预约演示
更新于:2025-12-07

Centre Hospitalier Universitaire Amiens-Picardie
更新于:2025-12-07
概览
关联
599
项与 Centre Hospitalier Universitaire Amiens-Picardie 相关的临床试验NCT07256470
Salivary Replication of BK Virus in Post-kidney Transplant
BK virus infection in kidney transplantation can compromise graft function. Current data suggest that BK virus nephropathy results not only from transmission of virus from the donor but also from reactivation of latent virus in the recipient. However, no study has investigated the possibility of respiratory transmission. This study would provide a better understanding of the pathophysiology of BK virus infection in kidney transplant recipients. The investigators would study viral replication of BK virus in saliva, urine and blood of patients who received a kidney transplant at the Amiens University Hospital. For this, the investigators will collect salivary self-collection on the day of the kidney transplant then at 1, 3, 6, 9 and 12 months as well as a urine and blood sample. The investigators will mesure BK viral load in these three samples at different times.
开始日期2025-12-01 |
NCT07211841
Correlative Analysis Between Magnetic Resonance Spectroscopy (MRS) and Essential Clinicobiological Data in Glioblatoma Multiforme (GBM)
Glioblastoma multiforme (GBM) is the most common primary brain tumor, and it is well-known to be associated with a poor prognosis. MRI is the key medical technique for the diagnosis and the follow-up of GBM. By allowing for MRS studies, MRI permits a non-invasive characterization of the TME of GBM, including their metabolic characterization. The investigators propose to address the link between the MRS profile of GBM and basic clinical and biological parameters, with the aim of : i) identifying correlations between these parameters, ii) attempting to integrate clinical, biological and spectroscopic profiles of GBM. The investigators plan to recruit 30 newly diagnosed GBM patients for which surgery / radiochemotherapy will be proposed in the Medical oncology unit of Amiens University Hospital. Following inclusion of patients with probable GBM, MRS study will be performed during the first (pre-therapeutic) MRI examination. Basic clinical and biological parameters of the blood (CRP, complete blood count, fibrinogen, lactate and choline) will be assessed. A metabolomic study will also be performed on the plasma of GBM patients before any therapeutics. A second biological, post-therapeutic assesment (one month after surgery/radiochemotherapy) will allow the same analyses (basic biological parameters + plasma metabolomics), in order to examine the stability of the blood parameters.
开始日期2025-12-01 |
NCT07030803
Comparative Study of the Efficacy of Treatment of Idiopathic Overactive Bladder (OAB) in Children: Oxybutynine vs. Transcutaneous Neurostimulation
The absence of infectious, urological and neurological causes defines the idiopathic character of overactive bladder (OAB). Although a progressive approach starting with behavioural therapy (urotherapy) is recommended, anticholinergic agents remain the mainstay of medical treatment of overactive bladder (OAB) in children. Bladder neuromodulation is also used but no study with sufficient evidence has assessed its effectiveness and tolerance compared to the reference treatment. The purpose of HAV-O-TENS is to demonstrate the non-inferiority of treating idiopathic overactive bladder (OAB) in children using posterior tibial nerve stimulation (PTNS) compared to the reference treatment with oxybutynin after three months of treatment.
Before inclusion, patients will receive instructions for urotherapy and a treatment plan. After confirming the diagnosis and obtaining informed consent, patients will be randomly assigned to either oxybutynin or PTNS (posterior tibial nerve stimulation) treatment, and their effectiveness, tolerance, and adherence will be monitored.
Before inclusion, patients will receive instructions for urotherapy and a treatment plan. After confirming the diagnosis and obtaining informed consent, patients will be randomly assigned to either oxybutynin or PTNS (posterior tibial nerve stimulation) treatment, and their effectiveness, tolerance, and adherence will be monitored.
