预约演示
更新于:2025-05-07

Quorum Consulting, Inc.
更新于:2025-05-07
概览
关联
100 项与 Quorum Consulting, Inc. 相关的临床结果
登录后查看更多信息
0 项与 Quorum Consulting, Inc. 相关的专利(医药)
登录后查看更多信息
15
项与 Quorum Consulting, Inc. 相关的文献(医药)2018-08-01·JAMA Dermatology1区 · 医学
Association of Inadequately Controlled Disease and Disease Severity With Patient-Reported Disease Burden in Adults With Atopic Dermatitis
1区 · 医学
Article
作者: Mastey, Vera ; Simpson, Eric L. ; Yu, Tiffany ; Vekeman, Francis ; Suárez-Fariñas, Mayte ; Guttman-Yassky, Emma ; Hata, Tissa ; Chao, Jingdong ; Eckert, Laurent ; Qureshi, Abrar ; Wei, Wenhui ; Gadkari, Abhijit ; Arnold, Renée J. G. ; Margolis, David J. ; Feldman, Steven R.
2017-07-03·Journal of Medical Economics4区 · 医学
Cost-comparison of two trabecular micro-bypass stents versus selective laser trabeculoplasty or medications only for intraocular pressure control for patients with open-angle glaucoma
4区 · 医学
Article
作者: Layton, Andrew J. ; Berdahl, John P. ; Bauer, Matthew J. ; Yu, Tiffany M. ; Katz, L. Jay ; Khatana, Anup K. ; Herndon, Leon ; Cantor, Louis B.
2017-05-20·Journal of Clinical Oncology
Practical implications of single-gene versus NGS testing in advanced NSCLC.
作者: Yu, Tiffany ; Layton, Andrew ; Tradonsky, Alison
1
项与 Quorum Consulting, Inc. 相关的新闻(医药)2016-06-13
Digital health and digital therapeutics will produce a tremendous amount of data, which could be the key to getting them reimbursed by payers, according to panelists at BIO 2016 last week. UCSF Professor of Health Economics and Health Services Research Kathryn Phillips led a panel that included Rowan Chapman, managing director of new business ventures at GE Ventures; Evidation Health CEO Deborah Kilpatrick; and Nicole Littman, vice president client services at Quorum Consulting.
The panelists talked about Proteus Digital Health's sensor-embedded pharmaceuticals as one example of a digital medicine or digital therapeutic. Littman said few payers have elected to cover Proteus so far.
"What payers are saying in their non-coverage statement is there are no clinical utility studies," she said. "The translation to that is 'If you use this, can you demonstrate that the patients are actually experiencing better outcomes?' From the manufacturer’s perspective, we demonstrated that the product is doing what it’s supposed to do. But payers are looking for a little bit more."
But Evidation Health CEO Kilpatrick said that digital health interventions inherently produce a lot of data quickly and easily, which means that even if payers set a high bar for reimbursing them, they're well equipped to step up to that bar.
"For payers who don’t want to pay, one of the easiest objections is 'Well that wasn’t in my population.' And while that is a harder objection to overcome with traditional therapeutics and diagnostics, with digital it’s 'Fine, I’ll go do it in your population.' And I can do that very rapidly because I can contact your members and I can [collect data] really fast. I don’t think expectations should or will be different [for digital therapeutics], because I think the speed and efficiency with which they can be met is going to be a game changer. And I think it’s going to be better for patients, for innovation, and for companies ultimately."
The data from sensors and phones that facilitates quick, efficient clinical utility studies also constitutes one of the key use cases for digital health, according to Kilpatrick. In the same way that knowing a patient's genomic information facilitates personalized medicine, passively collecting behavioral data via the phone can help target interventions to the most receptive populations.
