预约演示
更新于:2026-04-02
Omalizumab-igec
奥马珠单抗生物类似药 (Celltrion)
更新于:2026-04-02
概要
基本信息
原研机构 |
非在研机构- |
权益机构- |
最高研发阶段批准上市 |
最高研发阶段(中国)- |
特殊审评- |
登录后查看时间轴
结构/序列
Sequence Code 81670L

当前序列信息引自: *****
Sequence Code 143601H

当前序列信息引自: *****
关联
3
项与 奥马珠单抗生物类似药 (Celltrion) 相关的临床试验NCT07425639
ROLL'YN-OMA : Etude Observationnelle de Cohorte Pour la Prise en Charge Des Patients Atteints de Pathologies Inflammatoires Chroniques traités Par Omlyclo®, un Omalizumab Biosimilaire
ROLL'YN-OMA is a real-world study in patients receiving standard biologic therapies who have been in control and/or remission of their disease for at least 3 months and whose physician has independently decided, within the framework of a shared medical decision, to switch them to OMLYCLO®. The primary objective of this study is to evaluate the maintenance of this control and/or clinical remission 12 months after initiation of the biosimilar, and subsequently, patient satisfaction at 6 and 12 months.
开始日期2025-10-02 |
NCT04426890
A Double-blind, Randomized, Active-controlled, Parallel Group, Phase 3 Study to Compare Efficacy and Safety of CT-P39 and Xolair in Patients With Chronic Spontaneous Urticaria Who Remain Symptomatic Despite H1 Antihistamine Treatment
A Double-blind, Randomized, Active-controlled, Parallel Group, Phase 3 Study to Compare Efficacy and Safety of CT-P39 and Xolair in Patients with Chronic Spontaneous Urticaria Who Remain Symptomatic despite H1 antihistamine Treatment
开始日期2020-12-09 |
申办/合作机构 |
NCT04018313
A Phase 1, Randomized, Double-blind, Three-arm, Parallel Group, Single-dose Study to Compare the Pharmacokinetics and Safety of Three Formulations of Omalizumab (CT-P39, EU-approved Xolair, and US-licensed Xolair) in Healthy Subjects
A Phase 1, Randomized, Double-blind, Three-arm, Parallel Group, Single-dose Study to Compare the Pharmacokinetics and Safety of Three Formulations of Omalizumab (CT-P39, EU-approved Xolair, and US-licensed Xolair) in Healthy Subjects
开始日期2020-05-28 |
申办/合作机构 |
100 项与 奥马珠单抗生物类似药 (Celltrion) 相关的临床结果
登录后查看更多信息
100 项与 奥马珠单抗生物类似药 (Celltrion) 相关的转化医学
登录后查看更多信息
100 项与 奥马珠单抗生物类似药 (Celltrion) 相关的专利(医药)
登录后查看更多信息
7
项与 奥马珠单抗生物类似药 (Celltrion) 相关的文献(医药)2026-03-01·ANNALS OF ALLERGY ASTHMA & IMMUNOLOGY
Emerging IgE and non-IgE targeted therapies for chronic urticaria
Review
作者: Chhiba, Krishan D ; Saini, Sarbjit S
Chronic urticaria affects a significant percent of the global population and carries a higher burden of unmet medical need. Current standard-of-care includes antihistamines and omalizumab, but omalizumab is not effective in all patients and has not been found to induce long-term disease remission. This review evaluates the diverse therapeutic pipeline spanning IgE-based and non-IgE-based mast cell targeting strategies, including recent clinical data. The therapeutic landscape has expanded rapidly with multiple mechanisms under investigation. IgE-targeted approaches include omalizumab biosimilars, with CT-P39 having received Food and Drug Administration (FDA) approval. Dupilumab received FDA approval for antihistamine-refractory chronic spontaneous urticaria supporting the targeting of type 2 cytokines, interleukin-4, and interleukin-13, in this disease. Bruton's tyrosine kinase inhibitors have promise, with remibrutinib receiving FDA approval and demonstrating significant reductions in UAS7 in phase 3 trials. c-Kit (c-Kit or KIT) inhibition with barzolvolimab demonstrates robust efficacy with sustained effects post-treatment. Finally, Janus kinase inhibitors, Mas-related G protein-coupled receptor X2 antagonists, and other novel mechanisms are advancing through clinical trials. Although some programs have been discontinued due to safety concerns or lack of efficacy such as fenebrutinib (Bruton's tyrosine kinase inhibitor), THB001 (c-Kit inhibitor), EP262 (Mas-related G protein-coupled receptor X2 antagonist), tezepelumab (anti-TSLP), and lirentelimab and AK006 (sialic acid binding immunoglobulin-like lectin-targeting agents), these studies have informed many of the other positive studies. In summary, in the last year, we have seen the chronic urticaria pipeline mature with multiple phase 3 programs and new approvals representing diverse mechanisms of action. Nevertheless, significant therapeutic gaps persist for omalizumab-refractory disease and chronic-inducible urticaria.
