预约演示
更新于:2026-03-05

Saladax Biomedical, Inc.
更新于:2026-03-05
概览
关联
6
项与 Saladax Biomedical, Inc. 相关的临床试验NCT05711732
Collection of Plasma Samples Using Sodium Heparin From Subjects Undergoing Intravenous Busulfan Treatment
Busulfan (Busulfex®) is an alkylating drug used as a conditioning regimen prior to allogeneic hematopoietic stem cell transplantation. Busulfan has wide inter- and intra-patient pharmacokinetic variability resulting in variable exposure leading to increased risk of toxicities or sub-optimal treatment outcomes. Therapeutic drug monitoring of busulfan using patient plasma samples would benefit clinicians by providing the ability to personalize the dose to achieve a target busulfan exposure.
开始日期2024-02-08 |
申办/合作机构 |
NCT05422131
Collection of Capillary Fingerstick Blood, Venous Serum, and Venous K2EDTA Blood Samples From Subjects Receiving Clozapine Therapy
The method comparison study involves capillary fingerstick blood, venous serum, and venous K2EDTA blood sample collection from human subjects receiving clozapine treatment and their clozapine concentration measurement using a validated mass spectrometry method, the automated immunoassay MyCare Psychiatry Clozapine Assay Kit manufactured by SBI, and the point of care MyCare Insite Clozapine Test manufactured by SBI. Clozapine measurements obtained using the MyCare Insite Clozapine Test are intended for investigational purposes only and shall not be used in the management of patients receiving clozapine therapy.
开始日期2022-11-12 |
申办/合作机构 |
NCT02502864
Multicenter Study Investigating Utilization of Pharmacokinetic(PK)-Guided Docetaxel in Senior Adult Breast Cancer Patients Receiving Docetaxel and Cyclophosphamide (TC) Chemotherapy
The purpose of this study is to adjust the amount of docetaxel participants receive based on the level of docetaxel measured in their blood. This method of dose adjustment is called pharmacokinetic (PK)-adjusted docetaxel. The researchers believe that adjusting the dose of docetaxel using this method will lessen the side effects associated with docetaxel in cancer treatment.
开始日期2016-02-09 |
100 项与 Saladax Biomedical, Inc. 相关的临床结果
登录后查看更多信息
0 项与 Saladax Biomedical, Inc. 相关的专利(医药)
登录后查看更多信息
15
项与 Saladax Biomedical, Inc. 相关的文献(医药)2024-05-02·The journal of applied laboratory medicine
Evaluation of Busulfan as a Third-Party Immunoassay on a Clinical Chemistry Analyzer
Article
作者: To, Andrea ; Kulasingam, Vathany ; Yazdanpanah, Mehrdad ; Fritz, James ; Zhou, Janet R ; Jung, Benjamin
Abstract:
Background:
Busulfan is widely used in conditioning regimens to prepare patients for hematopoietic stem cell transplantation. Therapeutic drug monitoring (TDM) is critical due to large inter- and intra-individual variability in busulfan pharmacokinetics, and the risk of adverse consequences of toxicity including hepatic veno-occlusive disease. Busulfan is most commonly measured by liquid chromatography–mass spectrometry (LC-MS/MS), which is not as widely available in clinical laboratories as automated routine clinical chemistry analyzers. The objective was to perform analytical verification of a busulfan immunoassay on the Abbott Alinity c platform.
Methods:
The MyCare Oncology busulfan immunoassay was configured as a third-party reagent on the Abbott Alinity c. Imprecision, linearity, sample carryover, and onboard stability of reagent studies were evaluated. The performance of the busulfan immunoassay using the Abbott Alinity c was compared to the Beckman Coulter AU480 using sodium heparinized plasma, as well as to LC-MS/MS using lithium heparinized plasma.
Results:
The imprecision goal of 8% was met, and linearity within the analytical measurement range of 240 to 1700 ng/mL was verified. Sample carryover was negligible, and the reagents were stable onboard for at least 84 days. The busulfan immunoassay correlated well with LC-MS/MS (slope = 0.949, y-intercept = −7.8 ng/mL, r2 = 0.9935) and the Beckman Coulter AU480 (slope = 1.090, y-intercept = −34.5 ng/mL, r2 = 0.9988).
Conclusions:
This study demonstrated successful analytical verification of a busulfan third-party immunoassay on the Abbott Alinity c platform. The ability to perform TDM of busulfan on a routine clinical chemistry analyzer will positively impact turnaround times to improve patient outcomes.
2024-01-05·Clinical cancer research : an official journal of the American Association for Cancer Research
Project Confirm: Accelerated Drug Approvals for CML—Letter
Letter
作者: Salamone, Salvatore J. ; Beumer, Jan H.
