预约演示
更新于:2025-09-21
Scheie Eye Institute
更新于:2025-09-21
概览
关联
100 项与 Scheie Eye Institute 相关的临床结果
登录后查看更多信息
0 项与 Scheie Eye Institute 相关的专利(医药)
登录后查看更多信息
180
项与 Scheie Eye Institute 相关的文献(医药)2025-08-01·OPHTHALMOLOGY
Evaluation of an Association Between COVID-19 Infection and Retinal Hemorrhage in Children
Article
作者: Binenbaum, Gil ; He, Jocelyn ; Yu, Yinxi ; Spiller, Alyssa ; Zhao, Aaron T ; Laub, Natalie
OBJECTIVE:
To evaluate the association of retinal hemorrhage with COVID-19 infection in children.
DESIGN:
Retrospective cohort study.
PARTICIPANTS:
Inpatients and outpatients at Children's Hospital of Philadelphia, ages 1 month to 18 years, who had a dilated fundus examination by an ophthalmologist within one month of a COVID-19 test between January 2020 and October 2023.
METHODS:
Medical records were reviewed for the results of COVID-19 testing and retinal findings. Primary outcome was the association between COVID-19 and retinal hemorrhage assessed across 4 time periods: retinal exam within 7 days, 14 days, 21 days, or 28 days of COVID-19 testing. Generalized estimating equations were used to determine statistical significance and control for age and multiple COVID-19 tests.
MAIN OUTCOME MEASURES:
Association between COVID-19 infection and presence of retinal hemorrhage.
RESULTS:
Among 6,952 children (mean age 6.1 years) studied, 3,496, 4,758, 5,887, and 6,952 children underwent fundus exam within 1, 2, 3, and 4 weeks of a COVID test, respectively. There were no associations between COVID-19 infection and the presence of retinal hemorrhage in any of the time periods: 7 days (OR: 0.80; 95% CI: 0.20-3.32; P=0.76), 14 days (OR: 0.75; 95% CI: 0.24-2.00; P=0.63), 21 days (OR: 0.79; 95% CI: 0.29-2.15; P=0.64), or 28 days (OR: 0.63; 95% CI: 0.23-1.72; P=0.37). All four COVID-19 positive children with retinal hemorrhage had alternative plausible causes with hemorrhage patterns consistent with those other causes.
CONCLUSIONS:
COVID-19 infection is not associated with retinal hemorrhage in children. COVID-19 should not be considered as a potential cause of retinal hemorrhage in children, and this unsupported theory should not be accepted clinically or in legal proceedings.
2025-07-01·OPHTHALMIC PLASTIC AND RECONSTRUCTIVE SURGERY
The Relationship Between Blepharoptosis and Psychosocial Health in the All of Us Research Program
Article
作者: He, Jocelyn ; Ying, Gui-Shuang ; Katowitz, William R. ; Zhao, Aaron T.
Purpose::
The authors aimed to investigate the association between blepharoptosis (ptosis) and psychosocial stress levels, depression, and anxiety in a diverse population of American adults.
Methods::
Utilizing data from the National Institutes of Health’s All of Us Research Program, the authors analyzed responses from 104,456 participants who completed psychosocial assessments. Participants with a history of a ptosis diagnosis were 1:3 matched with controls using propensity score calculated based on demographics and comorbidities. Univariate and multivariable regression models were used to evaluate associations.
Results::
Among 1,032 participants (mean age: 70.0 years, 33.6% male) with ptosis, the prevalence of depression and anxiety (15.3% vs. 5.2%; p < 0.001) was significantly higher (43.7% vs. 18.2%; p < 0.001) compared to 3,096 matched controls. Multivariable analysis revealed increased odds of depression (OR: 3.25; 95% CI: 2.78–3.80; p < 0.001) and anxiety (OR: 3.13; 95% CI: 2.47–3.96; p < 0.001) among those with ptosis. Female participants with ptosis had greater odds of depression (OR: 3.44 vs. 2.90) and anxiety (OR: 3.13 vs. 3.04) compared with males. In univariate analysis, participants with ptosis had greater scores in the University of California Los Angeles Loneliness Scale (18.53 vs. 18.23; p = 0.03) and Everyday Discrimination Scale (0.62 vs. 0.57; p = 0.02) than controls. However, these associations were not significant in the multivariate analysis. In multivariate analysis, female participants with ptosis had greater Everyday Discrimination Scale scores than matched controls (1.10 vs. 1.02; p = 0.004).
Conclusions::
Ptosis is significantly associated with higher rates of depression and anxiety, particularly in females. This underscores the need for comprehensive treatment approaches that address both aesthetic and psychological needs.
2025-07-01·AMERICAN JOURNAL OF OPHTHALMOLOGY
Gender Differences in Patient-Physician Communication in Ophthalmic Practice, Pre- and Post-COVID-19 Period
Article
作者: Ross, Ahmara G ; Alexis, Dominique A ; Higginbotham, Eve J ; Mumford, Sunni ; Brown, Jasmine S
PURPOSE:
Physician communication patterns can increase patient satisfaction and adherence to therapy in the primary care setting. This study investigated gender differences in ophthalmologist communication patterns before and after the COVID-19 pandemic.
DESIGN:
Retrospective cohort study.
METHODS:
Messages sent by ophthalmic patients at Penn Medicine from 2017 to 2022 were collected. Differences in the number of physician messages sent for a given patient, median response length, and response time to patient inquiries and messages were examined based on year and physician gender.
RESULTS:
Female ophthalmologists sent longer response messages to their patients (median [25th, 75th percentiles] response length for women vs men: 672 [492-965] characters vs 637 [460, 918] characters; P < .0001) and a higher number of response messages per patient than their male counterparts (mean [SD] for women vs men: 5.5 [2.9] vs 3.0 [1.5]; P = .04). There was an increase in this gender difference in the peri- and post-COVID-19 period (ie, 2020-2022) (P = .007). Male ophthalmologists sent a higher percentage of same-day responses from 2017 to 2020 (P < .0001), whereas female ophthalmologists sent a higher percentage of same-day responses from 2021 to 2022 (P < .0001). The largest gender difference in same-day responses occurred in 2020 (34% for men vs 30% for women; P < .0001).
CONCLUSIONS:
Gender differences exist in ophthalmologist communication patterns, and the COVID-19 pandemic impacted these differences. Future studies will be helpful in determining the potential association of these specific communication patterns with patient satisfaction assessments, eye health outcomes, and physician burnout.
