预约演示
更新于:2026-03-05

Spatial Genomics, Inc.
更新于:2026-03-05
概览
关联
100 项与 Spatial Genomics, Inc. 相关的临床结果
登录后查看更多信息
0 项与 Spatial Genomics, Inc. 相关的专利(医药)
登录后查看更多信息
3
项与 Spatial Genomics, Inc. 相关的文献(医药)2024-06-01·Nature neuroscience
Single-cell long-read sequencing-based mapping reveals specialized splicing patterns in developing and adult mouse and human brain
Article
作者: Korkin, Dmitry ; Zhang, Bei ; Ross, M Elizabeth ; Tilgner, Hagen U ; Balacco, Jennifer ; Milner, Teresa A ; Joglekar, Anoushka ; Narykov, Oleksandr ; Fedrigo, Olivier ; Jarvis, Erich D ; Sheynkman, Gloria ; Ndhlovu, Lishomwa C ; Marrocco, Jordan ; Hu, Wen ; Diekhans, Mark
Abstract:
RNA isoforms influence cell identity and function. However, a comprehensive brain isoform map was lacking. We analyze single-cell RNA isoforms across brain regions, cell subtypes, developmental time points and species. For 72% of genes, full-length isoform expression varies along one or more axes. Splicing, transcription start and polyadenylation sites vary strongly between cell types, influence protein architecture and associate with disease-linked variation. Additionally, neurotransmitter transport and synapse turnover genes harbor cell-type variability across anatomical regions. Regulation of cell-type-specific splicing is pronounced in the postnatal day 21-to-postnatal day 28 adolescent transition. Developmental isoform regulation is stronger than regional regulation for the same cell type. Cell-type-specific isoform regulation in mice is mostly maintained in the human hippocampus, allowing extrapolation to the human brain. Conversely, the human brain harbors additional cell-type specificity, suggesting gain-of-function isoforms. Together, this detailed single-cell atlas of full-length isoform regulation across development, anatomical regions and species reveals an unappreciated degree of isoform variability across multiple axes.
2023-12-01·Cell1区 · 生物学
Parallel neural pathways control sodium consumption and taste valence
1区 · 生物学
Article
作者: Palmiter, Richard ; Oka, Yuki ; Zhang, Yameng ; Liu, Lu ; Zhang, Bei ; Kang, Elin ; Frieda, Kirsten ; Ding, Liang ; Pool, Allan-Hermann ; Wang, Tongtong
The hedonic value of salt fundamentally changes depending on the internal state. High concentrations of salt induce innate aversion under sated states, whereas such aversive stimuli transform into appetitive ones under sodium depletion. Neural mechanisms underlying this state-dependent salt valence switch are poorly understood. Using transcriptomics state-to-cell-type mapping and neural manipulations, we show that positive and negative valences of salt are controlled by anatomically distinct neural circuits in the mammalian brain. The hindbrain interoceptive circuit regulates sodium-specific appetitive drive , whereas behavioral tolerance of aversive salts is encoded by a dedicated class of neurons in the forebrain lamina terminalis (LT) expressing prostaglandin E2 (PGE2) receptor, Ptger3. We show that these LT neurons regulate salt tolerance by selectively modulating aversive taste sensitivity, partly through a PGE2-Ptger3 axis. These results reveal the bimodal regulation of appetitive and tolerance signals toward salt, which together dictate the amount of sodium consumption under different internal states.