In reviewing CML drug development, Sweet and colleagues touch on the importance of dose optimization and lament that "TKI dose-finding trials… determine the MTD", and that "it is unlikely that most patients… require the MTD" (1). While we agree with the latter, dose optimization of the first TKI certainly did not stop at the MTD.Novartis' efforts to personalize imatinib dosing through Therapeutic Drug Monitoring (TDM) of plasma concentrations is unprecedented and never-repeated (2). The FDA's reaction disincentivized such efforts, and locked the industry into the one-dose-fits-all approach. Project Optimus merely suggests shifting a single dose, usually lower (3). We propose aiming for an optimal exposure range (therapeutic window), at whatever individual dose required. Lowering the dose will certainly reduce the number of patients above the therapeutic window; but other patients will move to below the therapeutic window, depriving them of benefit (Fig. 1), while the number of patients within the therapeutic window may not change. Reduced toxicity with equal activity may then be celebrated as a success. But optimal it is not. From the imatinib exposure response relationships (4), the CML field has now come full circle with ponatinib which has a 48% CV interindividual pharmacokinetic variability, corresponding to a roughly 5-fold range in exposures when everyone is given the same dose (5).The plasma exposure of a 15-mg ponatinib dose increase imparts odds ratios of 1.63 for MR1, and 2.05 for ≥MR1 response. The exposure increase of 15 mg imparts a HR of 2.05 for arterial occlusive events (AOE, causing its temporary market withdrawal) and 1.31 for grade ≥3 thrombocytopenia (5). Decreasing the dose for everyone reduces risk of toxicity for some, and reduces probability of response for others. The updated dosing for ponatinib (45 then 15 mg) merely reduces the time some patients are exposed to toxic concentrations and has a limited impact on OAEs. Dosing individual patients to a therapeutic window would have resulted in a distribution of doses beyond 15–45 mg, and might have been both more tolerable and more active.The authors point to idiosyncratic side effect profiles of TKIs with effects in some patients and none in others, and also stress the need for response biomarkers, suggesting early molecular response, T-cell subsets, NK-cell activity, or combinations. We suggest they revisit the TDM principles already established with their first revolutionary drug imatinib. Plasma exposure may be the best biomarker yet and therapeutic windows should be part of drug labeling.See the Response, p. 237S.J. Salamone reports other support from Saladax Biomecical, Inc. outside the submitted work. No disclosures were reported by the other author.
2023-08-01·The British journal of psychiatry : the journal of mental science
Point of care assay for blood aripiprazole concentrations: development, validation and utility
Article
作者: Luiz Dratcu ; Philip McGuire ; Mary Rose Hilaire ; Salvatore J. Salamone ; David Taylor ; Edward Chesney ; Robert Harland ; Ana Catalan ; Thomas J. Reilly ; Matthew Atkins ; Irina Baburina ; Neville Desouza
Background:
The antipsychotic aripiprazole is often used in the treatment of first-episode psychosis. Measuring aripiprazole blood levels provides an objective measure of treatment adherence, but this currently involves taking a venous blood sample and sending to a laboratory for analysis.
Aims:
To detail the development, validation and utility of a new point of care (POC) test for finger-stick capillary blood concentrations of aripiprazole.
Method:
Analytical performance (sensitivity, precision, recovery and linearity) of the assay were established using spiked whole blood and control samples of varying aripiprazole concentration. Assay validation was performed over a 14-month period starting in July 2021. Eligible patients were asked to provide a finger-stick capillary sample in addition to their usual venous blood sample. Capillary blood samples were tested by the MyCare™ Insite POC analyser, which provided measurement of aripiprazole concentration in 6 min, and the venous blood sample was tested by the standard laboratory method.
Results:
A total of 101 patients agreed to measurements by the two methods. Venous blood aripiprazole concentrations as assessed by the laboratory method ranged from 17 to 909 ng/mL, and from 1 to 791 ng/mL using POC testing. The correlation coefficient between the two methods (r) was 0.96 and there was minimal bias (slope 0.91, intercept 4 ng/ml).
Conclusions:
The MyCare Insite POC analyser is sufficiently accurate and reliable for clinical use. The availability of this technology will improve the assessment of adherence to aripiprazole and the optimising of aripiprazole dosing.
