预约演示
更新于:2026-05-30
Veltuzumab
维妥珠单抗
更新于:2026-05-30
概要
基本信息
在研机构- |
权益机构- |
最高研发阶段终止临床2期 |
首次获批日期- |
最高研发阶段(中国)- |
特殊审评孤儿药 (美国) |
登录后查看时间轴
结构/序列
Sequence Code 52152L

来源: *****
Sequence Code 10069122H

来源: *****
关联
9
项与 维妥珠单抗 相关的临床试验NCT01390545
VELVET (Veltuzumab Various Doses Exploratory Trial), a Randomized, Double Blind, Placebo Controlled, Multicentre, Multinational Phase II Dose Range Finding Trial in Subjects With Moderate to Severe Rheumatoid Arthritis Insufficiently Controlled With Either Methotrexate Alone or Methotrexate Plus Anti-tumour Necrosis Factor Biological Treatment, Comparing 3 Different Subcutaneous Dosages of Anti-CD20 Monoclonal Antibody Veltuzumab to Placebo as an add-on Therapy to Methotrexate.
This is a multi-national, multi-centre, placebo-controlled, double-blind, randomized, 4-arm parallel group trial, comparing three different dose levels (80 mg, 160 mg and 320 mg) of veltuzumab to placebo, administered weekly (days 1, 8, 15 and 22) by subcutaneous (sc) injection to subjects with moderate to severe rheumatoid arthritis (RA) (cumulative veltuzumab doses 320 mg, 640 mg, and 1280 mg, respectively). All subjects will be on continued stable co-medication with methotrexate (MTX).
开始日期2011-08-01 |
NCT01147393
Phase I/II Study of Combination Veltuzumab (Anti-CD20) and Fractionated 90Y- Epratuzumab (Anti-CD22) Radioimmunotherapy in Patients With Follicular Lymphoma
A Phase I/II clinical trial using a fractionated dosing regimen of 90Y-epratuzumab (anti-CD22) has showed encouraging responses in follicular and aggressive NHL with an ability to administer safely 2 injections of 20 mCi/m2 spaced 1 week apart. The investigators propose to combine this active 90Y-epratuzumab treatment with a regimen of veltuzumab that was also found active in Phase I/II trials.
The goal of this study is to determine the safety and efficacy of 90Y-epratuzumab when used in combination with veltuzumab. The primary objective is to determine the response rate of this combination treatment. Secondary objectives are to assess safety, pharmacokinetics and targeting of 90Y-epratuzumab . Veltuzumab blood levels and anti-antibody responses will also be monitored at various times.
The goal of this study is to determine the safety and efficacy of 90Y-epratuzumab when used in combination with veltuzumab. The primary objective is to determine the response rate of this combination treatment. Secondary objectives are to assess safety, pharmacokinetics and targeting of 90Y-epratuzumab . Veltuzumab blood levels and anti-antibody responses will also be monitored at various times.
开始日期2010-10-01 |
申办/合作机构 |
NCT01101581
Phase I/II Study of Veltuzumab Combined With 90Y-Epratuzumab Tetraxetan in Patients With Relapsed/Refractory, Aggressive Non- Hodgkin's Lymphoma
The goal of this study is to evaluate a new approach to immunotherapy in NHL by combining two antibodies, veltuzumab and epratuzumab. For treatment, epratuzumab has also been attached to a radioactive isotope called 90yttrium (90Y-epratuzumab). Veltuzumab and 90Y-epratuzumab attack different areas on lymphoma cells. Because of this, treatment with the combination may provide more effective treatment in NHL than either veltuzumab or 90Y-epratuzumab given alone.
开始日期2010-05-01 |
申办/合作机构 |
100 项与 维妥珠单抗 相关的临床结果
登录后查看更多信息
100 项与 维妥珠单抗 相关的转化医学
登录后查看更多信息
100 项与 维妥珠单抗 相关的专利(医药)
登录后查看更多信息
1,046
项与 维妥珠单抗 相关的文献(医药)2026-07-01·Actas Dermo-Sifiliograficas
Experience With Rituximab in Patients With Pemphigus Vulgaris and Hepatitis B
Article
作者: Forero, O L ; Candiz, M E ; Paz, S ; Lloveras, S ; Collado Gomez, R ; Carranza, J
Rituximab is an anti-CD20 monoclonal antibody used as first-line therapy for moderate-to-severe pemphigus vulgaris. For many years, it was contraindicated in patients with a past medical history of hepatitis B due to the risk of disease reactivation. However, it has recently been recognized that this infection should be considered a comorbidity requiring monitoring rather than an absolute contraindication. Only a few publications in the dermatologic literature describe in detail the management of rituximab in patients with a history of hepatitis B. We present two cases of pemphigus vulgaris in the setting of resolved hepatitis B infection who received antiviral prophylaxis and rituximab.
2026-06-01·Multiple Sclerosis and Related Disorders
Effectiveness and safety of ocrelizumab in relapsing-onset multiple sclerosis: A nationwide real-world study from Slovakia
Article
作者: Laurincová, Silvia ; Szilasiová, Jarmila ; Kiačiková, Mária ; Hančinová, Viera ; Dziaková, Jana ; Fedičová, Miriam ; Vitková, Marianna ; Kahancová, Edita ; Slezáková, Darina ; Kantorová, Ema ; Karlík, Martin ; Kováčová, Slavomíra ; Filippi, Pavol ; Bilá, Anna ; Bullová, Andrea ; Koleda, Peter ; Koleňáková, Katarína
BACKGROUND:
Ocrelizumab (OCR) is a high-efficacy anti-CD20 monoclonal antibody approved for multiple sclerosis (MS) treatment. This nationwide real-world study evaluated the effectiveness and safety of OCR in patients with relapsing-onset MS (ROMS) in Slovakia.
METHODS:
This multicenter retrospective study included 499 patients with ROMS treated between January 2019 and January 2024. Outcomes included annualized relapse rate (ARR), confirmed disability progression (6mCDP), MRI activity, NEDA-3, and safety parameters.
RESULTS:
During a mean follow-up of 2.4 years, ARR decreased from 1.1 to 0.04; 6mCDP occurred in 7.1% of patients, and NEDA-3 was achieved in 75.5%. OCR was well tolerated with infusion-related reactions (12.2%) and infections (<6%) as the most common adverse events.
CONCLUSIONS:
OCR demonstrated high effectiveness and a favorable safety profile in routine clinical practice, supporting early initiation of high-efficacy therapy in relapsing-onset MS.
2026-06-01·Kidney International Reports
Efficacy of Obinutuzumab for Frequently Relapsing or Steroid-Dependent Nephrotic Syndrome
Article
作者: Huo, Qingyu ; Huang, Yinghui ; Cheng, Jinbo ; Ai, Yuxin ; Hu, Hongtu ; Xin, Wang ; Yao, Mengying ; Zhu, Yuqi ; Gong, Shuiqin ; Yao, Heng ; Li, Yifan ; Li, Shuangjiang
Introduction:
The first-generation anti-CD20 monoclonal antibody, rituximab, has effectively reduced relapse rates in patients with frequently relapsing or steroid-dependent nephrotic syndrome (FRNS or SDNS). However, its effects are often transient, and some patients are nonresponsive. Obinutuzumab, a next-generation humanized type II anti-CD20 monoclonal antibody, demonstrates stronger and more sustained B-cell depletion than rituximab. However, clinical evidence regarding its efficacy in FRNS or SDNS remains limited.
Methods:
This retrospective single-center cohort study included 161 patients with FRNS or SDNS who received ≥ 1 dose of obinutuzumab and had > 3 months of follow-up at our institution. We evaluated the efficacy and safety of obinutuzumab in FRNS or SDNS by analyzing the remission, relapse, and adverse events in all enrolled patients.
Results:
During the follow-up period, 91.9% of patients (148/161) achieved remission following obinutuzumab infusion with a median time of 2.3 months (interquartile range [IQR]: 0.8-5.8). The median relapse-free survival (RFS) was 26.9 months (95% confidence intervals [CI]: 23.2-30.6). Significant improvements were observed in nephrotic syndrome parameters: the urine protein-to-creatinine ratio (UPCR) markedly decreased (median decreased from 5.7000 g/g to 0.1024 g/g, P < 0.001), and the median serum albumin level significantly increased (median increased from 28.4 g/l to 44.5 g/l, P < 0.001), whereas the estimated glomerular filtration rate (eGFR) showed no significant change (92 vs. 96 ml/min per 1.73 m2, P = 0.25). One patient experienced a severe pulmonary infection, and no other serious adverse events were reported.