7
项与 Scheie Eye Institute 相关的新闻(医药)2025-05-15
ARVO presentation highlights 12-month results from Phase 1/2 study that support potential of OPGx-LCA5 gene therapy to restore meaningful vision Pediatric cohort of LCA5 study ongoing with initial multi-patient data anticipated in Q3 2025 OPGx-BEST1 on track for IND filing and initiation of Phase 1/2 trial with early data expected in Q1 2026 Leading healthcare investors provide funding to deliver on key milestones RESEARCH TRIANGLE PARK, N.C., May 15, 2025 (GLOBE NEWSWIRE) -- Opus Genetics, Inc. (Nasdaq: IRD), a clinical-stage ophthalmic biopharmaceutical company developing important new therapies for the treatment of inherited retinal diseases (IRDs) and other ophthalmic disorders (“Opus” or the “Company”), today announced financial results for the first quarter ended March 31, 2025, and provided a corporate update. “Opus is off to a strong start in 2025, with progress across our two product portfolios – the inherited retinal disease platform and the phentolamine eye drop franchise,” said George Magrath, M.D., Chief Executive Officer. “We reported positive 12-month data from the Phase 1/2 trial of OPGx-LCA5 for the treatment of Leber congenital amaurosis 5 (LCA5), an inherited disease which leads to severe vision loss from infancy. The evidence of durable efficacy in adult patients is very encouraging, with the treatment benefits previously seen at 6 months now sustained out to one year. We are now enrolling pediatric patients and are encouraged by the meaningful improvement in visual function and early safety profile observed in the first of these patients at one month.” Dr. Magrath continued, “We believe that the initial success with our lead IRD program, OPGx-LCA5, has the potential to translate to the rest of our pipeline, which includes gene therapy candidates for six additional IRDs. We plan to initiate a Phase 1/2 study with our BEST-1 program later this year with early data expected in the first quarter of 2026. “In the phentolamine eye drop pipeline, we look forward to near-term clinical data readouts from the Phase 3 data trials in dim light vision disturbances and in presbyopia. We ended the first quarter with a strong cash position, having completed a successful financing with leading institutional healthcare investors who share our confidence in the Company’s strategic direction,” concluded Dr. Magrath. Strategic Highlights Opus’s pipeline includes a portfolio of seven adeno-associated virus (AAV)-based gene therapy assets, each targeting a specific IRD, as well as Phentolamine Ophthalmic Solution 0.75%, which is currently being evaluated in presbyopia and mesopic (dim) light vision disturbances (DLD) after keratorefractive surgery.Emerging clinical data on OPGx-LCA5 provide evidence of clinical proof of concept and support the potential of this novel gene therapy to restore meaningful vision for individuals with mutations in the LCA5 gene.Another gene therapy candidate, OPGx-BEST1, which Opus is developing for treatment of bestrophin-1 (BEST1)-related IRD, is on track to enter the clinic by the fourth quarter of 2025, with preliminary data expected in the first quarter of 2026.In March 2025, Opus completed a successful underwritten public offering and concurrent private placement anchored by leading healthcare investors, Perceptive Advisors and Nantahala Capital. The transaction raised approximately $21.5 million in gross proceeds with the potential for up to $21.4 million in additional proceeds upon exercise of warrants that are tied to data release from the BEST1 program. Recent Business Highlights and Corporate Updates Gene Therapy Programs OPGx-LCA5 Opus’ most advanced investigational gene therapy candidate, OPGx-LCA5, is being developed to treat patients with inherited retinal degeneration due to biallelic mutations in the LCA5 gene, an early-onset, severe hereditary retinal degeneration.One-year open-label data on adult patients being treated in the ongoing Phase 1/2 clinical trial of OPGx-LCA5 were featured in an oral presentation by Dr. Tomas Aleman of the Scheie Eye Institute, University of Pennsylvania, at the Association for Research in Vision and Ophthalmology (ARVO) annual meeting, in Salt Lake City. All treated patients had late-stage disease. Improvements in subjective and objective measures of efficacy that had been observed at six months persisted for one year.Enrollment in a cohort of three pediatric patients in the Phase 1/2 trial began in February 2025. Preliminary data on the first patient showed an encouraging early safety profile and meaningful improvement in visual function at one month. The pediatric cohort is expected to complete enrollment in the second quarter of 2025, with initial data from all three patients anticipated in the third quarter of 2025.The U.S. Food and Drug Administration (the “FDA”) granted a Regenerative Medicine Advanced Therapy (“RMAT”) designation to OPGx-LCA5 based on the early data from the first three patients treated. The RMAT designation program offers the potential for expedited development and review of regenerative medicine therapies that demonstrate the potential to address serious or life-threatening diseases based on preliminary clinical evidence. The designation provides sponsors with early interactions with the FDA, guidance on efficient development and manufacturing, and the opportunity to discuss surrogate endpoints to support accelerated approval.A Type D meeting was held with the FDA in March 2025 to discuss the potential regulatory path for OPGx-LCA5, including the design of a potential registrational study. Opus will continue to work with the FDA on the most appropriate design, including the primary endpoint. OPGx-BEST1 OPGx-BEST1 is an investigational Phase 1/2-ready asset in development for IRDs associated with mutations in the BEST1 gene (sometimes referred to as “Best Disease”), which can lead to legal blindness.In IND-enabling studies of OPGx-BEST1 provided safety and efficacy data in support of a first-in-human clinical trial.Opus plans to file an IND and begin a Phase 1/2 trial by the fourth quarter of 2025, with preliminary data expected in the first quarter of 2026. Phentolamine Ophthalmic Solution 0.75% The LYNX-2 pivotal Phase 3 trial evaluating Phentolamine Ophthalmic Solution 0.75% for the treatment of visual loss in low light conditions associated with keratorefractive surgery completed enrollment in the first quarter of 2025 with topline data expected mid-year 2025. The LYNX-2 trial is covered by a Special Protocol Assessment (“SPA”) agreement with the FDA, which ensures agreement with the FDA on the trial design, endpoints, and study size (power).The FDA granted Fast Track designation for Phentolamine Ophthalmic Solution 0.75% for treatment of significant chronic night driving impairment with concomitant increased risk of motor vehicle accidents and debilitating loss of best spectacle corrected mesopic vision in keratorefractive patients with photic phenomena (i.e., glare, halos, starburst).The VEGA-3 pivotal Phase 3 trial evaluating Phentolamine Ophthalmic Solution 0.75% for the treatment of presbyopia completed enrollment in the first quarter of 2025, with topline data expected in the first half of 2025.The development portfolio related to Phentolamine Ophthalmic Solution 0.75% is being funded by the Company’s partner, Viatris Inc., in both indications (presbyopia and dim light vision disturbances). Expected Growth Drivers in 2025 and Beyond Initial data from three pediatric patients treated with OPGx-LCA5 anticipated in Q3 2025.IND filing and initiation of a Phase 1/2 clinical trial for OPGx-BEST1 is planned for 2025, with preliminary data expected in Q1 2026.Topline data from the LYNX-2 pivotal Phase 3 trial evaluating Phentolamine Ophthalmic Solution 0.75% for visual loss in low light conditions associated with keratorefractive surgery are expected mid-year 2025.Topline data from the VEGA-3 pivotal Phase 3 clinical trial evaluating Phentolamine Ophthalmic Solution 0.75% for the treatment of presbyopia are expected in the first half of 2025. Financial Highlights for the First Quarter Ended March 31, 2025 As of March 31, 2025, Opus had cash and cash equivalents of $41.8 million. Based on current projections, management believes that the cash on hand will be sufficient to fund operations into the second quarter of 2026. License and collaborations