预约演示
更新于:2025-05-07
Isophane Insulin
低精蛋白锌胰岛素
更新于:2025-05-07
概要
基本信息
原研机构 |
在研机构 |
非在研机构- |
权益机构- |
最高研发阶段批准上市 |
首次获批日期 中国 (1997-01-01), |
最高研发阶段(中国)批准上市 |
特殊审评- |
登录后查看时间轴
关联
1
项与 低精蛋白锌胰岛素 相关的临床试验NCT01854723
Basal Insulin Therapy in Patients With Insulin Resistance: A 6 Month Comparison of Insulin Glargine and NPH Insulin
This study will compare the safety, effectiveness, and cost of two different types of long-acting insulin.
开始日期2013-04-01 |
申办/合作机构 |
100 项与 低精蛋白锌胰岛素 相关的临床结果
登录后查看更多信息
100 项与 低精蛋白锌胰岛素 相关的转化医学
登录后查看更多信息
100 项与 低精蛋白锌胰岛素 相关的专利(医药)
登录后查看更多信息
106
项与 低精蛋白锌胰岛素 相关的文献(医药)2024-05-01·Therapeutic Innovation & Regulatory Science
A Cross-National Comparison of Biosimilars Pricing in Argentina, Australia, Brazil, and Italy
Article
作者: Albuquerque, Flavia Caixeta ; Cañás, Martín ; Lopes, Luciane Cruz ; Urtasun, Martín A ; Marín, Gustavo H ; Pont, Lisa ; Kirchmayer, Ursula ; Tuccori, Marco ; da Silva Machado, Fernanda Lacerda ; Bonaso, Marco ; Convertino, Irma
2024-03-01·Diabetic Medicine
A UK national survey of enteral feed use in people with diabetes 2022
Article
作者: Flanagan, Daniel ; Green, Mark ; Lake, Andrea K ; Roberts, Aled ; Dhatariya, Ketan
2023-11-01·The American Journal of Managed Care
Charitable Medication Distribution Improves Care for Uninsured Patients With Diabetes
Article
作者: Hughes, Jonathan ; McCormack, Tim ; Sparkman, Abby ; Blackburn, Hillary ; Smith, Priscilla ; Campbell, Tavajay
2
项与 低精蛋白锌胰岛素 相关的新闻(医药)2022-06-06
【2022年6月6日/医药资讯一览】云南白药任命前华为高管马加担任首席财务官;科兴制药与信立泰签署抗新冠病毒小分子药CDMO协议;BMS斥资超40亿美元囊获非小细胞肺癌突破性疗法……每日新鲜药闻医讯,速读社与您共同关注!
政策简报
北京朴石医学检验实验室有限公司7人被批准逮捕
6日,据“房山检察”微信公众号消息,近日,北京市公安局房山分局以北京朴石医学检验实验室有限公司周某某、武某某等7名犯罪嫌疑人涉嫌妨害传染病防治罪,提请北京市房山区人民检察院批准逮捕。检察机关经审查,于2022年6月6日,以涉嫌妨害传染病防治罪依法对周某某、武某某等7人作出批准逮捕决定。(房山检察)
