预约演示
更新于:2025-05-07
CD40 x GD2
更新于:2025-05-07
关联
1
项与 CD40 x GD2 相关的药物作用机制 CD40抑制剂 [+1] |
最高研发阶段临床2期 |
首次获批国家/地区- |
首次获批日期1800-01-20 |
4
项与 CD40 x GD2 相关的临床试验NCT02130869
A Pilot Study of Immunotherapy Including Haploidentical NK Cell Infusion Following CD133+ Positively-Selected Autologous Hematopoietic Stem Cells in Children With High Risk Solid Tumors or Lymphomas
This is a pilot clinical trial investigating the addition of haploidentical natural killer cell infusion to autologous stem cell transplantation. This intervention will be evaluated in children with high-risk solid tumors for whom autologous transplantation is indicated. Natural killer cells from a haploidentical family member will be given after high dose chemotherapy and positively selected autologous stem cells. In patients with neuroblastoma, the anti-GD2 antibody hu14.18K322A will also be given. The effect on normal hematopoietic cell recovery will be evaluated and survival of children treated with this approach will be determined.
The investigators expect to enroll 36 participants. Haploidentical family members (donors) will also be recruited to provide natural killer cells.
The investigators expect to enroll 36 participants. Haploidentical family members (donors) will also be recruited to provide natural killer cells.
开始日期2014-10-10 |
100 项与 CD40 x GD2 相关的临床结果
登录后查看更多信息
100 项与 CD40 x GD2 相关的转化医学
登录后查看更多信息
0 项与 CD40 x GD2 相关的专利(医药)
登录后查看更多信息
7
项与 CD40 x GD2 相关的文献(医药)2022-05-01·Journal for ImmunoTherapy of Cancer
Mechanism of effective combination radio-immunotherapy against 9464D-GD2, an immunologically cold murine neuroblastoma
Article
作者: Komjathy, David ; Rodriguez, Matthew ; Aiken, Taylor J ; Sondel, Paul M ; Morris, Zachary S ; Stuckwisch, Ashley ; Erbe, Amy K ; Rakhmilevich, Alexander L ; Zebertavage, Lauren ; Gillies, Stephen D ; Birstler, Jen ; Feils, Arika S
2019-12-01·Journal for ImmunoTherapy of Cancer2区 · 医学
Combined innate and adaptive immunotherapy overcomes resistance of immunologically cold syngeneic murine neuroblastoma to checkpoint inhibition
2区 · 医学
ArticleOA
作者: Morris, Zachary S ; Wang, Xing ; Slowinski, Jacob ; Farrel, Alvin ; Sondel, Paul M ; Erbe, Amy K ; Carlson, Peter M ; Gillies, Stephen D ; Rasmussen, Kayla ; Maris, John ; Hank, Jacquelyn A ; VandenHeuvel, Sabrina ; Hoefges, Anna ; Stuckwisch, Ashley ; Patel, Ravi B ; Voeller, Julie ; Rokita, Jo Lynne ; Rakhmilevich, Alexander L
2017-02-15·The Journal of Immunology2区 · 医学
Effective Combination of Innate and Adaptive Immunotherapeutic Approaches in a Mouse Melanoma Model
2区 · 医学
Article
作者: Korman, Alan J ; Sondel, Paul M ; Felder, Mildred ; Rakhmilevich, Alexander L ; Hoefges, Anna ; Gillies, Stephen D ; Lever, Lauren ; Loibner, Hans ; Van De Voort, Tyler J ; Rasmussen, Kayla ; Slowinski, Jacob
10
项与 CD40 x GD2 相关的新闻(医药)2024-11-08
摘要:双特异性抗体(bsAbs)能够实现传统基于IgG的抗体无法达到的新型作用机制和/或治疗应用。因此,这些分子在过去十年中引起了极大的兴趣,并且截至2023年底,已有14种bsAbs获得批准:11种用于治疗癌症,3种用于非肿瘤学指征。bsAbs有不同格式,针对不同的目标,并通过不同的分子机制介导抗癌功能。在这里,我们提供了bsAbs在癌症治疗领域最新进展的概述。我们专注于已批准或处于临床开发中的bsAbs,包括bsAb介导的信号通路双重调节剂、肿瘤靶向受体激动剂、bsAb-药物偶联物、双特异性T细胞、自然杀伤细胞和先天免疫细胞的招募者,以及双特异性检查点抑制剂和共刺激因子。最后,我们对处于更早开发阶段的下一代bsAbs进行了展望,包括三特异性抗体、bsAb前药、诱导肿瘤目标降解的bsAbs以及作为细胞因子模拟物的bsAbs。
引言
bsAbs用于双重受体抑制 bsAbs用于配体-受体抑制 bsAbs用于受体激活 bsAbs用于靶向载荷递送 bsAbs用于癌症免疫治疗、 新兴概念 、展望,双特异性抗体通过新生儿Fc受体(FcRn)循环利用。Fc部分的突变可以改变与FcRn的结合,从而改变抗体的半衰期。在不包含Fc部分的bsAbs中,可以通过其他方式实现类似IgG的药代动力学,例如结合到人血清白蛋白(HSA)或其他可以延长半衰期的分子。目前有超过几百种不同类型的bsAb格式,其中多种格式在已批准和处于临床开发中的分子中使用。目前,大多数已批准的bsAbs和处于药物开发高级阶段的分子主要用于癌症免疫治疗。其他针对新型药物递送的实体也在开发中,例如基于bsAb的抗体-药物偶联物(bsADCs)或双重靶向与癌症相关的信号通路(图1)。我们最近在ClinicalTrials.gov、Cortellis和The Antibody Society的数据搜索显示,有超过200种不同的双特异性分子的300多项临床试验正在进行中,其中约75%用于治疗实体瘤,25%用于治疗血液恶性肿瘤(图1)。目前有十种bsAb药物已获批准用于癌症治疗,其中九种在美国和/或欧洲获批准,卡多尼利单抗在中国获批准。在这十种bsAbs中,有九种可以归类为TCEs。卡塔莫单抗是首个获批准的bsAb,于2013年退出市场(表1和图2)。值得注意的是,今天在临床开发中的相当一部分bsAbs已经处于后期阶段(第二阶段和第三阶段)。我们发现,用于治疗实体瘤的bsAbs主要由免疫调节剂主导,包括双重CPIs(约45%)和TCEs(约33%),其次是针对双重通路的bsAbs、ICEs和双重ADCs。相比之下,TCEs是用于治疗血液恶性肿瘤的主要bsAbs类别(约75%),其次是ICEs、双重CPIs和NKCEs(图3)。我们数据集中的bsAbs针对60多个不同的目标,使用超过50种不同的bsAb格式,涉及100多种目标组合。然而,我们承认,该领域的增长速度很快,新的bsAbs,可能具有新的目标和格式,已经进入临床试验,自我们分析以来。尽管如此,本综述旨在提供一份基于MoA的全面概述,介绍作为癌症治疗开发的bsAbs的最新进展,重点关注截至2023年底在同行评审出版物中描述的bsAbs。
双受体抑制的bsAbs
许多参与细胞信号传导的细胞表面蛋白,如RTKs及其相关受体,是抗体基疗法的验证目标。几十年前,对这些蛋白的研究,包括历史上的先行者表皮生长因子受体(EGFR;也称为HER1)、HER2、血管内皮生长因子(VEGF)和针对它们的抗体,为几乎所有后续的抗体基治疗发展奠定了基础。尽管结合一个定义的信号实体的抗体基疗法相当有效,但与疾病相关的表现型通常由多个通路触发。这种冗余允许细胞通过使用其他补偿性信号通路来克服单一目标或通路的药理学生长抑制或诱导细胞毒性。同时调节不同的与疾病相关的信号受体和/或通路的bsAbs可以减少或克服这种限制。Amivantamab(JNJ-61186372)靶向EGFR和肝细胞生长因子受体(MET)。两种受体都会触发非小细胞肺癌(NSCLC)的增殖,因此,阻断两者可以比仅阻断一个通路更有效地抑制NSCLC的生长。Amivantamab已获批准用于治疗携带EGFR外显子20插入突变的NSCLC亚型。
图1 | 用于癌症治疗的双特异性抗体在临床开发中。目前有200多种双特异性抗体(bsAbs)正在进行临床开发,根据癌症类型、临床阶段和作用模式进行分组。正在进行临床开发的bsAbs中有50%处于II期和III期或已经获批。大约四分之三的bsAbs被开发用于治疗实体瘤,实体瘤治疗主要由T细胞招募剂(TCEs;32.9%)和具有检查点抑制和/或免疫调节作用机制(MoAs)的bsAbs(45.1%)所主导。相比之下,血液系统恶性肿瘤的治疗主要由TCEs(75%)和其他MoAs(21.9%)所主导,这些MoAs涉及免疫学活动,如通过检查点抑制和/或免疫调节激活自然杀伤细胞和其他免疫细胞,这归功于高度肿瘤选择性或谱系特异性抗原的可用性。值得注意的是,约有10%用于实体瘤治疗的bsAbs采用双重信号抑制。迄今为止,正在开发的bsAb抗体-药物偶联物(ADCs)用于治疗实体瘤。CPI,检查点抑制剂;ICE,先天细胞招募剂;NKCE,自然杀伤细胞招募剂。
双特异性抗体用于配体-受体抑制
受体激活可以通过干扰受体二聚体化或复合物形成,或通过阻断受体的配体结合位点来抑制。在癌症中,通常来自几个互补或补偿通路的配体和受体有助于肿瘤进展和治疗抗性。bsAbs可以同时阻断两种不同的配体,无论是可溶的还是细胞膜结合的,或者是配体和受体的组合。这种方法不仅用bsAbs来解决,也用双特异性或双位点基于支架的结合剂来解决,这里我们不包括。双重靶向VEGF和血管素2(ANG2)以阻断分别参与血管生成的VEGFR和血管素-1受体(TIE2)的激活,已成为包括微转移的血管生成转换在内的实体瘤中几项临床试验的主题。BI836880是一种三特异性纳米抗体(Nb)融合蛋白,由三个靶向VEGFA、ANG2和HSA的纳米抗体组成,后者用于延长其血清半衰期。这种化合物目前正在对头颈鳞状细胞癌、NSCLC和其他实体瘤患者进行I期研究。值得注意的是,vanucizumab,一种靶向VEGFA和ANG2的bsAb,在与化疗联合使用的临床前模型中显示出抗肿瘤、抗血管生成和抗转移效应,但在与化疗联合使用时,并未在结直肠癌患者中提高无进展生存期,超过VEGF抑制。将VEGF抑制与另一种拮抗活性相结合的概念进一步应用于靶向VEGF和Delta样规范Notch配体4(DLL4)的bsAbs。DLL4是一种细胞表面配体,激活Notch-1受体通路,该通路在肿瘤血管生成中起着核心作用。几种靶向VEGF和DLL4的双特异性抗体已经进入临床试验,包括navicixizumab、dilpacimab和CTX009/ABL001。Navicixizumab是一种四价双特异性抗体,具有四个结合位点,其中两个基于单链可变片段(scFv)融合,它在与紫杉醇联合使用时在铂类耐药卵巢癌患者中展示了有希望的临床活性,并具有可管理的毒性,表明这种方法可能在某些适应症中提供临床益处。相比之下,另一项针对四价双特异性抗体dilpacimab的II期研究,与亚叶酸、氟尿嘧啶和伊立替康(FOLFIRI)联合使用,揭示了安全问题。
表1 | 批准用于癌症治疗的双特异性抗体
ADCC,抗体依赖性细胞毒性;ALL,急性淋巴细胞性白血病;BCMA,B细胞成熟抗原;BiTE,双特异性T细胞招募剂;bsAb,双特异性抗体;DLBCL,弥漫性大B细胞淋巴瘤;EGFR,表皮生长因子受体;EpCAM,上皮细胞粘附分子;GPRC5D,G蛋白偶联受体C类5成员D;MoA,作用机制;NSCLC,非小细胞肺癌;NHL,非霍奇金淋巴瘤;scFv,单链可变片段;TCR,T细胞受体;TDCC,T细胞依赖性细胞毒性。批准区域限于美国、欧洲联盟(EU)、日本和中国;产品也可能在其他国家获得批准。状态截至2023年底。
靶向VEGF和PDL1或PD1的双特异性抗体
基于VEGF抗体和免疫检查点抑制剂(CPI)联合治疗的积极结果,上述概念进一步适应于设计靶向VEGF和肿瘤细胞上的PDL1或T细胞上的PD1的双特异性抗体,从而将抗血管生成与免疫肿瘤学方法相结合。使用这种方法最先进的分子是ivonescimab(AK112),它针对PD1和VEGF。目前,ivonescimab的上市申请正在中国接受监管审查。其他双特异性抗体靶向PDL1和VEGF,包括PM8002,目前正在进行II/III期研究(NCT05756972),针对NSCLC患者。
受体激活的双特异性抗体
许多抗肿瘤反应是通过激活细胞表面受体介导的,包括免疫反应或通过诱导凋亡的细胞死亡。癌症治疗的一种方法是通过将受体激活配体(如生长因子、细胞因子和(共)免疫刺激配体)融合到抗体或抗体片段上,实现受体激活配体的靶向递送,以诱导局部或组织特异性的激动活性,从而引发细胞反应。越来越多的这些抗体-配体融合蛋白正在进入临床试验。受体激活也可以通过激动性抗体来实现。肿瘤坏死因子(TNF)超家族的成员,包括死亡配体(如TNF配体超家族成员10(TNFSF10);也称为TRAIL)及其各自的死亡受体(如TRAIL受体1和2;也称为DR4和DR5),或具有免疫细胞共刺激活性的配体(如TNFSF9;也称为4-1BBL)及其受体(如TNFRSF9;也称为4-1BB或CD137)在癌症治疗中引起了特别关注。然而,单克隆抗体在临床试验中取得了相当令人失望的结果。原因是许多TNFRSFs需要超过两个受体的交联以激活,这只能通过Fc-FcγR介导的抗体在细胞表面的超聚集来实现,因此依赖于TME中表达足够数量FcγR的先天免疫细胞。作为替代方案,针对目标抗原和TNFRSF成员的双特异性抗体已被证明可以作为强大且肿瘤选择性的激动分子,模仿表面展示配体的活性。这尤其适用于DR4和DR5,DR5需要多个受体的聚集才能激活。值得注意的是,针对DR5和表面抗原的双特异性抗体,如成纤维细胞激活蛋白-α(FAPα;也称为脯氨酸内肽酶FAP)、钙粘蛋白17(CDH17)或叶酸受体-α(FRα),不仅有效地诱导受体激活,还避免了通过诱饵受体的隔离50。RG7386(RO6874813),一种针对癌症相关成纤维细胞上的FAPα和DR5的四价双特异性抗体,在体外和体内在表达FAPα的基质的小鼠中触发了强效且选择性的肿瘤细胞杀伤,并已进入临床测试,但由于战略投资组合优先级而随后中止。此外,BI905711,一种针对DR5和CDH17的四价双特异性IgG-scFv融合蛋白,目前正在进行I期临床研究,显示出在CDH17阳性目标细胞上的效力比单克隆抗体提高了1000倍以上,转化为在结直肠癌模型中的强效且选择性的抗肿瘤活性。相同的格式用于针对DR5和FOLR1的双特异性抗体,FOLR1是一种富集于卵巢癌的受体,已被证明介导顺式(在同一细胞上)和反式(在两个不同细胞上)的细胞毒性,其中FOLR1作为有效DR5激活的聚集点。从概念上讲,这种MoA也可以转移到依赖于受体聚集的TNFRSF家族的共刺激成员,包括4-1BB、OX40和CD40(见图3),使用针对肿瘤相关抗原(TAAs)的双特异性抗体,但也针对其他目标,如PDL1,从而将共刺激与检查点抑制相结合(见下文)。
用于靶向载荷递送的双特异性抗体
存在两种概念上不同的方法,用于使用双特异性抗体进行有效载荷(如细胞毒素或放射性)的靶向递送。第一种方法,预靶向治疗,使用双特异性抗体的一个结合特异性来靶向肿瘤细胞,另一个结合特异性随后捕获肿瘤上的载荷。这类双特异性抗体结合到肿瘤上的癌症靶标,如癌胚抗原(CEACAM5)或HER2,然后捕获由双特异性抗体的第二个结合特异性识别的放射性标记载荷/复合物。
图2 | 已批准用于癌症治疗的双特异性抗体概览。a, 双特异性T细胞招募剂(TCEs)。b, 其他双特异性抗体(bsAbs)(非T细胞招募剂(非TCEs))。11种已批准的bsAbs中有6种具有IgG样结构,由2条重链(恒定区域以深灰色显示,Vh结构域以深蓝色或深红色显示)和2条轻链(恒定结构域以浅灰色显示,Vl结构域以浅蓝色或浅红色显示)组成。它们大多数具有1+1的化学计量比 —— 每个抗原一个结合位点 —— 还有一个TCE通过将一个额外的Fab片段融合到一条重链上,利用2+1的化学计量比。其他的bsAbs要么是不含Fc的融合蛋白,由两个单链可变片段(scFv)片段组成(blinatumomab),要么是将scFv片段与T细胞受体(TCR)片段融合,或者是具有2+2化学计量比的IgG-scFv融合蛋白。除了由小鼠和大鼠杂交瘤细胞技术生产的catumaxomab外,所有其他的bsAbs都是通过重组技术生产的。对于IgG样异二聚体分子,通过在CH3域使用突变来强制异二聚体化 —— 如旋钮-入洞技术 —— 或控制的Fab臂交换(cFAE),解决了两种不同重链的正确组装问题,cFAE还允许从两种不同的单特异性IgG组装IgG样分子。cFAE还解决了轻链问题,即轻链和重链的配对。或者,如CrossMab方法所示,对Fab臂进行进一步的修改,以强制正确的轻链和重链配对。值得注意的是,所有重组IgG样bsAbs都包含一个具有沉默或减少效应功能的Fc区域,这是通过在铰链/CH2域引入突变来避免或减少Fcγ受体和补体结合来实现的。BCMA,B细胞成熟抗原;EGFR,表皮生长因子受体;EpCAM,上皮细胞粘附分子;GPRC5D,G蛋白偶联受体C类5成员D。
最近,被称为SADA的双特异性抗体利用改良的p53四聚体化域来延长GD2×DOTA在肿瘤中的滞留时间。GD2×DOTA是一种双特异性抗体,能够识别在癌症中高表达的二唾液酸神经节苷脂GD2,以及放射性载荷177Lu-DOTA,在肿瘤微环境中组装并滞留在那里,但没有四聚体化,它会迅速从周围清除,因为它缺乏半衰期延长。到目前为止,很少有临床试验中的双特异性抗体使用这种MoA,可能是由于与预靶向放射性相关的复杂物流限制了其普遍适用性。
图3 | 目前正在临床试验中的双特异性抗体的作用机制。a, 通过受体阻断两种不同的信号受体(以不同颜色表示)来抑制信号传导。b, 通过抑制可溶性配体(蓝色)和受体来抑制信号。c, 通过双重阻断两种不同的配体来抑制信号。d, 通过双特异性抗体(bsAb)药物偶联物(偶联物以浅蓝色表示)进行药物传递。e, 针对性阻断“别吃我信号”(CD47–SIRPα相互作用),导致巨噬细胞的吞噬作用。f, 结合检查点抑制,阻断“别吃我信号”。g, 通过T细胞受体(TCR)上的CD3或自然杀伤细胞上的CD16(FcγRIIIa)激活效应细胞。h, 肿瘤细胞结合介导的免疫细胞(共)刺激。i, PDL1结合介导的免疫细胞(共)刺激。j, 双重免疫细胞共刺激。k, 肿瘤靶向PDL1途径抑制。l, 肿瘤靶向PD1途径抑制。m, 检查点结合介导的免疫细胞(共)刺激。n, 双重检查点抑制。o, 通过配体阻断实现双重检查点和可溶性转化生长因子-β(TGFβ)信号的抑制。展示了用于实体瘤和血液系统恶性肿瘤的目标分子和肿瘤相关抗原(TAAs)的例子。注意:bsAbs可以同时发挥多种作用机制(MoAs)。Ang2,血管生成素2;APC,抗原呈递细胞;BCMA,B细胞成熟抗原;CDH17,钙粘蛋白17;DLL4,典型Notch配体4;EGFR,表皮生长因子受体;EpCAM,上皮细胞粘附分子;FRα,叶酸受体α;GPRC5D,G蛋白偶联受体C类5成员D;HLA,人类白细胞抗原;ICOS,诱导性T细胞共刺激因子;LAG3,淋巴细胞相关基因3;TIGIT,具有免疫球蛋白和ITIM结构域的T细胞免疫受体;VEGF,血管内皮生长因子。
