预约演示
更新于:2025-08-14

North Devon District Hospital
更新于:2025-08-14
概览
关联
100 项与 North Devon District Hospital 相关的临床结果
登录后查看更多信息
0 项与 North Devon District Hospital 相关的专利(医药)
登录后查看更多信息
236
项与 North Devon District Hospital 相关的文献(医药)2025-07-01·BMJ Open Gastroenterology
Triaging colorectal urgent referrals in the COVID-19 era using faecal immunochemical testing: a prospective UK real-world multicentre cohort study
Article
作者: McDonald, Timothy ; Feeney, Mark ; Balasubramanya, Supriya ; Ward-Booth, Sally ; Walker, Gareth ; Bain, Iain ; Spencer, Naomi ; Bowen, Joel ; Kantola, Venla ; Bethune, Robert ; Smolarek, Sebastian ; Hamilton, Willie ; Bailey, Sarah E R ; Debab, Nedal ; Cartmell, Mark ; Renninson, John ; Faux, William ; Kennedy, Nicholas A
Objective:
During the early COVID-19 pandemic, UK guidelines advocated faecal immunochemical tests (FIT) with a threshold of 10 µg/g to help secondary care clinicians triage urgent suspected colorectal cancer (CRC) referrals. We aimed to evaluate the real-world performance and impact of FIT in a high-risk cohort referred against National Institute for Health and Clinical Excellence NG12 (2015) criteria.
Methods:
Multicentre prospective observational cohort study of FIT at all four secondary care hospitals in Devon (UK) between 1 April 2020 and 31 December 2020. FIT use was at the discretion of primary and secondary care clinicians. Incident CRC cases were identified ≥12 months after general practitioner (GP) referral using regional National Bowel Cancer Audit data linkage. We assessed diagnostic accuracy and healthcare utilisation in patients with and without FIT.
Results:
Overall, 6698 patients were included: 55% female, median age 72 years (IQR 65–82). Just over half (53%, 3552) of patients underwent FIT with a positivity rate of 34% (n=1237). CRC prevalence in patients with no FIT, positive FIT and negative FIT was 6% (189), 11% (137) and 0.5% (11), respectively. The prevalence of all cancers, including non-CRCs, was similar among FIT and no-FIT cohorts (p=0.74). Sensitivity and specificity of FIT for CRC were 0.93 (95% CI 0.87 to 0.96) and 0.68 (95% CI 0.66 to 0.69), respectively. Patients with negative FIT underwent fewer lower gastrointestinal endoscopies (no FIT 62% (1964) vs positive FIT 69% (857) vs negative FIT 36% (835)), p=0.0005).
Conclusions:
FIT is a useful triage tool for patients with suspected CRC which safely reduces endoscopy demand and prioritises those at greatest cancer risk. Standardised regional referral pathways, greater use of ‘straight-to-test’ investigations and GP support are needed to maximise its impact.
2025-02-01·EUROPEAN JOURNAL OF CLINICAL PHARMACOLOGY
Evaluating the safety and effectiveness of tolvaptan in patients with heart failure and renal impairment: a systematic review and meta-analysis
Review
作者: Amin, Shafin Bin ; Shafique, Muhammad Ashir ; Shahid, Muhammad Saad ; Kumar, Aashish ; Naz, Aimen ; Iqbal, Umer ; Asuka, Emediong Santhus ; Arsal, Syed Ali ; Ali, Syed Muhammad Sinaan
PURPOSE:
Patients with heart failure and concomitant renal impairment are often prescribed loop diuretics, such as furosemide, as the primary treatment. The present meta-analysis is focused on analyzing the safety and efficacy of the implementation of tolvaptan as a novel approach in patients with renal impairment and heart failure.
METHODS:
Two reviewers conducted a screening of articles using online databases, including PubMed, Google Scholar, and Embase. Following a comprehensive literature search, seven articles that met all inclusion criteria (patients with heart failure and renal impairment) were selected for analysis. Subsequently, various primary and secondary outcomes were evaluated.
RESULTS:
The primary outcomes of our study included urine volume, worsening renal function, blood urea nitrogen (BUN) levels, and creatinine levels. Tolvaptan demonstrated superior efficacy in increasing urine output with a standardized mean difference of 2.18 (95% CI 0.62-3.75, p = 0.006) and resulted in a lower incidence of worsening renal function with odds ratio 0.41 (95% CI 0.22-0.77, p = 0.006). Additionally, there was no significant difference in the tolvaptan and conventional treatment groups in changing serum creatinine levels with a standardized mean difference of - 0.37 (95% CI - 0.86 to 0.12, p = 0.135), but tolvaptan tends to decrease blood urea nitrogen levels with a standardized mean difference - 0.18 (95% CI - 0.30 to - 0.06, p = 0.004) in comparison to conventional treatment group.