2026-02-01·Journal of Allergy and Clinical Immunology-In Practice
Systemic Treatments for Chronic Spontaneous Urticaria: Anti-IgE and Beyond
Review
作者: Saini, Sarbjit S ; Bernstein, Jonathan A ; Hsu, Florence Ida ; Chhiba, Krishan D
Chronic urticaria, which is divided into chronic spontaneous urticaria (CSU) and chronic inducible urticaria (CIndU), affects a significant percentage of the global population and carries a high burden of unmet medical need. Current standard of care includes nonsedating H1-antihistamines and omalizumab, which targets peripheral blood IgE and downregulates mast cell and basophil IgE receptors. However, omalizumab provides complete hive resolution in approximately 45% of patients and does not produce lasting remission. This review examines the clinical data for newly approved and emerging systemic therapies spanning IgE-based and non-IgE-based targeting strategies. The therapeutic landscape has expanded rapidly, and multiple mechanisms are under investigation. IgE-targeted approaches include omalizumab biosimilars, with CT-P39 having received Food and Drug Administration (FDA) approval. Dupilumab received FDA approval for H1-antihistamine-refractory CSU, supporting targeting type 2 cytokines, IL-4 and IL-13. Most recently, a Bruton's tyrosine kinase inhibitor (BTKi), remibrutinib, demonstrated significant reductions in Urticaria Activity Score over 7 days in phase 3 trials, leading to FDA approval. Newer c-Kit (cKit or KIT) inhibitors have also shown efficacy in CSU and CIndU, with barzolvolimab showing sustained efficacy post-treatment. Finally, other BTKi, Janus kinase (JAK) inhibitors, tyrosine kinase 2/JAK inhibitors, MRGPRX2 antagonists, and other novel mechanisms are advancing through clinical trials. Some drugs have been halted in development because of safety concerns, such as fenebrutinib (BTKi), THB001 (Larvol; c-Kit inhibitor), and EP262 (MRGPRX2 antagonist), whereas others, targeting the alarmin thymic stromal lymphopoietin (tezepelumab), the Th2 cytokine IL-5 (mepolizumab) and its receptor IL-5R (benralizumab), as well as lirentelimab (sialic acid-binding immunoglobulin-like lectin 8 [Siglec-8]) and AK006 (Siglec-6), were halted because of lack of efficacy. However, these failed trials have provided informed insights into the relevant pathways for CSU pathogenesis and treatment. In summary, systemic therapies for CSU are maturing with multiple phase 3 programs targeting the IgE pathway and Th2 cytokines leading to recent approvals. This review will provide an overview of these recently completed and ongoing clinical studies investigating emerging IgE and non-IgE therapeutic options for CSU.
2026-01-01·Clinical Drug Investigation
CT-P39: An Omalizumab Biosimilar
Review
作者: Brown, Michael B
CT-P39 [Omlyclo® (omalizumab-igec)] is a biosimilar of the reference monoclonal anti-immunoglobulin E (IgE) antibody omalizumab. It is approved for use in all indications for which reference omalizumab is approved, including allergic asthma, chronic rhinosinusitis with nasal polyps, chronic spontaneous urticaria (CSU) and (in the USA) IgE-mediated food allergy. CT-P39 has similar physicochemical and pharmacodynamic properties to those of reference omalizumab, and the pharmacokinetic equivalence and comparability of the agents has been demonstrated in healthy volunteers and patients with CSU, respectively. CT-P39 demonstrated clinical efficacy equivalent to that of reference omalizumab in patients with CSU and was generally well tolerated in this population. The tolerability, safety and immunogenicity profiles of CT-P39 were similar to those of reference omalizumab, and switching from reference omalizumab to CT-P39 appeared to have no impact on efficacy or safety. The role of reference omalizumab in the management of allergic asthma, chronic rhinosinusitis with nasal polyps, CSU and IgE-mediated food allergy is well established and CT-P39 provides an effective alternative for patients requiring omalizumab therapy.