A Spatially Coordinated Keratinocyte-Fibroblast Circuit Recruits MMP9
+
Myeloid Cells to Drive IFN-I-Driven Inflammation in Photosensitive Autoimmunity
Article
作者: Rashighi, Mehdi ; Wang, Yuqing ; Rosenbach, Misha ; Vleugels, Ruth Ann ; Wei, Kevin ; Harris, John E ; Linus Eng, Chee-Huat ; Afshari, Khashayar ; Anufrieva, Ksenia S ; Martinez, Nuria ; Whiteman, Leah ; Haddadi, Nazgol-Sadat ; Salomão Lopes, Carolina ; Garber, Manuel ; Frieda, Kirsten ; Gallucci, Stefania
Abstract:
Photosensitivity is a hallmark of cutaneous lupus erythematosus (CLE) and dermatomyositis (DM), yet the mechanisms linking ultraviolet B (UVB) exposure to tissue-specific autoimmunity remain incompletely defined. Here, we use an integrative human-based approach, including single-cell RNA sequencing, spatial transcriptomics (seqFISH+), in vivo UVB provocation, and in vitro modeling, to uncover a spatially coordinated inflammatory circuit that underlies interferon-I (IFN-I)-amplified skin pathology.
We identify MMP9
+
CD14
+
myeloid cells as central effectors of photosensitivity in both CLE and DM. These cells are markedly expanded in lesional skin, serve as the dominant source of IFN-β, and colocalize with cytotoxic CD4
+
T cells at the dermal–epidermal junction. Spatial transcriptomics further reveals a keratinocyte-fibroblast-myeloid axis, wherein keratinocytes activate discrete subsets of pro-inflammatory fibroblasts in the superficial dermis to produce monocyte-attracting chemokines, including CCL2, CCL19, CCL7, CCL8, and CXCL12, directing MMP9
+
CD14
+
cell recruitment toward the interface.
In our in-vitro model, IFN-I-primed basal keratinocytes undergo heightened UVB-induced cell death and release membrane-associated cytokines such as TNF-α, IL-1α, which activate monocyte-derived dendritic cells (moDCs) and induce transcriptional programs mirroring those of MMP9
+
CD14
+
cells in vivo. In vivo, UVB irradiation of non-lesional DM skin, but not healthy controls, elicits rapid infiltration of these myeloid cells, confirming their disease-specific responsiveness to UVB.
Finally, in a proof-of-concept clinical study, treatment with anifrolumab (anti-IFN-I receptor) blocked UVB-induced MMP9
+
CD14
+
infiltration and attenuated photosensitivity in CLE.
Together, these findings define a multicellular inflammatory cascade linking keratinocyte injury, fibroblast chemotactic programming, and myeloid effector function in IFN-I-driven skin autoimmunity and nominate MMP9
+
CD14
+
cells as actionable targets in photosensitive dermatoses.
Photosensitivity is central to cutaneous lupus erythematosus (CLE) and dermatomyositis (DM), but the mechanisms linking UVB exposure to tissue-specific autoimmunity are poorly defined. Using single-cell RNA sequencing, spatial transcriptomics, UVB provocation, and in vitro modeling, we identify MMP9
+
CD14
+
myeloid cells as critical mediators of photosensitivity. These cells expand significantly in lesional skin, produce IFN-β, and colocalize with cytotoxic CD4
+
T cells at the dermal-epidermal junction. Keratinocytes activate fibroblasts in the superficial dermis, prompting them to release chemokines (CCL2, CCL19, CCL7, CCL8, CXCL12) that recruit MMP9
+
CD14
+
cells. IFN-I-primed keratinocytes exposed to UVB release cytokines activating dendritic cells, mirroring in vivo responses. UVB irradiation of non-lesional DM skin rapidly recruits these myeloid cells. In a clinical proof-of-concept study, anti-IFN-I treatment with anifrolumab prevented UVB-induced myeloid infiltration and reduced photosensitivity. Thus, targeting MMP9
+
CD14
+
cells may offer therapeutic potential for managing photosensitive autoimmune skin conditions.
