预约演示
更新于:2026-02-26

Aetna, Inc.
更新于:2026-02-26
概览
关联
17
项与 Aetna, Inc. 相关的临床试验NCT03849144
The Effect of a Therapy Dog Activity on Employees' Stress, Mood, and Job Satisfaction and Commitment
The goal of the current study is to determine if participating in a therapy dog activity is associated with changes in perceived stress, mood, and job satisfaction and commitment. A secondary goal is to explore a potential dose effect of multiple treatments as well as control for novelty effect.
开始日期2019-03-15 |
申办/合作机构 |
NCT03259373
IMplementation of a Randomized Controlled Trial (RCT) to imProve Treatment With Oral AntiCoagulanTs in Patients With Atrial Fibrillation
The purpose of this study is to use a decentralized claims database to determine whether education on stroke prevention in atrial fibrillation (AF) among AF patients and their providers can result in increased use of oral anticoagulants (OAC) for stroke prevention among those AF patients with guideline-based indications for oral anticoagulation (CHA₂DS₂-VASc score of 2 or greater). Specifically, the investigators will conduct a prospective, randomized, open-label education intervention trial to evaluate the effect of the early patient and provider education interventions on the proportion of patients with evidence of at least one OAC prescription fill (defined as one OAC dispensing or 4 international normalized ratio [INR tests] over the course of the follow-up through the date on which at least 80% of eligible study participants have at least 12 months of follow-up time). A total of approximately 80,000 patients will be enrolled within multiple major health plans across the United States. The randomization will be performed by the central coordinating center, and the health plans will mail the educational intervention materials to their members and providers.
开始日期2017-09-25 |
申办/合作机构 |
NCT02788539
Reducing Disparities in the Treatment of Chronic Pain Using an Innovative mHealth Tool
This project will work to increase knowledge about the utility of a website for management of chronic pain, Our Whole Lives (OWL). It will do so by examining barriers and facilitators to patient use. In order to gather this information, the investigators will conduct a Science Cafe with 30 individuals (including participants with chronic pain, who have family members with chronic pain or are a stakeholder in the chronic pain community) to gather feedback about how to tailor the OWL website to their needs and preferences and how to improve ease of use for this tool. The investigators will also pilot two cohorts with 40 patients with chronic pain (2 groups of 20 patients) with OWL, the patient-centered, mobile health chronic pain management resource, measuring pain impact (pain severity, pain interference, physical function) and pain associated outcomes (e.g., depression, anxiety, fatigue, sleep disturbance, ability to participate in social roles and activities, pain self-efficacy, health education impact and internalized stigma related to chronic pain).
开始日期2016-06-01 |
申办/合作机构 |
100 项与 Aetna, Inc. 相关的临床结果
登录后查看更多信息
0 项与 Aetna, Inc. 相关的专利(医药)
登录后查看更多信息
1,189
项与 Aetna, Inc. 相关的文献(医药)2024-10-01·BJPsych Bulletin
Development of the Prevention of Suicide Behaviour in Prisons: Enhancing Access to Therapy (PROSPECT) logic model and implementation strategies
Article
作者: Pratt, Daniel ; Edge, Dawn ; Lennox, Charlotte ; Honeywell, David ; Awenat, Yvonne ; Knowles, Sarah ; Haddock, Gillian ; Brooks, Helen ; Gooding, Patricia ; Crook, Rebecca
Aims and method:
This study aimed to develop and articulate a logic model and programme theories for implementing a new cognitive–behavioural suicide prevention intervention for men in prison who are perceived to be at risk of death by suicide. Semi-structured one-to-one interviews with key stakeholders and a combination of qualitative analysis techniques were used to develop programme theories.
Results:
Interviews with 28 stakeholders resulted in five programme theories, focusing on: trust, willingness and engagement; readiness and ability; assessment and formulation; practitioner delivering the ‘change work’ stage of the intervention face-to-face in a prison environment; and practitioner training, integrating the intervention and onward care. Each theory provides details of what contextual factors need to be considered at each stage, and what activities can facilitate achieving the intended outcomes of the intervention, both intermediate and long term.
Clinical implications:
The PROSPECT implementation strategy developed from the five theories can be adapted to different situations and environments.