双特异性抗体药物偶联物
第二种方法通过同时靶向肿瘤细胞表面的两个表位或两个目标,实现了通过双特异性抗体药物偶联物(bsADCs)传递细胞毒素载荷的特异性靶向。处于临床开发中的bsADCs的例子包括zanidatamab zovodotin(ZW49),这是一种双特异性HER2结合抗体zanidatamab与auristatin衍生的细胞毒素载荷偶联,双特异性MET×MET bsADC REGN5093或izalontaxab brengitecan(BL-B01D1),一种EGFR×HER3 bsAb与一种新型TOPO-I抑制剂偶联(NCT05194982)(表2)。
双特异性抗体用于癌症免疫治疗
大多数用于癌症免疫治疗的双特异性抗体通过T细胞驱动的自然或内源性免疫发挥作用,例如通过增强现有的抗肿瘤反应和/或克服检查点抑制,或通过提供合成免疫,例如通过bsAb驱动的免疫细胞的参与、激活和招募(图3)。在这一部分中,我们提供了包括CPIs、效应细胞招募剂(包括TCEs和ICEs)和共刺激双特异性抗体在内的最突出的MoAs的概述。
双重CPIs
许多干扰免疫检查点(如CTLA4或PD1/PDL1)的单特异性抗体已获批准用于癌症免疫治疗,包括ipilimumab、tremelimumab、nivolumab、pembrolizumab、atezolizumab、avelumab、durvalumab或cemiplimab。将免疫检查点抑制抗体治疗扩展到包括双特异性抗体可能会减少不良副作用并提高观察到的单特异性抗体治疗的疗效。第一个方面,检查点抑制的安全性,包括预防自身免疫相关事件和/或不希望的免疫细胞激活。为了实现这一目标,正在开发针对检查点抑制功能和TAAs(如RTKs)的双特异性抗体,目的是将其活动更优先地集中在肿瘤上,正在开发中。第二个方面,检查点免疫治疗的疗效,通过双特异性抗体同时靶向两种不同的检查点蛋白来提高疗效并降低抗性的可能性,或提供互补的免疫刺激信号。值得注意的是,这些双特异性抗体的共同设计原则是提高对表达两种检查点蛋白的T细胞的选择性,如CTLA4/PD1或PD1/淋巴细胞相关基因3(LAG3),这些蛋白可能更具肿瘤反应性,目标是提供比单独检查点阻断更优越的治疗指数。
表2 | 晚期临床开发中选择的双特异性抗体概览
BiTE,双特异性T细胞招募剂;BCMA,B细胞成熟抗原;bsAb,双特异性抗体;BTC,胆管癌;cL,普通轻链;DART,双亲和重定向;DLL4,类似Delta的典型Notch配体4;EGFR,表皮生长因子受体;EpCAM,上皮细胞粘附分子;Fchet,异二聚体化Fc;LAG3,淋巴细胞相关基因3;Nb,纳米抗体;NHL,非霍奇金淋巴瘤;NSCLC,非小细胞肺癌;PDC,胰腺导管腺癌;scFv,单链可变片段;TIGIT,具有免疫球蛋白和ITIM结构域的T细胞免疫受体;TGFβ,转化生长因子β;VEGF,血管内皮生长因子。a晚期包括关键性II期、II/III期和III期临床研究。
例如,通过降低自身免疫不良事件的发生率 —— 而不是与联合检查点阻断相比。探索肿瘤靶向检查点抑制的工作包括开发双特异性抗体,这些抗体靶向肿瘤细胞表面的HER家族RTKs,并结合PD1/PDL1信号通路的阻断作为第二功能,从而将PDL1结合剂定向到肿瘤细胞。这些分子的特定肿瘤靶向导致了对表达EGFR的肿瘤细胞更具特异性和增强的活性。类似地,一种特别结合HER2和PDL1的双特异性抗体被证明可以在HER2表达的肿瘤细胞中特异性阻断PDL1活性,从而比单独使用每个实体或在不作为双特异性抗体结合时联合应用产生更大的治疗效果。
另一种双特异性抗体介导的靶向免疫治疗方法包括将PDL1阻断与识别黑色素瘤上的软骨素硫酸蛋白聚糖4(CSPG4)的结合物相结合。特定的肿瘤靶向增强了抗肿瘤T细胞的特异性、激活状态和疗效。概念上相关的方法包括将PDL1结合物与黑色素细胞刺激激素化学偶联。通过这种方式,PDL1抑制活性被定向到黑色素瘤细胞上的黑色素皮质素-1受体。同时靶向两个检查点蛋白而不额外包括常见的肿瘤细胞表面靶标的双特异性抗体的例子包括同时结合肿瘤细胞上的PD1和PDL1的双特异性抗体。Wan等人分析了这种双特异性抗体在高级别浆液性卵巢癌类器官与免疫细胞共培养中引发的联合活性。与单特异性结合物相比,双特异性抗体介导了优越的疗效,并在T细胞和自然杀伤细胞中诱导了表型变化,包括激活状态和细胞毒性的改变。双特异性抗体LY3434172也采用了这种方法。通过完全抑制PD1/PDL1途径,LY3434172显示出比每个亲本抗体或两者组合更大的抗肿瘤活性,再次证明以双特异性抗体形式的结合很重要,并且可以增加疗效。超越PD1/PDL1方法的界限,包括CTLA4在内的其他免疫受体的双特异性抗体正在开发或已获批准。同时靶向PD1和CTLA4是双特异性抗体cadonilimab的作用机制。Cadonilimab由于四价性,介导了对高密度PD1和CTLA4的增加亲和力驱动的目标结合,这与Fc突变以废除FcγR结合相结合,可能是其有利的治疗指数的基础。值得注意的是,cadonilimab还在PD1+和CTLA4+ T细胞之间介导了跨结合。在晚期实体瘤患者的I/Ib期研究中,cadonilimab显示出抗肿瘤活性和有利的安全性概况,免疫相关不良事件的发生率低。Cadonilimab已在中国获批准用于治疗在铂类化疗后或化疗期间进展的复发或转移性宫颈癌。其他在高级临床试验中结合相同特异性的双特异性抗体是MGD019和MEDI5752。MGD019结合了PD1和CTLA4结合物,在进行中的临床研究中观察到可接受的安全性和组合阻断以及在多种实体瘤中的客观反应。MEDI5752目前正在进行临床评估,它结合了PD1和CTLA4,并显示了PD1介导的靶向,因为它优先饱和了PD1+ T细胞上的CTLA4,并引起了PD1的快速内化和降解。与cadonilimab相比,MGD019和MEDI5752似乎对双阳性T细胞显示出更强的亲和力驱动的选择性增益。双重失活也在探索中,通过结合PD1/PDL1阻断与LAG3或TIM3抑制。例子是IBI323和FS118,它们都结合了PDL1和LAG3,并在临床前模型中显示出增强的双重功效。LY3415244结合了PDL1和TIM3的阻断,作为一种不同的免疫调节剂,但由于在I期研究中观察到的免疫原性,该分子的开发被终止。最近,I期剂量递增和扩展数据的临床试验显示,PD1×LAG3双特异性抗体tebotelimab在实体瘤或血液系统恶性肿瘤患者中作为单药治疗以及与HER2抗体margetuximab联合治疗时显示出有希望的活性。双配体抑制是另一种基于双特异性抗体的检查点抑制方法。PDL1和转化生长因子-β(TGFβ)是具有互补且非冗余免疫抑制活性的受体结合配体。TGFβ不仅具有免疫抑制作用,还可以进一步诱导促血管生成因子的上调和癌症相关成纤维细胞的激活。目前正在开发几种靶向PDL1和TGFβ的双特异性抗体,如类似双特异性抗体融合蛋白的bintrafusp alfa(M7824)。在这种情况下,PDL1的结合是通过一个“标准”的抗体结合模块实现的,而TGFβ则被人类TGFβ受体II的细胞外域捕获。Bintrafusp alfa在临床前研究中显示了激活先天和适应性免疫系统,从而比单独使用抗PDL1抗体或TGFβ陷阱模块更好地抑制肿瘤生长和转移,目前正在进行临床试验。Retlirafusp alfa(SHR-1701),另一种以类似方式靶向PDL1和TGFβ的双功能融合分子,正在对宫颈癌和胃癌或胃食管结合部癌症患者进行III期研究(表2)。YM101是一种TGFβ×PDL1双特异性抗体,目前处于临床前开发阶段。YM101的一个替代品,Y101D,正在对晚期实体瘤患者进行评估(NCT05028556)。所有同时对抗抑制性TGFβ和PD1/PDL1途径的方法在体内模型中显示出比单独使用各自结合物更高的抗肿瘤活性,但迄今为止尚未在临床上证明概念。针对性的TGFβ信号阻断也已经在临床前研究中通过阻断CD4+ T细胞中的TGFβ信号的双特异性抗体实现。为此,将非免疫抑制性的CD4靶向抗体ibalizumab与TGFβ陷阱以类似于上述的双特异性抗体方式结合。这导致在辅助T细胞中针对性阻断TGFβ信号,可以释放抗肿瘤反应。通过双特异性抗体招募磷酸酶抑制PD1是一种最近报道的新型MoA88。这是通过一个单域(Vhh)融合到一个scFv实现的,将PD1连接到细胞表面磷酸酶CD45,这反过来触发细胞内去磷酸化。这种方法与单独使用PD1抗体介导的配体阻断相比,增强了检查点阻断的抑制。按照同一原则,双特异性抗体可以将细胞表面磷酸酶CD45与抑制性自然杀伤细胞表面受体NKG2A或Ly49连接,以进行后续去磷酸化。这样的双特异性抗体可以阻断并同时去磷酸化它们的目标,可能比相应的单特异性抗体及其抑制信号的组合更有效的拮抗剂,以增强自然杀伤细胞和T细胞的抗肿瘤活性。使用双特异性抗体对CD73的不同表位进行双位点靶向是另一种双特异性抗体相关方法,以抵消免疫抑制活性或增强针对肿瘤的免疫能力。CD73产生免疫抑制性腺苷,其通过内化的双特异性抗体介导的抑制和耗尽比单一位点CD73抗体更有效。
效应细胞招募剂 T细胞招募剂
在过去二十年中,专门结合肿瘤表面抗原和TCR的CD3ε链的T细胞招募剂(TCEs)在这一类双特异性抗体中占据主导地位,描述了数百种TCEs,并且有100多种进入临床开发。事实上,第一个获准上市的双特异性抗体是鼠/大鼠嵌合的上皮细胞粘附分子(EpCAM)×CD3ε双特异性抗体catumaxomab,它在2009年被欧洲联盟(EU)批准用于恶性卵巢腹水的腹腔内治疗,但后来因商业原因退出市场。目前正在中国再次进行临床试验,用于腹腔内给药。系统应用的catumaxomab显示出严重的输注反应和高免疫原性发生率,可能由于其鼠/大鼠嵌合的恒定区域和保留的FcγR结合,导致在没有抗原结合的情况下非特异性FcγR和TCR激活。随后,下一代TCEs被设计为缺乏Fc部分,如基于串联scFv的CD19×CD3ε双特异性T细胞招募剂(BiTE)blinatumomab,它在2014年首次被批准用于治疗B细胞前体急性淋巴细胞性白血病(B-ALL)。然而,由于缺乏通过FcRn的循环,这种疗法需要持续输注,FcRn通过从分拣内体循环到细胞表面,从内溶酶体降解中挽救IgG。基于blinatumomab的成功,针对血液和实体瘤的各种目标的BiTEs被开发出来,但最终没有进入晚期临床试验,由于BiTEs和相关短半衰期的药代动力学特性不佳。人们尝试通过纳入FcγR结合惰性Fc结构域(沉默Fc)或HSA结合部分来实现bsAbs的IgG样半衰期,目前大多数处于开发中的TCEs是基于IgG和/或具有IgG样药代动力学的。值得注意的是,大多数TCEs使用单个单价结合位点用于CD3作为T细胞上的触发分子,以避免在没有同时目标结合的情况下TCR交联引起的系统性T细胞激活。然后它们使用一个(1+1)或两个(2+1)肿瘤目标的结合位点,因为双价结合可以在肿瘤选择性和效力方面提供优势。CD20×CD3ε双特异性抗体mosunetuzumab106和B细胞成熟抗原(BCMA)×CD3ε双特异性抗体teclistamab是第一批异二聚体1+1 IgG基TCEs,分别在2022年被批准用于治疗复发/难治性滤泡性非霍奇金淋巴瘤(NHL)或多发性骨髓瘤。在2023年,异二聚体2+1 CD20-TCE glofitamab104,108和1+1 CD20-TCE epcoritamab109被批准用于治疗复发/难治性弥漫大B细胞淋巴瘤(DLBCL),以及1+1 G蛋白偶联受体C类5成员D(GPRC5D)-TCE talquetamab110和BCMA-TCE elranatamab111用于复发/难治性多发性骨髓瘤(表1)。CD20-TCE odronextamab112和BCMA-TCE linvoseltamab的上市申请正在等待监管决定。鉴于它们在复发/难治性B细胞和浆细胞恶性肿瘤患者中显示出的有希望的临床疗效和完全缓解率 —— 包括在CAR-T细胞治疗后复发的患者中的活性 —— 以及它们作为现成疗法的简单可用性以及皮下给药的可能性,可以预期TCEs将成为CAR-T细胞疗法的主要替代品,特别是随着它们开始被开发用于更早期的治疗线并且可以让患者轻松获得。免疫动员单克隆T细胞受体针对癌症(ImmTACs)是结合了工程化TCR以识别人类白细胞抗原(HLA)呈递的肽抗原与抗CD3 scFv的TCEs,实现对细胞内TAAs的靶向。值得注意的是,短暂存在的ImmTAC tebentafusp,它包含一个针对由HLA-A*02:01呈递的黑色素细胞谱系特异性抗原糖蛋白(gp100)表位的可溶性TCR融合到CD3靶向scFv,已在2022年被批准用于治疗葡萄膜黑色素瘤,为TCEs在实体瘤中的细胞内靶标空间开辟了新的领域。值得注意的是,tebentafusp介导了总体生存益处,尽管它只诱导了少数临床反应,因此直接杀死肿瘤细胞可能不是其唯一的MoA。与此同时,各种基于重组TCR或使用类似TCR的抗体(TCR模拟物)的TCEs已进入临床开发,包括针对WT1和突变新抗原如KRAS122或p53的TCEs。重要的是,高通量动力学筛选和通用TCR类似库可以促进高度选择性的TCR和TCR模拟物的开发,用于TCEs。有趣的是,使用共价KRASG12C抑制剂sotorasib,可以产生一种类似TCR的TCE,可以特异性识别HLA呈递的sotorasib-肽共轭物,并随后诱导KRASG12C突变细胞的T细胞杀伤。细胞因子释放综合征的发生,主要是由于靶向T细胞激活,一直是TCEs临床开发的一个主要挑战。尽管在许多情况下,这可以通过使用类固醇预处理和逐步剂量增加来管理,但最近的努力已经研究了使用具有降低CD3ε亲和力的CD3ε抗体,目标是将T细胞杀伤与细胞因子分泌解耦。与CAR-T细胞一样,由于TCEs的杀伤效力非常高,因此需要严格肿瘤特异性和/或谱系特异性表达目标抗原,以避免靶向非肿瘤毒性。对于血液癌症中的B细胞和浆细胞抗原,如CD19、CD20、CD79b、BCMA140141和FcRH5,通常认为它们只存在于B细胞和浆细胞恶性肿瘤以及非必需的B细胞和浆细胞谱系中。然而,即使对于CD19等抗原,其在正常组织中的表达可能并非绝对不存在,有报道称CD19在围绕内皮细胞的壁细胞/血管周细胞上表达,这些细胞对血脑屏障完整性至关重要,作为一种靶向非肿瘤机制与神经毒性有关。相比之下,在急性髓系白血病中,典型的抗原如CD33或CD123也存在于髓系造血谱系上,使得它们的临床开发更具挑战性。类似地,许多主要的(上皮)实体瘤抗原如EGFR、HER2、EpCAM、肿瘤相关钙信号转导蛋白2(也称为细胞表面糖蛋白Trop-2)、MUC1、CEACAM5和glypican 3也可以在(必需的)正常组织中找到。因此,由于更免疫抑制性的肿瘤微环境,TCEs(和CAR-T细胞)在实体瘤的开发在过去几年中进展较少。重要的是,必须认识到对于TCEs,与ADCs150相比,由于更高的效力,对肿瘤选择性的要求更严格,固体瘤ADC靶标如HER2和TROP-2可能无法用传统的TCEs靶向。与此同时,与TCEs相比,ADCs可能由于在肿瘤微环境中释放有毒载荷而受益于更强的旁观者杀伤效应,对抗原阴性肿瘤细胞进行杀伤。因此,很少有肿瘤选择性抗原似乎是TCEs的可行靶标,包括新抗原如p95-HER2和EGFRvIII,或者MUC16、claudin 18.2、DLL3和STEAP1等靶标。对于DLL3靶向的TCE tarlatamab,目前正在美国食品药品监督管理局(FDA)的优先审查中,已在小细胞肺癌中报告了有希望的I期临床数据,总反应率达到23%。随后的II期研究证实了活动性,持久的客观反应和有希望的生存结果,使用每2周10毫克剂量治疗的患者。基于这些数据,已启动了一项随机关键研究,比较tarlatamab与标准护理(NCT05740566)。同样,xaluritamig,一种2+1 STEAP1 TCE,具有亲和力驱动的活性,能够选择性地针对高表达STEAP1的肿瘤细胞与正常细胞相比,已在转移性去势抵抗性前列腺癌患者的I期剂量递增研究中展示了有希望的临床活性。综上所述,这些概念验证数据表明,TCEs仅限于血液癌症活跃的共同假设,特别是B细胞恶性肿瘤,并不适用,并且TCEs也有可能治疗某些实体瘤,只要能够管理靶向非肿瘤活性。正在使用多种方法来克服实体瘤选择性挑战。例如,在双特异性抗体中使用具有降低亲和力的肿瘤抗原结合物(2+1格式)可以实现亲和力介导的选择性增益(也称为亲和力调节),目标是利用肿瘤和正常组织之间的表达差异,如CEACAM5、HER2和FOLR1,以提高肿瘤选择性。或者,双重靶向和亲和力介导的选择性增益应用于三特异性TCEs,这些TCEs选择性地杀死共同表达这些靶标的肿瘤细胞,但不会影响只表达这些靶标中一个的正常细胞。此外,针对两种不同的肿瘤抗原如CD19和CD22的三特异性TCEs可以防止通过抗原丢失的免疫逃逸。尽管大多数传统的TCEs可以招募常规T细胞和非传统先天样γδ T细胞(表达TCRγ/δ而非TCRα/β的T细胞),但一类特定的γδ TCEs已被设计为通过TCRγδ特别招募γδ T细胞,目标是通过只针对可以在患者中进一步扩展的T细胞亚群来提高安全性和有效性。在临床前研究中,γδ TCEs作为单一药物显示出强大的抗肿瘤活性。或者,为了此目的,制造了针对肿瘤的双特异性异二聚体BTN2A1和BTN3A1抗体融合蛋白。由于γδ T细胞生物学在小鼠模型中没有完全反映,这种方法的最终概念验证将不得不依赖于正在进行的临床试验的临床数据,如针对PSMA的γδ TCE LAVA-1207(NCT05369000)。而不是针对CD3ε或TCRα/β的双特异性抗体,肽-MHC复合物可以被应用来特别招募特定pMHC复合物的T细胞,如由于自然发生和普遍的巨细胞病毒感染而存在的巨细胞病毒衍生肽。在另一种方法中,病毒表位可以被传递到肿瘤细胞中,以便加载相应的MHC分子,并招募病毒特异性T细胞攻击这些细胞。还描述了用于更有效介导双特异性抗体介导的聚集和补体依赖性细胞毒性的双特异性抗体。有趣的是,通过应用两对独立的抗体,可以建立一种逻辑门,通过补体依赖性细胞毒性选择性地消除共表达两种抗原的细胞。例如,使用这种方法,可以消除共表达CD20和CD52的B细胞,而单独表达这些抗原的细胞则不会被杀死。随着对采用CAR-T细胞疗法的极大兴趣,一类特定的TCEs,作为CAR-T细胞和肿瘤细胞之间的双特异性适配器,已被设计为特别招募采用转移的T细胞用于治疗各种癌症,同时不涉及自然T细胞。其中一个例子是合成激动性受体(SAR)-T细胞系统,其中一种双特异性抗体识别肿瘤抗原和一个引入到采用转移的T细胞中的合成抗原受体。这种在合成生物学背景下的方法提供了多种方式。
进一步工程化和控制采用T细胞疗法方法,超出了传统抗体疗法或经典CAR-T细胞疗法所能提供的范围。另一种结合细胞疗法和双特异性抗体的方法是体外武装T细胞与多种TCEs,目标是克服肿瘤异质性。为此,T细胞在体外与针对肿瘤抗原如GD2、HER2、PSMA和STEAP1的TCEs孵育,并给药于肿瘤携带动物,在这些动物中,由于抗原丢失,它们阻止了肿瘤进展。
固有细胞招募剂
尽管TCEs在效应细胞招募剂领域占据主导地位,但正在大力开发下一代ICEs,包括NKCEs和双特异性抗体,这些抗体招募髓系衍生细胞(MDCs)进行吞噬作用,包括中性粒细胞和巨噬细胞/单核细胞。介导ADCC的单克隆抗体,如利妥昔单抗、西妥昔单抗或曲妥珠单抗,因为ADCC/抗体依赖性细胞吞噬作用对其MoA至关重要,除了其他作用如信号抑制外,可以被视为第一代ICEs。基于这种经验,已经批准了几种与常规单克隆抗体相比具有增强ADCC功能的Fc工程化IgG1抗体,包括obinutuzumab、mogamulizumab、tafasitamab、margetuximab和amivantamab。基于这种经验和目标,进一步增强ADCC功能,超越Fc工程化IgG1抗体,已经开发了各种双特异性NKCEs,它们针对自然杀伤细胞上的不同表面分子,如CD16、NKG2D、NKp46或NKp30,作为免疫疗法。这些NKCEs中最先进的是一种短半衰期的CD30×CD16双特异性抗体,用于治疗霍奇金淋巴瘤,可以作为单一疗法、与检查点抑制联合或与自然杀伤细胞输注联合使用。最近,开发了针对抗原如EGFR或BCMA的半衰期延长的四价IgG基双特异性抗体,以及利用双重靶向实现肿瘤选择性的三特异性抗体。对称的三特异性NKCEs通过ADCC特别针对通过其CD16结合区域共表达EGFR和PDL1的细胞,使用两种合一抗体技术。另一种激活自然杀伤细胞的方法依赖于双特异性融合蛋白,该蛋白由NKG2D配体(例如UL-16结合蛋白2(ULBP2))与针对HER2的scFv融合,以实现有效的ADCC介导的肿瘤细胞杀伤。或者,保留FcγRIII结合的双特异性抗体,针对NKp46或NKp30和各种肿瘤抗原,可以提供强大的抗肿瘤效果。与TCEs不同,其中FcγR结合是不需要的,这些双特异性抗体依赖于保留或增强的FcγRIII结合,以实现有效的自然杀伤细胞参与。值得注意的是,当IL-2变体被融合到NKp46双特异性抗体上,产生四功能分子时,由于同时诱导自然杀伤细胞扩增,效果大大增强。另一个积极研究的领域是双特异性抗体,这些抗体通过结合,例如,巨噬细胞和中性粒细胞上的FcαRI受体(CD89)或通过双特异性IgE抗体的IgE受体,参与吞噬作用或MDCs以及中性粒细胞的杀伤。或者,肿瘤靶向双特异性抗体可以阻断肿瘤细胞上基于'不要吃我信号'的CD47–SIRP1α相互作用,以便这些细胞被MDCs攻击和吞噬。双特异性CD19 x CD47或间皮素x CD47抗体结合了肿瘤靶向和CD47抑制以及通过效应功能完整的Fc部分招募效应细胞。在这种情况下,对CD47具有低亲和力的双特异性抗体有利于克服不必要的结合到红细胞上的CD47。