2
项与 Saladax Biomedical, Inc. 相关的新闻(医药)2024-12-28
·汇聚南药
如果说最像美欧MNC的中国医药公司,恐怕莫非复星医药(600196.SH|02196.HK)了。
如果要更具象的类比,复星医药与强生这样的医药巨头成长路径有几分相似,尤其在多元化业务布局和全球扩展战略上,都是通过收购兼并玩转了制药、医疗器械和健康消费三个领域。
以复星医药系的整体布局看,除了A+H上市公司外,还控股复宏汉霖(02696.HK)、复锐医疗科技(01696.HK)两家港股上市公司,此外就是复星凯特、万邦生化医药、药友制药、南药股份、红旗制药、二叶制药、奥鸿药业、Gland Pharma Limited等一众国内外子公司。
这段时间,第十批国谈集采落地又引发了医药行业的大讨论。药企还是哀鸿一片,连创新药企都无法摆脱盈利艰难的窘境,但这也引发了另一个话题就是出海。
当国内药企终于将目光投向海外的时候,复星医药已经在海外市场征战多年了,说其是最具全球化视野的中国药企,并不为过。
从2024年中期财报的收入结构看,今年上半年公司营收204亿元,其中海外收入55亿元,同比提升15.13%,海外营收占比26.93%。
实际上往前捯二十年,复星医药就在谋划海外市场,早在2008年时其海外市场收入就一度冲上过25%。后来国内医药市场进入繁荣期,复星医药海外收入占比似乎没那么显山露水,但海外市场战略是其从未放弃的。
2018年,国内医药市场进入集采前夜,复星医药也再次将海外市场收入占比拉升到20%以上,并且在2021年一度冲上了34.86%。这也为公司对冲国内市场的内卷和政策冲击,带来了极大的缓冲。
横向对比,如复星医药这般国内TOP级的综合性药企,海外销售占比超过20%的,实则寥寥无几。
也因此,我们基于丰厚的海外市场运营经验和全球资源,判断在下一波中国药企出海潮起时,复星医药将会是中国式MNC的一个标杆。
壹|“小目标”
野蛮生长的原点
在2024年《胡润全球富豪榜》上,郭广昌以约315亿元人民币的财富位列榜单758位,只是相比2020年时,郭广昌的财富值已经“腰斩”。
不过,这并不妨碍时至今日复星医药仍旧是国内医药企业成长历程中最励志的故事之一。某种程度上,复星医药的成功代表着中国民营经济在医药行业的崛起。
时间回到1992年,复旦大学毕业留校工作的郭广昌正式辞职,以3.8万元创立上海广信科技发展有限公司开始创业生涯,主营信息咨询业务。
次年,公司收入就突破了100万元。而也正是在这一年,郭广昌就把目光转向房地产销售和生物医药领域。
哲学专业的他对生物医药不了解,便当即决定拉毕业于遗传工程学的校友梁信军、汪群斌、范伟组织团队进行制药研发,自此广信正式更名“复星”,外界解读为“复旦之星”。
1994年,复星房地产代理营收突破1000万元,同年上海复星实业股份有限公司(2004年改名复星医药)成立;1995年,复星研究三年的成果PCR乙型肝炎诊断试剂推向市场,年收入达1亿元,公司也由此成为上海第一家民营高科技企业。
复星医药实际控制人郭广昌 图源:互联网
自此,郭广昌启动开挂模式,医药也成为复星野蛮生长的原点。
成立4年后,1998年复星实业在上海证券交易所发行上市,募集3.575亿元资金。在当时IPO还实行总量控制的审批制,复星成了上海首家民营上市企业。
31岁的郭广昌叩开了资本市场的大门,也开启了其“中国巴菲特”的投资家之旅。
通过持续的资本运作和资产并购,复星迅速成为中国最大的民营企业之一,横跨医药、地产、钢铁、矿产、零售、媒体、游戏、证券、保险、期货、私募等领域。
2008年开始,郭广昌将目光投向了海外以及更广的产业,银行、影业、旅游、酒业……截至2023年12月31日,复星集团总资产达人民币8084亿元,由3.8万起家,构建起一个帝国,郭广昌用26年就创造了资本2.1亿倍扩张的神话。
了解复星的极速崛起之路,能够让我们对复星系医药产业发展逻辑多一分理解。
对于复星的发展,郭广昌认为得益于“在合适的时间做了合适的投资”,但生物制药赚来的第一个“小目标”是起点。
当前,复星主要战略聚焦健康、快乐、富足的幸福生态系统。健康板块聚焦医药产品、器械和诊断、健康服务及消费三大领域,医药产业可以说是复星核心中的核心。
贰|做对的事
复星医药的养成
回到医药产业,复星系医药目前仍然坚持的是“运营+投资”共生的路线,这和郭广昌的投资逻辑不无关系。
在郭广昌的理念里,永远强调最基本的投资逻辑就是做“对”的事情。
投资和收购的目的一定要清晰,当复星集团提供不了或者提供方案的速度太慢时,就会用投资或者收购的方式,将内外部资源打通,为客户提供“令人尖叫”的产品和服务。
这一点,在复星系医药发展历史中展现得淋漓尽致。
1998年复星实业上市后,就着手在医疗产业扩张。先是和全国部分省市约150家医院达成合作新建现代生物医学技术研究应用中心;接着通过上市募集到的资金,收购了上海五洋药业健康产品有限公司60%股权;投资控股上海永信维生素有限公司,收购上海创新科技公司,正式在生物医药行业打开局面。
2000年,复星和友谊集团成立了联华超市药房,逐步建立起庞大的线下分销网络;2002年,复星出资6831.68万元,收购了以仿制药业务出名的重庆药友51%的股权;2003年,复星并购了桂林南药,将其研发生产的中国001号新药—抗疟药青蒿琥酯收入囊中。同年,复星出资5亿元,拿下其国药控股49%股权。
2004年,复星又1.3亿收购了主营胰岛素药品的万邦医药75.2%的股权,又通过国药控股投资了一致药业;同年,复星实业更名为“复星医药”,开始将其他业务剥离上市主体,专注于医药健康产业,致力于医药产业链的资源整合。