2024-07-01·European Journal of Obstetrics & Gynecology and Reproductive Biology
Surgical evacuation with intraoperative ultrasound (SEE U): A randomised controlled trial
Article
作者: Clark, T Justin ; Devall, Adam J ; Middleton, Lee ; Smith, Paul P ; Cheed, Versha ; Izzat, Feras
OBJECTIVES:
To test whether intraoperative ultrasound can reduce the incidence of early and late complications following surgical removal of products of conception.
DESIGN:
This was a prospective, multicentre, randomised, open clinical trial to assess feasibility. It was performed in two University Teaching hospitals in the West Midlands, England. The population consisted of women aged 16 years or over who were referred for surgical management of miscarriage. Patients were randomised to surgical management of miscarriage with either continuous intraoperative ultrasound or without intraoperative ultrasound. Process outcomes included the proportion of eligible women screened and proportion of eligible women randomised, attrition rates, evaluation of outcome measurement tools and acceptability. The primary clinical outcome was a composite outcome of unsuccessful procedure or a complication.
RESULTS:
Fifty-nine women requiring surgical management of miscarriage were randomised. The conversion rate for entry into the trial was 59/79(75 %; 95 %CI = 64-84 %). The composite clinical outcome was attained in 5/27(19 %) patients who had surgery without ultrasound and 7/28(25 %) patients who had surgery with ultrasound (RR = 0.74;95 %CI = 0.26, 2.10). When we excluded the patients that could not attend their hysteroscopy appointment, due to COVID-19 pandemic, 5/27(19 %) of patients who had surgery without ultrasound and 5/25(20 %) of patients who had surgery with ultrasound attained the composite clinical outcome (RR = 0.93;95 %CI = 0.30, 2.90).
CONCLUSIONS:
This multicentre pilot study showed that a large RCT comparing surgical management of miscarriage with and without intraoperative ultrasound is feasible.
2024-01-01·The European respiratory journal
Reply: Cognitive behavioural therapy sessions approach ineffective for anxiety and depression in COPD: is the door closed for good?
Letter
作者: White, Patrick ; Underwood, Martin ; Steed, Liz ; Marshall, Karen ; Pinnock, Hilary ; Sohanpal, Ratna ; Kelly, Moira J ; Taylor, Stephanie J C
Tweetable abstract
Our trial does not support using a CBA approach to alleviate mild/moderate anxiety and/or depression in people with moderate/severe COPD. New approaches are needed to relieve the substantial mental health burden in these patients with complex needs.https://bit.ly/3TkkDt3586
项与 Aetna, Inc. 相关的新闻(医药)2026-02-19
Second major national carrier partnership builds on Parallel Health's growing insurance footprint, lowering costs of precision care through microbiome science
We built this company on the belief that every patient deserves care tailored to their unique biology. Each new carrier partnership is a step toward making that vision a reality.”
— Dr. Nathan Brown, Chief Science Officer, Parallel Health
SAN FRANCISCO, CA, UNITED STATES, February 19, 2026 /
EINPresswire.com
/ --
Parallel Health
, the pioneering precision skin health company advancing the field of
Microbiome Dermatology™
, today announced that it has achieved in-network status with Cigna Healthcare in California. The agreement marks the second formal in-network partnership with a major national insurance carrier for Parallel Health, following its earlier agreement with Aetna in California, and further establishes the company as the only microbiome dermatology platform with multi-carrier insurance coverage in the United States.
"Every new in-network agreement brings us closer to our goal of making precision skin health the standard of care, not the exception," said Natalise Kalea Robinson, CEO and Co-Founder of Parallel Health. "We're proud to earn the trust of another leading national carrier through our commitment to clinical rigor, transparent practices, and real patient outcomes. With Cigna Healthcare and Aetna now in our network, we're building the insurance infrastructure that microbiome dermatology needs to reach the people who need it most."
Building Momentum in Precision Skin Health
Parallel Health's in-network agreement with Cigna Healthcare represents a significant expansion of the company's insurance footprint. Cigna Healthcare, a subsidiary of The Cigna Group (NYSE: CI), is one of the largest health benefits providers in the United States, with a broad network of physicians and facilities serving millions of members across California and nationwide. The agreement was reached through a formal credentialing process in which Cigna Healthcare evaluated Parallel Health's clinical protocols, provider qualifications, and operational standards.
Parallel Health believes it is the only microbiome dermatology platform in the United States to hold formal in-network agreements with multiple major national insurance carriers.With Cigna Healthcare and Aetna now in its network, Parallel Health continues to set the pace for an entirely new category of clinically grounded, insurance-covered skin health.
