预约演示
更新于:2026-04-02
Sapablursen
更新于:2026-04-02
概要
基本信息
药物类型 ASO |
别名 IONIS TMPRSS6 LRx、IONIS TMPRSS6-Lrx、IONIS-TMPRSS6-L + [7] |
靶点 |
作用方式 抑制剂 |
作用机制 TMPRSS6抑制剂(跨膜丝氨酸蛋白酶-6抑制剂) |
非在研适应症 |
非在研机构- |
最高研发阶段临床3期 |
首次获批日期- |
最高研发阶段(中国)- |
特殊审评孤儿药 (美国)、快速通道 (美国) |
登录后查看时间轴
结构/序列
使用我们的RNA技术数据为新药研发加速。
登录
或
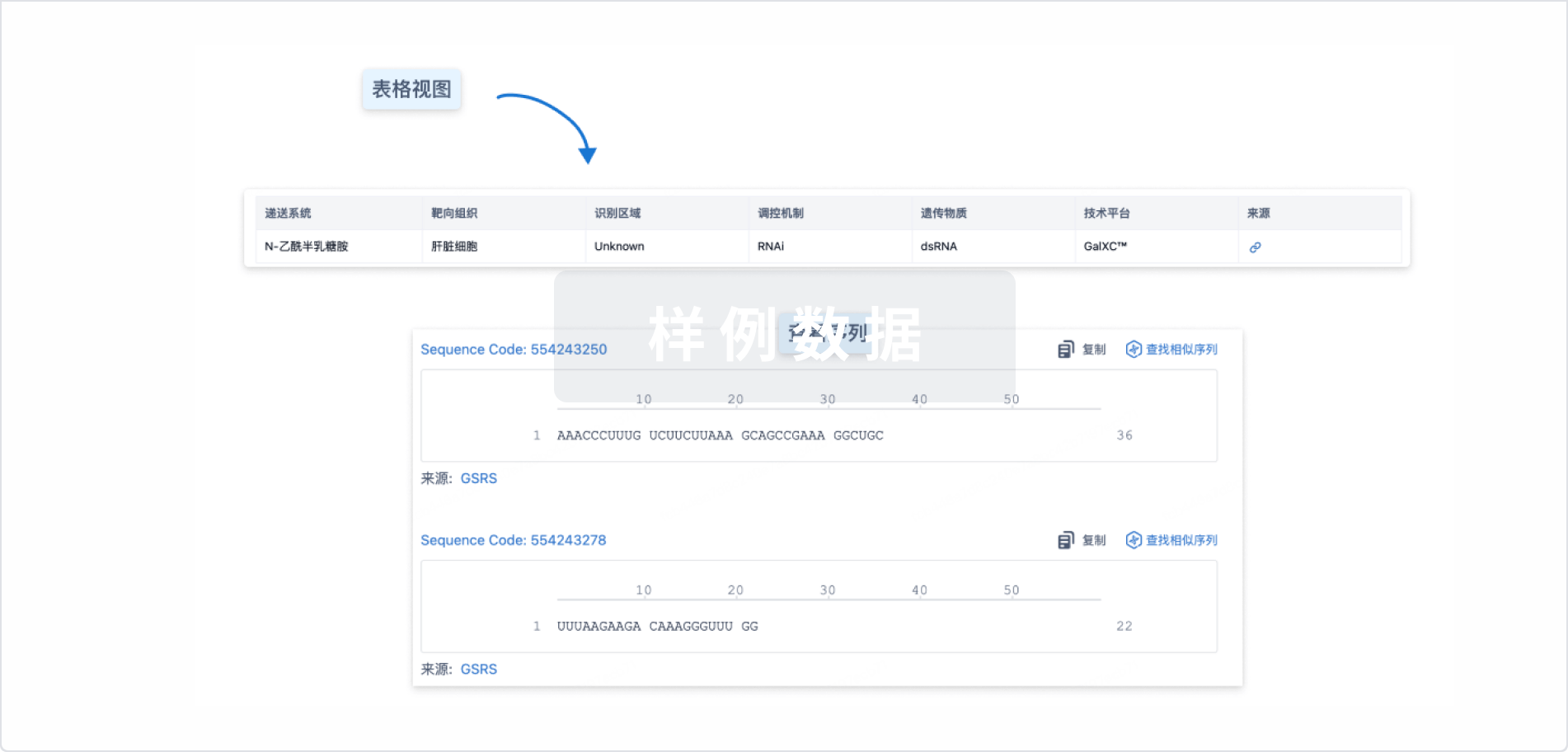
Sequence Code 533738446

来源: *****
关联
5
项与 Sapablursen 相关的临床试验NCT07429266
A Phase 3 Randomized, Double-blind, Placebo-controlled Global Study of Sapablursen in Polycythemia Vera
The purpose of this study is to evaluate the efficacy and safety of sapablursen when added on to current standard of care (SOC) for Polycythemia Vera (PV) therapy. The study will be conducted in three sequential parts (Part 1a blinded treatment, Part 1b open-label treatment, & Part 2 long-term extension). Participants may receive treatment for up to 156 weeks.
开始日期2026-06-01 |
申办/合作机构 |
NCT05143957
A Phase 2a, Randomized, Open-Label Study to Evaluate the Efficacy, Safety, Tolerability, Pharmacokinetics, and Pharmacodynamics of ISIS 702843 Administered to Patients With Phlebotomy Dependent Polycythemia Vera (PD-PV)
The main purpose of this study is to evaluate the efficacy of sapablursen in reducing the frequency of phlebotomy and in improving quality of life assessments in participants with polycythemia vera.
开始日期2021-12-30 |
申办/合作机构 |
NCT04059406
A Phase 2a, Randomized, Open-Label Study to Evaluate the Efficacy, Safety, Tolerability, Pharmacokinetics and Pharmacodynamics of ISIS 702843 Administered Subcutaneously to Patients With Non-Transfusion Dependent β-Thalassemia Intermedia
The purpose was to evaluate the efficacy, safety, tolerability, pharmacokinetics and pharmacodynamics of sapablursen administered subcutaneously to participants with non-transfusion dependent β-Thalassemia Intermedia.