图源:互联网
此后,复星医药开始在医疗服务与医疗器械方面布局,先是收购了佛山市禅城区中心医院,又收购了中国第一家外资医院和睦家医疗公司,接着把浙江迪安诊断、岳阳广济医院、安徽济民肿瘤医院、钟吾医院、南阳肿瘤医院等地方性医院也先后收入麾下。
2009年12月,复星医药与Henlix团队合资组建了复宏汉霖,正式开启创新药布局,生物制药的龙头地位正式站稳;2010年,复星医药与美中互利(北京)在香港共同成立美中互利医疗合资公司,在医疗器械领域持续发力。
在这个阶段上,复星医药参股的东富龙、金城医药、迪安诊断、佰利联等企业也陆续成功上市,复星医药的资本投资陆续收获果实。
如果说国内市场的风生水起让复星医药积累了资本经验,那海外业务的并购和投资,则让复星医药真正有了成为巨头的底气。
2013年,复星医药在以色列成立了子公司Sisram(复锐医疗科技),并以约2.2亿美元的价格收购了以色列医疗美容器械公司Alma Lasers Ltd. 95.2%的股权,布局海外医疗器械市场。
同一年,复星医药出资约2250万美元,认购了美国肿瘤检测公司Saladax 30%的股权,成为其单一最大的股东,布局抗癌产业链。
2016年,复星医药出资约1000万美元认购了硅谷呼吸疾病检测公司Spirosure约836万股C轮优先股,占Spirosure发行在外总股份的20.17%;复星和美国Intuitive Surgical(直观医疗器械公司)在中国境内成立了合资公司“复星医疗器械技术(上海)有限公司”,引进了新一代肺癌诊断与治疗机器人。
那一年,复星医药还创造了当时中国药企海外并购金额纪录,以12.6亿美元并购印度第一家获得美国FDA批准的注射剂药品生产制造企业Gland Pharma 86%的股权。
2017年,复星医药和关联方复星产业又共同收购了欧洲Breas公司呼吸机器械业务相关公司80%的股权。同年又收购主要从事专利药及仿制药研发、生产和销售的美国IPXL公司。
2020年,复星医药还投资了3.26亿元买入约158万股德国生物公司BioNTech的股票,BioNTech在新冠疫情发生后曾联合辉瑞公司开发了一款新冠疫苗,占据了欧美新冠疫苗市场大半江山,这笔投资也为复星医药带来了超过22亿元的收益。
2023年,复星医药之前收购的Gland Pharma公司又收购了欧洲公司Cenexi (专注于医药合同定制研发和生产服务)100%股权。
至此,复星医药的版图轮廓已经清晰展现。
从最初的生物医药公司,到现在的医药帝国,复星医药身上有着浓重的PE印记。也恰是如此,让复星医药系成为国内医药公司中最与众不同的。
叁|全球布局
规模并购与深度整合
近十年来,复星医药在海内外并购数量超过130起。
从国内走向国际市场的过程中,复星医药的策略并不仅仅是“大手笔并购”,更重要的是如何通过这些并购实现资源整合,最大化释放全球化带来的协同效应。
这也是复星医药走过跑马圈地阶段后,给行业最值得参考的答案。可以说复星医药是国内医药企业中,海外投资最多、涉猎品类最广的企业之一,因此也更具有参考性。
前文有说到,复星医药在2013年以2.2亿美元收购以色列Alma Lasers,首次大规模进入全球医疗器械市场。凭借Alma Lasers的先进医美设备制造经验,复星迅速拓展了在欧洲、亚洲等国际市场的版图。
另外一个案例是印度Gland Pharma,这笔并购完成后,复星医药获得了进入全球高端注射剂市场的机会。
当时Gland Pharma为了尽可能开拓全球市场,其制剂生产工厂依次取得了美国FDA、英国 MHRA、德国BGV、巴西国家卫生监督局(ANVISA)、澳大利亚治疗用品管理局 (TGA)、南非MCC(药品管理委员会)世界卫生组织和加拿大卫生部一系列监管机构的认证,在全球市场都有良好口碑。
图源:互联网
入主Gland Pharma后,复星医药保留了Gland Pharma的核心管理团队,并借助其生产线以及注册平台,进一步扩大了品牌的国际效应,进而曲线进入包括美国在内的海外市场。
此外,Gland Pharma公司的业务范围覆盖心脑血管、麻醉、抗感染和糖尿病等,核心产品包括肝素钠、依诺肝素钠注射液、罗库溴铵注射液、万古霉素和重组人胰岛素等多个领域。
这些资源与复星医药的创新药产品力结合,实现药品在印度的本土化和市场拓展。与此同时,Gland Pharma和很多全球知名药企都保持着长期合作,这也让复星医药能够迅速融入全球药品供应链网络。
仅仅4年,Gland Pharma正式宣布上市,此次募资额645亿卢比也被认为是印度制药公司规模最大的一次IPO。
今年6月20日,复星医药公告称,其控股子公司复星医药新加坡公司通过大宗交易出售所持有的990万股Gland Pharma股份(约占总股份6.01%),折合2.11亿美元,但复星医药仍保持对Gland Pharma的控股权。
这次并购对于复星医药的全球扩展来说都具有里程碑意义,极大提升了复星医药在全球仿制药和注射剂领域的竞争力。
在海外并购之外,复星医药在全球创新布局中的合作同样值得关注。
2017年,复星医药与美国凯特制药合作,成立了“复星凯特”,专注于开发前沿的CAR-T细胞免疫治疗。
这次合作带来了全球顶尖的抗肿瘤技术,也让复星医药迅速进入全球最先进的细胞治疗领域,尤其是在肿瘤治疗创新技术上完成了重要一跃。
2021年6月,复星凯特获批上市中国首款CAR-T细胞治疗产品——奕凯达®(阿基仑赛注射液),正式开启中国CAR-T治疗元年,实现了国内细胞治疗领域从“0”到“1”的突破。
图源:互联网