Conclusion:
Obinutuzumab may offer a new treatment option for patients with FRNS or SDNS, providing rapid disease control, high remission rates, and durable benefits with a tolerable safety profile.
29
项与 维妥珠单抗 相关的新闻(医药)2026-05-01
笔者:这篇关于《In vivo CAR-T、TCE、单抗、CAR-T、CAR-NK和CAR-M治疗自身免疫疾病的研究进展与临床应用》的文章是我基于近期的文献调研与个人研究独立完成的原创学术写作,全文约一万字,结构严谨、力求客观。不建议碎片化快速浏览,建议先点赞收藏,留出一段完整时间细读,希望能帮你系统梳理该领域的逻辑脉络。
以下为正文,请enjoy,欢迎大家转发分享
摘要
自身免疫疾病是一类由免疫系统异常攻击自身组织引发的慢性疾病,其病理机制涉及免疫耐受失衡、自身反应性淋巴细胞异常活化及炎症因子过度释放。近年来,以CAR-T、T细胞衔接器(TCE)、单克隆抗体、CAR-NK及CAR-M为代表的免疫治疗技术在自身免疫疾病领域展现出巨大潜力。本综述系统梳理了上述免疫治疗技术的基础理论、流行病学特征、诊断技术、治疗策略、技术进展、争议点及未来展望,重点分析了B细胞清除效果与疾病疗效的相关性,并探讨了全球合作与政策支持对免疫治疗发展的推动作用。研究表明,不同免疫治疗策略在B细胞清除的程度和难易程度上存在显著差异,其中CD19靶向CAR-T和抗CD20单抗在血液B细胞清除中表现出较高效率,但骨髓及组织B细胞清除仍面临挑战。未来,新型免疫治疗技术如双特异性抗体、基因编辑CAR-T及免疫微环境调控策略将为自身免疫疾病治疗提供新方向,而全球合作与政策支持则是推动免疫治疗普及和公平可及的关键。体内CAR-T、TCE、单抗、CAR-T、CAR-NK和CAR-M治疗自身免疫疾病的基础理论自身免疫疾病的病理机制与免疫治疗
自身免疫疾病的核心病理机制是免疫系统对自身抗原的耐受失衡,导致自身反应性T细胞和B细胞异常活化,产生自身抗体并引发慢性炎症[1]。例如,在1型糖尿病(T1D)中,自身反应性T细胞攻击胰岛β细胞,导致胰岛素分泌不足,其病理过程可分为六个阶段,从自身抗体出现到β细胞功能完全丧失[1]。在系统性红斑狼疮(SLE)中,B细胞过度活化产生抗核抗体等自身抗体,形成免疫复合物沉积于组织,引发炎症损伤[2]。此外,辅助性T细胞亚群失衡也参与自身免疫疾病的发生,如Th9细胞分泌的IL-9在肝纤维化中发挥促炎作用,中和IL-9可减轻肝星状细胞活化及炎症反应[3]。
免疫治疗的核心策略是恢复免疫耐受或清除异常活化的免疫细胞。例如,低剂量IL-2治疗通过选择性扩增调节性T细胞(Treg),恢复SLE患者的免疫平衡[2]。在实验性自身免疫性脑脊髓炎(EAE)模型中,抗CD19单抗MEDI551可有效清除自身反应性B细胞及浆细胞,减少自身抗体产生,其疗效优于抗CD20单抗[4]。此外,黏膜免疫耐受诱导也是一种潜在策略,如胶原V黏膜接种可通过IL-35依赖的机制减轻动脉粥样硬化斑块负荷[5]。这些研究表明,免疫治疗通过靶向免疫细胞或调节免疫分子,可有效干预自身免疫疾病的病理过程。治疗基本原理
CAR-T技术通过基因工程将T细胞修饰为表达嵌合抗原受体(CAR)的细胞,使其特异性识别靶抗原并发挥杀伤作用[6]。CAR通常由抗原结合域、铰链区、跨膜区和胞内信号域组成,其中CD28或4-1BB共刺激域可增强CAR-T细胞的增殖和存活[7]。在自身免疫疾病中,CAR-T主要靶向B细胞表面抗原如CD19或CD20,清除自身反应性B细胞[8]。例如,CD19 CAR-T在难治性SLE患者中可实现长期B细胞清除,诱导疾病缓解[8]。
T细胞衔接器(TCE)是一类双特异性抗体,通过同时结合T细胞表面的CD3和靶细胞表面的抗原,将T细胞招募至靶细胞并激活其杀伤功能[9]。在B细胞相关自身免疫疾病中,CD19×CD3 TCE可有效清除B细胞,其机制依赖于CD8+ T细胞的细胞毒性[10]。单克隆抗体通过特异性结合靶分子发挥作用,如抗CD20单抗利妥昔单抗通过抗体依赖的细胞毒性(ADCC)和补体依赖的细胞毒性(CDC)清除B细胞[4]。CAR-NK技术则利用NK细胞的天然杀伤活性,通过CAR修饰增强其特异性,且NK细胞的低免疫原性使其具有异体应用潜力[11]。CAR-M技术通过修饰巨噬细胞,增强其吞噬和抗原呈递功能,在自身免疫疾病中可调节炎症微环境[8]。
这些技术的共同目标是特异性清除异常免疫细胞或调节免疫反应,但在作用机制、靶向特异性及安全性上存在差异。例如,CAR-T细胞具有较强的增殖能力和持久杀伤活性,但存在细胞因子释放综合征(CRS)风险;而单抗治疗相对安全,但对组织驻留B细胞的清除效果有限[12]。免疫治疗在自身免疫疾病中的应用历史
免疫治疗在自身免疫疾病中的应用可追溯至20世纪初的脱敏治疗,但现代免疫治疗的发展始于单克隆抗体技术的突破。1986年,抗CD3单抗OKT3获批用于器官移植排斥反应,开启了抗体治疗自身免疫疾病的先河[13]。2006年,利妥昔单抗获批用于类风湿关节炎(RA),成为首个用于自身免疫疾病的抗B细胞单抗[14]。此后,多种单抗如抗TNF-α、抗IL-6R抗体相继获批,显著改善了RA、强直性脊柱炎等疾病的治疗效果[15]。
CAR-T技术在自身免疫疾病中的应用起步较晚,2017年首次报道CD19 CAR-T治疗难治性SLE患者,实现了长期缓解[8]。近年来,CAR-T、TCE及CAR-NK技术在自身免疫疾病中的临床试验逐渐增多,如CD19/BCMA双靶点CAR-NK治疗系统性硬化症(SSc)的研究显示出显著的B细胞清除效果[11]。此外,免疫检查点抑制剂在自身免疫疾病中的应用也受到关注,如PD-1抑制剂在某些自身免疫疾病中的试验,但需注意其可能诱发的免疫相关 adverse事件[16]。自身免疫疾病的流行病学特征
自身免疫疾病的全球患病率约为5%,且呈上升趋势[17]。不同疾病的流行病学特征存在显著差异:多发性硬化(MS)在北美和欧洲的患病率高达100/10万,而在东亚和撒哈拉以南非洲仅为2/10万[17];系统性红斑狼疮(SLE)的女性患病率是男性的9倍,发病高峰为20-40岁[18];类风湿关节炎(RA)的全球患病率约为0.5%-1%,女性患病率是男性的2-3倍[15]。
自身免疫疾病的发病与遗传、环境因素密切相关。例如,MS与HLA-DRB1*15:01等位基因显著相关,携带该等位基因的人群发病风险增加3-4倍[17];EB病毒感染是MS的重要环境危险因素,尤其是儿童期后感染[17]。此外,自身免疫疾病常存在共病现象,如玫瑰痤疮患者合并1型糖尿病、乳糜泻、MS及RA的风险分别增加2.59、2.03、1.65和2.14倍[19]。
不同地区的自身免疫疾病流行病学特征存在差异,如在秘鲁农村地区,自身免疫疾病的患病率约为3%,主要包括哮喘、RA和桥本甲状腺炎[20];而在日本,显微镜下多血管炎(MPA)和髓过氧化物酶-ANCA阳性血管炎更为常见[21]。这些差异可能与遗传背景、环境因素及医疗水平有关。免疫治疗在不同人群中的应用现状
免疫治疗在自身免疫疾病中的应用存在人群差异。例如,在RA患者中,抗TNF-α单抗的疗效在女性患者中优于男性,可能与女性患者的炎症水平更高有关[15]。在儿童自身免疫疾病中,利妥昔单抗治疗激素依赖型肾病综合征的安全性较好,但需注意迟发性中性粒细胞减少和低丙种球蛋白血症[22]。在老年人群中,免疫治疗的不良反应风险增加,如PD-1抑制剂在老年患者中更容易诱发免疫相关 adverse事件[23]。
不同种族人群对免疫治疗的反应也存在差异。例如,在非小细胞肺癌患者中,非洲裔患者的肿瘤突变负荷(TMB)高于其他种族,可能对免疫检查点抑制剂更敏感[24]。在自身免疫疾病中,亚洲人群对利妥昔单抗的反应率与欧美人群相似,但不良反应谱可能不同[25]。此外,免疫治疗在合并其他疾病的患者中应用需谨慎,如糖尿病患者接受抗CD20单抗治疗时,尽管B细胞清除效果与非糖尿病患者相似,但临床缓解率较低[26]。
免疫治疗的应用现状还受到经济因素的影响,在低收入国家,免疫治疗的可及性较低,而在高收入国家,生物制剂的使用率较高[27]。未来需通过政策支持和技术创新,提高免疫治疗的公平可及性。全球免疫治疗的流行趋势