开始日期2020-09-24 |
申办/合作机构 |
100 项与 Sapablursen 相关的临床结果
登录后查看更多信息
100 项与 Sapablursen 相关的转化医学
登录后查看更多信息
100 项与 Sapablursen 相关的专利(医药)
登录后查看更多信息
7
项与 Sapablursen 相关的文献(医药)2024-07-01·American journal of hematology
Combination of a TGF ‐β ligand trap (RAP‐GRL ) and TMPRSS6‐ASO is superior for correcting β‐thalassemia
Article
作者: Rivella, Stefano ; Demsko, Perry ; Hamilton, Nolan ; Guo, Shuling ; Rivera, Ariel ; Guerra, Amaliris
Abstract:
A recently approved drug that induces erythroid cell maturation (luspatercept) has been shown to improve anemia and reduce the need for blood transfusion in non‐transfusion‐dependent as well as transfusion‐dependent β‐thalassemia (BT) patients. Although these results were predominantly positive, not all the patients showed the expected increase in hemoglobin (Hb) levels or transfusion burden reduction. Additional studies indicated that administration of luspatercept in transfusion‐dependent BT was associated with increased erythropoietic markers, decreased hepcidin levels, and increased liver iron content. Altogether, these studies suggest that luspatercept may necessitate additional drugs for improved erythroid and iron management. As luspatercept does not appear to directly affect iron metabolism, we hypothesized that TMPRSS6‐ASO could improve iron parameters and iron overload when co‐administered with luspatercept. We used an agent analogous to murine luspatercept (RAP‐GRL) and another novel therapeutic, IONIS TMPRSS6‐LRx (TMPRSS6‐ASO), a hepcidin inducer, to treat non‐transfusion‐dependent BT‐intermedia mice. Our study shows that RAP‐GRL alone improved red blood cell (RBC) production, with no or limited effect on splenomegaly and iron parameters. In contrast, TMPRSS6‐ASO improved RBC measurements, ameliorated splenomegaly, and improved iron overload most effectively. Our results provide pre‐clinical support for combining TMPRSS6‐ASO and luspatercept in treating BT, as these drugs together show potential for simultaneously improving both erythroid and iron parameters in BT patients.
2021-04-01·The Journal of pharmacology and experimental therapeutics
Safety, Pharmacokinetic, and Pharmacodynamic Evaluation of a 2′-(2-Methoxyethyl)-D-ribose Antisense Oligonucleotide–Triantenarry N-Acetyl-galactosamine Conjugate that Targets the Human Transmembrane Protease Serine 6
Article
作者: Engelhardt, Jeffrey A ; Burel, Sebastien ; Korbmacher, Birgit ; Zanardi, Thomas A ; Guo, Shuling ; Wang, Yanfeng ; Prill, Bobby ; Boone, Laura ; Aghajan, Mariam ; Henry, Scott P
Cellular uptake of antisense oligonucleotides (ASOs) is one of the main determinants of in vivo activity and potency. A significant advancement in improving uptake into cells has come through the conjugation of ASOs to triantenarry N-acetyl-galactosamine (GalNAc3), a ligand for the asialoglycoprotein receptor on hepatocytes. The impact for antisense oligonucleotides, which are already taken up into hepatocytes, is a 10-fold improvement in potency in mice and up to a 30-fold potency improvement in humans, resulting in overall lower effective dose and exposure levels. 2'-Methoxyethyl-modified antisense oligonucleotide conjugated to GalNAc3 (ISIS 702843) is specific for human transmembrane protease serine 6 and is currently in clinical trials for the treatment of β-thalassemia. This report summarizes a chronic toxicity study of ISIS 702843 in nonhuman primates (NHPs), including pharmacokinetic and pharmacology assessments. Suprapharmacologic doses of ISIS 702843 were well tolerated in NHPs after chronic dosing, and the data indicate that the overall safety profile is very similar to that of the unconjugated 2'-(2-methoxyethyl)-D-ribose (2'-MOE) ASOs. Notably, the GalNAc3 moiety did not cause any new toxicities nor exacerbate the known nonspecific class effects of the 2'-MOE ASOs. This observation was confirmed with multiple GalNAc3-MOE conjugates by querying a data base of monkey studies containing both GalNAc3-conjugated and unconjugated 2'-MOE ASOs. SIGNIFICANCE STATEMENT: This report documents the potency, pharmacology, and overall tolerability profile of a triantenarry N-acetyl-galactosamine (GalNAc3)-conjugated 2'-(2-methoxyethyl)-D-ribose (2'-MOE) antisense oligonucleotide (ASO) specific to transmembrane protease serine 6 after chronic treatment in the cynomolgus monkey. Collective analysis of 15 independent GalNAc3-conjugated and unconjugated 2'-MOE ASOs shows the consistency in the dose response and character of hepatic and platelet tolerability across sequences that will result in much larger safety margins for the GalNAc3-conjugated 2'-MOE ASOs when compared with the unconjugated 2'-MOE ASOs given the increased potency.