revenue was $4.4 million and $1.7 million during the three months ended March 31, 2025 and 2024, respectively. Revenue during both quarterly periods was derived from the Company’s license and collaboration agreement (the “Viatris License Agreement”) with Viatris, Inc. (“Viatris”) largely from the reimbursement of research and development services and to a much lesser degree from royalty payments stemming from the sales of RYZUMVI™ by Viatris. General and administrative (“G&A”) expenses for the three months ended March 31, 2025 were $6.3 million compared to $4.7 million for the three months ended March 31, 2024. The increase was primarily attributable to professional services fees, corporate legal support, legal fees associated with intellectual property and public company costs, including filing fees and investor relations and governance costs, offset in part by decreases in general operating and other costs on a net basis. G&A expenses included $0.6 million and $0.8 million in stock-based compensation expense during the three months ended March 31, 2025 and 2024, respectively. Research and development (“R&D”) expenses for the three months ended March 31, 2025 were $8.0 million compared to $4.7 million for the three months ended March 31, 2024. The increase was primarily attributable to higher clinical costs and payroll related costs, offset partially by lower manufacturing expenses attributed to an activity reduction in the VEGA-2 trial and by lower regulatory and other costs on a net basis. Pursuant to the Viatris License Agreement, budgeted R&D expenses related to the development of the Phentolamine Ophthalmic Solution 0.75% products have been fully reimbursed by Viatris to date. R&D expenses included $0.3 million and $0.2 million in stock-based compensation expense during the three months ended March 31, 2025 and 2024, respectively. Net loss for the quarter ended March 31, 2025, was $8.2 million or $(0.24) per basic and diluted share, as compared to net loss of $7.1 million, or $(0.29) per basic and diluted share, for the quarter ended March 31, 2024. For further details on financial results, refer to the Company’s Quarterly Report on Form 10-Q for the quarter ended March 31, 2025 to be filed with the Securities and Exchange Commission (the “SEC”). About Opus Genetics Opus Genetics is a clinical-stage ophthalmic biopharmaceutical company developing therapies to treat patients with IRDs and other treatments for ophthalmic disorders. Our pipeline includes adeno-associated virus (AAV)-based investigational gene therapies that address gene mutations responsible for different forms of Leber congenital amaurosis (“LCA”), bestrophinopathy and retinitis pigmentosa. Our most advanced investigational gene therapy program is designed to address mutations in the LCA5 gene, which encodes the lebercilin protein and is currently being evaluated in a Phase 1/2 open-label, dose-escalation trial, with encouraging early data. Our pipeline also includes BEST1 investigational gene therapy, designed to address mutations in the BEST1 gene, which is associated with retinal degeneration. The pipeline also includes Phentolamine Ophthalmic Solution 0.75%, a non-selective alpha-1 and alpha-2 adrenergic antagonist being investigated to reduce pupil size that is currently being evaluated in Phase 3 trials for presbyopia and mesopic (dim) light vision disturbances. For additional information, please visit www.opusgtx.com. University of Pennsylvania (“Penn”) Financial Disclosure: The laboratory of Dr. Tomas Aleman has received clinical trial research funding from Opus Genetics. Penn and Dr. Aleman have either received, or may receive in the future, financial consideration related to the licensing of certain Penn intellectual property to Opus Genetics. Forward Looking Statements This press release contains forward-looking statements within the meaning of the Private Securities Litigation Reform Act of 1995. Such statements include, but are not limited to, expectations regarding our cash runway, expectations of potential growth, and statements concerning data from and future enrollment for our clinical trials and our pipeline of additional indications. These forward-looking statements relate to us, our business prospects and our results of operations and are subject to certain risks and uncertainties posed by many factors and events that could cause our actual business, prospects and results of operations to differ materially from those anticipated by such forward-looking statements. Factors that could cause or contribute to such differences include, but are not limited to, those described under the heading “Risk Factors” included in our Annual Report on Form 10-K for the fiscal year ended December 31, 2024, our Quarterly Report on Form 10-Q for the quarter ended March 31, 2025, and in our other filings with the SEC. Readers are cautioned not to place undue reliance on these forward-looking statements, which speak only as of the date of this press release. In some cases, you can identify forward-looking statements by the following words: “anticipate,” “believe,” “continue,” “could,” “estimate,” “expect,” “intend,” “aim,” “may,” “ongoing,” “plan,” “potential,” “predict,” “project,” “should,” “will,” “would” or the negative of these terms or other comparable terminology, although not all forward-looking statements contain these words. We undertake no obligation to revise any forward-looking statements in order to reflect events or circumstances that might subsequently arise. These forward-looking statements are based upon our current expectations and involve assumptions that may never materialize or may prove to be incorrect. Actual results and the timing of events could differ materially from those anticipated in such forward-looking statements as a result of various risks and uncertainties, including, without limitation: Our clinical data related to gene therapies for the treatment of IRDs are preliminary and related to a relatively small group of patients, and, as a result, data that initially appear promising may be revised, updated, or invalidated at a later data readout and/or may ultimately not be capable of duplication in additional patients;Failure to successfully integrate our businesses following our acquisition of former Opus Genetics Inc. (the “Opus Acquisition”) could have a material adverse effect on our business, financial condition and results of operations;The Opus Acquisition significantly expanded our product pipeline and business operations and shifted our business strategies, which may not improve the value of our common stock;Our gene therapy product candidates are based on a novel technology that is difficult to develop and manufacture, which may result in delays and difficulties in obtaining regulatory approval;Our planned clinical trials may face substantial delays, result in failure, or provide inconclusive or adverse results that may not satisfy FDA requirements to further develop our therapeutic products;Delays or difficulties associated with patient enrollment in clinical trials may affect our ability to conduct and complete those clinical trials and obtain necessary regulatory approvals;Changes in regulatory requirements could result in increased costs or delays in development timelines;We depend heavily on the success of our product pipeline; if we fail to find strategic partners or fail to adequately develop or commercialize our pipeline products, our business will be materially harmed;Others may discover, develop, or commercialize products similar to those in our pipeline before or more successfully than we do or develop generic variants of our products even while our product patents remain active, thereby reducing our market share and potential revenue from product sales;We do not currently have any sales or marketing infrastructure in place, and we have limited drug research and discovery capabilities;The future commercial success of our products could significantly depend upon several uncertain factors, including third-party reimbursement practices and the existence of competitors with similar products;Product liability lawsuits against us or our suppliers or manufacturers could cause us to incur substantial liabilities and could limit commercialization of any product candidate that we may develop;Failure to comply with health and safety laws and regulations could lead to material