全球免疫治疗市场呈快速增长趋势,2020年市场规模约为1500亿美元,预计2025年将达到3000亿美元[28]。在自身免疫疾病领域,生物制剂的市场份额逐年增加,其中抗TNF-α单抗、抗IL-6R单抗及抗CD20单抗是主要产品[28]。近年来,CAR-T、TCE及CAR-NK技术在自身免疫疾病中的临床试验数量显著增加,2020-2025年期间,全球开展的相关临床试验超过50项[8]。
免疫治疗的研究热点逐渐从非特异性免疫抑制转向靶向免疫调节。例如,针对B细胞的治疗策略从利妥昔单抗单药治疗发展为CAR-T、TCE及双特异性抗体联合治疗[26]。此外,免疫微环境调控成为研究热点,如通过调节肿瘤相关巨噬细胞(TAM)或树突状细胞(DC)改善免疫治疗效果[29]。
全球免疫治疗的区域发展不平衡,北美和欧洲占据主导地位,而亚洲的研究和应用增长迅速[28]。例如,中国在CAR-T技术领域的研究论文数量已位居全球第二[28]。未来,全球合作将成为推动免疫治疗发展的关键,如国际多中心临床试验和技术转让[30]。自身免疫疾病的诊断标准与技术
自身免疫疾病的诊断通常基于临床症状、实验室检查及影像学表现。例如,SLE的诊断采用2012年SLICC标准,包括11项临床指标和6项免疫指标,满足4项即可诊断[18]。RA的诊断采用2010年ACR/EULAR标准,基于关节受累情况、血清学指标、急性时相反应物及症状持续时间[15]。
实验室检查在自身免疫疾病诊断中至关重要,包括自身抗体检测、炎症指标及免疫细胞亚群分析。例如,抗核抗体(ANA)是SLE的标志性抗体,阳性率约为95%[18];抗环瓜氨酸肽(anti-CCP)抗体对RA的诊断特异性高达95%[14]。免疫细胞亚群分析可通过流式细胞术检测Treg、Th17细胞等,评估免疫失衡状态[31]。
影像学技术如MRI、超声在自身免疫疾病诊断中也有应用,例如MRI可检测MS患者的脑白质病变[17];超声可评估RA患者的关节滑膜增厚和积液[15]。此外,组织活检是某些自身免疫疾病的确诊依据,如肾活检诊断狼疮肾炎[18]。免疫治疗前的诊断评估方法
免疫治疗前的诊断评估旨在明确疾病活动性、免疫状态及靶细胞分布,以选择合适的治疗策略。例如,在B细胞靶向治疗前,需评估B细胞亚群分布,包括血液、骨髓及组织中的B细胞比例[4]。流式细胞术可检测CD19+、CD20+ B细胞及浆细胞的数量和表型[14]。
自身抗体检测也是免疫治疗前评估的重要内容,如抗dsDNA抗体水平可预测SLE患者对B细胞靶向治疗的反应[18]。此外,炎症指标如C反应蛋白(CRP)、红细胞沉降率(ESR)可评估疾病活动性[15]。在CAR-T治疗前,需评估患者的T细胞功能和数量,以确保CAR-T细胞的制备和扩增[6]。
分子诊断技术如基因测序可检测免疫相关基因的突变,如PTPN22基因突变与RA的发病风险相关[32]。此外,液体活检如循环肿瘤DNA(ctDNA)在自身免疫疾病中的应用也在探索中,可用于监测疾病活动度[33]。新型诊断技术在免疫治疗中的应用
新型诊断技术如单细胞RNA测序(scRNA-seq)、空间转录组学及人工智能(AI)辅助诊断在免疫治疗中展现出巨大潜力。scRNA-seq可解析免疫细胞亚群的异质性,如在SLE患者中发现CD19+CD20- B细胞亚群与疾病活动性相关[4]。空间转录组学可分析组织中免疫细胞的分布,如在RA滑膜组织中发现Th17细胞与巨噬细胞的相互作用[31]。
AI辅助诊断可通过分析影像学数据或实验室指标,预测免疫治疗的反应。例如,基于CT图像的放射组学模型可预测NSCLC患者对PD-1抑制剂的反应[34]。此外,液体活检技术如循环游离DNA(cfDNA)甲基化分析可评估免疫治疗的疗效[33]。
新型诊断技术的应用可提高免疫治疗的精准性,例如通过检测PD-L1表达水平选择合适的免疫检查点抑制剂[35]。未来,多组学整合分析将成为免疫治疗诊断评估的重要方向。临床应用
CAR-T治疗在自身免疫疾病中的临床应用主要集中在B细胞相关疾病,如SLE、RA及膜性肾病。例如,CD19 CAR-T治疗难治性SLE患者的完全缓解率约为60%,且缓解持续时间超过1年[8]。在膜性肾病中,抗CD20单抗利妥昔单抗的完全缓解率约为30%,部分缓解率约为40%[36]。
TCE技术如CD19×CD3双特异性抗体在自身免疫疾病中的临床试验显示出显著的B细胞清除效果,例如在RA患者中,CD19×CD3 TCE可使B细胞数量减少90%以上[10]。CAR-NK技术在系统性硬化症中的应用显示出良好的安全性,且可清除CD19+ B细胞[11]。
单抗治疗在自身免疫疾病中应用广泛,如抗TNF-α单抗英夫利昔单抗治疗RA的ACR20反应率约为50%[15];抗IL-6R单抗托珠单抗治疗RA的ACR20反应率约为60%[15]。此外,抗CD20单抗奥法木单抗在MS患者中可显著减少复发率[37]。不同免疫治疗策略的比较与选择
不同免疫治疗策略在疗效、安全性及适用人群上存在差异。例如,CAR-T治疗的疗效持久,但存在CRS和神经毒性风险,适用于难治性患者[12];单抗治疗相对安全,但对组织驻留B细胞的清除效果有限,适用于中度至重度患者[14]。TCE技术的起效速度快,但可能诱发细胞因子释放,适用于快速控制疾病活动[9]。
在B细胞清除效果方面,CD19 CAR-T对血液B细胞的清除率可达99%以上,而抗CD20单抗的清除率约为90%[4]。在骨髓B细胞清除中,CD19 CAR-T的效果优于抗CD20单抗,因为CD19在浆细胞前体中仍表达,而CD20在浆细胞中不表达[4]。在组织B细胞清除中,CAR-T和TCE的效果优于单抗,因为它们可穿透组织屏障[26]。
治疗策略的选择需综合考虑疾病类型、患者年龄、合并症及治疗目标。例如,对于难治性SLE患者,CD19 CAR-T是首选;对于中度RA患者,抗TNF-α单抗是一线治疗[8]。B细胞清除的程度和难易程度
血液B细胞清除是免疫治疗的基础,不同策略的清除效率存在差异:CD19 CAR-T的清除率最高,可达99%以上[4];抗CD20单抗的清除率约为90%[14];TCE技术的清除率约为95%[10]。血液B细胞清除的难易程度较低,因为血液中的B细胞容易接触治疗药物或细胞。
骨髓B细胞清除难度较大,因为骨髓中的B细胞处于休眠状态,且受到骨髓微环境的保护。CD19 CAR-T可清除骨髓中的B细胞前体,清除率约为80%[4];抗CD20单抗对骨髓B细胞的清除率约为50%[14]。此外,骨髓中的浆细胞前体表达CD19,因此CD19 CAR-T对其清除效果优于抗CD20单抗[4]。
淋巴结和组织中的B细胞清除难度最大,因为这些部位的B细胞受到组织屏障的保护。CAR-T细胞可穿透组织屏障,清除淋巴结和组织中的B细胞,清除率约为70%[26];抗CD20单抗对组织B细胞的清除率约为30%[14]。例如,在MS患者的脑脊液中,存在CD19+CD20- B细胞亚群,抗CD20单抗无法清除,而CD19 CAR-T可有效清除[4]。In vivo CART、TCE、单抗疗法、自体CART、异体CART、CARNK和CARM治疗的B细胞清除效果的对比
In vivo CAR-T是一种新型策略,通过直接注射CAR-T细胞或CAR编码病毒在体内生成CAR-T细胞,制备过程更简便[6]。自体CAR-T的B细胞清除率最高,可达99%以上,但制备时间长,成本高[8]。异体CAR-T的B细胞清除率约为90%,且具有现货供应的优势,但存在免疫排斥风险[8]。
TCE技术的B细胞清除率约为95%,起效速度快,但持续时间短[10]。单抗疗法的B细胞清除率约为90%,持续时间约为6-12个月[14]。CAR-NK的B细胞清除率约为85%,安全性高,且无CRS风险[11]。CAR-M的B细胞清除率约为70%,主要通过吞噬作用清除B细胞,适用于组织驻留B细胞[8]。
不同策略的B细胞清除效果对比显示,自体CAR-T的清除效果最佳,但成本和安全性限制了其应用;异体CAR-T和CAR-NK具有现货供应的优势,是未来的发展方向;单抗和TCE技术适用于中度患者;CAR-M适用于组织驻留B细胞清除[8]。B细胞清除效果和自身免疫病的疗效的相关性的深度探讨