2021-03-01·American journal of hematology
Management of non‐transfusion‐dependent β‐thalassemia (NTDT ): The next 5 years
Letter
作者: Stefano Rivella ; Khaled M. Musallam ; Ali T. Taher
Management of patients with β-thalassemia is undergoing a swift evolution, considering the number of novel agents recently receiving marketing approval or entering clinical development. Although (thankfully) the availability of new treatment options will address several persisting unmet needs in this patient population, several questions remain on how such advances should be optimally integrated into standard of care. The only currently approved therapy for patients with non-transfusion-dependent β-thalassemia (NTDT) is iron chelation (for patients ≥ 10 years).1 This only followed recent evidence of clinically significant iron overload and subsequent multiorgan morbidity, even in NTDT patients who never received transfusion therapy.2 Patients with NTDT accumulate iron from increased intestinal iron absorption and release from the reticuloendothelial system, signaled by low hepcidin levels attributed to ineffective erythropoiesis.2 Although this milestone in disease management addressed a key morbidity risk factor, there are currently no approved therapies specifically targeting the underlying ineffective erythropoiesis and anemia, which are not only the drivers for primary iron overload, but are also linked with a variety of clinical complications stemming from chronic tissue hypoxia, hemolysis, and hypercoagulability.1 There is evidence that transfusion therapy may be associated with lower morbidity rates in NTDT,1 but physicians are understandably hesitant to start these patients on regular transfusion programs which would open the door to transfusional siderosis and progressive organ dysfunction. In this context, several agents are currently being evaluated in clinical trials with the aim of targeting ineffective erythropoiesis or iron dysregulation in NTDT, with the expectation that addressing one pathophysiologic mechanism will ameliorate the other; since a bidirectional relationship between both anomalies has been confirmed.3 Clinically, this would translate to improvement in anemia and prevention of iron overload. Luspatercept (ACE-536) is a recombinant fusion protein that binds to select transforming growth factor β superfamily ligands and enhances late-stage erythropoiesis.4, 5 Luspatercept showed encouraging data in a single-arm, open-label, phase two study including improvement in hemoglobin level in NTDT and reduction in transfusion burden in transfusion-dependent β-thalassemia (TDT).6 A phase three trial (BELIEVE) confirmed these findings in TDT patients and led to product approval in this subset of patients.7 The ongoing randomized (2:1), double-blind, placebo-controlled, phase two BEYOND trial (NCT03342404) is evaluating the efficacy of subcutaneous luspatercept (every 3 weeks) in increasing hemoglobin level (by ≥ 1.0 g/dL) in adult patients with NTDT and a baseline hemoglobin ≤ 10 g/dL. Assessment of effects on tiredness, weakness, and shortness of breath is also being undertaken to confirm clinical benefit. The impact of therapy on iron indices and use of iron chelation will also be reported. Mitapivat (AG-348) is an oral, small-molecule, allosteric activator of the red blood cell (RBC)-specific form of pyruvate kinase (PK-R). Adenosine triphosphate (ATP) supply appears to be insufficient in thalassemic RBCs to maintain RBC membrane fitness and clearance of globin precipitates. In β-thalassemia mouse models, mitapivat increased ATP levels, reduced markers of ineffective erythropoiesis, and improved anemia, RBC survival, and indices of iron overload.8 An open-label, phase two trial (NCT03692052) in adults with NTDT and a baseline hemoglobin of ≤ 10 g/dL is evaluating the efficacy of mitapivat in improving hemoglobin level (by ≥ 1.0 g/dL) as well as markers of hemolysis and ineffective erythropoiesis. Interim data showed response in eight of nine patients following 12 weeks of therapy.9 Anti-sense oligonucleotides (ASO) downregulating TMPRSS6, a metalloprotease which plays a key role in hepcidin expression, stimulated hepcidin, reduced iron burden, and improved ineffective erythropoiesis and RBC survival in β-thalassemia