预约演示
更新于:2026-02-02
Maquet Critical Care AB
更新于:2026-02-02
概览
关联
5
项与 Maquet Critical Care AB 相关的临床试验NCT06114992
Servo-n High-Frequency Oscillatory Ventilation in Clinical Practice: A Prospective, Observational, Single-arm and Multi-center Study
The purpose of this study is to evaluate the safety and performance of High-Frequency Oscillatory Ventilation (HFOV) modes of the Servo-n ventilator in neonates and infants, by using a prospective, observational, single-arm (i.e., non-controlled) and multi-center Post-Market Follow-up (PMCF) study design. HFOV treatment will be evaluated by assessing ventilation and oxygenation variables, and safety will be evaluated by documentation of device related adverse events.
开始日期2024-07-15 |
申办/合作机构 |
NCT06249009
Impact of Increasing Flow Rates in High-flow Nasal Cannula and CPAP on Diaphragmatic Work in Newborn and Paediatric Population: Non-inferiority Study
The goal of this randomised controlled, cross-over clinical trial is to compare High Flow Nasal Cannulas (HFNC) and Continuous Positive Airways Pressure (CPAP) in neonates over 34 weeks' amenorrhoea (SA) up to children weighing less than 20 kg with respiratory failure.
The main question it aims to answer is the non-inferiority of high flows of high-flow nasal cannula compared with CPAP by analysis of diaphragmatic contraction (EAdi (Electrical activity of diaphragm)).
Participants with respiratory failure and need of non invasive ventilation and nasogastric tube will receive 4 different increasing flows of HFNC and Positive End-Expiratory Pressure of 7 cmH2O with CPAP during 30 minutes for each flow rate and CPAP. The electrical activity of diaphragm and clinical data of the patient upon each flow and support will be collected. According to the cross-over procedure, the patients will change groups (increasing flows of HFNC or CPAP) in order to perform the remaining analysis.
The main question it aims to answer is the non-inferiority of high flows of high-flow nasal cannula compared with CPAP by analysis of diaphragmatic contraction (EAdi (Electrical activity of diaphragm)).
Participants with respiratory failure and need of non invasive ventilation and nasogastric tube will receive 4 different increasing flows of HFNC and Positive End-Expiratory Pressure of 7 cmH2O with CPAP during 30 minutes for each flow rate and CPAP. The electrical activity of diaphragm and clinical data of the patient upon each flow and support will be collected. According to the cross-over procedure, the patients will change groups (increasing flows of HFNC or CPAP) in order to perform the remaining analysis.
开始日期2023-11-27 |
NCT05574829
Assessment of Neural Pressure Support Assisted Ventilation and Non-invasive Estimation of Transpulmonary Pressure in Spontaneous Ventilation Modes
The transition from controlled mechanical ventilation to assisted ventilation is one of the most complex and compromised phases of the ventilatory management during mechanical ventilation, affected by factors such as:
* Asynchronies, due to patient-respirator dis-synchrony in ins- and expiratory neural and mechanical times, as well as inadequate levels of assistance.
* Risks of self-induced lung injury resulting from uncontrolled increases in transpulmonary pressure when high inspiratory efforts are combined with inappropriate levels of inspiratory pressure assistance.
Current monitoring of assisted ventilation is complex and not well resolved by most conventional ventilators. Asynchronies are difficult to monitor with the pressure or flow/time curves present in conventional ventilators requiring an advanced level of expertise. Measurements of the patient's muscular effort and therefore of transpulmonary pressure, requires the use of esophageal manometry with cumbersome handling and interpretation.
NAVA (Neurally Adjusted Ventilatory Assist) is a ventilator mode that uses electrical activity of the diaphragm (EAdi), monitored via a modified nasogastric feeding catheter, to control and assist the respiratory cycle by the ventilator. Recently, a "hybrid" mode between the conventional pressure support assisted mode (PSV) and NAVA called Neural-Pressure Support Ventilation (N-PSV) has been developed. This mode uses a neural trigger based on the EAdi to match the patient's and ventilator's in- and expiratory time, but unlike NAVA, assisting in the same way as in pressure support. In addition the EAdi allows to assess the extent to which the patient's muscle strength contributes to the patient-ventilator breath (PVBC), and it has recently been suggested that on the basis of PVBC it may also be possible to directly estimate the patient's transpulmonary pressure (PL).