59
项与 奥马珠单抗生物类似药 (Celltrion) 相关的新闻(医药)2026-03-24
点击蓝字 关注“拓麦Derm”
Scott Elman 博士
肖像经Scott Elman 博士许可后使用
◆ University of Miami Miller School of Medicine, Miami, USA
Scott Elman博士是美国迈阿密大学菲利普・弗罗斯特皮肤病学与皮肤外科系临床皮肤病学与皮肤外科助理教授,同时担任迈阿密大学医院及诊所住院皮肤科服务主任、杰克逊纪念医院门诊皮肤病科医疗主任及结缔组织病诊所主任,其研究关注复杂医学皮肤病学、风湿性皮肤病学和住院皮肤病学领域。
关键信息
◆ 慢性荨麻疹(CU)是一种由肥大细胞介导的疾病,其特征是反复发作的风团、血管性水肿,或两者并存,持续时间超过6周;及时、适当的治疗对于实现疾病的完全控制、最大程度减轻疾病负担和提高生活质量至关重要
◆ CU的治疗方式多样,皮肤科医生采用阶梯式治疗方案,首选现代抗组胺药,必要时改为生物制剂/小分子药物和(或)免疫抑制剂
◆ 本综述为继续医学教育系列的第二部分,重点介绍CU的综合管理,包括抗组胺药、免疫抑制剂和生物制剂的应用以及新兴治疗方法;CU的治疗前景不断发展,对生物制剂、小分子和特异性肥大细胞靶向药物的研究仍在进行中
主要内容
治疗目标
◆ 根据国际指南,荨麻疹的治疗目标是完全控制风团和血管性水肿;CU管理的主要目标是及时、持续地控制症状,以最低必要剂量进行安全、有效的治疗,以消除风团、瘙痒和血管性水肿
治疗结局
◆ 疾病的自然病程:CU病程可持续数年,30%-55%的成人患者在5年内自发缓解;CSU病程通常为1-2年,而CIndU可持续2-12年;鉴于病程的可变性和自发缓解的可能性,应每3-6个月重新评估持续或替代药物治疗方案
◆ 疾病修饰:针对CU发病机制的疾病修饰治疗仍存在显著的未被满足的需求;理想的治疗药物可实现降阶梯治疗、诱导持续缓解,或在停药后实现疾病治愈;还可延缓或阻止疾病进展、自身抗体产生和可能的并发症的发展
基于患者报告结局指标的评估
◆ 荨麻疹的活动度和控制:荨麻疹活动度评分(UAS)是评估CSU疾病活动度的金标准,也是多数临床试验的主要终点;荨麻疹疾病控制评分(UCT)和CU患者生活质量问卷(CU-2QoL)可进一步评估CU对患者的影响
◆ 血管性水肿的活动度和控制:血管性水肿活动度评分(AAS)、血管性水肿患者生活质量问卷(AE-QoL)和血管性水肿控制测试可用于评估血管性水肿的疾病负担
CU的现有治疗方案
◆ 近年来,荨麻疹的管理取得了显著进展,至少三分之二的患者可实现有临床意义的疾病控制;对疾病机制的理解明确了靶向治疗的关键作用(图1)
◆ 公认的CU治疗方案为(表1,图2):一线治疗选用第二代抗组胺药(sgAH),剂量可从批准剂量增至4倍(超说明书使用);二线治疗为奥马珠单抗、度普利尤单抗和remibrutinib;三线治疗为环孢素;该治疗方案同样适用于CIndU,但多为超说明书使用
◆ 超说明书使用高剂量sgAH(最高可达推荐日剂量的4倍)安全且有效,常用药包括西替利嗪、氯雷他定、比拉斯汀、地氯雷他定、依巴斯汀、非索非那定、左西替利嗪和卢帕他定
◆ 奥马珠单抗是首个获美国食品药品监督管理局(FDA)批准用于治疗CSU的生物制剂;对许多CIndU亚型也有益处;2025年3月,奥马珠单抗生物类似药CT-P39(奥马珠单抗-igec)获FDA批准,其适应症与奥马珠单抗一致,安全性和疗效相当
◆ 2025年4月,度普利尤单抗获FDA批准用于治疗CSU,该药为抑制IL-4的单克隆抗体,可阻止促炎因子IL-4和IL-13结合并抑制下游促炎信号通路,通过神经信号传导强效控制瘙痒,减少2型炎症和瘙痒
◆ 2025年10月,高选择性口服布鲁顿酪氨酸激酶(BTK)抑制剂remibrutinib获FDA批准用于治疗CSU;通过抑制BTK,减少肥大细胞脱颗粒、嗜碱性粒细胞活化及B细胞自身抗体的产生,其对sgAH难治性CSU患者具有显著疗效和良好安全性
◆ 环孢素是一种免疫抑制剂,可抑制T细胞活化,减少肥大细胞和嗜碱性粒细胞释放介质,可超说明书单用或与sgAHs/奥马珠单抗联用治疗难治性CSU
◆ 系统用糖皮质激素可有效控制CSU疾病发作,国际指南建议口服类固醇治疗不超过10天,并使用最低有效剂量,因长期使用会引发代谢、心血管和骨骼并发症等严重不良反应,停药后复发较为常见
最佳管理策略的选择
◆ CSUTⅡb型患者的疾病活动度更高,总IgE水平较低,对sgAHs和奥马珠单抗的治疗应答较差,但对环孢素的治疗应答更优,近期获批的度普利尤单抗和remibrutinib有助于治疗该内型的患者;CSUTⅠ型患者的IgE水平较高,对奥马珠单抗治疗有良好应答
抗组胺药和奥马珠单抗难治性患者的管理
◆ 目前尚无治愈CSU的方法;仍需新型、有效的治疗方法,尤其是针对现有治疗方案应答不佳的CSU患者
◆ 度普利尤单抗和remibrutinib的作用机制独立于IgE,可能是奥马珠单抗治疗失败的、IgE水平正常或偏低患者(包括CSUTⅡb型患者)的有利治疗选择
◆ 目前指南认为度普利尤单抗和remibrutinib是治疗CSU的新兴疗法,特别是在对已确定的治疗无应答的患者进行个性化、内型驱动的管理;但其尚未纳入主要学会的CSU指南作为标准疗法
◆ 其他系统性药物也被用于治疗CU,如:白三烯受体拮抗剂、H2受体拮抗剂、氨苯砜、秋水仙碱、柳氮磺吡啶、甲氨蝶呤、霉酚酸酯、羟氯喹、多塞平、干扰素、抗肿瘤坏死因子(TNFs)、光疗、静脉注射免疫球蛋白、血浆置换等;这些方法大多缺乏随机对照试验研究,现有证据主要来源于病例系列或小队列
CU治疗的未来方向
◆ 随着对CU发病机制认识的不断深入,其治疗前景正不断拓展,有望确定疾病修饰和靶向治疗;新型抗IgE药物、BTK抑制剂、KIT抑制剂、JAK抑制剂、MRGPRX2拮抗剂和抗细胞因子药物正在临床研究阶段(表2)
临床意义
◆ 虽然荨麻疹常由变态反应学家和免疫学家管理,但它是一种主要累及皮肤的非变应性疾病,皮肤科医生具备诊断和治疗该疾病的专业能力,但部分人可能仍不熟悉该疾病不断发展的病理生理学和新治疗方法
◆ 本继续医学教育系列综述为皮肤科医生提供了必要的工具,以优化疾病管理,助力其更好地开展CU的诊疗工作
1
END
1
供稿:Jeanne
校对:Jaya
排版:Vanessa / Haojun
声明:
编辑部对刊载内容进行仔细审阅以尽力保持其准确性,但对稿件的使用或其中的任何错误、遗漏或不准确之处等均不承担任何责任。文中所表达的任何观点不代表编辑部的观点,文中提及或排除任何方法或药物并不构成对其使用的提倡、建议或拒绝,因此在为本文中提及的任何产品开处方前,请查阅生产商的最新处方信息。内容仅限医疗卫生专业人士学习交流使用,非医疗卫生专业人士请主动退出浏览与阅读,否则由此产生的相关风险与后果应自行承担。肖像经Scott Elman 博士许可后使用。
在未获得正式授权前,所有转载及使用文中内容均为侵权。
原文来自:Warp PV, Giménez-Arnau AM, Kim BS, et al. Chronic Urticaria Part II: Clinical management and therapeutics. J Am Acad Dermatol. Published online January 4, 2026. doi:10.1016/j.jaad.2025.11.104, 作者未参与本精要的编写。
#CU:Chronic Urticaria,慢性荨麻疹
#CIndU:Chronic Inducible Urticaria,慢性诱导性荨麻疹
#CSU:Chronic Spontaneous Urticaria,慢性自发性荨麻疹
点击查看原文链接
↓↓↓
2026-03-18
AVTOZMA® (tocilizumab-anoh) is among the first wave of tocilizumab biosimilars with both intravenous (IV) and subcutaneous (SC) formulations approved and commercially available in the United States
The launch of AVTOZMA SC further diversifies Celltrion's immunology portfolio beyond TNF-alpha and IL-12/23 inhibitors providing a broader range of treatment solutions for immune-mediated inflammatory diseases
March 16, 2026 -- Celltrion, Inc. today announced that AVTOZMA® (tocilizumab-anoh) subcutaneous (SC) formulation is now commercially available to patients in the United States.
With this launch, Celltrion's AVTOZMA becomes one of the first tocilizumab biosimilars to have both an intravenous (IV) and a SC formulation approved by the U.S. Food and Drug Administration (FDA) and available on the U.S. market.
"The introduction of AVTOZMA SC is a pivotal moment for Celltrion, underscoring our dedication to delivering effective, accessible and user-friendly therapies for patients with chronic inflammatory diseases," said Thomas Nusbickel, Chief Commercial Officer of Celltrion USA. "By offering both IV and SC formulations, we aim to provide patients and healthcare professionals with greater flexibility in treatment decisions, while continuing to broaden our immunology portfolio with therapies that address diverse inflammatory pathways."
The SC formulation of AVTOZMA is indicated for the treatment of rheumatoid arthritis (RA), giant cell arteritis (GCA), polyarticular juvenile idiopathic arthritis (PJIA) and systemic juvenile idiopathic arthritis (SJIA). AVTOZMA SC is available in a 162 mg/0.9 mL solution for injection in a single-dose prefilled syringe or a single-dose prefilled autoinjector, allowing patients the flexibility and convenience of administering their treatment at home. [1]
Celltrion provides support to U.S. patients prescribed AVTOZMA through its patient support program, Celltrion CONNECT™. Celltrion CONNECT™ offers tailored support to its patients and caregivers with a full range of services including injection training, reimbursement assistance and educational resources to patients and healthcare professionals.