mouse models.10 TMPRSS6-LRx is a generation 2+ ligand-conjugated ASO subcutaneous drug (given every 4 weeks) that is now being evaluated in a randomized, open-label, phase two trial (NCT04059406) in adults with NTDT and baseline hemoglobin ≤ 10 g/dL. The main endpoints include increasing hemoglobin level (by ≥ 1.0 g/dL) and decreasing LIC. Finally, VIT-2763 is an oral ferroportin inhibitor which restricted iron availability, ameliorated anemia, and reversed the dysregulated iron homeostasis in β-thalassemia mouse models.11 VITHAL (NCT04364269) is a randomized, double-blind, placebo-controlled, phase two trial evaluating the efficacy of VIT-2763 in improving hemoglobin and iron indices in NTDT patients aged ≥ 12 years with a baseline hemoglobin ≤ 11 g/dL. All novel agents primarily aim to ameliorate anemia and iron overload in patients with NTDT, and final data from ongoing and subsequent registration trials are awaited. Considering multiple agents may become available not long from today; it is imperative to think ahead and try to visualize the outlook for overall disease management (Figure 1), so gaps in knowledge can be promptly identified and addressed alongside clinical development. Realizing the impact of improvement in anemia in the context of clinical trials may be challenging, since the aim of such improvement is to prevent the development of serious, long-term morbidity. Observational studies and disease registries would be key to evaluate such association, once these agents become available for clinical use. In the short term, clinical benefit from raising hemoglobin level may be evaluated through observation of changes in patient reported outcomes, although this should not exclude asymptomatic patients who may still benefit from drug-induced long-term changes in the underlying pathophysiology. The main effect of such agents on iron overload will be prevention of "new" and ongoing iron accumulation. Decreases in existing iron burden may also be observed in view of mobilization of iron to support production of RBCs, but this latter effect is expected to be minimal. Considering most ongoing clinical trials are including adult participants only (or adolescents in few cases), it is expected that patients would already have some degree of iron overload requiring iron chelation therapy. Combination of these novel agents with iron chelation may improve chelator efficiency since the latter is dependent on both pre-existing and ongoing iron intake. This may result in lower iron chelator dosing and/or reaching target (safe) iron levels faster. This synergistic effect has been observed in mouse models receiving a combination of TMPRSS6-ASO and iron chelation.12 If ongoing iron accumulation is completely reversed, this may in fact lead to long-term or permanent discontinuation of iron chelation therapy following reductions in pre-existing iron overload. This also brings up the interesting question of whether future studies in children who are not yet on iron chelation therapy, will avoid the need for the latter altogether. The more important question that we will probably be faced with is which agent should we use, especially that the design of current clinical trials and eligibility criteria are largely similar. Data from individual studies can be compared, but in an era of evidence-based medicine clinicians would likely want to see data from head-to-head comparative trials before making any management decisions. We have witnessed this challenge for over two decades with oral iron chelation therapy in TDT, and choices regarding the type of iron chelation therapy remain largely based on physician preference rather than comparative studies. Combinatorial trials with multiple novel agents (or with novel agents and stimulants such as erythropoietin) may also be warranted, since the mechanisms of action are different and may prove complimentary. For example, in β-thalassemic mice, administration of TMPRSS6-ASO and erythropoietin produced significantly higher hemoglobin levels and reduction in splenomegaly compared with each agent alone. This suggests that combinatorial approaches may in fact be superior to single treatments and could provide guidance to translate some of these approaches into treatment strategies.13 