预约演示
更新于:2026-03-03

Orange Park Medical Center, Inc.
更新于:2026-03-03
概览
关联
4
项与 Orange Park Medical Center, Inc. 相关的临床试验NCT06336460
Pericapsular Nerve Group (PENG) Block vs. the Fascia Iliaca Compartment (FIC) Block for Patients With Isolated Hip Fractures in the Emergency Department
This study is a prospective, randomized clinical trial assessing the efficacy of physician-performed ultrasound-guided pericapsular nerve group (PENG) block vs fascia iliaca compartment (FIC) block for pain control in acute hip fracture.
开始日期2024-04-01 |
NCT05881434
Influence of a Questionnaire on Patients' Emergency Room Expectations
The goal of this study is to determine whether a novel questionnaire designed to illicit patient's self-reported expectations across four domains (overall purpose of visit, medication intervention, imaging intervention and disposition) improves patient-provider communication as evaluated by an exit survey during an emergency room visit.
开始日期2022-01-31 |
NCT05961137
Orange Park Out-of-Hospital Quality Improvement Study for Improving CMS Sepsis Core Measures
The goal of this quality improvement study is to measure the impact of incorporation of a manual rapid fluid infuser (RFI) for intravenous crystalloid infusion in patients with suspected sepsis in the prehospital interval.
The main question[s] it aims to answer are:
* Does the intervention affect the timeliness of fluid administration?
* Does the intervention affect CMS sepsis bundle care measure compliance?
* Does the intervention affect processes and outcomes of care?
* Are there any adverse effects?
Researchers will compare this intervention to use of more conventional gravity or pressure-infusion bag crystalloid infusion.
The main question[s] it aims to answer are:
* Does the intervention affect the timeliness of fluid administration?
* Does the intervention affect CMS sepsis bundle care measure compliance?
* Does the intervention affect processes and outcomes of care?
* Are there any adverse effects?
Researchers will compare this intervention to use of more conventional gravity or pressure-infusion bag crystalloid infusion.
开始日期2021-04-01 |
申办/合作机构 |
100 项与 Orange Park Medical Center, Inc. 相关的临床结果
登录后查看更多信息
0 项与 Orange Park Medical Center, Inc. 相关的专利(医药)
登录后查看更多信息
78
项与 Orange Park Medical Center, Inc. 相关的文献(医药)2025-04-01·Journal of the American College of Emergency Physicians Open
Artificial Intelligence in Emergency Medicine: A Primer for the Nonexpert
Article
作者: Gottlieb, Michael ; Garg, Nidhi ; Lam, Samuel H F ; Goebel, Mat ; Wegman, Martin ; Lee, Sangil ; Zalesky, C Christopher ; Smith, Moira E ; Adhikari, Srikar
Artificial intelligence (AI) is increasingly being utilized to augment the practice of emergency medicine due to rapid technological advances and breakthroughs. AI applications have been used to enhance triage systems, predict disease-specific risk, estimate staffing needs, forecast patient decompensation, and interpret imaging findings in the emergency department setting. This article aims to help readers without formal training become informed end-users of AI in emergency medicine. The authors will briefly discuss the principles and key terminology of AI, the reasons for its rising popularity, its potential applications in the emergency department setting, and its limitations. Additionally, resources for further self-studying will also be provided.
2024-12-01·EUROPEAN CHILD & ADOLESCENT PSYCHIATRY
Problems most concerning to parents of children with ADHD and emotional dysregulation in a randomized controlled trial of multinutrients: MADDY secondary analysis
Article
作者: Srikanth, Priya ; Tost, Gabriella ; Leung, Brenda My ; Johnstone, Jeanette M ; Bruton, Alisha ; Williams, Craig ; Eugene Arnold, L ; Ast, Hayleigh K ; Eiterman, Leanna P ; Gracious, Barbara ; Hatsu, Irene E ; Robinette, Lisa M
OBJECTIVE:
With dual focus on structured, objective quantification of parent observations of child's behavior and identifying behaviors most amenable to change, this report examines Parent Target Problems (PTP) as a secondary outcome in a randomized clinical trial (RCT) of children with attention-deficit/ hyperactivity disorder (ADHD) in which one primary outcome, Clinical Global Impression-Improvement, showed a significant advantage of multinutrients over placebo and the other, Likert-type parent ratings, showed significant improvement in both groups, without significant difference between them.
METHOD:
In a multisite 8-week RCT of broad-spectrum micronutrients ("multinutrients"), parents of children ages 6-12 (N = 126, 73% male, 88% white) with ADHD and emotional dysregulation nominated their child's most concerning problem(s) at baseline and quantified them by frequency, duration, impairment, and consequences. At subsequent visits, parents re-quantified the problem(s). Blinded child psychiatrists independently reviewed the PTPs and rated change at two timepoints compared to baseline. PTPs were grouped into 9 categories. Mean ratings were compared between active and placebo groups and explored by category.