A New Approach to Skin Health
Dermatologists have an extraordinary depth of clinical expertise in diagnosing and treating skin conditions. Parallel Health's Microbiome Dermatology™ platform is designed to complement that expertise by adding a new layer of microbial insight — leveraging quantitative whole genome sequencing performed in a CLIA-certified laboratory, proprietary AI-driven skin microbiome analysis, and precision therapeutics including bacteriophage formulations and custom compounded prescriptions. By revealing the unique microbial ecosystem living on each patient's skin, the platform equips dermatologists with actionable data to deliver even more personalized care for conditions including acne, rosacea, eczema, hidradenitis suppurativa, body odor, and hair loss — with an expanding scope of clinical applications on the horizon.
Built on Science, Governed by Clinical Rigor
Parallel Health's approach to precision skin health is anchored in rigorous proprietary research, institutional-grade infrastructure, and physician-led clinical oversight. The company's proprietary biobank houses more than 10,000 characterized microbial strains—90% of which are novel to science—supported by 8 pending patents. Every personalized treatment protocol is developed and overseen by Parallel Health's in-house board-certified dermatology team, ensuring that patients receive care grounded in both cutting-edge microbiome science and established clinical dermatology standards.
Lowering the Cost of Precision Skin Health
For patients, in-network status means that dermatologist consultations, telehealth visits, and personalized treatment plans through Parallel Health are now more affordable and accessible. By lowering the overall cost of precision skin health, these insurance partnerships reduce the financial barrier that has historically kept microbiome-informed healthcare out of reach for many patients.
"Precision health should not be a luxury reserved for those who can pay entirely out of pocket," said Dr. Nathan Brown, Ph.D., Co-Founder and Chief Science Officer of Parallel Health. "Your skin microbiome is one of the most important and overlooked components of skin health, skin longevity, and overall wellness. We built this company on a foundation of scientific transparency, clinical accountability, and the belief that every patient deserves care tailored to their unique biology. Each new carrier partnership is a step toward making that vision a reality."
Scaling Precision Skin Health to the Masses
Parallel Health was founded with a mission to make precision health real and accessible to everyone. The company's telehealth platform combines advanced skin microbiome analysis with AI-powered insights and board-certified dermatologist expertise to deliver care that is personalized to each patient's unique microbial profile.
The Cigna Healthcare partnership announced today builds on the momentum established by Parallel Health's earlier agreement with Aetna and reflects growing insurer confidence in the clinical and economic value of microbiome dermatology. Earning in-network status requires meeting stringent credentialing, compliance, and quality standards—a process that validates not only Parallel Health's clinical model but the emerging category of precision skin health as a whole. The company plans to pursue additional in-network agreements with major insurers across California and nationally, with a long-term goal of making microbiome-informed dermatology an affordable, covered benefit for the majority of commercially insured Americans.
Patients interested in checking their insurance eligibility with Parallel Health can email insurance@parallelhealth.io.
Olivia Jensen
Parallel Health
+1 415-917-1660
email us here
Visit us on social media:
LinkedIn
Instagram
Facebook
YouTube
TikTok
X
Legal Disclaimer:
EIN Presswire provides this news content "as is" without warranty of any kind. We do not accept any responsibility or liability
for the accuracy, content, images, videos, licenses, completeness, legality, or reliability of the information contained in this
article. If you have any complaints or copyright issues related to this article, kindly contact the author above.

微生物疗法
2026-02-03
The Centers for Medicare and Medicaid Services has never played a significant role in regulating pharmacy benefit managers, the middlemen that have historically relied on high drug prices for profits. But the government spending package that’s nearing the finish line this week is poised to change that.
The sweeping, bipartisan reforms would begin to take effect in 2028 and are seen by many as a win for the pharma industry. The changes, which have been floated in various forms in Congress for at least three years, will redefine how PBMs can be compensated and make CMS the new standard-setter for how they operate.
The Senate passed the spending bill last week, and the House narrowly passed the bill on Tuesday, paving the way for President Donald Trump’s signature.
Under the bill, CMS would get about $190 million in funding to crack down on pharmacy benefit managers and ensure they’re complying with the new law. That includes ensuring PBMs can no longer receive revenue or compensation in any way tied to the cost of the drug.