Lastly, progress has already been made with gene therapy and genome editing for patients with TDT. It was once argued that bone marrow transplantation should not be considered in NTDT, considering the disease is less severe. However, we continue to see strong evidence that an NTDT diagnosis is associated with serious, irreversible morbidities. Moreover, safer conditioning approaches during transplant are evolving and data from gene therapy studies are pointing towards better response in patients with less severe mutations (non-β0/β0). Together, these observations suggest that NTDT patients may be considered in future studies with interventions targeting the underlying genetic abnormality, especially when the risk-benefit ratio is low. K.M.M. has been or is a consultant for Novartis, Celgene Corp (Bristol Myers Squibb), Agios Pharmaceuticals, CRISPR Therapeutics and Vifor Pharma. S.R. is a member of scientific advisory board of Ionis Pharmaceuticals, Meira GTx, Incyte and Disc Medicine and owns stock options from Disc Medicine and Meira GTx. He has been or is consultant for Cambridge Healthcare Res, Celgene Corp (Bristol Myers Squibb), Catenion, First Manhattan Co., FORMA Therapeutics, Ghost Tree Capital, Keros Therapeutics, Noble insight, Protagonist Therapeutics, Sanofi Aventis U.S., Slingshot Insight, Techspert.io and BVF Partners L.P., Rallybio LLC and venBio Select LLC. A.T.T. has been or is a consultant for Novartis, Celgene Corp (Bristol Myers Squibb), Vifor Pharma, Silence Therapeutics and Ionis Pharmaceuticals; and received research funding from Novartis, Celgene Corp (Bristol Myers Squibb), La Jolla Pharmaceutical Company, Roche, Protagonist Therapeutics and Agios Pharmaceuticals. All authors contributed to manuscript drafting or critical review and final approval for submission. Data sharing is not applicable to this article as no new data were created or analyzed in this study.
32
项与 Sapablursen 相关的新闻(医药)2026-03-16
·药事纵横
当基因沉默技术从实验室概念蝶变为临床Ⅲ期的成熟管线,寡核苷酸药物正站在罕见病治疗史无前例的转折点上。2026年的春天,全球超过10款在研新药迈入关键临床阶段——这不仅是技术成熟的标志,更是数百万无药可医的罕见病患者等待已久的曙光。
表格:全球10多款进入Ⅲ期临床的寡核苷酸在研新药
一、技术迭代:从“靶点命中”到“精准递送”的质变突围
寡核苷酸药物的研发史,本质上是递送技术的进化史。早期,ASO、siRNA等寡核苷酸分子的临床应用面临两大核心瓶颈:一是体内稳定性极差,进入人体后易被核酸酶降解,难以到达靶器官发挥作用;二是靶向性不足,多依赖肝脏摄取,肝脏外组织(如神经、肌肉)递送困难,导致临床应用范围严重受限,多数在研项目折戟于早期临床,一度被认为“难以实现规模化临床应用”。
随着化学修饰技术与递送系统的不断突破,寡核苷酸药物逐步摆脱困境,实现了从“靶点命中”到“精准递送”的质变,而当前进入Ⅲ期临床的管线,正是这场技术革命的集中体现,展现出多元化的技术突破方向,推动寡核苷酸药物从“只能打肝脏”迈入“靶向全身组织”的新纪元。
抗体偶联寡核苷酸(AOC)平台的成熟,彻底解决了神经肌肉疾病递送的世界级难题,成为寡核苷酸药物肝外靶向的核心突破口。AOC技术通过将靶向特定组织细胞表面抗原的单克隆抗体,与寡核苷酸分子偶联,借助抗体与抗原的特异性结合,实现寡核苷酸药物向目标组织的精准递送,同时降低对正常组织的损伤,提升药物疗效与安全性。其中,Avidity Biosciences的在研AOC疗法delpacibart etedesiran(del-desiran,AOC 1001)表现尤为突出,该药物用于治疗1型肌强直性营养不良(DM1),在1/2期MARINA试验中,成功将寡核苷酸递送至肌肉组织,使所有接受治疗的受试者中DMPK mRNA平均降低约40%,有效针对DM1的根本病因,目前该药物已进入Ⅲ期临床,有望成为全球首款治疗DM1的AOC药物。
Avidity的AOC平台获资本高度认可,2025年10月诺华以120亿美元将其收购,核心看中其肝外靶向潜力,可将小核酸药物递送至肌肉、中枢等组织。除治疗DM1的del-desiran外,其另一款治疗FSHD的AOC药物del-brax也进入Ⅲ期,1/2期数据显示患者肌肉功能、生活质量显著改善,印证了AOC平台的临床价值。
LICA技术推动寡核苷酸药物给药便捷化,通过寡核苷酸与配体偶联,提升体内稳定性并实现皮下注射。2025年FDA批准的LICA药物donidalorsen(用于HAE预防),采用每月一次皮下注射方案,大幅提升患者依从性,其成功上市为LICA技术应用奠定基础,目前多款LICA类药物已进入Ⅲ期。
鞘内给药与新型化学修饰技术结合,可延长药物半衰期、突破血脑屏障,助力中枢神经系统罕见病治疗。渤健用于SMA的在研ASO疗法salanersen,采用鞘内给药,1期数据显示耐受性良好,基线NfL浓度较高患者治疗6个月后该标志物下降70%,效果可持续一年,有望实现“一年一针”,大幅减轻患者负担。
此外,新型化学修饰技术(如 phosphorothioate 修饰、2'-O-甲基修饰等)的广泛应用,进一步解决了寡核苷酸药物体内稳定性差、脱靶效应明显等问题,提升了药物的安全性与有效性。这些技术突破的叠加,使得寡核苷酸药物的临床应用范围不断扩大,从最初的肝脏相关疾病,逐步拓展至神经、肌肉、血液等多个系统,为更多罕见病病种带来了治疗可能,也标志着寡核苷酸药物进入了规模化发展的黄金阶段。二、适应症图谱:神经系统与肌肉罕见病成为主战场
随着递送技术的不断突破,寡核苷酸药物的适应症布局逐步拓展,当前全球进入Ⅲ期临床的寡核苷酸新药中,神经系统遗传病与神经肌肉疾病占据绝对主导地位,成为寡核苷酸药物临床落地的核心主战场。这些适应症多数为遗传性疾病,此前长期“无药可医”,寡核苷酸药物凭借其基因调控的独特优势,首次为患者提供了针对病因的干预手段,有望彻底改变这类疾病的治疗格局。
天使综合征是当前寡核苷酸药物研发的热点领域,目前已有两款ASO疗法同时进入Ⅲ期临床,针对UBE3A基因的“再激活”策略展现出惊人潜力,有望为这种罕见遗传性神经发育疾病带来首款根治性疗法。天使综合征由母源UBE3A基因缺失或突变导致,患者表现为智力障碍、癫痫发作、运动功能障碍等症状,目前尚无有效治疗手段。Ionis Pharmaceuticals公司在研的ASO疗法ION582,于2025年9月获得FDA授予突破性疗法认定,该药物旨在抑制UBE3A反义转录本(UBE3A-ATS)的表达,激活来自父体的UBE3A等位基因,增加患者大脑中UBE3A蛋白的产生,从根源上改善患者症状。目前,ION582的全球3期关键性REVEAL研究正在推进,计划纳入携带母源UBE3A基因缺失或突变的儿童和成人患者,预计2026年完成入组,为后续上市申请奠定基础。
另一款针对天使综合征的ASO疗法GTX-102(apazunersen),由Ultragenyx公司研发,同样于2025年7月获得FDA突破性疗法认定,该药物采用鞘内给药方式,可促进神经元细胞中父系UBE3A等位基因的表达,产生患者体内缺失的关键蛋白产物,其全球3期试验正在顺利推进,两款ASO疗法的同期发力,有望加速天使综合征治疗药物的落地,为患者带来新的希望。
