预约演示
更新于:2025-05-07
HBX
更新于:2025-05-07
基本信息
别名 HBx、Peptide X、pX |
简介- |
关联
9
项与 HBX 相关的药物靶点 |
作用机制 HBX抑制剂 |
非在研适应症- |
最高研发阶段临床前 |
首次获批国家/地区- |
首次获批日期1800-01-20 |
靶点 |
作用机制 HBX抑制剂 |
非在研适应症- |
最高研发阶段临床前 |
首次获批国家/地区- |
首次获批日期1800-01-20 |
靶点 |
作用机制 HBX抑制剂 |
非在研适应症- |
最高研发阶段临床前 |
首次获批国家/地区- |
首次获批日期1800-01-20 |
100 项与 HBX 相关的临床结果
登录后查看更多信息
100 项与 HBX 相关的转化医学
登录后查看更多信息
0 项与 HBX 相关的专利(医药)
登录后查看更多信息
3,134
项与 HBX 相关的文献(医药)2025-12-01·Immunologic Research
HBx/WDR5 enhances IGF-1 transcription in hepatocellular carcinoma cells and promotes recruitment, infiltration, and activity of Treg cells
Article
作者: Jia, Yi ; Wang, Erli ; Bai, Zhe ; Sun, Shuhua ; Li, Hui
2025-05-01·Current Molecular Medicine
A Systematic Review of the Impact of Resveratrol on Viral
Hepatitis and Chronic Viral Hepatitis-related Hepatocellular
Carcinoma
Article
作者: Heidari-Soureshjani, Saeid ; Nouri, Majid ; Darvishi, Mohammad ; Rahimi, Rasoul ; Hashemi Rafsanjani, Seyed Mahmoud Reza
2025-04-30·The FASEB Journal
Hepatitis B Virus Disrupts the Blood‐Testis Barrier via the Induction of mTOR ‐Dependent Autophagy in Sertoli Cells
Article
作者: Zhang, Hanbin ; Li, Lei ; Ahmed, Mohamed Morsi M. ; Ding, Yue ; Kang, Xiangjin ; Feng, Na ; Chen, Zhenguo ; Lian, Jingyao ; Xie, Minyu
13
项与 HBX 相关的新闻(医药)2025-03-10
·学术经纬
▎药明康德内容团队编辑(来源:中国科学院生物物理研究所)
乙型肝炎病毒感染是导致肝癌的最重要因素之一。有研究表明,乙型肝炎病毒感染过程中,病毒编码的HBx等抗原可诱导TGF-β信号高度活化,激活肿瘤细胞发生间充质转化或者作用于免疫细胞引起免疫耐受以促进肿瘤的发生发展,但其调控机制有待阐明。
近日,中国科学院生物物理研究所杨鹏远研究组和陈润生研究组阐明了乙型肝炎病毒相关肝癌外泌体中非编码RNA HDAC2-AS2调控免疫逃逸新机制,有望为乙型肝炎病毒相关肝癌提供新的诊疗靶标。相关研究成果以HBV-associated hepatocellular carcinomas inhibit antitumor CD8+ T cell via the long noncoding RNA HDAC2-AS2为题,发表在《自然-通讯》(Nature Communications)上。
该研究筛选出TGF-β刺激后差异表达最显著的lncRNA——HDAC2-AS2,发现过表达或敲低HDAC2-AS2不影响肿瘤自身生长,但显著促进C57小鼠皮下肿瘤生长。机制研究显示,肿瘤细胞中的HDAC2-AS2可通过外泌体分泌到微环境里,肝癌患者血浆外泌体中可检测到更高水平的HDAC2-AS2表达。