开始日期2025-11-05 |
100 项与 Centre Hospitalier Universitaire Amiens-Picardie 相关的临床结果
登录后查看更多信息
0 项与 Centre Hospitalier Universitaire Amiens-Picardie 相关的专利(医药)
登录后查看更多信息
175
项与 Centre Hospitalier Universitaire Amiens-Picardie 相关的文献(医药)2025-12-01·ENCEPHALE-REVUE DE PSYCHIATRIE CLINIQUE BIOLOGIQUE ET THERAPEUTIQUE
Validation of a French Fear of Missing Out Scale
Article
作者: Del Monte, Jonathan ; Andraos, Elie ; Graziani, Pierluigi
This study aimed to translate and assess the psychometric properties of a French Fear of Missing Out scale (PPC). The Fear of missing out is defined as a "pervasive apprehension that others might be having rewarding experiences from which one is absent; it is characterized by the desire to remain continually connected to what others are doing". One hundred and thirty-eight participants completed the PPC, a French version of the Internet Addiction Test - Social Media (IAT-RS), a French Smartphone Addiction Scale - Short Version (SAS-SV) and some subscales of the French Revised Symptom Checklist (SCL-90-R) to test the validity of the scale. A principal components analysis revealed an 8-item PPC with a single factor and good internal validity. Correlations with the SAS-SV and the IAT-RS revealed moderate positive correlations confirming the convergent validity of the scale and supporting the use of the scale for further research findings related to the SCL-90-R subscales. Additional analyses allowed us to note that PPC fully mediated the relationship between anxiety and smartphone addiction, as well as between depression and smartphone addiction. It was also revealed that PPC partially mediated the relationship between anxiety and social media addiction and depression and social media addiction. The PPC has good psychometric qualities and opens up the possibility of assessing the fear of missing out in French populations and testing its relationships with various psychological disorders such as addictive behaviors.
2025-11-01·Gynecologie Obstetrique Fertilite & Senologie
Article
作者: Luisin, Marion ; Arene, Marie-Laure ; Touzart, Laurent ; Sergent, Fabrice ; Copin, Henri ; Morin, Gilles
OBJECTIVES:
Congenital anomalies of the kidney and urinary tract (CAKUT) account for one-third of all congenital malformations detected by ultrasound. With the introduction of chromosomal microarrays, over 50 genes involved in CAKUT have been identified. The main objective of our study was to assess the contribution of chromosomal analysis performed for CAKUT within our fetal diagnosis and treatment center.
MATERIAL AND METHODS:
We included pregnancies with CAKUT confirmed by ultrasound from January 2013 to December 2020. Once the diagnosis of CAKUT was established, we collected data about proposal for a fetal sampling, type of fetal sampling and results of fetal sampling. When chromosomal aberration was detected, we recorded the type, size, mode of inheritance (de novo or inherited).
RESULTS:
We realized 53 amniocentesis (70.7%), 12 chronionic villus sampling (16%) and 10 fetal blood sampling (13.3%). Three fetal sampling were excluded and we finally studied 72 samples. Among all cases, four fetuses (5.5%) showed aneuploidies: one case of trisomy 18, one case of trisomy 20 and two cases of trisomy 21. Six fetuses (8.3%) showed copy number variations. After diagnosis and at the request of couple, 9 medical termination of pregnancy were performed.
CONCLUSION:
Chromosomal analysis carried out in the exploration of congenital renal anomalies make it possible to establish a diagnosis in certain cases, and on the other hand make it possible to modify the outcome of pregnancy or the management of future pregnancies. Faced with new emerging techniques and considering the diagnostic rate of congenital renal malformations, these analysis have their place.
2025-11-01·Cancer Radiotherapie
Radiotherapy for hypopharynx cancers: 2025 update
Review
作者: Coutte, Alexandre ; Biau, Julian ; Bocha, Dylan ; Lapeyre, Michel ; Blanchard, Pierre ; Huertas, Andrès ; Delaby, Nolwenn ; Pointreau, Yoann
We present the update of the recommendations of the Société française de radiothérapie oncologique on radiotherapy for hypopharynx. Intensity-modulated radiotherapy is the gold standard treatment for hypopharynx cancers. Early T1 and T2 tumours can be treated by exclusive radiation or surgery followed by postoperative radiation in case of high recurrence risk. For locally advanced tumours requiring total pharyngolaryngectomy (T2 or T3) or with significant lymph nodes involvement, they can be treated by chemoradiation or by induction drugs followed by exclusive radiation. For T4 tumour, surgery must be proposed. Different fractionation schedules are possible: for 35 fractions, the curative dose is 70Gy (delivered at 2Gy per fraction) and prophylactic doses are 50 to 56Gy (delivered at 2Gy per fraction in case of sequential radiotherapy or 1.6Gy in case of simultaneous integrated boost radiotherapy; for 33 fractions, the curative dose is 69.96Gy (delivered at 2.12Gy per fraction) and the prophylactic dose is 52.8Gy (delivered at 1.6Gy per fraction in simultaneous integrated boost radiotherapy or 54Gy in 1.64Gy per fraction); for 30 fractions, curative dose is 66Gy (delivered at 2.2Gy per fraction) and prophylactic dose is 54Gy (delivered at 1.8Gy per fraction in simultaneous integrated boost radiotherapy. Doses over 2Gy per fraction can be delivered when chemotherapy is not used regarding potential larynx toxicity. Postoperatively, radiotherapy is used for locally advanced cancer with dose levels based on pathologic criteria, delivering 60 to 66Gy for R1 resection and 57.6 to 60Gy for complete resection in bed tumour; 50 to 66Gy in lymph nodes areas regarding extracapsular spread. Target volume delineation recommendations were based on guidelines cited in this article.