RESULTS:
By week 8, a significant separation favored multinutrients: 38% of the multinutrient group were "definitely improved" or better, compared to 25% of the placebo group, and ratings of "no change" or "worse" occurred in 35% with placebo versus 23% with multinutrients (p = 0.04). Inattention (72.2%) and emotional dysregulation (69.1%) were the most frequently reported PTP categories. Inattention and internalizing symptoms improved more with multinutrients than placebo (p = 0.01, d = 0.55; p = 0.03, d = 0.80, respectively). The multinutrient advantage was not significant for 7 other symptoms, including hyperactivity/impulsivity, aggression, autistic symptoms, or emotional dysregulation/irritable oppositionality.
CONCLUSIONS:
This secondary analysis found that the multinutrients, compared to placebo, were associated with improvements in parental concerns overall, and in two domains specifically: inattention and internalizing symptoms (anxiety/depression), but not in seven domains: hyperactivity/impulsivity, aggression, autistic symptoms or physiological symptoms, peer relationships or emotional dysregulation/irritable oppositionality.
2024-05-05·Cureus Journal of Medical Science
Phytophotodermatitis From Lime Margaritas on a Mexico Vacation
作者: Jallo, Jennifer ; Cochran, Brigitte L ; Sagasser, Josie ; Coican, Alexis ; Greenfield, Melinda F ; Hurst, Kala
Phytophotodermatitis is a type of contact dermatitis that occurs upon skin exposure to certain plant chemicals, known as furocoumarins, along with simultaneous sun exposure. This case details a 34-year-old patient who presented to the office with an asymptomatic, irregularly shaped, and hyperpigmented patch located on the left inferior middle back that had been present since a recent beach vacation in Mexico. Upon gathering the history, clinicians should inquire about recent sunlight exposure while consuming and/or touching phytotoxic plant derivatives found in most citrus plants. The history should correspond with the skin examination findings and conclude that a cutaneous phytotoxic reaction had occurred when a lime margarita contacted the hand, which was subsequently rubbed onto the patient's back. This case highlights the importance of both taking