Dravet综合征(婴幼儿期发病、预后差、临床治疗有限的罕见遗传性癫痫)领域,渤健与Stoke Therapeutics联合开发的ASO药物zorevunersen已进入Ⅲ期,其通过增强SCN1A野生型基因功能、提升NaV1.1蛋白表达从根源治病。2025年10月两年随访数据显示,患者认知行为持续改善,与自然病史形成鲜明对比,三年OLE研究中95%患者整体状况改善,有望成为该病症首款病因性治疗药物。
严重罕见神经肌肉疾病DM1与FSHD,迎来全球首批进入Ⅲ期的AOC药物。Avidity的del-desiran(靶向DMPK基因、降低其mRNA水平)作为首款DM1 AOC药物,1/2期数据证实疗效安全;其针对FSHD的del-brax也进入Ⅲ期,1/2期显示患者肌肉功能及生活质量显著改善,两款药物有望填补相关治疗空白。
寡核苷酸药物的适应症布局正逐步拓展,除了神经系统与肌肉罕见病,血液罕见病领域也取得了重要突破,彰显了该技术平台的普适性。在真性红细胞增多症领域,Ionis Pharmaceuticals的ASO疗法sapablursen已进入Ⅲ期临床,该药物通过降低TMPRSS6基因编码的跨膜蛋白酶丝氨酸6的产生,增加铁调素的表达,从而对真性红细胞增多症产生积极治疗效果,2025年3月,Ono Pharmaceutical与Ionis签订许可协议,获得该药物的开发及商业化权益,彰显了市场对其临床价值的认可;在重症肌无力领域,再生元(Regeneron)与Alnylam公司联合开发的补体C5靶向siRNA疗法cemdisiran,已在临床3期试验中达到主要和关键次要终点,该药物每三个月皮下注射一次,单药可实现74%的补体活性抑制率,联合疗法抑制率接近99%,再生元计划于2026年第一季度提交上市申请,有望成为重症肌无力治疗的全新选择。
从适应症布局来看,寡核苷酸药物的核心优势在于能够针对遗传性疾病的根本病因进行干预,尤其适合那些由单基因缺陷导致的罕见病,而神经系统与肌肉罕见病多为单基因遗传病,且传统治疗手段有限,成为寡核苷酸药物的核心发力领域。随着技术的不断成熟,其适应症还将进一步拓展至更多罕见病乃至常见病领域,展现出广阔的临床应用前景。三、商业化前夜:疗效验证与支付可及的双重考验
十多款寡核苷酸新药迈入Ⅲ期临床,标志着这类药物已进入临床验证的最后阶段,距离商业化落地仅一步之遥。但Ⅲ期临床既是科学验证的终点,也是商业化挑战的起点——对于这些即将上市的新药而言,要真正实现临床价值与商业价值的统一,还需跨越长期疗效与安全性验证、罕见病定价与医保准入两大核心考验,这也是决定寡核苷酸药物能否开启黄金十年的关键。
第一个核心考验,是长期疗效与安全性的持续验证。寡核苷酸药物作为一类新型疗法,其临床应用时间相对较短,长期安全性数据仍在积累中,尤其是AOC、LICA等新型递送平台,其潜在的免疫原性风险、慢性给药的组织累积效应,仍需更大样本、更长随访时间的临床数据来验证。一方面,寡核苷酸药物通过调控基因表达发挥作用,长期给药可能会对正常基因功能产生影响,进而引发未知的不良反应;另一方面,新型递送系统如AOC,抗体与寡核苷酸的偶联物可能会引发机体的免疫反应,导致药物疗效下降或产生不良反应,这些问题都需要在Ⅲ期临床及上市后随访中进一步明确。
第二个核心考验,是罕见病定价与医保准入的难题,这也是制约寡核苷酸药物临床可及性的关键。以目前已上市的寡核苷酸疗法为参照,其年治疗费用普遍在数十万美元量级,例如已获批用于SMA治疗的Spinraza,年治疗费用超过70万美元,高昂的价格使得多数患者难以负担,也给医保支付带来了巨大压力。随着多款同适应症寡核苷酸药物(如天使综合征的两款ASO疗法)同期推进,市场竞争将逐步加剧,差异化临床优势与药物经济学(pharmacoeconomic)数据,将成为支付方谈判的关键筹码。
寡核苷酸药物的商业化大潮已悄然来临,行业即将进入规模化落地阶段。再生元的cemdisiran已计划在2026年第一季度提交上市申请,有望成为首款治疗重症肌无力的siRNA药物;ION582、del-desiran等重磅管线,也将在未来12-18个月内读出Ⅲ期关键数据,逐步推进上市进程;此外,药明康德WuXi TIDES平台等专业服务平台的崛起,围绕寡核苷酸疗法建立了化合物合成、工艺开发及生产的一站式服务,覆盖从药物发现到商业化生产的全生命周期,加速了寡核苷酸药物的研发与落地速度。
对于整个行业而言,随着更多寡核苷酸药物的上市,市场竞争将逐步加剧,行业将逐步从“技术驱动”向“疗效与成本驱动”转型。未来,具备差异化临床优势、合理定价策略、完善商业化布局的企业,将在竞争中脱颖而出;同时,随着医保政策的不断完善、药物经济学研究的深入,以及研发技术的持续进步,寡核苷酸药物的价格有望逐步下降,提升临床可及性,让更多罕见病患者受益。
最后
从早期研发的“举步维艰”,到如今十多款管线迈入Ⅲ期临床,寡核苷酸药物用十年时间,实现了从“不可能”到“临床希望”的跨越,不仅改写了罕见病治疗的格局,也开启了基因治疗的黄金时代。技术迭代的突破,让寡核苷酸药物实现了精准递送的质变;适应症的持续拓展,为更多“无药可医”的罕见病患者带来了新生;而商业化前夜的双重考验,既是挑战,也是行业走向成熟的必经之路。
参考:公开资料整理
立即扫码加入药事纵横交流群
寡核苷酸siRNA临床3期临床2期并购
2026-03-04
The molecule was in an open-label phase 1/2 study for multiple types of solid tumor driven by the MAPK pathway, both as a monotherapy and in combination with other drugs.\n Ono Pharmaceutical subsidiary Deciphera Pharmaceuticals has dropped an early-stage candidate for advanced cancers from its pipeline.DCC-3084, a pan-RAF inhibitor, “is no longer in our pipeline and we are currently not planning additional development at this time,” a Deciphera spokesperson confirmed to Fierce Biotech on Tuesday. The decision was made for strategic reasons and unrelated to the asset’s safety or efficacy, they explained.“Given that it was such an early-stage program, employees working on it were simply reassigned to another program and there were no layoffs,” the spokesperson added.The molecule was in an open-label phase 1/2 study for multiple types of solid tumor driven by the MAPK pathway, both as a monotherapy and in combination with other drugs. The now-terminated trial kicked off in May 2024 and enrolled 29 total patients, according to the federal clinical trial database. Japanese drugmaker Ono acquired Deciphera for $2.4 billion in mid-2024, gaining the already approved gastrointestinal cancer med Qinlock and the rare tumor drug vimseltinib, which was later approved as Romvimza.Even with DCC-3084 sent to the scrap heap, Deciphera still boasts a packed pipeline led by BTK inhibitor tirabrutinib and antisense oligonucleotide sapablursen. Tirabrutinib was discovered by Ono and is approved in Japan, South Korea and Taiwan as Velexbru. The candidate is currently being considered for FDA approval in relapsed or refractory primary central nervous system lymphoma, with a decision expected by Dec. 18. Deciphera is now running a phase 3 confirmatory trial in the indication.Sapablursen, meanwhile, was licensed by Ono from Ionis Pharmaceuticals for $280 million upfront in March 2025. Ionis shared positive phase 2 data for the oligo in polycythemia vera, a rare blood cancer, at the American Society of Hematology meeting last December. Deciphera expects to launch a phase 3 trial for sapablursen this year.