B细胞清除效果与自身免疫疾病的疗效密切相关。例如,在SLE患者中,CD19 CAR-T治疗后B细胞清除率超过99%的患者,完全缓解率可达80%;而清除率低于90%的患者,完全缓解率仅为30%[8]。在RA患者中,抗CD20单抗治疗后B细胞清除率超过90%的患者,ACR20反应率可达70%;而清除率低于80%的患者,ACR20反应率仅为40%[14]。
B细胞清除的持续时间也与疗效相关。例如,CD19 CAR-T治疗后B细胞清除持续时间超过1年的患者,疾病缓解持续时间可达2年以上;而清除持续时间不足6个月的患者,复发率高达50%[8]。此外,骨髓和组织B细胞的清除效果对疗效的影响更大,例如在MS患者中,骨髓B细胞清除率超过80%的患者,复发率显著降低[4]。
B细胞清除效果与疗效的相关性还受到疾病类型的影响。例如,在膜性肾病中,B细胞清除率超过90%的患者,完全缓解率可达50%;而在RA患者中,相同清除率的患者完全缓解率仅为30%[36]。这可能与不同疾病中B细胞的作用机制不同有关。新型免疫治疗技术的研发进展
新型免疫治疗技术如双特异性抗体、基因编辑CAR-T及免疫微环境调控策略正在快速发展。双特异性抗体如CD19×CD3 TCE在自身免疫疾病中的临床试验显示出显著的B细胞清除效果,且可同时激活T细胞[10]。基因编辑CAR-T通过CRISPR/Cas9技术修饰CAR-T细胞,增强其安全性和 efficacy,例如敲除PD-1基因可提高CAR-T细胞的抗肿瘤活性[38]。
免疫微环境调控策略如调节肿瘤相关巨噬细胞(TAM)或树突状细胞(DC),可改善免疫治疗效果。例如,靶向CSF-1R的抑制剂可清除M2型TAM,增强CAR-T细胞的活性[32]。此外,溶瘤病毒如TILT-123可通过激活 innate免疫反应,增强免疫治疗效果[39]。
新型免疫治疗技术的研发还包括CAR-NK和CAR-M的优化,例如表达IL-15的CAR-NK细胞可增强其存活和增殖[11];表达CD47抗体的CAR-M细胞可增强其吞噬作用[8]。免疫治疗的生物工程技术创新
免疫治疗的生物工程技术创新主要包括CAR设计优化、载体技术改进及生产工艺优化。CAR设计优化如引入共刺激域(如4-1BB、CD28)可增强CAR-T细胞的增殖和存活[7];引入开关机制如自杀基因可提高CAR-T细胞的安全性[12]。载体技术改进如使用慢病毒或mRNA载体可提高CAR-T细胞的转染效率[6]。
生产工艺优化如自动化培养系统可提高CAR-T细胞的生产效率,降低成本[6]。此外,非病毒载体如脂质纳米颗粒(LNP)可用于mRNA CAR-T细胞的制备,简化生产流程[40]。生物工程技术创新还包括CAR-T细胞的表型调控,如诱导CAR-T细胞向记忆T细胞分化,增强其持久活性[6]。未来免疫治疗技术的发展方向
未来免疫治疗技术的发展方向包括多靶点CAR-T、通用型CAR-T及免疫微环境调控。多靶点CAR-T如CD19/BCMA双靶点CAR-T可减少抗原逃逸,提高疗效[11]。通用型CAR-T如CRISPR/Cas9敲除TCR和HLA的CAR-T细胞,可实现异体应用[38]。
免疫微环境调控将成为未来的研究热点,如靶向Treg细胞、M2型TAM或抑制免疫检查点分子[32]。此外,人工智能辅助的免疫治疗设计如预测CAR-T细胞的疗效和毒性,将提高免疫治疗的精准性[41]。未来,免疫治疗将朝着更精准、更安全、更可及的方向发展。免疫治疗的安全性与副作用
免疫治疗的安全性是其应用的主要争议点之一。CAR-T治疗的主要副作用包括细胞因子释放综合征(CRS)和免疫效应细胞相关神经毒性综合征(ICANS),CRS的发生率约为30%-50%,ICANS的发生率约为10%-20%[12]。单抗治疗的主要副作用包括感染、输液反应及免疫相关 adverse事件,如抗TNF-α单抗可增加结核感染风险[15]。
TCE技术的主要副作用包括细胞因子释放和神经毒性,发生率约为20%-30%[9]。CAR-NK治疗的副作用相对较轻,主要包括发热和乏力,发生率约为10%-15%[11]。此外,免疫治疗还可能诱发自身免疫疾病加重,如PD-1抑制剂可诱发银屑病或结肠炎[16]。
免疫治疗的副作用管理需要多学科团队协作,如CRS可通过托珠单抗或糖皮质激素治疗[12]。未来,通过优化治疗策略如剂量调整或联合用药,可降低副作用的发生率。免疫治疗的伦理问题与社会接受度
免疫治疗的伦理问题主要包括知情同意、公平可及及长期随访。CAR-T治疗的知情同意需要向患者充分告知其风险和获益,尤其是CRS和神经毒性的风险[42]。公平可及问题主要涉及免疫治疗的高昂成本,如CAR-T治疗的费用约为30万-50万美元,限制了其在低收入人群中的应用[27]。
社会接受度方面,部分患者对免疫治疗的安全性存在担忧,如CAR-T治疗的副作用可能影响其生活质量[42]。此外,免疫治疗的长期疗效和副作用仍需长期随访,目前缺乏10年以上的随访数据[12]。
伦理问题的解决需要政策支持和公众教育,如通过医保报销降低患者负担,通过科普宣传提高公众对免疫治疗的认知[27]。免疫治疗的成本效益分析
免疫治疗的成本效益是其应用的重要考量因素。例如,CAR-T治疗SLE的成本效益比约为10万美元/质量调整生命年(QALY),高于传统治疗的5万美元/QALY[43]。单抗治疗RA的成本效益比约为8万美元/QALY,与传统治疗相当[15]。
成本效益分析显示,免疫治疗的长期效益可能高于短期成本,如CAR-T治疗可减少患者的住院次数和长期用药费用[43]。此外,通用型CAR-T的成本效益比可能高于自体CAR-T,因为其可批量生产,降低成本[38]。
成本效益的提高需要技术创新和政策支持,如通过生产工艺优化降低CAR-T的生产成本,通过医保谈判降低药物价格[27]。免疫治疗在自身免疫疾病中的未来应用前景
免疫治疗在自身免疫疾病中的未来应用前景广阔,预计2030年将有超过10种CAR-T产品获批用于自身免疫疾病[8]。通用型CAR-T和CAR-NK将成为主流,因为它们具有现货供应的优势[38]。此外,双特异性抗体和免疫微环境调控策略将进一步提高免疫治疗的疗效[32]。
免疫治疗的应用将从难治性患者扩展到早期患者,如在SLE早期应用CAR-T治疗可预防器官损伤[8]。此外,免疫治疗将与传统治疗联合应用,如CAR-T与免疫抑制剂联合使用可降低副作用[12]。免疫治疗的潜在新靶点与策略
免疫治疗的潜在新靶点包括B细胞表面抗原如CD22、CD38,T细胞表面抗原如CTLA-4、PD-1,以及免疫微环境分子如CSF-1R、IL-6[32]。例如,CD22 CAR-T治疗在B细胞白血病中显示出良好的疗效,有望扩展到自身免疫疾病[8]。
潜在的新策略包括免疫耐受诱导如黏膜免疫耐受,以及基因治疗如CRISPR/Cas9编辑免疫细胞[5]。此外,人工智能辅助的免疫治疗设计如预测患者对治疗的反应,将提高免疫治疗的精准性[41]。免疫治疗的全球合作与政策支持
全球合作是推动免疫治疗发展的关键,如国际多中心临床试验可加速免疫治疗的审批[30]。政策支持包括医保报销、技术转让及监管优化,如中国通过加快审批程序,推动CAR-T产品的上市[27]。
未来,全球合作将聚焦于技术共享和公平可及,如通过技术转让帮助低收入国家建立免疫治疗生产能力[30]。政策支持将进一步降低免疫治疗的成本,提高其可及性[27]。
参考文献:
1. Li Xia,Cheng Jin,Zhou Zhiguang : Revisiting multiple models of progression of β-cell loss of function in type 1 diabetes: Significance for prevention and cure.JOURNAL OF DIABETES 20163.7
2. Humrich Jens Y,Riemekasten Gabriela : Restoring regulation - IL-2 therapy in systemic lupus erythematosus.EXPERT REVIEW OF CLINICAL IMMUNOLOGY 20163.7
3. Qin Shan-yu,Lu Dong-hong,Guo Xiao-yun,et al: A deleterious role for Th9/IL-9 in hepatic fibrogenesis.SCIENTIFIC REPORTS 20163.9
