预约演示
更新于:2025-08-29

Hospital General de México
更新于:2025-08-29
概览
关联
53
项与 Hospital General de México 相关的临床试验NCT06786364
Types of Photoplethysmographic Waves in Adult Patients with Septic Shock
The objective of this study is to identify the types of Photoplethysmographic waves present in adults with septic shock and determine whether these waves correlate with other variables of tissue hypoperfusion such as capillary refil, serum lactate and mottling score.
开始日期2024-11-01 |
申办/合作机构 |
NCT06622538
Orotracheal Intubation with the ORION Videolaryngoscope Versus the King Vision Videolaryngoscope in Adult Patients Without Predictors of a Difficult Airway
This study aims to compare the ORION video laryngoscope with the King Vision video laryngoscope for orotracheal intubation in patients without predictors of difficult airway scheduled for elective surgery under general anesthesia.
开始日期2024-10-01 |
申办/合作机构 |
NCT06589973
IImpact of Clinical and Biochemical Variables on Mortality and Morbidity of Patients With Alcohol Withdrawal Syndrome Under Treatment According to the CIWA-AR Scale"
The goal of this observational study is to describe the impact measured through the Odds Ratio (OR) of different variables of clinical and biochemical alterations on the duration of the syndrome alcohol withdrawal patients measured in days of symptoms and stay; it could include any patients with a diagnosis of admission of alcohol withdrawal syndrome (AWS) who have been treated in the department of Internal Medicine for 5 years.
The main question it aims to answer is: What is the relationship between the different clinical, biochemical, and hematic factors on the duration of symptoms, morbidity, and mortality in individuals with alcohol syndrome withdrawal?
• If the patient has a greater number of risk factors, such as advanced age, a long and chronic history of alcohol consumption, the type of distillate consumed, as well as the deterioration of liver function and presence of leukocytosis and neutrophilia, then it is postulated that the duration of alcohol withdrawal syndrome will be longer.
Clinical records will be used to describe the proportion of complications associated with alcohol withdrawal syndrome including pneumonia bronchial aspiration, seizures, need for mechanical ventilation, digestive tract hemorrhage, toxic-alcoholic hepatitis, and pancreatitis.
The main question it aims to answer is: What is the relationship between the different clinical, biochemical, and hematic factors on the duration of symptoms, morbidity, and mortality in individuals with alcohol syndrome withdrawal?
• If the patient has a greater number of risk factors, such as advanced age, a long and chronic history of alcohol consumption, the type of distillate consumed, as well as the deterioration of liver function and presence of leukocytosis and neutrophilia, then it is postulated that the duration of alcohol withdrawal syndrome will be longer.
Clinical records will be used to describe the proportion of complications associated with alcohol withdrawal syndrome including pneumonia bronchial aspiration, seizures, need for mechanical ventilation, digestive tract hemorrhage, toxic-alcoholic hepatitis, and pancreatitis.
开始日期2024-09-09 |
申办/合作机构 |
100 项与 Hospital General de México 相关的临床结果
登录后查看更多信息
0 项与 Hospital General de México 相关的专利(医药)
登录后查看更多信息
1,358
项与 Hospital General de México 相关的文献(医药)2025-11-01·ARCHIVES OF MEDICAL RESEARCH
Changing Landscape of Liver Cirrhosis Etiologies
Article
作者: Cortez-Hernández, Carlos ; Guzmán-Rodríguez, Nubia ; Castillo-Barradas, Mauricio ; Monsiváis-Morales, Juan D ; Remes-Troche, José M ; González-Huezo, María S ; Cornejo-Hernández, Stefanny ; Higuera-de-la-Tijera, Fatima ; Ramírez-Mejía, Mariana M ; Zheng, Ming-Hua ; Tovar-Bojorquez, Elianee M ; Barranco-Fragoso, Beatriz ; Cerda-Reyes, Eira ; Valentin-Cortez, Francisco J ; Cano-Contreras, Ana D ; Pérez-Hernández, José L ; Contreras-Omaña, Raúl ; Córdova-Gallardo, Jacqueline ; Méndez-Sánchez, Nahum ; Montalvo-Gordon, Iaarah ; Borbolla-Schega, Itziar ; Sandez-Araiza, Adrian ; Sabanes-Hernández, Montserrat ; Chávez-Tapia, Norberto ; Lozano-Salazar, Rubén R ; Rodríguez-Hernández, Heriberto
BACKGROUND AND AIMS:
Liver cirrhosis is a major public health problem worldwide. In Mexico, the increased prevalence of obesity and type 2 diabetes mellitus (T2DM) has contributed to an increase in the prevalence of metabolic dysfunction-associated steatotic liver disease (MASLD). This study examines the current etiologies of cirrhosis in Mexico, highlighting regional and demographic differences.
