预约演示
更新于:2025-05-07
Geisinger Health Plan
更新于:2025-05-07
概览
关联
100 项与 Geisinger Health Plan 相关的临床结果
登录后查看更多信息
0 项与 Geisinger Health Plan 相关的专利(医药)
登录后查看更多信息
11
项与 Geisinger Health Plan 相关的新闻(医药)2024-02-22
SAYLORSBURG, Pa., Feb. 22, 2024 /PRNewswire/ -- Blue Ridge Eating Disorder Care Center has announced that they now offer young women in need of Residential eating disorder care in-network coverage with Geisinger Health Plan and Highmark Blue Cross Blue Shield. Blue Ridge Eating Disorder Care Center's Clinical Director and Founder, Erica Butler, notes, "Eating Disorder treatment can be hard to find, and when you do find a facility that can meet your family's needs, it can be especially challenging to navigate care if they aren't in-network with your insurance provider. We are thrilled to continue to give families access to exceptional eating disorder care without the financial barriers."
Blue Ridge Eating Disorder Care Center is an in-network Residential treatment facility for young women ages 12-17 with a primary diagnosis of an eating disorder serving patients in Saylorsburg, Pennsylvania. "While we are rural and situated in pastoral Saylorsburg, we have families travel from all over the country due to our adolescent specific programming and warm homelike setting," says Butler.
Nearly 30 million Americans will experience an eating disorder in their lifetime, and about 30% of those are adolescents. Blue Ridge is committed to the recovery of young women with disordered eating and offers individualized treatment for girls diagnosed with ARFID, Anorexia, Bulimia, OSFED, and other disordered eating presentations.
The priority at Blue Ridge is to provide young women with nutritional therapy, individual therapy, group therapy, medication management, educational support, and medical care while they build relationships with their peers and staff. At Blue Ridge, families are their main focus, and the team believes that long-lasting recovery is built on a collaborative approach that is family focused. The team notes that their home like environment utilizes expressive therapies tailored to the needs of young women, which is vital to finding freedom from disordered eating.
SOURCE Blue Ridge Eating Disorder Care Center
2023-10-26
Awards catalyze community commitments to addressing the unmet needs of people with rare neurological diseases and sleep disorders
[26-October-2023]
PLYMOUTH MEETING, Pa., Oct. 26, 2023 /PRNewswire/ -- Harmony Biosciences Holdings, Inc. ("Harmony") (Nasdaq: HRMY), a pharmaceutical company dedicated to developing and commercializing innovative therapies for patients with rare neurological diseases, has selected the latest round of nonprofit organizations for its Patients at the Heart and Progress at the Heart awards. These awards provide funding support to nonprofit organizations addressing the complex challenges affecting individuals with sleep disorders and rare neurological diseases through unique and impactful initiatives.
Over the past four years, Patients at the Heart has supported 24 initiatives aimed at addressing the comprehensive needs of individuals and their families affected by sleep disorders and rare neurological diseases. The newest awardees include the following organizations:
Awareness & Patient Support Progression – Kleine-Levin Syndrome Foundation
This initiative builds educational and support resources for people with Kleine-Levin syndrome (KLS) and the broader scientific community by creating a new ambassador program that connects patients, caregivers, educators, and professionals to enhance care.
"KLS is an exceptionally rare neurological disorder, affecting only one in a million individuals worldwide, primarily adolescents, and is characterized by episodes of excessive sleep, altered behavior, and a diminished understanding of the world," said Dani Farber, VP of the Kleine-Levin Syndrome Foundation. "With support from a previous Patients at the Heart award, we achieved the 'Strategic Communications for Awareness' project, which fortified and expanded our patient registry and outreach endeavors. Building on this success, our 'KLS Awareness and Patient Support Progression' initiative will enhance resources for education, raise awareness, and establish a KLS ambassadorship program that will provide crucial support to patients, caregivers, educators, and professionals alike."
PWS Sleep Within Reach Resources – Prader-Willi Syndrome Association | USA
This program educates health care professionals, caregivers of people with Prader-Willi syndrome (PWS), as well as residential and educational staff on the most misunderstood forms of sleep disorders, including those among people with PWS.
"We are honored to be recognized with a Patients at the Heart award for our 'Reach Resources' program, which provides free, multi-tiered support to individuals living with and affected by PWS," said Stacy Ward, MS, Interim CEO of the Prader‐Willi Syndrome Association | USA. "This initiative underscores our commitment to fostering collaborative care, involving professionals, caregivers, and educational staff. Through project elements like 'PWS ECHO Sleep Within Reach' and 'ECHO Debrief,' alongside the development of educational toolkits, we reaffirm our dedication to making a meaningful impact in the lives of those affected by this rare and challenging condition, as well as their loved ones."