fines;We have not generated significant revenue from sales of any products and expect to incur losses for the foreseeable future;Our future viability is difficult to assess due to our short operating history and our future need for substantial additional capital, access to which could be limited by any adverse developments that affect the financial services market;Raising additional capital may cause our stockholders to be diluted, among other adverse effects;We operate in a highly regulated industry and face many challenges adapting to sudden changes in legislative reform or the regulatory environment, which affects our pipeline stability and could impair our ability to compete in international markets;We may not receive regulatory approval to market our developed product candidates within or outside of the U.S.;With respect to any of our product candidates that receive marketing approval, we may be subject to substantial penalties if we fail to comply with applicable regulatory requirements;Our potential relationships with healthcare providers and third-party payors will be subject to certain healthcare laws and regulations, which could expose us to extensive potential liabilities;We rely on third parties for material aspects of our business, such as conducting our nonclinical and clinical trials and supplying and manufacturing bulk drug substances, which exposes us to certain risks;We may be unsuccessful in entering into or maintaining licensing arrangements (such as the Viatris License Agreement) or establishing strategic alliances on favorable terms, which could harm our business;Our current focus on the cash-pay utilization for future sales of RYZUMVI™ may limit our ability to increase sales or achieve profitability with this product;Inadequate patent protection for our product candidates may result in our competitors developing similar or identical products or technology, which would adversely affect our ability to successfully commercialize;We may be unable to obtain full protection for our intellectual property rights under U.S. or foreign laws;We may become involved in lawsuits for a variety of reasons associated with our intellectual property rights, including alleged infringement suits initiated by third parties;We are dependent on our key personnel, and if we are not successful in attracting and retaining highly qualified personnel, we may not be able to successfully implement our business strategy;As we grow, we may not be able to operate internationally or adequately develop and expand our sales, marketing, distribution, and other corporate functions, which could disrupt our operations;The market price of our common stock is expected to be volatile;Our common stock may be subject to delisting from the Nasdaq Capital Market and delisting could adversely affect our ability to access capital markets;Factors out of our control related to our securities, such as securities litigation or actions of activist stockholders, could adversely affect our business and stock price and cause us to incur significant expenses; andImpact from current or proposed tariffs on imported goods we purchase. The foregoing review of important factors that could cause actual events to differ from expectations should not be construed as exhaustive. Readers are urged to carefully review and consider the various disclosures made by us in this report and in our other reports filed with the SEC that advise interested parties of the risks and factors that may affect our business. All forward-looking statements contained in this press release speak only as of the date on which they were made. We undertake no obligation to update such statements to reflect events that occur or circumstances that exist after the date on which they were made. Contacts Corporate Investor RelationsNirav Jhaveri, CFOir@ocuphire.comCorey Davis, Ph.D. LifeSci Advisors cdavis@lifesciadvisors.com Opus Genetics, Inc.Condensed Consolidated Balance Sheets(in thousands, except share amounts and par value) As of March 31, December 31, 2025 2024Assets (Unaudited) Current assets:
Cash and cash equivalents $41,792 $30,321 Accounts receivable 3,080 3,563 Contract assets and unbilled receivables 1,675 2,209 Prepaids and other current assets 1,380 515 Short-term investments 1 2 Total current assets 47,928 36,610 Property and equipment, net 239 252 Total assets $48,167 $36,862
Liabilities and stockholders’ equity
Current liabilities:
Accounts payable $2,430 $3,148 Accrued expenses and other liabilities 9,106 8,147 Warrant liabilities 12,715 — Total current liabilities 24,251 11,295 Total liabilities 24,251 11,295
Commitments and contingencies
Series A preferred stock, par value $0.0001; 14,146 shares were designated as of March 31, 2025 and December 31, 2024; 14,145.374 shares issued and outstanding at March 31, 2025 and December 31, 2024. 18,843 18,843
Stockholders’ equity:
Preferred stock, par value $0.0001; 9,985,854 shares authorized as of March 31, 2025 and December 31, 2024; no shares issued and outstanding at March 31, 2025 and December 31, 2024. — — Common stock, par value $0.0001; 125,000,000 shares authorized as of March 31, 2025 and December 31, 2024; 45,483,823 and 31,574,657 shares issued and outstanding at March 31, 2025 and December 31, 2024, respectively. 5 3 Additional paid-in capital 152,260 145,719 Accumulated deficit (147,192) (138,998)Total stockholders’ equity 5,073 6,724 Total liabilities, series A preferred stock, and stockholders’ equity $48,167 $36,862
Opus Genetics, Inc.Condensed Consolidated Statements of Comprehensive Loss(in thousands, except share and per share amounts)(Unaudited) Three Months Ended March 31,
2025 2024
License and collaborations revenue $4,370 $1,711
Operating expenses:
General and administrative 6,346 4,670 Research and development 7,953 4,749 Total operating expenses 14,299 9,419 Loss from operations (9,929) (7,708)Financing costs (1,372) — Fair value change in warrant liabilities 2,805 — Other income, net 302 602 Loss before income taxes (8,194) (7,106)Benefit (provision) for income taxes — — Net loss (8,194) (7,106)Other comprehensive loss, net of tax — — Comprehensive loss $(8,194) $(7,106)Net loss per share:
Basic and diluted $(0.24) $(0.29)Number of shares used in per share calculations:
Basic and diluted 33,884,920 24,520,475
临床3期财报快速通道基因疗法
2025-04-02
REDWOOD CITY, Calif., April 2, 2025 /PRNewswire/ -- Avisi Technologies, a clinical-stage ophthalmic device company, today announced encouraging six‐month interim results from the VITA trial evaluating its VisiPlate® device, an ultrathin, multichannel aqueous shunt in study subjects diagnosed with open-angle glaucoma. Data were presented by Eydie Miller-Ellis, MD, as a Top Paper at the American Glaucoma Society Annual Meeting in Washington, D.C.
Key Trial Data
The multi‐site VITA trial, a prospective pilot study designed to assess the safety and effectiveness of Avisi Technologies' investigational VisiPlate® device, enrolled and treated 15 subjects (mean age 55.6±17.1 years) with open-angle glaucoma and no prior filtration surgery. Subjects were implanted in one eye at three South African centers. Baseline intraocular pressure (IOP) of the cohort averaged 24.1 mmHg (ranging from 18.8 mmHg to 40.2 mmHg), with the study eyes requiring an average of 2.0 glaucoma medications (ranging from 0 to 4 medications). At six months following standalone VisiPlate® implantation:
Mean IOP decreased by 40.4%, to 14.0 mmHg with a corresponding reduction to 0.8 medications.
78.6% of study eyes achieved a ≥20% IOP reduction on the same or fewer medications, exceeding the study's primary effectiveness endpoints.
57.1% of study eyes required no IOP-lowering medication.
The VisiPlate® device demonstrated a favorable safety profile with no subject losing ≥2 lines of best-corrected visual acuity (BCVA), and no need for device removal or additional glaucoma procedures.
Device Features
Avisi Technologies' VisiPlate® shunt is a unique design made of a patented metamaterial that has been designed to be non-fibrotic and is many times thinner than a human hair. The device is both doctor and patient-centric, designed for ease of implantation, longevity, comfort, and aesthetics. Its multiple, redundant microchannels are engineered to provide healthy aqueous flow while minimizing the risk of blockage, a common challenge with currently available glaucoma surgical solutions.