Hypothesis:
1. EAdi allows direct estimation of PL during the assisted ventilation phase without the need of an oesophageal pressure balloon.
2. N-PSV can provide advantages over PSV by better matching ventilator and patient respiratory cycle times, thus reducing the risk of asynchronies.
* Asynchronies, due to patient-respirator dis-synchrony in ins- and expiratory neural and mechanical times, as well as inadequate levels of assistance.
* Risks of self-induced lung injury resulting from uncontrolled increases in transpulmonary pressure when high inspiratory efforts are combined with inappropriate levels of inspiratory pressure assistance.
Current monitoring of assisted ventilation is complex and not well resolved by most conventional ventilators. Asynchronies are difficult to monitor with the pressure or flow/time curves present in conventional ventilators requiring an advanced level of expertise. Measurements of the patient's muscular effort and therefore of transpulmonary pressure, requires the use of esophageal manometry with cumbersome handling and interpretation.
NAVA (Neurally Adjusted Ventilatory Assist) is a ventilator mode that uses electrical activity of the diaphragm (EAdi), monitored via a modified nasogastric feeding catheter, to control and assist the respiratory cycle by the ventilator. Recently, a "hybrid" mode between the conventional pressure support assisted mode (PSV) and NAVA called Neural-Pressure Support Ventilation (N-PSV) has been developed. This mode uses a neural trigger based on the EAdi to match the patient's and ventilator's in- and expiratory time, but unlike NAVA, assisting in the same way as in pressure support. In addition the EAdi allows to assess the extent to which the patient's muscle strength contributes to the patient-ventilator breath (PVBC), and it has recently been suggested that on the basis of PVBC it may also be possible to directly estimate the patient's transpulmonary pressure (PL).
Hypothesis:
1. EAdi allows direct estimation of PL during the assisted ventilation phase without the need of an oesophageal pressure balloon.
2. N-PSV can provide advantages over PSV by better matching ventilator and patient respiratory cycle times, thus reducing the risk of asynchronies.
开始日期2022-05-20 |
100 项与 Maquet Critical Care AB 相关的临床结果
登录后查看更多信息
0 项与 Maquet Critical Care AB 相关的专利(医药)
登录后查看更多信息
19
项与 Maquet Critical Care AB 相关的文献(医药)2025-09-12·JOURNAL OF CLINICAL MONITORING AND COMPUTING
Towards reliable prediction of intraoperative hypotension: a cross-center evaluation of deep learning-based and MAP-derived methods.
Article
作者: Jacobsson, Martin ; Björne, Håkan ; Lundström, Niclas ; Winski, Greg ; Chaari, Nada ; Hallbäck, Magnus
Intraoperative hypotension (IOH) is associated with an increased risk of heart and kidney complications. Although AI tools aim to predict IOH, their real-world reliability is often overstated due to biased data selection. This study introduces a framework to enhance reliability by: (1) including borderline blood pressure cases (65-75 mmHg, the "Gray Zone"), (2) comparing AI model to simple blood pressure threshold, and (3) validating across diverse surgical cohorts, centers and demographics. Using datasets from Karolinska University Hospital (Sweden) and VitalDB (Korea), we found AI model performs better than MAP threshold method in more ambiguous cases. In contrast, when hypotensive and non-hypotensive cases had clearly separated MAP values, both methods performed similarly well. Cross-validation revealed asymmetric generalizability: models trained on datasets containing more borderline (Gray Zone) cases generalized better to datasets with clearer class separation, whereas the reverse struggled. To ensure fair model comparison and reduce dataset-specific bias, we standardized the MAP difference between positive (hypotension) and negative (non-hypotension) samples at the time of prediction. This virtually eliminated the class separation and demonstrated that inflated performance in some datasets can be attributed to selection bias rather than true model generalizability. Age also influenced generalization: Cross-age validation revealed models trained on older patients generalized better to younger cohorts, whereas differences in ASA classification had minimal effect. These findings highlight the need for realistic validation to bridge the gap between AI research and clinical practice.
