预约演示
更新于:2025-05-07
Amgen (Europe) GmbH
子公司|Switzerland
子公司|Switzerland
更新于:2025-05-07
概览
关联
1
项与 Amgen (Europe) GmbH 相关的临床试验DRKS00026023
Description of (re-)induction therapies prior to a planned stem cell transplantation in patients with relapsed / refractory multiple myeloma in Germany
开始日期2021-08-10 |
申办/合作机构 |
100 项与 Amgen (Europe) GmbH 相关的临床结果
登录后查看更多信息
0 项与 Amgen (Europe) GmbH 相关的专利(医药)
登录后查看更多信息
331
项与 Amgen (Europe) GmbH 相关的文献(医药)2025-04-01·Rheumatology and Therapy
Real-World Osteoporosis Treatment Gap and Costs in Spain: Data from Women with a First Fragility Fracture or Diagnosis of Postmenopausal Osteoporosis
Article
作者: Gatell, Sonia ; Sorio-Vilela, Francesc ; Sicras-Mainar, Antoni ; Sacrest-Soy, Marta ; Sicras-Navarro, Aram ; Villoro-Valdés, Renata ; Hernández, Ignacio ; Rebollo-Gómez, Elena
2025-02-01·Journal of Clinical Oncology
Real-world biomarker testing and first-line treatment patterns among locally advanced, unresectable or metastatic gastric and gastroesophageal junction adenocarcinoma patients in the US.
作者: Gleason, Michelle Kathleen ; Majer, Istvan Matyas ; Wellen, Maria ; Tzala, Lia ; Reading, Stephanie Rummans ; Luu, Tony
2024-12-31·Biotechnology & Biotechnological Equipment
Routine use of denosumab for prevention of skeletal-related events in patients with bone metastases from prostate carcinoma in Bulgaria: a prospective observational study
作者: Olszewski, Adrian ; Bjorklof, Katja ; Petrova, Miglena ; Ianakieva, Valentina ; Tomova, Antoaneta