Dr. Miller-Ellis, Vice President of the American Glaucoma Society and Director of Glaucoma at the University of Pennsylvania, Scheie Eye Institute, shared her excitement about the positive VisiPlate® performance in Ultrathin Shunt Shows Promising Results in Trial, an article by Jim Gallagher, Senior Managing Editor at Glaucoma Physician. "I call it 'building a better bleb,' because after trabeculectomy or other filtering surgeries blebs can be very elevated and cause the patient some discomfort," she noted. "That tendency of bleb shape is partially attributable to the single lumen outflow of other available stents. If all the aqueous is coming out in one outflow path, then the aqueous force is more concentrated centrally in the bleb, causing more elevation in that area. Our goal is to have a more diffuse outflow of aqueous that's more comfortable for the patient."
Dr. Miller-Ellis also noted that surgeons in the VITA trial found the VisiPlate® surgical procedure to be easier and faster than a standard trabeculectomy, with less involved postoperative management being required.
Expert Commentary
Joseph F. Panarelli, MD, Director of Glaucoma Services at NYU Langone Health and Professor of Ophthalmology at NYU Grossman School of Medicine, commented, "These results are very exciting and I'm anticipating having VisiPlate be a part of my practice in the future. I like the multichannel design and the potential for a straightforward surgery and simpler follow up. If we could have pediatric applications one day, that would be fantastic too."
Ehsan Sadri, MD, FACS, FAAO, Founder of Visionary Eye Institute, also shared his enthusiasm stating,
"The six-month VITA trial results for the VisiPlate® aqueous shunt are truly remarkable. A 40% reduction in IOP and over half of study eyes completely off medications—these are the kinds of outcomes we strive for in glaucoma care, especially when achieved through a minimally invasive approach. The metamaterial design and multichannel architecture of VisiPlate® represent a new frontier in safe, sustained IOP control.
As a surgeon committed to offering the most advanced and patient-centered care, I'm excited about the potential to incorporate VisiPlate® into my practice. Its ultrathin profile, ease of implantation, and impressive safety profile underscore the promise of this technology. I believe VisiPlate® could fundamentally shift how we manage moderate to advanced open-angle glaucoma and open the door to a better quality of life for our patients."
The paper presented by Dr. Miller-Ellis at the American Glaucoma Society Annual Meeting was the result of a strong international collaboration, with co-authors including Jonathan S. Myers, MD (Chief, Glaucoma Service at Wills Eye Hospital, Professor, Sidney Kimmel Medical College at Thomas Jefferson University), Lynette Venter, MD, MBChB, MMed (Ophth), FC Ophth(SA), Paul Roux, MD (Former Head of the Department of Ophthalmology at Pretoria University), Petrus Gous, MD (Founder of Pretoria Eye Institute), Laura Straub, Morné de Bruin, OD, and Eydie G. Miller-Ellis, MD.
Next Steps
The VITA trial is now complete. Full 12-month results will be announced at a future date.
About VisiPlate®
The investigational VisiPlate® aqueous shunt is Avisi Technologies' flagship "minimally invasive bleb surgery" (MIBS) device. Made from non-fibrotic nanotechnology-enabled metamaterials, it works by wicking pent-up aqueous humor from the inside of the eye to a secondary drainage zone via a network of interconnected microchannels, rather than a large tube. The device is engineered to lower IOP while maintaining patient comfort and aesthetics. It is an investigational device and is not yet available for sale.
About Glaucoma
Glaucoma is the leading cause of irreversible blindness worldwide and currently has no cure. In glaucoma patients, excess fluid builds up within the eye, increasing pressure on the optic nerve and leading to permanent vision loss. Glaucoma is a group of diseases, the most common of which are primary open-angle glaucoma (POAG) and angle-closure glaucoma.
POAG, the most prevalent form of glaucoma, often has no early warning signs or symptoms. It occurs when the eye's drainage system (trabecular meshwork) becomes clogged, preventing normal fluid outflow and leading to elevated eye pressure. Without diagnosis and treatment, POAG can cause gradual vision loss over time.
About Avisi Technologies
Avisi Technologies is a clinical-stage medical device company committed to advancing vision care through innovative ophthalmic solutions. The company's portfolio includes state-of-the-art treatments for glaucoma and other ocular conditions. These include its flagship VisiPlate® aqueous shunt, a sustained drug delivery platform, and a device to treat mild glaucoma. Avisi Technologies' VisiPlate device has been recognized as a promising new technology by numerous organizations, including the National Science Foundation, the Glaucoma Research Foundation, SXSW, Johnson & Johnson JLABs, Medtech Innovator Accelerator, UCSF Rosenman Institute, and the University of Pennsylvania, among others. Avisi has been funded by early-stage venture capital investors, angel investors, and research grants from the National Science Foundation. For more information, visit avisitech.com.
SOURCE Avisi Technologies
WANT YOUR COMPANY'S NEWS FEATURED ON PRNEWSWIRE.COM?
440k+
Newsrooms &
Influencers
9k+
Digital Media
Outlets
270k+
Journalists
Opted In
GET STARTED
临床结果临床研究
2024-12-03
6-month efficacy and safety data from ongoing Phase 1/2 trial of OPGx-LCA5 to be presentedFARMINGTON HILLS, Mich., Dec. 03, 2024 (GLOBE NEWSWIRE) -- Opus Genetics, Inc. (Nasdaq: IRD), a clinical-stage ophthalmic biotechnology company developing gene therapies for the treatment of inherited retinal diseases (IRDs) and other ophthalmic disorders, today announced that it will host a virtual key opinion leader (KOL) event on Wednesday, December 11, 2024 at 4:00 PM ET. To register, click here.
The event will feature Jean Bennett, MD, PhD, and Tomas Aleman, MD, from the University of Pennsylvania, along with Christine Kay, MD, and Arshad Khanani, MD, MA, FASRS, who will discuss detailed, patient level 6-month efficacy and safety data on OPGx-LCA5, an adeno-associated virus (AAV)-based gene therapy, in Phase 1/2 development for LCA5-associated inherited retinal disease (IRD).
The event will focus on the OPGx-LCA5 clinical data and will dive into the key efficacy assessments in detail. The presenters will also highlight the current unmet need with respect to LCA5-associated inherited retinal disease, next steps in the development program, and the potential of Opus Genetics’ therapeutic approach.
A live question and answer session will follow the formal presentations.