2024-10-01·ANESTHESIA AND ANALGESIA
Validation of a Novel Method for Noninvasive Mixed Venous Oxygen Saturation Monitoring in Anesthetized Children
Article
作者: Steiner, Kristoffer ; Karlsson, Jacob ; Andersson, Andreas ; Wallin, Mats ; Sjöberg, Gunnar ; Svedmyr, Anders ; Lönnqvist, Per-Arne ; Hallbäck, Magnus
BACKGROUND::
Mixed venous oxygen saturation (SvO2) is a critical variable in the assessment of oxygen supply and demand but is rarely used in children due to the invasive nature of pulmonary artery catheters. The aim of this prospective, observational study was to investigate the accuracy of noninvasively measured SvO2 acquired by the novel capnodynamic method, based on differential Fick equation (Capno-SvO2), against gold standard CO-oximetry.
METHODS::
Capno-SvO2 was compared to SvO2 measured by pulmonary artery blood gas CO-oximetry in children undergoing cardiac catheter interventions and subjected to moderate hemodynamic challenges. Bland-Altman analysis was used to describe the agreement of absolute values between CO-oximetry and Capno-SvO2, and a concordance rate was calculated to evaluate the ability of Capno-SvO2 to track change.
RESULTS::
Twenty-five procedures were included in the study. Capno-SvO2 showed a bias toward CO-oximetry of +3 percentage points; upper and lower limits of agreement were +11 percentage points (95% confidence interval [CI], 9–14) and −5 percentage points (95% CI, −8 to −3), respectively. The concordance rate was 92% (95% CI, 89–96).
CONCLUSIONS::
In conclusion, this first clinical application of a novel concept for noninvasive SvO2 monitoring without the need for a pulmonary artery catheter indicates that Capno-SvO2 generates absolute values and trending capacity in close agreement with the gold standard reference method.
2023-12-01·Journal of clinical monitoring and computing
Capnodynamic monitoring of lung volume and pulmonary blood flow during alveolar recruitment: a prospective observational study in postoperative cardiac patients
Article
作者: Hallbäck, M ; Aneman, A ; McCanny, P ; Schulz, L F ; Iftikhar, H ; Austin, D ; Stewart, A ; Wallin, M ; O'Regan, W ; Keleher, E
Alveolar recruitment manoeuvres may mitigate ventilation and perfusion mismatch after cardiac surgery. Monitoring the efficacy of recruitment manoeuvres should provide concurrent information on pulmonary and cardiac changes. This study in postoperative cardiac patients applied capnodynamic monitoring of changes in end-expiratory lung volume and effective pulmonary blood flow. Alveolar recruitment was performed by incremental increases in positive end-expiratory pressure (PEEP) to a maximum of 15 cmH2O from a baseline of 5 cmH2O over 30 min. The change in systemic oxygen delivery index after the recruitment manoeuvre was used to identify responders (> 10% increase) with all other changes (≤ 10%) denoting non-responders. Mixed factor ANOVA using Bonferroni correction for multiple comparisons was used to denote significant changes (p < 0.05) reported as mean differences and 95% CI. Changes in end-expiratory lung volume and effective pulmonary blood flow were correlated using Pearson's regression. Twenty-seven (42%) of 64 patients were responders increasing oxygen delivery index by 172 (95% CI 61-2984) mL min-1 m-2 (p < 0.001). End-expiratory lung volume increased by 549 (95% CI 220-1116) mL (p = 0.042) in responders associated with an increase in effective pulmonary blood flow of 1140 (95% CI 435-2146) mL min-1 (p = 0.012) compared to non-responders. A positive correlation (r = 0.79, 95% CI 0.5-0.90, p < 0.001) between increased end-expiratory lung volume and effective pulmonary blood flow was only observed in responders. Changes in oxygen delivery index after lung recruitment were correlated to changes in end-expiratory lung volume (r = 0.39, 95% CI 0.16-0.59, p = 0.002) and effective pulmonary blood flow (r = 0.60, 95% CI 0.41-0.74, p < 0.001). Capnodynamic monitoring of end-expiratory lung volume and effective pulmonary blood flow early in postoperative cardiac patients identified a characteristic parallel increase in both lung volume and perfusion after the recruitment manoeuvre in patients with a significant increase in oxygen delivery.Trial registration This study was registered on ClinicalTrials.gov (NCT05082168, 18th of October 2021).