The current system incentivizes PBMs to seek higher drug prices so they can pull in higher rebates. But under the spending bill, the drug middlemen would no longer be able to derive revenue from rebates they retain, whether in full or a percentage of them.
“You’re turning around the Titanic here,” Jesse Dresser, a partner in the law firm Frier Levitt’s life sciences department, told
Endpoints News.
Dresser helped Congress draft the PBM portions of the bill.
The bill also requires CMS to investigate and enforce any PBM complaints from pharmacies, making “a complete 180” from past practices on PBMs, Dresser said. He said CMS may have to hire new experts to help collect new data on PBMs and do research in order to be able to set appropriate standards.
Drug middlemen have long been under scrutiny for their allegedly deceptive practices, like overcharging insurers while underpaying pharmacies. How the bill plays out in reality will depend on how CMS cracks down on PBMs — and how they react.
For example, CVS Health owns the PBM Caremark as well as Aetna and SilverScript, which Dresser said are two of the nation’s largest Part D plan sponsors.
“So if CVS Caremark improperly retains money at a PBM level and has to disgorge it to the Part D level, it’s just kind of moving it from one pocket to the other. So there’s a big question mark as to what this is going to look like,” Dresser said.
A spokesperson for CVS Health said in a statement that “[i]n this spending bill, Pharma wins. To drugmakers’ credit, they’ve funded a decades’ long lobbying and advertising campaign to try to shift the blame for rising drug prices to anyone but them.”
Dresser also noted that PBMs “are very good at playing games,” adding that there is a concern that PBMs will “double down” on other components within the pharma supply chain or lobby CMS when it begins setting new standards for PBMs in ways that make them less effective.
PBMs, however, claim that this bill will increase the price of drugs across the board.
David Marin, president and CEO of the PBM industry group the Pharmaceutical Care Management Association, said in a statement following the Senate’s passage of the bill last week: “Congratulations to the big drugmakers, who have lobbied for years to enact these mandates. They will now have more power, and employers and patients will pay the consequences through higher drug prices. Americans already pay the highest prescription drug prices in the world, and under this bill, they will pay even more.”
2026-01-29
Reimbursements in healthcare have been at the top of leader’s minds for decades, creating a burdensome process for providers, patients, and manufacturers.
Physicians are more hesitant to use certain devices, or perform certain procedures, if they don’t believe they will be reimbursed at a fair rate.
Reimbursement debates often cause heated arguments between providers, insurance plans, and players in the same, much like recent
drama
surrounding CMS coverage for TAVR.
To overcome these decades old healthcare challenges, companies are trying to figure out how to better use the AI tools at their disposal to make payment systems easier, faster, and less cumbersome for patients, providers, and devicemakers.
MD+DI
connected with Roshan Patel, founder and CEO of healthcare technology firm Arrow, to discuss AI’s role in medical billing, predictive analytics for cash flow operations, and more.
Arrow, formerly known as Walnut, emerged from stealth in 2024 following its founding in 2020, offering payments solutions featuring advanced error detection, predictive analytics, denial management, and comprehensive visibility into revenue cycles to streamline claim processes, boost claim accuracy, and drive smarter decision-making and operational efficiency.
The company secured a $110 million Series A funding round in 2022, and is backed by major players in the space including Google, Plaid, Mercury, and Ramp.
How is AI transforming medical billing and payments specifically for medical device companies and their revenue cycles?
Patel:
AI is impacting every industry. Billing and revenue cycle is a knowledge and information type of work, and so we are starting to see AI take a lot of the tedious and repetitive manual processes in getting an insurance claim paid, which to go from a patient visit to money in the bank there is a large arduous process with tons of friction, and that is usually by design by insurance companies. They don't make it very easy to get paid as a healthcare provider. To even just ask the status of a claim, sometimes you can go and check the portal if they have one, but many times you have to call. Half the time, revenue cycle teams are just calling and that's a huge time suck in their day, just being stuck on hold for 30 minutes. Something like that is very easy for AI to take over, so billing teams can focus on what actually requires their judgment and knowledge, and not just be bogged down with so much easy, repetitive manual work.
How can predictive analytics help companies better forecast payment timelines and cash flow?
Patel:
There is a ton of data healthcare providers are sitting on that they are not utilizing because they are already so busy and underwater. If you can put payment and revenue cycle data into a business intelligence tool, you can start to see a lot of trends and forecast things out. EMRs aren't really built for financial forecasting, they're built for clinical work. A lot of people are trying to find those tools to project out, so they can project out, ‘when I submit this claim to Aetna, what is the probability I will get paid and how long will it take to happen?’ And then you can start to build your business around that.