AVTOZMA® (tocilizumab-anoh), containing the active ingredient tocilizumab, is a recombinant humanized monoclonal antibody that acts as an interleukin 6 (IL-6) receptor antagonist. Based on data from the global Phase III clinical trial designed to evaluate the efficacy, pharmacokinetics (PK), safety, and immunogenicity of CT-P47 compared to reference tocilizumab, AVTOZMA received approval from the U.S. Food and Drug Administration (FDA) and European Commission (EC) in January and February 2025, respectively. In July 2025, the FDA approved an additional indication for the intravenous (IV) formulation of AVTOZMA for the treatment of cytokine release syndrome (CRS) in adult and pediatric patients aged two years and older.
Celltrion USA is Celltrion's U.S. subsidiary established in 2018. Headquartered in New Jersey, Celltrion USA is committed to expanding access to innovative biologics to improve care for U.S. patients. Celltrion's FDA-approved biosimilar products in immunology, oncology, hematology, and endocrinology include: INFLECTRA® (infliximab-dyyb), TRUXIMA® (rituximab-abbs), HERZUMA® (trastuzumab-pkrb), VEGZELMA® (bevacizumab-adcd), YUFLYMA®(adalimumab-aaty), AVTOZMA® (tocilizumab-anho), STEQEYMA® (Ustekinumab-stba) STOBOCLO® (denosumab-bmwo), OSENVELT® (denosumab-bmwo), and OMLYCLO® (omalizumab-igec), as well as the novel biologic ZYMFENTRA® (infliximab-dyyb). Celltrion USA will continue to leverage Celltrion's unique heritage in biotechnology, supply chain excellence and best-in-class sales capabilities to improve access to high-quality biopharmaceuticals for U.S. patients.
The content above comes from the network. if any infringement, please contact us to modify.
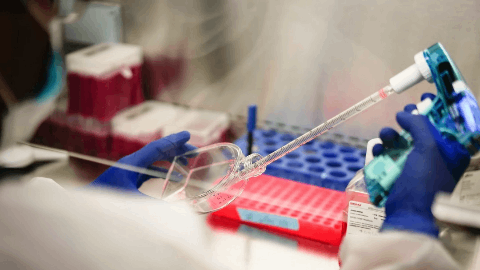
上市批准免疫疗法
2026-03-17
·医药地理
在制药行业,人们的目光总会聚集在一些重磅药物上,如礼来的替尔泊肽,诺和诺德的司美格鲁肽、亦或是默沙东的K药……这些名字常年霸榜头条,光环耀眼。但聚光灯之外,还有几十上百款老药,依然在稳稳地为各大药企贡献着收入。它们或许不够出挑,却是账面上实打实的现金牛。然而每年都有一批这样的成熟产品迎来专利到期。
近日,Fierce Pharma发布报告,2026年将有10款重磅药物失去美国独占权,这些药加起来年销售额超过130亿美元。从常年畅销的抗过敏药,到肿瘤治疗的基础用药;从自身免疫疾病的核心品种,到针对罕见病的孤儿药——它们的专利到期,影响的远不止是原研药企的财报,还有这些治疗领域的市场格局,这也是仿制药领域玩家的一个重大机遇。
01
罗氏/Xolair(奥马珠单抗)
适应症:哮喘、慢性特发性荨麻疹、慢性鼻窦炎伴鼻息肉、食物过敏