1
项与 Maquet Critical Care AB 相关的新闻(医药)2025-07-21
This
recall
involves updating instructions for using devices, and does not involve removing them from where they are used or sold.
The FDA has identified this recall as the most serious type. This device may cause serious injury or death if you continue to use it without following the updated instructions.
Affected Product
Product Names: Servo Ventilator Systems (Servo-u, Servo-n, and Servo-u MR devices)
Model/Unique Device Identifier (UDI): 6694800/07325710001110, 6688600/07325710001042, and 6888800/07325710010518
What to Do
All Servo-u, Servo-n, and Servo-u MR ventilators are recommended to be configured with “Extended leakage test” set to “Off”; see chapter 8.2.4 Configuration in the user’s manuals.
All users are recommended to follow the updated instructions for use of the user’s manuals chapter 9.5.1 Patient circuit test, in appendix 1.
On May 30, 2025, Maquet Critical Care AB sent all affected customers an urgent medical device correction letter recommending the following actions:
Ensure all affected devices in your inventory have been properly addressed.
Ensure this message is forwarded to any individuals that need notification within your organization or any organization where the affected devices have been transferred.
Reason for Updates to Use Instructions
Maquet Critical Care AB, a subsidiary of Getinge, is updating use instructions for Servo Ventilator Systems due to risk of inaccurate compliance measurement leading to improper tidal volume delivery in neonatal patients.
The Servo ventilator systems can be used with several different patient circuits and active humidifiers. Before being used on a patient, the ventilator must pass a safety check that measures leakage, compliance, and resistance in the circuit. Some humidifiers may not pass the standard leak test due to their design, even if there’s no actual leak. To address this, there is an optional configuration for the ventilator with an “Extended leakage test” in the ventilator’s Service & Settings menu.
This extended test should only be used with humidifiers that cannot pass the standard leak test. If a hospital uses multiple types of humidifiers, there’s a risk that the ventilator could be set to the wrong test for the humidifier in use.
If a ventilator is configured for the extended leakage test but used with an active humidifier that doesn’t require it, it may result in:
In Pressure Control mode: The displayed tidal volume may be higher than the volume actually delivered.
In PRVC mode: The ventilator may deliver a lower tidal volume than what is set and displayed.
When using tidal volumes of 5 mL or less in PRVC mode, there can be up to a 50% difference between the displayed and actual delivered volume. This may lead to hypoventilation and hypoxia, though these issues should be detected by external monitoring and alarms.
The use of affected product may cause serious adverse health consequences, including not enough oxygen (hypoxia) and too much carbon dioxide (hypercapnia) in extremely premature neonates.
There has been one reported injury. There have been no reports of death.
Device Use
A continuous ventilator (respirator) is a device intended to mechanically control or assist patient breathing by delivering a predetermined percentage of oxygen in the breathing gas.
The Servo-u Ventilator System is:
intended for respiratory support, monitoring, and treatment of neonatal, pediatric, and adult patients
to be used only by healthcare providers
to be used only in professional healthcare facilities and for transport within these facilities
The Servo-n Ventilator System is:
intended for respiratory support, monitoring, and treatment of neonatal and pediatric patients
to be used only by healthcare providers
to be used only in professional healthcare facilities and for transport within these facilities
The Servo-u MR Ventilator System is:
intended for respiratory support, monitoring, and treatment of neonatal, pediatric and adult patients
to be used only by healthcare providers
to be used only in professional healthcare facilities and for transport within these facilities
to be used in MR environment according to specified conditions
with 1.5 T or 3 T MR scanners
outside magnetic fields >20 mT/200 Gauss
Contact Information
Customers in the U.S. with questions about this recall should contact technical services at 1-888-943-8872, Option 4, Monday through Friday, between the hours of 8:00 a.m. and 6:00 p.m. ET
Additional FDA Resources:
Unique Device Identifier (UDI)
The unique device identifier (UDI) helps identify individual medical devices sold in the United States from manufacturing through distribution to patient use. The UDI allows for more accurate reporting, reviewing, and analyzing of adverse event reports so that devices can be identified, and problems potentially corrected more quickly.