各种团队应用这一概念进行PDL1×CD47共靶向。或者,SIRPα融合蛋白可以用来阻断CD47–SIRPα“不要吃我”信号。
共刺激双特异性抗体
有效、持久且局部限制的抗肿瘤免疫反应需要共刺激和共抑制信号来紧密调节细胞毒性T细胞、自然杀伤细胞和巨噬细胞的激活、分化和维持。TNFRSF家族成员(如4-1BB、CD40、OX40、TNFRSF18(也称为糖皮质激素诱导的TNFR相关蛋白(GITR))、CD27或CD30)以及CD28免疫球蛋白超家族(如CD28、CTLA4、PD1、诱导性T细胞共刺激因子(ICOS)和B淋巴细胞和T淋巴细胞衰减因子(BTLA))及其相应的配体,在通过细胞-细胞接触(如抗原呈递细胞(APCs)和T细胞之间)提供的局部免疫调节信号中发挥着显著作用。这些受体为T细胞提供了所谓的信号2,这对于维持TCR通过肽-MHC-TCR相互作用或通过TCE交联TCR所提供的信号1是必需的。针对这些免疫调节途径的靶向可能增强免疫疗法。研究表明,针对共刺激受体的激动性单克隆抗体通常只会导致微弱的激活,但这种激活可以通过FcγR介导的受体超聚集显著增加。此外,抗体与受体之间的化学计量比、结合亲和力和表位特异性等因素可以影响共刺激抗体的活性。因此,降低免疫调节抗体的亲和力可以作为一种策略,通过增加受体聚集来增强激动性活性,这一原则经常应用于双特异性抗体激动剂(见上文)。然而,由于增加的趋化因子和细胞因子产生导致的免疫相关系统性不良事件是共刺激抗体药物开发的限制因素。抗体-细胞因子融合蛋白和双特异性抗体能够以目标依赖的方式提供共刺激信号,通过双重靶向两种不同的共刺激受体或通过靶向共刺激受体和CPI来规避这一限制。
肿瘤靶向共刺激双特异性抗体
用一个臂结合到TAA上,另一个臂结合到免疫细胞上的共刺激受体上的双特异性抗体,可以通过在癌细胞和免疫细胞之间跨作用来局部介导受体聚集,从而提供信号2。目前正在临床试验中的共刺激双特异性抗体包括针对4-1BB、CD40和CD28的分子。T细胞激活后诱导表达的4-1BB使其成为增强CD8 T细胞反应的T细胞共刺激的有吸引力的靶标。使用针对4-1BB的激动性抗体(如urelumab和utomilumab)作为单一疗法在临床试验中的安全性问题和较差的疗效,使人们重新将努力集中在可以克服这些毒性的双特异性抗体上,通过引入肿瘤特异性共刺激。大约一半的癌症靶向共刺激双特异性抗体在临床试验中通过4-1BB发挥作用。先进的双特异性抗体包括PRS-343(cinrebafusp),一种针对HER2和4-1BB的四价双特异性抗体-抗钙蛋白融合蛋白,在IND使能研究中被发现耐受性良好,没有明显和相关药物相关毒性;FAP-4-1BBL(RG7872),作为单一疗法和与PDL1抑制联合使用时显示出药理活性;或englumafusp alfa,正在研究中作为与glofitamab联合用于DLBCL的信号2提供者。其他在临床试验中通过4-1BB进行肿瘤选择性共刺激的双特异性抗体目标包括EGFR、PSMA、CLDN18.2、B7H4、CEACAM5、HER2、PDL1(见下文)和FAP48。此外,使用CD28作为共刺激受体的双特异性抗体,目前在临床试验中。通过与APC上的CD80(也称为B7.1)或CD86(也称为B7.2)的结合,CD28为幼稚T细胞提供了必要的二次信号,以实现完全的T细胞激活和存活。这种信号也可以通过激动性CD28抗体提供,即使在没有初级TCR参与的情况下,如超激动剂TGN1412所示,它在I期研究中因大量细胞因子释放综合征而显著失败。后来发现,TGN1412特别在低剂量下作用于调节性T细胞(Treg细胞),而在高剂量下激活传统T细胞和Treg细胞,为选择性靶向T细胞亚群提供了窗口,但也突出了T细胞共刺激与超激活之间的微妙平衡。一些双特异性抗体可以以目标依赖的方式提供这种二次共刺激信号,以增强肿瘤限制性的抗肿瘤T细胞反应。值得注意的是,双特异性抗体可以被设计为单独使用时活性有限且无毒性,但可以增强T细胞激活和TCEs的抗肿瘤活性。REGN5837是一种针对CD22和CD28的双特异性抗体,已进入与针对CD20的TCE odronextamab联合用于NHL治疗的I期试验。肿瘤靶向CD28双特异性抗体也可以与PD1协同作用,提供长期抗肿瘤免疫反应,目前,多个针对TAAs如EGFR、MUC16、PSMA、B7-H3、CD19、CD22或PDL1的双特异性抗体正在进行临床试验,与检查点抑制联合使用或作为单一疗法。
MDCs和树突细胞激活双特异性抗体
CD40在包括APCs、其他MDCs和B细胞在内的多种细胞类型中表达,但也在广泛的恶性细胞上表达。单克隆激动性CD40抗体可以通过诱导APCs成熟和激活抗原特异性T细胞和其他免疫细胞来触发抗肿瘤效应,从而促进肿瘤特异性免疫反应,特别是通过启动细胞毒性T细胞。除了具有剂量限制毒性的激动性CD40抗体外,还开发了针对CD40和各种TAAs如CEACAM5、EpCAM或间皮素的双特异性抗体。与其他TNF超家族成员一样,受体聚集在受体激活中起着关键作用。将CD40激动性抗体与针对肿瘤靶向抗原的抗体结合在双特异性抗体中,允许共刺激活性定向到TME,从而提高安全性和有效性。例如,针对CD40和CEACAM5或EpCAM的四价双特异性抗体的概念验证表明,与单一CD40抗体相比,它们增强了T细胞交叉启动。针对间皮素和CD40的双特异性抗体(ABBV-428)在体外和体外模型中展示了增强的APC和T细胞激活,并且在I期试验中显示出可接受的安全性概况。为了在肿瘤内而不是外周选择性激活CD40,生成了FAP×CD40,一种包含两个CD40结合位点和一个FAP结合位点的双特异性抗体。该抗体提供了一个强烈的FAP依赖性CD40刺激信号,展示了良好的安全性概况以及肿瘤积聚和肿瘤内免疫激活,目前正在进行I期临床试验。MP-0317是一种多功能设计ankyrin重复蛋白(DARPin),应用相同的概念,针对FAP、CD40和HSA进行半衰期延长,目前正在进行I期临床研究。或者,双特异性抗体可以通过Clec12a标记物直接靶向树突细胞。
双特异性抗体的双重共刺激
在免疫细胞上双重靶向两种不同的共刺激受体已被用于诱导强大的抗肿瘤反应。FS120是一种针对活化T细胞上表达的4-1BB和OX40的四价双特异性抗体,以一种不依赖FcγR的方式激活CD4和CD8 T细胞。这种活性需要两个受体的共刺激才能有效激活免疫细胞并发挥抗肿瘤活性,支持使用四价双特异性抗体双重靶向共刺激受体以诱导有效的受体聚集和激活的概念。在动物研究中,FS120的替代品没有引起肝脏炎症和肝毒性,这是激动性4-1BB抗体观察到的限制。FS120目前正在进行I期临床试验。类似的方法中,开发了一种双价双特异性抗体,用于双重靶向4-1BB和CD40(BNT-312,tecaginlimab),因此靶向T细胞和APCs。APCs的CD40激活导致共刺激分子的上调和免疫刺激性细胞因子的分泌,从而在不依赖CD4 T细胞帮助的情况下,实现强大的CD8 T细胞介导的抗肿瘤免疫反应。
双特异性抗体用于双重检查点抑制和共刺激
抗共刺激受体的抗体还被与CPIs结合使用,以释放T细胞免受抑制信号的影响,同时增强T细胞反应,特别是在对检查点抑制有抵抗力或难治性的肿瘤中。大多数目前正在临床试验中的双特异性抗体使用跨作用的方式结合这些信号,通过靶向肿瘤细胞上的PDL1和免疫细胞上的共刺激受体,其中4-1BB是最突出的靶标。超过十种不同的针对PDL1和4-1BB的双特异性抗体正在进行I期或II期试验。II期候选物包括一种IgG-anticalin融合蛋白(PRS-344),其中配体结合anticalin框架代表第二特异性,一种双价双特异性IgG抗体(acasunlimab,也称为GEN1046)和一种三价,三特异性单链二抗体-scFv融合蛋白,进一步包含一个HSA结合位点以延长半衰期(NM21-1480)。这些类型的双特异性抗体可以增强免疫反应,超越单一抗体及其组合,进一步提供针对PDL1表达肿瘤细胞的靶向共刺激,以及TME中的MDCs和肿瘤引流淋巴结。与此一致,TME中表达4-1BB的肿瘤浸润CD8 T细胞亚群表达高水平的PD1,因此容易受到PDL1×4-1BB双特异性抗体的治疗。值得注意的是,由于4-1BB信号需要超聚集,与PDL1的结合可以导致TME中条件聚集和激活的4-1BB,减少肝脏毒性,如四价双特异性IgG-scFv(ABL503)所示。遵循这一概念的进一步双特异性抗体包括四价双特异性单克隆抗体(FS222)和双价双特异性IgGs,如MCLA-145。同样,CD28共刺激和检查点抑制可以通过在肿瘤内顺式作用的T细胞双重靶向进一步实现。ATOR-1015的可行性已得到证明,它是一种针对OX40的IgG,融合到针对CTLA4的优化版本的V型域的CD86上。与4-1BB类似,CTLA4和OX40在活化的T细胞上上调,并由Treg细胞表达,特别是在TME中。与GITR和ICOS不同,CD27由naive T细胞表达,因此有助于促进新的T细胞反应。
PDL1×CD27双特异性抗体在临床前研究中比PD1阻断和CD27共刺激的组合更有效,同时展现出良好的安全性概况。在概念上类似的方法中,PD1的结合位点与其他TNF超家族的共刺激成员结合,包括4-1BB(如与IBI319结合)、GITR和ICOS(XmAb23104)。GITR也在活化的T细胞上上调,并由Treg细胞恒定表达,在其中发挥着增强初始免疫反应的关键作用。PD1×GITR-L双特异性融合蛋白的概念验证已经展示。对于这些药物中的一些,与联合或分别协同效应相比,检查点抑制的相对贡献并不一定确立。
新兴概念
支持双特异性抗体开发的概念从早期探索性方法迅速发展到临床开发,双特异性抗体现在已确立为治疗原则。然而,双特异性抗体领域仍在不断进展,以进一步探索和扩展技术和应用。学术界以及生物技术和制药工业追求的各种早期探索性双特异性抗体方法是有希望的,其中一部分可能提供尚未由当前开发中的双特异性抗体解决的治疗概念。本综述的范围不允许我们涵盖所有或许多这样的早期方法,实际上在这个快速增长的领域中可能无法全面覆盖。因此,我们通过提及一些我们认为相关并有潜力进一步推动基于双特异性抗体的癌症治疗界限的新兴主题来结束我们的综述。
三特异性TCEs与集成共刺激
共刺激信号可以与双特异性TCEs结合,以促进有效的T细胞激活。这已经通过上述的双特异性TCEs和共刺激双特异性抗体的组合实现,但也通过在双特异性TCE中包含第三个结合位点来针对共刺激受体,从而生成三特异性抗体。目前有两种这样的三特异性TCE正在进行临床试验,它们针对TAA和CD3,并进一步包含一个针对CD28的结合位点。SAR443216是一种三价三特异性免疫球蛋白基抗体,针对HER2×CD3×CD28,包含一个突变的IgG4,缺乏Fc介导的效应功能。这种三特异性抗体目前正在I期临床试验中,能够激活初级CD4和CD8 T细胞,诱导T细胞增殖,释放细胞因子和颗粒酶B以及T细胞介导的HER2表达肿瘤细胞的杀伤,包括HER2表达低的细胞。类似地,一种针对在多发性骨髓瘤中过度表达的CD38的结合位点与CD3和CD28结合位点结合在三特异性抗体SAR442257中,目前也在I期临床试验中。
前药方法
一种新兴的方法旨在通过提供“安全关键”的特异性作为前药,在肿瘤处选择性激活,从而生成具有高度肿瘤特异性功能的双特异性抗体。一些应用于失活抗体以生成前药并在肿瘤处重新激活的概念如图4所示。前药转化为功能性双特异性抗体可以通过肿瘤微环境中存在的肿瘤特异性蛋白酶等环境触发因素来实现。例如,具有空间屏蔽的双特异性抗体可以通过蛋白酶激活。需要肿瘤特异性蛋白酶表达的蛋白酶激活TCEs,即所谓的probodies,需要肿瘤特异性蛋白酶在TME中的表达才能激活。另一种早期阶段的双重肿瘤靶向方法依赖于从两个具有分裂CD3ε结合基团的双特异性抗体中肿瘤特异性组装功能性CD3ε抗体片段。这些实体需要被设计为在循环中作为单独实体时不活跃,以便它们只在肿瘤抗原结合和随后的原位组装后被激活,如已经为半抗体或前药激活链交换(PACE)分子所描述的那样。这类分子面临的主要挑战仍然是以单体形式大规模生产它们,并防止在没有目标结合的情况下过早组装。通过目标链交换介导的分裂型I细胞因子的重建就是一个例子,说明如何实现肿瘤特异性组装。值得注意的是,最近开发了一种引入到抗4-1BB抗体结合位点的ATP依赖性开关,以增加肿瘤选择性并避免靶上、靶外毒性。这种开关使用肿瘤中升高的ATP水平作为触发因素,可能也适用于其他结合实体。
图4 | 双特异性抗体领域的新兴概念。a, 带有集成共刺激的三特异性T细胞招募剂(TCEs),用于通过CD3结合同时激活T细胞受体(TCR)(信号1)和通过结合CD28进行共刺激(信号2)。b, 双特异性抗体(bsAb)前药的作用方式。用于生成前药并重新激活所需作用位点的抗体的一般概念包括:阻断结合位点以使抗体失活,以及通过蛋白酶诱导激活被阻断的抗原结合位点,对目标环境(如酸性pH或ATP)的亲和性调节,以及由于通过高浓度局部富集互补前药而进行的组装或交换反应。c, 通过结合表面抗原(肿瘤相关抗原(TAA))和降解分子,例如膜E3连接酶,实现蛋白酶体靶向嵌合体(PROTAC)方法,这导致细胞表面目标的内化和蛋白酶体降解。d, 例如通过基因疗法将bsAb传递到CAR-T细胞中。e, 细胞因子模拟bsAb触发细胞因子受体途径,如通过将受体域引入立体接近性,模仿细胞因子作用的IL-2Rβ–IL-2Rγ异二聚体。
PROTAC双特异性抗体
另一个新兴概念和新的作用机制最近被描述,它使用双特异性抗体通过靶向降解来灭活与增殖相关的过程。类似于新兴的双特异性或多特异性小分子蛋白水解靶向嵌合体(PROTACs)领域,双特异性抗体可以被设计为触发内部化并随后降解参与癌症发展和/或进展的表面蛋白。这样的双特异性抗体同时结合到被靶向降解的蛋白质,以及触发结合目标蛋白的内部化和随后降解的因素,如膜可及的E3泛素连接酶或转铁蛋白受体。目前还没有已知的抗体-PROTAC概念进入临床研究,但这类实体的开发与“标准”双特异性抗体的开发完全兼容,并为靶向新途径并尽快将其概念带入临床提供了独特的可能性。
双特异性抗体的传递
双特异性抗体发展的另一个重要新兴概念是局部生产和随后的局部传递双特异性抗体,例如通过脂质纳米粒子介导的mRNA传递CLADN6 TCE,溶瘤病毒或类似基因疗法的方法,包括CAR-T细胞。
细胞因子模拟抗体
最后,双特异性抗体也可以作为细胞因子模拟物或所谓的合成细胞因子激动剂。在这种情况下,已经描述了scFvs或基于单一结构域Vhh的方法,通过模仿IL-2或IL-15、IL-18、I型干扰素和IL-10有效地触发细胞因子信号。或者,可以通过使用分裂方法使用新设计的IL-2模拟蛋白neoleukin实现肿瘤特异性细胞因子受体激动活性。这种基于抗体的细胞因子模拟物在癌症免疫疗法中可能有各种应用。
展望
双特异性抗体领域近年来取得了显著进展,到2023年底,已有十多种双特异性抗体获得批准,许多不同的方法正在临床测试中。然而,我们认为,由于癌症的异质性和适应性,这些方法中不太可能有一种成为通用的癌症免疫疗法。相反,抗体将需要为特定应用量身定制,并将依赖于与其他方法的结合,以最大化它们的疗效和安全窗口。具有多重特异性的抗体治疗的发展增长可能会在未来几个领域发生:针对具有明确依赖性的肿瘤的肿瘤相关RTKs的双特异性抗体;用于以增加的选择性靶向肿瘤的双特异性ADCs;用于靶向降解适用于各种途径的细胞表面蛋白的双特异性PROTACs;以及用于癌症免疫疗法的多特异性抗体。在后一个领域,特别是对于非常有效的基于T细胞的疗法,如TCEs或CAR-T细胞,识别高度肿瘤选择性抗原将是至关重要的,将需要能够通过肿瘤特异性蛋白酶激活和更好地调节效应功能来特别实现肿瘤特异性活性,同时保护正常组织。另一个重要方面是提供双重检查点抑制和/或补充共刺激信号给T细胞,以维持和延长T细胞反应,如已被证明对CAR-T细胞疗法的临床成功至关重要。重要的是,这种方法不仅适用于与TCEs的组合,也适用于与内源性免疫方法的组合。另一个重要方面是通过激活先天免疫系统,包括自然杀伤细胞、MDCs和树突细胞,促进二次免疫反应的产生。与其他癌症药物一样,通过改进的诊断方法和新的发展范式,使双特异性抗体和多特异性基于抗体的治疗能够在疾病早期应用于患者将是实现治愈癌症患者目标的关键。
免疫疗法引进/卖出抗体药物偶联物细胞疗法申请上市
2024-09-25
摘要:过继免疫治疗使用嵌合抗原受体(CAR)重定向的T细胞是一种新的治疗范式,它使用一类新的治疗“药物”在某些迄今为止难以治疗的B细胞恶性肿瘤患者中产生完全且持久的缓解。CAR T细胞源自患者自身的免疫细胞,这些细胞在体外通过基因工程改造,带有能够结合特定目标并在目标结合时传递激活信号的CAR。CAR激活细胞毒性T细胞以有效、重复和持久的方式破坏和消除识别的癌细胞。然而,各种障碍限制了CAR T细胞在其他类型的癌症或其他疾病中的广泛应用。目前的挑战包括设计最优的CAR、积极穿透肿瘤病变,并在不诱导对健康组织产生毒性的情况下维持T细胞的抗肿瘤激活。本章回顾了CAR的代际、增强CAR T细胞效力和选择性的策略,以及为日益增多的患者建立高效的制造流程。
1.原型嵌合抗原受体(CAR,T-Body,免疫受体)
在20世纪80年代中期,Steven A. Rosenberg(美国国立卫生研究院)将从黑色素瘤活检中分离并大量体外扩增的肿瘤浸润性淋巴细胞(TILs)重新注入黑色素瘤患者体内时,患者T细胞识别和有效摧毁癌细胞的能力变得显而易见。这些以及随后的发展促使了采用自体免疫细胞治疗肿瘤患者的概念,这些免疫细胞有能力在大量患者中诱导肿瘤退缩和长期缓解。这些扩增的TILs被认为对特定肿瘤抗原具有特异性,并具有迁移能力以进入肿瘤病变;然而,抗原特异性大多仍然未知。
接下来的几年中,为了给患者的T细胞提供明确的靶向特异性,人们付出了巨大的努力;与T细胞受体(TCR)链或重组嵌合抗原受体(CAR)的遗传工程化,证明是成功的策略之一。与TCR不同,CAR是一个复合的、单多肽链跨膜受体,它在目标识别时提供靶向特异性和T细胞激活能力。原型CAR由四个主要结构域模块化组成:在细胞外末端是用于目标识别的单链可变区(scFv)抗体,一个连接到跨膜结构域的间隔区,以及主要来自TCR/CD3ζ或Fcε受体I(FcεRI)的细胞内信号传导结构域,有或没有连接的共刺激结构域(图1)。目标细胞表面的同源抗原的参与启动了CAR工程化免疫细胞的激活,导致持久的T细胞反应。每个CAR结构域都有独特的功能,并对重定向的T细胞激活产生影响;对于每个特定应用,CAR设计需要进行一些调整,以提供优化的靶向和T细胞激活,如下文详细描述。
图1 嵌合抗原受体(CARs)的世界在不断增长。第一代CAR在细胞外域(外域)中拥有抗原结合和间隔基团,在跨膜域中,在细胞内域(内域)中拥有来自CD3ζ或FcεRI γ链的激活基团。第二代CAR除了拥有一个共刺激域之外,第三代CAR在内域中拥有两个共刺激域。第四代CAR(“TRUCK”,“T细胞重定向用于通用细胞因子介导的杀伤”)由第二代或第三代CAR组成,该CAR在CAR信号传导后诱导转基因蛋白的表达。虽然在规范设计中描绘,但已经工程化了大量CAR变体,每种变体都针对不同的应用进行了优化。
原型CAR的基本设计最初由Zelig Eshhar及其同事(魏茨曼科学研究所)提出,他们展示了一个模块化复合受体,最初命名为“T-Body”或“免疫受体”,具有用于结合的抗体衍生结合域和用于T细胞激活的TCR信号域,为工程化T细胞提供了特异性识别和激活。在随后的几年中,引入了许多修改,允许靶向广泛的抗原,并通过各种细胞内结构域发送信号,以启动和重定向定义的免疫细胞功能(表1)。
表 1 CAR构建模块及其替代模块。
EMA(欧洲药品管理局)批准。其他使用其他宿主细胞和不同CAR设计的应用程序也在早期临床试验中越来越多地被研究。
规范的CAR由抗体衍生的结合域、间隔区、跨膜域和细胞内主要及共刺激信号域模块化组成。每个结构域可以通过不同的模块构建,这些模块影响不同的变量,并最终影响T细胞的激活和性能。