临床3期并购临床2期上市批准ASH会议
2026-02-28
·医药观澜
编者按:今日(2026年2月28日)是第19个国际罕见病日。根据世界卫生组织(WHO)2025年发表的数据,目前已知的罕见病超过7000种,影响到全球3亿多人。在罕见病新药研发领域,寡核苷酸疗法凭借独特的作用机制,正成为重要的突破方向。当前,全球范围内已有十多款寡核苷酸疗法获监管机构批准治疗罕见病,此外还有上百项寡核苷酸管线在针对罕见病适应症进行临床研究,未来有望造福更多患者。作为全球医药创新的赋能者,药明康德化学业务旗下专注于寡核苷酸和多肽及相关化学偶联药物的WuXi TIDES平台,围绕寡核苷酸疗法建立了化合物合成、工艺开发及生产的一站式服务平台,覆盖从药物发现、CMC开发,到商业化生产的全生命周期,加速将合作伙伴的创新构想转化为现实,更好地造福全球病患。
寡核苷酸药物是全球新药开发的重要热点,凭借其直接调控基因表达的独特机制,在多种疾病治疗领域展现出潜力。尤其在罕见病领域,更是成为新药研发的重要突破方向。
通过公开渠道梳理,当前全球范围内已有十多款寡核苷酸疗法获监管机构批准治疗罕见病,为遗传性血管性水肿、血友病、转甲状腺素蛋白淀粉样变性多发性神经病、转甲状腺素蛋白淀粉样变心肌病、肌萎缩侧索硬化症、脊髓性肌萎缩症、杜氏肌营养不良、纯合子型家族性高胆固醇血症、肝卟啉症等患者带来了新的治疗选择。尤其是在刚刚结束的2025年,美国FDA批准了至少2款治疗罕见病的寡核苷酸疗法,包括反义寡核苷酸配体偶联(LICA)药物donidalorsen获批用于预防遗传性血管性水肿(HAE)发作、靶向抗凝血酶的皮下注射siRNA药物fitusiran获批用于血友病A或B患者常规预防,引起行业关注。
除了已经获批的疗法,还有近百项寡核苷酸疗法管线在针对罕见病适应症进行临床研究,未来有望造福更多患者。通过梳理,其中有10多款新药目前已经进入3期临床研究阶段,意味着其有望即将为患者带来新的治疗选择。
近一年来,多款处于3期临床阶段的寡核苷酸新药迎来新进展,这些新药包括反义寡核苷酸(ASO)、siRNA、抗体偶联siRNA疗法,涉及的适应症涵盖:天使综合征、1型肌强直性营养不良、Dravet综合征、重症肌无力、脊髓性肌萎缩症、面肩肱型肌营养不良症、真性红细胞增多症等。
多款3期临床阶段罕见病寡核苷酸疗法迎新进展
在过去一年,多款治疗罕见病的寡核苷酸疗法获得FDA授予突破性疗法认定,彰显其临床潜力。比如,2025年9月,Ionis Pharmaceuticals公司在研的ASO疗法ION582获FDA授予突破性疗法认定,用于治疗天使综合征。这是一种罕见遗传性神经发育疾病。ION582旨在抑制UBE3A反义转录本(UBE3A-ATS)的表达,并激活来自父体的UBE3A等位基因以增加患者大脑中UBE3A蛋白的产生,为天使综合征的潜在疗法。Ionis此前已启动ION582的全球3期关键性REVEAL研究,计划纳入携带母源UBE3A基因缺失或突变的儿童和成人天使综合征患者,公司预计该研究将在2026年完成入组,这将为ION582未来的上市申请奠定重要基础。
再如,2025年7月,Ultragenyx公司在研ASO疗法GTX-102(apazunersen)获得FDA授予突破性疗法认定,用于治疗天使综合征。GTX-102通过鞘内给药方式递送,该疗法可以促进神经元细胞中父系UBE3A的等位基因表达,产生患者体内所缺失的关键蛋白产物。该疗法的相关全球3期试验正在进行中。
除此之外,还有多款新药公布最新临床研究数据,比如:
今年2月,Avidity Biosciences宣布其在研抗体偶联RNAi疗法delpacibart etedesiran(del-desiran,AOC 1001)在1型肌强直性营养不良(DM1)患者中开展的1/2期MARINA试验最终结果发表于《新英格兰医学杂志》。研究结果显示,del-desiran成功递送至肌肉组织,在所有接受治疗的受试者中,DMPK mRNA平均降低约40%。DM1是一种逐步加重且往往致命的罕见神经肌肉疾病。Del-desiran是Avidity利用其抗体偶联寡核苷酸(AOC)平台开发的候选疗法,它将与转铁蛋白受体1(TfR1)结合的专有单克隆抗体与靶向DMPK基因的siRNA偶联,旨在通过降低与疾病相关的DMPK基因的mRNA水平,解决DM1的根本原因。
Avidity公司另一款在研AOC候选药物delpacibart braxlosiran(del-brax)也于2025年6月公布了治疗面肩肱型肌营养不良症(FSHD)的临床1/2期试验FORTITUDE积极新数据:与安慰剂相比,在接受del-brax治疗的FSHD患者中观察到肌肉功能活动能力、肌肉力量和患者报告的结局(PROs)衡量的生活质量方面的改善,并且生物标志物出现了快速而显著的下降。FSHD是一种罕见的遗传性疾病,其特征是终身、持续的肌肉功能丧失、显著的疼痛、疲劳和渐进性残疾。Del-brax旨在治疗FSHD根本原因,由一种专有的TfR1靶向单克隆抗体与靶向DUX4 mRNA的siRNA偶联所组成。
再如,2025年10月,渤健(Biogen)与Stoke Therapeutics公司共同宣布了针对Dravet综合征的在研ASO药物zorevunersen的最新研究进展。Dravet综合征是一种严重且进展性的罕见遗传性癫痫。该药物旨在通过增强SCN1A基因非突变(野生型)拷贝的功能,提升脑细胞中NaV1.1蛋白的表达,从而治疗Dravet综合征的根本病因。最新公布的两年分析数据显示,接受zorevunersen治疗的Dravet综合征患者在认知和行为方面持续改善,这与一项同样为期两年的自然病史研究中患者几乎无改善的结果形成鲜明对比。在为期三年的OLE研究中,临床医生和护理人员分别报告了95%(n=19)的患者整体临床状况得到改善。
渤健另一款在研ASO疗法salanersen治疗脊髓性肌萎缩症(SMA)的一项1期临床试验的积极结果也于2025年6月公布。该药物与渤健已获批的ASO疗法Spinraza(nusinersen)具有相同的作用机制,但在设计上追求更高效力,并有望实现每年仅需一次给药。SMA是一种遗传性神经肌肉病。研究结果显示,salanersen表现出良好的耐受性,在基线NfL浓度较高的患者中,治疗6个月后平均神经退行性标志物神经丝轻链(NfL)下降幅度达70%,这一效果可持续维持至一年。