Progress at the Heart provides funding support for novel initiatives addressing disparities, injustices, and inequities in rare neurological disease and sleep disorder communities. In the two years since it started, it has supported 15 initiatives, including the newest recipients:
The Restful Revolution – Rare & Black
The Restful Revolution, an innovative pilot program, will provide support to up to five Historically Black Colleges and Universities in the Washington, DC and Baltimore area for the 2023-2024 academic school year. Its mission is to educate and empower students to cultivate healthy sleep habits and raise awareness about sleep disorders.
"For far too long, the sleep health of students at Historically Black Colleges and Universities and institutions with significant Black student populations has been unjustly overlooked," said Dionne L. Stalling, Founder of Rare & Black. "This innovative program marks an important step forward. In the upcoming academic year, we will visit up to five institutions in the Washington, DC, and Baltimore area, equipping students with essential sleep habits and shedding light on the challenges of sleep disorders. Together, with this funding support, we can create a future where every student's overall well-being, particularly those from historically underserved communities, takes equal precedence."
Wake Up and Learn – Geisinger Health Foundation
Wake Up and Learn is a virtual K-12 educational and surveillance program that facilitates a culture shift towards a valuation of sleep as essential for health and removing barriers to timely recognition, diagnosis, and management of sleep disorders in school-aged children. The 2024 program will expand the video curriculum, translate materials into Spanish, and assess impact through interviews with a focus on diverse geographic, ethnic and gender perspectives.
"We are facing a critical issue of sleep-wake disorders in the US, affecting a significant portion of the population, including many students," said Anne Marie Morse, DO, a board-certified and fellowship-trained pediatric neurologist and sleep medicine specialist at Geisinger Health System. "Racial and economic disparities worsen this dire situation, leading to limited access to care and heightened stigma, particularly in historically underserved communities. Our latest effort, Wake Up and Learn, introduces a transcultural, school-based program emphasizing the importance of sleep for students' well-being and their potential in life. Through this initiative, we seek to emphasize the crucial role of sleep in their journey to success and urge greater attention to recognizing poor sleep and addressing it promptly."
Harmony is dedicated to supporting significant transformation within the rare neurological disease and sleep disorder communities. The next call for Patients at the Heart and Progress at the Heart award nominations will be announced next year.
"Our Patients at the Heart and Progress at the Heart awards exemplify our commitment to empathy and innovation, catalyzing our commitment to these nonprofit organizations who are leading the way in addressing complex challenges posed by sleep and rare neurological disorders," said Cate McCanless, Chief Corporate Affairs Officer at Harmony Biosciences. "We are honored to support these initiatives, which collectively hold the potential to make a lasting impact on individuals and communities facing significant unmet needs, while always placing patients at the heart of everything that we do."
To learn more about Patients at the Heart, please visit: .
To learn more about Progress at the Heart, please visit: .
About Harmony Biosciences
At Harmony Biosciences, we specialize in developing and delivering treatments for rare neurological diseases that others often overlook. We believe that where empathy and innovation meet, a better life can begin for people living with neurological diseases. Established by Paragon Biosciences, LLC, in 2017 and headquartered in Plymouth Meeting, PA, our team of experts from a wide variety of disciplines and experiences is driven by our shared conviction that innovative science translates into therapeutic possibilities for our patients, who are at the heart of everything we do. For more information, please visit .
Harmony Biosciences Media Contact:
Cate McCanless
202-641-6086
cmccanless@harmonybiosciences.com
Harmony Biosciences Investor Contact:
Luis Sanay, CFA
445-235-8386
lsanay@harmonybiosciences.com
Company Codes: NASDAQ-NMS:HRMY
2023-09-06
First blood-only liquid biopsy test for minimal residual disease now covered for patients with stage II or III colorectal cancer
Test used after surgery or curative treatment to inform physician decisions about adjuvant therapy and to monitor for disease progression, recurrence or relapse
PALO ALTO, Calif.--(BUSINESS WIRE)-- Guardant Health, Inc. (NASDAQ:GH), a leading precision oncology company, announced today that Geisinger Health Plan now offers coverage for the Guardant Reveal™ minimal residual disease (MRD) test. Guardant Reveal is a blood test that detects circulating tumor DNA (ctDNA) in blood after treatment, including surgery, to help oncologists identify cancer patients with residual or recurring disease who may benefit most from adjuvant therapy or surveillance. It is the first blood-only liquid biopsy test commercially available for MRD testing.