CAR工程化的细胞毒性T细胞重定向至癌细胞是该技术研究最多的应用;自体抗CD19 CAR T细胞的过继转移成为美国食品药品监督管理局(FDA)批准的首个基因工程细胞疗法;随后,欧洲药品管理局(EMA)也批准了。使用其他宿主细胞和不同CAR设计的其他应用也越来越多地在早期临床试验中研究。
2.CAR的模块化组成:细胞外CAR结构域
2.1.结合域
抗原结合域传统上由来自小鼠或人类单克隆抗体的单链可变区(scFv)组成。通过短柔性连接子(通常是(Gly4Ser)3肽)将重链(H)和轻链(L)抗体链的可变(V)区域连接起来,形成VH-linker-VL或VL-linker-VH的顺序。甘氨酸残基提供了灵活性,以允许VH和VL正确折叠形成抗原结合口袋,而丝氨酸则为连接子提供了一些溶解性。VH和VL链的空间位置和相互作用可以显著影响亲和力、特异性和溶解性。足够高的结合亲和力对于诱导T细胞激活至关重要;然而,存在一个亲和力上限,超过该上限CAR介导的T细胞激活不会改善,但会导致激活诱导的细胞死亡(AICD)。在CAR的背景下,一些scFvs通过张力信号独立于抗原参与诱导AICD、耗竭和T细胞的终端分化。除了亲和力和细胞表面的抗原密度外,目标表位在抗原内的位置也很重要;通常,靶向膜近端表位比靶向膜远端表位诱导更强的T细胞激活。
通过使用抗体进行靶向,CAR介导的识别是MHC独立的。这在靶向MHC-肽处理和呈递机制有缺陷的肿瘤时是有益的。此外,通过抗体识别目标,还可以识别传统T细胞看不见的抗原,如碳水化合物、脂质或抗原的结构变体。规范的CAR识别目标细胞表面的抗原;也可以通过使用特异性针对定义的MHC-肽复合物的抗体,工程化MHC-肽识别CAR,使其能够感知由MHC呈递的细胞内抗原。例如,一个scFv识别HLA-A2背景下的NY-ESO-1肽的CAR提供了与相应TCR类似的TCR样识别目标。
2.CAR的模块化组成:细胞外CAR结构域
2.2.间隔区
原型CAR经常在抗原结合域和跨膜域之间包含一个“间隔区”,以便接近目标抗原;连接的铰链区提供了一定的灵活性。间隔区的类型和长度对于最佳目标结合和信号传递至关重要。间隔区并非必需,因为有些CAR在scFv直接融合到跨膜域时是活跃的,而其他CAR只有在具有一定长度的间隔区时才活跃。间隔区通常来源于IgG1或IgG4恒定域或来自细胞外CD28、CD4或CD8(图2)。一般的想法是,间隔区在工程化T细胞和相应目标细胞之间提供最佳距离,以允许与目标细胞形成有效的接触区。基于TCR-MHC相互作用的知识,人们普遍认为CAR-目标相互作用需要在T细胞和目标细胞之间创建约15纳米的距离,以最佳形成接触区。因此,针对膜近端表位需要较长的间隔区,而较小的间隔区对更远离膜的表位是最佳选择;通过使用不同长度的间隔区可以轻松调整距离。在这个背景下,IgG衍生的间隔区具有可以通过结合一个、两个或三个CH1-CH2-CH3部分来调整长度的优势。IgG1衍生的间隔区还有利于CAR分子的稳定;然而,它可能与髓系细胞上的Fcγ受体(FcγR)(CD64)结合,介导CAR T细胞和髓系细胞的“非肿瘤”激活。这可以通过删除间隔区内的IgG1 CH2域或通过删除IgG1 Fc受体结合部分内的Asn297糖基化位点来预防。类似的修改也可以引入到IgG4间隔区。
图 2 第二代CAR设计的变体。由于模块化组成,可以使用各种替代域来构建CAR,其中一些示例性地列出。各个组分的变化允许调节CAR的结合和信号传导,最终调节细胞功能、代谢和工程化T细胞的抗肿瘤活性。其他变体旨在提高结合亲和力、目标的可及性、信号强度和细胞膜上的持久性等。最后,安全预防措施导致CAR设计中进一步的修改。
2.3.跨膜区
典型CAR的跨膜区来源于如CD3ζ、CD4、CD8α、CD28或OX40等类型1跨膜蛋白,由20-23个疏水性氨基酸组成,富含亮氨酸、异亮氨酸和缬氨酸(图2)。带有CD3ζ跨膜域的CAR似乎比其他CAR更有效地整合到TCR/CD3复合体中,因此在表达和信号传导方面更为稳健;带有CD28跨膜区域的CAR似乎同样稳定。另一方面,带有CD8α铰链和跨膜域的CAR不易于AICD;然而,它们通过减少促炎细胞因子的释放来介导较少的T细胞激活。
2.4.细胞内信号传导域
“第一代”CAR完全通过主要信号传导域(信号-1)进行信号传导。TCR/CD3ζ细胞内链含有三个免疫受体酪氨酸激活基序(ITAMs),FcεRI γ链含有一个ITAM,这些在磷酸化后作为下游信号蛋白的特定适配器。因此,CAR利用内源性TCR信号机制来启动T细胞激活事件的级联。下游激酶如Lck或Fyn也可以作为CAR介导的T细胞激活的主要信号,等等(图2)。CAR信号传导域本身足以与下游激酶结合并启动有效的激活级联,因为CAR在TCR敲除细胞和非T细胞如NK细胞中也是功能性的。然而,仅有主要信号的CAR不足以激活以允许长期持久;这样的CAR T细胞迅速进入凋亡。根据“双信号假说”,静息T细胞还需要一个共刺激信号以持续激活。这就是将主要信号与共刺激信号(信号-2),如CD28或4-1BB(CD137),结合在“第二代”CAR中的理由。也在临床前和临床上探索带有替代共刺激域的CAR,如OX40、ICOS、CD27、CD40-MyD88、CD2和CD244。为了方便下游激酶的接近,CD28通常位于膜近端位置,随后是远端位置的CD3ζ;OX40和4-1BB在膜远端和近端位置都活跃。与第一代CAR相比,第二代CAR T细胞在细胞因子释放、扩增和抗肿瘤活性方面显示出稳健和持久的反应。
CAR介导的共刺激以不同的方式影响T细胞效应功能、存活、持久性和代谢。例如,4-1BB CAR T细胞在患者血液中的持久性超过6个月,而CD28 CAR T细胞在3个月之后大多无法检测到。经过重复刺激后,CD28 CAR T细胞重新编程为CD45RO+ CCR7−效应记忆细胞,这些细胞随后需要OX40来延长持久性并避免快速耗竭;4-1BB CAR T细胞主要转化为CD45RO+ CCR7+中央记忆细胞,并在外围血液中长期持久。CD28 CAR信号激活PI3K/Akt/mTOR途径,刺激有氧糖酵解,增加葡萄糖摄取和ATP生成,而4-1BB CAR信号激活Wnt/β-catenin途径和脂肪酸氧化,增加代谢和线粒体呼吸链能力。典型的Wnt/β-catenin有利于中央记忆细胞的形成和T细胞的长期存活,而CD28诱导的PI3K/Akt信号维持效应细胞的即时响应。在高剂量下,CD28和4-1BB CAR T细胞都能在临床前模型中根除大型已建立的肿瘤;在低剂量下,CD28 CAR T细胞比4-1BB CAR T细胞表现出更大的耗竭程度,结果是4-1BB CAR T细胞在长期内更有效地根除大型肿瘤负荷。另一方面,带有4-1BB CAR的T细胞仍然对肿瘤介导的通过TGF-β的抑制敏感,这对CD28 CAR T细胞来说较少见。因此,选择CAR设计的标准取决于多个参数,包括T细胞持久性、抗抑制能力、共刺激和共抑制配体的模式、肿瘤细胞上的抗原密度、T细胞上的CAR密度等。
“第三代”CAR结合两个共刺激域以及主要激活信号。联合共刺激的好处只在少数情况下得到证明,例如,通过CAR提供CD28-OX40共刺激对T细胞在终端成熟中的进展有益。
3.TRUCK:“第四代”CAR T细胞
CAR T细胞可以用来按需将转基因蛋白输送到预定的、靶向的组织。因此,CAR T细胞被设计成带有CAR诱导表达盒的额外“有效载荷”。所谓的“第四代”CAR T细胞,即TRUCKs(“T细胞重定向用于通用细胞因子介导的杀伤”),旨在在靶向组织中沉积分泌型转基因蛋白,以实现治疗有效浓度(图3)。“有效载荷”的表达受NFAT6-IL-2最小启动子的控制,该启动子在CAR信号传导时被激活;有效载荷可以是转基因编码的任何蛋白或肽。这种策略特别有趣,因为它结合了重定向CAR T细胞攻击和局部沉积的生物活性蛋白的作用,同时避免了系统毒性。只要CAR T细胞保持激活状态,TRUCKs就会沉积转基因产物,例如,IL-12或IL-18作为转基因免疫调节剂,以特定方式塑造靶向肿瘤环境,而不引起系统毒性。累积的TRUCK产生的IL-12在CAR靶向的肿瘤组织中招募天然免疫细胞,如NK细胞和巨噬细胞,在那里反过来启动二次抗肿瘤免疫反应。IL-12 TRUCKs抵抗Treg细胞的抑制,并显示出增加的细胞因子释放和扩增。当快速进展的肿瘤积累抗原丢失的癌细胞,导致对CAR T细胞不可见的肿瘤复发时,这种策略特别有趣。释放IL-18的TRUCKs将CAR T细胞转化为T-bet高FoxO1低效应细胞,抵抗耗竭并显示出对大型已建立肿瘤的优越细胞毒性。IL-18 CAR T细胞治疗改变了整个肿瘤免疫细胞景观,特别是通过增加CD206− M1型巨噬细胞和NKG2D+ NK细胞的数量,减少抑制细胞如Tregs、抑制性CD103+ DCs和M2型巨噬细胞。其他例子包括释放过氧化氢酶以保护T细胞免受过氧化压力介导的抑制和释放肝素酶以改善T细胞通过肿瘤基质的穿透。
图 3 第四代CAR T细胞(“TRUCKs”)。在抗原结合时,第二代或第三代CAR诱导表达一种转基因蛋白,该蛋白在细胞内作用、整合到膜中或由CAR T细胞释放。释放的转基因蛋白旨在改变肿瘤环境、重塑肿瘤组织或吸引二次免疫反应。CAR T细胞被诱导仅在CAR与其靶标结合时释放蛋白质,从而将“有效载荷”在预定义的交付点作为“TRUCK”进行交付。这种CAR T细胞被理解为“活体工厂”,用于精确和持续地交付治疗性细胞产品。
所谓的“装甲CAR”通过产生4-1BB配体提供增加的共刺激通过刺激4-1BB途径。工程化的T细胞被设计为分泌Toll样受体(TLR)配体,可以刺激T细胞和抗原呈递细胞上的TLR途径,然后可以激活一组T细胞进行广泛的抗肿瘤攻击。靶向Muc16ecto(即黏蛋白-16(CA-125)的膜保留残余物)并分泌IL-12的CAR T细胞正在临床试验中评估(NCT02498912)。IL-15 TRUCK细胞显示出改善的扩增和抗肿瘤活性,但在未受控制的扩增情况下需要自杀基因,由于其白血病潜力。“装甲”CAR通过与CAR共表达IL-7受体-α链来恢复对IL-7的反应性,并促进Th1反应。类似地,在IL-4水平增加的前列腺癌中,共表达IL-4结合/IL-7信号传导受体提高了抗PSCA CAR T细胞的抗肿瘤活性。另一方面,CAR T细胞上共表达的显性负性TGF-β DNRII受体可以在TGF-β存在的情况下与TGF-β竞争,以改善T细胞的抗肿瘤活性。也可以设想提供细胞因子或细胞因子受体之外的应用,如输送可溶性HVEM外域,以靶向肿瘤血管,以维持肿瘤穿透。
4.具有双重特异性、组合抗原识别和条件性CAR的CAR T细胞
原型CAR通过一个scFv将特异性重定向到一个抗原;多种原因要求具有多重特异性的CAR:(1)肿瘤病变在可靶向抗原方面可能是异质的,或在肿瘤进展过程中丢失抗原;(2)靶向癌细胞和肿瘤基质或血管可能有益或需要增加治疗效果。将两种或更多CAR T细胞产品应用于癌症患者基本上是可行的,尽管需要在GMP条件下制造两种细胞产品。例如,通过顺序输注应用CD19和CD22 CAR T细胞目前正在评估治疗难治性B-ALL的试验中(NCT03620058)。或者,T细胞被设计为表达两个CAR,即所谓的双顺反子CAR,每个CAR针对不同的抗原(图4)。通过灵活的连接子将两个scFv相互连接,设计出具有双重特异性的CAR。这种串联排列的双特异性CAR(“串联CAR”,“Tan-CAR”)或环状结构,针对两种不同的抗原,并能够在结合任一抗原时提供T细胞激活(“或”门控);具有其中一种相应抗原的目标细胞仍然被识别。除了两个连接的scFv外,双抗体、二合一抗体和双变量域抗体也可以用来设计具有两种特异性的CAR。三特异性CAR包含单价和/或多价CAR结构的组合,以针对三种抗原,进一步扩大靶向特异性。一个例子是设计了一种双特异性CAR,将针对CD20和CD19的scFv连接起来,旨在减轻在接受CD19 CAR T细胞治疗后经常发生的B细胞白血病/淋巴瘤的复发。CD19− CD20+白血病细胞的复发旨在通过CD20-CD19双特异性CAR T细胞得到控制。双特异性CAR中scFv的顺序取决于特定抗原中目标表位的空间可及性。CD20-CD19 CAR对CD19和CD20都具有相同的结合能力,并重定向T细胞激活,而CD19-CD20 CAR则效率要低得多。其他双特异性CAR的例子是针对CD19和CD123治疗B-ALL或CD19共靶向CD22、ROR1和免疫球蛋白κ轻链(Igκ)。多特异性CAR T细胞目前正在早期临床试验中评估。通过双顺反子表达盒设计了同时具有CD19和CD22 CAR的T细胞,正在进行治疗高风险B-ALL或干细胞移植后复发的试验(NCT03289455)。具有CD19和CD22特异性的双价CAR正在评估治疗B-ALL或B细胞淋巴瘤(NCT03241940, NCT03233854, NCT03330691, NCT03448393, NCT03019055)。目前正在进行的II期试验中评估了针对BCMA两个表位的双特异性CAR(NCT03758417)。
图4 基于逻辑门控的CAR介导的T细胞激活,以证明在肿瘤靶向中的选择性。共表达两种CAR,每种CAR在与相应的目标抗原结合时都能完全激活T细胞;双特异性CAR(串联CAR,Tan-CAR)也是如此。在这种情况下,通过表达抗原A或B或两者的细胞激活T细胞("OR"门控)。为了仅通过同时表达A和B抗原的细胞激活CAR T细胞,识别A的CAR仅通过CD3ζ提供基本激活,这不足以实现完全和持续的激活,而识别B的CAR提供共刺激;通过两种CAR的同时信号传导诱导T细胞完全激活("AND"门控)。识别抗原A的synNotch CAR驱动转录并表达第二种CAR,该CAR在识别抗原B时驱动T细胞完全激活。具有ITIM(免疫受体酪氨酸基抑制基序)的抑制性CAR在其识别的抗原B结合时阻止通过激活CAR的信号传导。当抗原B不存在时,CAR可以在结合抗原A时激活T细胞("A-not-B"门控)。
当结合两种抗原时,双特异性CAR比单特异性CAR具有更高的亲和力,理论上稳定了突触并改善了T细胞对低抗原水平目标细胞的反应。这种情况可以用来只将CAR T细胞重定向到表达两种抗原而不是一种的细胞(图4)。这种“与”门控的抗原模式旨在提高对癌细胞的靶向选择性,同时保留健康细胞。两个共表达的抗原被两个共表达的CAR识别,每个CAR识别特定的抗原,并分别提供主要或共刺激信号。这样,只有同时结合两种抗原才提供完全T细胞激活所需的两个信号;结合一种抗原是不足够的。组合抗原识别的例子是,通过CD3ζ CAR靶向ErbB2和通过CD28 CAR靶向Muc1,或通过CD3ζ CAR靶向间皮素和通过CD28 CAR靶向叶酸受体-α。靶向CD13和TIM3的双特异性和分裂CAR T细胞在临床前模型中根除患者衍生的急性髓性白血病细胞,减少了对骨髓和外周髓性细胞的毒性。
通过异二聚体化两个多肽链,可以加强两个CAR上的初级和共刺激信号的组合;一个链由细胞外和跨膜以及初级信号传导部分组成,第二个链提供共刺激信号传导部分,并通过添加“二聚体化剂”与第一个链相连。CAR在二聚体化剂允许异二聚体化和功能性CAR形成之前保持沉默。通过滴定二聚体化剂剂量可以微调T细胞活性;撤除二聚体化剂终止CAR信号。只有当每个CAR信号单独不足以驱动T细胞激活时,才能通过组合抗原识别实现清晰的“开-关”T细胞激活。由于预先激活的T细胞中的CD3ζ信号可能重新诱导T细胞反应,因此需要调整信号或降低结合亲和力以实现平衡的激活阈值。
可调CAR的另一种策略基于合成Notch(synNotch)受体。Notch由一个细胞外受体、一个跨膜域和一个细胞内转录调节器组成,激活后介导内部域的蛋白水解,释放细胞内转录调节器。这些特性用于控制与Notch受体不同特异性的真正CAR的转录。优点在于Notch受体的抗原识别基于逻辑“与”门控,并以空间定义的方式控制CAR T细胞功能。在CD19结合后,CD19特异性synNotch受体释放转录效应域Gal4-VP64或TetR-VP64以诱导抗间皮素CAR的表达。只有当在靶向组织中同时识别synNotch配体和CAR配体时,T细胞才被激活。另一个例子是通过CAR靶向ROR1和通过Notch受体靶向EpCAM或B7-H3。虽然CAR的“开开关”决定了靶向癌细胞的选择性,但这种策略可能受到诱导足够水平的CAR表达和在没有Notch信号进一步发生时衰减CAR所需的时间的限制。
工程化T细胞的TCR特异性也可以用来提供更复杂的识别轮廓。带有γδ TCR的T细胞识别肿瘤细胞特有的磷酸化抗原;转基因表达GD2特异性CAR和共刺激域只会在γδ TCR和CAR同时结合它们相应的抗原时提供完全的T细胞激活;由于缺乏γδ TCR激活,不会攻击GD2+的健康细胞。
虽然许多可靶向的抗原既表达于健康细胞也表达于癌细胞,但有些抗原仅由健康细胞表达,而癌细胞缺乏表达。在这种情况下,结合共同抗原“A”但在结合健康细胞上的抗原“B”时阻断,将阻止CAR T细胞激活对抗健康细胞(图4)。带有ITIM(免疫受体酪氨酸基抑制基序)的抑制性CAR只要结合其相应的抗原“B”,就阻止通过激活性CAR的信号传导。结合缺乏抗原“B”的“A”癌细胞允许CAR T细胞激活,因为缺乏通过抑制性CAR的信号传导(“A非B”门控)。
5.具有植入多重抗原特异性的通用CAR
目前,原型CAR具有一个确定的抗原特异性;改变特异性需要用新的CAR工程化T细胞。在这种情况下,开发了一种“通用”CAR,它识别一种抗体,该抗体转而提供癌症特异性(图5)。例如,抗癌抗体的免疫球蛋白Fc区域被具有CD16作为结合域的CAR结合。CD16 CAR T细胞结合抗癌抗体,从而获得对癌细胞的特异性。或者,CAR结合至与抗癌靶向抗体相关联的蛋白质表位。具有荧光素异硫氰酸酯(FITC)特异性CAR的T细胞识别FITC标记的叶酸,该叶酸与叶酸受体阳性癌细胞结合。也可以设想将其他表位与桥接抗体相关联,如亲和素。同时添加不同特异性的抗体,允许将相同的CAR T细胞产品(“UniCAR”)重定向至多种抗原,无需重新制造CAR T细胞。该策略的优点是同时使用不同的抗体靶向广泛的抗原,同时只应用一种制造的CAR T细胞产品。实际的特异性由应用的抗体混合物在治疗足够浓度下定义。随着应用的抗体的短半衰期,此外,意外的不良事件在抗体撤除后很快就会有限。从机制上讲,有效的肿瘤控制需要CAR T细胞和连接抗体都渗透到肿瘤病变中;目前尚不清楚这是否适用于晚期实体瘤。也尚未解决“通用”CAR T细胞是否能够建立对癌症抗原的持久免疫记忆,这被认为是长期控制癌症所需的。
图 5 “通用”CAR的概念。T细胞表达一种特异性针对标签的CAR,该标签与连接分子相连,最好是天然抗体、单链抗体(scFv)或双特异性T细胞导向抗体(BiTE),这些分子能够识别肿瘤细胞上的目标抗原。通过添加不同的连接分子,无需工程化新的CAR T细胞,就可以为T细胞配备不同的特异性。这被认为在将CAR T细胞应用于患者后也是可行的;注入针对不同肿瘤抗原的抗体,为CAR T细胞提供不同的特异性。
6.转换抑制信号为激活信号的Switch CAR
在肿瘤病变中,重定向的T细胞攻击通常以各种方式受到抑制;抑制性配体如程序性细胞死亡配体-1(PD-L1)和PD-L2与激活的T细胞表达的程序性细胞死亡-1(PD-1)结合。一种结合这种抑制性配体但向工程化T细胞传递激活信号的CAR,不仅可以与抑制性受体竞争结合,还可以通过提供激活信号克服抑制(图6a)。理想情况下,PD-L1:CD28 “开关”CAR在工程化T细胞中克服PD-1介导的抑制信号。特别是,一个具有PD-1细胞外域结合PD-L1和CD28细胞内信号传导域的CAR,将抑制信号转换为激活信号,导致ERK磷酸化增加,促炎细胞因子释放,T细胞扩增和目标细胞的细胞溶解。由TIGIT(具有Ig和ITIM结构域的T细胞免疫受体)的外域与CD28共刺激域融合而成的嵌合受体,在结合TIGIT配体CD155时增强T细胞功能。鉴于肿瘤组织提供的大量抑制信号,确定需要克服的“关键”抑制因素以维持有效的T细胞反应仍然是一个挑战。
图 6 开关CAR和抑制性CAR(iCAR)。(a) 开关CAR与生理性T细胞抑制性受体的配体结合,但为工程化T细胞提供激活信号。(b) 抑制性CAR在与抗原结合后,通过ITIM信号向工程化T细胞提供负信号。抑制信号压倒了通过TCR或共表达的激活CAR的激活。
7.抑制性CAR:iCARs
虽然原型CAR向工程化T细胞提供激活信号,但具有抑制信号的CAR旨在在结合健康细胞时抑制CAR T细胞激活。理想情况下,抑制性CAR通过在面对健康组织时覆盖激活CAR信号来减轻非肿瘤毒性。与激活性、肿瘤特异性CAR共表达的具有优势抑制信号的CAR,识别健康细胞;从而CAR T细胞只在结合癌细胞时激活,抑制性CAR不结合健康细胞(图6b)。这种抑制性CAR提供PD-1或CTLA-4信号,并覆盖癌症特异性CAR的激活信号。
8.异体CAR T细胞和CAR NK细胞