a thorough history and physical examination and being aware of the broad range of skin manifestations to prevent unnecessary treatment, such as topical corticosteroids, for other skin disorders (the irregular presentation of atopic dermatitis, allergic contact dermatitis, and dermatitis unspecified) or improperly suspected child abuse in younger patient presentations.
100 项与 Orange Park Medical Center, Inc. 相关的药物交易
登录后查看更多信息
100 项与 Orange Park Medical Center, Inc. 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年04月06日管线快照
无数据报导
登录后保持更新
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
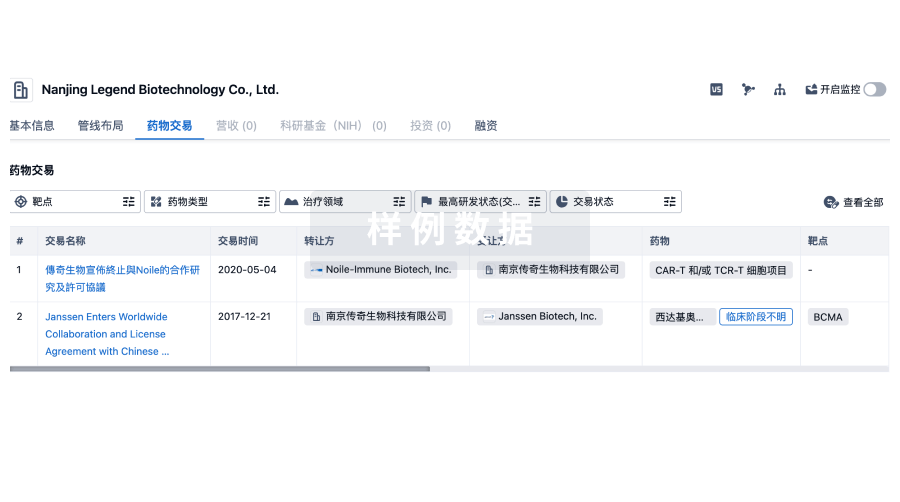
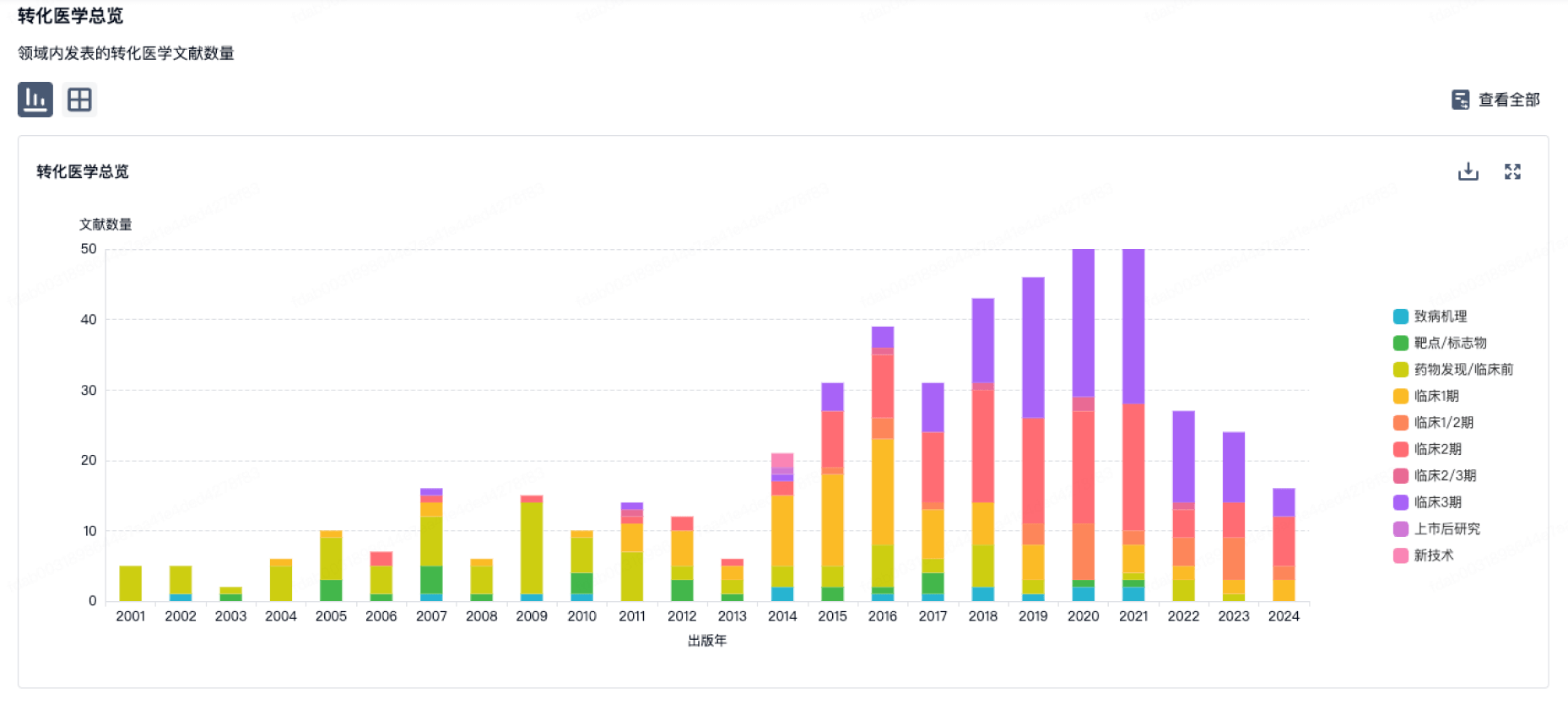
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
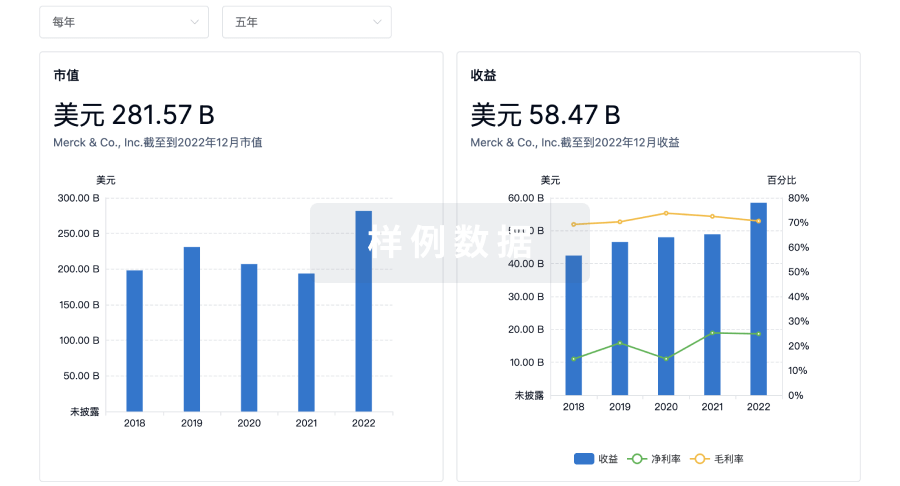
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
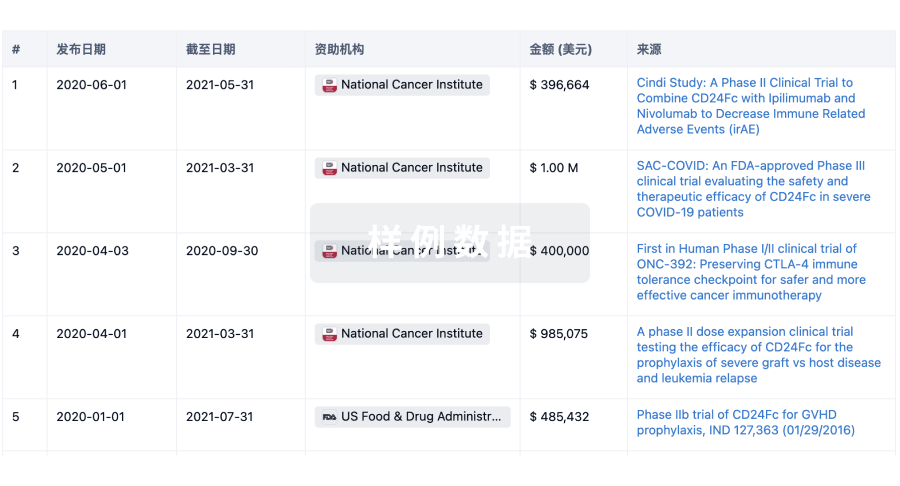
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
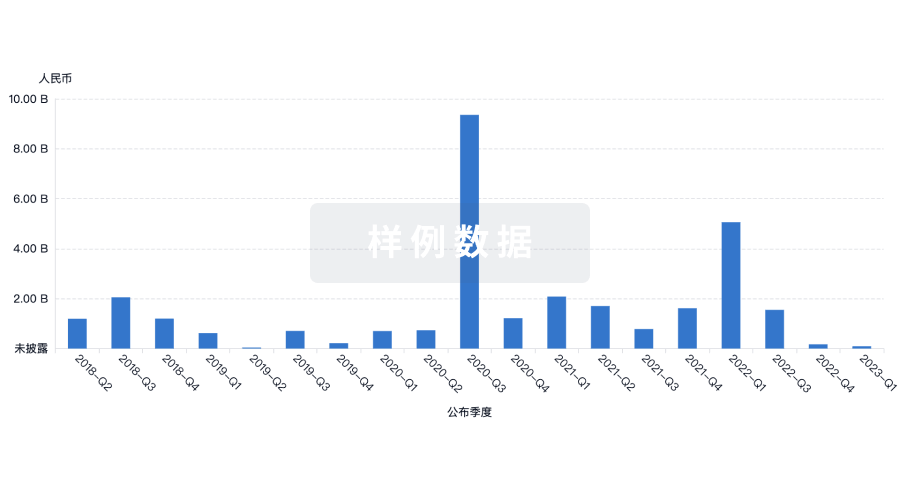
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
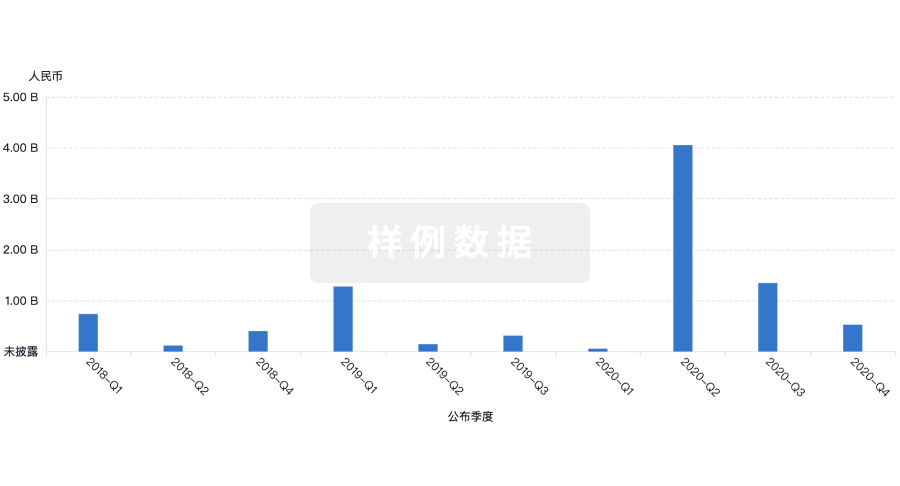
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用