免疫功能研究发现,外泌体中的HDAC2-AS2可被CD8+ T细胞摄取,通过结合胞内的细胞周期蛋白依赖激酶9(CDK9),导致胞内CDK9蛋白水平下降从而诱导CD8+ T细胞的耗竭及凋亡,并抑制CD8+ T细胞杀伤功能。多组学分析发现,CDK9在CD8+ T细胞活化和杀伤效应中发挥关键的调节作用。
▲肿瘤外泌体中HDAC2-AS2通过拮抗CDK9抑制CD8+ T细胞功能(图片来源:原始论文[1])
进一步,该研究分析接受免疫检查点阻断治疗的肝癌患者sc-RNA数据库发现,CDK9可以增强免疫检查点阻断治疗时CD8+ T细胞的功能,HDAC2-AS2高表达的肝癌在PD-1抗体治疗中获益更多。
上述研究表明,乙型肝炎病毒阳性肝癌中TGF-β信号通路上调的非编码RNA HDAC2-AS2通过外泌体靶向CD8+ T细胞中CDK9蛋白,导致CD8+ T细胞功能受损,促进肿瘤细胞的免疫逃逸。
研究工作得到国家自然科学基金、国家重点研发计划、中国科学院相关项目等的支持。
原始论文:
[1]Gao, Y., Zhang, Z., Huang, X. et al. HBV-associated hepatocellular carcinomas inhibit antitumor CD8+ T cell via the long noncoding RNA HDAC2-AS2. Nat Commun 16, 2055 (2025). https://doi.org/10.1038/s41467-025-57367-8
免责声明:药明康德内容团队专注介绍全球生物医药健康研究进展。本文仅作信息交流之目的,文中观点不代表药明康德立场,亦不代表药明康德支持或反对文中观点。本文也不是治疗方案推荐。如需获得治疗方案指导,请前往正规医院就诊。
更多推荐
点个“在看”再走吧~
免疫疗法临床研究
2024-11-15
·今日头条
【导读】
在对中国587例弥漫大B细胞淋巴瘤(DLBCL)患者的临床数据进行回顾性分析时发现,13.8%的病例与乙型肝炎病毒(HBV)感染有关,导致其具有独特的临床特征和更差的预后。此外,HBV感染对GCB型DLBCL患者的生存影响比ABC型更为显著。
11月12日,同济大学与海军军医大学(第二军医大学)研究人员合作共同在期刊《Cell Death&Disease》上发表了研究论文,题为“LncRNA MALAT1 promotes 埃拉斯汀-induced ferroptosis in the HBV-infected diffuse large B-cell lymphoma”,本研究中,研究人员发现在乙型肝炎病毒感染的GCB型滤泡性淋巴瘤患者中,长链非编码RNA MALAT1的表达下调,而乙型肝炎核心蛋白(HBX)直接抑制MALAT1在DLBCL细胞中的表达。值得注意的是,HBX过表达可以减轻埃拉斯汀诱导的GCB型DLBCL细胞的铁死亡,而MALAT1重新表达则在体外和体内恢复了HBX过表达的DLBCL细胞对埃拉斯汀的敏感性。机制上,MALAT1通过共享的TTGGTCT序列竞争性抑制SFPQ有效地剪接SLC7A11的前mRNA,从而阻碍SLC7A11前mRNA的成熟,进而降低其对铁死亡的负调控作用。综上所述,本研究确定了HBX通过抑制MALAT1表达、促进SFPQ介导的SLC7A11前mRNA剪接以及降低GCB型DLBCL对埃拉斯汀诱导的铁死亡的敏感性发挥作用。
结合最近的研究表明,铁死亡可能参与了DLBCL的发生和发展,这些发现解释了研究人员对DLBCL患者的临床数据分析,即MALAT1表达低的患者预后较差,总生存期较短,并为HBV感染的GCB型DLBCL患者提供了有价值的治疗靶点。
https://www.nature.com/articles/s41419-024-07209-0
背景信息
01
弥漫性大B细胞淋巴瘤(DLBCL)是非霍奇金淋巴瘤(NHL)中最常见的类型,约占NHL病例的30-40%。DLBCL具有复杂的临床和分子遗传特征,进展迅速且侵袭性强。根据特定的B细胞分化转录本,DLBCL被分为GCB(中心母细胞样B细胞)和ABC(激活B细胞样)亚型,它们具有与不同致病机制相关的独特突变谱。尽管CHOP方案是大多数DLBCL患者改善预后的一线治疗方案,但由于DLBCL的高异质性,仍有30-40%的患者面临治疗耐药或复发的风险。