这种MNC式的“并购+整合+合作”全球化扩展模式,让复星医药逐步适应了全球市场的复杂性,可以视作中国式MNC的一种成长路径。
肆|“必选项”
中国MNC的探路者
在本土药企中,复星医药的独特性在于其通过市场化的并购策略和全球资本运作,在国际市场上逐步形成了自己的竞争力。
但复星医药和强生等传统MNC也不尽相同,最起码两者的驱动模式就不同。强生是研发技术驱动模式,依靠其长期的研发投入和技术积累,推动了全球市场的扩展,形成了独特的技术优势。
而复星医药则更偏重于资本驱动模式,并不依赖长期的技术积累,而是通过收购国际领先的医药企业和技术平台,快速弥补自身技术短板。
不管是通过并购以色列的Alma Lasers进入了全球医疗美容市场,还是收购Gland Pharma打入了高端注射剂市场,抑或是通过与BioNTech合作引进了mRNA疫苗技术。这些策略极具郭广昌的投资风格,哪里不足快速补哪里。
如果把复星医药单纯理解成一个医药投资型公司,也不全面。
因为复星医药并未完全依赖外部技术,而是通过这些并购逐步提升了自主研发能力。比如在抗肿瘤药物和生物制品领域,复星医药已经建立自己的研发体系。
此外,复宏汉霖作为复星医药的生物制药平台,也已经在全球范围内取得了一定的成绩,特别是在PD-1和HER2抗体药物的研发方面展现出强劲的竞争力。
而在两个点上,我们需要进一步观察复星医药:
一个是复星医药的成长动能更多是通过投资收益获取。数据显示,2021年至2023年,复星医药的投资收益分别为46.24亿元、43.78亿元、35.02亿元,同期归属净利润分别为47.29亿元、37.31亿元、23.86亿元,可见其盈利高度依赖投资收益。
图源:上市公司财报
在日趋紧张的国际地缘关系和逆全球化思潮中,对于复星医药乃至更多出海的中国药企来说,资产并购的难度也在肉眼可见的提升,而已并购的资产也需要进一步提升控制力与盈利能力。
其二,资本驱动模式可能带来高杠杆风险不可忽视。如何在保持并购扩展的同时降低财务压力,是复星医药着重需要思考的问题。
截至2024年6月末,复星医药担保总额已高达331.81亿元,占归属于上市公司股东的净资产的比例为74.12%(正常情况下不允许超过50%),一旦子公司暴雷,后果不堪设想。
图源:上市公司财报
无论如何,在国际化布局及资源整合方面,复星医药已经遥遥领先于其他本土药企,这对于其对冲国内发展环境的局促有着极为重要的意义。
目前,复星医药拥有近1000人的海外商业化团队,覆盖美国、欧洲、非洲等海外市场,致力于成为全球领先的医疗创新整合者。毫无疑问,其海外扩张的每一步,都将是中国医药行业出海的经验累积。
喜欢我们文章的朋友点个“在看”和“赞”吧,不然微信推送规则改变,有可能每天都会错过我们哦~
免责声明
“汇聚南药”公众号所转载文章来源于其他公众号平台,主要目的在于分享行业相关知识,传递当前最新资讯。图片、文章版权均属于原作者所有,如有侵权,请在留言栏及时告知,我们会在24小时内删除相关信息。
信息来源:原创 王金星 多肽链
往期推荐
本平台不对转载文章的观点负责,文章所包含内容的准确性、可靠性或完整性提供任何明示暗示的保证。
财报并购
2023-09-11
DUBLIN, Sept. 11, 2023 /PRNewswire/ -- The "Immunoassay Markets. Strategies and Trends. Forecasts by Application, Technology, Product, User and by Country. With Executive Guides, Customized Forecasting and Analysis. 2023 to 2027" report has been added to
ResearchAndMarkets.com's offering.
In the ever-evolving landscape of the diagnostic industry, immunoassay is emerging as a steadfast workhorse, finding new relevance driven by the demands of the ongoing pandemic. The need for rapid, easily accessible diagnostics has propelled immunoassay to the forefront, as it adapts and advances in response to shifting market dynamics.
Advancements in genetic knowledge are opening up new avenues for immunoassay technologies, with multiplex capabilities becoming the standard. This transformation extends to rapid diagnostics, point-of-care solutions, biomarker exploration, and the expanding consumer market, while traditional immunoassay methods continue to hold a strong position within the growing realm of clinical diagnostics.