Jean Bennett, MD, PhD is the F.M. Kirby Emeritus Professor of Ophthalmology at the Perelman School of Medicine and continues to serve as director of the Center for Advanced Retinal and Ocular Therapeutics (CAROT) at the University of Pennsylvania. In addition to Dr. Bennett’s positions at the University of Pennsylvania, she has been an Investigator at the Center for Cellular and Molecular Therapeutics at The Children’s Hospital of Philadelphia (CHOP) for more than a decade. She also co-founded life science companies Spark Therapeutics (acquired by Roche), GenSight Biologics and Limelight Bio. Dr. Bennett received her PhD in Zoology and Cell Biology from the University of California, Berkeley, and obtained her MD from Harvard University. She also completed postdoctoral fellowships in Radiobiology and Environmental Health at the University of California, San Francisco, Human Genetics at the Yale School of Medicine and Development Genetics at the Johns Hopkins University School of Medicine. She received her BS in Biology from Yale University.
Tomas Aleman, MD is the Irene Heinz-Given and John LaPorte Research Professor at the Perelman School of Medicine, University of Pennsylvania. He is an Attending Physician in the Department of Ophthalmology at the Hospital of the University of Pennsylvania. He is part of the Retinal Degeneration Center at Scheie Eye Institute and the Center for Advanced Retinal & Ocular Therapeutics (CAROT), also at the University of Pennsylvania. Dr. Aleman has extensive expertise in the study of hereditary retinal degenerations. Most of the studies in which he has been investigator have aimed to lead patients with incurable retinal degenerations into clinical trials as well as in the detailed characterization of patients with these conditions. Dr. Aleman received an M.D. with High Honors from Sup de Cien Med de la Habana and completed a fellowship at the Scheie Eye Institute.
Christine N. Kay, MD is a board-certified ophthalmologist and vitreoretinal surgeon and has been conducting clinical research since 2012. Her focus and passion are inherited retinal diseases, including but not limited to Stargardt disease, Retinitis Pigmentosa, and Achromatopsia. Dr. Kay is the Director of Research at Vitreoretinal Associates in Gainesville, Florida. She and her research team aim to improve the lives of people diagnosed with these and other diseases, as well as prevent blindness. Currently, the clinical trial team is conducting over 20 different studies targeting a multitude of retinal diseases. She was previously an Assistant Professor at the University of Florida and is currently Affiliate faculty at the University of South Florida. Dr. Kay is a member of the Macula Society, Retina Society, and American Society of Retina Specialists.
Arshad M. Khanani, MD, MA, FASRS is the Managing Partner, Director of Clinical Research, and Director of Fellowship at Sierra Eye Associates, as well as a Clinical Professor at the University of Nevada, Reno School of Medicine. Dr. Khanani founded the clinical research department at Sierra Eye Associates, which has since become one of the nation's leading centers for clinical research. He has served as the principal investigator in over 120 clinical trials and has been a top enroller for several Phase 1-3 trials. He is also at the forefront of several collaborative studies examining real-world outcomes for newly approved treatments. Additionally, Dr. Khanani has been the first to perform surgical procedures in various clinical trials focused on sustained drug delivery and gene therapy. His extensive body of work includes numerous publications in highly regarded journals such as The Lancet, Ophthalmology, and JAMA Ophthalmology. Dr. Khanani is a lead principal investigator for several ongoing clinical trials and contributes to national and international clinical trial steering committees and scientific advisory boards. These efforts are aimed at developing new treatment options for patients with retinal diseases. A sought-after speaker, he is frequently invited to present at major national and international meetings. In 2021, Dr. Khanani founded the Clinical Trials at the Summit meeting to foster discussion on clinical trial design and data. Dr. Khanani is a distinguished member of both the Macula Society and the Retina Society, and he has earned various honors throughout his career. In 2019, he was named Healthcare Heroes Physician of the Year by Nevada Business Magazine for his dedication to ophthalmology. In 2023, he was chosen to deliver the prestigious Ernst Bodenheimer Memorial Lecture at the Wilmer Eye Institute, Johns Hopkins University. Dr. Khanani was also the recipient of the American Society of Retina Specialists (ASRS) Presidents’ Young Investigator Award in 2021 and the ASRS Presidential Award in 2024.
About OPGx-LCA5
OPGx-LCA5 is designed to address a form of Leber congenital amaurosis (LCA) due to biallelic mutations in the LCA5 gene (LCA5), which encodes the lebercilin protein. LCA5-associated inherited retinal disease is an early-onset severe inherited retinal dystrophy. Studies in patients with this mutation have reported evidence for the dissociation of retinal architecture and visual function in this disease, suggesting an opportunity for therapeutic intervention through gene augmentation. OPGx-LCA5 uses an adeno-associated virus 8 (AAV8) vector to precisely deliver a functional LCA5 gene to the outer retina. OPGx-LCA5 is currently being evaluated in a Phase 1/2 clinical trial at the University of Pennsylvania designed to evaluate its safety and preliminary efficacy in patients with inherited retinal degeneration due to biallelic mutations in the LCA5 gene. New 6-month efficacy and safety data on OPGx-LCA5 for treatment of LCA5-associated inherited retinal disease will be presented at a virtual KOL event on December 11, 2024.
About Opus Genetics
Opus Genetics is a clinical-stage ophthalmic biotechnology company developing gene therapies to treat patients with inherited retinal diseases (IRDs) and other treatments for ophthalmic disorders. The pipeline includes adeno-associated virus (AAV)-based gene therapies that address mutations in genes that cause different forms of bestrophinopathy, Leber congenital amaurosis (LCA) and retinitis pigmentosa. The company’s most advanced gene therapy program is designed to address mutations in the LCA5 gene, which encodes the lebercilin protein and is currently being evaluated in a Phase 1/2 open-label, dose-escalation trial. BEST1 gene therapy is designed to address mutations in the BEST1 gene, which is associated with retinal degeneration; a Phase 1/2 study is expected to be initiated in 2025. The pipeline also includes Phentolamine Ophthalmic Solution 0.75%, a non-selective alpha-1 and alpha-2 adrenergic antagonist to reduce pupil size, and APX3330, a novel small-molecule inhibitor of Ref-1 to slow the progression of non-proliferative diabetic retinopathy. Phentolamine Ophthalmic Solution 0.75% is currently being evaluated in Phase 3 trials for presbyopia and dim (mesopic) light vision disturbances. For more information, please visit www.opusgtx.com.
Forward Looking Statements
This press release contains forward-looking statements within the meaning of the Private Securities Litigation Reform Act of 1995. Such statements include, but are not limited to, statements concerning expectations regarding data from and future enrollment for our clinical trials and the effectiveness of our pipeline of indications and gene therapies. These forward-looking statements relate to us, our business prospects and our results of operations and are subject to certain risks and uncertainties posed by many factors and events that could cause our actual business, prospects and results of operations to differ materially from those anticipated by such forward-looking statements. Factors that could cause or contribute to such differences include, but are not limited to, those described under the heading “Risk Factors” included in our Quarterly Report on Form 10-Q for the quarter ended September 30, 2024 and in our other filings with the U.S. Securities and Exchange Commission (the “SEC”). Readers are cautioned not to place undue reliance on these forward-looking statements, which speak only as of the date of this press release. In some cases, you can identify forward-looking statements by the following words: “anticipate,” “believe,” “continue,” “could,” “estimate,” “expect,” “intend,” “aim,” “may,” “ongoing,” “plan,” “potential,” “predict,” “project,” “should,” “will,” “would” or the negative of these terms or other comparable terminology, although not all forward-looking statements contain these words. We undertake no obligation to revise any forward-looking statements in order to reflect events or circumstances that might subsequently arise.