Geisinger is providing coverage for the Guardant Reveal test for individuals with stage II or III colorectal cancer after curative treatment (including surgery) to inform physician decisions about post-treatment therapy and to monitor for disease progression, recurrence or relapse. The frequency of testing covered is aligned with monitoring guidelines established by the National Comprehensive Cancer Network for colorectal cancer. It includes the initial ctDNA test 4 to 6 weeks after surgery (or 2 to 4 weeks after completion of systemic therapy) and thereafter every 3 to 6 months for the first two years, and every 6 to 12 months for the following 3 years.
“We are pleased that Geisinger Health Plan has taken this important step to make blood testing for residual disease more accessible to its members,” said Helmy Eltoukhy, Guardant Health chairman and co-CEO. “This decision will help oncologists make more informed decisions about treatment and monitoring for colorectal cancer patients and survivors, to help improve their outcomes.”
Minimal residual disease refers to a subclinical measure of cancer burden that remains during and following treatment. A patient’s MRD status is a reliable indicator of clinical outcome and response to therapy and can be used for risk stratification and to guide treatment options when used in conjunction with other clinical data.
The Geisinger Health Plan provides coverage for more than half a million members. This policy decision adds to the payor coverage of Guardant Reveal, which received Medicare coverage in August 2022 and additional commercial payor coverage in July 2023.
About Guardant Health
Guardant Health is a leading precision oncology company focused on helping conquer cancer globally through use of its proprietary tests, vast data sets and advanced analytics. The Guardant Health oncology platform leverages capabilities to drive commercial adoption, improve patient clinical outcomes and lower healthcare costs across all stages of the cancer care continuum. Guardant Health has commercially launched Guardant360®, Guardant360 CDx, Guardant360 TissueNext™, Guardant360 Response™, and GuardantINFINITY® tests for advanced stage cancer, and Guardant Reveal™ for early-stage cancer. The Guardant