海南省发布第六批集采(胰岛素专项)未中选品种调整挂网价格
6日,海南省公共资源交易服务中心发布关于国家集采第六批(胰岛素专项)未中选品种调整挂网价格的通知。经过梳理发现,本次预计有31批药品调价,涉及10家企业。已在海南省挂网的国家集采第六批(胰岛素专项)未中选品种:德谷门冬双胰岛素注射液、低精蛋白锌胰岛素注射液、甘精胰岛素注射液、精蛋白生物合成人胰岛素注射液(预混30R)、精蛋白重组人胰岛素注射液等。涉及企业:Novo Nordisk A/S、江苏万邦生化医药集团有限责任公司、通化东宝药业股份有限公司、酒泉大得利制药股份有限公司、LillyFrance等。(海南省公共资源交易服务中心)
产经观察
云南白药任命前华为高管马加担任首席财务官
日前,云南白药发布公告称,经公司首席执行官提名,董事会提名委员会审议通过,建议聘任马加担任公司首席财务官。在加入云南白药前,马加的职业生涯主要在科技巨头华为,做过中国区运营商BGCFO、中国区CFO等,负责中国区ICT经营管理、风控、税务以及财经组织建设等工作。(企业公告)
哈药股份董事黄荣凯辞职
6日晚间,哈药股份发布公告称,哈药集团股份有限公司董事会于近日收到公司董事黄荣凯递交的书面辞职报告。因个人原因,黄荣凯辞去公司董事、提名委员会委员职务,辞职后不在公司担任其他任何职务。根据《公司法》、《公司章程》等有关规定,其递交的辞职报告自送达董事会之日起生效。(企业公告)
复星医药受让ONCOCARE MEDICAL PTE. LTD. 60%股权
6日晚间,复星医药发布公告称,公司控股子公司Fosun Pharma Pte.与Solid Success(即“卖方一”)及其控股股东 Aurora Healthcare 签订《Solid Success 股权转让协议》,Fosun Pharma Pte.拟现金出资不超过18,502.1万新币受让卖方一持有的 OncoCare51%的股权,卖方一之控股股东 Aurora Healthcare 担保 Solid Success 在协议项下各项义务的履行。同日,Fosun Pharma Pte.与 SMS 及 3 名持股医生(即“卖方二”)签订《其他股东股权转让协议》,Fosun Pharma Pte.拟合计现金出资不超过 3,265.1万新币受让卖方二持有的 OncoCare 9%的股权。(企业公告)
南京医药控股子公司辽宁南药民生康大医药有限公司终结破产程序
6日,南京医药发布公告称,公司控股子公司辽宁南药民生康大医药有限公司近日收到辽宁省沈阳市铁西区人民法院《民事裁定书》,法院认为,辽宁南药无财产可供分配,裁定终结辽宁南药破产程序。(企业公告)
康希诺与辉瑞终止MCV4疫苗产品推广合作
6日,康希诺生物发布公告称,经友好协商,该公司与辉瑞(PFE.US)于2022年6月4日签署了《推广服务协议之终止协议》,约定合作协议自终止协议签署之日起终止。据公告显示,2020年7月,康希诺生物与辉瑞签署了合作协议,约定公司授权辉瑞在合作协议签署之日起至MCV4获得药品注册证书之日起最长10年的合作期限内在中国大陆地区独家推广公司MCV4疫苗产品曼海欣®,授权辉瑞有权在合作期限内为推广MCV4疫苗产品而在授权区域内使用公司商标和技术信息。(企业公告)
科兴制药与信立泰签署抗新冠病毒小分子药CDMO协议
5日,科兴制药公告披露,为加快推进公司用于治疗新冠及其他病毒感染的抗病毒药物SHEN26项目,公司全资子公司深圳科兴药业有限公司与深圳信立泰药业股份有限公司及其子公司惠州信立泰签署CDMO技术服务及委托生产协议。根据协议,深圳科兴委托信立泰及惠州信立泰开展SHEN26项目药品CDMO技术服务(包括但不限于药品注册阶段的技术转移、临床样品生产等)及原料药、制剂的委托加工。协议总金额人民币888.26万元,由深圳科兴按协议进展分七期支付。(企业公告)
药明康德:预计第二季度收入仍将实现63%至65%的增长