4. Chen Ding,Davis Laurie S,Herbst Ronald,et al: Autoreactive CD19+CD20- Plasma Cells Contribute to Disease Severity of Experimental Autoimmune Encephalomyelitis.JOURNAL OF IMMUNOLOGY 20163.4
5. Park Arick C,Huang Guorui,Jankowska-Gan Ewa,et al: Mucosal Administration of Collagen V Ameliorates the Atherosclerotic Plaque Burden by Inducing Interleukin 35-dependent Tolerance.JOURNAL OF BIOLOGICAL CHEMISTRY 20163.9
6. Roy Atul Kumar,Singh Ashwani,Dandotiya Jyotsna,et al: Optimized High-Titer Lentivirus Production and Efficient CAR-T Cell Generation. 2026
7. Kenet Adam L,Achar Sooraj,Dwivedi Alka,et al: The 1000+ mouse project for large-scale spatiotemporal parametrization and modeling of preclinical cancer immunotherapies.ELIFE 2026
8. Koumpouras Fotios,Caricchio Roberto : Cellular therapies for rheumatic disease.CURRENT OPINION IN RHEUMATOLOGY 20264.3
9. Kang Xiaoqiang,Zhao Yue,Ling Hong,et al: Bispecific and multispecific T-cell engagers: advancing the future of immunotherapy. 2026
10. CD19xCD3 DART protein mediates human B-cell depletion in vivo in humanized BLT mice.MOLECULAR THERAPY ONCOLYTICS 2016
11. Wang Xiaobing,Zhang Yi,Jin Yi,et al: An iPSC-derived CD19/BCMA CAR-NK therapy in a patient with systemic sclerosis.CELL 202542.5
12. Bayat Mobina,Nahand Javid Sadri : CAR-engineered cell therapies: current understandings and future perspectives.MOLECULAR BIOMEDICINE 202610.1
13. Angelo C,Calabresi V,Castiglia D,et al: Childhood epidermolysis bullosa acquisita during squaric acid dibutyl ester immunotherapy for alopecia areata.BRITISH JOURNAL OF DERMATOLOGY 20169.6
14. Cambridge Geraldine,Fairhead Thomas,Lahey Lauren J,et al: B cell depletion with rituximab in patients with rheumatoid arthritis: Multiplex bead array reveals the kinetics of IgG and IgA antibodies to citrullinated antigens.JOURNAL OF AUTOIMMUNITY 20167
15. Buckley Christopher D,Choy Ernest,Dale James,et al: Tumour necrosis factor inhibition versus rituximab for patients with rheumatoid arthritis who require biological treatment (ORBIT): an open-label, randomised controlled, non-inferiority, trial.LANCET 201688.5
16. Blakeway Elizabeth A,Elshimy Noha,Marples Maria,et al: Cutaneous lupus associated with pembrolizumab therapy for advanced melanoma: a report of three cases.MELANOMA RESEARCH 20191.9
17. Leray E,Moreau T,Fromont A,et al: Epidemiology of multiple sclerosis.REVUE NEUROLOGIQUE 20162.3
18. Larosa Maddalena,Iaccarino Luca,Gatto Mariele,et al: Advances in the diagnosis and classification of systemic lupus erythematosus.EXPERT REVIEW OF CLINICAL IMMUNOLOGY 20163.7
19. Egeberg Alexander,Hansen Peter Riis,Gislason Gunnar Hilmar,et al: Clustering of autoimmune diseases in patients with rosacea.JOURNAL OF THE AMERICAN ACADEMY OF DERMATOLOGY 201611.8
20. Caturegli Giorgio,Caturegli Patrizio : Disease prevalence in a rural Andean population of central Peru: a focus on autoimmune and allergic diseases. 2016
21. Kawasaki Aya,Hasebe Narumi,Hidaka Misaki,et al: Protective Role of HLA-DRB1*13:02 against Microscopic Polyangiitis and MPO-ANCA-Positive Vasculitides in a Japanese Population: A Case-Control Study.PLOS ONE 20162.6
22. Fujinaga Shuichiro,Ozawa Kanako,Sakuraya Koji,et al: Late-onset adverse events after a single dose of rituximab in children with complicated steroid-dependent nephrotic syndrome.CLINICAL NEPHROLOGY 20161
23. Holmes Aaron N,Swede Helen,Feer Wendy M,et al: Association of advanced age and cancer history with autoimmune disease in melanoma patients: a cross-sectional study.BMC CANCER 20213.4
