预约演示
更新于:2026-05-23

British University of Egypt
更新于:2026-05-23
概览
标签
肿瘤
小分子化药
疾病领域得分
一眼洞穿机构专注的疾病领域
暂无数据
技术平台
公司药物应用最多的技术
暂无数据
靶点
公司最常开发的靶点
暂无数据
| 疾病领域 | 数量 |
|---|---|
| 肿瘤 | 4 |
| 排名前五的药物类型 | 数量 |
|---|---|
| 小分子化药 | 4 |
| 排名前五的靶点 | 数量 |
|---|---|
| TrkA(神经生长因子受体Trk-A) | 4 |
关联
4
项与 British University of Egypt 相关的药物靶点 |
作用机制 TrkA 拮抗剂 |
在研适应症 |
非在研适应症- |
最高研发阶段临床前 |
首次获批国家/地区- |
首次获批日期- |
靶点 |
作用机制 TrkA 拮抗剂 |
在研适应症 |
非在研适应症- |
最高研发阶段临床前 |
首次获批国家/地区- |
首次获批日期- |
靶点 |
作用机制 TrkA 拮抗剂 |
在研适应症 |
非在研适应症- |
最高研发阶段临床前 |
首次获批国家/地区- |
首次获批日期- |
80
项与 British University of Egypt 相关的临床试验NCT07492576
Evaluation of the Magnesium Shield Compared to Dual Zone Grafting Approach in Immediate Implant Site Management: a Randomized Controlled Clinical Trial
Will (GBR) by application of magnesium membrane with immediate implant will have more volume gain , higher pink esthetic score, and lower visual analogue scale than dual zone grafting technique? Several methods have been suggested for the preservation of post-extraction resorption and promoting an increase in the bone density with immediate implant placement. one of these techniques is the dual zone concept (DZ), atraumatic tooth extraction using peristomes and luxators, implant placement along with the bone grafting material applied to both the bone and tissue zones.
The aim of (DZ) is to augment the soft tissue using a bone graft to avoid mucosal recession after implant placement thus keeping the gingival contour providing optimal soft tissue aesthetic.
The use of magnesium membrane in combination with inorganic bovine bones will be placed between the membrane and immediate implant. This allows implant placement while simultaneously rehabilitating the entire socket, due to its unique material properties, a magnesium membrane is used to rebuild, support the buccal or oral walls in compromised sockets, and promotes cortical bone growth . Many techniques available for preserving the bone of the socket post-tooth extraction, but in comparison to the current materials and techniques used , magnesium membrane is completely resorbable and does not require second surgery to be removed; it is synthetic and therefore does not need to be sourced from an additional surgical. magnesium membrane is excellent in providing both esthetic and functional outcomes that meet patient expectations.
The procedure involves flapless approach in which atraumatic tooth extraction using peristomes and forceps will be performed to preserve the available alveolar bone. The implant site will be prepared, and the implant will be placed palatal and 3-4m.m apical to the free gingival margin (FGM). magnesium membrane will be placed between the soft tissue and thin buccal wall. The edges of the membrane will be shaped and flattened with sculptor to prevent perforation of the soft tissue, and a layer off inorganic bovine bone will be placed between the e buccal wall and implant. Then immediate provisional restoration will be constructed and placed to allow an ideal final crown mimicking the natural emergence profile.
The aim of (DZ) is to augment the soft tissue using a bone graft to avoid mucosal recession after implant placement thus keeping the gingival contour providing optimal soft tissue aesthetic.
The use of magnesium membrane in combination with inorganic bovine bones will be placed between the membrane and immediate implant. This allows implant placement while simultaneously rehabilitating the entire socket, due to its unique material properties, a magnesium membrane is used to rebuild, support the buccal or oral walls in compromised sockets, and promotes cortical bone growth . Many techniques available for preserving the bone of the socket post-tooth extraction, but in comparison to the current materials and techniques used , magnesium membrane is completely resorbable and does not require second surgery to be removed; it is synthetic and therefore does not need to be sourced from an additional surgical. magnesium membrane is excellent in providing both esthetic and functional outcomes that meet patient expectations.
The procedure involves flapless approach in which atraumatic tooth extraction using peristomes and forceps will be performed to preserve the available alveolar bone. The implant site will be prepared, and the implant will be placed palatal and 3-4m.m apical to the free gingival margin (FGM). magnesium membrane will be placed between the soft tissue and thin buccal wall. The edges of the membrane will be shaped and flattened with sculptor to prevent perforation of the soft tissue, and a layer off inorganic bovine bone will be placed between the e buccal wall and implant. Then immediate provisional restoration will be constructed and placed to allow an ideal final crown mimicking the natural emergence profile.