How do I report a problem?
Health care professionals and consumers may
report adverse reactions or quality problems
they experienced using these devices to MedWatch: The FDA Safety Information and Adverse Event Reporting Program.
Content current as of:
07/21/2025
Legal Disclaimer:
EIN Presswire provides this news content "as is" without warranty of any kind. We do not accept any responsibility or liability
for the accuracy, content, images, videos, licenses, completeness, legality, or reliability of the information contained in this
article. If you have any complaints or copyright issues related to this article, kindly contact the author above.
100 项与 Maquet Critical Care AB 相关的药物交易
登录后查看更多信息
100 项与 Maquet Critical Care AB 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年02月08日管线快照
无数据报导
登录后保持更新
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
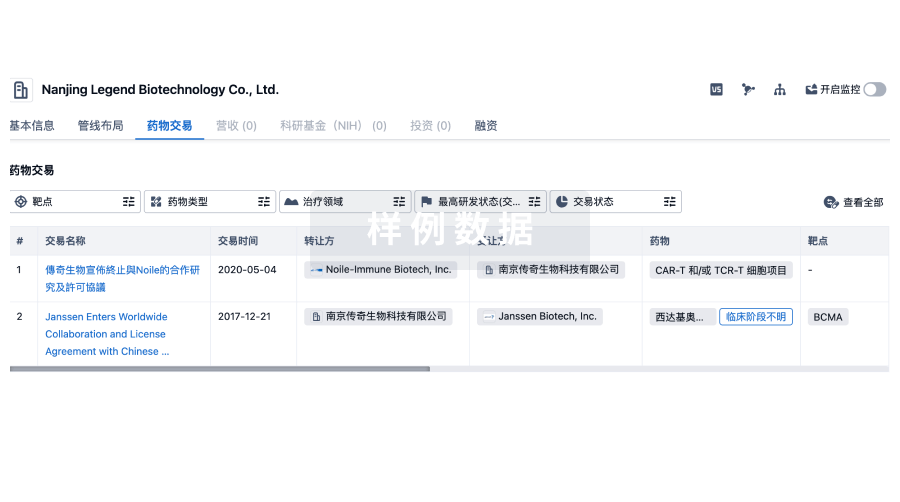