These forward-looking statements are based upon our current expectations and involve assumptions that may never materialize or may prove to be incorrect. Actual results and the timing of events could differ materially from those anticipated in such forward-looking statements as a result of various risks and uncertainties, including, without limitation:
Our ability to successfully integrate the business of former Opus Genetics Inc. and manage our expanded combined product pipeline;Our ability to develop and obtain regulatory approval for newly acquired gene therapies to treat inherited retinal diseases;Our ability to obtain and maintain orphan drug designation or rare pediatric disease designation for our current and future product candidates;The success and timing of regulatory submissions and pre-clinical and clinical trials, including enrollment and data readouts;Regulatory requirements or developments;Changes to or unanticipated events in connection with clinical trial designs and regulatory pathways;Delays or difficulties in the enrollment of patients in clinical trials;Substantial competition;Rapid technological change;Our development of sales and marketing infrastructure;Future revenue losses and profitability;Changes in capital resource requirements;Risks related to our inability to obtain sufficient additional capital to continue to advance our product candidates and our preclinical programs;Domestic and worldwide legislative, regulatory, political and economic developments;Our dependency on key personnel;Changes in market opportunities and acceptance;Reliance on third parties to conduct our clinical trials and supply and manufacture drug supplies;Future, potential product liability and securities litigation;System failures, unplanned events, or cyber incidents;The substantial number of shares subject to potential issuance associated with our equity line of credit arrangement;Risks