开始日期2026-03-19 |
申办/合作机构 |
NCT07457749
Clinical Performance of a Novel Self-cured Resin Composite Compared to a Light-cured Bioactive Resin Composite Restoration in Proximal Cavities of Posterior Teeth: A 2-year Randomized Controlled Clinical Trial
The development of dental caries is multi-factorial mainly due to the presence of 4 elements which are: dental biofilm, fermentable carbohydrates , dental hard tissue and time. Other additional social and environmental factors can have a substantial impact on the onset and course of the disease. Dietary habits, oral hygiene, salivary flow and fluoride exposure are key factors that influence the susceptibility to dental caries. If dental caries is properly managed, it is a preventable and reversible disease. The proximal teeth surfaces are the most susceptible sites for demineralization from the acidic byproducts. In modern restorative dentistry, clinicians always seek solutions that streamline procedures, improve outcomes and reduce chair time for patients. Traditional light-cured composite systems often involve a complex seven step process which includes etching, priming, bonding and curing which consumes from 90 to 120 seconds to be completed. With each additional step, the risk of technique errors increases, potentially compromising the longevity of the restoration. Self-cure composites, with their simplified application process, are emerging as a preferred choice over the traditional seven-step composite materials. Recently, a novel self-cured high-performance bulk-fill restorative material has been introduced into the market (Stela, SDI, Victoria, Australia). It's particularly known for its "unlimited" depth of cure and self-adhesive properties.
开始日期2026-02-18 |
申办/合作机构 |
NCT07368621
Effectiveness of Connective Tissue Graft With and Without Leukocyte Platelet Rich Fibrin on Peri-implant Soft Tissue Thickness Around Delayed Implants in Patients With Thin Gingival Phenotype: A Randomized Controlled Clinical Trial
A stable soft and hard tissues around Osseo-integrated implants are very crucial. Soft tissue thickness around implants is crucial as it prevents peri-implant bone loss and enhance the esthetic outcomes. The treatment of thin tissue phenotype should be improved as the thin tissue phenotype will lead to plaque accumulation. There are some techniques that can increase the thickness of the peri-implant mucosa including connective tissue graft, platelet- rich fibrin and xenogeneic collagen matrix .Leukocyte and Platelet rich fibrin is a second generation platelet concentrate that was introduced by choukroun et al in 2001 after platelet rich plasma. PRF is the first source of autogenous blood derived growth factors harvested without the use of anticoagulants5. It contains various growth factors that are believed to contribute to periodontal regeneration. It promotes neovascularization and accelerated wound closing
开始日期2026-01-16 |
申办/合作机构 |
100 项与 British University of Egypt 相关的临床结果
登录后查看更多信息
0 项与 British University of Egypt 相关的专利(医药)
登录后查看更多信息
602
项与 British University of Egypt 相关的文献(医药)2026-05-01·PERSONALITY AND SOCIAL PSYCHOLOGY BULLETIN
Are Mediterranean Societies “Cultures of Honor?”: Prevalence and Implications of a Cultural Logic of Honor Across Three World Regions
Article
作者: Uskul, Ayse K. ; Ishii, Keiko ; Gezici-Yalçın, Meral ; Na, Jinkyung ; Harb, Charles ; Psaltis, Charis ; Karamaouna, Panagiota ; Cross, Susan E. ; Rabie, Dina ; Matamoros-Lima, Juan ; Bossom, Isabella R. L. ; Miniesy, Rania ; Vignoles, Vivian L. ; Özkan, Zafer ; Castillo, Vanessa A. ; Rodriguez-Bailón, Rosa ; Kateri, Evangelia ; Uchida, Yukiko ; Kafetsios, Konstantinos ; Teresi, Manuel ; Wohl, Michael J. A. ; Pagliaro, Stefano ; Kirchner-Häusler, Alexander
Mediterranean societies are often labeled as “honor cultures,” in contrast with presumed “dignity” and “face” cultures of Anglo-Western and East Asian societies. We measured these cultural logics in two large-scale surveys (Studies 1 & 3:
N
= 2,942 students from 11 societies; Study 2:
N
= 5,471 adults from 14 societies). Middle Eastern and North African groups perceived honor values as the most normative in their societies, followed by Southeast European, and then Latin-European groups (who were comparable to Anglo-Western and East-Asian groups). East-Asian and Anglo-Western groups, respectively, perceived face and dignity values as most normative. Culture-level variation in perceived normative honor values, but not personal values, accounted for previously reported differences between Mediterranean and non-Mediterranean samples in several (but not all) measures of social cognitive tendencies. We conclude that a cultural logic of honor plays a role in Mediterranean societies, but labeling these societies as “honor cultures” is oversimplistic.
