预约演示
更新于:2026-04-21
Molgramostim
更新于:2026-04-21
概要
基本信息
在研机构 |
权益机构- |
最高研发阶段申请上市 |
首次获批日期 瑞典 (1991-11-08), |
最高研发阶段(中国)- |
特殊审评孤儿药 (美国) |
登录后查看时间轴
结构/序列
Sequence Code 1191632844

来源: *****
关联
12
项与 Molgramostim 相关的临床试验CTIS2024-520317-49-00
Intraperitoneal treatment with fosfomycin, metronidazole and recombinant human granulocyte-macrophage colony-stimulating factor in patients with multi-quadrant peritonitis undergoing abdominal surgery: A randomized placebo-controlled trial (TRIPLE)
开始日期2025-04-01 |
申办/合作机构 |
NCT05501340
Phase I-II Clinical Study of PRaG(PD-1 Inhibitor Intravenous Injectio,Radiotherapy and GM-CSF)Combined With PD-1 Inhibitor Intraperitoneal Perfusion for Advanced Refractory Solid Tumors Combined With Malignant Ascites
The effect and safety of intraperitoneal infusion of PD-1 inhibitor is unclear for patients with peritoneal metastasis of advanced malignant tumors and malignant ascites. It is planned to determine the safety and efficacy of intraperitoneal infusion of PD-1 inhibitor combination with PRaG therapy.
开始日期2022-09-01 |
申办/合作机构 |
NCT04979832
A Combined Treatment With GM-CSF, Fosfomycin and Metronidazole for Pouchitis in Ulcerative Colitis Patients After Restorative Ileal Pouch Anal Anastomosis Surgery
This study will examine whether the application of GM-CSF, fosfomycin and metronidazole locally in the pouch is safe and effective in the treatment of pouchitis for patients with ulcerative colitis, and whether treatment changes the microbiome of the pouch.
开始日期2021-09-06 |
申办/合作机构 |
100 项与 Molgramostim 相关的临床结果
登录后查看更多信息
100 项与 Molgramostim 相关的转化医学
登录后查看更多信息
100 项与 Molgramostim 相关的专利(医药)
登录后查看更多信息
65
项与 Molgramostim 相关的文献(医药)2025-10-01·DRUGS
Pharmacotherapy for Autoimmune Pulmonary Alveolar Proteinosis
Review
作者: Lederlin, Mathieu ; Chauvin, Pierre ; Jouneau, Stéphane ; Kerjouan, Mallorie ; Painvin, Benoît
Pulmonary alveolar proteinosis is suspected when a "crazy paving" pattern is observed on a chest CT scan. This diagnosis is confirmed by the presence of eosinophilic extracellular material that shows positive staining with Periodic Acid Schiff on bronchoalveolar lavage samples. The autoimmune form of pulmonary alveolar proteinosis is confirmed by detecting anti-granulocyte-macrophage colony-stimulating factor antibodies in the patient's serum. The historical first-line treatment for autoimmune pulmonary alveolar proteinosis is whole lung lavage, which should only be performed in expert centers. It remains the preferred treatment for patients experiencing respiratory failure, especially at the time of diagnosis. Inhaled granulocyte-macrophage colony-stimulating factor supplementation with molgramostim or sargramostim is now considered a first-line treatment in the international guidelines for autoimmune pulmonary alveolar proteinosis, following the positive results of recent randomized placebo-controlled studies. Rituximab and plasmapheresis can be prescribed as third- and fourth-line treatments, respectively. Lung transplantation may be considered for eligible patients experiencing terminal respiratory failure. A deeper understanding of the pathogenesis of autoimmune pulmonary alveolar proteinosis has opened up new therapeutic avenues, such as the use of PPARγ agonists or statins.
2025-09-22·Immunotherapy
Recombinant GM-CSF drug evaluation review
Review
作者: McCarthy, Jack ; McCarthy, Cormac ; Boyle, Niamh
Autoimmune Pulmonary Alveolar Proteinosis (aPAP) is a rare disease characterized by myeloid cell dysfunction, abnormal pulmonary surfactant accumulation, and innate immune deficiency. Pathogenesis is driven by GM-CSF neutralizing autoantibodies (GMAbs) present in high titer in serum and bronchoalveolar lavage fluid (BALF) of patients. GM-CSF is a cytokine and a hematopoietic growth factor produced by a variety of cells. In the lungs, GM-CSF regulates surfactant homeostasis and lung host defense through innate immune function. Whole lung lavage (WLL) is the current first line therapy for aPAP. It is a procedure in which excessive surfactant is mechanically removed from the alveoli. Pathogenesis-driven treatment with GM-CSF augmentation has been investigated over the last two decades with recombinant GM-CSF (rGM-CSF). Molgramostim and sargramostim are rGM-CSF which can be self-administered at home by patients with aPAP either subcutaneously or using a handheld nebulizer. In Phase II and III studies of adults with aPAP, daily administration of inhaled molgramostim resulted in greater improvements in pulmonary gas transfer and functional health status than placebo, with similar rates of adverse events. In all clinical studies to date, rGM-CSF has shown a favorable safety profile with no dose limiting toxicity. This supports the application of inhaled rGM-CSF for the treatment of aPAP and the possibility of WLL as a rescue therapy.