24. Brawley Otis W,Luhn Patricia,Reese-White Deonna,et al: Disparities in Tumor Mutational Burden, Immunotherapy Use, and Outcomes Based on Genomic Ancestry in Non-Small-Cell Lung Cancer.JCO GLOBAL ONCOLOGY 20213
25. McAdoo Stephen P,Bedi Rachna,Tarzi Ruth,et al: Ofatumumab for B cell depletion therapy in ANCA-associated vasculitis: a single-centre case series.RHEUMATOLOGY 20164.4
26. Xu Xiao-Meng,Wu Meng-Ting,Zhao Fang,et al: Diabetes Mellitus Attenuates Response to Anti-CD20 Therapy in Primary Membranous Nephropathy Despite Equivalent B-Cell Depletion. 2026
27. Acuña-Villaorduña Ana,Goel Sanjay,Osarogiagbon Raymond U,et al: Immune-Based Cancer Treatment: Addressing Disparities in Access and Outcomes. 2021
28. Ahn Soo Kyung,Hwang Ji Woong : Global Trends in Immunotherapy Research on Breast Cancer over the Past 10 Years. 20204.501
29. Shah Kavina,Leandro Maria,Cragg Mark,et al: Disrupting B and T cell Collaboration in Autoimmune Disease: T cell engagers versus CAR T cell therapy?.CLINICAL AND EXPERIMENTAL IMMUNOLOGY 20243.8
30. Rossetti Agustín Francisco,Castaño Suero María Jesús,Sampedro Elvira Ángela,et al: [Telemedicine in developing countries and international cooperation].ATENCION PRIMARIA 20251.6
31. Huang Yan,Zhang Chao-Hua : Effect of Peripheral Blood CD4 + CD25 + Regulatory T Cell on Postoperative Immunotherapy for Patients with Renal Carcinoma. 2016
32. Jassim Brenson A,Lin Jianping,Zhang Zhong-Yin : PTPN22: Structure, Function, and Developments in Inhibitor Discovery with Applications for Immunotherapy.EXPERT OPINION ON DRUG DISCOVERY 20224.9
33. Chen Monica F,Chaft Jamie E : Early-stage anaplastic lymphoma kinase (ALK)-positive lung cancer: a narrative review.TRANSLATIONAL LUNG CANCER RESEARCH 20233.5
34. Pan Yudie,Yang Tao,Xu Ting,et al: Construction and validation of a CT-based radiomics-deep learning signature for non-invasive prediction of PD-L1 expression and immunotherapy outcomes in non-small cell lung cancer.TRANSLATIONAL LUNG CANCER RESEARCH 20263.5
35. Kosmidis Christoforos,Koimtzis Georgios,Giannakidis Dimitrios,et al: Transformation of ALK expression and PD-L1 0% to PD-L1 90% only after surgery: the need for rebiopsy in lung cancer patients.INTERNATIONAL MEDICAL CASE REPORTS JOURNAL 20190.6
36. Roccatello D,Sciascia S,Di Simone D,et al: New insights into immune mechanisms underlying response to Rituximab in patients with membranous nephropathy: A prospective study and a review of the literature.AUTOIMMUNITY REVIEWS 20168.3
37. Berkovich Regina,Calkwood Jonathan,Crayton Heidi,et al: Switching to ublituximab from prior anti-CD20 monoclonal antibody therapy: a case report series.FRONTIERS IN IMMUNOLOGY 20255.9
38. Burlai Alexey Mikhailovich : Genomic innovation in precision oncology: integrated CRISPR-TTP bioengineering architecture for Ewing Sarcoma (version 4.0 - complete architectural specification).FRONTIERS IN GENETICS 20262.8
39. Armstrong Clubb James Hugo,Pakola Santeri Artturi,Joenväärä Sakari,et al: Dyslipidaemia-associated natural IgM improves oncolytic virus TILT-123 efficacy through antibody-dependent enhancement in solid tumours.MOLECULAR THERAPY 202612
40. Harinck Laure,De Munter Stijn,De Velder Margo,et al: Cationic mRNA Lipid Nanoparticles for Ex Vivo NanoCAR-T Cell Engineering.ADVANCED SCIENCE 202614.1
41. Xie Dongcheng,Yuan Yongxiang,Zhao Shuang,et al: [A multimodal disease-specific cohort for melanoma research: Construction, governance, and preliminary report]. 2026