2026-05-01·European journal of dentistry
Bovine Teeth as Substitutes for Human Teeth in Dental Research: Ultrastructural and Radiographic Analysis
Article
作者: Shamel, Mohamed ; Mahmoud, Heba ; Baz, Safaa ; Bakr, Mahmoud M ; Al Ankily, Mahmoud
Abstract:
Obtaining an alternative for human teeth in research remains challenging. The current study aimed to determine the validity of utilizing bovine teeth as a substitute for human teeth.Sound human maxillary premolars and bovine permanent lower central incisors were obtained. The human and bovine teeth were divided into groups (n = 35) for scanning electron microscope (SEM) analysis alongside energy-dispersive X-ray spectroscopy (EDX) and optical radiographic density.The data was statistically analyzed using the one-way analysis of variance along with a paired sample t-test, comparing the means of each two groups. The results were expressed as means ± standard deviations, and statistical significance was determined at an alpha level of 0.05.SEM analysis of human and bovine samples in different hard tissues showed minor changes, mainly the human enamel had a smoother surface with distinct prism profiles, whereas the bovine dentin had larger and more widely separated dentinal tubules. EDX analysis revealed that the compositions of Ca and P, along with their Ca/P ratios in terms of enamel, dentin, and cementum, were comparable. For radiographic density, the findings revealed minor differences between human and bovine samples. No statistically significant differences among the studied groups were detected.This study revealed minor variations in structure, chemical composition, and radiographic density between human and bovine hard tissues, but without statistical significance, supporting the utilization of bovine teeth as a substitute for that of humans in dental research.
2026-04-01·Odontology
Enhancing severely compromised premolar strength: role of cusp reduction design in CAD/CAM composite restorations
Article
作者: Mohamed, Ahmed Refaat ; Schafer, Edgar ; Swelam, Samar Elsayed ; Saber, Shehabeldin ; Haridy, Mohamed F ; Haridy, Youssef M ; Ahmed, Hend S
Abstract:
The objective of this study was to assess the effect of different designs and depths of cusp reduction on fracture resistance of maxillary permanent premolars restored with CAD/CAM composite restorations. A total of 42 sound maxillary premolars were used. Standardized MOD cavities were prepared in all specimens. Teeth were randomly divided according to form of cusp reduction into three main groups (
n
= 14); G1:MOD cavities restored with inlays with no cusp reduction, G2:MOD cavities restored with overlays with buccal and palatal anatomical cusps reduction, G3; MOD cavities restored with overlays with buccal and palatal flat cusps reduction. Groups 2 and 3 were further sub-divided into two sub-groups (
n
= 7) according to amount of cusp reduction either 1.5 mm or 2.5 mm. All groups were restored by CAD/CAM resin composite indirect restorations and cemented by adhesive resin cement. Thermocycling was done for all specimens. Fracture resistance was tested by universal testing machine and failure modes were examined by stereomicroscope. Statistically analysis was done for all data. Fracture resistance showed significant differences among the experimental groups (
p
< 0.001) with the highest fracture resistance for overlays with 2.5 mm of anatomical reduction. Regarding the modes of failure, there were no significant differences between experimental groups (
p
= 0.489). The fracture resistance of the composite CAD/CAM fabricated restorations is highly influenced by the restoration/prep design. The overlay design with anatomical cusps reduction of 2.5 mm can reinforce maxillary premolars teeth with MOD cavities.
1
项与 British University of Egypt 相关的新闻(医药)2022-10-20
Researchers at the British university have developed a proof of concept for a new diagnostic tool that could deliver health test results in two minutes using a fingertip sample
The new diagnostic tool can deliver health test results in two minutes because of the use of AI and ML. (Credit: Swansea University)
Scientists at the UK-based Swansea University are developing a new artificial intelligence (AI)-based diagnostic tool to speed up the process of biomarkers detection in biofluids.
The researchers have developed a proof of concept for the new diagnostic platform that could deliver health test results in two minutes using a fingertip sample.
According to the university, the test can enable faster test results for health issues like cardiovascular disorders, Alzheimer’s, and joint quality.