100 项与 Centre Hospitalier Universitaire Amiens-Picardie 相关的药物交易
登录后查看更多信息
100 项与 Centre Hospitalier Universitaire Amiens-Picardie 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年06月08日管线快照
管线布局中药物为当前组织机构及其子机构作为药物机构进行统计,早期临床1期并入临床1期,临床1/2期并入临床2期,临床2/3期并入临床3期
其他
1
登录后查看更多信息
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
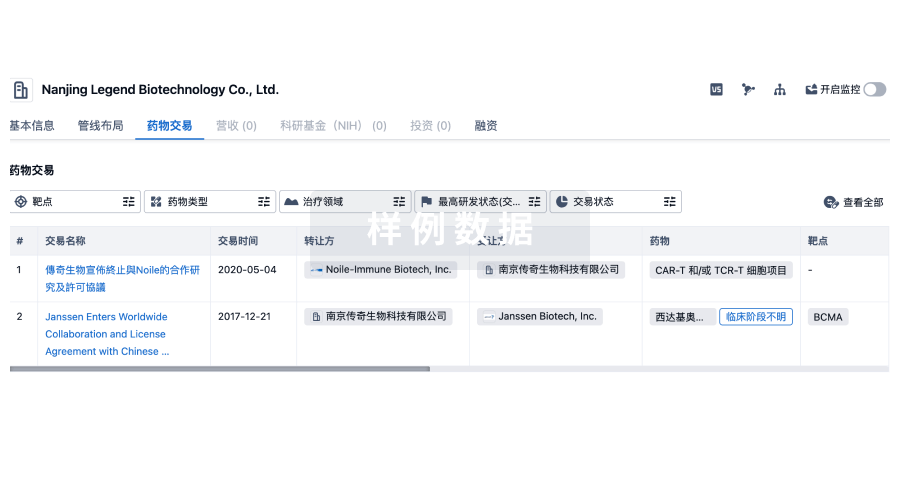
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
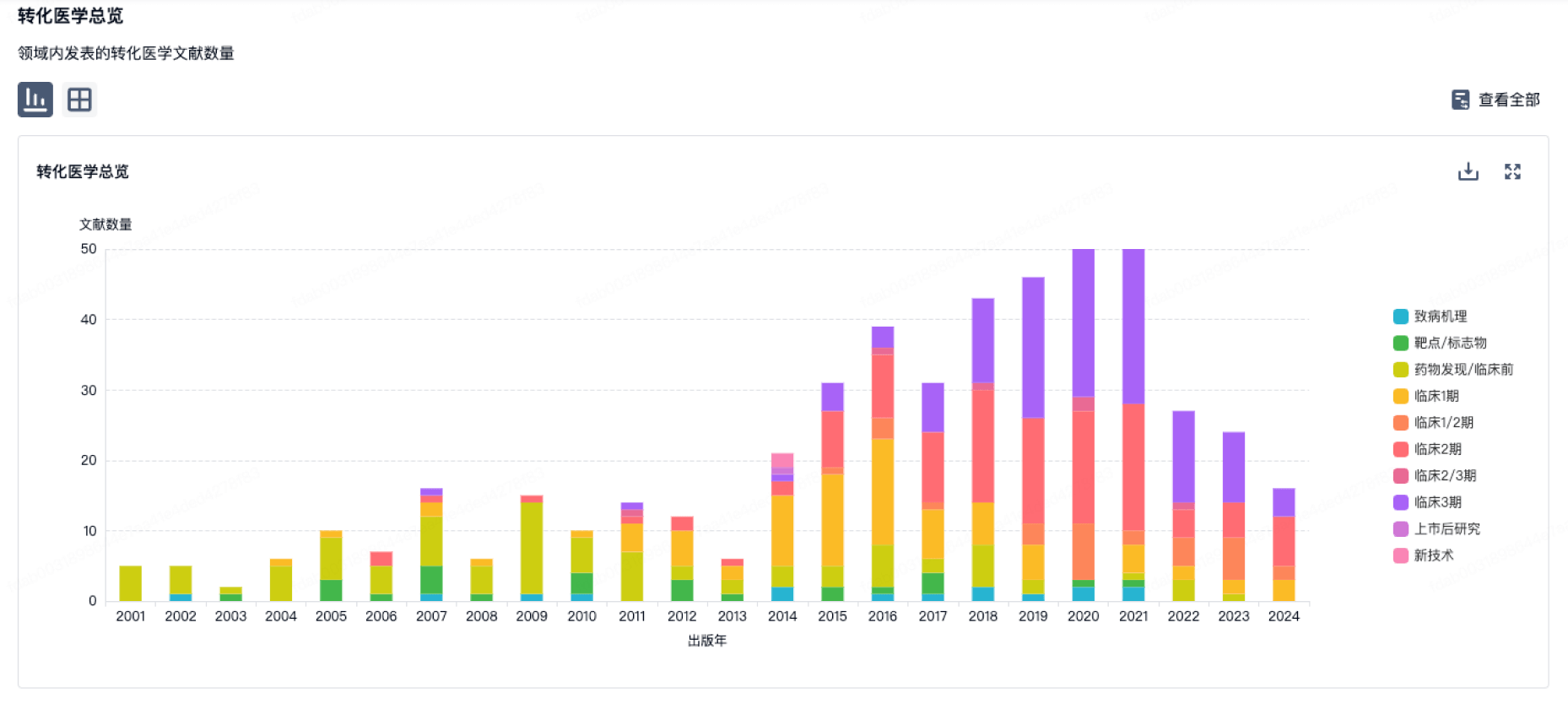
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
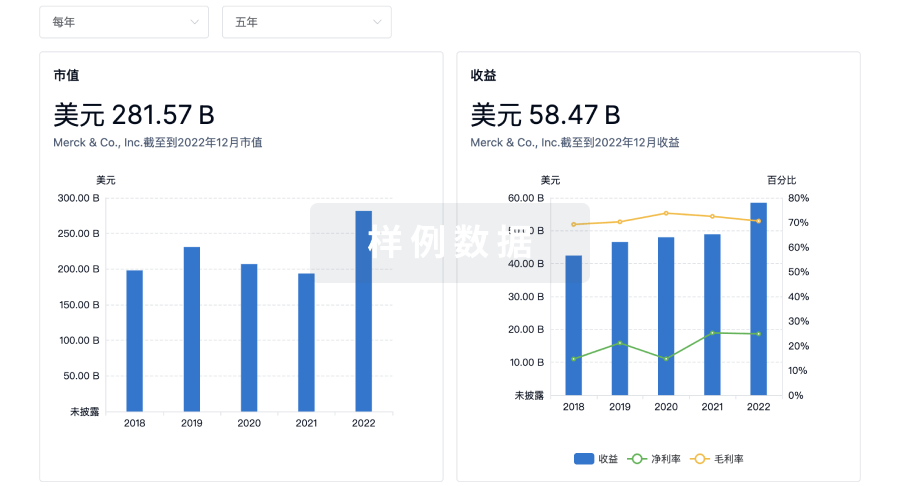
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