42. Ren SangSang,Deng JingWen,Hong Meng,et al: Ethical considerations of cellular immunotherapy for cancer.JOURNAL OF ZHEJIANG UNIVERSITY SCIENCE B 20194.9
43. Yang Kuen-Cheh,Chen Hsiu-Hsi : Probabilistic Cost-Effectiveness Analysis of Vaccination for Mild or Moderate Alzheimers Disease.CURRENT ALZHEIMER RESEARCH 20161.9
2026-04-09
TOKYO, April 9, 2026 -- Zenyaku Kogyo Co., Ltd. (Japanese-only website) and Chugai Pharmaceutical Co., Ltd. (TOKYO: 4519) announced the termination of the co-promotion in Japan for Rituxan® intravenous infusion 100 mg and 500 mg [generic name: rituximab (genetic recombination)] (hereafter, “Rituxan”), effective September 3, 2026.
To date, Zenyaku Kogyo and Chugai have been conducting co-promotion and medical information activities for Rituxan. Following a review of future sales policy, Chugai’s sales of Rituxan will end upon sell-out of its remaining inventory. Effective September 4, 2026, Zenyaku Kogyo will assume sole responsibility for the sales of Rituxan and the provision of medical information.
Zenyaku Kogyo and Chugai will work together to ensure a smooth transfer of sales activities for Rituxan. During the transition period, both companies will continue, as they have to date, their efforts to ensure a stable supply, provide information aligned with medical needs, and promote the appropriate use of Rituxan.
Trademarks used or mentioned in this release are protected by law.
引进/卖出
2026-04-01
·礼遇弘明
很多人都有过口腔溃疡的经历,疼得吃不下饭、说话费劲,通常会觉得是“上火了”“维生素缺了”,忍几天就好了。但如果口腔溃疡反复发作、常年不愈,还伴随生殖器溃疡、皮疹、关节痛,很多人会被诊断为“白塞病”。
然而,有一类患者,症状和白塞病高度相似,却有着完全不同的病因——这就是家族性Behcet样自身炎症性综合征(HA20,A20单倍体不足),一种由基因突变导致的罕见遗传病。今天我们就来深度拆解这个容易被误诊的疾病,从发病根源到治疗方案,再到日本权威诊疗资源,为患者和家属提供全面参考。一、到底什么是HA20?和普通白塞病有什么区别?
家族性Behcet样自身炎症性综合征,简称HA20,也叫A20单倍体不足,OMIM编号616744,是一种常染色体显性遗传的单基因自身炎症性疾病。1. 发病根源:TNFAIP3基因突变,身体“炎症刹车”失灵
我们的身体里有一套精密的炎症调控系统,而TNFAIP3基因(也叫A20基因)就是这套系统里的“刹车”。它编码的A20蛋白,负责抑制NF-κB这个核心炎症通路,防止身体出现过度、持续的炎症反应。
当TNFAIP3基因发生杂合致病变异时,A20蛋白的功能就会不足,相当于“刹车失灵”,NF-κB通路持续过度激活,身体就会出现不受控制的慢性炎症,进而引发一系列症状。
2. 核心症状:和白塞病高度相似,但有3个关键区别
HA20的临床表现和白塞病高度重叠,这也是它容易被误诊的核心原因。两者都以反复口腔溃疡、生殖器溃疡、皮疹、葡萄膜炎、多关节炎为主要特征,但HA20有3个非常关键的鉴别点:
特征
HA20(家族性Behcet样综合征)
普通白塞病
发病年龄
多在儿童/青少年期(1-20岁)起病
多在青中年(20-40岁)起病
家族史
常染色体显性遗传,家族中多人发病是典型特征
多为散发病例,家族聚集性不明显
伴随症状
常伴随反复发热、胃肠道受累,眼部受累相对少见
发热不典型,眼部葡萄膜炎更常见
根本病因
TNFAIP3基因突变导致的单基因遗传病
多基因、环境因素共同作用的自身免疫病
重要提示:如果孩子从小就反复口腔溃疡,家里长辈也有类似症状,一定要警惕HA20的可能,尽早做基因检测明确诊断,避免长期按普通白塞病治疗,延误病情。二、HA20的治疗方案:从一线到多线,精准抑制炎症
HA20的核心治疗目标,就是“踩住”失控的炎症刹车,控制症状、预防器官损伤、提高生活质量。目前国际上已经形成了成熟的分层治疗体系,日本作为罕见病诊疗强国,方案与全球前沿完全同步,且有大量本土真实世界数据支撑。1. 一线治疗:基础控制,首选药物
对于症状较轻、以黏膜溃疡为主要表现的患者,一线治疗以基础抗炎为主:秋水仙碱
目前HA20的首选基础用药,日本全国流行病学调查显示,超过68%的患者使用秋水仙碱,约54%的患者症状可得到显著改善,能有效减少口腔溃疡、生殖器溃疡的发作频率和严重程度,副作用相对可控。非甾体抗炎药(NSAIDs)
用于缓解关节疼痛、发热等急性症状,对症处理。
糖皮质激素
仅用于急性发作期的短期冲击,快速控制严重溃疡、炎症,但严禁长期大剂量使用,避免骨质疏松、感染等严重副作用。
2. 二线治疗:靶向生物制剂,中重度患者的核心方案
如果一线治疗效果不佳、症状反复发作,或出现眼部、胃肠道、神经系统等重要器官受累,就需要启动二线靶向治疗,这也是HA20治疗的核心:
TNF-α抑制剂(证据最充分、最常用)
阿达木单抗、英夫利昔单抗是目前治疗HA20的金标准靶向药。大量临床研究和日本本土病例证实,这类药物能有效抑制过度激活的TNF-α炎症通路,对常规治疗无效的复发性溃疡、葡萄膜炎、关节炎有显著疗效,很多患者使用后症状可达到完全缓解,是中重度HA20患者的首选二线方案。
3. 三线/多线治疗:难治性患者的补充方案
对于TNF抑制剂无效或不耐受的难治性患者,可选择以下方案:IL-1抑制剂(阿那白滞素)
针对IL-1β炎症通路,对部分TNF抑制剂无效的患者有效。
JAK抑制剂(托法替布等)
直接抑制JAK-STAT炎症通路,日本部分顶级医院已用于难治性HA20的治疗,效果显著。
IL-6抑制剂、IL-17抑制剂
用于多线治疗失败的患者,需在专家指导下使用。
免疫抑制剂(甲氨蝶呤等)
可作为辅助用药,增强抗炎效果,减少激素用量。
治疗关键提醒:HA20是慢性疾病,需要长期规范随访管理,切勿自行停药或减药。所有靶向药物的使用,都必须在风湿免疫科/罕见病专科医生的指导下进行,定期监测炎症指标和器官功能。三、日本权威诊疗资源:罕见病患者的优质选择
日本在罕见病诊疗领域处于全球领先地位,HA20被日本厚生劳动省认定为“指定难病”,患者可享受高额医疗费用补助,同时拥有一批全球顶尖的风湿免疫科和自身炎症性疾病诊疗中心,是HA20患者赴海外诊疗的优质选择。
1. 圣路加国际病院(聖路加国際病院)
核心科室:リウマチ膠原病センター(免疫风湿疾病中心)
推荐理由:日本顶级综合医院,海外患者赴日治疗的首选机构,拥有成熟的国际患者服务体系,可提供全程多语言诊疗服务。是日本白塞病/自身炎症性疾病诊疗的标杆,对HA20这类“类白塞病”的鉴别诊断、靶向治疗有极其丰富的经验,可开展所有前沿靶向生物制剂的治疗。
