预约演示
更新于:2025-05-07
Saint-Pierre University Hospital
更新于:2025-05-07
概览
关联
8
项与 Saint-Pierre University Hospital 相关的临床试验NCT05856396
Maternal Determinants of Infant Immunity to Pertussis
The overall objective of the project is to identify the determinants of antibody-mediated immunity in infants born to mothers immunized during pregnancy. Using maternal pertussis immunization as a model, the project will identify key predictors and potential determinants of vaccine responses in pregnant women, of the transfer of maternal antibodies to the newborn and of vaccine responses in infants. A systems biology approach will be used to delineate pre-vaccination and post-vaccination cellular and molecular correlates of the immune response to pertussis immunization in peripheral blood and in breastmilk.
开始日期2023-09-12 |
申办/合作机构 |
NCT05751148
Cardiovascular Effects of Intrathecal Hyperbaric Prilocaine or Bupivacaine in Surgery Under Spinal Anesthesia: A Multicenter Prospective Pilot Study Based on Non- Invasive Haemodynamic Monitoring
Spinal anesthesia remains a mainstay in lower limbs- as in day-case surgeries as well. It consists in injecting a local anesthetic drug into the intrathecal space of a patient's spinal canal. To achieve a suitable sensory and motor block for elective or emergent surgery, the anesthetist must adapt his choice of local anesthetic to the surgery's requirements and the patient's comorbidities, too.
Spinal anesthesia is often associated with adverse cardiovascular events, notably hypotension which is a major concern in current anesthetic practice, especially in specific patient populations.
Spinal induced hypotension is reported to be commonly related to the sympathetic block level and may be linked to perioperative cardiac and renal complications. Several mechanisms might play a role in the incidence of perioperative hypotension after spinal puncture. A decrease in peripheric systemic vascular resistance from arterial vasodilatation, a reduction of cardiac output due to a decrease in preload from a redistribution of venous blood into lower limbs or even an occurrence or increment of cardiac dysfunction, might compound proper blood flow towards noble organs such as brain, heart and kidneys. Spinal induced hypotension may also be related to a direct reduction of cardiac contractibility by the local anesthetic injection.
Compensating mechanisms might be inhibited depending on the level of sympathetic blockade, usually related to the dose of the local anesthetic. Former studies found that intrinsic left ventricular depression might occur during spinal anesthesia as left ventricular volumes per se remain stable. One noticed that diastolic and systolic function (i.e., ventricular outflow tract velocity) decreased significantly after intrathecal levobupivacaine plus fentanyl injection based on transthoracic ultrasound assessment. Other authors use Pro-Brain Natriuretic Peptide to assess myocardial stress induced by surgery and anesthetic management. Other serum markers such as Cortisol, Adreno Cortico-Trope Hormone, Angiotensin are identified to screen and monitor myocardial stress as for instance acute myocardial dysfunction.
Hyperbaric prilocaine is an intermediate-acting local anesthetic, whereas bupivacaine may be intermediate- or long-acting depending on the employed dose. Both drugs provide comparable sensory and motor block that meet the anesthesia level requirements in various surgical procedures.
In regard to the hemodynamic effects, hypotension has been largely reported following hyperbaric bupivacaine in a dose-dependent way. However, discrepancy exists between the rare studies having investigated prilocaine's effects, probably related to the methodology and the employed doses. Moreover, the hemodynamics effects of these local anesthetics have been barely specifically investigated in a non-cesarean section context.
The aim of this study is to compare the cardiovascular effects inflicted by hyperbaric prilocaine and bupivacaine under spinal anesthesia. Cardiovascular response will be assessed by non-invasive hemodynamic monitoring whereas metabolic stress will be evaluated using serum stress markers.
Spinal anesthesia is often associated with adverse cardiovascular events, notably hypotension which is a major concern in current anesthetic practice, especially in specific patient populations.
Spinal induced hypotension is reported to be commonly related to the sympathetic block level and may be linked to perioperative cardiac and renal complications. Several mechanisms might play a role in the incidence of perioperative hypotension after spinal puncture. A decrease in peripheric systemic vascular resistance from arterial vasodilatation, a reduction of cardiac output due to a decrease in preload from a redistribution of venous blood into lower limbs or even an occurrence or increment of cardiac dysfunction, might compound proper blood flow towards noble organs such as brain, heart and kidneys. Spinal induced hypotension may also be related to a direct reduction of cardiac contractibility by the local anesthetic injection.
Compensating mechanisms might be inhibited depending on the level of sympathetic blockade, usually related to the dose of the local anesthetic. Former studies found that intrinsic left ventricular depression might occur during spinal anesthesia as left ventricular volumes per se remain stable. One noticed that diastolic and systolic function (i.e., ventricular outflow tract velocity) decreased significantly after intrathecal levobupivacaine plus fentanyl injection based on transthoracic ultrasound assessment. Other authors use Pro-Brain Natriuretic Peptide to assess myocardial stress induced by surgery and anesthetic management. Other serum markers such as Cortisol, Adreno Cortico-Trope Hormone, Angiotensin are identified to screen and monitor myocardial stress as for instance acute myocardial dysfunction.
Hyperbaric prilocaine is an intermediate-acting local anesthetic, whereas bupivacaine may be intermediate- or long-acting depending on the employed dose. Both drugs provide comparable sensory and motor block that meet the anesthesia level requirements in various surgical procedures.
In regard to the hemodynamic effects, hypotension has been largely reported following hyperbaric bupivacaine in a dose-dependent way. However, discrepancy exists between the rare studies having investigated prilocaine's effects, probably related to the methodology and the employed doses. Moreover, the hemodynamics effects of these local anesthetics have been barely specifically investigated in a non-cesarean section context.
The aim of this study is to compare the cardiovascular effects inflicted by hyperbaric prilocaine and bupivacaine under spinal anesthesia. Cardiovascular response will be assessed by non-invasive hemodynamic monitoring whereas metabolic stress will be evaluated using serum stress markers.
开始日期2023-03-22 |
NCT06716567
Maternal Determinants of Immunity to Influenza (MADI-01)
The overall objective of the project is to determine the impact of pregnancy on the response to influenza immunization.