Health screening portfolio, including the commercially launched Shield™ test, aims to address the needs of individuals eligible for cancer screening. For more information, visit guardanthealth.com and follow the company on LinkedIn and X (Twitter).
View source version on businesswire.com:
Contacts
Investor Contact:
investors@guardanthealth.com
Source: Guardant Health, Inc.
View this news release online at:
100 项与 Geisinger Health Plan 相关的药物交易
登录后查看更多信息
100 项与 Geisinger Health Plan 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年03月24日管线快照
无数据报导
登录后保持更新
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
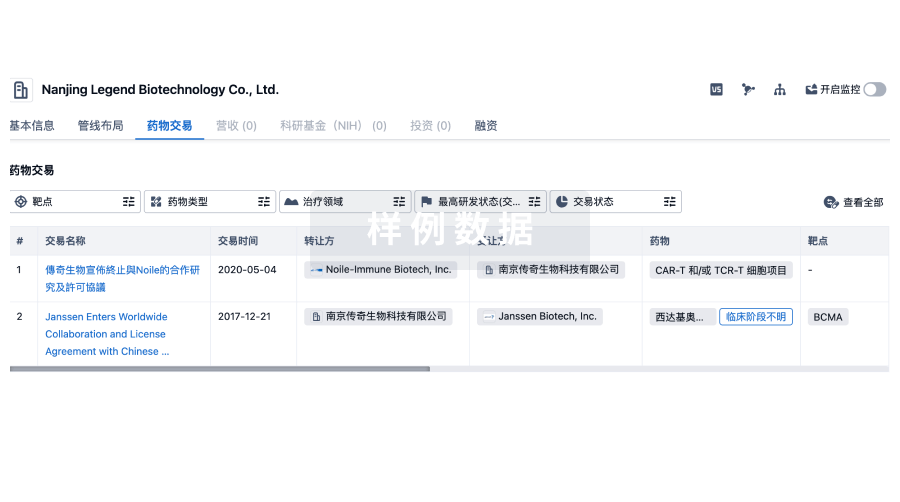
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
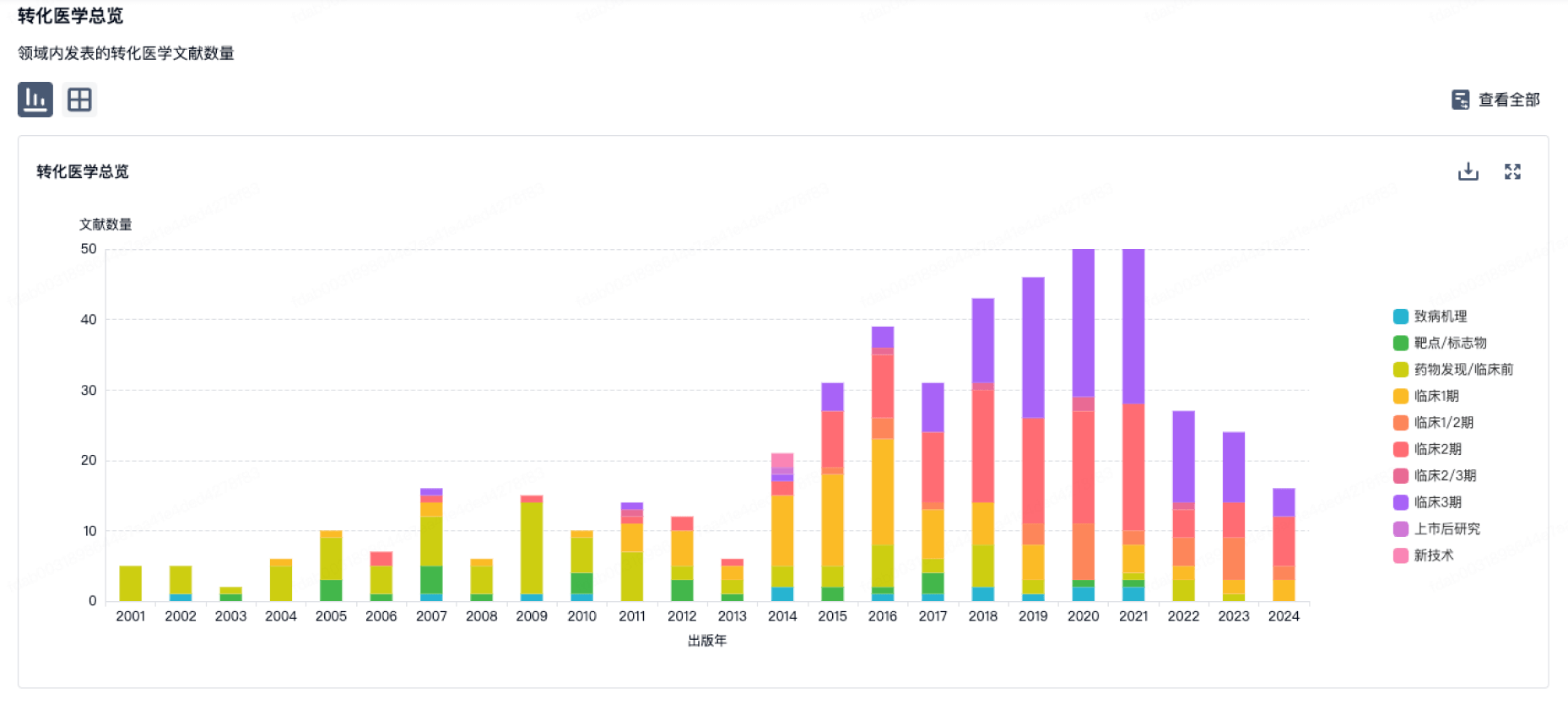
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
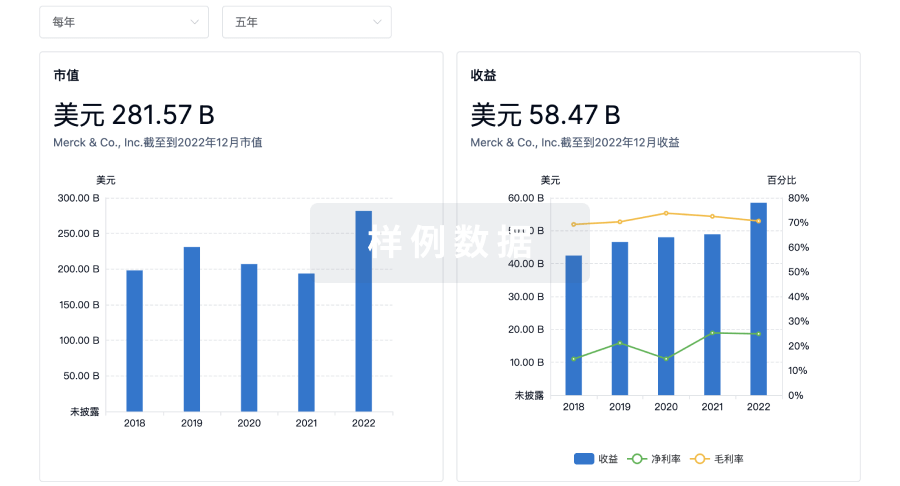
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
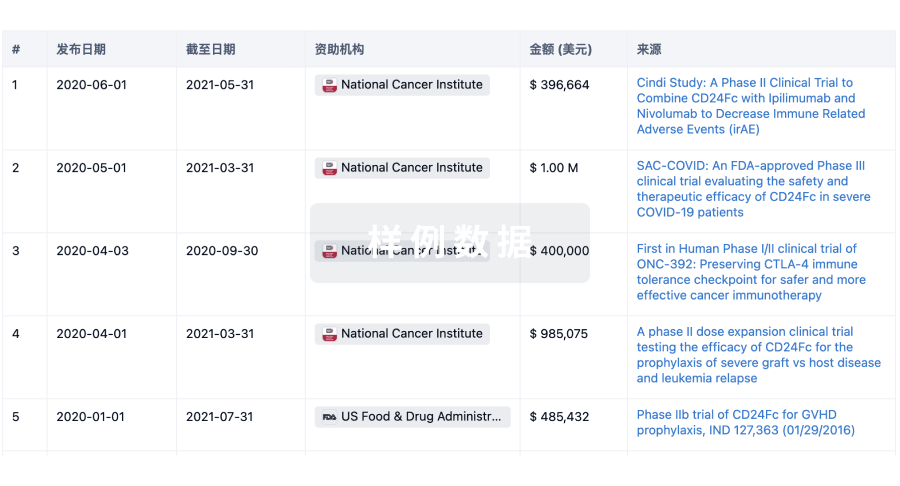
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
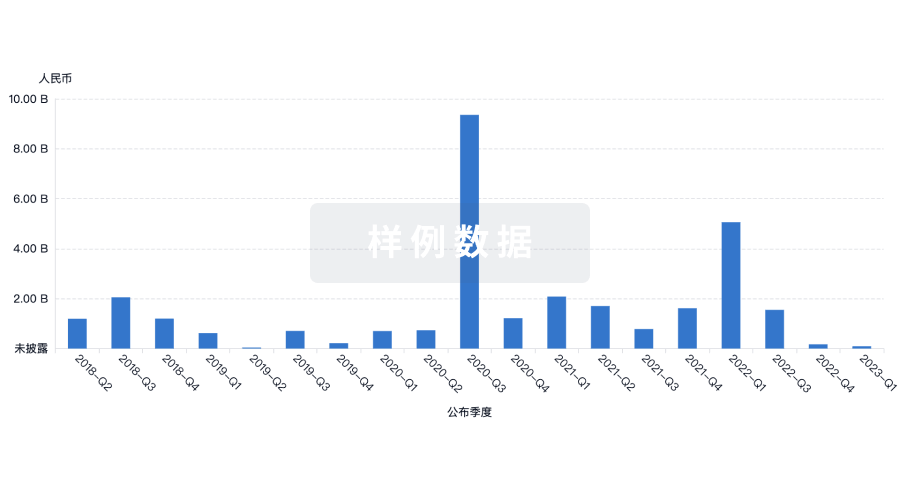
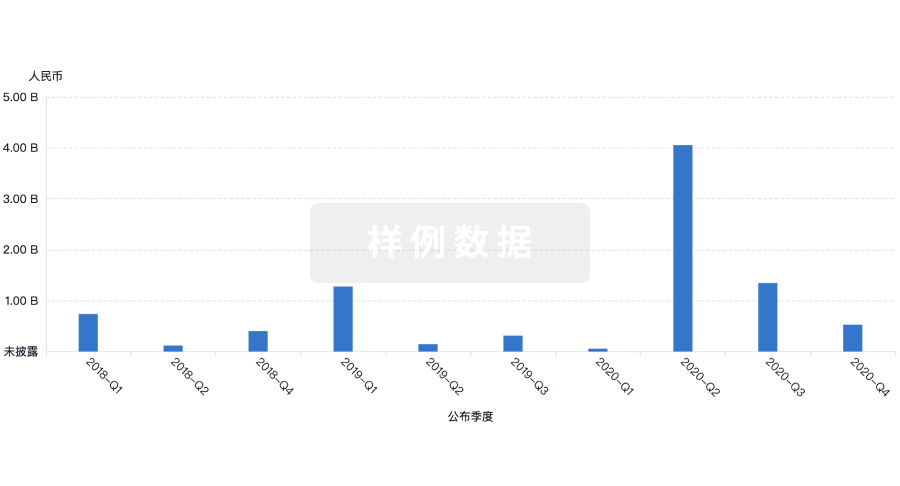
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用