that our licensing or partnership arrangements may not facilitate the commercialization or market acceptance of our product candidates;Future fluctuations in the market price of our common stock;The success and timing of commercialization of any of our product candidates;Obtaining and maintaining our intellectual property rights; andThe success of mergers and acquisitions.
The foregoing review of important factors that could cause actual events to differ from expectations should not be construed as exhaustive. Readers are urged to carefully review and consider the various disclosures made by us in this report and in our other reports filed with the SEC that advise interested parties of the risks and factors that may affect our business. All forward-looking statements contained in this press release speak only as of the date on which they were made. We undertake no obligation to update such statements to reflect events that occur or circumstances that exist after the date on which they were made.
Contacts
CorporateInvestor RelationsNirav JhaveriCFOir@opusgtx.comCorey Davis, Ph.D.LifeSci Advisorscdavis@lifesciadvisors.com
临床3期
100 项与 Scheie Eye Institute 相关的药物交易
登录后查看更多信息
100 项与 Scheie Eye Institute 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年04月01日管线快照
无数据报导
登录后保持更新
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
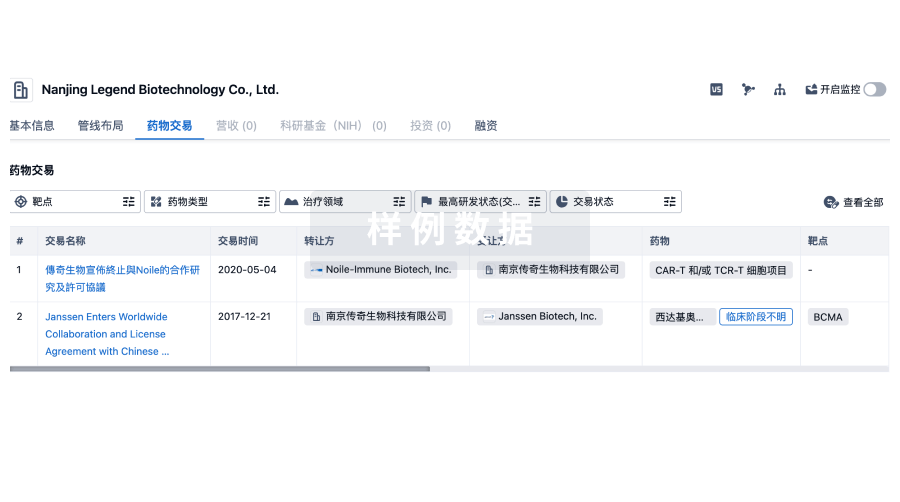
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
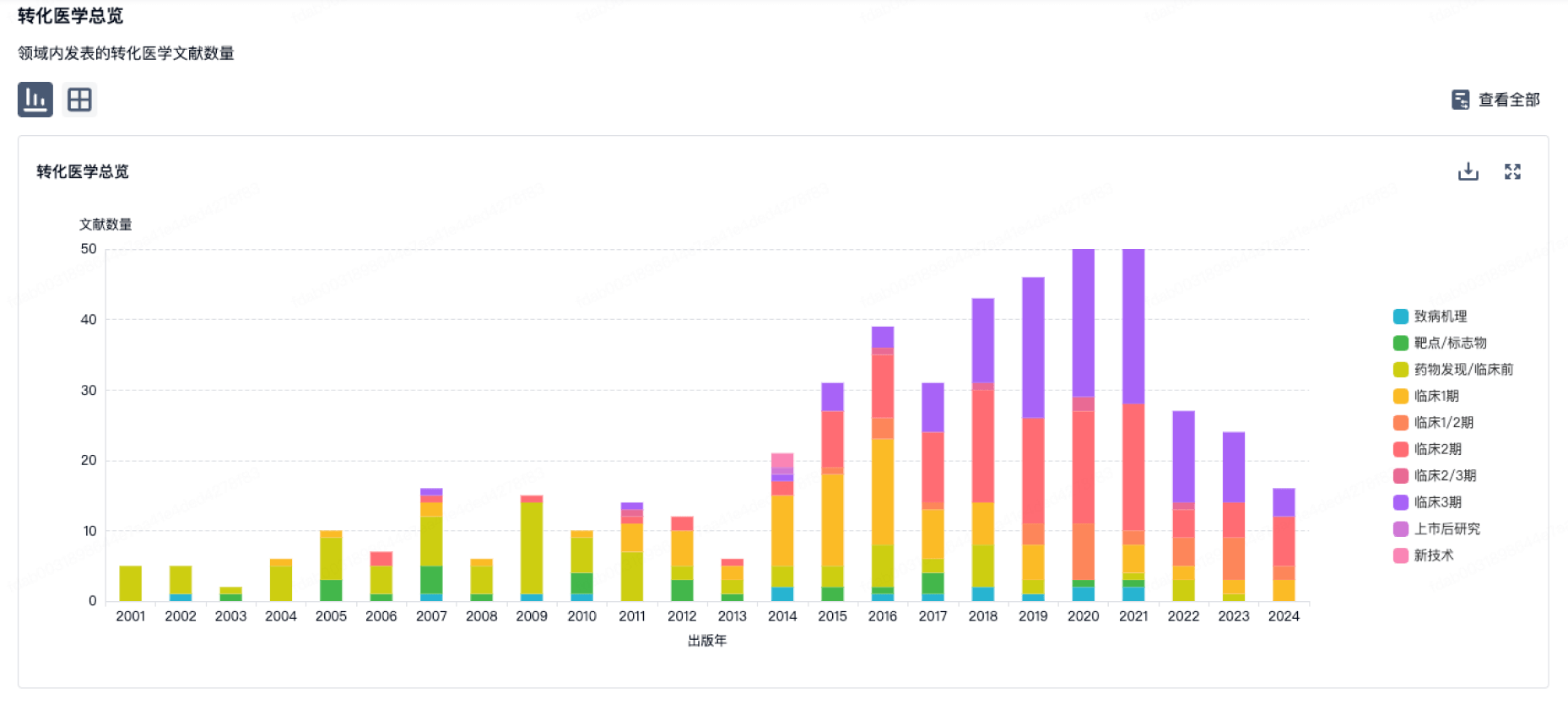
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
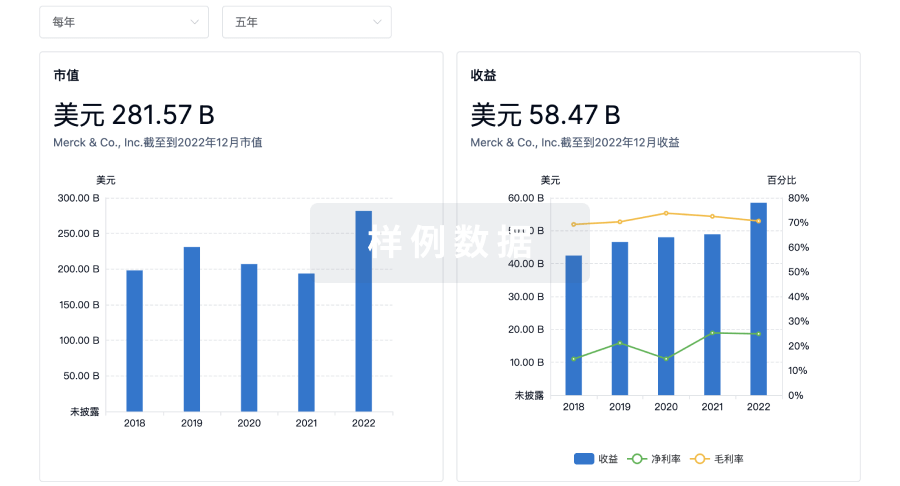
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
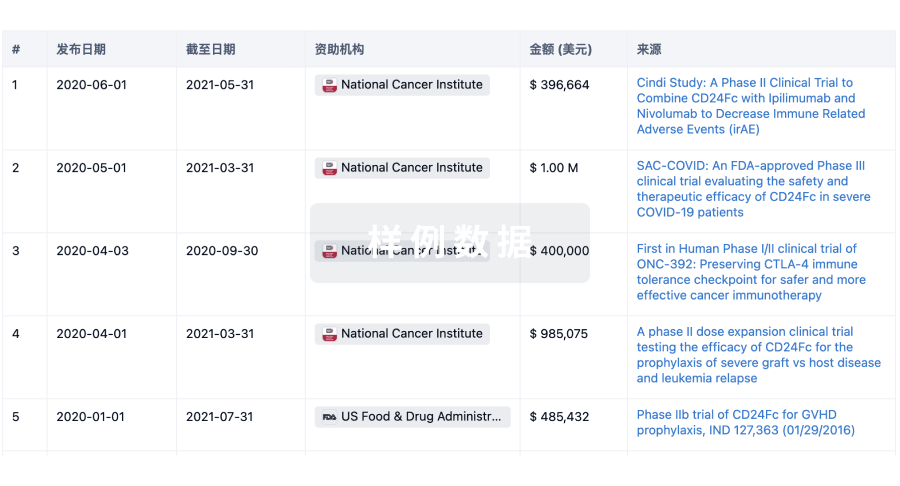
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
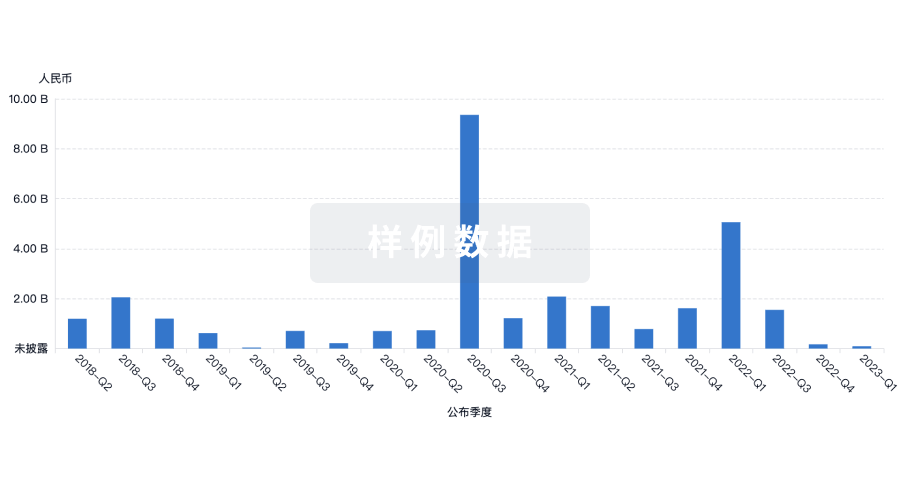
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
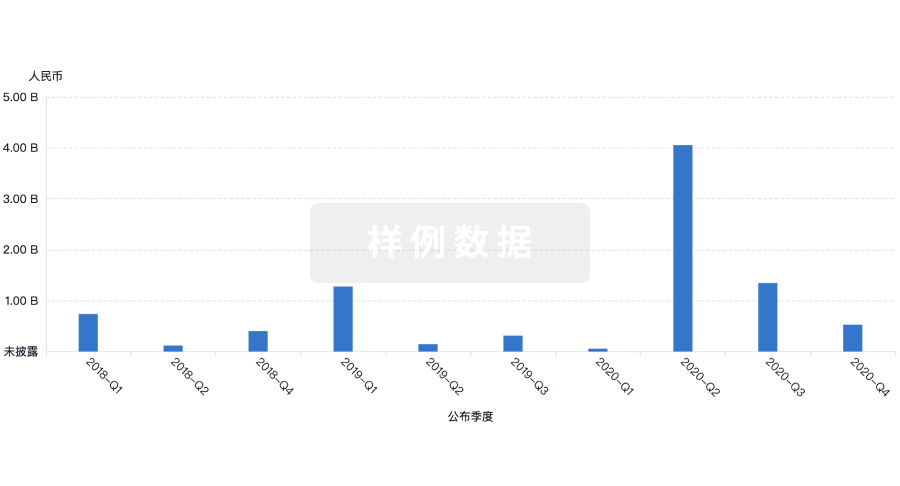
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用