到目前为止,CAR T细胞治疗是一种通过体外制造患者自己的T细胞的个性化治疗。这不仅繁琐、成本密集和耗时,而且在患者晚期疾病无法提供足够或足够活跃的T细胞进行CAR工程化时通常也不适用。在这种情况下,异体“现成的”CAR T细胞将为广泛的患者群体带来好处。为了避免移植物抗宿主病(GvHD),需要删除内源性的αβ TCR和HLA分子,这可以通过锌指核酸酶或CRISPR/Cas技术实现。随后清除剩余的TCRαβ T细胞,通过污染的异体TCR+细胞降低GvHD风险。T细胞通过转录激活样效应核酸酶(TALENs)技术在TCRα和CD52位点进行基因编辑,用于治疗无法生产自体CAR T细胞的患者的儿童CD19+ ALL。CD52存在于患者的恶性B细胞上,需要从CAR T细胞中删除,以允许消除恶性淋巴细胞,同时保留注入的CD52阴性CAR T细胞。对于工程化异体CAR T细胞,CRISPR导向RNA和Cas9目前由病毒载体编码以实现组成性表达;当前的研究旨在短暂提供基因编辑工具,而不持久的载体,以最小化非目标编辑。
针对BCMA治疗多发性骨髓瘤的异体CAR T细胞,通过BCMA CAR和基因编辑技术进行了改造,以限制TCR介导的免疫反应。通过将CD20模拟表位整合到CAR的细胞外域,使CAR T细胞能够通过利妥昔单抗消除,从而提供了异体BCMA CAR T细胞的安全性。
关于使用异体效应细胞,NK细胞也可以用于诱导有效的抗肿瘤反应,因为它们具有细胞毒性潜力和分泌促炎细胞因子。除了使用异体细胞,使用NK细胞进行癌症的过继细胞治疗有很强的生物学理由;NK细胞表现出广泛的抑制性和激活性受体库,以识别外来、感染或恶性细胞。两种信号的平衡最终诱导或阻断细胞毒性CD56dim NK细胞释放细胞毒性颗粒以杀死目标细胞。虽然可能存在广泛的NK细胞亚群多样性,基于激活和抑制受体的库,但通过CAR工程化NK细胞将为特定癌细胞提供预定的特异性。原型CAR具有CD28-CD3ζ信号也在NK细胞中活跃;具有NK细胞2DS2和DAP12信号蛋白的CAR产生了更强的抗肿瘤活性。为NK细胞工程化的CAR通常包含DAP10或DAP12用于激活,单独或与CD3ζ一起。具有NKG2D作为结合物和DAP10-CD3ζ用于激活的CAR有效地激活了小鼠模型中针对骨肉瘤的原代NK细胞。CD3ζ在NK细胞中作为激活域优于DAP10,而DAP12优于CD3ζ。
9.制造CAR T细胞用于临床应用
对于临床应用,CAR T细胞产品是根据良好生产规范(GMP)规则,使用预期接受患者的自体T细胞制造的(图7)。在大多数情况下,通过白细胞分离术收集血液,分离T细胞,通过病毒感染或电穿孔进行基因工程改造,并扩增到临床相关的数量。大多数临床试验使用通过γ-逆转录病毒或慢病毒基因转移修饰的T细胞;基于转座子的载体,如Sleeping Beauty和PiggyBac,越来越多地应用于临床,其好处是避免了成本和时间密集型的病毒生产。病毒和转座子介导的基因转移程序旨在永久性地修改患者的T细胞以表达CAR;一些试验使用通过RNA电穿孔修饰的T细胞进行短暂的CAR表达。在永久性基因改造后,插入突变和随后成熟T细胞的致癌转化的风险似乎很低,到目前为止在这方面还没有报告致癌事件。一个需要注意的问题是,通过慢病毒转移,CAR基因插入到Tet2位点导致T细胞的克隆扩增,然而,它们自发地收缩了。然而,白细胞分离产品中污染的恶性细胞也可能意外地被CAR改造,存在重新输注给患者后通过CAR介导的肿瘤促进的风险。
图7 CAR T细胞制造和患者治疗时间表。(a) 通过白细胞分离术从患者体内收集T细胞,并在体外处理以获得最终的CAR T细胞产品,包括T细胞工程化以携带CAR、扩增至临床相关数量,以及最终的质量控制程序(QC)。在输注CAR T细胞产品之前,患者需接受非清髓性淋巴细胞减少(“预处理”),以促进CAR T细胞的植入和体内扩增。随后需要院内护理以管理潜在的副作用,如CRS或神经毒性。(b) 体外CAR T细胞制造过程通常从白细胞分离产品开始,并涉及多个后续生产步骤,包括T细胞分离和激活、基因工程、CAR T细胞扩增、制剂、CAR T细胞产品的冷冻保存,以及最终的质量控制以供释放。整个过程可以手动运行,或在监督下(半)自动化进行。
经过基因改造后,CAR T细胞在细胞因子存在的情况下在体外广泛扩增到临床相关的细胞数量;目前使用手动处理的摇动反应器或袋子以及完全自动化和监督处理设备。自动化的目标是允许以高再现性和质量进行生产,并从越来越多的患者中并行生产细胞,并缩短静脉到静脉的时间。
最适合CAR治疗的T细胞群体被认为是具有急性炎症特征的原始或年轻中央记忆细胞。在IL-2存在下扩增CAR T细胞优先触发效应T细胞,而IL-7或IL-2加IL-15扩增具有持续细胞因子释放和抗肿瘤活性能力的中央记忆T细胞。添加IL-21使CAR T细胞保持较少分化状态。刺激方式不仅决定了扩增CAR T细胞的产量,还决定了代谢依赖性;IL-15增加氧化代谢以及肉碱棕榈酰转移酶,这是脂肪酸氧化的限速步骤。IL-7通过STAT5和Akt激活增加Glut1,并诱导甘油运输和甘油三酯合成,从而改善T细胞持久性和存活。在体外扩增期间抑制Akt触发具有高水平脂肪酸氧化的中央记忆表型,最终改善CAR T细胞的抗肿瘤活性。CD45RO+ CD62L+记忆CAR T细胞比更高级分化阶段的效应T细胞提供更持久的抗肿瘤反应,使富含CD62L的CAR T细胞成为进一步探索的有吸引力的选择。
因此,中央记忆CAR T细胞在临床应用中似乎更优越,因为响应的患者没有累积具有早期记忆和耗竭特征的T细胞,而非响应的患者则累积了。最终产品中工程化细胞的活性可能影响治疗效果。然而,基于制造的细胞产品的活性对CAR T细胞治疗结果的首次回顾性分析表明,当患者接受70-80%活性的产品与至少80%活性的产品相比,CD19 CAR T细胞扩增或患者存活没有差异的证据。
制造T细胞产品是一种个性化方法,当前程序有一些显著的限制:
一些癌症患者淋巴细胞减少或具有低数量的原始T细胞,导致生产延迟或失败,如在为儿科患者生产时所经历的。
生产过程耗时,这对急性或晚期疾病的患者不利。
由于疾病,患者的T细胞可能功能失调,如CLL和一些实体瘤所报告的,导致产品反应率低。
在某些情况下,工程化异体T细胞可能是另一种策略。在接受造血干细胞移植的患者中,使用移植的异体T细胞制造CAR T细胞产品。这样的异体CD19特异性CAR T细胞诱导了部分和完全缓解;然而,一些患者遭受了GvHD。病毒抗原特异性、部分HLA匹配的供体T细胞缺乏异体反应性,并且通过CAR工程化,显示出抗淋巴瘤活性。NK细胞以其MHC独立活性也是第三方供体细胞CAR工程化的来源;然而,它们在患者中表现出较差的持久性。
10.通过CAR T细胞的过继治疗在血液学恶性肿瘤中诱导持久缓解
过继转移CAR T细胞的治疗效果取决于多个参数,包括CAR设计、CAR信号传导、结合亲和力、目标细胞上的抗原数量、目标抗原表位的空间可及性、T细胞的成熟阶段、CAR T细胞的持久性和扩增、患者免疫系统的预处理等。目前的努力旨在优化特定疾病的状况;一些治疗方案已在CAR T细胞治疗恶性疾病的方面证明成功,特别是B细胞白血病/淋巴瘤;少数试验旨在治疗实体癌。
在迄今为止难以治疗的B细胞白血病和淋巴瘤的治疗中,使用“第二代”抗CD19 CAR T细胞的早期临床试验实现了完全且持久的缓解;使用“第一代”CAR T细胞的治疗大多失败,因为CAR T细胞从循环中迅速清除。目前,近600项早期阶段的CAR T细胞试验正在进行临床探索,主要由学术中心进行(截至2020年初,中国有268项,美国有227项,欧洲有67项)。用于治疗儿童B-ALL(Kymriah™,tisagenlecleucel,诺华)和成人大B细胞淋巴瘤(Yescarta™,axicabtagene ciloleucel,Kite-Gilead)的抗CD19 CAR T细胞已获得FDA和EMA的批准;其他将很快跟进。
CAR T细胞治疗的标准程序从患者的白细胞分离开始,分离T细胞,体外基因工程改造相应的CAR,CAR T细胞扩增,以及在非清髓性淋巴细胞减少和IL-2支持后,通过静脉输注将最终的细胞产品重新给患者(图7)。由于CAR T细胞的持久性对临床效果至关重要,目前在试验中使用的CAR具有一个或两个共刺激内域,其中大多数提供CD28或4-1BB共刺激。在持久性方面,4-1BB共刺激的CAR T细胞似乎优于CD28 CAR T细胞,在循环中持续4年以上,而CD28 CAR T细胞持续30天。由于CD19 CAR T细胞不区分健康和恶性B细胞,只要CD19 CAR T细胞持续存在,患者就会经历持久的B细胞耗竭。尽管B细胞耗竭在临床上是可管理的,但这种情况要求在靶向恶性B细胞时更具选择性。最近,Fcμ(IgM)受体被确定为治疗慢性淋巴细胞白血病(CLL)时可能更具肿瘤选择性的目标,由于目标表达水平较低,因此大多数健康B细胞免于被淘汰。目前也在探索其他替代靶标。
在缓解期间,大多数接受4-1BB CAR T细胞治疗的白血病/淋巴瘤患者没有接受进一步的癌症特异性治疗;接受CD28 CAR治疗的患者经常接受异体干细胞移植,这似乎是有益的,因为CD28 CAR T细胞的持久性不如4-1BB CAR T细胞。需要进一步探索以确定长期内更成功的策略。
迄今为止,患有DLBCL、CLL、B细胞急性淋巴细胞性白血病(B-ALL)和滤泡性淋巴瘤的患者已通过CD19 CAR T细胞成功治疗。值得注意的是,接受CD19 CAR T细胞治疗的多发性骨髓瘤患者也经历了缓解,尽管通过流式细胞术评估,骨髓瘤细胞是CD19low或CD19阴性。目前也在探索用于治疗B细胞恶性肿瘤的其他替代靶标,包括CD20、CD22、Igκ轻链、ROR-1和CD30。
由于缺乏标准化的试验设计、CAR组成、靶向抗原、预处理等方面,很难比较各种试验中CAR T细胞治疗的成功。然而,越来越明显的是,CAR T细胞剂量和淋巴细胞减少的程度或淋巴细胞减少方案对于允许广泛的T细胞扩增、持久性和最终治疗效果至关重要。应用后对CAR T细胞的重复再刺激可能改善它们在长期内的持久性和抗肿瘤效果。这是使用病毒特异性T细胞进行CAR植入的合理性,它们在接触病毒抗原时通过TCR重复再刺激;例如,Epstein-Barr病毒(EBV)特异性T细胞通过CAR工程化,并被EBV感染的细胞触发扩增。事实上,EBV特异性CAR T细胞的表现优于没有病毒特异性的CAR T细胞。
11.治疗实体癌的CAR T细胞面临的挑战
虽然血液学恶性肿瘤的治疗越来越成功,但实体癌的治疗仍然具有挑战性(表2)。作为“活药”的CAR T细胞基本上非常适合治疗实体癌,特别是由于T细胞固有的迁移和组织穿透能力,穿透血脑屏障,并在几乎所有组织中积累,包括睾丸和眼睛等特权组织,因此特别适合消除(微)转移。然而,大多数实体肿瘤具有大量策略,以非常有效的方式对抗CAR T细胞的迁移、渗透和激活。其中,改变的趋化因子环境损害了CAR T细胞向肿瘤的迁移;肿瘤内皮细胞上丢失了一些粘附因子,妨碍了T细胞的渗透。通过局部沉积TNF-α可以对抗后者,它增加了血管粘附分子,如血管细胞粘附蛋白-1和内皮细胞上的细胞间粘附分子-2。靶向血管内皮生长因子(VEGF)受体-2或阻断迁移抑制因子如内皮素B受体也改善了内皮细胞粘附和/或T细胞的跨内皮迁移。在T细胞上下调的趋化因子受体被重新表达,如CXCR2(CXCL1受体),以便于靶向黑色素瘤或CCR2b用于靶向神经母细胞瘤。
表 2 CAR T细胞疗法面临众多挑战。
为了绕过迁移障碍,CAR T细胞被瘤内植入或分别注入胸膜或腹膜以治疗间皮瘤和卵巢癌。通过内窥镜将抗CEA CAR T细胞应用于肝转移;抗c-Met CAR T细胞被注入乳腺癌转移。一旦进入肿瘤病变,CAR T细胞需要突破基质细胞和细胞外基质的障碍,才能接近癌细胞以执行它们的细胞毒性攻击。通过基因工程释放的肝素酶在基质中降解肝素硫酸蛋白多糖,改善T细胞的渗透;需要高水平的IFN-γ来消除基质细胞并根除大型已建立的肿瘤病变。通过直接针对基质细胞的CAR T细胞特异性针对成纤维细胞激活蛋白(FAP),一种参与细胞外基质重塑的丝氨酸蛋白酶,整体抗肿瘤活性得到改善。
许多过程使肿瘤病变对重定向的CAR T细胞产生敌意,使它们变成耗竭状态或进入凋亡。调节性T(Treg)细胞、髓源性抑制细胞(MDSCs)和肿瘤相关M2型巨噬细胞释放抑制性细胞因子,如IL-4、IL-10、白血病抑制因子(LIF)和TGF-β。MDSCs和巨噬细胞降低肿瘤内色氨酸水平;基质细胞释放吲哚胺2,3-双加氧酶(IDO)和犬尿氨酸,抑制T细胞效应功能并剥夺组织中的葡萄糖和其他营养物质。严重的酸中毒也对抗肿瘤活性的CAR T细胞产生反作用。由于MDSCs释放的精氨酸酶,低精氨酸水平抑制CD3ζ表达和TCR信号传导。
12.CAR T细胞治疗与毒性相关
作为“活药”的CAR T细胞治疗在一些试验中取得了显著的治疗效果;然而,CAR T细胞在初始应用后的几天甚至几周内可能导致严重的副作用,需要重症监护干预,甚至可能致命。大多数毒性是由于CAR T细胞的特殊生物学特性,其他与CAR T细胞相关的毒性目前尚未完全理解。从机制上讲,主要毒性是(1)由于大量T细胞激活、细胞因子释放和肿瘤溶解引起的全身毒性,以及(2)由于CAR T细胞与健康组织相互作用引起的特异性毒性(“靶上非肿瘤”毒性)。
12.1.系统性毒性
细胞因子释放综合征(CRS):大量CAR T细胞与目标细胞的结合导致大量细胞因子释放,血清中促炎细胞因子(包括IFN-γ和TNF-α、IL-10和IL-6)的水平异常高,这本身会导致其他免疫细胞的交叉激活,以及进一步的细胞因子释放,直至达到有毒水平。这些毒性被称为细胞因子释放综合征(CRS),临床上伴有高烧、不适、疲劳、肌肉痛、恶心、厌食、心动过速、低血压、毛细血管渗漏、心脏功能障碍、肾功能损害、肝功能衰竭和弥散性血管内凝血。CRS常与血管渗漏综合征(VLS)一起出现,与巨噬细胞激活综合征(MAS)和巨噬细胞激活密切相关,临床上类似于噬血细胞性淋巴组织细胞增多症(HLH)。CRS的风险与T细胞激活和扩增有关,这可能与总体肿瘤负荷相关,但并非绝对。为了避免CRS,需要在肿瘤负荷高的患者中使用较低剂量的CAR T细胞,这是一个需要通过精确定义治疗窗口来解决的悖论,通过调整T细胞激活、细胞因子释放和抗肿瘤活性。
CRS的早期诊断和临床管理通过新建立的评分系统和治疗指南得到便利。C反应蛋白,即由肝细胞在IL-6水平增加时释放的蛋白质,目前作为CRS发作和严重程度的实验室标志物;成人的预测标志物还包括可溶性gp130(sgp130)、IFN-γ和IL-1Rα的增加,在儿科患者中,IFN-γ、IL-13和MIP1α的增加。目前CRS的治疗基于阻断IL-6/IL-6受体信号轴,通过阻断抗体如抗IL-6受体抗体tocilizumab或抗IL-6抗体siltuximab,这似乎不会干扰CAR T细胞的疗效。短期系统性皮质类固醇治疗也能迅速逆转CRS,且不影响最初的抗肿瘤反应;然而,它可能在长期内损害CAR T细胞反应。在CRS期间中和促炎细胞因子有助于减轻CRS的严重程度。在CRS期间,活化的单核细胞和/或巨噬细胞释放高水平的IL-1;通过IL-1受体拮抗剂中和可以改善临床模型中的CRS和神经毒性。通过给予lenzilumab抗体中和巨噬细胞-单核细胞激活细胞因子GM-CSF,降低了CRS的风险。通过阻断酪氨酸羟化酶减少儿茶酚胺,降低了小鼠模型中的细胞因子水平,暗示了临床干预的途径。
与CAR T细胞相关的HLH/MAS通常与CRS症状一起出现,伴有铁蛋白和肝酶血清水平升高、噬血细胞现象、细胞减少、肺水肿、脾肿大、肾功能衰竭和NK细胞丢失。治疗包括使用依托泊苷或阿糖胞苷进行系统性化疗,如果与神经毒性相关,也可以鞘内应用;在这种情况下,IL-6/IL-6R阻断大多无效。
神经毒性(ICANS):CAR T细胞治疗相关的神经毒性现在被称为免疫效应细胞相关神经毒性综合征(ICANS)。神经系统效应包括失语症、幻觉、混乱、谵妄、表达性失语症、肌阵挛、谵妄、癫痫发作和脑水肿。这种神经毒性发生在大约40%的患者中,是可逆的,并且在CD19 CAR T细胞治疗期间频繁发生;其他CAR T细胞也可以引起神经毒性,指向由于活化CAR T细胞的浸润导致的弥漫性但暂时性脑病。神经毒性的机制尚不清楚,但与破坏血脑屏障和脑脊液中细胞因子水平增加有关。如果与CRS一起治疗,用IL-6阻断和类固醇治疗可以成功。
12.2.“靶上非肿瘤”毒性
由于大多数靶向抗原也由健康细胞表达,CAR T细胞治疗与攻击健康组织的风险相关,导致巨大的“靶上非肿瘤”毒性。治疗B细胞白血病的CD19靶向CAR T细胞也消除了健康的B细胞;持久的B细胞耗竭需要免疫球蛋白替代和抗生素及抗真菌保护,这在临床上是可管理的。当目标抗原由重要组织表达时,毒性更严重。在一项针对肾癌患者的碳酸酐酶IX特异性CAR T细胞治疗试验中,患者由于胆管上皮细胞上碳酸酐酶IX水平较低而出现肝毒性;通过预先给予阻断抗体,可以减少“非肿瘤”毒性的严重程度。避免“靶上非肿瘤”毒性的策略目前旨在增加肿瘤选择性,并以空间和时间的方式限制CAR活性。T细胞给药的替代途径可能是避免通过血液系统分布大量CAR T细胞的选项。通过内窥镜或胸膜内或腹膜内应用局部CAR T细胞给药,在肿瘤部位提供高剂量的CAR T细胞,并在一定程度上避免了非肿瘤毒性。然而,这种应用是有限的,因为在大多数情况下,肿瘤病变无法接触或肿瘤广泛扩散。
12.3.“靶外非肿瘤”毒性
大多数过去工程化的CAR在细胞外部分包含IgG1 CH2CH3结构域作为间隔区,这可能会与Fcγ受体(FcγR)(CD64)结合,从而激活NK细胞和巨噬细胞等先天细胞。尽管到目前为止在临床上并不突出,但理论上可以通过删除IgG1 CH2结构域或突变FcγR结合位点内的Asn297来减少风险。替代间隔区包括IgG4 Fc结构域或细胞外CD8结构域。
第三代曲妥珠单抗衍生的CAR T细胞靶向ErB2导致可能由于急性呼吸窘迫综合征和CRS导致的致命的心肺衰竭。同样,在用EGFR变体3特异性CAR T细胞和CEA特异性CAR T细胞治疗时记录了肺水肿,而没有直接证据表明CAR T细胞攻击肺上皮。由于使用针对同一目标的不同表位或传递不同信号的CAR可能产生显著不同的毒性,因此毒性概况更加复杂,例如,使用来自FRP5抗体的第二代ErB2 CAR的T细胞在肉瘤患者中并未诱导靶外非肿瘤毒性。
12.4.改善CRS的策略
基本上,当CRS在临床上显著时,需要对CAR T细胞进行下调或去激活;瞬时CAR表达、“关闭开关”和“自杀开关”是常用工具。
当存在严重CAR T细胞相关毒性的重大风险时,瞬时CAR表达可能有益。RNA转移产生瞬时表达的CAR。CAR在T细胞表面存在数天,并在目标细胞结合时介导有效的T细胞激活,然而,随着RNA降解和T细胞扩增时RNA稀释,CAR表达会下降。这种RNA修饰的T细胞在试验中显示出一些虽短暂但有效的效果。然而,由于CAR T细胞迅速清除,其缺点是短期效果。
然而,永久性修改的CAR T细胞需要在毒性不受控制的情况下主动消除这些细胞的策略。大剂量脉冲治疗类固醇在应用碳酸酐酶IX特异性CAR T细胞后停止了自身免疫。虽然这是非选择性地清除激活的T细胞,但可以通过特定靶向更有选择性地消除CAR T细胞。CAR结合域基本上也可以通过抗独特型抗体进行靶向,以诱导CAR T细胞的溶解性消除。通过给予识别细胞外CAR结构域中整合的表位的消耗性、FDA批准的抗体,也可以实现CAR T细胞的消耗。例子包括使用利妥昔单抗来消耗具有CD20表位或模拟表位的CAR T细胞,或使用西妥昔单抗来消耗具有EGFR表位的CAR T细胞。是否能够迅速实现足够的CAR T细胞清除以逆转正在进行的CRS,还有待在临床情况下证明。
诱导凋亡的CAR T细胞消除似乎是这种情况下更快速的解决方案。转基因脲酶-9(Cas9)与FKBP1A相连,在系统应用原本惰性的小分子AP1903后,会在工程化CAR T细胞中诱导凋亡,该分子促进二聚体化和激活诱导性Cas9(iCas9)。这种策略是有效的,因为供体T细胞介导的GvHD可以在实验系统中通过iCas9介导的T细胞凋亡在一小时内停止。
与其消除CAR T细胞,不如通过整合模块控制细胞表面的CAR。CAR被设计为融合蛋白,整合了一个自切割降解结构域,该结构域被可以被特定蛋白酶抑制剂特异性阻断的蛋白酶反向调节。在蛋白酶存在的情况下,产生的CAR融合蛋白从连接的降解结构域分离并表达在细胞表面;抑制蛋白酶导致CAR降解和缺乏表面表达。
CAR也可以通过添加酪氨酸激酶抑制剂dasatinib来降低其表达或调节其信号强度,该抑制剂可以迅速且可逆地阻断Lck激活;从而在小鼠模型中减少CRS的严重程度。该策略的好处是,只要存在dasatinib,CAR T细胞的信号强度就会减弱,但不会被清除;然而,该策略仍需临床验证。
需要进一步开发以降低细胞因子介导毒性风险的CAR。调节信号强度的一个关键是CAR共刺激。CD28-ζ CAR更快地诱导T细胞激活,并诱导更高的细胞因子释放、扩增和随后的耗竭,而4-1BB-ζ CAR则驱动较少的急性扩增,但具有较低的细胞因子水平,因此与严重CRS的风险较低。因此,4-1BB-ζ CAR可能更适用于肿瘤负荷和抗原密度高的患者,而CD28-ζ CAR可能需要用于肿瘤负荷低的情况。
降低CAR介导的T细胞激活的其他策略,例如,修改CD8跨膜和铰链区域,从而降低ICANS或高于1级CRS的风险。作为一种替代策略,“通用”CAR允许通过调整将CAR T细胞与目标细胞链接的适配器分子来动态控制T细胞激活。
13.CAR T细胞治疗的挑战
在过去的几年里,临床试验正致力于将CAR T细胞治疗确立为治疗几种类型的B细胞白血病和淋巴瘤;然而,在治疗其他恶性疾病的方面,仍然存在重大障碍。
13.1.如何选择最佳的肿瘤选择性抗原作为靶标?