开始日期2020-11-16 |
100 项与 Saint-Pierre University Hospital 相关的临床结果
登录后查看更多信息
0 项与 Saint-Pierre University Hospital 相关的专利(医药)
登录后查看更多信息
675
项与 Saint-Pierre University Hospital 相关的文献(医药)2025-05-01·Resuscitation Plus
Postresuscitation pleth variability index-guided hemodynamic management of out-of-hospital cardiac arrest survivors: A randomised controlled trial
Article
作者: Domont, Pierre ; Matta, Silvia ; Dumay, Paul ; Bouazza, Fatima Zohra ; Herpain, Antoine ; Grignard, Jolan ; Ochogavia, Queitan ; Claus, Marc ; Malinverni, Stefano
2025-04-01·Gynécologie Obstétrique Fertilité & Sénologie
Impact d’HypnoVR©, associé à une anesthésie locale, sur la douleur et l’anxiété ressenties lors d’une ponction ovocytaire
Article
作者: Vanderstraeten, Anne-Laure ; Dumont, Coralie ; Delotte, Jérôme ; Boukaidi, Samir ; Cruzel, Coralie
2025-04-01·Neurocritical Care
Contribution of an Automatic Algorithm for Quantifying the Volume of Aneurysmal Subarachnoid Hemorrhage to the Evaluation of the Risk of Occurrence of Delayed Cerebral Ischemia: A Cohort Study
Article
作者: Velly, Lionel ; Girard, Nadine ; Cardoso, Dan ; Dufour, Henry ; Reyre, Anthony ; Brunel, Hervé ; Boussen, Salah ; Graillon, Thomas ; Simeone, Pierre ; Couret, David ; Alonzo, Audrey ; Bruder, Nicolas ; Corrias, Thomas
3
项与 Saint-Pierre University Hospital 相关的新闻(医药)2025-03-10
Johnson & Johnson's icotrokinra (JNJ-2113) met the primary endpoint of a Phase IIb ulcerative colitis (UC) study, building on its recent success in psoriasis. The IL-23-blocking oral peptide could also boost the company's efforts to stay ahead in immunology as Stelara (ustekinumab) stares down biosimilar competition.In the ANTHEM-UC study, J&J tested three once-daily doses of icotrokinra and found that the highest one led to a clinical response in 63.5% of patients after 12 weeks, compared to just 27% for placebo. The drug also showed "meaningful differences" on secondary measures like clinical remission, with 30.2% of patients on the highest dose achieving remission versus 11.1% for placebo. J&J said the benefits kept improving through week 28, with a favourable safety profile.The trial enrolled 252 patients with moderately to severely active UC who'd had an inadequate response or intolerance to conventional therapy. More ANTHEM-UC results will be shared at upcoming medical congresses."These impressive findings show the potential of icotrokinra to transform the treatment paradigm… by offering a distinctive combination of therapeutic benefit, tolerability, and convenience with a once-daily oral treatment," said Esi Lamousé-Smith, gastroenterology disease area lead at J&J, in a release Monday.The icotrokinra results complement J&J's recent efforts to strengthen its IL-23 lineup, including September's FDA approval of Tremfya (guselkumab) for UC with intravenous induction and subcutaneous maintenance, and a pending application for a fully subcutaneous regimen. According to data presented last month, Tremfya's SC induction demonstrated significantly higher rates of clinical remission (27.6% vs 6.5%) and response (65.6% vs 34.5%) versus placebo at week 12 in the Phase III ASTRO trial.Both icotrokinra and Tremfya are being positioned to help offset expected revenue declines from Stelara, which saw a 4.6% global sales drop in 2024 as biosimilars enter the market.The UC data for icotrokinra follows its strong showing in psoriasis at the American Academy of Dermatology (AAD) meeting over the weekend. The ICONIC-ADVANCE 1 and 2 trials not only met their primary endpoints of achieving clear or nearly clear skin, but also demonstrated superiority to Bristol Myers Squibb's oral TYK2 inhibitor Sotyktu (deucravacitinib). See – ViewPoints: AAD25 – J&J leadership tells how icotrokinra is upping the ante across the board in psoriasis.
临床结果临床3期上市批准临床2期
2025-02-21
Phase 3 ASTRO study achieves primary and all secondary endpoints at Week 12 in ulcerative colitis patients
The only SC induction data for an IL-23 inhibitor show statistically significant and clinically meaningful improvements across clinical and endoscopic measures versus placebo, consistent with IV induction
SPRING HOUSE, Pa., Feb. 21, 2025 /PRNewswire/ -- Johnson & Johnson (NYSE: JNJ) today announced data from the Phase 3 ASTRO study of TREMFYA® (guselkumab) subcutaneous (SC) induction therapy in adults with moderately to severely active ulcerative colitis (UC) at the 20th Congress of the European Crohn's and Colitis Organization (ECCO). Study findings through Week 12 showed statistically significant and clinically meaningful improvements compared to placebo across all clinical and endoscopic measures consistent with the U.S. Food and Drug Administration (FDA)-approved intravenous (IV) induction regimen in this population.1
"The Week 12 results from the ASTRO study build on data from the QUASAR study demonstrating that both guselkumab SC and IV induction achieved clinically differentiated results in patients with moderately to severely active UC," said Laurent Peyrin-Biroulet, M.D., Ph.D., Head of the Inflammatory Bowel Disease (IBD) Unit at Nancy University Hospital in France and study investigator.a "The flexibility of a fully SC treatment regimen would be a welcome option for many patients, especially those with busy and active lifestyles."
At Week 12, significantly greater proportions of patients treated with TREMFYA® 400 mg SC induction compared with patients receiving placebo achieved all of the following multiplicity-controlled endpoints:
Clinical remission (27.6% vs 6.5%; P<0.001)b Clinical response (65.6% vs 34.5%; P<0.001)c Endoscopic improvement (37.3% vs 12.9%; P<0.001)d
In prespecified analyses of subpopulations defined by prior advanced therapy treatment status, TREMFYA® demonstrated statistically significant results across endpoints in both biologic and JAK inhibitor-naïve and biologic and JAK inhibitor-refractory patients.
Safety data from the ASTRO study were consistent with the well-established safety profile of TREMFYA®. The proportions of patients with ≥1 adverse event (AE), serious AE, or AE leading to treatment discontinuation were similar across the TREMFYA® and placebo treatment groups.
"We aim to offer treatment options for patients with IBD that allow them to effectively manage their disease while also meeting the daily demands of life. These results further underscore the potential of TREMFYA to transform the UC treatment paradigm," said Esi Lamousé-Smith, M.D., Ph.D., Vice President, Gastroenterology Disease Area Lead, Immunology, Johnson & Johnson Innovative Medicine. "Pending approval, TREMFYA would be the first IL-23 inhibitor with a fully SC induction and maintenance regimen, increasing options for both patients and healthcare providers."
TREMFYA® is the first and only approved fully-human, dual-acting monoclonal antibody that blocks IL-23 while also binding to CD64, a receptor on cells that produce IL-23. IL-23 is a cytokine secreted by activated monocyte/macrophages and dendritic cells that is known to be a driver of immune-mediated diseases including UC.1,2,3,4,5
Applications seeking approval of TREMFYA® for both UC and Crohn's disease (CD) have been submitted in Europe. TREMFYA® received FDA approval in September 2024 for the treatment of adult patients with moderately to severely active UC and is currently administered via an IV induction regimen, followed by a SC maintenance regimen. In November 2024, a supplemental Biologics License Application (sBLA) was submitted to the FDA seeking approval of a SC induction regimen of TREMFYA® for the treatment of adults with moderately to severely active UC. An application for the treatment of adults with moderately to severely active CD has also been submitted in the U.S.
For a full list of all data being presented at ECCO visit: https://innovativemedicine.jnj.com/our-innovation/focus-areas/immunology/gastroenterology/gastroenterology-newsroom
Editor's Notes:
a. Dr. Peyrin-Biroulet is a paid consultant for Johnson & Johnson. He has not been compensated for any media work.b. Clinical remission is defined as a Mayo stool frequency subscore of 0 or 1 and not increased from baseline, a Mayo rectal bleeding subscore of 0, and a Mayo endoscopic subscore of 0, or 1 with no friability present on the endoscopy.c. Clinical response was defined as a decrease from induction baseline in the modified Mayo score by ≥30 percent and ≥2 points, with either a ≥1-point decrease from baseline in the rectal bleeding subscore or a rectal bleeding subscore of 0 or 1.d. Endoscopic improvement was defined as an endoscopy subscore of 0 or 1 with no friability present on the endoscopy.