5日晚间,药明康德发布公告称,公司目前在上海地区的生产经营活动已基本恢复正常。公司预计2022年第二季度收入仍将实现此前公告的63%-65%的增长,公司继续对2022年全年实现收入增长65%-70%的目标充满信心。(企业公告)
BMS斥资超40亿美元囊获非小细胞肺癌突破性疗法
近日,BMS和Turning Point Therapeutics联合宣布,双方已达成协议,百时美施贵宝将斥资超过40亿美元,收购Turning Point Therapeutics。Turning Point致力于开发靶向癌症相关常见突变的精准疗法。该公司的主打在研疗法repotrectinib是一款潜在“best-in-class”下一代酪氨酸激酶抑制剂(TKI),靶向驱动非小细胞肺癌(NSCLC)和其它晚期实体瘤的ROS1和NTRK基因变异。这款精准疗法已经获得美国FDA授予的三项突破性疗法认定,用于治疗携带NTRK基因融合的晚期实体瘤患者,以及ROS1阳性的不同转移性NSCLC患者群体。(药明康德)
再生元向赛诺菲购买抗癌药 交易金额高达11亿美元
近日,再生元同意向合作伙伴赛诺菲购买免疫肿瘤药物Libtayo(西米普利单抗),交易金额达11亿美元。根据协议,赛诺菲将把Libtayo的全部权利(包括在全球范围内进行开发、商业化和制造的权利)转让予再生元,再生元获得Libtayo的全球独家许可权。而赛诺菲将就此获前期付款9亿美元,然后待药物达致若干监管和销售目标后收取里程碑付款2亿美元。此外,赛诺菲将就Libtayo的全球销售净利润收取11%的特许使用权费用。(新浪医药新闻)
三叶草生物全面进军新冠业务 获最高3亿美元授信
5日,三叶草生物发布业务最新资料,资料显示,为支持产品商业化上市期间潜在的营运资金需求,招商银行已批准为期一年的最高可达3亿美元的授信协议。该协议的提款取决於招商银行对公司业务进展的评估,公司业务状况的变化可能会导致提前还款。还款日期和利率等附加条款将於提款获得批准时确定。(企业公告)
药闻医讯
外用维生素A衍生物获FDA突破性疗法认定
近日,Timber Pharmaceuticals公司宣布,美国FDA已授予其在研局部外用异维A酸药物TMB-001突破性疗法认定,用于治疗先天性鱼鳞病(CI)。TMB-001是一种通过Timber Pharmaceuticals公司专有递送系统开发的局部外用异维A酸药物,用于治疗中度至重度CI。异维A酸是一种维生素A的衍生物。(药明康德)
浙江医药喹诺酮类抗菌药物盐酸环丙沙星片获MHRA上市许可
6日晚间,浙江医药发布公告称,于近日收到英国药品和健康产品管理局(MHRA)核准签发的盐酸环丙沙星片 250mg、500mg 两个规格的上市许可。盐酸环丙沙星为第三代喹诺酮类抗菌药物,适用于治疗成年人革兰氏阴性菌引起的下呼吸道感染、囊性纤维化或支气管扩张中的支气管肺部感染、肺炎、慢性 化脓性中耳炎、尿路感染、复杂的尿路感染等。(企业公告)
恒瑞医药创新药吡咯替尼用于乳腺癌新辅助治疗获批
近日,恒瑞医药收到国家药监局核准签发的《药品注册证书》,批准公司自主研发的1类新药马来酸吡咯替尼片(商品名:艾瑞妮®)与曲妥珠单抗和多西他赛联合,用于表皮生长因子受体2(HER2)阳性早期或局部晚期乳腺癌患者的新辅助治疗。(新浪医药新闻)
诺泰生物磷酸奥司他韦胶囊获《药品注册证书》
6日,诺泰生物发布公告称,于近日收到国家药监局核准签发的磷酸奥司他韦胶囊的《药品注册证书》(证书编号:2022S00486)。磷酸奥司他韦胶囊为一款抗流感病毒药物,主要用于成人和1岁及1岁以上儿童的甲型和乙型流感治疗,以及用于成人和13 岁及13岁以上青少年的甲型和 乙型流感的预防。(企业公告)
BMS泊马度胺在中国申报上市
CDE官网最新公示,BMS已递交5.1类新药泊马度胺胶囊的上市申请,并获得受理。公开资料显示,泊马度胺是BMS公司旗下新基开发的一种免疫调节剂类药物,此前已在海外获批用于多发性骨髓瘤和卡波西肉瘤。(CDE)
君实生物JS116胶囊获得药物临床试验批准通知书