Within the realm of immunoassay instrumentation, multiple factors are fueling growth, including ongoing diagnostic breakthroughs, the retirement of older instruments driven by evolving technologies, wider consumer adoption, and the maturation of immunity-related technology.
However, these opportunities are not without their challenges. Heightened competition is exerting downward pressure on prices, while the threat from PCR-based instruments looms. Lower barriers to entry and potential drawbacks associated with wellness trends also present limitations to growth.
This dynamic landscape is characterized by enduring instruments, industry structures in flux due to declining instrument costs, and meticulous instrument specifications, which play a pivotal role in shaping the field. Innovations like CRISPR diagnostics further contribute to the evolving immunoassay landscape.
With profiles of over 60 companies, spanning both large and small players in this field, this comprehensive report offers invaluable insights into the pitfalls and opportunities that define the immunoassay industry. It equips stakeholders to make informed investment decisions and valuations, providing the latest data to navigate this ever-changing landscape with confidence.
Key Topics Covered:
Industry Overview
Players in a Dynamic Market
Academic Research Lab
Diagnostic Test Developer
Instrumentation Supplier
Chemical/Reagent Supplier
Pathology Supplier
Independent Clinical Laboratory
Public National/regional Laboratory
Hospital Laboratory
Physicians Office Lab (POLS)
Audit Body
Certification Body
The Clinical Laboratory Market Segments
Traditional Market Segmentation
Laboratory Focus and Segmentation
Hospital Testing Share
Economies of Scale
Hospital vs. Central Lab
Physician Office Lab's
Physician's and POCT
Immunoassay - Markets and Discussion
Instruments - Genetics changes the picture
RIA - A Technology Shows its Age
Immunoassay vs. PCR vs. Sequencing - A See Saw Battle
The Smart Shrinking Instrument - Serious Implications
Research Funding and Capital Expense - Instrument Pooling
Multiplex vs. POC - A Tradeoff Analysis
Reagents and Kits - Genetics changes the picture
Bigger Test Menus a Boon for Kit Market
Physician Office Labs - A New Frontier
Rapid and POCT to Threaten Instrument Markets
OTC and DTC - Huge Market Potential
Economies of Scale. Going Away?