ABOUT THE ASTRO STUDY (NCT05528510)
ASTRO is a randomized, double-blind, placebo-controlled, parallel-group, multicenter, treat-through Phase 3 study designed to evaluate the efficacy and safety of TREMFYA® SC induction therapy (400 mg at Weeks 0, 4, and 8) in adults with moderately to severely active ulcerative colitis who had an inadequate response or intolerance to conventional therapy (e.g., thiopurines or corticosteroids), prior biologics (TNF antagonists or vedolizumab) and/or ozanimod or approved JAK inhibitors. Patients (n = 418) were randomized 1:1:1 to receive TREMFYA® 400 mg SC induction at Weeks 0, 4 and 8 followed by TREMFYA® 200 mg SC every 4 weeks (q4w); or TREMFYA® 400 mg SC induction at Weeks 0, 4 and 8, followed by TREMFYA® 100 mg SC every 8 weeks (q8w); or placebo. The maintenance dose regimens in ASTRO (200 mg SC q4w and 100 mg SC q8w) are the same as those evaluated in the Phase 3 QUASAR program which established the efficacy and safety profile of IV induction followed by SC maintenance therapy in patients with moderate to severely active UC.6
ABOUT THE QUASAR PROGRAM (NCT04033445)
QUASAR is a randomized, double-blind, placebo-controlled, parallel group, multicenter, Phase 2b/3 program designed to evaluate the efficacy and safety of TREMFYA® in adults with moderately to severely active ulcerative colitis who had an inadequate response or intolerance to conventional therapy (e.g., thiopurines or corticosteroids), prior biologics (TNF antagonists or vedolizumab) and/or JAK inhibitors (tofacitinib). QUASAR included a Phase 2b dose-ranging induction study, a confirmatory Phase 3 induction study, and a Phase 3 randomized withdrawal maintenance study. In the Phase 3 induction study, patients received either TREMFYA® 200 mg or placebo by IV infusion at Weeks 0, 4, and 8. In the Phase 3 maintenance study, patients received a SC maintenance regimen of either TREMFYA® 200 mg q4w, TREMFYA® 100 mg q8w, or placebo.7
ABOUT ULCERATIVE COLITIS
Ulcerative colitis (UC) is a chronic disease of the large intestine, also known as the colon, in which the lining of the colon becomes inflamed and develops tiny open sores, or ulcers, that produce pus and mucus. It is the result of the immune system's overactive response. Symptoms vary but may typically include loose and more urgent bowel movements, rectal bleeding or bloody stool, persistent diarrhea, abdominal pain, loss of appetite, weight loss, and fatigue.8
ABOUT CROHN'S DISEASE
Crohn's disease is one of the two main forms of inflammatory bowel disease, which affects an estimated three million Americans.9 Crohn's disease is a chronic inflammatory condition of the gastrointestinal tract with no known cause, but the disease is associated with abnormalities of the immune system that could be triggered by a genetic predisposition, diet, or other environmental factors. Symptoms of Crohn's disease can vary, but often include abdominal pain and tenderness, frequent diarrhea, rectal bleeding, weight loss, and fever.10
ABOUT TREMFYA® (guselkumab)
Developed by Johnson & Johnson, TREMFYA® is the first approved fully-human, dual-acting monoclonal antibody designed to neutralize inflammation at the cellular source by blocking IL-23 and binding to CD64 (a receptor on cell that produce IL-23). Findings for dual-acting are limited to in vitro studies that demonstrate guselkumab binds to CD64, which is expressed on the surface of IL-23 producing cells in an inflammatory monocyte model. The clinical significance of this finding is not known.
TREMFYA® is a prescription medicine approved in the U.S. to treat:
adults with moderate to severe plaque psoriasis who may benefit from taking injections or pills (systemic therapy) or phototherapy (treatment using ultraviolet or UV light). adults with active psoriatic arthritis. adults with moderately to severely active ulcerative colitis.2
TREMFYA® is approved Europe, Canada, Japan, and a number of other countries for the treatment of adults with moderate-to-severe plaque psoriasis and for the treatment of adults with active psoriatic arthritis.
Johnson & Johnson maintains exclusive worldwide marketing rights to TREMFYA®. For more information, visit: www.tremfya.com.
IMPORTANT SAFETY INFORMATIONWhat is the most important information I should know about TREMFYA® (guselkumab)?
TREMFYA® is a prescription medicine that may cause serious side effects, including:
Serious Allergic Reactions. Stop using TREMFYA® and get emergency medical help right away if you develop any of the following symptoms of a serious allergic reaction:
fainting, dizziness, feeling lightheaded (low blood pressure)
swelling of your face, eyelids, lips, mouth, tongue, or throat
trouble breathing or throat tightness
chest tightness
skin rash, hives
itching
Infections. TREMFYA® may lower the ability of your immune system to fight infections and may increase your risk of infections. Your healthcare provider should check you for infections and tuberculosis (TB) before starting treatment with TREMFYA® and may treat you for TB before you begin treatment with TREMFYA® if you have a history of TB or have active TB. Your healthcare provider should watch you closely for signs and symptoms of TB during and after treatment with TREMFYA®.
Tell your healthcare provider right away if you have an infection or have symptoms of an infection, including:
fever, sweats, or chills
muscle aches
weight loss
cough
warm, red, or painful skin or sores on your body different from your psoriasis
diarrhea or stomach pain
shortness of breath
blood in your phlegm (mucus)
burning when you urinate or urinating more often than normal
Do not take TREMFYA® if you have had a serious allergic reaction to guselkumab or any of the ingredients in TREMFYA®.
Before using TREMFYA®, tell your healthcare provider about all of your medical conditions, including if you:
have any of the conditions or symptoms listed in the section "What is the most important information I should know about TREMFYA®?" have an infection that does not go away or that keeps coming back. have TB or have been in close contact with someone with TB. have recently received or are scheduled to receive an immunization (vaccine). You should avoid receiving live vaccines during treatment with TREMFYA®. are pregnant or plan to become pregnant. It is not known if TREMFYA® can harm your unborn baby.Pregnancy Registry: If you become pregnant during treatment with TREMFYA®, talk to your healthcare provider about registering in the pregnancy exposure registry for TREMFYA®. You can enroll by visiting www.mothertobaby.org/ongoing-study/tremfya-guselkumab, by calling 1-877-311-8972, or emailing MotherToBaby@health.ucsd.edu. The purpose of this registry is to collect information about the safety of TREMFYA® during pregnancy. are breastfeeding or plan to breastfeed. It is not known if TREMFYA® passes into your breast milk.
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements.
What are the possible side effects of TREMFYA®?
TREMFYA® may cause serious side effects. See "What is the most important information I should know about TREMFYA®?"
The most common side effects of TREMFYA® include respiratory tract infections, headache, injection site reactions, joint pain (arthralgia), diarrhea, stomach flu (gastroenteritis), fungal skin infections, herpes simplex infections, and bronchitis.
These are not all the possible side effects of TREMFYA®. Call your doctor for medical advice about side effects.
Use TREMFYA® exactly as your healthcare provider tells you to use it.
Please read the full Prescribing Information, including Medication Guide, for TREMFYA® and discuss any questions that you have with your doctor.
You are encouraged to report negative side effects of prescription drugs to the FDA. Visit www.fda.gov/medwatch, or call 1-800-FDA-1088.
Dosage Forms and Strengths: TREMFYA® is available in a 100 mg/mL prefilled syringe and One-Press patient-controlled injector for subcutaneous injection, a 200 mg/2 mL prefilled syringe and prefilled pen (TREMFYA® PEN) for subcutaneous injection, and a 200 mg/20 mL (10 mg/mL) single dose vial for intravenous infusion.
ABOUT JOHNSON & JOHNSON
At Johnson & Johnson, we believe health is everything. Our strength in healthcare innovation empowers us to build a world where complex diseases are prevented, treated, and cured, where treatments are smarter and less invasive, and solutions are personal. Through our expertise in Innovative Medicine and MedTech, we are uniquely positioned to innovate across the full spectrum of healthcare solutions today to deliver the breakthroughs of tomorrow, and profoundly impact health for humanity.
Learn more at https://www.jnj.com/ or at www.innovativemedicine.jnj.com
Follow us at @JNJInnovMed.
Janssen Research & Development, LLC and Janssen Biotech, Inc. are Johnson & Johnson companies.