乙型肝炎病毒(HBV)具有淋巴细胞毒性,与淋巴瘤的发生和发展密切相关。研究发现,非霍奇金淋巴瘤(NHL)患者的HBV感染状况与他们的无进展生存期(PFS)和总生存期(OS)存在显著相关性,这表明持续的HBV复制可能是影响化疗疗效和预后的关键因素。中国是HBV感染的高发地区,对587例滤泡性淋巴瘤(DLBCL)患者的临床数据进行回顾性分析发现,13.8%的DLBCL病例与HBV感染有关,HBV感染的DLBCL患者具有独特的临床特征和更差的预后。此外,HBV感染对GCB型DLBCL患者的生存影响更为显著,较之于ABC型。因此,阐明HBV感染的GCB型DLBCL患者不良预后的分子机制并识别新的治疗靶点,以改善其临床预后至关重要。
乙型肝炎感染与铁死亡有关,并影响患者预后
02
既往研究已经表明,感染乙肝病毒的DLBCL患者的生存时间较短,乙肝病毒感染被认为是DLBCL患者预后的独立因素,尤其是GCB-型DLBCL患者。研究人员首先从TCGA数据库(TCGA-DLBCL)中将48例DLBCL患者分为HBV阳性和阴性两组,并鉴定出889个差异表达基因(p<0.05和|Log2(FC)|>1.0;上调基因:179个;下调基因:710个)。KEGG通路分析显示,这些差异表达基因主要富集在铁死亡、HIF-1信号通路和甲状腺激素合成等通路中。此外,研究人员比较分析了与铁死亡相关的259个基因和HBV阳性组与阴性组之间的889个差异表达基因(DEGs),发现73个基因。然后,研究人员使用ROC曲线分析对这些73个基因在预测DLBCL患者预后的价值进行了评估,得出曲线下面积为0.706的结果,这表明这些基因可能作为DLBCL患者的预后标志物的潜力。这些分析表明,HBV感染与DLBCL患者的铁死亡和预后显著相关。
MALAT1增强HBX表达肿瘤对铁死亡的敏感性,并与HBV感染的DLBCL患者的SLC7A11呈负相关
03
为了研究MALAT1在体内促进铁死亡的作用,研究人员首先在小鼠异种移植模型中进行了实验。研究人员将对照组、HBX组和HBX+MALAT1细胞注射到6周大的NOD-SCID免疫缺陷小鼠体内。IKE治疗显著减少了对照组肿瘤的体积和重量,证实其具有诱导铁死亡的功效,而HBX表达组的IKE治疗效果明显较弱。更重要的是,在HBX表达的肿瘤中过表达MALAT1恢复了对IKE治疗的敏感性。此外,同时给予IKE和利普司他丁完全消除了其抑制肿瘤生长的作用,表明观察到的抗肿瘤作用是铁死亡特异性的。与IKE治疗的结果一致,HBX过表达也显著降低了埃拉斯汀对肿瘤生长的抑制作用,导致肿瘤体积和重量增加,而MALAT1重新表达有效地恢复了这些抑制作用。对铁死亡标志物(SLC7A11、ACSL4和GPX4)和脂质过氧化水平(4-HNE和MDA)的分析进一步证实,MALAT1可以抵消HBX的作用并促进铁死亡。此外,研究人员对患者样本的分析发现,HBV感染的GCB型DLBCL患者的MALAT1 mRNA水平显著降低,而SLC7A11表达增加,MALAT1和SLC7A11表达之间存在负相关关系,进一步证实MALAT1在HBV感染的DLBCL中调节铁死亡过程中的关键作用。
MALAT1增强HBX表达肿瘤对铁死亡的敏感性,并与HBV感染的DLBCL患者的SLC7A11呈负相关
结论
04
综上,本研究揭示了MALAT1/SFPQ相互作用在调节铁死亡过程中调节SLC7A11表达的全新功能。这些发现揭示了SLC7A11在铁死亡通路中的新的上游调节机制。因此,MALAT1有望成为一种新型的生物标志物,为基于铁死亡的HBV感染的GCB型DLBCL治疗提供了新的见解。
【参考资料】
https://www.nature.com/articles/s41419-024-07209-0
【关于投稿】
转化医学网(360zhyx.com)是转化医学核心门户,旨在推动基础研究、临床诊疗和产业的发展,核心内容涵盖组学、检验、免疫、肿瘤、心血管、糖尿病等。如您有最新的研究内容发表,欢迎联系我们进行免费报道(公众号菜单栏-在线客服联系),我们的理念:内容创造价值,转化铸就未来!