METHODS:
We conducted a multicenter cross-sectional study of 2182 patients with cirrhosis diagnosed between 2018 and 2024 in 13 tertiary care hospitals in northern, central, and southern Mexico. Demographic data, etiology, and complications were analyzed.
RESULTS:
MASLD was the most frequent cause of cirrhosis (42.8 %), followed by alcohol-related liver disease (ALD, 23.8 %) and hepatitis C virus (HCV, 12.2 %). MASLD was more common in older patients and women, while ALD was more frequent in younger patients and men. HCC was observed in 8.9 % of patients, with a higher prevalence in the central region. The most common complications were portal hypertension (59.5 %) and ascites (30.4 %). Regional differences were observed, with a higher prevalence of MASLD in central and southern Mexico, while ALD was more prominent in the northern region.
CONCLUSION:
This cross-sectional study underscores the changing etiologies of liver cirrhosis in Mexico, with MASLD emerging as the leading cause, particularly in older patients and women. Regional differences were evident, with ALD being more frequent in younger patients and in men, especially in the northern region.
2025-08-04·ARCHIVOS DE CARDIOLOGIA DE MEXICO
Article
作者: Sánchez-Grande, Paulina ; López-Terrazas, Javier ; Rivera-Parrado, Camilo A ; Colín-Ortiz, José L ; Munive-Molina, Ever ; Barrera-Colín, Miguel F ; Rivera-Parrado, Diego F
Objectives:
Patients with congenital heart disease with ductus arteriosus-dependent pulmonary flow have as a palliative procedure the placement of a Blalock-Taussig-Thomas fistula (BTTF) or ductal stent (DSt) and subsequently undergoing to definitive palliation or repair. BTTF has been associated with increased morbidity and mortality. The objective of this research is to compare the morbidity and mortality of BTTF versus DSt, as well as their short- and medium-term outcomes.
Methods:
The study population was patients undergoing BTTF or DSt placement from January 2012 to December 2022.
Results:
164 patients were identified, 128 with BTTF and 36 with DSt. 87.5% of the BTTF group presented complications, and 22.2% of the DSt group (p < 0.001). The OR for BTTF for development of complications was 19.58 (95%CI: 7.79-51.17). Intensive care unit stay was shortzer in DSt compared to FBTT (MD: -4.69 days; 95%CI: -7.30 to -2.07; I2 = 80%; p = 0.0004). The relative risk of FBTT patients for death was 2.32 (95%CI: 0.755-7.149), but there was no statistically significant difference for mortality (p = 0.135).
Conclusions:
Mortality presented a lower tendency in patients with DSt. However, in other variables such as morbidity, hospital stay and reintervention were less frequent in the DSt group and were statistically significant. This evidence is the first in Latin-America and supports DSt as the safest and most effective option compared to FBTT in our setting.
2025-08-01·LUPUS
Definition and application of systemic lupus erythematosus disease modification in emerging markets: Delphi panel consensus recommendations
Article
作者: Mejia-Vilet, Juan Manuel ; Scolnik, Marina ; Attar, Suzan M ; Alzahrani, Zeyad ; Magri, Sebastián Juan ; Gouhar, Raef ; Torres Dos Reis Neto, Edgard ; Al-Homood, Ibrahim ; Khamashta, Munther ; Almaghlouth, Ibrahim A ; García, Mercedes A ; Montezuma Sales, Gabriel Teixeira ; Elbadawi, Faisal ; Badsha, Humeira ; Yuki, Emily Figueiredo Neves ; Rocha, Bruno ; Monticielo, Odirlei Andre ; Al Wahshi, Humaid A ; Medrano-Ramirez, Gabriel ; Abdulkarim, Saadeya ; Pons-Estel, Guillermo J ; Al-Jayyousi, Reem ; Seguro, Luciana Parente Costa ; Babini, Alejandra ; Hussain, Razia ; Asiri, Alhussain
Objective:
To better understand the acceptance and potential application of the systemic lupus erythematosus (SLE) and lupus nephritis (LN) disease modification framework, which was first proposed in 2022, among experts in the Gulf region and Latin America.
Methods:
Two cross-sectional Delphi surveys of a panel of expert SLE physicians were conducted, with a workshop discussion held between the two surveys. Surveys comprised multiple choice and open-response questions. Experts from Argentina, Bahrain, Brazil, Mexico, Oman, Saudi Arabia and United Arab Emirates were selected based on their demonstrated expertise in SLE. Consensus was indicated by >75% agreement among experts in survey responses. Consensus was also evaluated by Gulf and Latin American regions to identify any regional differences.