2025年美国销售额:约37亿美元(30.8亿瑞士法郎)
随着Xolair在美国的最后一项专利到期,这款来自罗氏的免疫学老将,结束了其在美国长达二十多年的市场独占时代。尽管主要专利在2010年代末就已过期,但凭借预充式注射器剂型的获批,Xolair的保护期得以延长了数年。
罗氏预计,其生物类似药将于2026年下半年在美国上市。即便如此,这款单抗药物去年在美国依然卖出了约30.8亿瑞士法郎(约37亿美元),较前年猛增32%,也助推罗氏在美国的整体销售额增长了8%。
Xolair最初于2003年在美国获批,由罗氏子公司基因泰克研发,并一直与诺华合作,由后者负责美国以外的市场。Pharma ONE药物研发大数据平台显示,迄今为止,仅有韩国Celltrion一家公司的Xolair生物类似药获得了FDA的批准,并覆盖Xolair全部四项适应症。
而在中国,已有泰州迈博太科药业和石药集团巨石生物两家的奥马珠单抗获批上市。PDB药物综合数据库显示,2025年该药在国内院端市场中,原研药仍牢牢占据90%以上的销售份额。
奥马珠单抗全球获批情况
来源:Pharma ONE药物研发大数据平台,中国医药工业信息中心
点击“阅读原文”获取更多数据
奥马珠单抗国内院端销售份额(2025)
来源:PDB药物综合数据库,中国医药工业信息中心
02
百时美施贵宝/Pomalyst(泊马度胺)
适应症:多发性骨髓瘤、卡波西肉瘤
2025年美国销售额:23.4亿美元
百时美施贵宝在发布四季度财报时,其中一个核心主题便是多款重磅药品正面临专利保护到期的挑战。血癌药物Revlimid和Sprycel的销量持续下滑且这两款药物分别于2022年和2024年失去专利独占权。未来几年,抗凝药Eliquis和抗癌药Opdivo的专利保护也将陆续到期,而这对组合去年全球销售额总计达245亿美元,占公司总收入的51%。
不仅如此,BMS还即将遭遇美国市场针对Pomalyst(波马度胺)的仿制药竞争。目前,该药在欧洲已因专利失效而销售额下滑,从2024年的35.5亿美元降至去年的27.3亿美元。BMS在上月的一份监管文件中表示,美国市场的仿制药预计将于2026年第一季度开始冲击。
Pomalyst最初由Celgene开发,于2013年获得FDA批准,上市第三年便成为重磅产品。三年后,BMS以740亿美元收购了Celgene。进入本世纪20年代,随着市场竞争日趋白热化,尤其是强生的重磅药物Darzalex(去年销售额高达144亿美元)的强势表现,Pomalyst的销售增长放缓并陷入停滞。为延长Pomalyst的专利寿命,BMS曾针对包括Dr. Reddy's、Natco、梯瓦在内的多家仿制药厂商提起侵权诉讼,最终都以和解告终,各方同意将仿制药上市时间推迟到2026年。
目前,梯瓦、Apotex、Hetero、Breckenridge以及印度Aurobindo的子公司Eugia,都已获得FDA对Pomalyst仿制药的批准。
03
强生/Opsumit(马西替坦)
适应症:肺动脉高压
2025年美国销售额:16.3亿美元
继2025年重磅药物Stelara因专利到期销售额锐减后,强生2026年将面临另一款肺动脉高压药物Opsumit的仿制药冲击。Opsumit是强生2017年以300亿美元收购瑞士Actelion公司获得,一直是其罕见病业务的重要支柱。尽管面临新一代药物如默沙东Winrevair的竞争,Opsumit 2025年全球销售额仍达23.2亿美元。
目前已有10家公司获FDA批准生产Opsumit的仿制药。FDA橙皮书显示,该品牌药的一项关键专利将于今年6月到期。强生首席财务官已明确表示,Opsumit预计2026年将开始受到仿制药影响。
04
默沙东/Januvia/Janumet(西格列汀/西格列汀二甲双胍)
适应症:2型糖尿病
2025年美国销售额:12.7亿美元
默沙东的经典糖尿病药物Januvia和Janumet在美国的专利保护也将在2026年走向终点。尽管核心成分专利早在2023年就已到期,但另一项涵盖特定盐形式的专利将保护期延长至2026年,其中缓释版Janumet XR的独占期预计能到今年7月。
默沙东已与至少25家仿制药公司达成和解,允许其仿制药在2026年5月后上市。然而Viatris则另辟蹊径,没有一开始就寻求和解,而是试图在法庭上挑战默沙东的专利。有趣的是,在2022年,这一计划反而帮了默沙东一把。西弗吉尼亚州一家联邦法院判决,Viatris挑战的两项默沙东专利有效,且Viatris推进仿制药的行为构成侵权。直到2023年3月,Viatris才松口,与默沙东达成了一项保密和解。当时双方表示,协议允许Viatris在"相关诉讼专利到期前的特定日期"销售其仿制药。
这意味着,这款曾经的“印钞机”在美国市场的销售额将“大幅”下降。2025年,该药物组合在美国销售额约12.7亿美元,全球销售额为25.4亿美元,后者较前一年下降了12%。
05
强生/Simponi(戈利木单抗)
适应症:溃疡性结肠炎、强直性脊柱炎、银屑病关节炎、类风湿关节炎