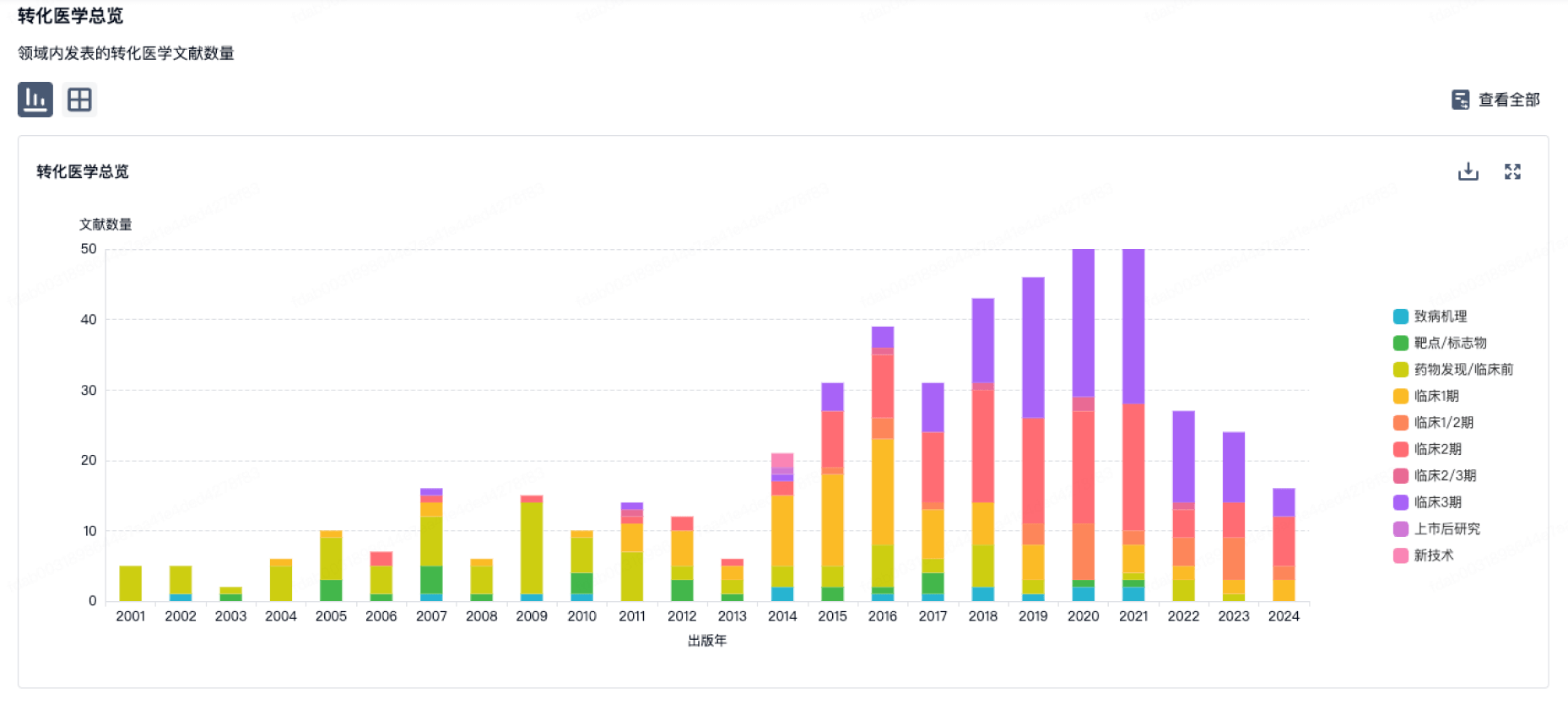
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
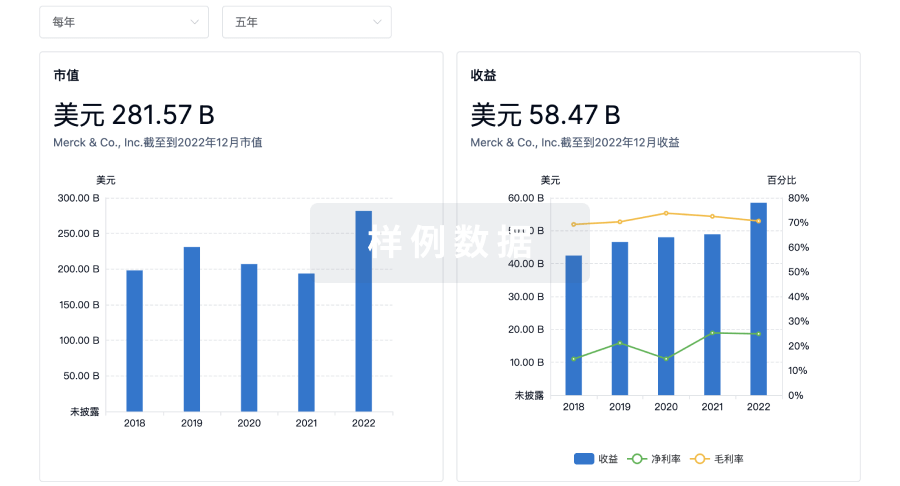
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
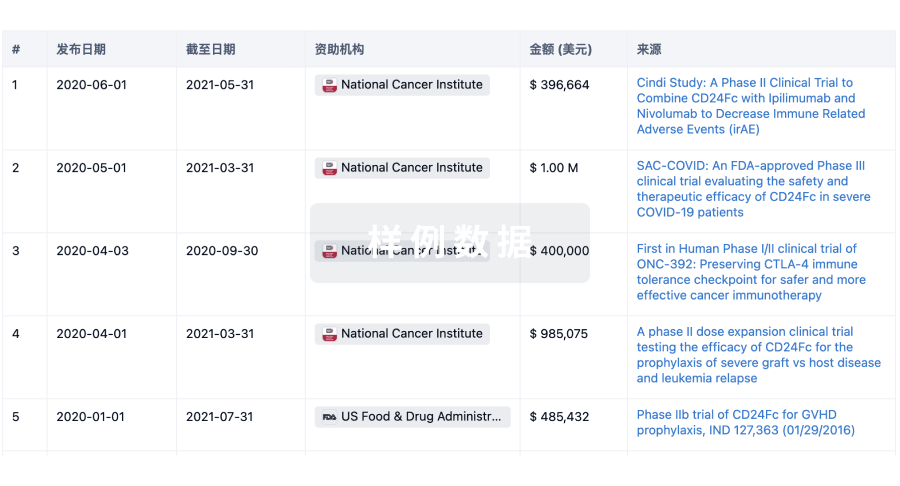
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
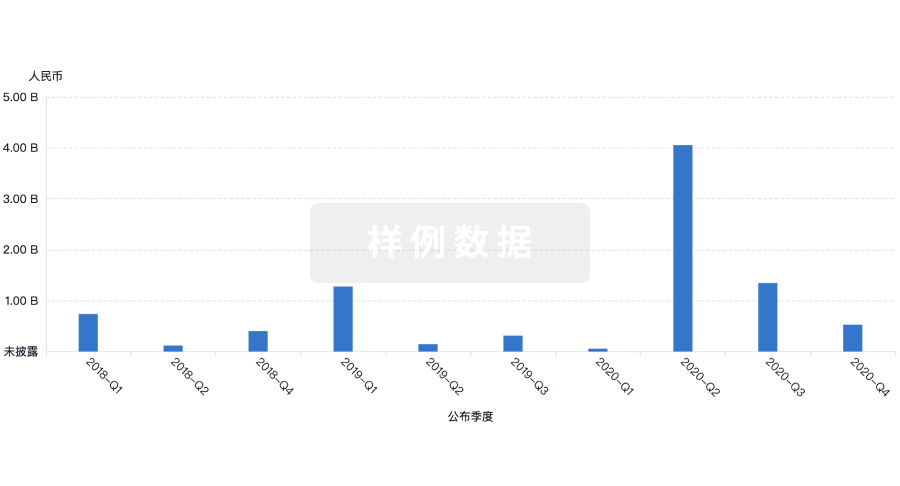
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
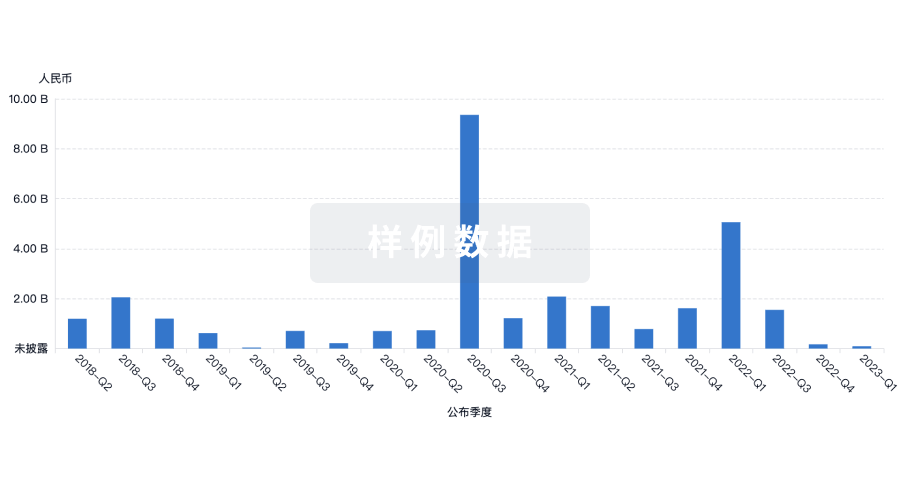
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用