What payment friction points do you see most commonly?
Patel:
The most common one is denied claims. There is a statistic that roughly 20% of all claims get denied, and a lot of times that is due to errors in billing early in the process, like wrong patient insurance, coding errors, things like that. A huge chunk of the time it's an error on the insurance company's side because they have denied something incorrectly. Once a claim is denied, it kicks off a huge process on the billing team side, since they have to figure out why it was denied, was it a mistake, and what needs to be done to fix the claim. Then you get a back and forth with the insurance company, so that's where we are seeing most of the time suck, but also the most high return on their time, because they are getting an unpaid claim turned into a paid claim.
What trends are you seeing in patient financial responsibility, and how is this impacting the industry?
Patel:
Patients want more transparency, especially into what things will cost and assurance of that cost upfront before getting care. That is hard to provide that information, because so many things downstream affect how much the patient will know. If a claim is denied, we cannot predict that with 100% certainty. You can have a good chance of knowing, but you’ll never know what an insurance company will do. Also, the core treatment for a patient can change, making it hard to know what services will be rendered, making it hard to estimate costs upfront when you don’t know what will happen in a specific treatment.
What payment and billing trends should executives be watching in 2026?
Patel:
Everyone is evaluating AI and how to best use it in their workflows. There is AI for almost everything in payment and billing- every slice of the revenue cycle. I think it’s about trying to find one where, right now, everyone is promising the