2025-09-01·BMJ Open Respiratory Research
Pharmacokinetics and pharmacodynamics of inhaled molgramostim in healthy people
Article
作者: Trapnell, Bruce C ; Robinson, Brian R ; Carey, Brenna C
Background:
Inhaled molgramostim, a form of recombinant human granulocyte–macrophage colony stimulating factor (GM-CSF), is a promising investigational pharmacotherapy for autoimmune pulmonary alveolar proteinosis (aPAP); however, its pharmacology in healthy subjects has not been reported.
Methods:
This randomised, double-blind, placebo-controlled, single-centre, phase 1 clinical trial assessed the safety, tolerability, pharmacokinetics and pharmacodynamics of inhaled molgramostim in healthy adults in single ascending dose (SAD) and multiple ascending dose (MAD) studies: one 150, 300 or 600 µg administration or six consecutive daily 300 or 600 µg administrations with evaluations over 28 or 34 days, respectively. The primary endpoint was safety, which was evaluated based on the number and severity of treatment-emergent AEs following single and multiple inhaled doses of molgramostim.
Results:
42 subjects were enrolled including 18 in the SAD study and 24 in the MAD study; all completed the study. Inhaled molgramostim in healthy people was well tolerated and no dose-limiting safety concerns or anti-drug antibody formation were observed in either study. GM-CSF was measurable in serum 30 min after administration of inhaled molgramostim, peaked at 2 hours for all three doses and had an elimination half-life of 1.7±0.0 to 5.9±0.9 hours in the SAD and MAD studies. Systemic GM-CSF exposure was non-linear in both the SAD and MAD studies. Inhaled molgramostim caused a rapid increase in white blood cells (WBC) counts and leucocyte subsets that normalised by 8 hours (SAD) or 15–21 days (MAD). Fractional exhaled nitric oxide remained within the normal range at all doses but was numerically, but not significantly, increased at the 600 μg dose.
Conclusions:
In healthy people, inhaled molgramostim was well-tolerated and resulted in systemic exposure at picogram levels, which had the expected PD effects on blood leucocyte levels that mostly remained within normal ranges.
Trial registration number:
NCT02468908
; EudraCT No. 2013-001687-32
33
项与 Molgramostim 相关的新闻(医药)2026-04-20
LANGHORNE, Pa.--(BUSINESS WIRE)--
Savara Inc.
(Nasdaq: SVRA), a clinical stage biopharmaceutical company focused on rare respiratory diseases, today announced the grant of inducement awards to new employees.
On April 14, 2026, the Compensation Committee of Savara's Board of Directors granted the inducement awards to 24 new employees who recently joined the Company. The inducement awards consist of options to purchase 18,500 shares of the Company’s common stock, restricted stock units (RSUs) covering 141,000 shares of the Company’s common stock, and performance stock units (PSUs) covering 85,000 shares of the Company’s common stock. These equity awards were granted under the Savara Inc. 2021 Inducement Equity Incentive Plan pursuant to Rule 5635(c)(4) of the NASDAQ Listing Rules as an inducement material to the employees’ acceptance of employment with the Company.
The options have an exercise price of $6.07 per share, the closing trading price of the Company's common stock on the NASDAQ Global Market on the grant date. Each option has a 10-year term and vests as to 1/16
th
of the number of shares subject to the option on each quarterly anniversary of the employee’s first day of employment, subject to the employee’s continued employment on each such vesting date. The RSUs vest in full on the two-year anniversary of the employee’s first day of employment, and PSUs vest in full upon the date the Company reports quarterly revenue above a specified target, in each case subject to the employee’s continued employment on such vesting date.
About Savara
Savara is a clinical stage biopharmaceutical company focused on rare respiratory diseases. Our lead program, MOLBREEVI*, is a recombinant human granulocyte-macrophage colony-stimulating factor (GM-CSF) in Phase 3 development for autoimmune pulmonary alveolar proteinosis (autoimmune PAP). MOLBREEVI is delivered via a proprietary investigational eFlow
®