Cautions Concerning Forward-Looking Statements
This press release contains "forward-looking statements" as defined in the Private Securities Litigation Reform Act of 1995 regarding TREMFYA®. The reader is cautioned not to rely on these forward-looking statements. These statements are based on current expectations of future events. If underlying assumptions prove inaccurate or known or unknown risks or uncertainties materialize, actual results could vary materially from the expectations and projections of Janssen Research & Development, LLC, Janssen Biotech, Inc., Janssen-Cilag International NV and/or Johnson & Johnson. Risks and uncertainties include, but are not limited to: challenges and uncertainties inherent in product research and development, including the uncertainty of clinical success and of obtaining regulatory approvals; uncertainty of commercial success; manufacturing difficulties and delays; competition, including technological advances, new products and patents attained by competitors; challenges to patents; product efficacy or safety concerns resulting in product recalls or regulatory action; changes in behavior and spending patterns of purchasers of health care products and services; changes to applicable laws and regulations, including global health care reforms; and trends toward health care cost containment. A further list and descriptions of these risks, uncertainties and other factors can be found in Johnson & Johnson's most recent Annual Report on Form 10-K, including in the sections captioned "Cautionary Note Regarding Forward-Looking Statements" and "Item 1A. Risk Factors," and in Johnson & Johnson's subsequent Quarterly Reports on Form 10-Q and other filings with the Securities and Exchange Commission. Copies of these filings are available online at www.sec.gov, www.jnj.com or on request from Johnson & Johnson. None of Janssen Research & Development, LLC, Janssen Biotech, Inc., Janssen-Cilag International NV nor Johnson & Johnson undertakes to update any forward-looking statement as a result of new information or future events or developments.
1 Peyrin-Biroulet, et al. Efficacy and safety of subcutaneous guselkumab induction therapy in patients with Ulcerative Colitis: Results through week 12 from the phase 3 ASTRO study. Results from the Phase 3 ASTRO study. Oral presentation (#OP10) at the 20th Congress of the European Crohn's and Colitis Organization (ECCO). February 2025.2 Kreuger JG, Eyerich K, Kuchroo VK. Il-23 past, present, and future: a roadmap to advancing IL-23 science and therapy. Front Immunol. 2024; 15:1331217. doi:10.3389/fimmu.2024.13312173 TREMFYA® Prescribing Information. Available at: https://www.janssenlabels.com/package-insert/product-monograph/prescribing-information/TREMFYA-pi.pdf Accessed October 2024.4 Skyrizi® [Prescribing Information]. North Chicago, IL: AbbVie, Inc.5 Omvoh™ [Prescribing Information]. Indianapolis, IN: Eli Lilly and Company.6 National Institutes of Health: Clinicaltrials.gov. A Study of Guselkumab Therapy in Participants With Moderately to Severely Active Ulcerative Colitis (ASTRO). Identifier: NCT05528510. https://clinicaltrials.gov/study/NCT05528510?term=astro&intr=guselkumab&rank=1. Accessed January 2025.7 National Institutes of Health: Clinicaltrials.gov. A Study of Guselkumab in Participants With Moderately to Severely Active Ulcerative Colitis (QUASAR). Identifier: NCT04033445. https://classic.clinicaltrials.gov/ct2/show/NCT04033445. Accessed January 2025.8 Crohn's & Colitis Foundation. What is ulcerative colitis? Available at: https://www.crohnscolitisfoundation.org/what-is-ulcerative-colitis. Accessed April 2024.9 Crohn's & Colitis Foundation. Overview of Crohn's disease. Available at: https://www.crohnscolitisfoundation.org/what-is-crohns-disease/overview. Accessed October 2024.10 Crohn's & Colitis Foundation. Signs and symptoms of Crohn's disease. Available at https://www.crohnscolitisfoundation.org/patientsandcaregivers/what-is-crohns-disease/symptoms. Accessed October 2024.
Media contact:Craig Stoltz
cstoltz@its.jnj.com
Investor contact:Lauren Johnsoninvestor-relations@its.jnj.com
View original content to download multimedia:https://www.prnewswire.com/news-releases/tremfya-guselkumab-subcutaneous-sc-induction-data-support-potential-to-be-the-first-and-only-in-its-class-to-offer-the-option-of-both-intravenous-and-sc-induction-therapy-in-ulcerative-colitis-302381823.html
SOURCE Johnson & Johnson
临床结果临床3期上市批准
2024-03-09
SPROUT 52-Week Data Demonstrate Durable Response and Consistent Safety Profile of Oral Otezla in Children with Moderate to Severe Plaque Psoriasis
Late-Breaking Phase 3 Study of Otezla in Palmoplantar Pustulosis Achieves Primary and Secondary Endpoints at 16 Weeks
THOUSAND OAKS, Calif., March 9, 2024 /PRNewswire/ -- Amgen (NASDAQ:AMGN) today announced new, 52-week results from the Phase 3 SPROUT study examining the use of Otezla® (apremilast) in children and adolescents aged 6 to 17 years with moderate to severe plaque psoriasis. These data, along with findings from a Phase 3 late-breaking study on Otezla in palmoplantar pustulosis, will be presented at the 2024 American Academy of Dermatology (AAD) Annual Meeting, March 8-12 in San Diego.
"These data reflect Amgen's commitment to exploring new ways to treat inflammatory skin disease," said Ponda Motsepe-Ditshego, vice president, Global Medical, at Amgen. "A decade after the launch of Otezla, we continue to study how this oral therapy can help improve care and reduce disease burden in underserved patient populations."
SPROUT Phase 3 Study
Results from SPROUT, a multicenter, randomized, placebo-controlled, double-blind study, demonstrated the efficacy and safety of Otezla in pediatric patients aged 6 to 17 years with moderate to severe plaque psoriasis inadequately controlled by or intolerant to topical therapy. Continued Otezla use resulted in sustained improvements in psoriasis severity and skin involvement in patients for up to one year. The safety profile was consistent with previous Otezla studies. These findings add to the published 16-week results.1
"For the first time, we have a full year of data on a potential oral treatment for children and adolescents with moderate to severe plaque psoriasis, who currently lack any approved oral treatment options," said Loretta Fiorillo, M.D., FRCPC, clinical professor of pediatrics, University of Alberta. "At 52 weeks, more than half of patients achieved clear or almost clear skin. Otezla showed increased efficacy beyond that seen at the week 16 primary endpoint, with a durable maintenance of response – an important finding for families living with this chronic inflammatory disease."
All patients in the study received Otezla for a 36-week extended active treatment period following the 16-week randomized placebo-controlled treatment period, providing up to 52 weeks of data. There were 186 patients who completed the 36-week extension: 125 who continued to receive Otezla, and 61 patients switched from placebo to Otezla.
Study findings include:2
56.3% of patients who received Otezla through week 52 achieved static Physician Global Assessment (sPGA) response (score of ≥3), an investigator assessment of overall disease severity of plaque psoriasis, the study's primary endpoint.
52.5% of patients who switched from placebo to Otezla achieved sPGA response at week 52.
71.4% of patients who received Otezla through week 52 achieved Psoriasis Area and Severity Index (PASI)-75, an investigator assessment of disease severity and skin involvement, a secondary endpoint.
75.4% of patients who switched from placebo to Otezla achieved PASI-75 at week 52.
Treatment-emergent adverse events (AEs) were consistent with the known safety profile of Otezla in adults. The most common AEs (>10%) throughout the study were nausea, diarrhea, abdominal pain, vomiting and headache.
Findings will be presented as an e-poster with an oral presentation on Saturday, March 9 at 4:50 p.m. PST.