在CAR T细胞治疗中,肿瘤靶向的选择性对于长期兼容性至关重要。大多数可靶向的肿瘤相关抗原并不具有肿瘤选择性,这增加了CAR T细胞疗法中诱导靶上非肿瘤毒性的风险。肿瘤特异性的表面蛋白突变或肿瘤相关糖基化变体如Muc1或Muc16是罕见的。然而,有些抗原虽然由健康组织表达,但似乎是安全的靶标。例如,癌胚抗原(CEA,CD66e)严格表达在胃肠道和肺部健康上皮的腔面,而在癌细胞上以去极化方式表达。系统性应用CEA特异性CAR T细胞(NCT01212887, NCT02349724)和通过肝动脉输注局部给药的抗CEA CAR T细胞(NCT01373047)在减缓肿瘤进展的同时,并未诱发治疗相关结肠炎。其他如ErB2等抗原可能在高表达ErB2的肿瘤细胞被选择性靶向时是合适的靶标,同时保留中低表达的健康细胞。
为了增加肿瘤选择性,优先考虑靶向一组抗原模式而不是单一特定抗原。技术上,在同一T细胞中共表达两种具有不同特异性的CAR,以在两种CAR同时结合它们相应的抗原时仅诱导完全的T细胞激活;一种CAR提供主要信号,另一种CAR提供共刺激信号,从而仅在存在两种抗原的情况下补充完全T细胞激活所需的信号。该策略需要一个弱的主要信号,以避免在存在一种抗原的情况下进行一些基本的CAR T细胞激活,以及一个强的共刺激信号以驱动完全的T细胞激活。
为了在结合健康细胞时阻断CAR T细胞激活,与激活性CAR共表达具有细胞内PD-1或CTLA-4信号传导的抑制性CAR(iCAR)。iCAR识别健康细胞上存在但在癌细胞上不存在的抗原。因此,仅在结合缺乏iCAR识别的抗原的目标细胞时才发生CAR T细胞激活。
有些抗原在癌细胞上的表达水平高于健康细胞;“亲和力调节”CAR结合域可能有助于区分这两种组织。虽然在临床前模型中证明了可行性,但癌细胞可能通过下调相应抗原来逃避监视。亲和力调节的治疗窗口狭窄,因为增加亲和力可能导致识别健康细胞,如GD2特异性CAR在实验模型中诱发致命性脑炎。
13.2.如何优化CAR结构?
目前临床评估中的大多数CAR基于近二十年前设计的原型CAR结构。临床前研究表明,对于每种抗原,特定CAR需要针对目标抗原表位、结合亲和力、间隔区长度以及信号传导和跨膜结构域等进行优化。由于各组分之间复杂的依赖性,目前无法预测特定抗原的最佳CAR组成。例如,结合亲和力和目标表位的位置为靶向高抗原负载的癌细胞同时保留低抗原负载的健康细胞提供了狭窄的亲和力窗口。
13.3.如何在CAR T细胞治疗后建立长期癌症控制?
尽管在儿童B-ALL中可以高频率诱导完全缓解,但约40%的白血病患者在持续存在CAR T细胞的情况下仍然复发。多种原因导致复发频率高,包括整个CD19分子的丢失或表达缺乏目标外显子2的CD19异构体,从而使其对CAR T细胞不可见。在CD19 CAR治疗后,B-ALL的两个案例中通过转换为CD19阴性的髓系谱系丢失CD19。在这种情况下,靶向对癌细胞存活至关重要的抗原将是一个理想的策略。由于这样的抗原通常不可用,通过双特异性CAR共靶向第二种抗原(例如CD20或CD22)可能会增加对白血病细胞的治疗压力。在实体瘤中这种情况更为重要,因为它们在抗原表达上通常表现出深刻的异质性;在初始肿瘤消退后的早期肿瘤复发可能是由于选择抗原丢失的癌细胞。这些癌细胞可能以抗原非依赖性方式被先天免疫细胞反应识别和消除。为了吸引和激活先天细胞并启动更广泛的免疫反应,CAR T细胞在实验模型中被赋予了诱导释放转基因IL-12的能力,使抗肿瘤攻击更有效。有一些迹象表明,结合抗原依赖性和非依赖性免疫反应可能在长期内控制肿瘤。
13.4.哪种T细胞亚群提供长期肿瘤控制?
临床前模型表明,具有增强扩增能力和长期持久性的原始或早期中央记忆T细胞是过继治疗最合适的细胞。沿着这条线,CD62L+记忆T细胞似乎表现出优越的性能。发现中央记忆干细胞(TSCMs),这是CD62L+中央记忆T细胞库的一部分,具有非凡的扩增潜力,激发了对这些细胞进行过继细胞治疗的探索。人们对识别和调节干细胞样T细胞形成和维持的因素和调控网络越来越感兴趣,因为这些细胞在过继转移到患者后似乎对长期治疗效果至关重要。另一种策略是基于预测性地诱导T细胞成熟。例如,4-1BB共刺激在年轻T细胞中启动中央记忆T细胞反应,这与CD28 CAR T细胞表现出更短暂的效应细胞反应形成对比。另一方面,更成熟的阶段的细胞在大多数肿瘤所在的外围显示出优先积累。然而,这些细胞需要不同的共刺激信号,即优先迁移到外围的CCR7− T细胞从联合CD28-OX40共刺激中受益。特定T细胞亚群的功能能力也可以通过与激酶抑制剂的联合治疗来调节;ibrutinib,一种布鲁顿酪氨酸激酶(BTK)抑制剂,降低了PD-1和CAR T细胞的耗竭,从而增加了持久性和抗肿瘤活性。
13.5.如何使CAR T细胞制造适应日益增长的患者数量?
目前,大多数CAR T细胞由专门的GMP设施生产,冷冻并运送到患者的医院。生产越来越多的细胞产品将使当前程序达到极限,特别是当及时需要数千个自体细胞产品时。在医院内(半)自动化、完全控制和完全封闭系统的分散制造是解决这种情况的首选概念之一。这也将需要在制造过程中高度标准化,并避免血液和细胞产品运输中的复杂物流。作为另一种概念,一个高度专业化的、集中的生产设施,具有多个并行的自动化制造过程,可能作为患者细胞产品的区域供应商。
另一个限制是由患者自体T细胞治疗的需要设定的;对于每位患者来说,“通用”供体将使治疗在多个方面更容易。一个包含不同工程化CAR的“通用”供体T细胞产品库将在临床应用中提供更大的灵活性,根据患者的具体情况。此外,扩大生产规模将使更多的患者能够使用CAR T细胞产品。正在努力生成可以应用于众多患者的这种“通用”T细胞。这需要使CAR T细胞对宿主免疫细胞“隐形”,缺乏对患者健康组织的异体反应性,同时保留CAR介导的抗肿瘤活性。在这种情况下,通过基因组编辑技术获得的MHC缺陷、CAR修饰的病毒特异性T细胞和TCRα敲除T细胞,目前正在开发作为“现成的”或“第三方”细胞产品,GvHD风险低。CAR基因插入TCRα位点一步实现CAR的遗传工程和TCR表达的废除。编辑MHC I类以防止宿主识别和排斥供体T细胞可能通过NK细胞诱导消除,并不防止MHC II类介导的排斥。然而,目前探索的所有基因编辑程序在某种程度上都容易受到非目标修饰的影响,因此与意外的突变风险相关。该领域发展迅速,首次使用异体CAR T细胞治疗B细胞恶性肿瘤和实体瘤的试验已经启动。
13.6.如何平衡CAR T细胞的疗效和副作用?
目前,一些CAR T细胞治疗与高风险的严重副作用相关,可能需要重症监护住院治疗。尽管各种CAR T细胞协议和治疗程序不同,并且没有在比较性的临床环境中进行评估,但一些临床管理规则变得明显。例如,CRS的早期诊断、分级和临床管理将标准化,建立共识的治疗方案。在毒性不受控制的情况下,可以通过各种手段选择性地和迅速地消除CAR T细胞。通过添加二聚体化剂AP1903二聚体化转基因诱导的脲酶-9(iCasp9),在30分钟内消除超过90%的T细胞。或者,通过给予针对CAR结构域或共表达表位的抗体,诱导抗体依赖性细胞毒性(ADCC)清除循环中的CAR T细胞。免疫介导的CAR T细胞消除的缺陷仍然是,癌症患者的潜在功能障碍免疫系统可能通过ADCC消除CAR T细胞的能力有限。
13.7.我们是否需要针对每种癌症类型的特定预处理?
在大多数试验中,患者在过继T细胞治疗前接受非清髓性淋巴细胞减少,使用氟达拉滨和环磷酰胺;这种预处理的理由是暂时提供“空间”和细胞因子,以实现转移的CAR T细胞在体内的充分扩增。淋巴细胞减少还通过免疫调节提供抗肿瘤效果,因为它耗尽抑制细胞,并在肿瘤破坏时释放肿瘤相关抗原到免疫系统。尽管目前的预处理方案基本上是有效的,但基本方案可能需要针对每种癌症实体进行调整。例如,用于治疗Her2+肿瘤的调节方案通过应用nab-紫杉醇来耗尽间质性基质,并促进Her2呈递,并通过应用环磷酰胺耗尽Treg和MDSC,用于胆道和胰腺癌的修改。另一方面,预处理在CAR T细胞治疗的背景下可能具有高度毒性,通过诱导脑水肿和神经系统毒性,特别是在最近的一项试验(NCT02535364)中观察到的氟达拉滨治疗后。
13.8.如何激活免疫网络以诱导广泛的炎症性抗肿瘤反应?
CAR T细胞作为“活药”,越来越成为在目标器官产生和释放生物活性化合物的“活工厂”。使用CAR T细胞作为工厂的合理性基于实验肿瘤模型的证据,即宿主免疫系统在肿瘤排斥中起着重要且必要的作用,这使得在目标肿瘤组织内产生免疫刺激性条件成为必要。释放IL-12的CAR T细胞(IL-12 TRUCKs)可以通过吸引和激活M1型巨噬细胞来在肿瘤组织中诱发免疫反应,这些巨噬细胞可以消除CAR T细胞未能识别的癌细胞。其他具有特定影响局部免疫环境的细胞因子也可以使用;释放IL-18的CAR T细胞增加了肿瘤相关CD206+ M1型巨噬细胞和NKG2D+ NK细胞的数量,并减少了如Treg细胞、CD103+树突细胞和M2型巨噬细胞等抑制细胞。目前正在试验中探索使用靶向PD-1的检查点阻断,以激活CAR T细胞和浸润性淋巴细胞(NCT02650999);其他检查点的阻断或组合,以重新激活肿瘤内源性免疫细胞,同样值得进行临床探索。
14.CAR T细胞用于其他疾病的治疗
将T细胞激活重定向的CAR不仅限于靶向癌细胞,还可以用于靶向任何由目标抗原定义的细胞。通过抗Dsg3 CAR靶向记忆B细胞的CAR T细胞被设计用来消除导致天疱疮病理的细胞。通过识别MHC呈递的自身抗原的CAR T细胞靶向自反应性T细胞。CAR被工程化以靶向病毒感染的细胞,如乙型肝炎病毒、丙型肝炎病毒、巨细胞病毒和HIV感染的细胞。源自Dectin-1的CAR T细胞被用于破坏真菌Aspergillus的发芽。实验模型暗示,CAR重定向的Treg细胞可用于促进自身免疫疾病如结肠炎、过敏性哮喘和移植物抗宿主病的免疫耐受治疗,通过靶向HLA。最近,通过识别心脏成纤维细胞激活蛋白(FAP)的CAR T细胞靶向心脏纤维化,该蛋白在心肌损伤重塑时由心脏成纤维细胞高度表达。采用FAP特异性CAR的T细胞过继转移减少了心脏纤维化并恢复了小鼠的损伤后功能。该报告暗示CAR T细胞作为“活药”,在治疗目前疗法非常有限的心脏病中消除激活的心脏成纤维细胞。CAR T细胞用于治疗非恶性疾病其他应用的临床前开发正在进行中。
要点
采用嵌合抗原受体(CAR)重定向的T细胞的过继细胞治疗在某些血液学恶性肿瘤中取得了显著的治疗效果;然而,在其他疾病中的治疗效力仍然有限。
CAR是由结合域、跨膜域和细胞内信号传导域组成的模块化、重组的跨膜分子,用以激活工程化细胞。最佳分子设计需要通过变化组成域在每种情况下探索。
原型CAR设计可以通过使用各种靶向和信号传导元件进行修改,使CAR更加通用。此外,各种免疫细胞可以通过CAR重定向,提供方便的治疗细胞。
CAR T细胞治疗经常与毒性相关,这些毒性可以通过同时进行的治疗、改变CAR设计和靶向替代抗原来减少靶上非肿瘤毒性来减轻。
通过共同激活广泛的免疫反应、共同靶向肿瘤基质、癌症干细胞和其他与肿瘤相关的结构,可以提高CAR工程化免疫细胞的抗肿瘤效力。
生产CAR T细胞产品仍然具有挑战性,为所有患者提供个性化治疗;正在努力为广泛的患者群体制造异体细胞产品“现成”。
下章预告:抗体关键特性的改进
往期内容:
第二章:抗体:发现及特性的历史
第三章:单克隆抗体和杂交瘤细胞
第四章:抗体展示系统
第五章:转基因动物用于产生人类抗体
第六章:抗体在治疗、诊断和科学中的应用
第七章:双特异性抗体
第八章:抗体偶联药物
第九章:替代性结合框架:用于基础研究和治疗应用的多功能结合剂
为促进抗体行业的交流与创新,2024年10月16-17日第七届金秋十月抗体产业发展大会如约而至。会议旨在为研究人员提供一个互动交流的平台,有助于推动抗体产业的进一步发展。
会议内容
时间:2024年10月16-17日
地点:上海张江(酒店定向通知)
规模:600-800人
主办单位:生物制品圈、抗体圈
演讲支持:Entegris、瑞孚迪、AS ONE CORPORATION
会议费用:免费FREE!(仅收取100元报名定金,含参会学习、茶歇、会议手册,定金概不退还),先到先得,报完即止!
报名方式:扫描下方二维码或点击文章最底部“阅读原文”→ 填写表格 → 报名成功(报名志愿者,承担一定工作,请慎重考虑,免交定金)!
组委会获得报名信息后,根据报名信息进行初筛,并进一步与报名者沟通确认,实现精准邀请。最终有机会进入大会微信群(严格审核通过)。
日程安排
更多嘉宾正在邀请中
识别微信二维码,添加生物制品圈小编,符合条件者即可加入
生物制品微信群!
请注明:姓名+研究方向!