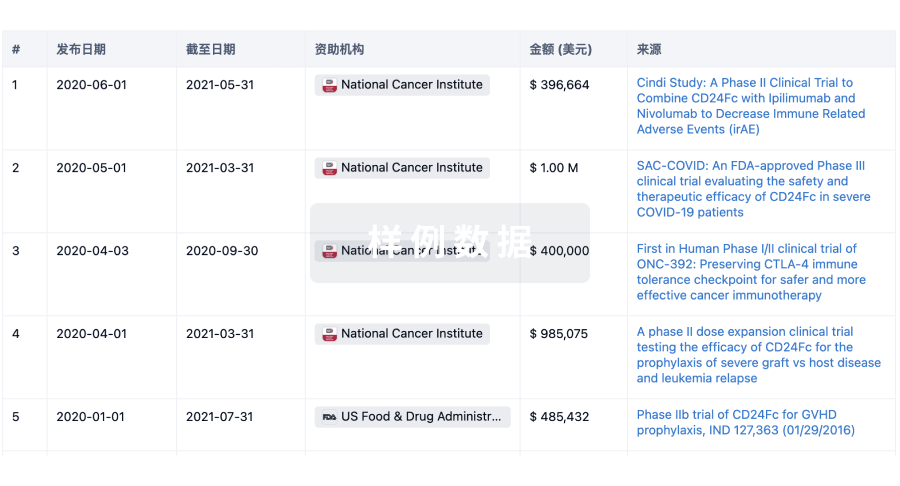
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
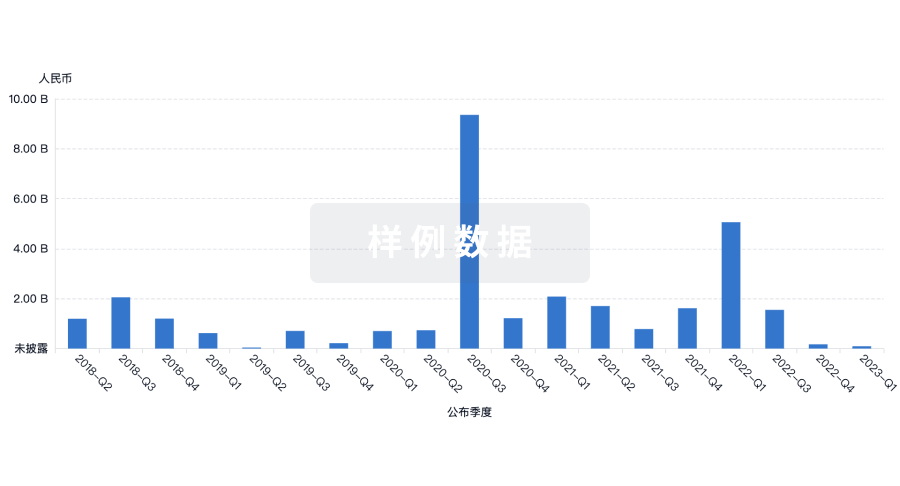
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
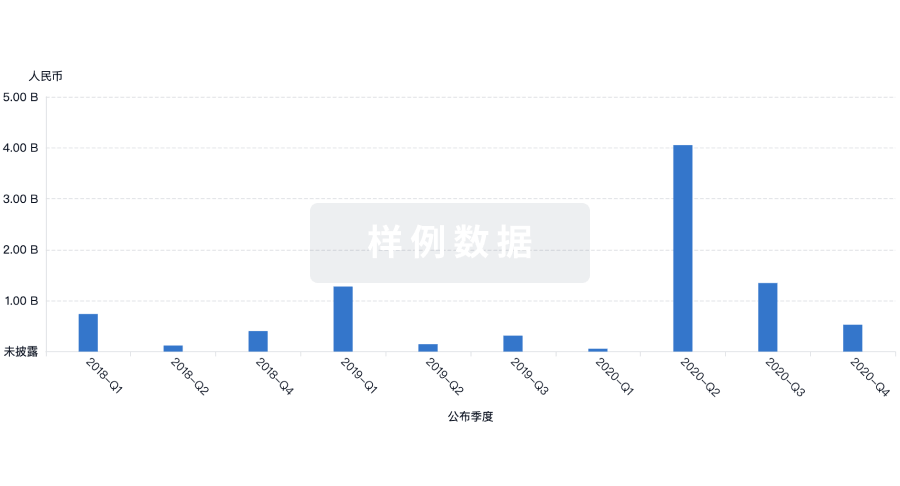
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用