转化医学网(360zhyx.com)发布的文章旨在介绍前沿医学研究进展,不能作为治疗方案使用;如需获得健康指导,请至正规医院就诊。
热门推荐活动 点击免费报名
🕓 上海|11月15日-16日
▶ 2024第一届中国类器官转化医学大会
🕓 上海|11月21日-24日
▶ 第七届上海国际肿瘤内科学论坛
🕓 全国|2024年12月-2025年03月
▶ 中国转化医学产业大会
🕓 上海|2025年02月28日-03月01日
▶ 第四届长三角单细胞组学技术应用论坛暨空间组学前沿论坛
点击对应文字 查看详情
信使RNA临床研究细胞疗法
2024-10-22
JENKINTOWN, Pa., Oct. 22, 2024 /PRNewswire/ -- SFA Therapeutics, Inc., a clinical-stage biopharmaceutical company developing oral small-molecule biosynthetic compounds for the treatment of inflammatory diseases, today announced the expansion of its intellectual property in autoimmune disease and hepatocellular carcinoma. SFA Therapeutics has been issued a new patent in the United States (11963938) and has been allowed two patent applications in Canada (2,974,510) and in Korea (10-2017-7023391) with patent coverage through 2036. SFA Therapeutics has also been issued one new patent in Korea (10-2646764) with patent coverage through 2038.
The United States patent and the allowed Canadian and Korean patent applications protect the short chain fatty acid composition that comprises SFA's proprietary oral small-molecule biosynthetic compound SFA-001. SFA-001 is a potent immunomodulator being evaluated for the prevention, delay of onset, and treatment of hepatocellular carcinoma. In preclinical studies, SFA-001 demonstrated cytotoxicity against two common human liver cancer cell lines expressing the hepatitis B oncoprotein, HBx. Huh7x and Hep3BX are highly sensitive to SFA-001 without damage to normal liver cells. In 2019, the United States Food and Drug Administration granted an Orphan Drug Designation (ODD) to SFA-001 for the treatment of hepatocellular carcinoma.
The Korean patent protects the short chain fatty acid composition that comprises SFA-002, SFA Therapeutics' lead candidate and Phase-2 ready potent immunomodulator being evaluated for the treatment of psoriasis. SFA-002 acts on multiple therapeutic pathways with the aim of restoring balance to the immune system. While SFA-002 inhibits pathways of pro-inflammatory cytokines such as IL-17, IL-23, TNF-α, and IFN-y, it also increases Treg differentiation and upregulates the anti-inflammatory cytokine IL-10.
"As SFA's clinical development progresses, we understand the importance of strengthening our intellectual property portfolio to protect SFA Therapeutics' proprietary therapeutic candidates," said Dr. Ira Spector, Chief Executive Officer of SFA Therapeutics. "The expansion of our patent portfolio allows us to continue the research and development necessary to bring drug candidates like SFA-001 and SFA-002 through the clinic to patients of autoimmune and inflammatory diseases. This brings the total number of issued and allowed SFA Therapeutics patents to 15, with 33 additional patents pending."
"These patents demonstrate the novel nature of SFA Therapeutics' platform and drug candidates which are developed by adding disease-specific adjuvants to compounds that are naturally found in the human body," said Dr. Mark Feitelson, Chief Scientific Officer of SFA Therapeutics. "Our therapeutic candidates target multiple pathways in autoimmune and inflammatory conditions, working to inhibit pro-inflammatory cytokines, up-regulate anti-inflammatory targets, and suppress autoimmunity. We believe the intellectual property protected by these patents has the potential to not only manage symptoms from diseases, but to also address the underlying cause of these conditions and prevent or delay their onset."
About SFA Therapeutics
SFA Therapeutics, Inc. is a clinical-stage biopharmaceutical company developing oral small-molecule biosynthetic compounds for the treatment of inflammatory diseases. Based on breakthrough research licensed from Temple University, SFA Therapeutics' platform has the potential to develop safer and more efficacious treatments for a number of chronic inflammatory diseases by uniquely tailoring the effects of patented formulations with target-specific adjuvants. Its lead asset, SFA-002, a potent immunomodulator, is approaching Phase 2 clinical trials and has shown promising Phase 1a and Phase 1b results for the treatment of psoriasis. SFA Therapeutics has also received clearance of its Investigational New Drug (IND) application from the U.S. Food and Drug Administration (FDA) to investigate SFA-001N in patients with metabolic dysfunction-associated steatohepatitis (MASH), also known as non-alcoholic steatohepatitis (NASH), with or without fibrosis. SFA Therapeutics has an Orphan Disease Designation from the FDA for SFA-001 in the treatment of hepatocellular carcinoma, the most prevalent form of liver cancer.
SFA Therapeutics is headquartered in Jenkintown, Pennsylvania. Please visit
to learn more.
Company Contact
Ira Spector, Ph.D.
SFA Therapeutics, Inc.
+1 267-584-1080
Media Contacts
Tony Russo, Ph.D.