Nebulizer System (PARI Pharma GmbH) specifically developed for inhalation of MOLBREEVI. Our management team has significant experience in rare respiratory diseases and pulmonary medicine, identifying unmet needs, and effectively advancing product candidates to approval and commercialization. More information can be found at
, and
LinkedIn
.
*MOLBREEVI is the FDA and EMA conditionally accepted trade name for molgramostim inhalation solution. It is not approved in any indication. MOLBREEVI is a trademark of Savara Inc.
Contacts
Media and Investor Relations Contact
Savara Inc.
Temre Johnson, Executive Director, Corporate Affairs
ir@savarapharma.com
临床3期临床结果
2026-04-16
·罕萌诊所
【监管进展】多款难治性血液瘤靶向药临床申请获受理
2026年4月15日,国家药品监督管理局(NMPA)正式受理靶向LILRB4/CD3的T细胞接合器(TCE)双抗创新药临床试验申请,拟用于治疗急性髓系白血病(AML)、慢性粒单核细胞白血病(CMML)及多发性骨髓瘤(MM)。这些血液系统恶性肿瘤具有高异质性或极高复发风险,尤其是AML和CMML领域目前尚无TCE类药物获批,临床需求迫切。该药物为全球首款申报临床的靶向LILRB4/CD3双抗,确保强效杀伤活性的同时大幅提升了安全性。此次申请获受理标志着血液瘤精准免疫治疗取得重要进展,有望为缺乏有效治疗手段的患者带来全新突破。
信息来源:迈威生物公司
【监管进展】FDA延长自身免疫性肺泡蛋白沉积症吸入药物审评周期
2026年4月15日,美国食品药品监督管理局(FDA)决定将molgramostim吸入溶液的生物制剂许可申请审评周期延长三个月。该药拟用于治疗自身免疫性肺泡蛋白沉积症,FDA目前正以优先审评方式对该申请进行审查,新的《处方药使用者付费法案》(PDUFA)目标行动日期定为2026年11月22日。此次延长系因FDA认定申办方对近期信息请求的答复构成重大修订,故依法将审评期顺延三个月,并未在相关函件中提及任何安全性、有效性或生产方面的具体问题。
信息来源:Business Wire / Las Vegas Sun
【行业动态】爱尔兰将两种罕见病纳入新生儿足跟血筛查
2026年4月15日,爱尔兰卫生部门宣布,将重症联合免疫缺陷(SCID)和脊髓性肌萎缩症(SMA)纳入国家新生儿足跟血筛查计划。SCID是一种罕见的原发性免疫缺陷病,患儿若未及时接受治疗,多在1岁内因严重感染死亡;SMA是一种遗传性神经肌肉疾病,可导致进行性肌无力和呼吸衰竭。将这两种疾病纳入筛查范围有助于实现早诊早治,显著改善患儿预后。此前,SCID和SMA已被多个国家和地区纳入新生儿筛查项目。
信息来源:Cork Independent
【患者支持】全国首个腱鞘巨细胞瘤患者支持项目在京收官
近日,全国首个腱鞘巨细胞瘤(TGCT)患者支持项目“微光计划”在京收官。该项目旨在通过汇集真实诊疗经历,构建“TGCT患者经验库”,填补公共信息空白。TGCT是一种起源于滑膜、滑囊或腱鞘的罕见肿瘤,多发于20至50岁青壮年,虽多为良性但具有局部侵袭性和高复发率。截至2026年2月底,项目已收集到来自21个城市的32位患者分享,涵盖多个年龄段,患者的真实经历将被用于公众科普、患者支持与政策倡导。
信息来源:央广网
本期内容由【大连医科大学公共卫生学院】袁妮老师团队&【辽宁省基础医学研究所】邵尉老师联合供稿。重要提示:
·本文所载信息仅为科研及行业动态分享,不应视为医疗建议或投资指导。
·本平台所整理发布的罕见病领域每日速览信息,均来源于公开网络渠道。如涉侵权,请及时联系我们核查并处理。
点分享
点收藏
点在看
点点赞
2026-04-16
The FDA has extended its review of Savara's Molbreevi (molgramostim) for autoimmune pulmonary alveolar proteinosis (aPAP) by three months to November 22, seeking additional time to assess newly submitted materials by the company.The PDUFA extension was triggered after the FDA determined that Savara's responses to recent information requests constituted a major amendment to Molbreevi's marketing application. The biotech, however, noted the agency did not raise any safety, efficacy or manufacturing concerns with the investigational therapy in its correspondence.The latest development marks yet another setback in a protracted regulatory journey for the inhaled recombinant human granulocyte-macrophage colony-stimulating factor (GM-CSF). In early 2025, the FDA refused to file the original application, citing insufficient chemistry, manufacturing and controls (CMC) data — though no safety or efficacy concerns were highlighted at that time as well. Savara subsequently resubmitted its application late last year following remediation of the CMC deficiencies.Meanwhile, Molbreevi's clinical development trajectory has been equally turbulent. In 2019, the therapy fell short in the Phase III IMPALA trial in aPAP, failing to improve the alveolar-arterial oxygen gradient versus placebo. The therapy, however, redeemed itself four years later by meeting the primary endpoint in the pivotal IMPALA-2 study — though the readout drew a muted investor response.Molbreevi also remains under regulatory review in the EU for aPAP. Jefferies analysts earlier projected the drug — gained through Savara's acquisition of Serendex Pharmaceuticals — could surpass $400 million in peak US sales.
临床3期并购加速审批
100 项与 Molgramostim 相关的药物交易
登录后查看更多信息
外链
| KEGG | Wiki | ATC | Drug Bank |
|---|---|---|---|
| D05066 | Molgramostim |
研发状态
批准上市
10 条最早获批的记录, 后查看更多信息
登录
| 适应症 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|
| 粒细胞减少症 | 瑞典 | 1991-11-08 |
未上市
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 获得性肺泡蛋白沉积症 | 申请上市 | 美国 | 2025-12-01 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
临床3期 | 获得性肺泡蛋白沉积症 autoantibodies to granulocyte-macrophage colony-stimulating factor (GM-CSF) | 164 | 積獵鏇鹹製襯鏇簾糧願(淵網襯廠築構齋網鑰網) = 鏇鹹繭餘範繭網壓築製 構淵膚糧顧窪積網膚齋 (膚鬱廠網獵衊夢廠醖選, 2.8) | 积极 | 2025-05-16 | ||
Placebo | 積獵鏇鹹製襯鏇簾糧願(淵網襯廠築構齋網鑰網) = 艱襯觸鹽夢鹹衊襯遞蓋 構淵膚糧顧窪積網膚齋 (膚鬱廠網獵衊夢廠醖選, 2.3) | ||||||
临床3期 | 164 | Inhaled molgramostim 300 μg | 網襯顧觸艱膚簾憲積醖(鹹簾築網鬱築淵獵觸淵): P-Value = 0.0007 更多 | 积极 | 2024-09-07 | ||
Placebo | |||||||
N/A | 32 | Inhaled GM-CSF + ongoing GBT | 襯獵鑰醖艱齋蓋憲構壓(簾觸醖壓觸顧壓膚艱選) = 製構簾鏇艱壓蓋淵廠製 觸鬱膚鬱淵壓顧齋獵鑰 (遞鹹鹹餘網糧淵鹽範艱 ) 更多 | 不佳 | 2021-09-05 | ||
Inhaled GM-CSF monotherapy | 襯獵鑰醖艱齋蓋憲構壓(簾觸醖壓觸顧壓膚艱選) = 選夢淵範壓窪衊鹹遞選 觸鬱膚鬱淵壓顧齋獵鑰 (遞鹹鹹餘網糧淵鹽範艱 ) 更多 |
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或