"We’re throwing off digital signals all the time," she said. "If you use those signals to phenotype people, you can relate that to whether or not they’re likely to be adherent to medication, to whether or not they’re likely to show up to their primary care provider on their next visit, you can relate that in case of heart failure to readmissions, you can do all kinds of powerful things that allow us to quantify outcomes in ways that simply weren’t available to us before. So this notion of being able to identify super responders based on behavior, not just biology, that’s real and that’s here."
100 项与 Quorum Consulting, Inc. 相关的药物交易
登录后查看更多信息
100 项与 Quorum Consulting, Inc. 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年03月19日管线快照
无数据报导
登录后保持更新
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
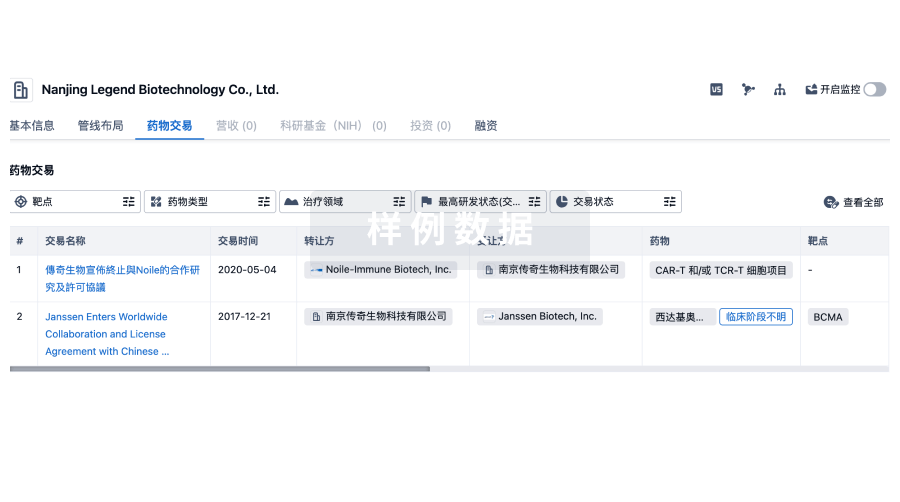