CONCLUSION:
While tolvaptan administration was related to better renal outcomes, unresolved heterogeneities and various factors could have influenced our findings. Further research is needed to evaluate the role of tolvaptan in the treatment of this patient population.
2025-01-01·BMJ Open
Knowledge translation in Anglo-American paramedicine: a scoping review
Article
作者: Burton, Christopher ; Hanson, Ashley
Objective:
To map what is currently known about knowledge translation (KT) in Anglo-American paramedicine. The review focuses on reported barriers and facilitators to the implementation of new knowledge, and the use of models, theories and frameworks to guide implementation practice.
Design:
Scoping review reported as per both the Joanna Briggs Institute and Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews reporting guidelines.
Data sources:
CINAHL (EBSCO Host) and Medline (OVID interface) were searched from January 2000 to May 2023. Reference lists of all included papers were reviewed, and several key professional journals were hand-searched.
Eligibility criteria for selecting studies:
Primary sources that focused on KT models, theories or frameworks, or barriers and facilitators to KT implementation, involving paramedics or Emergency Medical Technicians (Paramedic in America) working in an out-of-hospital, Anglo-American Emergency Medical Service (EMS) system were eligible for inclusion.
Data extraction and synthesis:
One reviewer used a data extraction template developed for this review and 10% of the papers were checked by the second author. Findings were summarised in tables and synthesised both quantitatively and qualitatively.
Results:
The search yielded 1268 primary sources, of which 48 were included in the review. Thirty-two papers examining KT interventions and 16 papers examining the barriers and facilitators to KT were found. Only one randomised controlled trial was found, and only one paper made explicit use of any KT framework. Overall, eight themes describing barriers and facilitators to KT arose from the qualitative literature, with clinicians’ perception of the evidence being the dominant theme. All 32 papers describing KT interventions included some form of educational intervention.