Phase 3 Late-Breaking Palmoplantar Pustulosis Findings
Amgen also will present late-breaking findings from a Phase 3 study evaluating the efficacy and safety of Otezla in patients with moderate to severe palmoplantar pustulosis in Japan following inadequate response to topical therapy. Palmoplantar pustulosis is a chronic inflammatory condition characterized by pustules on the palms and soles. The condition can be difficult to treat, with limited available treatment options.3,4
"Palmoplantar pustulosis can severely impact daily functioning due to its painful effects on the hands and feet, necessitating new therapeutic options for this impactful inflammatory skin condition," said Melinda Gooderham, M.D., FRCPC, dermatologist and clinical investigator at SKiN Centre for Dermatology and assistant professor, Queen's University, Ontario, Canada. "The study presented at AAD highlighted significant improvement in disease severity, symptoms such as itch, pain, discomfort, and patient-reported quality of life among those treated with Otezla compared to placebo."
The randomized, placebo-controlled, double-blind study included 176 patients who received Otezla (n=88) or placebo (n=88) for 16 weeks. All primary and secondary endpoints were met.
Study findings include:5
67.8% of patients who received Otezla achieved the primary endpoint of PPPASI 50 (>50% improvement in the Palmoplantar Pustulosis Area and Severity Index); this was a significantly greater response as compared to placebo (35.3%; P<0.0001).
Statistically significant improvements in all secondary endpoints were observed with Otezla relative to placebo, including changes from baseline to week 16 in PPPASI, PPSI (Palmoplantar Pustulosis Severity Index), Patient Visual Analogue Scale of palmoplantar pruritus and pain/discomfort and DLQI (Dermatology Life Quality Index).
Treatment-emergent AEs were consistent with the known safety profile of Otezla. The most common AEs (>10%) throughout the study were diarrhea, soft feces, headache and nausea.
Findings will be presented as a late-breaking oral presentation on Saturday, March 9 at 9:20 a.m. PST.
Additional Amgen data to be presented at AAD include:
Otezla Abstracts
Long-term Impact of Apremilast on Cardiometabolic Parameters and the Relationship of Cardiometabolic Changes with Psoriasis Efficacy
Abstract #50668, E-Poster and Oral Presentation of Poster on Saturday, March 9 at 3:55 p.m. PST
Beyond Race-Ethnicity: Fitzpatrick Skin Type Analysis Highlights Unmet Needs and Differing Treatment Patterns in Psoriasis Among the Conventional Systemics Cohort of British Association of Dermatologists Biologic and Immunomodulators Register (BADBIR)
Abstract #51067, E-Poster and Oral Presentation of Poster on Saturday, March 9 at 4:15 p.m. PST
Apremilast Improves Clinical Outcomes and Pain in Patients with Oligoarticular Psoriatic Arthritis
Abstract #51246, E-Poster
Efficacy of Apremilast in Adults with Mild-to-Moderate Plaque Psoriasis with Scalp Involvement: Pooled Data from PROMINENT, ADVANCE, and EMBRACE Trials
Abstract #51480, E-Poster
Proportion of the US Psoriasis Population Impacted by Common Warnings for Moderate-to-Severe Plaque Psoriasis Treatment
Abstract #52846, E-Poster
Rocatinlimab (AMG 451/KHK4083) Abstract
Rocatinlimab Significantly Improves Clinical Responses in Patients with Moderate-to-Severe Atopic Dermatitis by Week 2 in a Randomized Double-Blind Placebo-Controlled Phase 2b Study
Abstract #50233, E-Poster
About Psoriasis
Psoriasis is a chronic disease where skin cells build up quickly, typically causing red or discolored, scaly, and itchy patches on the skin.6 Approximately 125 million people worldwide have psoriasis, including around 14 million people in Europe and more than 8 million people in the United States.7,8 About 80% of those patients have plaque psoriasis.9
About Otezla® (apremilast)
Otezla® (apremilast) is an oral small-molecule inhibitor of phosphodiesterase 4 (PDE4) specific for cyclic adenosine monophosphate (cAMP). PDE4 inhibition results in increased intracellular cAMP levels, which is thought to indirectly modulate the production of inflammatory mediators. The specific mechanism(s) by which Otezla exerts its therapeutic action in patients is not well defined.
Since its initial FDA approval in 2014, Otezla has been prescribed to more than 920,000 patients worldwide.10
Otezla® (apremilast) U.S. INDICATIONS
INDICATIONS
Otezla® (apremilast) is indicated for the treatment of adult patients with plaque psoriasis who are candidates for phototherapy or systemic therapy.
Otezla is indicated for the treatment of adult patients with active psoriatic arthritis.
Otezla is indicated for the treatment of adult patients with oral ulcers associated with Behçet's Disease.
Otezla® (apremilast) U.S. IMPORTANT SAFETY INFORMATION
Contraindications
Otezla® is contraindicated in patients with a known hypersensitivity to apremilast or to any of the excipients in the formulation
Warnings and Precautions
Hypersensitivity: Hypersensitivity reactions, including angioedema and anaphylaxis, have been reported during postmarketing surveillance. If signs or symptoms of serious hypersensitivity reactions occur, discontinue Otezla and institute appropriate therapy
Diarrhea, Nausea, and Vomiting: Cases of severe diarrhea, nausea, and vomiting were associated with the use of Otezla. Most events occurred within the first few weeks of treatment. In some cases, patients were hospitalized. Patients 65 years of age or older and patients taking medications that can lead to volume depletion or hypotension may be at a higher risk of complications from severe diarrhea, nausea, or vomiting. Monitor patients who are more susceptible to complications of diarrhea or vomiting; advise patients to contact their healthcare provider. Consider Otezla dose reduction or suspension if patients develop severe diarrhea, nausea, or vomiting
Depression: Carefully weigh the risks and benefits of treatment with Otezla for patients with a history of depression and/or suicidal thoughts/behavior, or in patients who develop such symptoms while on Otezla. Patients, caregivers, and families should be advised of the need to be alert for the emergence or worsening of depression, suicidal thoughts or other mood changes, and they should contact their healthcare provider if such changes occur
Plaque Psoriasis: Treatment with Otezla is associated with an increase in depression. During clinical trials in patients with moderate to severe plaque psoriasis, 1.3% (12/920) of patients reported depression compared to 0.4% (2/506) on placebo. Depression was reported as serious in 0.1% (1/1308) of patients exposed to Otezla, compared to none in placebo-treated patients (0/506). Suicidal behavior was observed in 0.1% (1/1308) of patients on Otezla, compared to 0.2% (1/506) on placebo. One patient treated with Otezla attempted suicide; one patient on placebo committed suicide
Psoriatic Arthritis: Treatment with Otezla is associated with an increase in depression. During clinical trials, 1.0% (10/998) reported depression or depressed mood compared to 0.8% (4/495) treated with placebo. Suicidal ideation and behavior was observed in 0.2% (3/1441) of patients on Otezla, compared to none in placebo-treated patients. Depression was reported as serious in 0.2% (3/1441) of patients exposed to Otezla, compared to none in placebo-treated patients (0/495). Two patients who received placebo committed suicide compared to none on Otezla
Behçet's Disease: Treatment with Otezla is associated with an increase in depression. During the clinical trial, 1% (1/104) reported depression or depressed mood compared to 1% (1/103) treated with placebo. No instances of suicidal ideation or behavior were reported in patients treated with Otezla or treated with placebo
Weight Decrease: Monitor body weight regularly; evaluate unexplained or clinically significant weight loss, and consider discontinuation of Otezla
Plaque Psoriasis: Body weight loss of 5-10% occurred in 12% (96/784) of patients with moderate to severe plaque psoriasis treated with Otezla and in 5% (19/382) of patients treated with placebo. Body weight loss of ≥10% occurred in 2% (16/784) of patients treated with Otezla compared to 1% (3/382) of patients treated with placebo
Psoriatic Arthritis: Body weight loss of 5-10% was reported in 10% (49/497) of patients taking Otezla and in 3.3% (16/495) of patients taking placebo
Behçet's Disease: Body weight loss of >5% was reported in 4.9% (5/103) of patients taking Otezla and in 3.9% (4/102) of patients taking placebo
Drug Interactions: Apremilast exposure was decreased when Otezla was co-administered with rifampin, a strong CYP450 enzyme inducer; loss of Otezla efficacy may occur. Concomitant use of Otezla with CYP450 enzyme inducers (e.g., rifampin, phenobarbital, carbamazepine, phenytoin) is not recommended
Adverse Reactions
Plaque Psoriasis: The most common adverse reactions (≥ 5%) are diarrhea, nausea, upper respiratory tract infection, and headache, including tension headache. Overall, the safety profile of Otezla in patients with mild to moderate plaque psoriasis was consistent with the safety profile previously established in adult patients with moderate to severe plaque psoriasis
Psoriatic Arthritis: The most common adverse reactions (≥ 5%) are diarrhea, nausea, and headache
Behçet's Disease: The most common adverse reactions (≥ 10%) are diarrhea, nausea, headache, and upper respiratory tract infection
Use in Specific Populations
Otezla has not been studied in pregnant women. Advise pregnant women of the potential risk of fetal loss.