100 项与 Spatial Genomics, Inc. 相关的药物交易
登录后查看更多信息
100 项与 Spatial Genomics, Inc. 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年04月01日管线快照
无数据报导
登录后保持更新
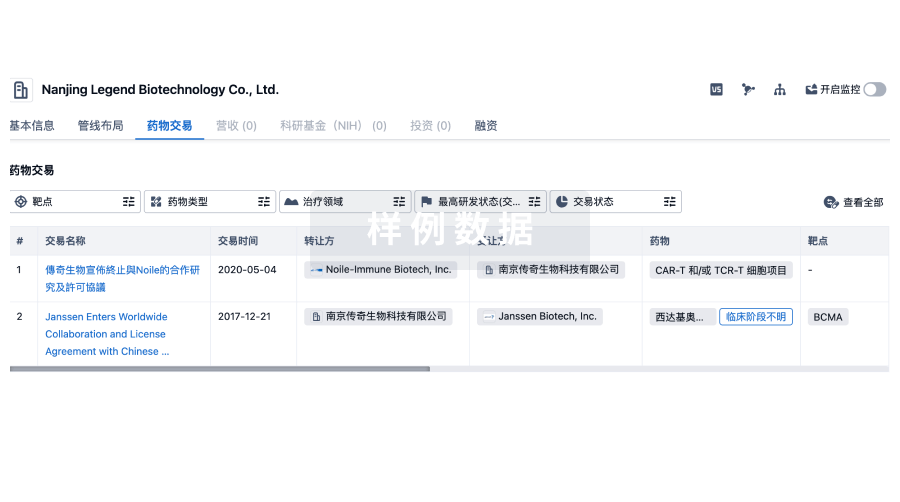
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