版
权
声
明
本公众号所有转载文章系出于传递更多信息之目的,且明确注明来源和作者,不希望被转载的媒体或个人可与我们联系(cbplib@163.com),我们将立即进行删除处理。所有文章仅代表作者观点,不代表本站立场。
免疫疗法细胞疗法
2024-09-15
摘要:疫苗是人类历史上最重要的发明之一,已经彻底改变了全球健康。通常,疫苗通过触发先天免疫反应和刺激抗原呈递细胞,引发针对特定病原体抗原的防御性适应性免疫反应。作为关键要素,佐剂通常是作为添加剂使用的化学材料,以增加疫苗的效力和免疫原性。90多年来,佐剂一直是许多人类疫苗中不可或缺的组成部分,通过增强、调节和延长免疫反应来提高其效力。在这里,我们及时并全面地回顾了佐剂的历史发展和当前状态,包括它们的分类、作用机制以及在不同疫苗中的角色。此外,我们对当前的许可流程进行了系统分析,并重点介绍了涉及疫苗佐剂的临床试验中的显著例子。展望未来,我们预测该领域的未来趋势,包括新佐剂配方的开发、创新佐剂的创造以及它们在系统疫苗学和疫苗递送更广泛范围内的整合。文章认为,对生物化学、材料科学和疫苗免疫学的更深入理解对于推进疫苗技术至关重要。这些进步预计将导致未来开发出更有效的疫苗,能够对抗新兴传染病并增强公共卫生。
1.引言:疫苗佐剂的历史
自20世纪初以来,疫苗佐剂研究领域取得了显著进展(图1)。随着传染病的日益流行,免疫接种已成为限制其传播和减少相关伤害的最有效方法。然而,早期疫苗往往证明是无效的,因为纯化的抗原本身无法引发足够强烈的免疫反应。为了克服这一挑战,引入了佐剂的概念。佐剂是添加到疫苗中以增强其免疫原性,从而提高其效力的材料。
图1.疫苗佐剂发展重大事件时间线。这个时间线展示了疫苗佐剂的逐步发展,从RNA和DNA等天然成分演变为合成工程佐剂。
现代佐剂的发展一直是一个缓慢而充满挑战的过程。研究人员旨在创造能够引发强烈免疫反应的同时保持安全性的疫苗。这涉及到选择性地结合明确定义的分子和配方,并探索天然和合成化合物。正如图1所总结的,佐剂的组成随着时间的推移而演变。它已经从早期的天然成分发展到当代的合成化合物。
尽管佐剂开发面临挑战,但目前有超过30种来自不同制造商的许可疫苗含有佐剂。铝盐是最早发现的佐剂,已被发现可以增强针对乙型肝炎、破伤风、白喉、百日咳和人类乳头瘤病毒等疾病的疫苗的免疫反应。铝盐的有效性归因于它们能够在注射部位形成仓库、诱导炎症以及激活树突细胞和T细胞等因素。尽管铝盐在疫苗中使用了七十多年,但其确切的免疫机制仍然不完全了解。
1990年代后期的佐剂发展包括油包水乳液。这些乳液有助于抗原在较长时间内缓慢释放,激活先天免疫系统,并诱导体液和细胞免疫反应。这种乳液的首次使用之一是在Fluad中,Fluad是一种针对65岁以上成人的许可季节性流感疫苗。其他FDA许可的佐剂包括MF59(一种含有角鲨烯、一种可生物降解油和表面活性剂的油包水乳液佐剂,用于流感疫苗)和AS03(由α-生育酚、角鲨烯和表面活性剂组成,用于H1N1流感疫苗和一些大流行流感疫苗)。AS01(一种脂质体和单磷酰脂A的混合物)已在RTS,S/AS01疟疾疫苗和带状疱疹疫苗Shingrix中使用。
尽管许多其他佐剂在临床前模型中显示出高效力,但由于安全或耐受性问题,大多数尚未获得人类使用的许可。此外,包括铝、MF59和佐剂系统AS0佐剂在内的现有佐剂在人类中的作用分子机制仍然不甚了解。
2.佐剂的好处和效果
总体而言,疫苗佐剂在增强疫苗的有效性和可及性以及减轻全球传染病负担方面发挥着关键作用。它们的用途和其他实际应用如下(图2):
1.缓解有限的疫苗供应:佐剂增强免疫反应,允许较少的疫苗剂量实现完全保护。这减轻了卫生系统的负担,并增加了无法接受多剂疫苗的人的可及性。佐剂还可以降低疫苗中必要的抗原剂量,从而可能减少副作用并增加可用性。例如,重组疫苗在制造上具有显著优势,但通常自身免疫原性较弱。将佐剂与重组大流行流感蛋白结合可以大幅减少实现目标抗体水平所需的抗原量,从而显著增加制造能力。例如,AS03是一种油包水乳液佐剂,已在H1N1流感疫苗等疫苗中使用。它已被证明可以改善免疫反应并允许抗原节约,这意味着可以使用更少的疫苗抗原量,同时仍然产生强烈的免疫反应,这有助于延长现有疫苗供应。
2.促进快速免疫反应:佐剂刺激对疫苗抗原的更强、更持久的反应,提供更好的保护。例如,将AS04佐剂添加到GSK的乙肝抗原Fendrix中,使得三剂方案减少到两剂。例如,Advax是一种基于delta菊粉的佐剂,已被证明可以加速免疫反应。它激活先天免疫系统,并促进细胞因子和趋化因子的产生,这有助于增强适应性免疫反应。
3.扩大抗体反应:佐剂扩大了对具有显著抗原漂移或株变体的病原体的抗体反应,这对于流感、人类乳头瘤病毒(HPV)和疟疾寄生虫等疾病至关重要。例如,MF59是一种已被证明可以增强细胞和体液免疫反应并显著增加抗体滴度和改善抗体反应质量的油包水乳液佐剂。
4.增强抗体反应的幅度和功能性:佐剂不仅增加了抗体反应的幅度,还增加了它们的功能性、亲和力或免疫系统产生的功能性抗体数量。例如,AS04是一种将铝盐与单磷酰脂A(MPLA)结合的佐剂,MPLA是一种Toll样受体4激动剂。AS04已被证明可以增强抗体反应的幅度和功能性。它促进了高质量抗体的产生,包括增加抗体滴度和改善抗体亲和力和亲和力。
5.增强T细胞反应:正在开发新的疫苗候选物以改善T细胞反应,现有的人类使用批准的佐剂未能有效诱导这些反应。目标是更有效地吸引T辅助细胞,以优化抗体反应的质量和持久性,或诱导能够针对和消除细胞内病原体的效应CD4+或CD8+ T细胞。因此,新疫苗可能包括Toll样受体(TLRs)和其他先天免疫受体的激动剂,以促进T辅助细胞反应的产生。这种方法旨在克服传统佐剂的局限性,创造更有效的疫苗,能够提供更持久的保护,对抗更广泛的病原体。通过改善T细胞反应,这些疫苗也可能为免疫系统减弱的个体或对传统疫苗反应不佳的人提供好处。例如,CpG ODNs是含有特定免疫刺激性序列的合成DNA分子,作为Toll样受体9(TLR9)激动剂,已被证明能够通过促进抗原特异性CD4+和CD8+ T细胞的激活和分化来增强T细胞反应。它们诱导Th1型免疫反应,导致T细胞增殖、细胞因子产生和细胞毒性T细胞活性增加。
6.开发新疫苗:佐剂在开发传统疫苗无效的疾病疫苗中至关重要,增强免疫反应并针对多种病原体株。它们可以增强对疫苗的免疫反应,并帮助针对病原体的多种株。例如,在流感疫苗的情况下,已使用佐剂来创建可以对不同流感病毒株提供更好保护的疫苗。此外,佐剂可用于开发尚未有有效疫苗的病原体引起的疾病疫苗,如HIV或疟疾。开发能够刺激针对这些病原体的强烈和针对性免疫反应的佐剂是一个重要的研究领域。例如,在病毒样颗粒(VLP)佐剂中,VLP是自组装结构,模仿病毒的整体结构但缺乏病毒遗传物质,使其不具传染性。VLP既可以作为抗原也可以作为佐剂。它们已用于新疫苗的开发,以增强免疫反应,提高疫苗效力,并扩大对不同病毒株或亚型的免疫反应。
7.提高安全性:通过增强免疫反应,佐剂可以降低疫苗相关不良事件的风险。这是因为免疫系统能够更好地针对和消除抗原,降低可能导致副作用的过度免疫反应的风险。因此,疫苗中使用佐剂已成为提高疫苗效力、安全性和可及性的重要策略。例如,病毒体是将病毒蛋白(如流感血凝素)纳入其结构的类脂质体颗粒。它们已被用作疫苗中的佐剂以提高安全性。病毒体提供了病毒的抗原特性,但没有传染性遗传物质,降低了疫苗相关不良事件的风险。病毒体佐剂已用于流感和甲型肝炎等疾病的疫苗中。
图2.佐剂的潜在好处。
3.佐剂的类别及其作用机制
在这一部分,我们讨论典型的疫苗佐剂,包括它们的组成、功能机制、在疫苗中的应用以及它们的优点和缺点,以及与它们相关的挑战。铝盐基佐剂。
铝盐基佐剂,通常称为铝佐剂,是最早用于许可的人类疫苗中的佐剂,并且仍然是使用最广泛的佐剂。它们由氢氧化铝、磷酸铝或两者的组合组成,已知能够在注射部位形成仓库,随着时间的推移缓慢释放疫苗抗原,从而产生更强和更持久的免疫反应。它们已被证明能够增强对广泛抗原的免疫反应,包括乙型肝炎、人类乳头瘤病毒(HPV)和肺炎球菌病疫苗中的抗原。由于它们经过验证的安全性记录、广泛增强免疫反应的能力以及制造的便利性,它们仍然是疫苗开发的有吸引力的选择。然而,人们对铝盐可能引起不良反应(如注射部位的局部反应和罕见的过敏反应)的潜力有一些担忧。使用铝盐作为疫苗佐剂的好处通常大于风险。
图3.疫苗佐剂的类型。
铝盐基佐剂的确切作用机制尚不完全了解,但有几种提出的理论(图4a)。铝佐剂之所以受欢迎的一个关键原因是它们能够在注射部位形成仓库。这个仓库随着时间的推移缓慢释放疫苗抗原,为免疫系统提供对抗原的长期暴露。这种长期暴露有助于增强免疫反应,导致更强大和更持久的免疫力。
图4.疫苗佐剂的作用机制。a) 基于铝盐的佐剂。b) 乳液佐剂。c) 基于TLR激动剂的佐剂。
此外,也认为铝佐剂通过在注射部位诱导炎症来激活先天免疫系统。这种炎症被认为是由炎症体激活触发的,炎症体是一种在先天免疫反应中起关键作用的蛋白质复合体。激活的炎症体释放促炎细胞因子,这有助于吸引免疫细胞到炎症部位并激活它们。
铝盐基佐剂还被认为是通过诱导促炎细胞因子(如IL-1β和TNF-α)的释放来激活树突细胞,这些细胞是专门呈递抗原给T细胞的免疫细胞,负责识别和攻击外来入侵者。铝盐基佐剂通过吸引树突细胞到注射部位并激活它们来激活树突细胞。反过来,树突细胞促进效应T细胞的分化,这在诱导免疫中起着关键作用。
铝佐剂还被认为是通过刺激CD4+ T细胞的分化和诱导B细胞产生抗体来刺激免疫反应,这对于诱导免疫至关重要。这一过程是通过树突细胞产生IL-1β和IL-18来介导的,它们促进效应T细胞的分化。仓库中抗原的缓慢释放也有助于延长B细胞对抗原的暴露,这可以增强抗体的产生。
总之,铝盐基佐剂通过在注射部位形成仓库、激活炎症体、诱导促炎细胞因子的释放、吸引树突细胞到注射部位以及增强B细胞的抗体产生来发挥作用。这些机制共同作用,增强疫苗中抗原的免疫反应,提高对目标疾病的保护。
3.1.无机纳米颗粒基佐剂
无机纳米颗粒基疫苗佐剂,如纳米铝、层状双氢氧化物(LDH)、纳米/介孔硅、纳米金刚石、量子点等,已被研究其增强疫苗免疫反应的潜力。无机纳米颗粒提供了一个多功能的平台,用于表面修饰,允许精确控制大小和形状参数。这种多功能性便于设计旨在引发特定免疫反应的定制结构。此外,这些纳米颗粒通常表现出强大的化学和物理化学稳定性,确保在储存和运输过程中无需冷藏即可延长货架寿命。这些属性对于实际疫苗部署和分发场景至关重要,特别是在资源有限的环境中,使它们成为储备疫苗以应对未来紧急需求的理想选择。
无机纳米颗粒基疫苗佐剂的作用机制涉及其与免疫系统的相互作用,以增强和调节疫苗中抗原的免疫反应。无机纳米颗粒作为抗原的载体,确保其有效地传递给抗原呈递细胞(APCs)。纳米颗粒被设计为被APCs(如树突细胞和巨噬细胞)有效摄取。这种摄取是通过纳米颗粒的大小、表面电荷和表面修饰来促进的。一些无机纳米颗粒佐剂,如基于铝的佐剂,会在注射部位诱导局部炎症。这吸引免疫细胞到该部位并促进APCs的招募。无机纳米颗粒佐剂有助于发展持久的免疫记忆。这确保免疫系统“记住”遇到的抗原,为后续暴露于病原体提供保护。
其中,具有纳米纤维形态的γ相氧化铝水合物(γ-AlOOH)纳米颗粒已被制备并用作人结核杆菌(HTB)水热提取物的传递系统。由于其独特的介孔纤维结构,合成的γ-AlOOH显著增强了类巨噬细胞的细胞摄取,与商业铝佐剂相比增加了约两倍。
介孔硅具有有序的多孔结构,孔径均匀在介尺度范围内(2至50纳米)。这种结构提供了大的表面积和可调节的属性,使其适合于包括药物传递和疫苗佐剂在内的各种应用。介孔硅的表面可以被修饰以定制其属性,以适应特定的疫苗配方和应用。介孔硅也可以用来封装免疫调节剂,进一步增强佐剂效果。例如,无定形硅可以用作疫苗佐剂以增强免疫反应。纳米尺度和微米尺度的硅都促进了髓样细胞中NLRP3炎症体的激活,而只有纳米尺度的硅激活了角质形成细胞中的炎症体。
LDHs是具有正电荷的类水镁石层和层间阴离子的层状材料,为包括药物传递和免疫调节在内的各种应用提供了独特的结构。LDHs由于其层状结构,为抗原提供了高负载能力。LDHs可以设计为以受控的方式释放抗原,促进持久和持久的免疫反应。LDHs可以表面修饰以整合额外的功能,如靶向配体或免疫调节剂,以进一步定制其性能。
总之,无机纳米颗粒基作为疫苗佐剂是一个活跃的研究领域,它们在疫苗开发中的应用有望增强免疫反应,提高疫苗的整体有效性。
3.2.乳液佐剂
当两种无法形成均匀混合物的液体混合在一起时,就会形成乳液。抗原包含在这些水滴中,油作为仓库,缓慢释放抗原,并通过减少清除时间来增强免疫反应,延长抗原暴露。乳液是另一种已开发用于增强疫苗免疫反应的疫苗佐剂。乳液由两种不相混溶的液体组成,通常是一个油相和一个水相,由表面活性剂稳定。乳液通过在油相中形成小滴的抗原,然后将它们分散在整个水相中来工作。
最早被批准用于人类疫苗的油包水佐剂之一是MF59,它包含角鲨烯、聚山梨酯80、三油酸甘油酯和柠檬酸钠脱水物。MF59诱导ATP释放,并上调细胞因子和趋化因子,以增强接种部位的抗原特异性免疫反应。它已被证明是安全且耐受性良好的。另一种基于油包水乳液的佐剂是AS03,它含有表面活性剂聚山梨酯80和两种可生物降解的油,角鲨烯和DL-α-生育酚。欧洲委员会在2009年授予AS03佐剂的Pandemrix市场授权,AS03佐剂的流感A(H5N1)单价疫苗在2013年获得了FDA的许可。AS03已越来越多地用于流感和疟疾疫苗。
乳液已在各种疫苗中使用,包括流感、乙型肝炎和人类乳头瘤病毒(HPV)疫苗。它们提高了疫苗效力,特别是在对传统疫苗可能反应不佳的人群,如老年人或免疫受损个体中。乳液佐剂通过几种机制增强疫苗的免疫反应。图4b41中提出了几种理解基于乳液的佐剂如何工作的机制:
一个主要机制是抗原在较长时间内缓慢释放。乳液滴的小尺寸允许延长表面积与体积比,这增强了抗原呈递和抗原呈递细胞的摄取。这种缓慢释放的抗原可以在较长时间内激活免疫系统,从而产生更强大和持久的免疫反应。
乳液佐剂还激活先天免疫系统。乳液滴被免疫系统识别为外来物质,导致激活树突细胞、巨噬细胞和单核细胞等抗原呈递细胞。然后这些细胞产生促炎细胞因子和一系列趋化因子,如TNF-α和IL-1β,这进一步激活免疫系统并吸引免疫细胞到注射部位,形成一个免疫能力环境,以增强抗原运输到引流淋巴结。
乳液佐剂的另一个重要机制是它们能够诱导体液和细胞免疫反应。乳液滴可以被抗原呈递细胞摄取,然后呈递给T细胞和B细胞。T细胞负责直接攻击感染的细胞,而B细胞产生可以中和病原体的抗体。已证明乳液佐剂可以激活T细胞和B细胞,导致更全面的免疫反应。
总之,乳液佐剂已成为疫苗开发中的重要工具。它们通过几种机制增强疫苗的免疫反应,包括缓慢释放抗原、激活先天免疫系统,并诱导体液和细胞免疫反应。
3.3.Toll样受体(TLR)激动剂
Toll样受体(TLRs)是一种模式识别受体,对入侵病原体的先天免疫反应起着至关重要的作用。TLRs是跨膜受体,主要由先天免疫系统的细胞表达。这些受体分为两组:细胞表面TLRs(TLR1、TLR2、TLR4、TLR5和TLR6)和细胞内TLRs(TLR3、TLR7、TLR8和TLR9),它们在内体膜上表达。每个TLR都包含一个跨膜域、一个富含亮氨酸的重复(LRR)段,该段识别与病原体相关的分子模式(PAMPs)和与损伤相关的分子模式(DAMPs),以及一个Toll/白细胞介素-1受体(TIR)域,该域启动下游信号传导并诱导炎症反应。因此,TLRs是佐剂刺激有效免疫反应的有吸引力的靶标,为病原体提供持久保护。Toll样受体(TLR)激动剂作为疫苗佐剂在对抗癌症、艾滋病和疟疾等致命和复杂疾病方面非常有前景。
CpG寡脱氧核苷酸(ODNs)是具有磷酸硫酯骨架的合成DNA分子,包含未甲基化的CpG基序。图4c描述了基于TRL的佐剂如何作用:CpG ODN是一种强效佐剂,诱导1型辅助T(Th1)反应,并促进细胞毒性T淋巴细胞(CTLs)的产生和干扰素-γ(IFN-γ)的分泌。CpG ODN通过TLR9激活增强了对抗原的特异性体液和细胞免疫反应。由于其独特的特性,CpG ODN可以用作通过肌肉内、皮下、口服和鼻内途径进行免疫接种的佐剂。作为有效的疫苗佐剂,CpG ODN可以促进抗原的免疫刺激效应,激活抗原呈递细胞(APCs),并加速免疫反应。CpG ODN有助于浆细胞样树突细胞(pDCs)上主要组织相容性复合体(MHC)、CD40和CD86的表达,并增强抗原处理,导致强大和持久的免疫反应。
3.4.脂质体
脂质体是一种疫苗佐剂,由磷脂和胆固醇组成,是能够包裹抗原和其他免疫刺激性分子的小球形结构。它们是可生物降解的、生物相容的,并且允许进行多功能的结构修饰,以实现可调节的特性和毒性。脂质体可用于将抗原传递给抗原呈递细胞,如树突细胞,这可以激活免疫系统。此外,脂质体能够增强体液和细胞免疫反应,诱导对清除细胞内病原体和增强抗体反应很重要的Th1偏向反应,使它们成为疫苗开发的有吸引力的佐剂。脂质体的一个独特特性是它们能够被修改以针对特定的细胞类型。它们可以被修饰有针对树突细胞上特定受体的抗体或肽,增加脂质体包裹的抗原的摄取。脂质体也可以用来共同传递多个抗原或免疫刺激性分子,从而引发更强大的免疫反应,特别是对于可能需要多个抗原来诱导保护性免疫反应的复杂病原体。
基于脂质体的佐剂系统AS01包含两种免疫刺激性剂,3-O-去酰基-4'-单磷酰脂A(MPL)和QS-212。使用AS01佐剂的疫苗包括新开发的疟疾疫苗RTS, S(Mosquirix),以及针对带状疱疹(HZ/su)、HIV和结核病的疫苗候选物。AS01可以促进产生针对抗原的抗体和针对抗原的CD4+ T细胞,这使其区别于其他佐剂。
3.5.其他佐剂
细胞因子 - 细胞因子是一类在免疫反应中起重要作用的信号分子。它们由免疫系统的各种细胞分泌,作用于特定受体以介导一系列生物学功能,如炎症、细胞增殖和分化。细胞因子可以根据其结构和功能被划分为不同的类别,包括白细胞介素、干扰素、肿瘤坏死因子和趋化因子。
聚合物 - 聚合物是由通过共价键连接在一起的重复单元组成的化合物。它们可以是天然的或合成的,并且在材料科学、医学和生物技术中有广泛的应用。在疫苗方面,聚合物可以用作载体,创建缓慢释放的仓库,在其大的交联结构中携带抗原和其他免疫调节剂。这导致持续的抗原呈递和免疫系统的激活,可以导致更强大和更持久的免疫反应。
皂苷 - 皂苷是具有两性属性的天然化合物,意味着它们既有亲水区也有疏水区。它们在传统医学中已被使用数个世纪,并且有许多潜在的药物应用,包括作为疫苗的佐剂。皂苷可以通过刺激树突细胞等抗原呈递细胞以及促进细胞因子和趋化因子的产生来增强免疫反应。皂苷基佐剂的一个例子是QS-21,它与MPL(单磷酰脂A)一起在AS01佐剂系统中使用。AS01是一种有效的佐剂,已被用于开发针对疟疾、结核病和带状疱疹等疾病的疫苗。
病毒体 - 病毒体由磷脂和病毒包膜蛋白组成,通常来源于不引起人类疾病的病毒。病毒包膜蛋白提供了可以激活免疫系统的免疫原性表面,而磷脂有助于稳定病毒体结构并增加其被抗原呈递细胞的摄取。
4.各种疫苗及其佐剂的作用
在这一部分,我们讨论了佐剂在各种疫苗中的作用。图5总结了当前正在开发的已确认的主要疫苗和方法。这些包括全病毒疫苗(如活减毒疫苗、灭活疫苗和病毒载体疫苗)、亚单位疫苗和核酸疫苗(包括pDNA和mRNA)。
图5.各种疫苗及其佐剂的总结。
4.1.灭活疫苗
灭活疫苗通常由病毒感染的细胞制成并灭活,这确保了病毒不再具有传染性,但保留了它们的抗原特性,使它们有助于产生免疫反应。可以向灭活疫苗中添加佐剂以增强免疫反应。氢氧化铝和磷酸铝等铝盐是灭活疫苗中最常用的佐剂。它们通过将抗原吸附到其表面来增强免疫反应,这允许抗原缓慢释放并在较长时间内刺激免疫系统。灭活疫苗中使用的其他佐剂包括MF59、AS03和AS04。MF59是一种油包水乳液,通过在注射部位创建抗原仓库以及刺激先天免疫系统来增强免疫反应。这些佐剂已在H1N1流感疫苗和人类乳头瘤病毒(HPV)疫苗等疫苗中使用。在一项研究中,带有铝佐剂的CoronaVac灭活疫苗对SARS-CoV-2显示出高效的中和效果。
4.2.活减毒病毒疫苗
活减毒病毒疫苗由于其在注射后能在宿主体内迅速扩增,从而有效免疫,因此已成为成功的免疫策略。活减毒病毒疫苗是病毒的弱化形式,能在体内复制但不引起疾病。因此,它们可以引发强烈且持久的免疫反应。通常不与活减毒病毒疫苗一起使用佐剂,因为疫苗本身已经是免疫系统的强刺激剂。然而,一些研究已经探索了与活减毒病毒疫苗一起使用佐剂以潜在增强其有效性的可能性。一个例子是使用油包水乳液MF59作为活减毒流感疫苗的佐剂,已被证明可以改善老年人的免疫反应。然而,需要更多的研究来确定活减毒病毒疫苗中佐剂的安全性和有效性。