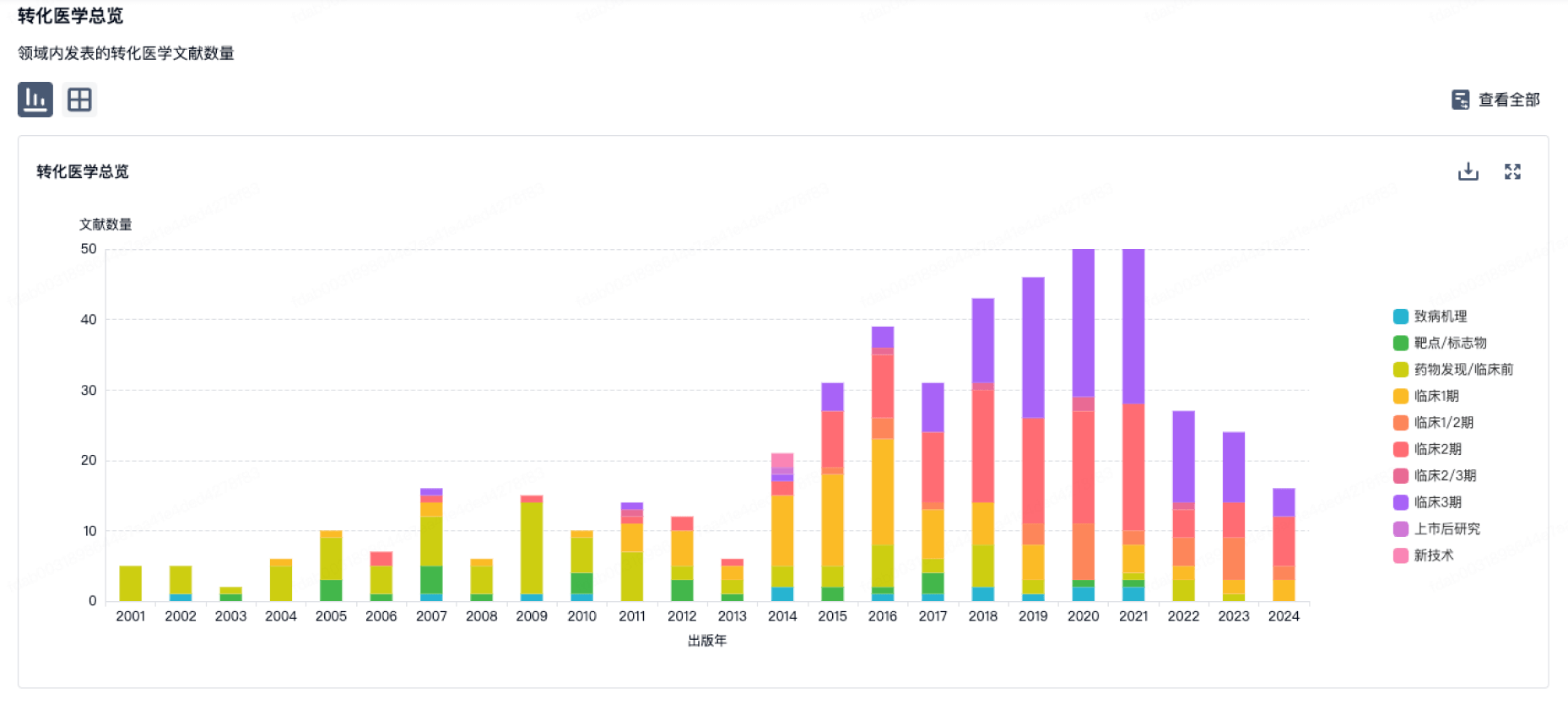
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
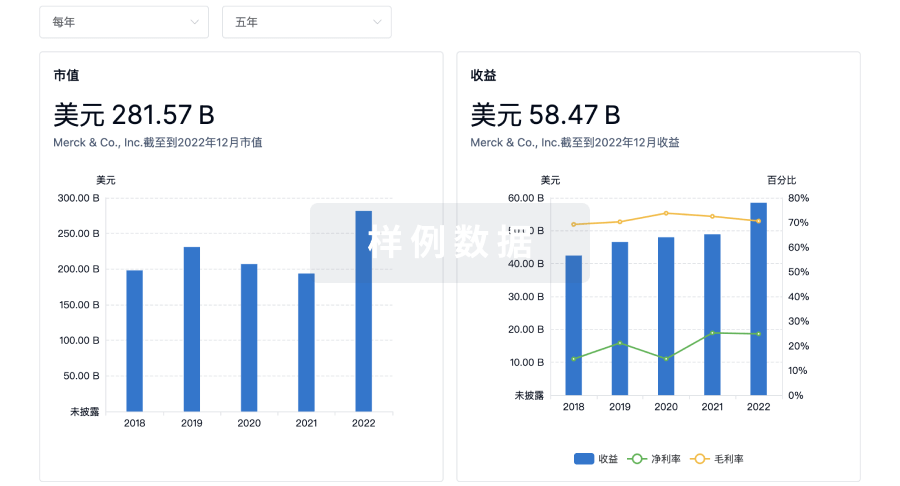
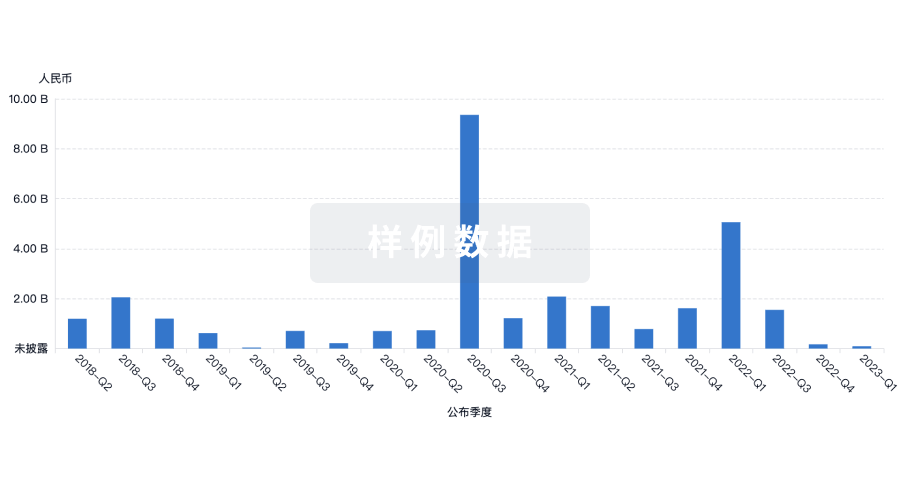
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
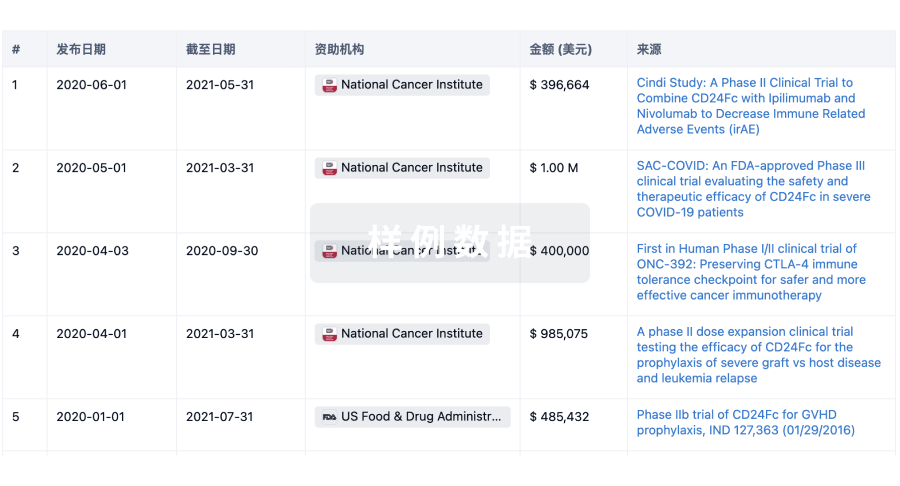
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
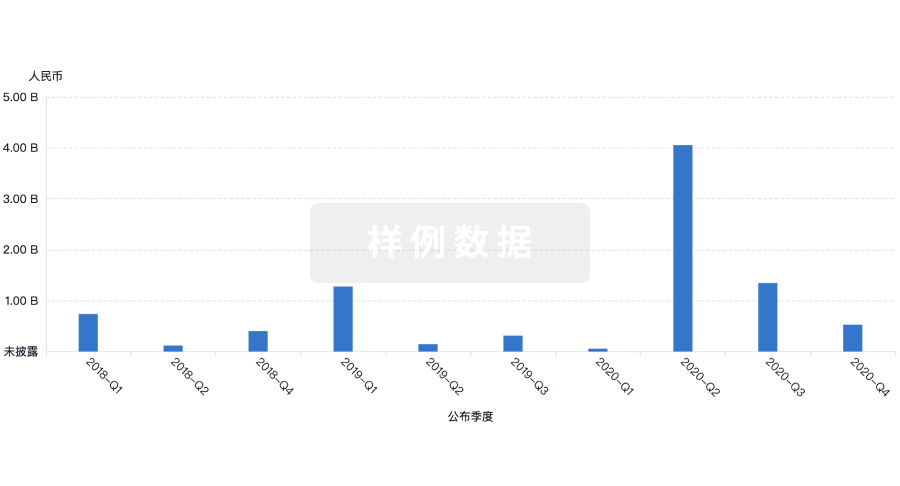
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用