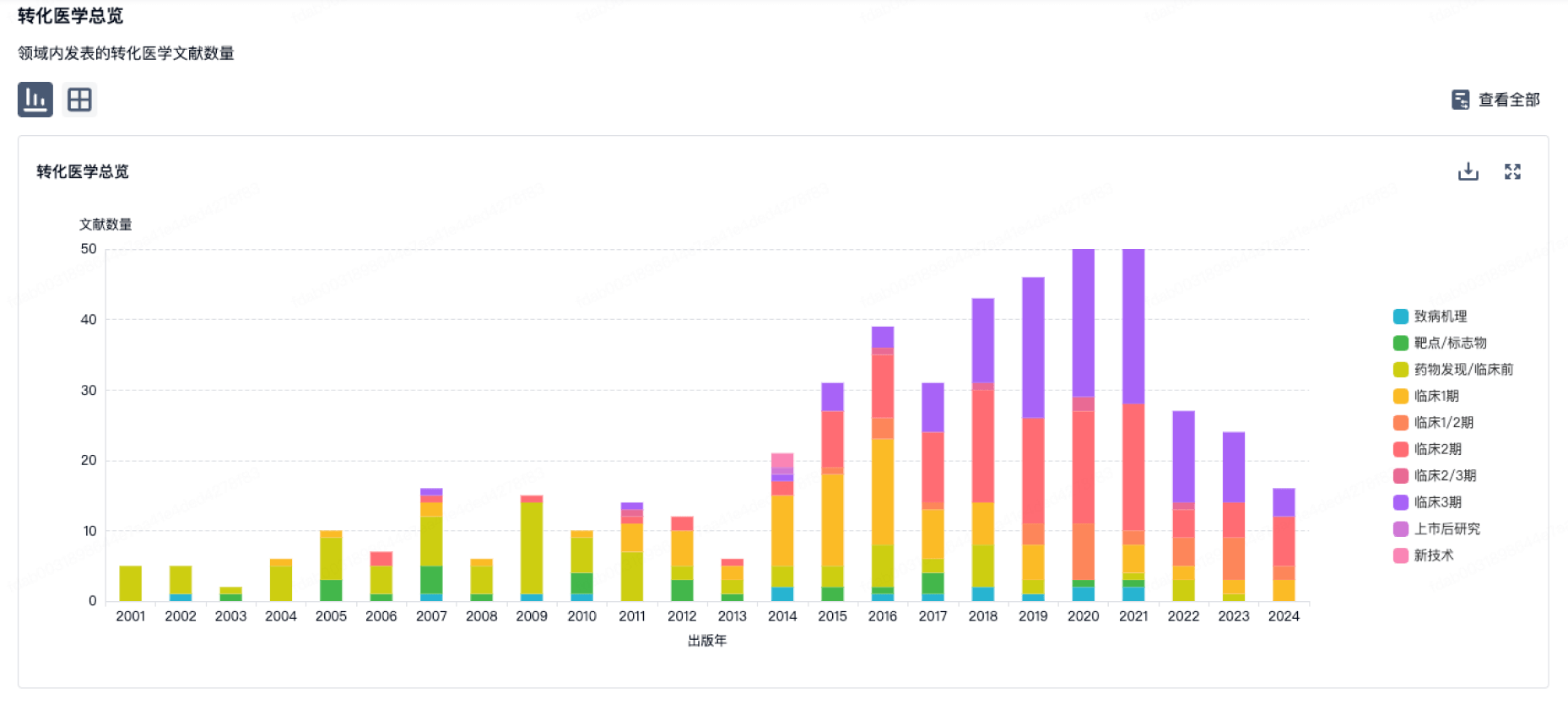
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
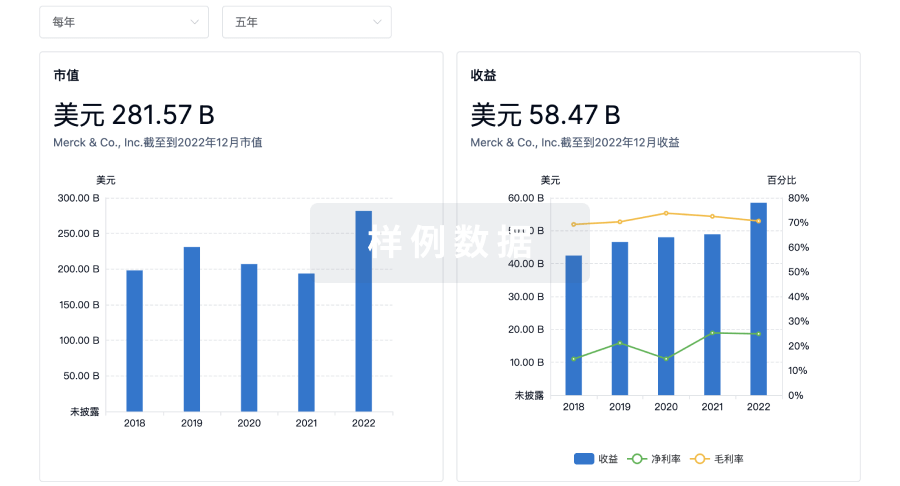
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
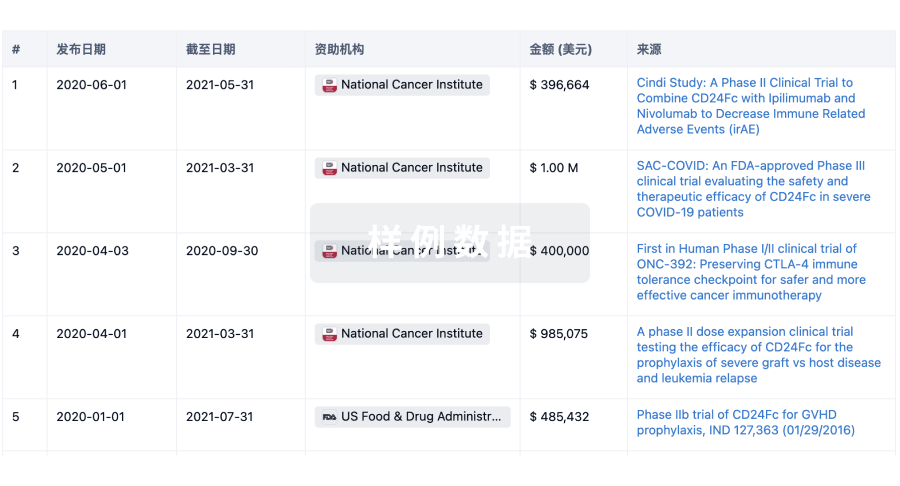
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用