Please click here for Otezla® Full Prescribing Information.
About Atopic Dermatitis
Atopic dermatitis is a chronic inflammatory disease that causes excessively dry, itchy skin that can be painful. Repeated scratching can cause the skin to thicken, harden or become vulnerable to infection. Atopic dermatitis is the most common form of eczema – affecting 1-3% of adults worldwide – and the prevalence is increasing. The disease typically manifests in childhood followed by other allergy symptoms.
About
rocatinlimab
Rocatinlimab (AMG 451/KHK4083), an investigational product, is a potential first-in-class anti-OX40 monoclonal antibody that is being studied for its ability to inhibit and reduce the number of OX40+ pathogenic T cells responsible for driving systemic and local AD inflammatory responses.
It has been reported that effector T cells expressing OX40 are present in the lesions of patients with atopic dermatitis and are critical in the disease pathophysiology. The initial antibody was discovered in collaboration between Kyowa Kirin US Research and La Jolla Institute for Immunology.
Amgen and Kyowa Kirin Collaboration
On June 1, 2021, Kyowa Kirin and Amgen entered into an agreement to jointly develop and commercialize rocatinlimab. Under the terms of the agreement, Amgen will lead the development, manufacturing, and commercialization for KHK4083/AMG 451 for all markets globally, except Japan, where Kyowa Kirin will retain all rights. If approved, the companies will co-promote the asset in the United States and Kyowa Kirin has opt-in rights to co-promote in certain other markets including Europe and Asia.
About Amgen
Amgen is committed to unlocking the potential of biology for patients suffering from serious illnesses by discovering, developing, manufacturing and delivering innovative human therapeutics. This approach begins by using tools like advanced human genetics to unravel the complexities of disease and understand the fundamentals of human biology.
Amgen focuses on areas of high unmet medical need and leverages its expertise to strive for solutions that improve health outcomes and dramatically improve people's lives. A biotechnology pioneer since 1980, Amgen has grown to be one of the world's leading independent biotechnology companies, has reached millions of patients around the world and is developing a pipeline of medicines with breakaway potential.
Amgen is one of the 30 companies that comprise the Dow Jones Industrial Average and is also part of the Nasdaq-100 index. In 2023, Amgen was named one of "America's Greatest Workplaces" by Newsweek, one of "America's Climate Leaders" by USA Today and one of the "World's Best Companies" by TIME.
For more information, visit Amgen.com and follow us on X (formerly known as Twitter), LinkedIn, Instagram, TikTok, YouTube and Threads.
Amgen Forward-Looking Statements
This news release contains forward-looking statements that are based on the current expectations and beliefs of Amgen. All statements, other than statements of historical fact, are statements that could be deemed forward-looking statements, including any statements on the outcome, benefits and synergies of collaborations, or potential collaborations, with any other company (including BeiGene, Ltd. or Kyowa Kirin Co., Ltd.), the performance of Otezla® (apremilast) (including anticipated Otezla sales growth and the timing of non-GAAP EPS accretion), our acquisitions of Teneobio, Inc., ChemoCentryx, Inc., or Horizon Therapeutics plc (including the prospective performance and outlook of Horizon's business, performance and opportunities, any potential strategic benefits, synergies or opportunities expected as a result of such acquisition, and any projected impacts from the Horizon acquisition on our acquisition-related expenses going forward), as well as estimates of revenues, operating margins, capital expenditures, cash, other financial metrics, expected legal, arbitration, political, regulatory or clinical results or practices, customer and prescriber patterns or practices, reimbursement activities and outcomes, effects of pandemics or other widespread health problems on our business, outcomes, progress, and other such estimates and results. Forward-looking statements involve significant risks and uncertainties, including those discussed below and more fully described in the Securities and Exchange Commission reports filed by Amgen, including our most recent annual report on Form 10-K and any subsequent periodic reports on Form 10-Q and current reports on Form 8-K. Unless otherwise noted, Amgen is providing this information as of the date of this news release and does not undertake any obligation to update any forward-looking statements contained in this document as a result of new information, future events or otherwise.
No forward-looking statement can be guaranteed and actual results may differ materially from those we project. Discovery or identification of new product candidates or development of new indications for existing products cannot be guaranteed and movement from concept to product is uncertain; consequently, there can be no guarantee that any particular product candidate or development of a new indication for an existing product will be successful and become a commercial product. Further, preclinical results do not guarantee safe and effective performance of product candidates in humans. The complexity of the human body cannot be perfectly, or sometimes, even adequately modeled by computer or cell culture systems or animal models. The length of time that it takes for us to complete clinical trials and obtain regulatory approval for product marketing has in the past varied and we expect similar variability in the future. Even when clinical trials are successful, regulatory authorities may question the sufficiency for approval of the trial endpoints we have selected. We develop product candidates internally and through licensing collaborations, partnerships and joint ventures. Product candidates that are derived from relationships may be subject to disputes between the parties or may prove to be not as effective or as safe as we may have believed at the time of entering into such relationship. Also, we or others could identify safety, side effects or manufacturing problems with our products, including our devices, after they are on the market.
Our results may be affected by our ability to successfully market both new and existing products domestically and internationally, clinical and regulatory developments involving current and future products, sales growth of recently launched products, competition from other products including biosimilars, difficulties or delays in manufacturing our products and global economic conditions. In addition, sales of our products are affected by pricing pressure, political and public scrutiny and reimbursement policies imposed by third-party payers, including governments, private insurance plans and managed care providers and may be affected by regulatory, clinical and guideline developments and domestic and international trends toward managed care and healthcare cost containment. Furthermore, our research, testing, pricing, marketing and other operations are subject to extensive regulation by domestic and foreign government regulatory authorities. Our business may be impacted by government investigations, litigation and product liability claims. In addition, our business may be impacted by the adoption of new tax legislation or exposure to additional tax liabilities. If we fail to meet the compliance obligations in the corporate integrity agreement between us and the U.S. government, we could become subject to significant sanctions. Further, while we routinely obtain patents for our products and technology, the protection offered by our patents and patent applications may be challenged, invalidated or circumvented by our competitors, or we may fail to prevail in present and future intellectual property litigation. We perform a substantial amount of our commercial manufacturing activities at a few key facilities, including in Puerto Rico, and also depend on third parties for a portion of our manufacturing activities, and limits on supply may constrain sales of certain of our current products and product candidate development. An outbreak of disease or similar public health threat, such as COVID-19, and the public and governmental effort to mitigate against the spread of such disease, could have a significant adverse effect on the supply of materials for our manufacturing activities, the distribution of our products, the commercialization of our product candidates, and our clinical trial operations, and any such events may have a material adverse effect on our product development, product sales, business and results of operations. We rely on collaborations with third parties for the development of some of our product candidates and for the commercialization and sales of some of our commercial products. In addition, we compete with other companies with respect to many of our marketed products as well as for the discovery and development of new products. Further, some raw materials, medical devices and component parts for our products are supplied by sole third-party suppliers. Certain of our distributors, customers and payers have substantial purchasing leverage in their dealings with us. The discovery of significant problems with a product similar to one of our products that implicate an entire class of products could have a material adverse effect on sales of the affected products and on our business and results of operations. Our efforts to collaborate with or acquire other companies, products or technology, and to integrate the operations of companies or to support the products or technology we have acquired, may not be successful. There can be no guarantee that we will be able to realize any of the strategic benefits, synergies or opportunities arising from the Horizon acquisition, and such benefits, synergies or opportunities may take longer to realize than expected. We may not be able to successfully integrate Horizon, and such integration may take longer, be more difficult or cost more than expected. A breakdown, cyberattack or information security breach of our information technology systems could compromise the confidentiality, integrity and availability of our systems and our data. Our stock price is volatile and may be affected by a number of events. Our business and operations may be negatively affected by the failure, or perceived failure, of achieving our environmental, social and governance objectives. The effects of global climate change and related natural disasters could negatively affect our business and operations. Global economic conditions may magnify certain risks that affect our business. Our business performance could affect or limit the ability of our Board of Directors to declare a dividend or our ability to pay a dividend or repurchase our common stock. We may not be able to access the capital and credit markets on terms that are favorable to us, or at all.