4.3.病毒载体疫苗
复制能力和非复制能力的腺病毒载体通常用于表达其他病毒蛋白的抗原以进行免疫接种。佐剂可以与病毒载体疫苗一起使用,以增强疫苗产生的免疫反应。例如,牛津-阿斯利康COVID-19疫苗是一种病毒载体疫苗,它使用一种减毒的黑猩猩腺病毒来传递SARS-CoV-2刺突蛋白的遗传物质。这种疫苗含有一种名为AS03的佐剂,这是一种由角鲨烯(一种天然油)、聚山梨酯80(一种洗涤剂)和维生素E组成的混合物。
4.4.病毒样颗粒疫苗
在这种策略中,结构病毒蛋白被共同表达以形成非感染性颗粒作为疫苗免疫原。它们类似于真正的病毒颗粒,但缺乏病毒基因组。在细胞中生产VLPs,然后进一步重建为稳定和免疫原性形式是一个多阶段过程。佐剂可以用于病毒样颗粒疫苗中,以增强免疫反应并提高疫苗效力。用于病毒样颗粒疫苗的常见佐剂包括铝盐、MF59(一种油包水乳液)和CpG寡核苷酸(TLR-9激动剂)。这些佐剂刺激免疫系统产生对VLP疫苗更强大和更持久的反应。在某些情况下,VLP本身可以作为佐剂,因为它已经显示出通过多种途径刺激免疫系统。总体而言,VLP疫苗中佐剂的使用可以帮助增加其效力,减少所需剂量,并提高疫苗覆盖率。
4.5.DNA疫苗
基于DNA的疫苗使用DNA质粒作为载体,将编码抗原的基因转移到宿主细胞中,特别是抗原呈递细胞。这些疫苗的机制依赖于将遗传物质传递到细胞核中,激活载体中的哺乳动物启动子,并通过宿主细胞机制启动目标基因的转录。然而,与其他疫苗类型相比,DNA疫苗通常具有有限的免疫原性,这可能限制了它们的有效性。佐剂可以通过增强对编码抗原的免疫反应来帮助克服这一限制。在DNA疫苗中测试了各种佐剂,包括铝、CpG寡脱氧核苷酸(CpG ODNs)和脂质体。铝已被证明可以增强小鼠对DNA疫苗的免疫反应,但在人类试验中的成功有限。CpG ODNs是模拟细菌DNA的合成分子,可以通过与免疫细胞上的Toll样受体(TLRs)相互作用来激活免疫系统。脂质体是小的脂质囊泡,可以包裹DNA和佐剂,并直接传递给抗原呈递细胞。基于脂质体的佐剂在DNA疫苗的临床前研究中显示出前景。
4.6.mRNA疫苗
mRNA疫苗涉及将mRNA分子直接注入宿主细胞中,然后在细胞质中翻译成目标蛋白。这些疫苗通常包含一个带有3'聚腺苷酸尾的开放阅读框(ORF),可以刺激细胞和体液免疫反应。与传统疫苗相比,mRNA疫苗提供了许多优势,如安全性、灵活性、可扩展性和成本效益。mRNA疫苗通常不需要佐剂,因为mRNA分子本身就会刺激免疫系统。例如,针对COVID-19的mRNA疫苗使用脂质纳米颗粒传递系统来保护mRNA并促进其进入细胞,但这种传递系统在传统意义上不被视为佐剂。然而,一些研究正在进行中,以探索在mRNA疫苗中使用佐剂以增强其有效性,特别是对于可能对疫苗有较弱免疫反应的某些人群,如老年人。
4.7.基于蛋白质亚单位的疫苗
基于蛋白质亚单位的疫苗仅包含来自病原体的特定蛋白质或蛋白质,而不是整个病原体。佐剂通常与基于蛋白质亚单位的疫苗一起使用,以通过增加对蛋白质抗原的免疫反应来增强其有效性。铝盐(如氢氧化铝)是最常用的基于蛋白质亚单位疫苗的佐剂,因为它们已被证明可以增强对抗原的抗体反应。其他佐剂,如MF59(油包水乳液)、AS03(角鲨烯油包水乳液)和AS04(氢氧化铝和MPL),也已用于基于蛋白质亚单位的疫苗中以提高其免疫原性。此外,正在研究使用Toll样受体激动剂等新型佐剂与基于蛋白质亚单位的疫苗一起使用,以进一步增强其免疫反应。
5.疫苗佐剂的临床试验和许可
开发含佐剂的疫苗是一项艰巨的任务,可能需要数年时间,因为必须确保疫苗的每个组分单独和组合使用时都兼容。美国食品和药物管理局生物制品评估和研究中心(CBER)发布了一份指南,以促进新疫苗配方的开发,以应对开发针对传染病疫苗的紧迫需求。指南建议从使用适当的动物模型进行临床前测试开始,以评估配方(包括佐剂)的安全性和免疫原性,以及佐剂对免疫反应的影响。必须包括单独的佐剂和抗原对照组,以提供佐剂效应的证据。免疫原性评估可能包括体液和细胞反应,如果疾病有动物模型,可以获得初步的保护效力信息。在临床前测试和疫苗配方的良好生产规范(GMP)生产之后,开始人体临床试验。I期研究评估健康个体的安全性和剂量,获得初步的免疫原性信息。IIa期试验涉及数百名志愿者,以评估免疫原性、耐受性和安全性。当测试进入IIb/III期时,重点是确定疫苗目标人群中的免疫原性和效力,随着参与志愿者人数的增加,研究持续时间也在增加。
确认疫苗的安全性和有效性后,疫苗可以获得许可并上市销售。然而,疫苗在IV期进行上市后安全监测,以评估其他罕见的不良反应。这些活动的目的是确保根据安全监测的结果采取适当的行动。监管机构严格应用药物警戒流程,以评估许可后出现的潜在安全信号。然而,评估试图建立与疫苗接种因果关系的研究所可能是复杂的和不确定的,尽管许可后有大量安全信息。
在某些情况下,疫苗在获得许可后因证实疫苗与不良事件之间存在因果关系或因效力不佳改变了收益-风险比而被撤回。虽然也有一些例子表明疫苗接种与不良事件之间的所谓因果关系被证明是没有根据的。疫苗制造商和监管机构在安全信号监测或报告新的重要不良事件时采取迅速行动。他们将证据迅速传达给医疗专业人员和公众,以便对最新的收益-风险概况做出明智的决策。
6.疫苗佐剂的临床试验示例
6.1.乳液
MF59是开发能够引发针对HIV的体液和细胞免疫反应的疫苗的一个例子,这对于预防HIV感染是理想的。在一项I期临床试验中,研究了DNA初免后用重组包膜糖蛋白加MF59佐剂增强的联合疫苗方案在未感染HIV的成年人中的安全性和免疫反应。此外,正在II期临床试验中评估含和不含MF59佐剂的灭活流感A/H9N2疫苗在门诊成人中的安全性。Montanide ISA 51和Montanide ISA 720是两种已在临床研究中调查的水包油乳液佐剂。它们具有不同的油水比率。Montanide ISA 51已在古巴的疟疾疫苗I期和流感疫苗II期研究中进行了评估,并已在古巴获得治疗性肺癌疫苗的许可。Montanide ISA 720已在疟疾疫苗的II期临床试验中进行了测试。这两种佐剂都已被证明可以促进有效的免疫反应,特别是增强特定的细胞毒性T淋巴细胞(CTL)反应。然而,观察到短暂的副作用,如发烧、头痛或类似流感的症状,尽管两者似乎都能很好地耐受。AS03佐剂在赛诺菲H1N1流感疫苗中在健康成人和老年人群不同剂量水平下进行了测试,以了解身体对不同强度的H1N1流感疫苗的反应,无论是单独使用还是与“佐剂”一起使用。
6.2.基于铝的佐剂
在一项I期临床试验中,评估了单剂量默克0657nI金黄色葡萄球菌疫苗加或不加默克铝佐剂的安全性、耐受性和免疫原性。此外,还评估了MN重组可溶性gp120/HIV-1(MN rsgp120/HIV-1)与QS21有或无铝佐剂结合使用的安全性和免疫原性。
6.3.基于脂质的佐剂
脂质材料自发现其独特的囊泡结构非常适合包裹各种生物活性物质(如DNA和脂肪酸)以来,一直被用作疫苗佐剂。在早期,科学家专注于脂质A,这是LPS的疏水锚,被认为是一种有效的佐剂,可以显著增加体液和细胞免疫反应。然而,由于其高毒性,基于脂质A的佐剂被认为不适合人类疫苗。相反,GLA-SE和GLA-AF都是脂质A类似物,被发现在增强对H5N1的保护方面特别有效,毒性低,副作用有限。GLA-AF也已作为乳液在许多疫苗中作为替代品进行了测试,最值得注意的是在大流行流感中。
6.4.基于Toll样受体(TLR)激动剂的佐剂
TLR3激动剂Poly-ICLC已在治疗黑色素瘤患者的佐剂疫苗安全性研究中进行了研究。这是一项I期开放标签剂量递增研究,研究TLR3激动剂Poly-ICLC作为高风险黑色素瘤患者NY-ESO-1蛋白疫苗的佐剂。佐剂疫苗治疗的目标是训练内源性免疫系统识别和靶向最小残留疾病。
6.5.皂苷
基于皂苷的OPT-821已在三价神经节苷脂在临床III期试验中用于无病生存的肉瘤患者。如果三价疫苗能刺激患者的免疫系统产生识别和靶向GM2、GD2和GM3糖的抗体,那么患者的抗体可能会攻击并杀死任何剩余的肉瘤细胞,从而可能预防肉瘤的复发。MatrixMTM也在大流行流感和RSV疫苗的I期和II期临床试验中进行了测试,显示出安全且耐受性良好,增强了体液和细胞免疫反应。其他基于皂苷的佐剂,如QS-21,已在癌症疫苗和传染病疫苗的临床试验中进行了评估,并显示出能诱导强烈的免疫反应并提高疫苗效力。然而,它们的复杂结构和可变组成可能会影响它们的一致性和可复制性,它们的潜在毒性和溶血活性需要在临床前和临床研究中仔细评估。
6.6.核苷酸
CpG ODN、dsRNA和IL-12 DNA等佐剂成分是激活模式识别受体(PRRs)以刺激免疫反应的核苷酸基佐剂的例子。例如,dsRNA可以分泌IFN-a和IFN-c等细胞因子,通过TLR3、MDA-5和NLRP3炎症体信号传导,目前正在进行流感和狂犬病疫苗的临床试验。用IL-12 DNA佐剂的DNA疫苗被引入以提供针对广泛HIV变体的有效保护,最近的试验表明它们耐受性良好,可以增强免疫反应。Pika佐剂是另一种核苷酸基佐剂,是稳定的卡那霉素和钙的dsRNA合成类似物,促进干扰素、IL-2和IL-12的产生。这种佐剂可以将主要产生体液免疫的预防性疫苗转变为具有强大细胞免疫的治疗性疫苗。
6.7.细胞因子
在最近的研究中,分子佐剂已被证明能有效刺激免疫反应,特别是在亚单位疫苗中。例如,IL-2和GM-CSF等细胞因子已在针对口蹄疫的疫苗中进行了研究,GM-CSF目前正在评估用于乙型肝炎和HIV疫苗。其佐剂效应归因于其促进巨噬细胞分化和增殖,以及激活抗原呈递细胞的能力。同样,IL-12和IL-15作为佐剂在一项正在进行的I期临床试验的HIV疫苗中被使用。这些细胞因子已证明能够刺激NK细胞和T细胞的增殖。
6.8.病毒体
病毒体是包膜病毒样颗粒,已在欧洲获得许可,用于针对甲型肝炎和流感的疫苗,并已在恶性疟原虫疟疾和慢性丙型肝炎疫苗的临床试验中使用。
6.9.肽
肽,MUC1-聚ICLC疫苗正在II期试验中进行测试,旨在评估在因有晚期腺瘤病史而增加结直肠癌风险的受试者中,MUC1疫苗的抗体和T细胞反应。MUC1-聚ICLC疫苗正在开发中,以防止息肉发展成结直肠癌,并防止息肉复发,这有助于体内免疫系统识别MUC1的变化,这些变化伴随着向癌症的进展,并消除产生异常的细胞。
6.10.其他
其他形式的佐剂也在临床试验中进行调查。一项I期临床研究针对研究性的PIKA(基于聚肌苷酸-聚胞苷酸的佐剂)狂犬病疫苗,包括灭活和纯化的狂犬病病毒和PIKA佐剂,以评估疫苗组合在健康成年志愿者中的临床安全性,并根据加速疫苗接种方案评估疫苗的效力。Mayo Clinic与Agri-King Corporation联合开发了一种新型合生元AKSB(Agri-King合生元)。一项针对正常人类志愿者(65岁以上)的AKSB的I期安慰剂对照试验,旨在研究当患者同时接受流感疫苗时,这种益生菌的安全性。磷酸钙,以羟基磷灰石的形式,已在法国获得许可,用于白喉、破伤风、百日咳和脊髓灰质炎疫苗。磷酸钙被认为是人体内的天然化合物,耐受性良好,使其成为可能替代铝佐剂的潜在替代品,铝佐剂可能会产生不良副作用。细菌鞭毛蛋白,TLR5的配体,也显示出可导致混合Th1和Th2反应的佐剂效应。在临床试验中,双价P. aeruginosa鞭毛蛋白佐剂疫苗帮助囊性纤维化患者降低了感染P. aeruginosa的风险。多糖是另一种潜在的佐剂,可以增强疫苗的免疫反应,并促进细胞免疫、体液免疫和粘膜免疫。还有一些新型佐剂结合了上述几种佐剂,有效成分协同作用以产生最佳的免疫反应。
7.针对COVID-19的疫苗佐剂
COVID-19大流行突显了开发安全有效疫苗以控制SARS-CoV-2病毒传播的需求。开发理想的疫苗需要广泛的研究和资源,以确保其满足当前形势的需求。疫苗旨在诱导保护性免疫反应,可以预防或减轻病毒感染的严重程度。
7.1.COVID-19疫苗中佐剂的好处
在COVID-19疫苗中使用佐剂有几个原因/动机:1)一个有效的COVID-19疫苗的主要要求之一是其能够刺激强大的免疫反应,能够产生高水平的中和抗体。为了实现这一点,疫苗可能需要多剂或佐剂。佐剂可以帮助减少疫苗中所需的抗原量,从而降低其成本。2)在SARS-CoV-2疫苗中结合适当的佐剂可以通过减少产生保护性免疫反应所需的抗原量来满足这些要求。疫苗的生产和分发应该是成本效益高且可扩展的,以满足压倒性的需求。鉴于大流行影响全球大多数国家,迫切需要一种可以快速高效生产和分发的疫苗。3)此外,佐剂还可以通过提供持久的免疫反应并扩大其对病毒不同株的保护范围来增强疫苗的效力。因此,针对COVID-19的佐剂疫苗的研发对于开发安全、有效和成本效益高的疫苗以控制大流行至关重要。
7.2.针对Covid-19的许可佐剂和候选物
NVX-CoV2373是Novavax开发的一种有前景的疫苗候选物,用于预防COVID-19。它是一种基于蛋白质的疫苗,使用引起COVID-19的SARS-CoV-2病毒的遗传序列创建。S蛋白是COVID-19疫苗的关键靶标,因为它是病毒附着和感染人类细胞的主要手段。为了增强免疫反应并刺激高水平的中和抗体,NVX-CoV2373与Novavax的专利基于皂苷的Matrix-M™佐剂配方。这种佐剂经过广泛测试,并通过刺激抗原呈递细胞进入注射部位并在局部淋巴结中增强抗原呈递,从而增强免疫反应,表现出强大且耐受良好的效果。这种基于蛋白质的疫苗候选物旨在教会免疫系统如何识别和对抗SARS-CoV-2病毒,提供针对COVID-19的保护。临床试验表明,NVX-CoV2373在预防COVID-19方面非常有效,总体有效性超过90%。获批后,NVX-CoV2373在抗击COVID-19中可能发挥关键作用,特别是在其他疫苗可能不太容易获得或有效的地区。世界各地已授权紧急使用几种COVID-19疫苗,其中一些使用了佐剂。例如,阿斯利康COVID-19疫苗使用了MF59佐剂,这是一种油包水乳液角鲨烯油,以增强疫苗的免疫反应。科兴COVID-19疫苗使用了铝佐剂,这是一种有助于增强免疫反应的铝盐。
图6.疫苗开发的演变阶段。
8.新疫苗佐剂的新兴发展
8.1.新型佐剂的设计原则
为了开发有效的佐剂疫苗,了解佐剂的工作原理并遵循一些设计原则是很重要的。问题导向原则涉及考虑四个主要问题:(1) 预防特定病原体引起的疾病所需的免疫反应类型,(2) 能够诱导所需免疫反应的相关先天免疫细胞,(3) 这些先天细胞亚群在体内的定位,以及 (4) 这些细胞上模式识别受体(PRRs)的表达。基于这些问题,在设计疫苗佐剂时需要考虑四个步骤。首先,应确定疫苗效力所需的免疫效应元素类型。这应考虑抗原类型、目标细胞亚群和表型以及免疫途径,以指导传递系统和免疫刺激剂的选择。由于PRRs是产生有效疫苗生成的关键靶标,因此在设计疫苗佐剂时,评估相关先天免疫细胞在体内的定位和目标细胞上的PRR表达非常重要。不同的PRR信号通路可能被用来开发针对不同侵害的定制反应。其次,应基于对免疫识别和保护的分子机制的理解来确定合适的疫苗抗原。合适的抗原还应能够在目标人群中实现疫苗诱导的反应定位。此外,疫苗必须向适当的细胞群体呈现足够数量的正确构象的抗原,以诱导免疫反应保护,同时考虑诱导炎症反应的耐受性和安全性问题。第三,佐剂需要一个传递系统,无论是合成的还是天然的。这需要设计感兴趣的抗原的适当传递方式,结合相关的免疫刺激剂。第四,疫苗和佐剂的制备过程应该简单。例如,如果不需要特殊的乳化剂,生产过程就更简单。如果佐剂与抗原的比例低,可能会增加疫苗改进的范围。
8.2.新型疫苗的佐剂配方
已经为已许可产品中的佐剂建立了几种配方方法。这些包括用作吸附剂的不溶性铝盐、易于注射的低油含量、油包水乳液和脂质体传递系统。虽然成分不同,但这些系统在结构上有一些显著的相似之处,它们都是作为纳米颗粒制造的。此外,这些系统可以作为抗原和免疫增强剂(包括TLR激动剂)的有效“传递系统”。适当选择佐剂的免疫刺激剂和配方成分对于诱导针对控制目标病原体的适当免疫反应至关重要。同一免疫调节分子的不同配方可能会诱导显著不同的免疫反应,如在疟疾疫苗计划中所示。例如,与AS02配方的RTS,S疫苗候选物保护了七个疫苗接种者中的六个免受感染,而相同的抗原与AS03或AS04配方的保护率分别为七个中的两个或八个中的一个。为了构建改进的佐剂,确保每个组分都是必要的并增加明确的价值,同时不引入重大的不合理责任至关重要。AS01是目前最成功的许可产品中包含的佐剂,对带状疱疹的有效性>97%。AS01佐剂的开发基于两个关键组分,MPL和QS-21,当一起使用时会产生先天激活的协同作用。这种协同作用无法通过任一分子单独实现,并且开发了一种脂质体传递系统,将两种免疫增强剂共同传递给相同的免疫细胞群体。此外,脂质体配方在减少QS-21诱导显著局部和系统反应原性方面也有效。然而,新型系统疫苗学方法可以用来识别新的佐剂途径和配方,这些可以用来设计下一代佐剂。
8.3.推进系统疫苗学
Bali等人提出了一种基于系统疫苗学的跨学科方法,以加速临床中佐剂的发现和开发,该方法涉及早期使用人类研究来生成“组学”数据,这些数据可以用来制定关于候选佐剂如何刺激强大和持久的抗原特异性T和B细胞反应的新假设。然后可以在动物模型中重新测试这些假设,随后得到的机制见解可以用来设计新的佐剂概念。所提出的佐剂开发框架更加强调在它们的发展管道早期(0/I期)在小型临床试验中测试许多潜在的佐剂概念,这可以快速测试新的佐剂并使用系统疫苗学方法获得机制见解。此外,系统疫苗学方法可以用来定义佐剂的作用机制,以及配方的作用机制、疫苗接种后不久发生的不良反应的潜在机制,以及疫苗传递的最佳配方的合理设计。总体而言,这种基于系统疫苗学的跨学科方法有潜力转变佐剂的科学并振兴新型佐剂的开发,以用于疫苗。
8.4.非侵入性疫苗传递
非侵入性疫苗传递的研究是一个关键焦点,可能对全球大规模疫苗接种活动产生重大影响。开发安全、有效和低成本的疫苗配方和佐剂,以产生期望的免疫反应和长期免疫,是一个优先事项。广泛的研究已经导致了几个新型佐剂的开发,这些佐剂目前正在临床试验中评估或已获得许可。一个研究重点是开发含有脂质的安全并提高非侵入性传递的疫苗效力的佐剂。然而,关于佐剂分子刺激后细胞表面受体之间的相互作用以及这些佐剂与现有或新型配方的兼容性,还需要更多信息。随着我们对免疫保护所涉及的分子机制的理解的提高和合成化学新方法的发展,预计疫苗开发将取得突破。新技术开发,如新的糖苷缀合方法、反向疫苗学和下一代测序技术,应该会导致针对HBV、百日咳毒素、莱姆病和HPV等疾病的新型疫苗策略,无论是否使用佐剂。研究界旨在通过引入新的免疫刺激剂和结合效力、持久记忆免疫反应和安全性的新型传递系统,确保高水平的广泛保护。这种新方法将不再仅仅依赖于结构疫苗学,因为目标表位的变异性和新病原体和肿瘤抗原的不断出现。
9.结论和展望
佐剂在近一个世纪的疫苗开发中发挥了至关重要的作用,增强了免疫原性。最初,佐剂的选择大多是经验性的,但最近的进展已经导致了更有针对性和合理的方法。对免疫系统的更深入理解使得开发更有效的疫苗配方成为可能。本综述概述了疫苗中使用的佐剂,从传统疫苗到COVID-19疫苗,重点关注它们的类型、对免疫反应的作用机制以及在疫苗配方中的作用。这些见解为选择适合传统和冠状病毒疫苗的佐剂奠定了基础。
了解各种佐剂对免疫反应的影响、它们与不同抗原类型和疫苗平台的协同作用,以及对这些佐剂的全面分析,将有助于选择提供必要免疫保护的佐剂。像基于铝的盐、TLR激动剂、乳液以及其他新型选项等佐剂具有独特的物理化学属性,显著影响免疫反应的强度、持续时间和类型。这些新型佐剂已经增强了流感疫苗和乙型肝炎和HPV疫苗。
随着COVID-19等新兴疾病的持续挑战和寻找更明确的治疗方法,开发安全有效的疫苗至关重要。更有信息的佐剂和抗原选择不仅能够增强对传统疫苗反应不佳的人群的保护,而且还可以开辟预防应用之外的新途径。这种方法在应对当前和未来的全球健康挑战中可能至关重要。
识别微信二维码,添加生物制品圈小编,符合条件者即可加入
生物制品微信群!
请注明:姓名+研究方向!
版
权
声
明
本公众号所有转载文章系出于传递更多信息之目的,且明确注明来源和作者,不希望被转载的媒体或个人可与我们联系(cbplib@163.com),我们将立即进行删除处理。所有文章仅代表作者观点,不代表本站立场。
疫苗
分析
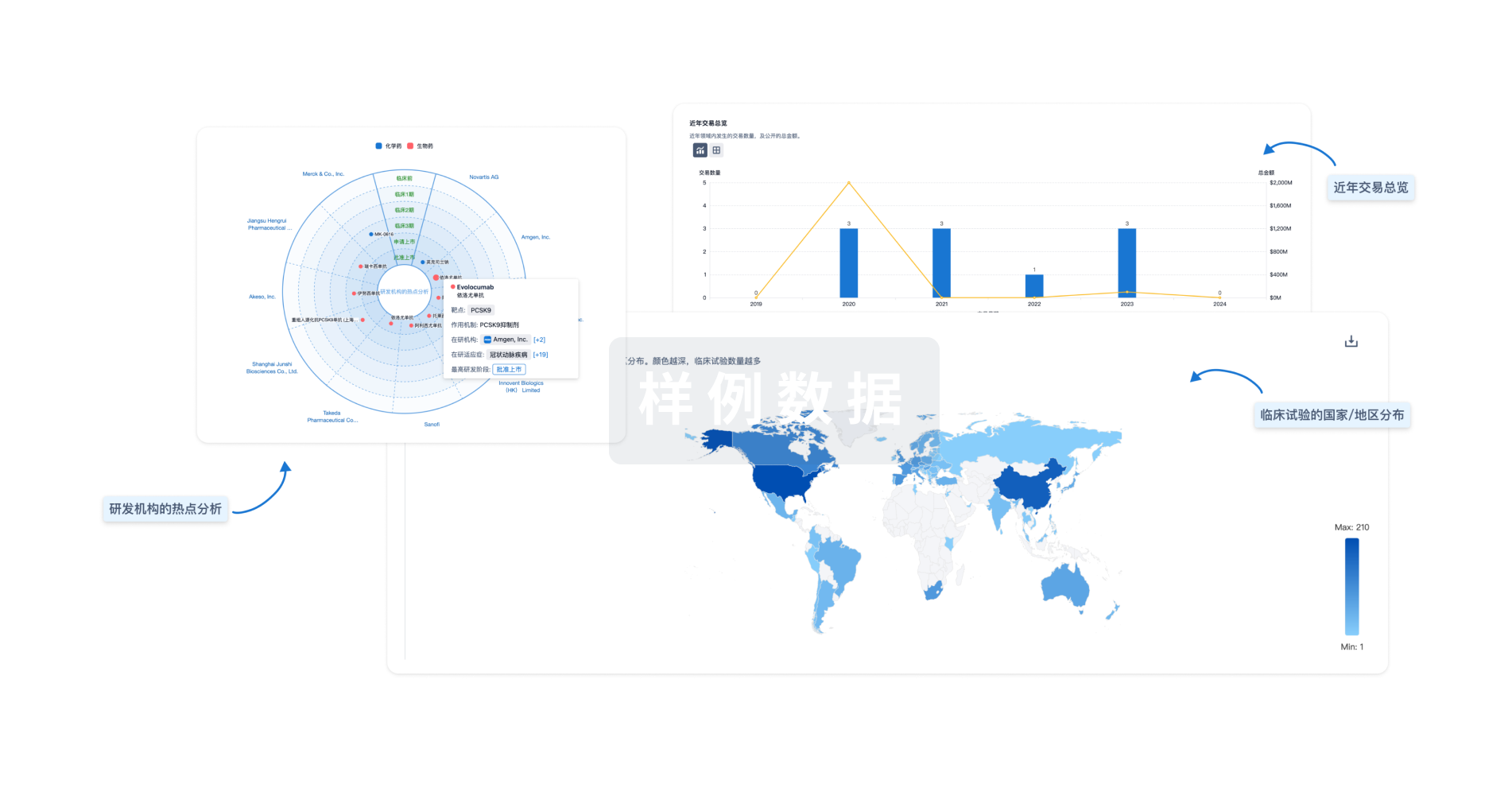
对领域进行一次全面的分析。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用