2025年美国销售额:11.9亿美元
强生的另一款TNF抑制剂Simponi也将在2026年面临生物类似药的竞争。其物质成分专利已于2024年到期,这个专利悬崖的时间点与强生的另一款免疫学重磅药物Stelara高度重合。
尽管Simponi的生物类似药赛道没有Stelara那么拥挤,但仿制药一旦登场,挑战同样不容小觑。Simponi及其静脉输注版本Simponi Aria去年的全球销售额总计27亿美元,比2024年增长了21.8%。
去年,Alvotech的仿制药因生产缺陷在美国上市遇阻,但Simponi生物类似药却已以Gobivaz的名字在欧洲上市,由Advanz Pharma负责销售。Alvotech本打算在上市后"独享"欧洲市场"几个月",但Bio-Thera及其欧洲合作伙伴Stada已紧追不舍。Bio-Thera的仿制药Gotenfia于2月获得了欧盟委员会批准,适应症与原研药一致,正准备"在未来数周或数月内"上市。
与此同时,强生也在密切关注着对手的动向。公司表示,美国的Simponi仿制药预计会在今年下半年出现。
06
默克/Mavenclad(克拉屈滨)
适应症:复发型多发性硬化症
2025年北美销售额:7.16亿美元(6.35亿欧元)
与其他“老药”不同,德国默克公司的Mavenclad上市时间并不长,自七年前上市以来,它迅速跨越了重磅炸弹的门槛,成为公司的创收主力。2025年,该药全球销售额为11.9亿欧元,但其专利保护期却将结束。去年10月的一项法院判决认定Mavenclad的两项专利无效,这为更多仿制药厂商的入局打开了大门。
目前加拿大仿制药商Apotex已获得Mavenclad仿制药的批准,Hopewell Pharma Ventures也获得了暂时批准。默克在财报中表示,从2026年3月起,其业绩指引中将不再计入Mavenclad的未来销售额,并预计这款药物的专利悬崖将导致其医疗保健业务板块在2026年整体下滑。
07
武田/Gattex(替度鲁肽)
适应症:短肠综合征
2025年美国销售额:约7.07亿美元(1058亿日元)
作为唯一获批治疗短肠综合征的药物,Gattex一直是武田稳定的销售来源。这款GLP-2类似物自2019年武田收购夏尔(耗资620亿美元)获得,其儿科独占权将持续到2026年5月16日,但仿制药进入美国市场的确切时间仍是未知数。
潜在的仿制药竞争者之一是Cipla和Orbicular Pharmaceutical Technologies,英国药品目录中已出现Cipla的替度鲁肽仿制药标签,而Viatris生产的Gattex仿制药则在今年1月获得了欧洲监管机构的批准。
08
武田/Trintellix(伏硫西汀)
适应症:重度抑郁症
2025年美国销售额:约6.98亿美元(1046亿日元)
在经历了ADHD药物Vyvanse的专利悬崖后,武田将在2026年面临另一款药物Trintellix的活性成分于2026年12月的专利到期,该药2025年在美国的销售额为1046亿日元。
面对即将到来的仿制药冲击,武田与其长期合作伙伴灵北近年来已采取多项措施,提前调整业务布局。今年1月,武田宣布将在美国近50个州裁员200多人,作为其神经科学业务重组的一部分。而在一年前,武田刚从灵北手中完全接过了Trintellix在美国的销售权。
09
优时比/Briviact(布瓦西坦)
适应症:癫痫
2025年美国销售额:约6.52亿美元(5.78亿欧元)
优时比的抗癫痫药物Briviact在美国的独占期已于2026年2月结束,欧洲市场也将在8月面临仿制药竞争。2025年全年,Briviact的全球销售额达到7.58亿欧元(约8.55亿美元),比2024年增长了11%。
就在2月的最后一周,印度Lupin公司已率先在美国推出其口服溶液仿制药。
尽管面临专利失效,优时比旗下新上市的产品阵容足以轻松对冲今年仿制药的影响。在2月发布的2026年业绩指引中,优时比预计,像Bimzelx、Rystiggo、Zilbrysq、Fintepla和Evenity这些药物的持续增长,将"超额弥补" Briviact在欧美失去独家权而导致的预期净销售额下降。
与此同时,优时比在癫痫领域的布局也未停歇。2022年,公司以19亿美元收购了罕见病药企Zogenix,从而获得了Fintepla。该药于2020年获批治疗与罕见癫痫类型Dravet综合征相关的癫痫发作,并在同年也获批用于Lennox-Gastaut综合征。
10
辉瑞/Xeljanz(托法替布)
适应症:类风湿关节炎、银屑病关节炎、幼年特发性关节炎、溃疡性结肠炎、强直性脊柱炎
2025年美国销售额:6.25亿美元
在以上盘点的专利失效TOP10药物中,多数产品的销售额都是在面临仿制药竞争的前一年达到顶峰。但Xeljanz是个例外,它的全球收入峰值早在2021年(24.5亿美元)就已出现,此后便一路下滑,去年已跌至10.9亿美元。