The scientific information discussed in this news release related to our product candidates is preliminary and investigative. Such product candidates are not approved by the U.S. Food and Drug Administration, and no conclusions can or should be drawn regarding the safety or effectiveness of the product candidates. Further, any scientific information discussed in this news release relating to new indications for our products is preliminary and investigative and is not part of the labeling approved by the U.S. Food and Drug Administration for the products. The products are not approved for the investigational use(s) discussed in this news release, and no conclusions can or should be drawn regarding the safety or effectiveness of the products for these uses.
CONTACT: Amgen, Thousand Oaks
Kate Meyer, 872-867-0754 (media)
Jessica Akopyan, 805-440-5721 (media)
Justin Claeys, 805-313-9775 (investors)
References
1Fiorillo L, Becker E, de Lucas R, Belloni-Fortina A, Armesto S, Maes P, Oberoi R, Paris M, Zhang W, Zhang Z, & Arkin L. Efficacy and safety results of apremilast in pediatric patients with moderate to severe plaque psoriasis: 16-week results from SPROUT, a phase 3, randomized, controlled study. SKIN, 2023;7(2):s109; .
2Fiorillo L, et al. Efficacy and Safety of Apremilast in Pediatric Patients With Moderate to Severe Plaque Psoriasis: 52-Week Results From the SPROUT Randomized Controlled Trial. AAD Annual Meeting, March 2024.
3Brunasso AMG and Massone C. Recent advances in palmoplantar pustulosis. Faculty Reviews 2021 10:(62) .