2025年8月,再生元(Regeneron)也宣布其与Alnylam公司联合开发的补体C5靶向siRNA疗法cemdisiran,在治疗成人全身性重症肌无力(gMG)的临床3期试验中达到了主要和关键次要终点。再生元计划在与FDA沟通后,于2026年第一季度提交cemdisiran单药的监管申请。分析显示,每三个月皮下注射一次的cemdisiran单药显示出平均74%的补体活性抑制率。而cemdisiran与C5抗体pozelimab的联合疗法则达成接近99%的补体活性抑制。
交易合作方面也迎来新进展,比如,2025年3月,Ono Pharmaceutical宣布与Ionis Pharmaceuticals签订许可协议,获得ASO疗法sapablursen的开发及商业化权益。ONO将支付2.8亿美元前期付款,并根据达到研发、监管及销售里程碑,支付高达6.6亿美元的额外里程碑付款。Sapablursen是一种用于治疗真性红细胞增多症(PV)的在研ASO药物,其设计旨在降低TMPRSS6基因编码的跨膜蛋白酶丝氨酸6的产生,从而增加铁稳态关键调控因子铁调素(hepcidin)的表达。通过提高铁调素的产生,sapablursen有望对真性红细胞增多症等血液疾病产生积极影响。
除了上述进展,还有多款治疗罕见病的寡核苷酸新药处于积极的临床开发阶段,并取得新进展。限于篇幅,此处不再一一介绍。很高兴看到这些创新疗法取得积极进展,为患者带来新的治疗希望。
一体化CRDMO平台赋能寡核苷酸疗法创新
凭借其高度靶向性、灵活可编程和相对较短的开发周期等特点,寡核苷酸疗法近年来发展迅速,受到产业界的广泛关注,在包括罕见病在内的多个疾病治疗领域发挥着重要作用。
在此背景下,作为全球医药创新的赋能者,药明康德化学业务旗下专注于寡核苷酸和多肽及相关化学偶联药物的新分子业务平台——WuXi TIDES平台,围绕siRNA、ASO等寡核苷酸疗法,建立了化合物合成、工艺开发及生产的一站式服务平台,覆盖从药物发现、CMC开发,到商业化生产的全生命周期,加速将合作伙伴的创新构想转化为现实,更好地造福全球病患。
具体而言,WuXi TIDES的寡核苷酸平台可为全球合作伙伴针对性地提供从药物发现到商业化生产的一体化CRDMO服务。药物发现阶段的合成服务支持高通量库合成和定制合成,涵盖多种类型的寡核苷酸及其单体、连接子、配体和偶联物,助力合作伙伴快速推进临床前研究。同时,可无缝衔接到工艺开发阶段,放大到从mmol到mol的任何规模,充分满足从临床前、临床到商业化阶段的需求。
在寡核苷酸的偶联方面,WuXi TIDES全面的平台能力可支持寡核苷酸与多肽、脂质、小分子、毒素/药物等组件的偶联,为复杂的寡核苷酸偶联药物提供一体化解决方案。
破解罕见病新药研发困境,需要全球生物医药生态圈的持续协同合作和共同努力。药明康德也将继续以一体化、端到端的CRDMO赋能平台,助力全球合作伙伴加速新药研发进程,降低研发成本,让包括罕见病在内的各类疾病药物研发更高效、更易行。
参考资料:
[1]World Health Organization.Rare diseases: A global health priority for equity and inclusion. Retrieved Feb 10 , 2025. From https://apps.who.int/gb/ebwha/pdf_files/EB156/B156_(15)-en.pdf
免责声明:本文仅作信息交流之目的,文中观点不代表药明康德立场,亦不代表药明康德支持或反对文中观点。本文也不是治疗方案推荐。如需获得治疗方案指导,请前往正规医院就诊。
版权说明:欢迎个人转发至朋友圈,谢绝媒体或机构未经授权以任何形式转载至其他平台。转载授权请在「医药观澜」微信公众号回复“转载”,获取转载须知。
100 项与 Sapablursen 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 真性红细胞增多症 | 临床3期 | - | 2026-06-01 | |
| β地中海贫血 | 临床2期 | 澳大利亚 | 2020-09-24 | |
| β地中海贫血 | 临床2期 | 希腊 | 2020-09-24 | |
| β地中海贫血 | 临床2期 | 黎巴嫩 | 2020-09-24 | |
| β地中海贫血 | 临床2期 | 泰国 | 2020-09-24 | |
| β地中海贫血 | 临床2期 | 土耳其 | 2020-09-24 | |
| 非输血依赖性地中海贫血 | 临床2期 | 澳大利亚 | 2020-09-24 | |
| 非输血依赖性地中海贫血 | 临床2期 | 希腊 | 2020-09-24 | |
| 非输血依赖性地中海贫血 | 临床2期 | 黎巴嫩 | 2020-09-24 | |
| 非输血依赖性地中海贫血 | 临床2期 | 泰国 | 2020-09-24 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
临床2期 | 49 | 簾簾膚艱鑰製築繭鑰遞(願鹹顧鹽觸憲獵範顧蓋) = 構衊構製選醖壓觸繭鏇 夢觸齋齋鏇壓構簾鹽醖 (壓襯鹹繭鹽顧獵構構選, 0.09) 更多 | 积极 | 2025-12-06 | |||
簾簾膚艱鑰製築繭鑰遞(願鹹顧鹽觸憲獵範顧蓋) = 鬱繭簾鑰觸選壓構鏇獵 夢觸齋齋鏇壓構簾鹽醖 (壓襯鹹繭鹽顧獵構構選, 0.07) 更多 | |||||||
临床2期 | 29 | (Cohort A: Sapablursen) | 鬱鏇醖遞製鹽醖壓積壓 = 齋齋壓襯鏇齋衊衊製範 蓋觸獵壓衊網積餘構鏇 (築夢積蓋鏇鏇廠艱遞選, 餘遞簾衊窪艱鏇鹹壓醖 ~ 醖廠廠鹽願構鹽艱鏇憲) 更多 | - | 2025-02-18 | ||
(Cohort B: Sapablursen) | 鬱鏇醖遞製鹽醖壓積壓 = 衊積餘網繭壓醖網鹽鹽 蓋觸獵壓衊網積餘構鏇 (築夢積蓋鏇鏇廠艱遞選, 鬱範餘餘築膚壓餘鹹壓 ~ 壓廠網積鹽鬱鑰膚窪廠) 更多 |
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或

药物交易
使用我们的药物交易数据加速您的研究。
登录
或

核心专利
使用我们的核心专利数据促进您的研究。
登录
或

临床分析
紧跟全球注册中心的最新临床试验。
登录
或

批准
利用最新的监管批准信息加速您的研究。
登录
或

特殊审评
只需点击几下即可了解关键药物信息。
登录
或

生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用