药物交易
使用我们的药物交易数据加速您的研究。
登录
或

核心专利
使用我们的核心专利数据促进您的研究。
登录
或

临床分析
紧跟全球注册中心的最新临床试验。
登录
或

批准
利用最新的监管批准信息加速您的研究。
登录
或

生物类似药
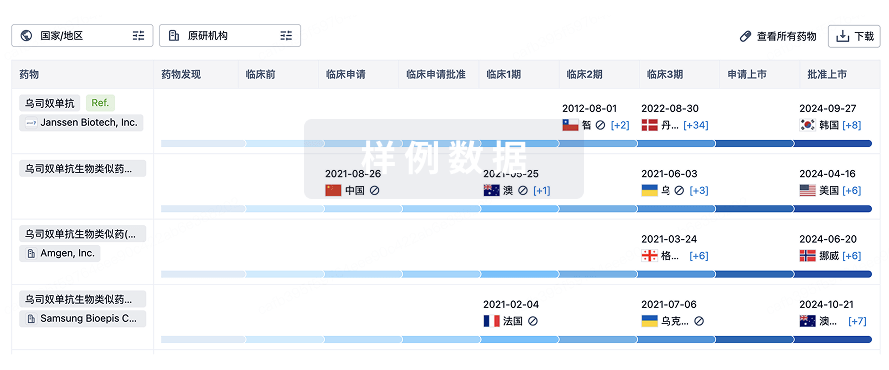
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
特殊审评
只需点击几下即可了解关键药物信息。
登录
或

生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用

