研究关注点与常规单抗类、ADC类药物略有不同。应结合ARC类产品实际储存和运输条件开展稳定性研究,并且合理设置稳定性研究考察项目。另外,还需关注ARC产品的运输、贮存、临床剂量的确认以及残余药品、患者排泄物等的处理方式等。放射性类药物包材一般包括直接接触药品的包材和放射性屏蔽容器。对于直接接触药品的包材首要应考虑与产品之间可能的相互作用,证明容器包装系统不会对产品质量产生负面影响(如吸附、纯度降低等),开展全面的相容性(浸出物、可提取物等)、密封性研究。对于预充针等包装的放射性药品,除了考察包材本身对活性成分质量的影响,以及包材相容性研究外,还应关注包材性能稳定性对产品使用上的影响。对于放射性屏蔽容器应充分研究或评估说明包装可以确保放射性物质泄露的风险。4结语随着核医疗与核技术的创新和迭代,近年来RDC迎来了研发热潮,其突出特点还在于更换使用的放射性核素种类、可以发挥诊断或治疗等不同功能。根据靶向配体的不同类型,RDC可分为ARC,PRC和SMRC。目前已上市RDC产品多以PRC/SMRC产品为主,ARC作为RDC药物重要的产品类型,除了靶向性强,还兼顾单抗的疗效,使其具有不可比拟的临床优势和更强的发展潜力。ARC类产品是大分子药物、小分子以及核素的组合产品,其从产品设计、生产工艺、质量研究和控制、处方开发、稳定性等方面均面临诸多挑战。本文结合ARC产品的相关法规及最新研究进展,从生产工艺、质量控制、稳定性等方面对此类产品的药学研究与评价的关注点展开了讨论,以期促进此类产品的临床转化与应用。参考文献详见《中国新药杂志》2023年第32卷第2期文章信息源于公众号凡默谷,登载该文章目的为更广泛的传递行业信息,不代表赞同其观点或对其真实性负责。文章版权归原作者及原出处所有,文章内容仅供参考。本网拥有对此声明的最终解释权,若无意侵犯版权,请联系小编删除。学如逆水行舟,不进则退;心似平原走马,易放难收。行舟Drug每日更新 欢迎订阅+医药大数据|行业动态|政策解读
抗体药物偶联物放射疗法
100 项与 Arcitumomab technetium-99m 相关的药物交易
登录后查看更多信息
外链
| KEGG | Wiki | ATC | Drug Bank |
|---|---|---|---|
| - | Arcitumomab technetium-99m |
研发状态
10 条最早获批的记录, 后查看更多信息
登录
| 适应症 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|
| 结直肠癌 | 欧盟 | 1996-10-04 | |
| 结直肠癌 | 冰岛 | 1996-10-04 | |
| 结直肠癌 | 列支敦士登 | 1996-10-04 | |
| 结直肠癌 | 挪威 | 1996-10-04 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
No Data | |||||||
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或

药物交易
使用我们的药物交易数据加速您的研究。
登录
或

核心专利
使用我们的核心专利数据促进您的研究。
登录
或

临床分析
紧跟全球注册中心的最新临床试验。
登录
或

批准
利用最新的监管批准信息加速您的研究。
登录
或

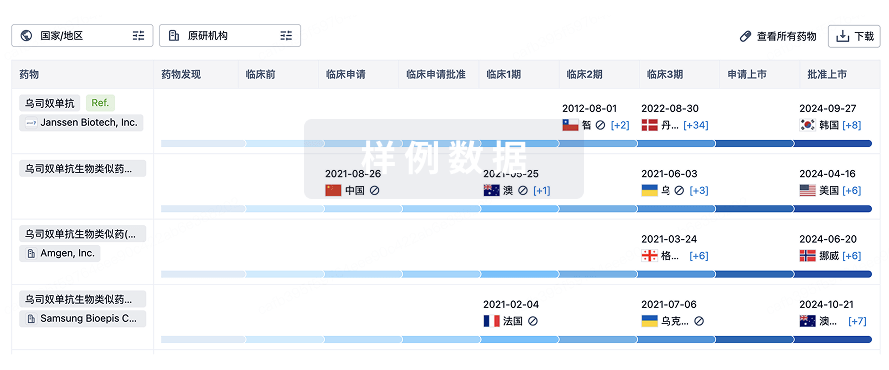
生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
特殊审评
只需点击几下即可了解关键药物信息。
登录
或

生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