6日,君实生物发布公告称,于近日收到国家药监局核准签发的《药物临床试验批准通知书》,JS116胶囊的临床试验申请获得批准。S116为具有全新结构的KRASG12C小分子不可逆共价抑制剂,用于治疗KRASG12C突变的非小细胞肺癌患者。(企业公告)
和誉生物泛FGFR抑制剂与替雷利珠单抗联合治疗UC二期临床获批
今日,和誉生物发布公告,该公司在研的泛FGFR抑制剂ABSK091与百济神州百济神州 )的抗PD-1抗体替雷利珠单抗的联合用药在尿路上皮癌(UC)中的II期研究获得中国国家药品监督管理局的临床试验批准。(企业公告)
驯鹿生物/信达生物伊基仑赛注射液新药上市申请获NMPA正式受理
2日,驯鹿生物与信达生物共同宣布NMPA正式受理由双方合作开发的伊基仑赛注射液治疗复发/难治性多发性骨髓瘤的上市许可申请。伊基仑赛注射液是国内第一款全流程自主研发的CAR-T细胞治疗产品,该产品已于2021年2月获得CDE授予"突破性治疗药物"认定。(新浪医药新闻)
阿斯利康/第一三共Enhertu最新临床研究结果发布
今日,阿斯利康和第一三共在ASCO年会的全体大会上,汇报了重磅抗体偶联药物(ADC)Enhertu,在治疗HER2低表达的不可切除或转移性乳腺癌患者的3期临床试验结果。结果显示,Enhertu与化疗相比,在HER2低表达患者群体中将疾病进展或死亡风险降低50%!(药明康德)
杨森BTK抑制剂治疗65岁以上新确诊套细胞淋巴瘤患者展现长期疗效
近日,强生集团旗下杨森公司宣布,布鲁顿氏酪氨酸激酶(BTK)抑制剂Imbruvica(ibrutinib),加入到bendamustine-rituximab(BR)和rituximab构成的维持治疗中,将65岁以上的新确诊套细胞淋巴瘤(MCL)患者的疾病进展或死亡风险降低25%。在中位随访时间为84.7个月时,Imbruvica组合疗法组的中位无进展生存期为6.7年,比对照组(4.4年)延长2.3年,具有临床意义。(药明康德)
诺诚健华公布BTK抑制剂治疗系统性红斑狼疮最新数据
6日,诺诚健华宣布,在刚刚结束的2022年欧洲风湿病学大会(EULAR)上,研究人员报告了布鲁顿酪氨酸激酶(BTK)抑制剂奥布替尼治疗系统性红斑狼疮(SLE)的最新临床研究数据。结果显示,在所有可评估的患者中,口服奥布替尼50毫克、80毫克和100毫克治疗的患者在第12周SLE反应指数-4(SRI-4)的应答率分别为50.0%(7/14)、61.5%(8/13)和64.3%(9/14),而服用安慰剂的患者SRI-4应答率为35.7%(5/14),这表明疗效呈剂量依赖性的改善趋势。(新浪医药新闻)
辉瑞公布BCMA-CD3双特异性抗体elranatamab 2期注册研究首批数据
近日,辉瑞在ASCO年会上公布了BCMA-CD3双特异性抗体elranatamab治疗复发/难治性多发性骨髓瘤(RRMM)2期MagnetisMM-3研究的中期分析数据。中位随访3.71个月,初步疗效结果显示,elranatamab治疗的客观缓解率为60.6%。截至数据截止,89.5%的客观缓解者仍处于缓解状态,无确认的疾病进展或死亡。(新浪医药新闻)
安进RNAi疗法2期临床结果积极 降低心血管疾病重要风险因子水平90%以上
近日,安进公布了其RNAi疗法olpasiran(曾用名:AMG 890)在2期临床试验中获得的积极顶线数据。试验结果表明olpasiran可显著降低脂蛋白(a)——Lp(a)水平。试验数据表明,在第36周(主要终点)和第48周(治疗期结束)时,大多数治疗剂量患者组的Lp(a)水平与基线相比,降低达到或超过了90%。在治疗期间未发现新的安全问题。(药明康德)
Zuranolone治疗产后抑郁症达关键3期主要终点
近日,Sage Therapeutics和渤健共同宣布,Zuranolone治疗产后抑郁症的3期SKYLARK研究达到了主要终点和所有关键次要终点。根据17项汉密尔顿抑郁量表(HAMD-17)总分较基线的变化,与安慰剂组(n=97)相比,接受zuranolone治疗的女性(n=98)在第15天(主要终点)的抑郁症状具有统计学意义和临床意义的改善。(药明康德)