Conclusions:
Overall, there is little depth and breadth in the literature, with many papers focusing on trauma and airway management. There are large gaps in the evidence surrounding the use of KT theories and frameworks in Anglo-American EMS. Further research is needed to identify appropriate KT models and frameworks that are contextualised to EMS to ensure that paramedic-led research finds its way to the clinicians needing to use it.
100 项与 North Devon District Hospital 相关的药物交易
登录后查看更多信息
100 项与 North Devon District Hospital 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年04月08日管线快照
无数据报导
登录后保持更新
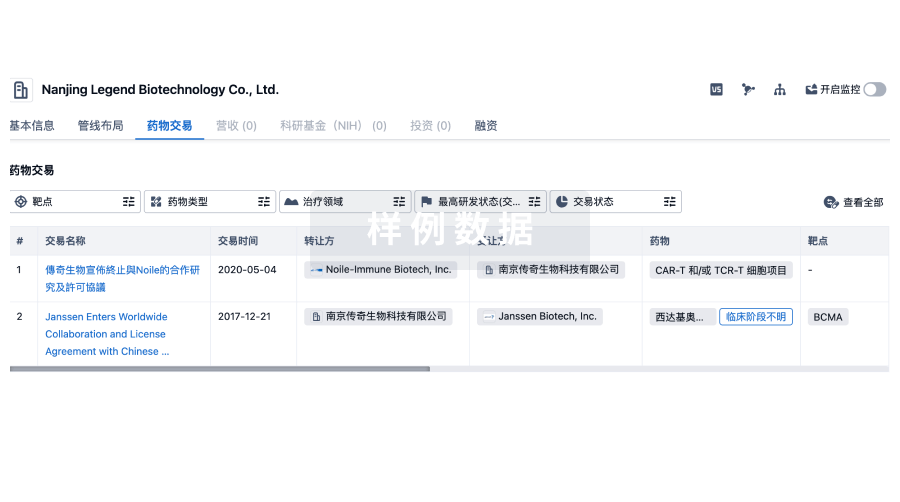
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
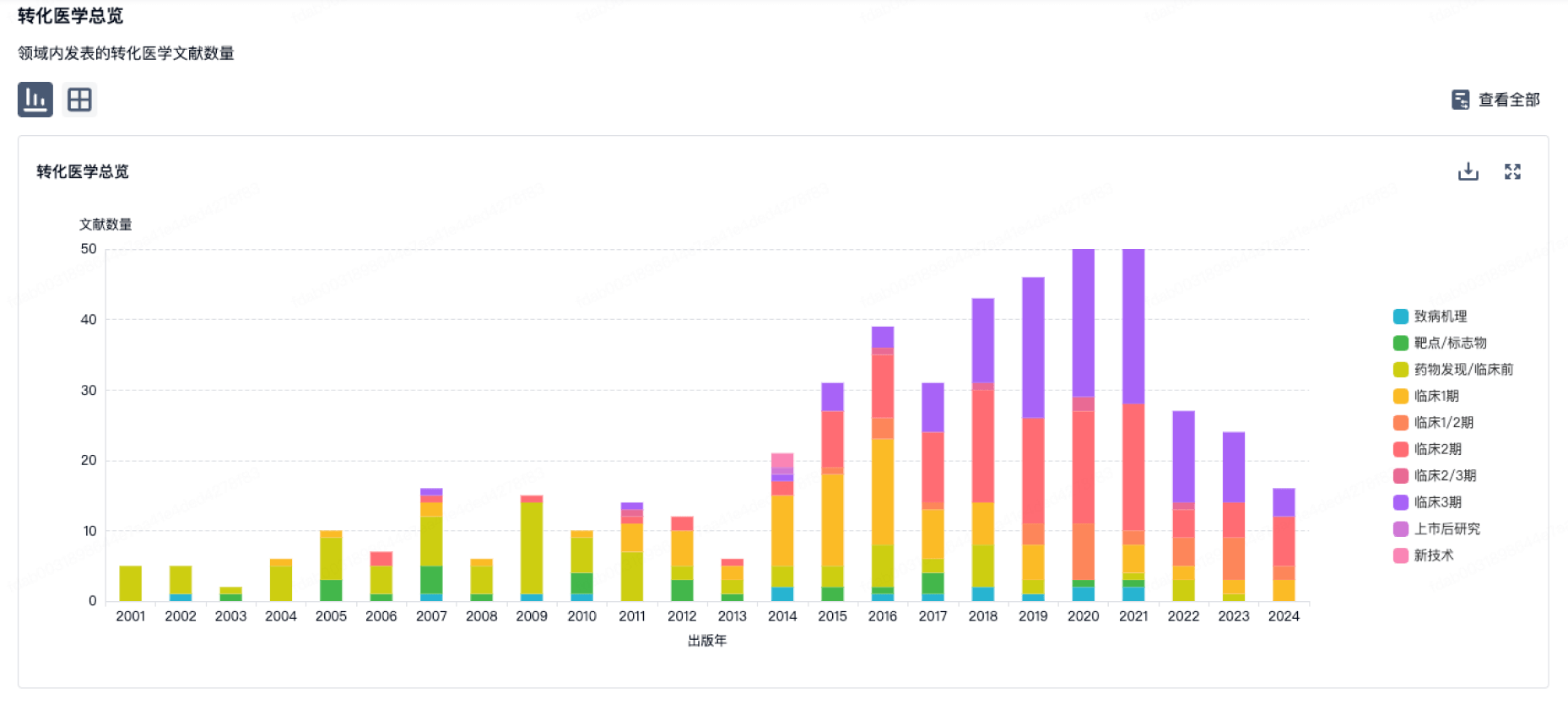
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
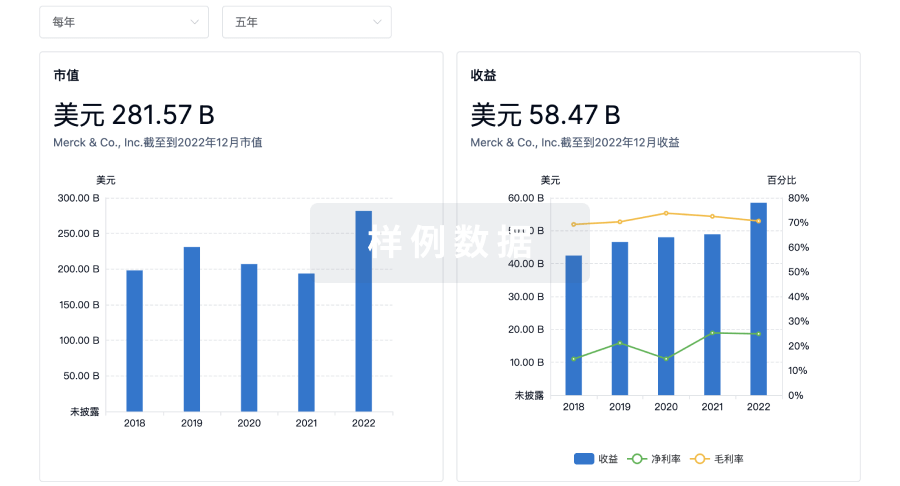
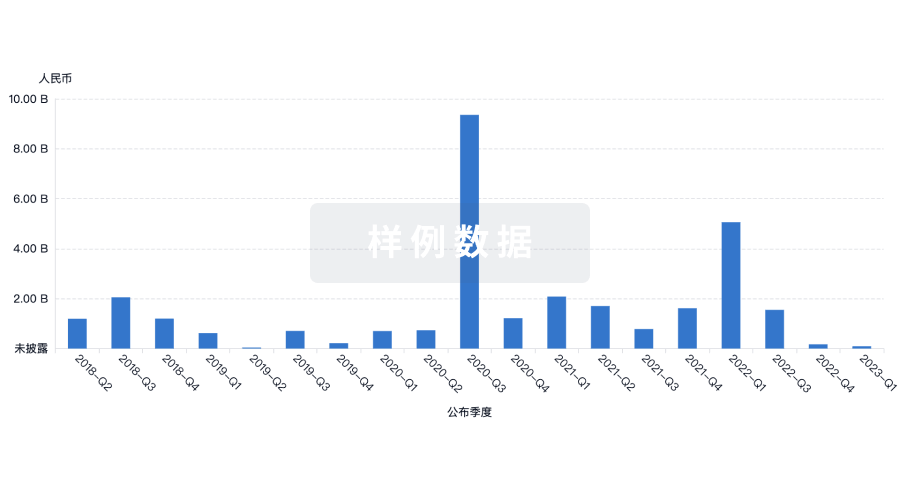
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
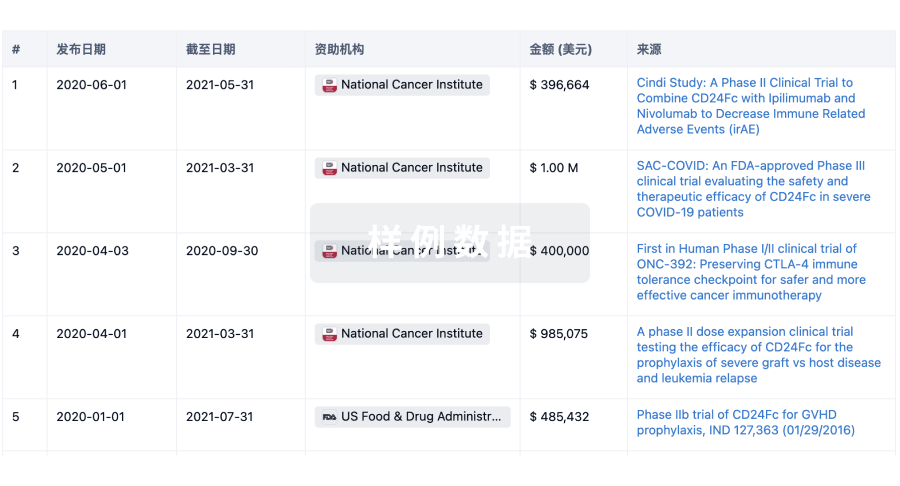
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
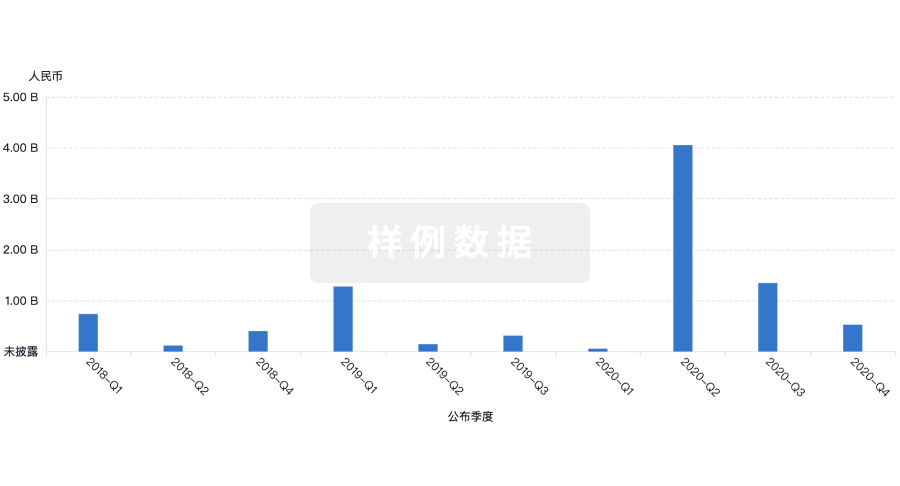
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用