4Chung J, Callis Duffin K, Takeshita J, Shin DB, Krueger GG, Robertson AD, et al. Palmoplantar psoriasis is associated with greater impairment of health-related quality of life compared with moderate to severe plaque psoriasis. J Am Acad Dermatol. 2014 Oct; 71(4):623-32. doi: 10.1016/j.jaad.2014.04.063.
5 Terui T, et all. Efficacy and Safety of Apremilast for the Treatment of Japanese Patients With Palmoplantar Pustulosis (PPP): 16-Week Results From a Phase 3, Randomized, Placebo-Controlled Study. AAD Annual Meeting, March 2024.
6National Psoriasis Foundation. About Psoriasis. Available at: . Accessed January 30, 2024.
7National Psoriasis Foundation. Statistics. Available at: . Accessed January 30, 2024.
8Ortonne JP, Prinz JC. Alefacept: a novel and selective biologic agent for the treatment of chronic plaque psoriasis. Eur J Dermatol. 2004;14(1):41–45.
9National Psoriasis Foundation. Plaque Psoriasis. Available at: . Accessed January 30, 2024.
10Amgen Data on File. November 2023.
SOURCE Amgen
临床结果临床2期临床3期上市批准引进/卖出
100 项与 Saint-Pierre University Hospital 相关的药物交易
登录后查看更多信息
100 项与 Saint-Pierre University Hospital 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年04月05日管线快照
无数据报导
登录后保持更新
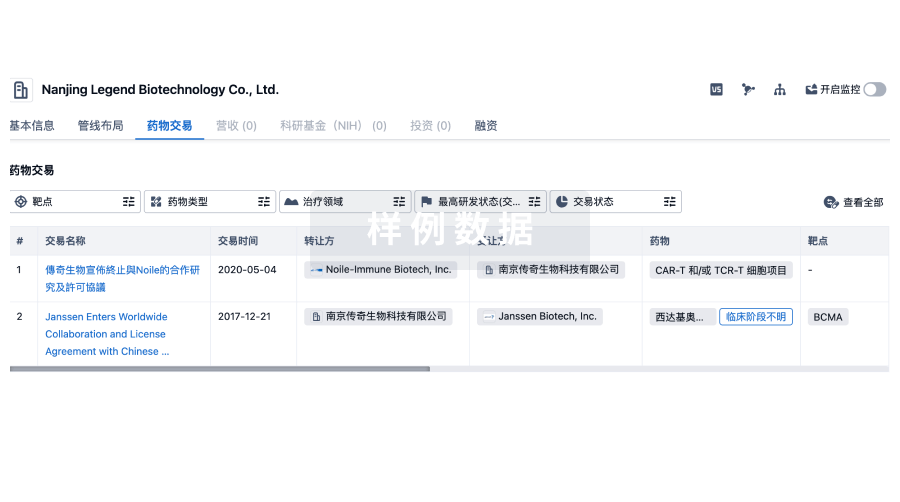
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
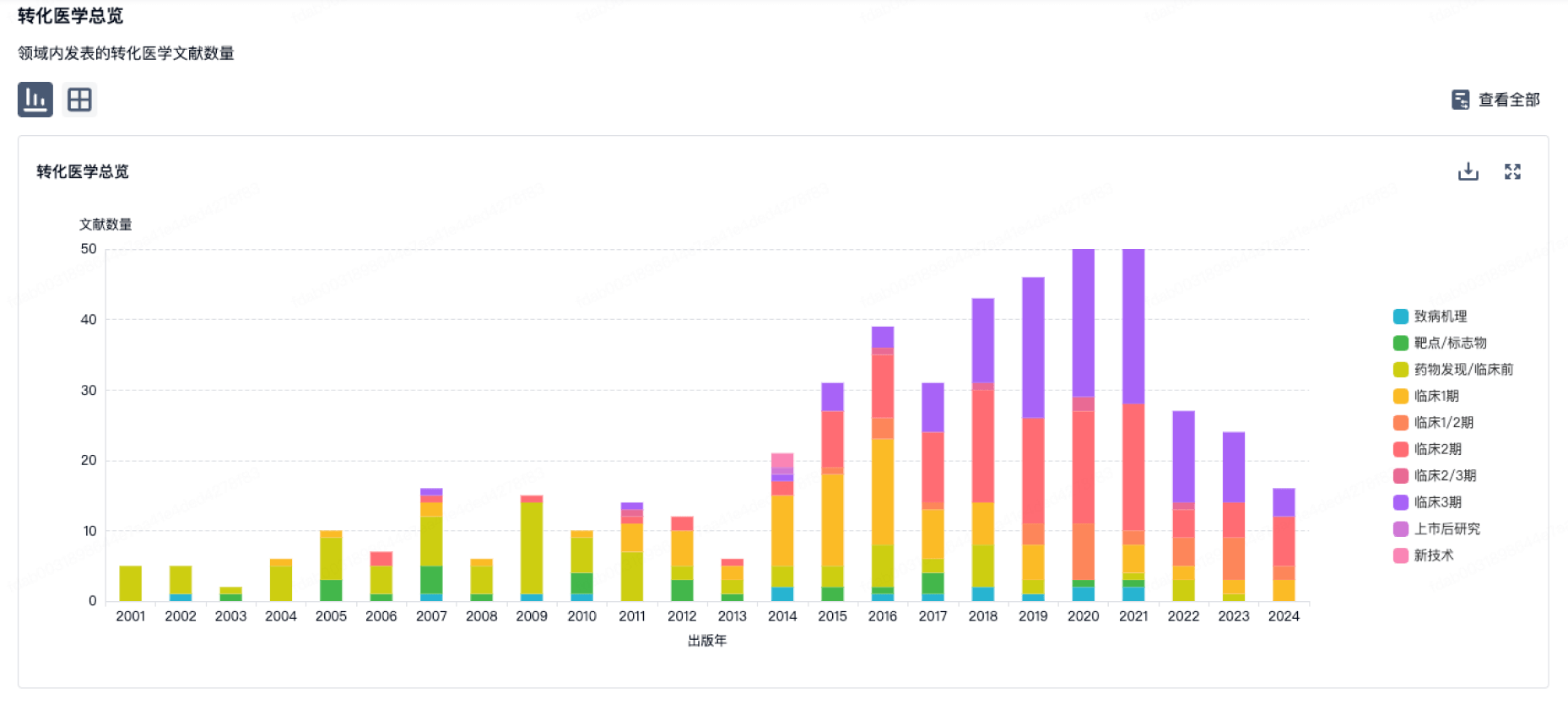
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
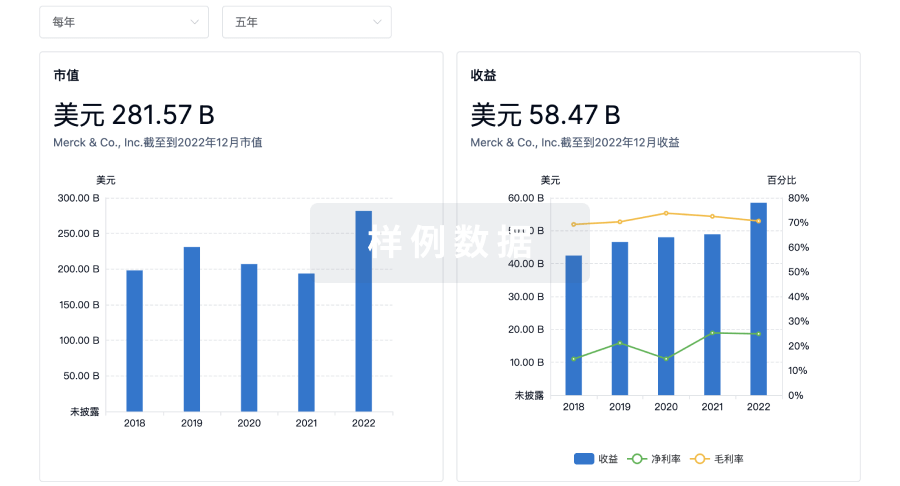
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
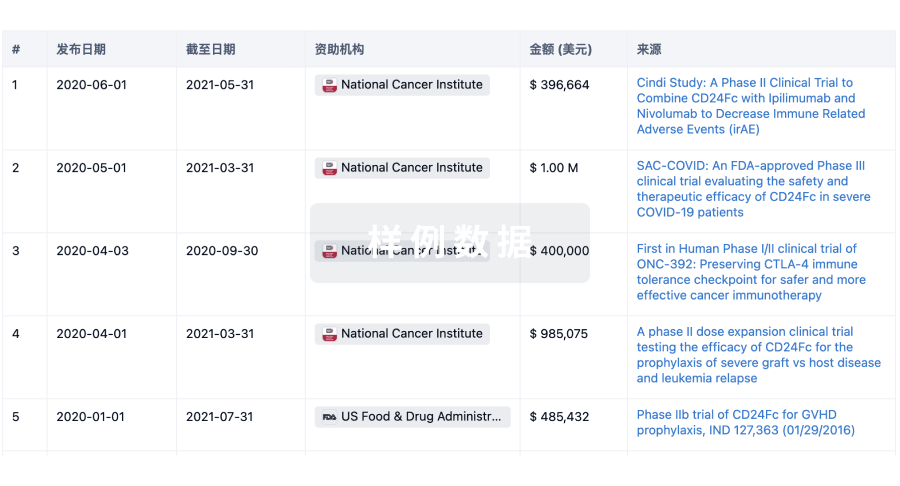
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
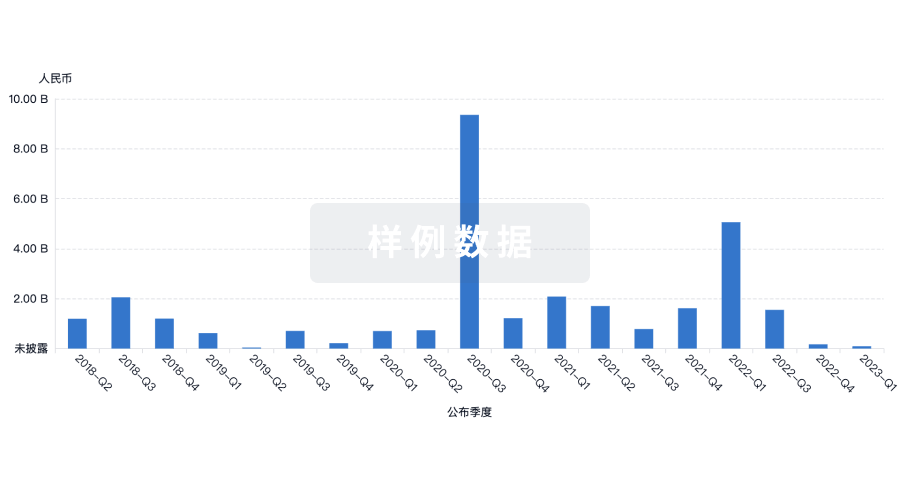
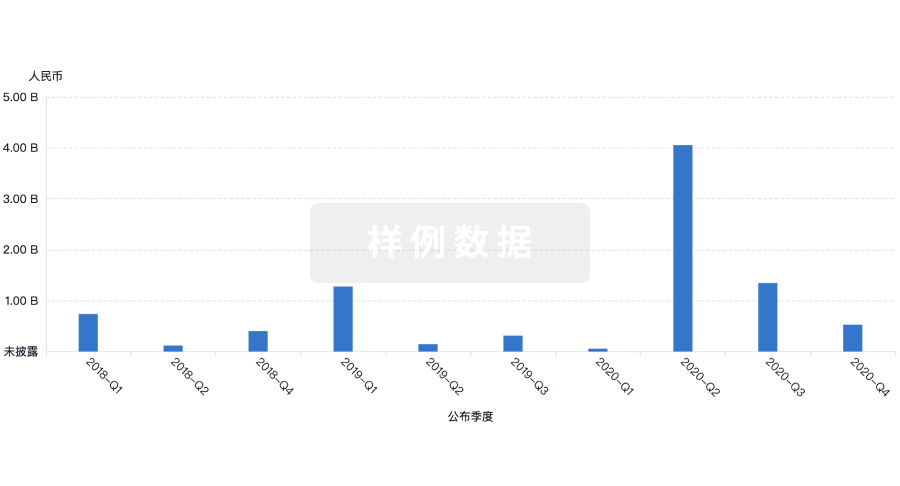
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用