荣昌生物维迪西妥单抗治疗尿路上皮癌最新数据公布
近日,荣昌生物维迪西妥单抗(Disitamab Vedotin, DV) 治疗尿路上皮癌最新数据亮相ASCO 2022年会,数据显示:RC48-ADC (DV)联合toripalimab在mUC患者中显示出良好的疗效。在mUC患者中,cORR为71.8%。随着HER2或PD-L1的表达增加,ORR值升高。
AXS-05治疗重度抑郁症3期临床结果发表
近日,Axsome Therapeutics宣布,其在研疗法AXS-05(右美沙芬+安非他酮)治疗重度抑郁症的关键3期临床试验结果在The Journal of Clinical Psychiatry上发表。临床试验结果显示,与安慰剂相比,AXS-05在抑郁症状和诱导缓解方面表现出快速、实质性和统计学意义上显著的改善。AXS-05组第6周时MDRS评分变化显著大于安慰剂。而且在接受治疗第1周和之后的每个评估时间点,AXS-05组的MADRS评分变化均显著大于安慰剂组。(药明康德)
再鼎医药肿瘤电场组合疗法达到2期临床主要终点
日前,再鼎医药与Novocure公司共同宣布,评估肿瘤电场治疗(TTFields)联合标准治疗(化疗单药或联合曲妥珠单抗用于治疗HER2阳性患者),一线治疗胃腺癌的2期临床研究EF-31达到客观缓解率的主要研究终点。接受组合疗法治疗的患者确认客观缓解率为50%。(药明康德)
加科思药业首次公布KRAS抑制剂1期临床数据
6日,加科思药业宣布,其自主研发的KRAS G12C抑制剂JAB-21822治疗非小细胞肺癌的1期临床数据已经在2022年美国临床肿瘤学会(ASCO)首次公布。数据显示,JAB-21822在每日400毫克及每日800毫克的剂量组中,使患者疾病控制率达到100%(12/12)。(新浪医药新闻)
合作疫苗免疫疗法抗体小分子药物
2022-06-06
6月6日,海南省公共资源交易服务中心发布关于国家集采第六批(胰岛素专项)未中选品种调整挂网价格的通知。通知中显示,已在海南省挂网的国家集采第六批(胰岛素专项)未中选品种,请于2022年6月9日前进行调价,并提交全国最低价承诺函。若逾期未调整为全国最低价的,将暂停交易。
经过梳理发现,本次预计有31批药品调价,涉及10家企业。已在海南省挂网的国家集采第六批(胰岛素专项)未中选品种:德谷门冬双胰岛素注射液、低精蛋白锌胰岛素注射液、甘精胰岛素注射液、精蛋白生物合成人胰岛素注射液(预混30R)、精蛋白重组人胰岛素注射液等。涉及企业:Novo Nordisk A/S、江苏万邦生化医药集团有限责任公司、通化东宝药业股份有限公司、酒泉大得利制药股份有限公司、LillyFrance等。
100 项与 低精蛋白锌胰岛素 相关的药物交易
登录后查看更多信息
研发状态
10 条最早获批的记录, 后查看更多信息
登录
| 适应症 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|
| 糖尿病 | 中国 | 1997-01-01 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
No Data | |||||||
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或

药物交易
使用我们的药物交易数据加速您的研究。
登录
或

核心专利
使用我们的核心专利数据促进您的研究。
登录
或

临床分析
紧跟全球注册中心的最新临床试验。
登录
或

批准
利用最新的监管批准信息加速您的研究。
登录
或

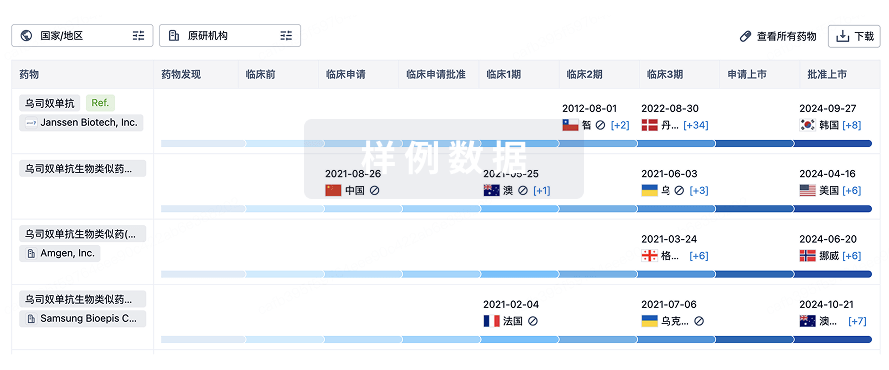
生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
特殊审评
只需点击几下即可了解关键药物信息。
登录
或

生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用