Results:
There was consensus across all the queried statements on the concept and components of disease modification, with some minor regional differences observed. Experts unanimously agreed that early diagnosis, early referral to a lupus specialist and a multidisciplinary approach are key factors for achieving disease modification and better patient outcomes. Aspects of the published SLE/LN disease modification definition were either ‘routinely’ (31%) or ‘sometimes’ (62%) assessed in current clinical practice. A consensus was reached that biomarkers are a key component of evaluating disease modification (91%), but that currently available biomarkers are sub-optimal (96%). There was consensus that immunosuppressants (96%), biologics (92%) and hydroxychloroquine (88%) are disease modifying treatments. Experts from the Gulf, but not Latin America, agreed that glucocorticoids are not disease modifying.
Conclusions:
There was strong consensus across experts from the Gulf and Latin America that the concept of disease modification can provide a valuable framework to support clinicians for the management of patients with SLE and LN. Experts emphasised that clear guidance is required for clinicians to apply the disease modification framework to their routine practice, and in varying local healthcare systems.
100 项与 Hospital General de México 相关的药物交易
登录后查看更多信息
100 项与 Hospital General de México 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年02月08日管线快照
无数据报导
登录后保持更新
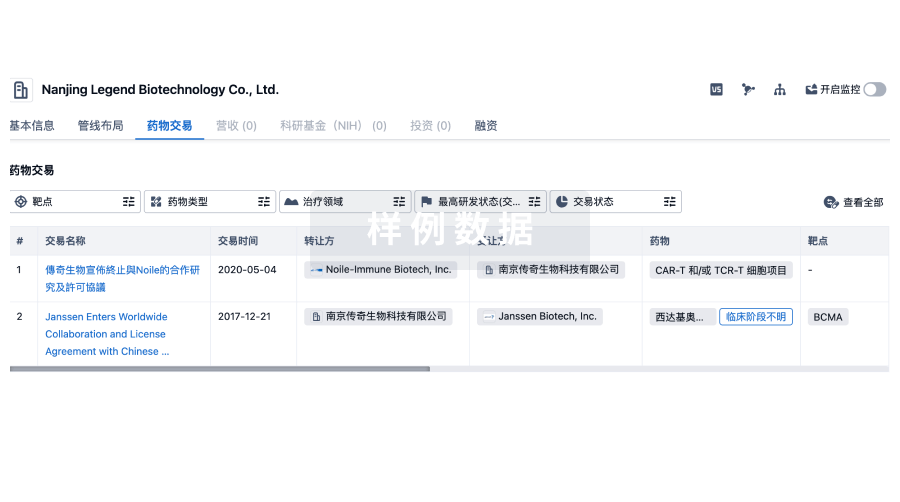
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
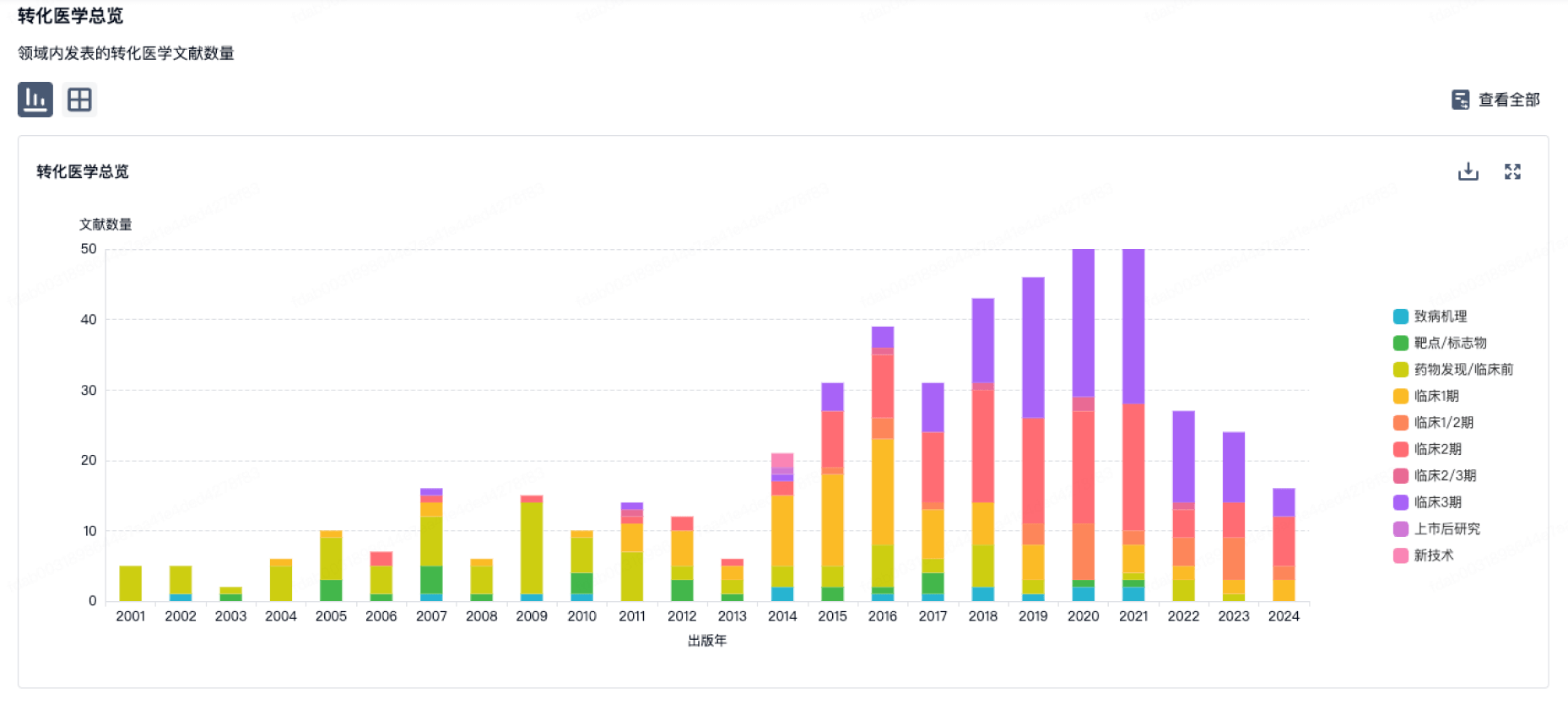
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
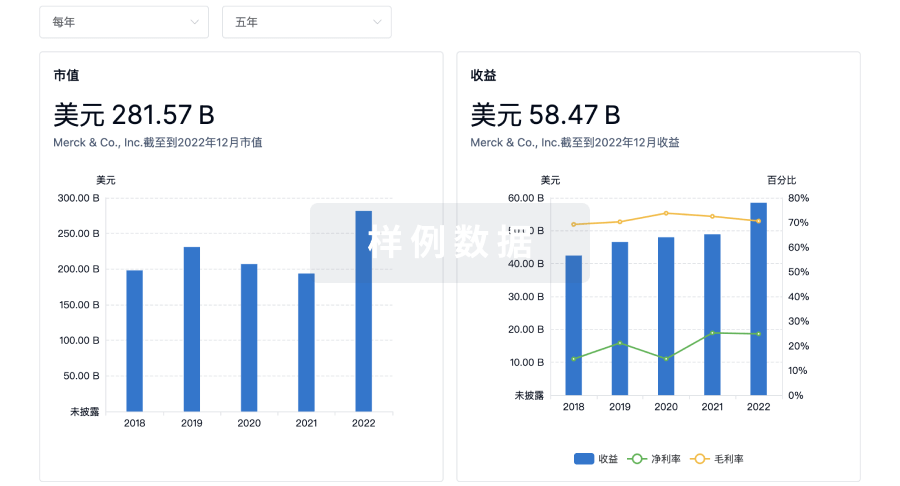
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
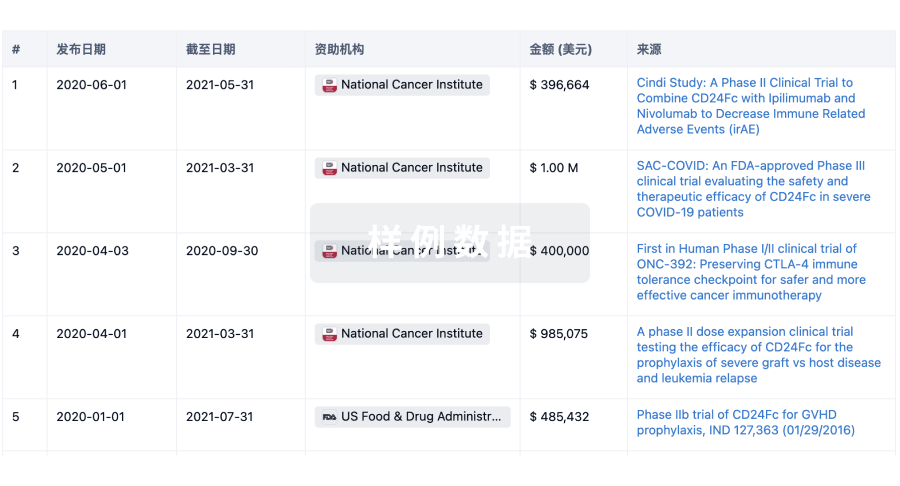
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用