100 项与 Amgen (Europe) GmbH 相关的药物交易
登录后查看更多信息
100 项与 Amgen (Europe) GmbH 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年03月21日管线快照
无数据报导
登录后保持更新
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
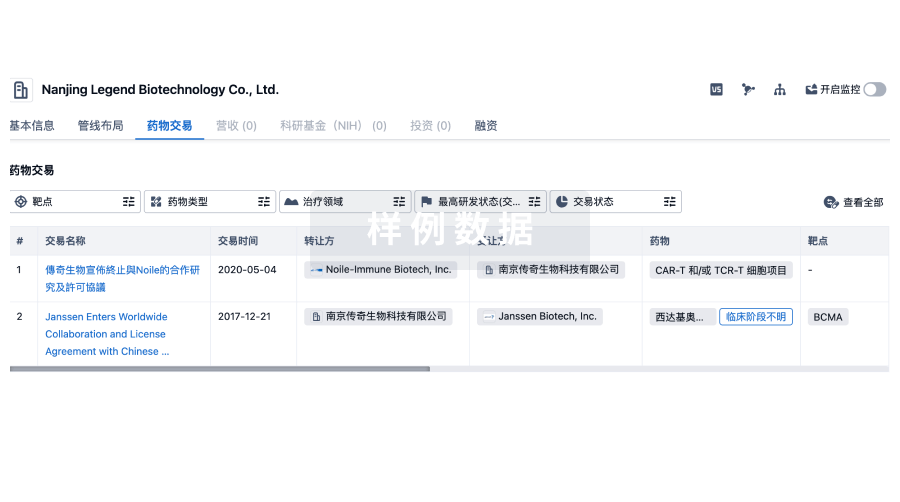
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
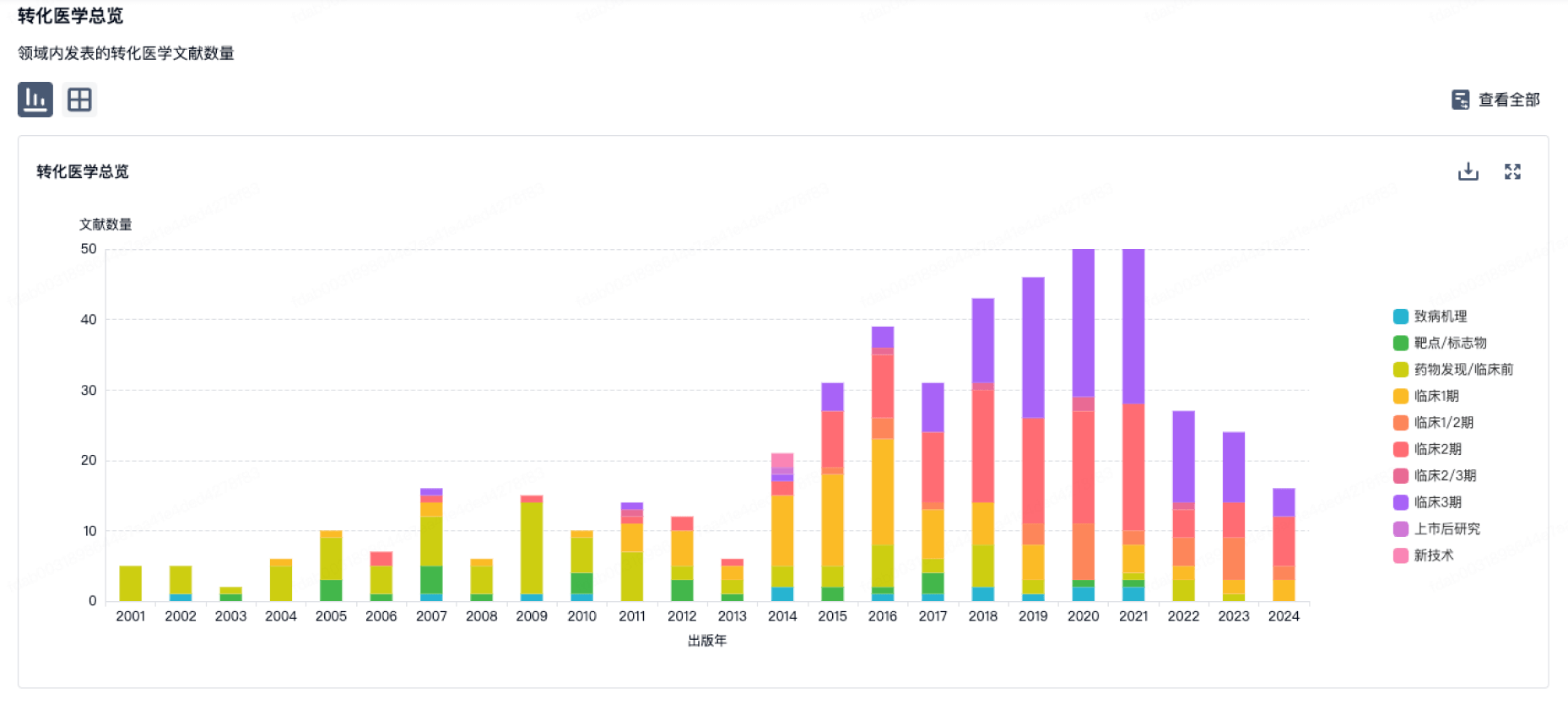
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
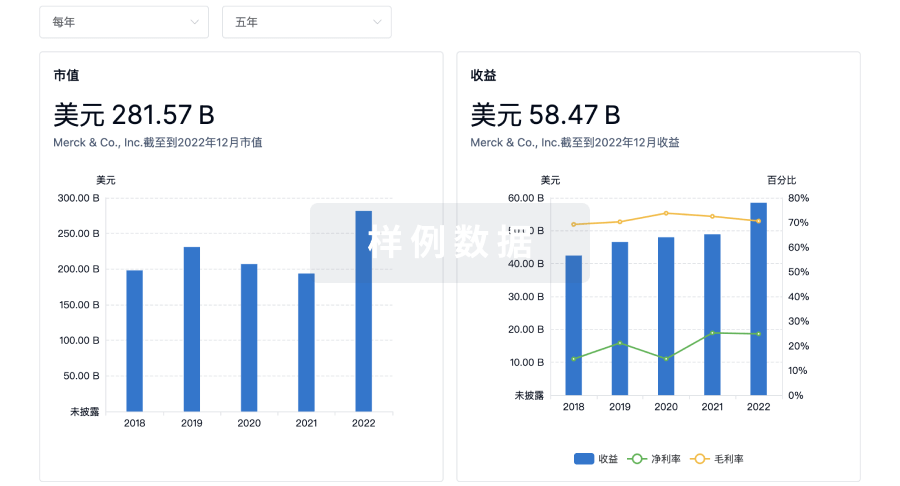
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
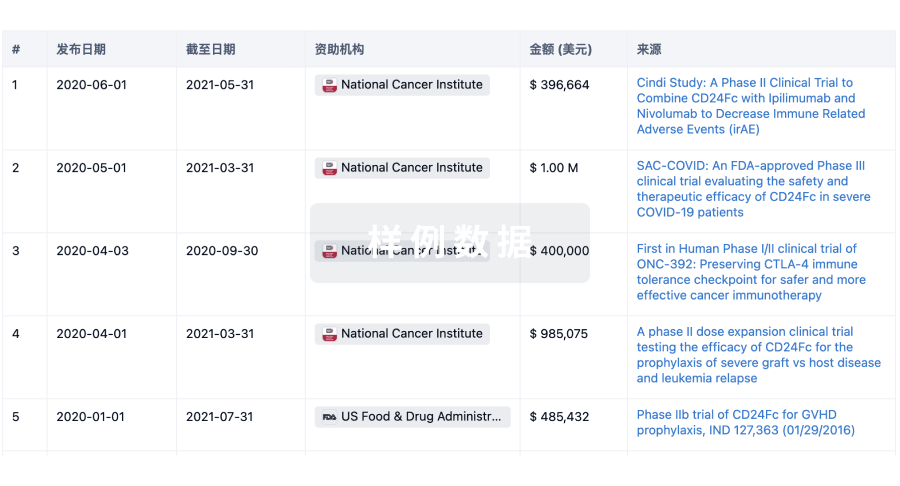
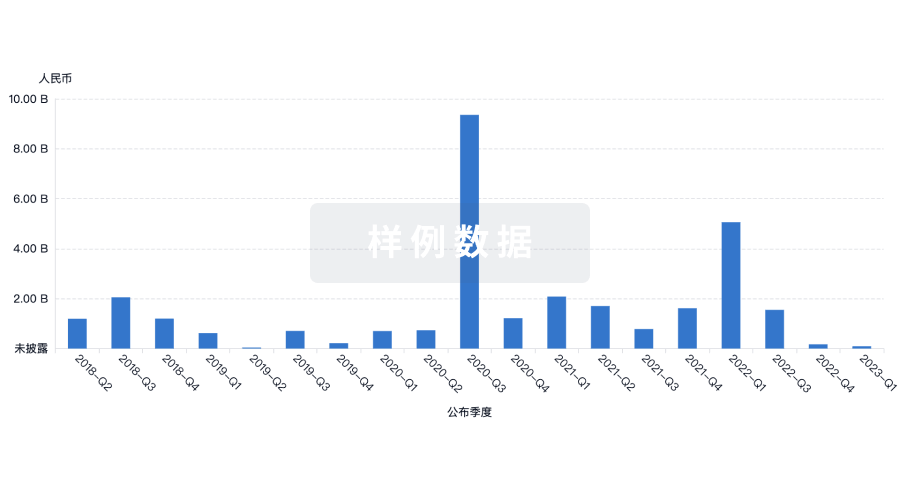
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
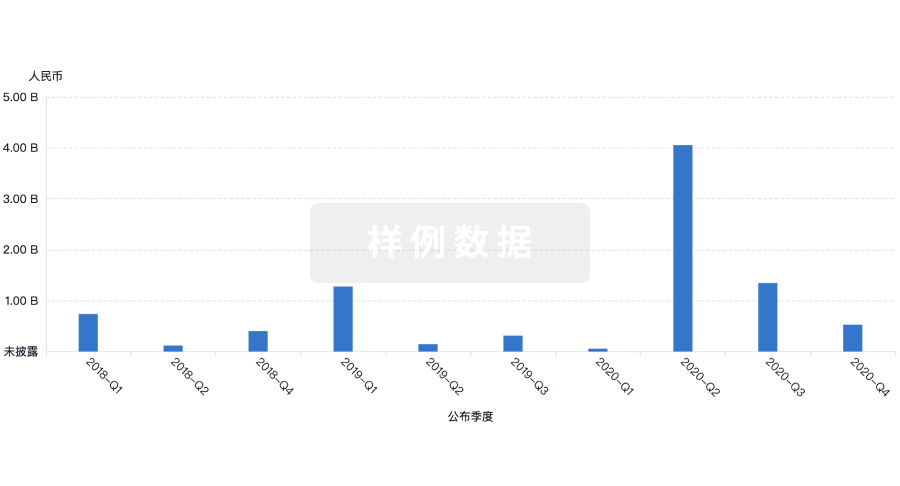
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用