Swansea University claimed that the diagnostic tool may revolutionise the healthcare industry because of the application of a form of AI and machine learning (ML). The ML can help in producing test results within minutes, said the university.
Project lead Francesco Del Giudice said: “Existing technologies for the measurements of macromolecules in biofluids are limited; they require a long turnaround time, or require complex protocols, thus calling for alternative, more suitable, methodologies aimed at such measurements.
“In our research, we looked at whether we could rapidly detect different concentration of macromolecules in solution at different temperatures using only 100 mL of sample (equivalent to 2 drops of blood).
“The key innovation is the fact of providing a result within 2 minutes, which is a leap forward compared to standard testing that can take several hours.”
Swansea University said that the proteins found in biofluids such as synovial fluid, saliva, and blood plasma serve as significant biomarkers for the identification of a number of medical disorders. It stated further that the specially created diagnostic tool has been engineered to detect the concentration of the proteins to aid in diagnosing and tracking disease development.
According to the researchers, there is potential for at-home diagnostic kits in the future in which self-screening and self-monitoring options could be available and hospital wait times might be significantly reduced, Swansea University noted.
100 项与 British University of Egypt 相关的药物交易
登录后查看更多信息
100 项与 British University of Egypt 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年06月09日管线快照
管线布局中药物为当前组织机构及其子机构作为药物机构进行统计,早期临床1期并入临床1期,临床1/2期并入临床2期,临床2/3期并入临床3期
临床前
4
登录后查看更多信息
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
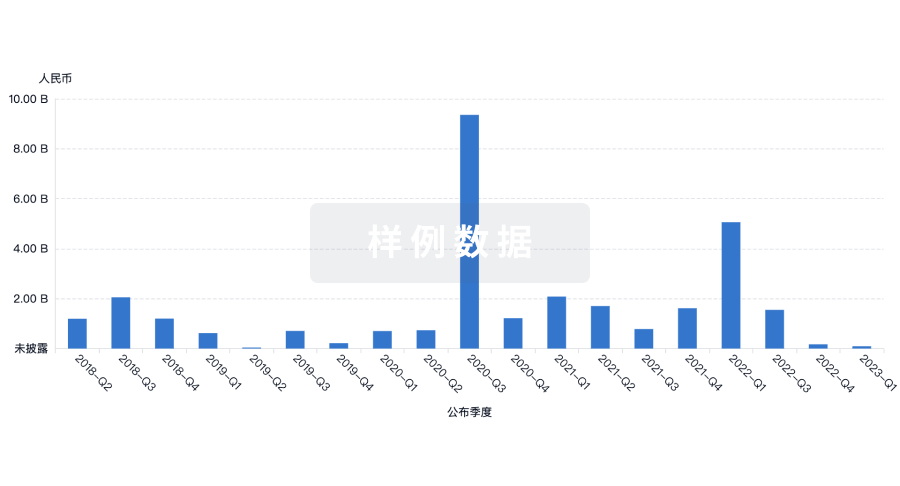
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
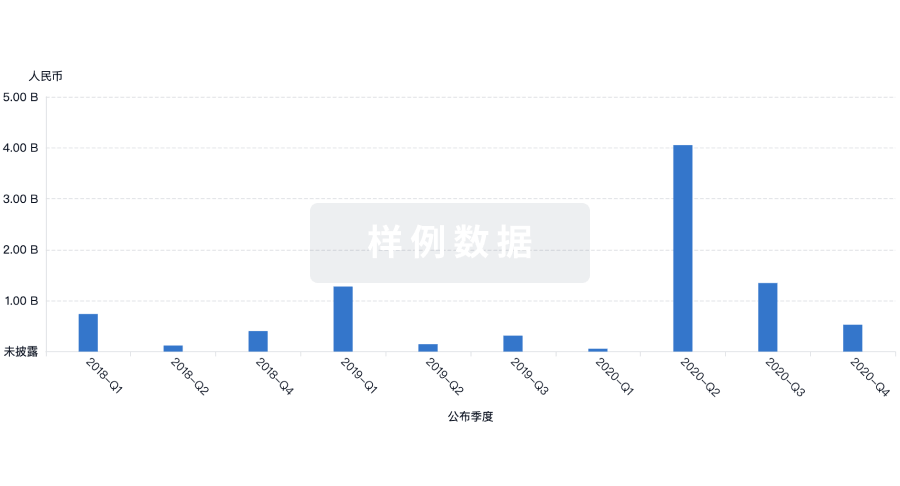
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用