Lower Barriers to Entry for Instruments/Analyzers
Miniturization and Technology Drive Acquisition
Immunoassay Recent Developments
Recent Developments - Importance and How to Use This Section
EDP Biotech, New Day Diagnostics to Merge
Sorrento Therapeutics Nabs Contract for Dx Platform
Beckman Coulter Diagnostics DxI 9000 Access Immunoassay Analyzer
Qorvo Eyes Multiplex Immunoassay
BioMerieux Launches New Products
Senzo to Commercialize Infectious Disease Lateral Flow Tests
Nanomix Plans Instrument, Test Launches
Startup GLX Analytix Prepares for Commercialization
Nonagen Gets CE Mark for Bladder Cancer Immunoassay
Qualigen Acquires Majority Stake in NanoSynex
Saladax Biomedical Using Immunoassay Dx
Prolight Diagnostics to Acquire Psyros Diagnostics
Quidel to Acquire Ortho Clinical Diagnostics
FDA Grants EUA to Xtrava Health
Alamar Biosciences Develops Immuno-Sandwich Platform
FDA grants breakthrough device to multiplex immunoassay
Quidel, Beckman Settle Cardiac Immunoassay Dispute
BGI Americas, Advaite Form SARS-CoV-2 Testing Partnership
BioMerieux Gets CE Mark for Three Dengue Immunoassays
COVID-19 Portfolio to Accelerate At-Home Infectious Disease Testing
Roche Diagnostics Expanding Testing Portfolio in 2021
PerkinElmer Long-Term Outlook
Quidel Updates Outlook for C19 Testing
Dx Companies Look at Multiplex Tests for SARS-CoV-2, Influenza
Becton Dickinson and NAT Diagnostics Acquisition
Market Trends
Factors Driving Growth
Diagnostic Factors
Changing Technologies Spur Early Instrument Retirement
Consumer Channels Open Wider
Immunity Technology Comes of Age
Factors Limiting Growth
Increased Competition Lowers Price
Threat from PCR Based Instruments
Lower Barriers to Entry
Wellness has a downside
Immunoassay Instrumentation
Instrumentation Tenacity
Declining Cost of Instruments Changes Industry Structure
LISTING of INSTRUMENT SPECIFICATIONS
Immunoassay - CRISPR Diagnostics
Market Guides
Immunoassay Market - Strategic Situation Analysis
Guide for Executives, Marketing, Sales and Business Development Staff
Guide for Management Consultants and Investment Advisors
Market Definition
Immunoassay Markets Definition In This Report
Enzyme Based
Immunofluorescence
Chemiluminescence
DNA/NAT
RIA & Other
Reagents/Kits, Analyzers, Software & Services
Infectious Disease
Auto Immune
Endocrinology
Oncology
Cardiology
Other Specialty
Market Definition
Methodology
Perspective: Healthcare and the IVD Industry
Global Healthcare Spending
Spending on Diagnostics
Important Role of Insurance for Diagnostics
Appendices
United States Medicare System: Laboratory Fees Schedule
The Most Used IVD Assays
The Highest Grossing Assays
Profiles of Key Companies
Abbott Laboratories
Abcam
Abionic
Accel Diagnostics
Applied BioCode
Arlington Scientific
Arrayit Corporation
Atomo Diagnostics
Aureum Diagnostics
Aurora Biomed
Autobio Diagnostics
AVIVA Systems Biology
Awareness Technology
Axis-Shield Diagnostics Ltd.
Beckman Coulter Diagnostics
Becton, Dickinson and Company
Biocartis
Biomatik
bioMerieux Diagnostics
Bioneer Corporation
Bio-Rad Laboratories, Inc.
BioTek Instruments
Boditech Med, Inc
Boster Biological Technology
Diamedix (Erba Diagnostics)
Diasorin S.p.A.
Dynex Technologies
Enzo Biochem
Eurofins Scientific
FUJIFILM Wako Diagnostics
Fujirebio
Gold Standard Diagnostics
Grifols
Hycor Biomedical
Immunodiagnostic Systems (IDS)
Immunodiagnostik AG
Inova Diagnostics
JR Biomedical
Luminex Corp
Maxim Biomedical
Mbio Diagnostics
Meso Scale Discovery
Millipore Sigma
Mindray
Molecular Devices
MP Biomedical
Operon
Ortho Clinical Diagnostics
Perkin Elmer
Qiagen
Quidel
R&D Systems
Randox Toxicology
Roche Molecular Diagnostics
SD Biosensor
Siemens Healthineers
Sysmex
Tecan
Thermo Fisher Scientific Inc.