Russo Partners, LLC
[email protected]
Maddie Stabinski
Russo Partners, LLC
[email protected]
SOURCE SFA Therapeutics, Inc.
WANT YOUR COMPANY'S NEWS FEATURED ON PRNEWSWIRE.COM?
440k+
Newsrooms &
Influencers
9k+
Digital Media
Outlets
270k+
Journalists
Opted In
GET STARTED
孤儿药临床2期临床结果临床1期免疫疗法
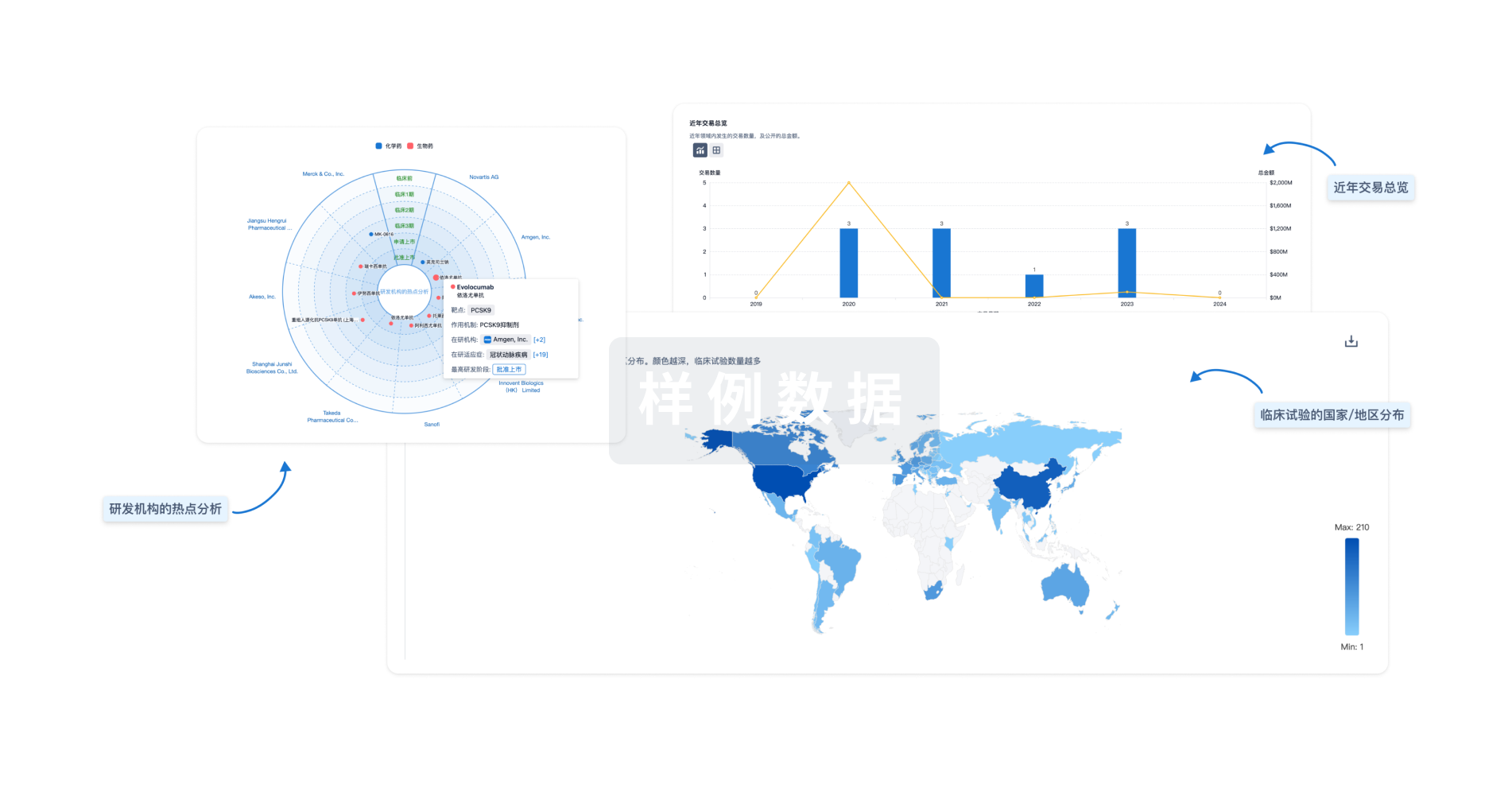
分析
对领域进行一次全面的分析。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