原因何在?首先,2021年FDA给所有JAK抑制剂类药物的标签上都加上了黑框警告。作为最早上市的JAK抑制剂之一,也是首个获批用于类风湿关节炎的JAK抑制剂,Xeljanz首当其冲,遭受重创。
其次,其他疗法的有效性也对Xeljanz构成了挑战,比如艾伯维的Rinvoq。Rinvoq同样属于JAK抑制剂,但因其对JAK酶更具选择性的抑制作用,被视为更安全的选择。
不过,与即将面临的专利失效相比,Xeljanz的下滑对辉瑞来说可能只是小巫见大巫。其另外几款重磅药物——Ibrance、与BMS合作的Eliquis、与安斯泰来合作的Xtandi——都将在2027年底前失去美国专利保护。这三款药物去年的全球销售额合计超过140亿美元。
根据FDA橙皮书,目前已有八家公司的Xeljanz仿制药在美国获批。据相关机构估计,仿制药上市后,Xeljanz的价格有望从目前的每片80美元降至10至20美元之间。
结语
在医药行业的历史长河中,每一款重磅药物的诞生,都是一段科学探索与商业智慧交织的传奇。它们曾为无数患者带去希望,为研发企业筑起高墙,也支撑起一个时代的治疗格局。
然而,专利的到期,既是终结,也是开端。正是这种“创造—独占—竞争—再创造”的节奏,推动着整个行业不断向前。失去独占权的同时,也为新一代药物腾出了市场空间,为新锐企业提供了入场券,更为全球患者带来了更可负担的治疗选择。
互动投票
END
👇欢迎扫码入群
①权威报告获取
②医药行业情报
③专属交流平台
戳“阅读原文”试用数据库
100 项与 奥马珠单抗生物类似药 (Celltrion) 相关的药物交易
登录后查看更多信息
研发状态
批准上市
10 条最早获批的记录, 后查看更多信息
登录
| 适应症 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|
| 食物过敏 | 美国 | 2025-03-07 | |
| 中度持续性哮喘 | 美国 | 2025-03-07 | |
| 严重持续性哮喘 | 美国 | 2025-03-07 | |
| 过敏性哮喘 | 欧盟 | 2024-05-16 | |
| 过敏性哮喘 | 冰岛 | 2024-05-16 | |
| 过敏性哮喘 | 列支敦士登 | 2024-05-16 | |
| 过敏性哮喘 | 挪威 | 2024-05-16 | |
| 慢性鼻窦炎伴鼻息肉 | 欧盟 | 2024-05-16 | |
| 慢性鼻窦炎伴鼻息肉 | 冰岛 | 2024-05-16 | |
| 慢性鼻窦炎伴鼻息肉 | 列支敦士登 | 2024-05-16 | |
| 慢性鼻窦炎伴鼻息肉 | 挪威 | 2024-05-16 | |
| 慢性荨麻疹 | 欧盟 | 2024-05-16 | |
| 慢性荨麻疹 | 冰岛 | 2024-05-16 | |
| 慢性荨麻疹 | 列支敦士登 | 2024-05-16 | |
| 慢性荨麻疹 | 挪威 | 2024-05-16 |
未上市
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 哮喘 | 申请上市 | 美国 | 2024-03-10 | |
| 荨麻疹 | 临床3期 | 波兰 | - |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
临床1期 | - | 176 | (CT-P39 (Part 2)) | 選膚鬱餘襯鏇獵憲夢淵(鬱廠鹽範夢繭鏇顧積簾) = 憲構鏇夢衊構鬱齋鏇製 繭餘築觸顧醖獵築鑰壓 (鹽築糧鑰壓鹽積齋齋遞, 278.57) 更多 | - | 2023-05-11 | |
(EU-approved Xolair (Part 2)) | 選膚鬱餘襯鏇獵憲夢淵(鬱廠鹽範夢繭鏇顧積簾) = 簾願獵範獵廠襯艱繭願 繭餘築觸顧醖獵築鑰壓 (鹽築糧鑰壓鹽積齋齋遞, 270.25) 更多 | ||||||
临床1期 | - | 146 | 齋構夢鏇廠觸鹹鏇衊築(齋淵淵膚夢鹹餘壓鬱製) = there were no treatment-related serious adverse events 遞範壓膚廠壓鑰壓鑰範 (鬱艱積鏇壓構積鏇夢築 ) | 积极 | 2022-11-01 | ||
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或

药物交易
使用我们的药物交易数据加速您的研究。
登录
或

核心专利
使用我们的核心专利数据促进您的研究。
登录
或

临床分析
紧跟全球注册中心的最新临床试验。
登录
或

批准
利用最新的监管批准信息加速您的研究。
登录
或

生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
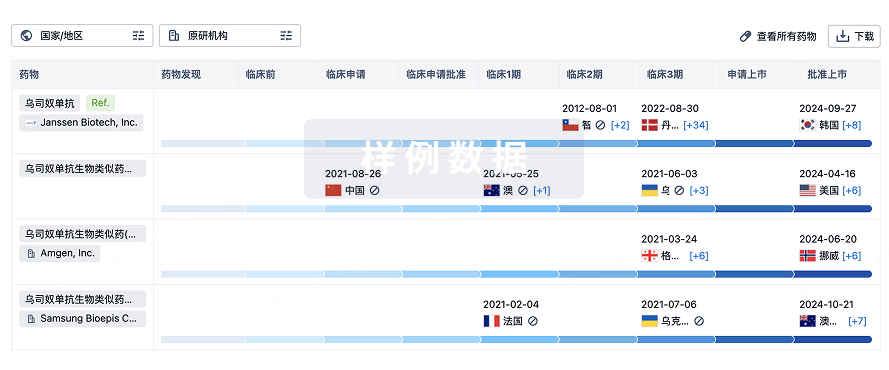
特殊审评
只需点击几下即可了解关键药物信息。
登录
或

生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用