TOSOH Bioscience
Veredus Laboratories
Vircell
YD Diagnostics
Zhejiang Orient Gene Biotech
Scope of the Report
Global Market by Application
Endocrinology Applications
Immune Applications
Oncology Applications
Infectious Disease Applications
Cardiology Applications
Other Applications
Immunoassay by Technology
Enzyme
Flourescence
Chemiluminescence
Nucleic Acid
Rapid/POC
Other Technology
Immunoassay by Product
Instrument
Reagents
Services
Immunoassay by User
Hospital
Outpatient Lab
POC/Other
12 Vision of the Future of Immunoassay
For more information about this report visit
About ResearchAndMarkets.com
ResearchAndMarkets.com is the world's leading source for international market research reports and market data. We provide you with the latest data on international and regional markets, key industries, the top companies, new products and the latest trends.
Media Contact:
Research and Markets
Laura Wood, Senior Manager
[email protected]
For E.S.T Office Hours Call +1-917-300-0470
For U.S./CAN Toll Free Call +1-800-526-8630
For GMT Office Hours Call +353-1-416-8900
U.S. Fax: 646-607-1907
Fax (outside U.S.): +353-1-481-1716
Logo:
SOURCE Research and Markets

并购诊断试剂免疫疗法
100 项与 Saladax Biomedical, Inc. 相关的药物交易
登录后查看更多信息
100 项与 Saladax Biomedical, Inc. 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年05月01日管线快照
无数据报导
登录后保持更新
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
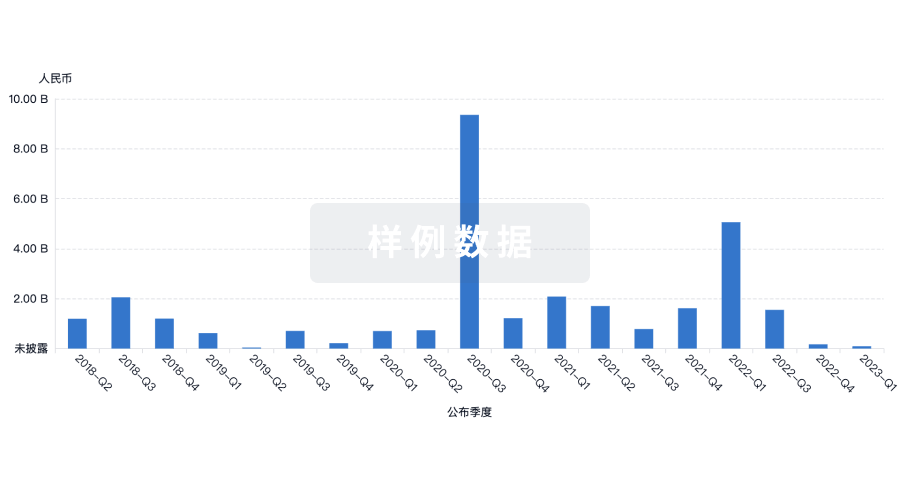
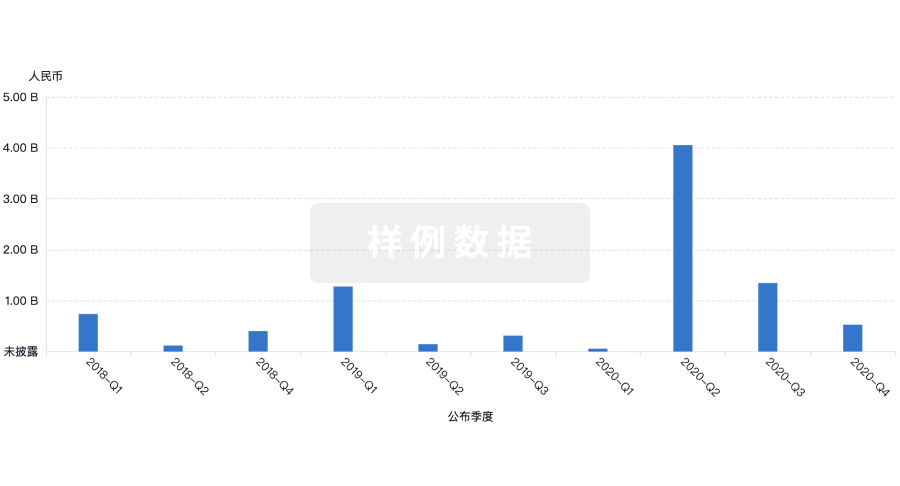
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