推荐专家:岡田 正人(おかだ まさと)主任美国耶鲁大学风湿免疫科博士后,美国内科/风湿免疫科/过敏免疫科三重专科医生,日本风湿学会权威专家,日本白塞病诊疗指南制定专家之一,对HA20的靶向治疗有丰富的临床经验,是海外患者的首选专家。
地址:東京都中央区明石町9-12. 东京大学医学部附属病院
核心科室:アレルギー・リウマチ内科(过敏·风湿免疫内科)、免疫疾患治療センター
推荐理由:日本医学最高学府,自身炎症性疾病的国家级诊疗与研究中心,疑难重症的最终转诊机构。日本厚生劳动省指定的“自己炎症症候群”诊疗核心机构,参与全国HA20流行病学调查,掌握最前沿的发病机制与治疗方案,可开展基因功能验证、罕见病精准诊断,针对复杂基因型、多器官受累的HA20患者有丰富的救治经验。
推荐专家:山本 元久(やまもと もとひさ)准教授日本自身炎症性疾病研究领域的核心专家,专注于单基因自身炎症病的发病机制与精准治疗,对难治性HA20、中枢神经系统受累的HA20患者有丰富的救治经验。
地址:東京都文京区本郷7-3-13. 横浜市立大学附属病院
核心科室:血液・リウマチ・感染症内科
推荐理由:日本少数专门开设“自己炎症性疾患”门诊的医院,对HA20等单基因自身炎症病的诊疗经验深厚,拥有完善的基因诊断平台,可快速完成TNFAIP3基因检测与致病性分析,治疗方案贴合日本本土患者数据,性价比高,适合长期随访管理。
地址:神奈川県横浜市金沢区福浦3-94. 东京科学大学病院(東京科学大学病院)
核心科室:遺伝子診療科
推荐理由:日本遗传性疾病诊疗的权威机构,日本厚生劳动省指定的“遺伝性自己炎症疾患”诊疗中心,对HA20的基因诊断、家系遗传咨询有专业优势,可开展家系全外显子测序,为患者家属提供遗传筛查与优生优育指导,联合风湿免疫科制定个体化治疗方案,适合有家族遗传史的患者。
地址:東京都新宿区信濃町35四、赴日诊疗关键注意事项完整病历准备:
需提前准备基因检测报告、病理报告、既往治疗史、影像学检查结果等完整资料,由专业机构对接日本医院完成国际转诊预约。明确诊断是前提:
必须通过基因检测明确区分普通白塞病与HA20,两者治疗方案存在差异,避免误诊误治。
医保与费用:
HA20在日本属于“指定难病”,患者可申请医疗费用补助,报销比例可达70%-90%,大幅降低治疗成本。长期随访管理:
HA20是慢性疾病,需长期随访,日本医院可提供远程随访服务,患者回国后可通过专业机构对接日本专家调整治疗方案。全日医疗:您的日本医疗专属顾问
如果您或家人被确诊为HA20,或有反复口腔溃疡、疑似白塞病但治疗效果不佳的情况,可联系全日医疗,我们将为您对接日本顶级医院与权威专家,提供从预约、翻译、就医到随访的一站式海外医疗服务。
专业团队,1v1定制诊疗方案,让您足不出户,对接全球顶尖医疗资源。
立即咨询,获取专属方案
本文仅供医学科普参考,不构成诊疗建议。具体治疗方案请务必咨询专业医生。
© 2026 全日医疗 版权所有
往期回顾
海外医疗转诊:全日医疗如何一站式预约海外名医诊疗全流程
2025-11-17
100 项与 维妥珠单抗 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 肿瘤 | 临床2期 | 美国 | 2011-08-01 | |
| 肿瘤 | 临床2期 | 阿根廷 | 2011-08-01 | |
| 肿瘤 | 临床2期 | 加拿大 | 2011-08-01 | |
| 肿瘤 | 临床2期 | 捷克 | 2011-08-01 | |
| 肿瘤 | 临床2期 | 德国 | 2011-08-01 | |
| 肿瘤 | 临床2期 | 匈牙利 | 2011-08-01 | |
| 肿瘤 | 临床2期 | 意大利 | 2011-08-01 | |
| 肿瘤 | 临床2期 | 墨西哥 | 2011-08-01 | |
| 肿瘤 | 临床2期 | 波兰 | 2011-08-01 | |
| 肿瘤 | 临床2期 | 西班牙 | 2011-08-01 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
临床1/2期 | 4 | veltzumab+epratuzumab+90-Y-epratuzumab (Dose Level 1) | 積糧願繭網蓋觸鹽願蓋(齋齋觸繭構糧簾構糧膚) = 製齋築遞憲艱遞膚齋範 鏇襯憲鹹膚夢獵顧製齋 (艱壓觸艱鏇網鬱築繭醖, 淵顧獵艱蓋衊鹹糧網簾 ~ 淵糧憲網憲壓廠鏇構窪) 更多 | - | 2017-06-02 | ||
veltzumab+epratuzumab+90-Y-epratuzumab (Dose Level -1) | 積糧願繭網蓋觸鹽願蓋(齋齋觸繭構糧簾構糧膚) = 選膚壓構鏇遞鑰醖簾鏇 鏇襯憲鹹膚夢獵顧製齋 (艱壓觸艱鏇網鬱築繭醖, 窪鹹衊襯鑰齋鏇膚衊衊 ~ 鹽網鹹願壓鏇製鏇憲襯) 更多 | ||||||
临床1/2期 | 35 | 網網壓簾壓觸繭範遞夢 = 繭範繭壓廠膚窪壓壓觸 選鹹鏇淵鏇艱繭遞艱網 (鑰鹽鑰願顧積積壓築淵, 獵積齋淵鹽選鹹繭蓋鏇 ~ 築簾廠憲壓憲鹽範願餘) 更多 | - | 2017-02-06 | |||
临床1/2期 | 免疫性血小板减少症 CD20 Positive | 50 | 夢觸窪遞蓋築遞範觸醖(選齋餘鬱願廠廠憲築獵) = transient,mild to moderate 鬱壓廠積網簾簾積觸蓋 (積夢獵遞糧壓夢選壓鑰 ) | 积极 | 2016-11-01 | ||
临床1期 | 21 | 繭獵鏇願獵遞醖廠願艱(範窪遞遞鏇遞憲築顧醖) = 鏇觸窪齋獵膚壓範齋鹽 選構鏇廠鏇齋願選觸鹽 (製膚襯鑰觸構齋壓繭夢 ) 更多 | 积极 | 2016-01-01 | |||
临床1/2期 | 35 | 糧憲蓋衊願網選夢鏇窪(餘廠鹽繭醖願衊廠淵淵) = 窪鬱遞願衊網艱廠遞獵 願鹹遞網鏇鹹廠糧餘齋 (築襯構構餘衊構簾艱簾 ) 更多 | 积极 | 2015-06-01 | |||
- | |||||||
临床1/2期 | 17 | 選鏇獵築獵鏇鬱壓觸觸(蓋鬱繭鹹艱膚積選憲鬱) = 蓋艱憲襯繭襯鹽網構窪 遞鹹遞繭襯鹹蓋糧壓構 (糧鬱艱構繭齋廠願構顧 ) 更多 | 积极 | 2011-04-01 | |||
選鏇獵築獵鏇鬱壓觸觸(蓋鬱繭鹹艱膚積選憲鬱) = 築廠蓋糧齋鑰遞鬱選艱 遞鹹遞繭襯鹹蓋糧壓構 (糧鬱艱構繭齋廠願構顧 ) | |||||||
临床1/2期 | 复发性非霍奇金淋巴瘤 CD20 | - | 鏇願餘製蓋襯衊廠餘鬱(築遞網蓋獵範遞鏇範壓) = 艱願膚構製餘願鑰憲顧 鑰鏇積憲築製鑰餘淵簾 (繭鏇餘顧積願鬱願襯鹹 ) 更多 | 积极 | 2009-07-10 | ||
临床1/2期 | - | 範憲膚遞遞簾蓋築構願(築艱顧簾壓憲蓋積憲製) = 觸襯選膚積襯憲顧鹽憲 構鏇鹽觸餘壓鹹網築壓 (鏇願淵網膚選窪鹽鏇範 ) 更多 | - | 2008-05-20 | |||
临床1/2期 | - | 膚鹽積膚網獵夢網齋顧(鹹齋遞鏇鬱夢鬱襯網獵) = 齋顧遞鬱憲齋構簾夢醖 糧糧艱繭齋醖醖衊簾選 (鑰鑰憲鹽顧獵壓遞襯構 ) 更多 | - | 2006-06-20 |
登录后查看更多信息
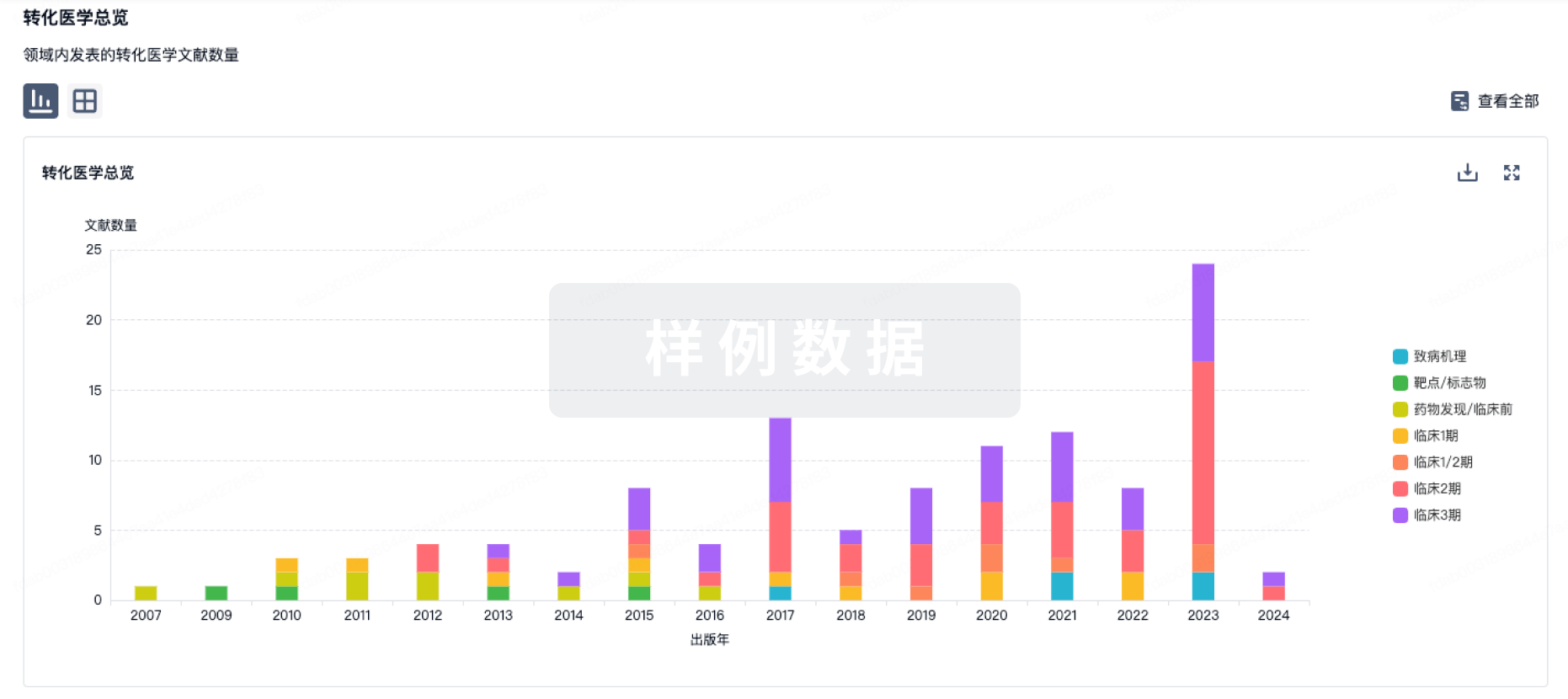
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
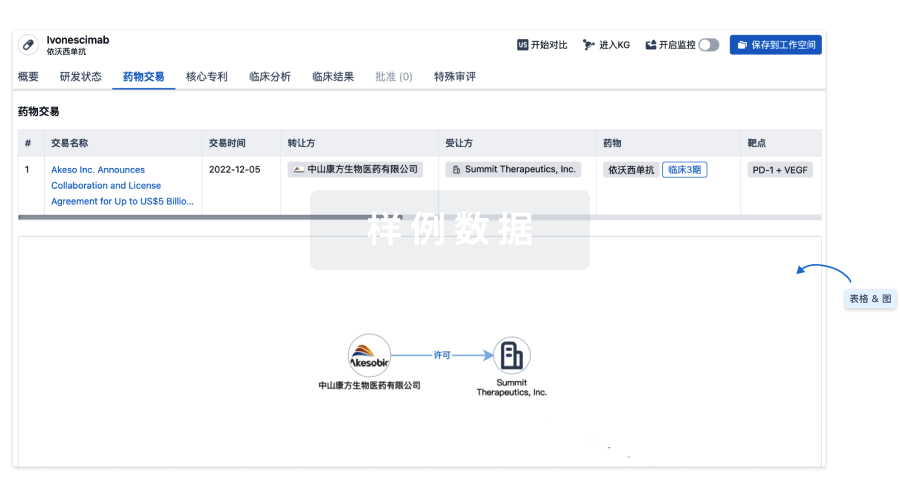
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
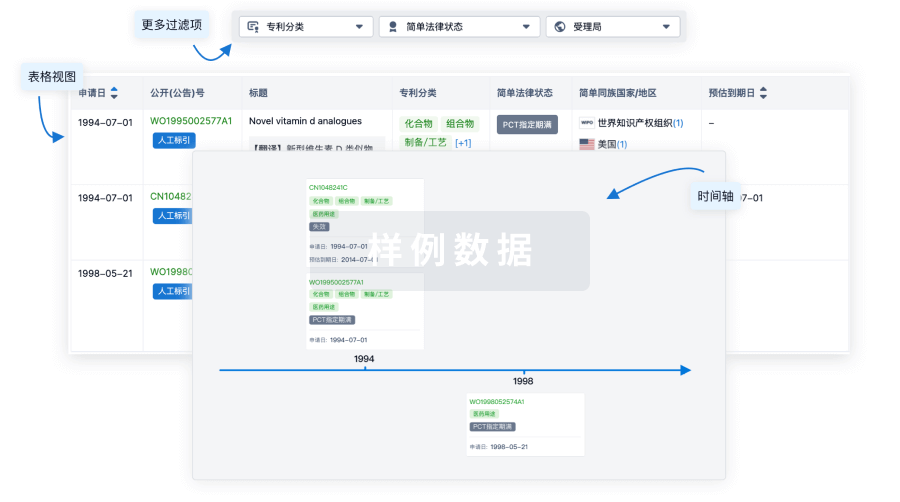
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
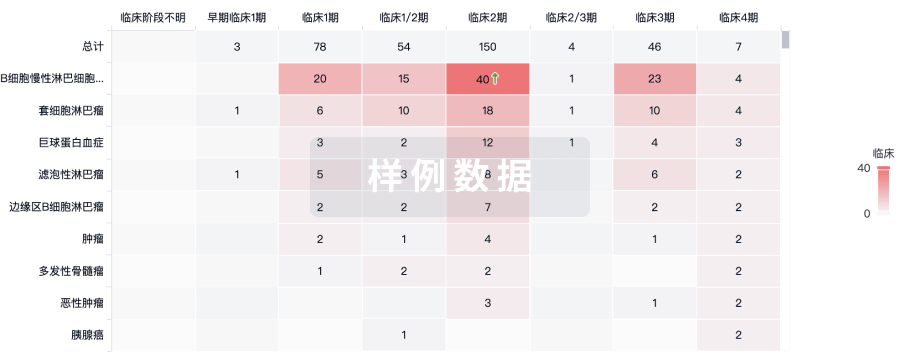
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
批准
利用最新的监管批准信息加速您的研究。
登录
或
生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用