world, but how do you know what will work? I think that is the biggest challenge for executives. People are now simply asking their peers what systems they are using, and what is working. That is how things are getting adopted nowadays.
100 项与 Aetna, Inc. 相关的药物交易
登录后查看更多信息
100 项与 Aetna, Inc. 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年03月21日管线快照
无数据报导
登录后保持更新
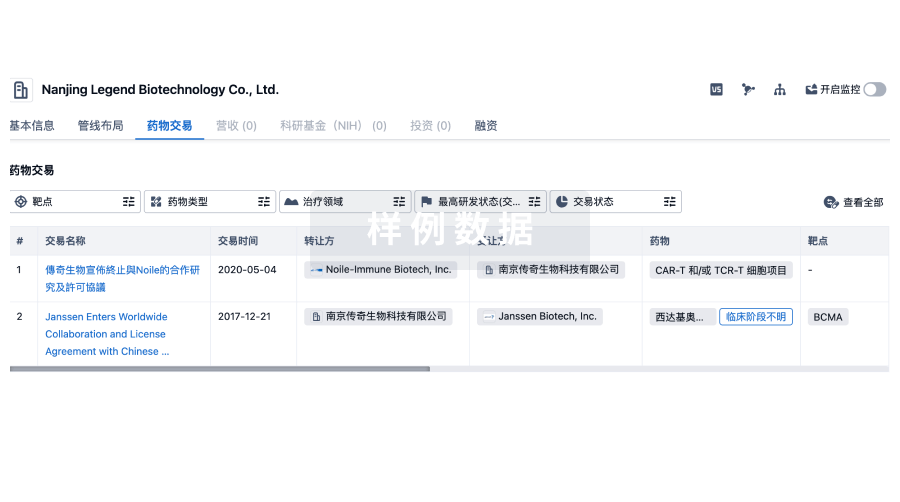
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
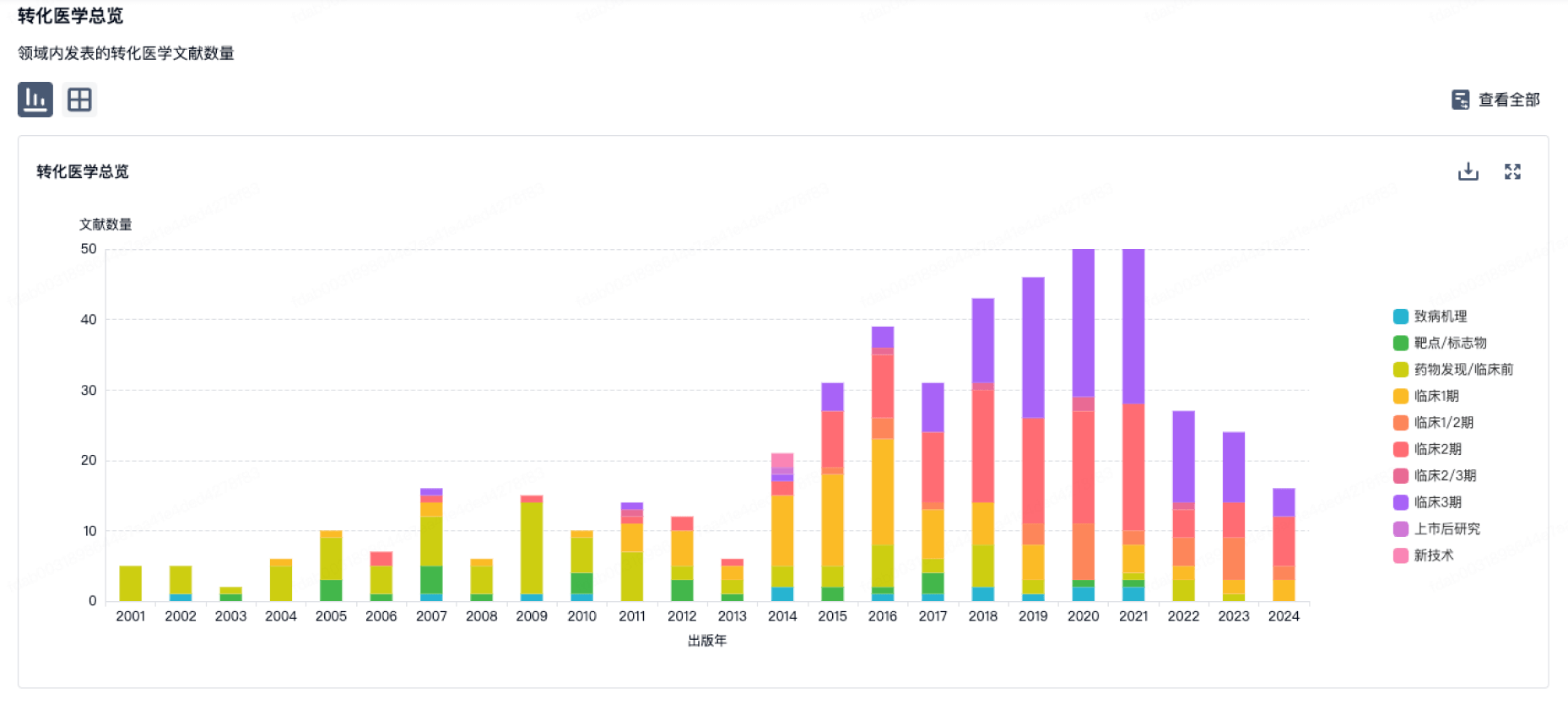
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
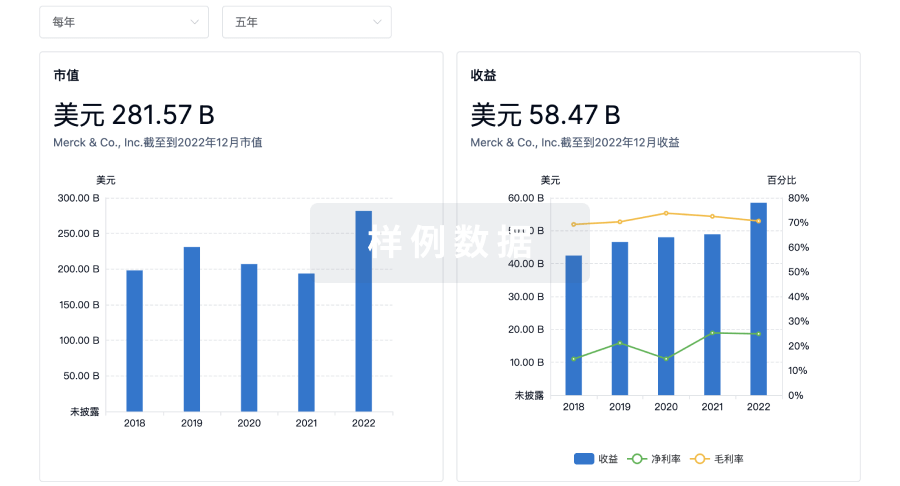
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
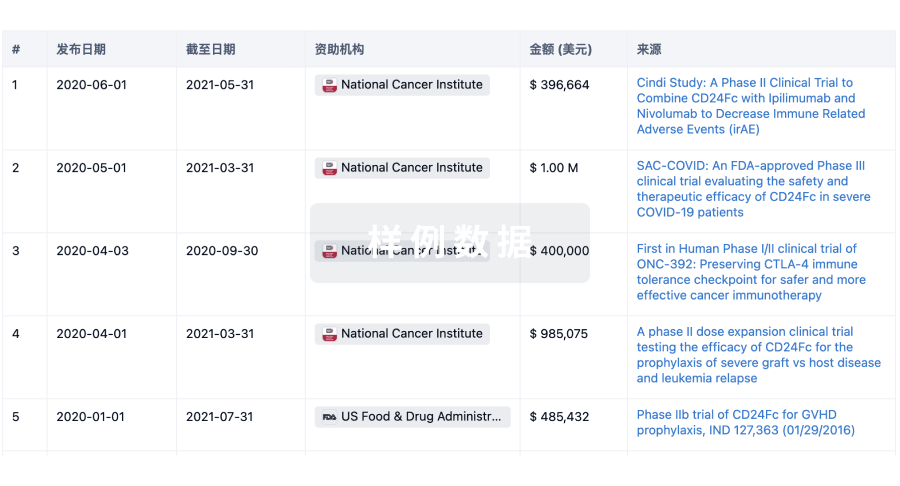
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
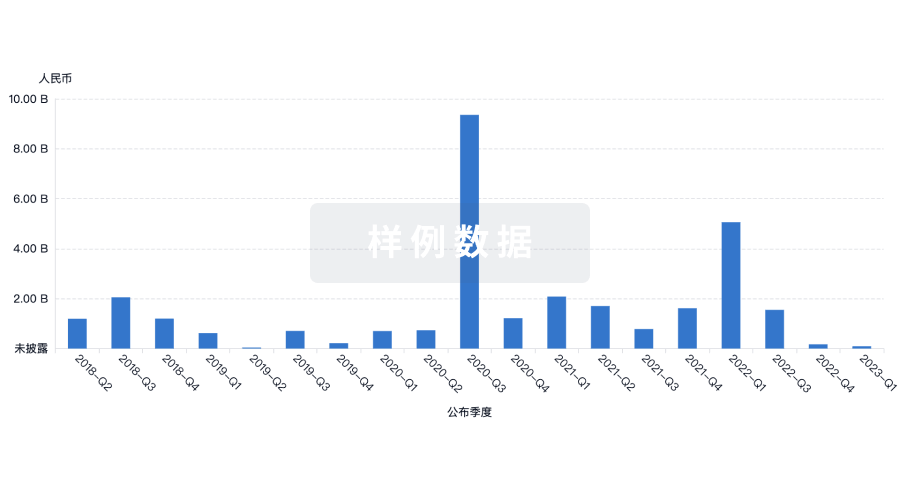
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
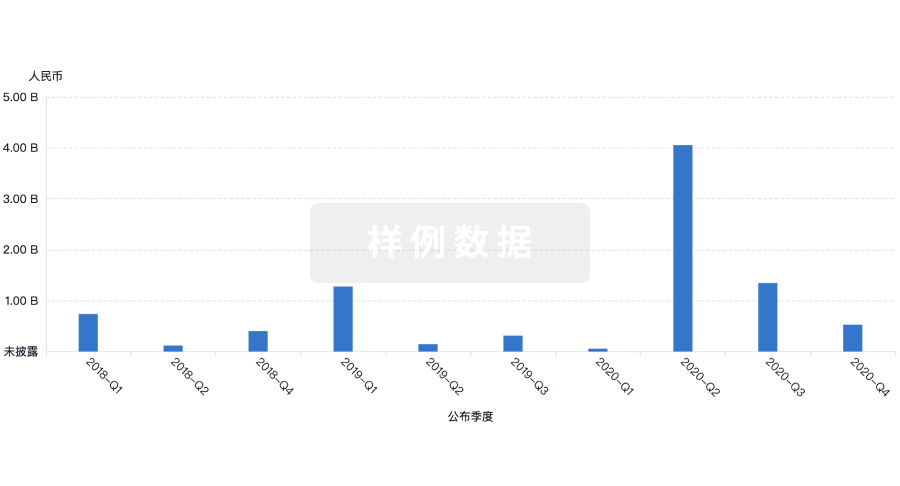
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用