预约演示
更新于:2025-05-07
INCLIVA
更新于:2025-05-07
概览
标签
其他疾病
肿瘤
神经系统疾病
生物药
小分子化药
疾病领域得分
一眼洞穿机构专注的疾病领域
暂无数据
技术平台
公司药物应用最多的技术
暂无数据
靶点
公司最常开发的靶点
暂无数据
| 排名前五的药物类型 | 数量 |
|---|---|
| 生物药 | 2 |
| 小分子化药 | 1 |
| 排名前五的靶点 | 数量 |
|---|---|
| ABCC3 | 2 |
| PPAR(过氧化物酶体增殖物活化受体) | 1 |
关联
3
项与 INCLIVA 相关的药物11
项与 INCLIVA 相关的临床试验NCT05343611
Combining Vitamin E-functionalized CHOcolate With Physical Exercise to Reduce the risK Of Protein Energy Malnutrition in Pre-dementia AGEd People
We hypothesize that the antioxidant and cytoprotective functions of vitamin E combined with the cortisol-lowering effect of chocolate polyphenols and physical activity may help prevent the age-dependent decline of mitochondrial function and nutrient metabolism in skeletal muscle, key underpinning events in protein-energy malnutrition (PEM) and muscle wasting in the elderly. To test this hypothesis, a vitamin E functionalized dark chocolate rich in polyphenols will be developed with the collaboration of Nestlè Company, and its effects will be investigated combined with physical activity in a 6-month randomized case-control trial on pre-dementia elderly patients, a well-defined population of subjects at risk of undernutrition and frailty. Subjects stabilized on a protein-rich diet (0.9-1.0 g protein/Kg ideal body weight/day) and physical exercise program (High Intensity Interval Training specifically developed for these subjects), will be randomized in 3 groups (n = 34 each): controls (Group A) will maintain the baseline diet and cases will receive either 30 g/day of dark chocolate containing 500 mg total polyphenols (corresponding to 60 mg epicatechin) and 100 mg vitamin E (as RRR-alpha-tocopherol) (Group B) or the high polyphenol chocolate without additional vitamin E (Group C). Diet will be isocaloric and with the same intake of polyphenols and vitamin E in the 3 groups. Muscle mass will be the primary endpoint and other clinical endpoints will include neurocognitive status and previously identified biomolecular indices of frailty in pre-dementia patients. Muscle biopsies will be collected to assess myocyte contraction and mitochondrial metabolism. Laboratory endpoints will include the nutritional compliance to the proposed intervention (blood polyphenols and vitamin E status and metabolism), 24-h salivary cortisol, steroid hormones and IGF-1, and molecular indices of inflammation, oxidant stress, cell death and autophagy. These parameters will be investigated in muscle and blood cells by state-of-the-art omics techniques. Molecular and nutritional findings will also be confirmed in vitro using skeletal myotubes, blood leukocytes and neural cell lines. Clinical and laboratory results will be processed by a dedicated bioinformatics platform (developed with the external collaboration of the omics company Molecular Horizon Srl) to interpret the molecular response to the nutritional intervention and to personalize its application.
开始日期2022-05-01 |
申办/合作机构  University of Verona University of Verona [+3] |
NCT04850300
Efficiency Assessment of the Methodology for the Follow-up of Patients With Knee Prostheses
Total knee arthroplasty (TKA) is currently the international standard for the treatment of degenerative and rheumatological diseases of the knee joint, as well as certain types of fractures. Although TKA is a procedure that has been shown to be effective in relieving pain and improving function in patients with osteoarthritis, approximately 20% of patients are dissatisfied with the results. Traditional methods of assessing the outcome after joint arthroplasty often focus on objective indicators of surgery and neglect the needs and opinions of patients. Because of this, this research project has the aim to know the effectiveness of two models of stabilization of total knee prostheses on the functionality achieved and perceived by the patient, as well as in the knee joint biomechanics during movement in activities of daily life. On the other hand, as a secondary objective, we propose to determine prognostic biomarkers of knee prosthesis function based on radiological information, quantification of cytokines, intra-articular markers, and biomechanical functional evaluation that correlate and predict a correct evolution of patients with a knee replacement.
To carry out these objectives, 80 participants will be included with an indication to perform total knee joint replacement surgery. Participants will be randomized allocated into two groups: i. participants with a prosthesis with medial condylar stabilization ii. participants with a traditional prosthesis with central pivot stabilization. Participants will be evaluated at five-times: before surgery, immediate postsurgical, at 3 months of evolution, 6 months of evolution, and one year of evolution.
To carry out these objectives, 80 participants will be included with an indication to perform total knee joint replacement surgery. Participants will be randomized allocated into two groups: i. participants with a prosthesis with medial condylar stabilization ii. participants with a traditional prosthesis with central pivot stabilization. Participants will be evaluated at five-times: before surgery, immediate postsurgical, at 3 months of evolution, 6 months of evolution, and one year of evolution.
开始日期2021-09-27 |
申办/合作机构 |
NCT04795271
Biomechanical Study of Patients With Diabetic Foot for the Establishment of a Preventive Orthopedic Treatment Protocol for Major Complications
Spain is the country with the second-highest rate of population amputation due to the development of ulcers, behind the United States, where 2 out of 3 non-traumatic amputations derive from diabetes. This is why the main objective of this project is to establish a study protocol for alterations in plantar pressures and gait abnormalities in diabetic patients, parallel to the preventive orthopedic treatment of major complications such as Charcot's foot, ulcers in the plantar support surface, and amputations. The study methodology will be based on the evaluation prior to the personalized orthopedic treatment for each patient and the evaluation after the orthopedic treatment, specifically at one week, one month, three months, and six months after the treatment. At each evaluation time, plantar pressure and reaction forces during walking and local infrared thermography will be analyzed. In the basal and final evaluation at six months, the muscular strength and range of motion of the lower limbs will also be evaluated. The orthopedic intervention is personalized to the requirements of the patients and is based on the use of an insole with the possible inclusion of orthopedic footwear in order to reduce plantar pressure.
开始日期2020-11-12 |
申办/合作机构 |
100 项与 INCLIVA 相关的临床结果
登录后查看更多信息
0 项与 INCLIVA 相关的专利(医药)
登录后查看更多信息
100 项与 INCLIVA 相关的药物交易
登录后查看更多信息
100 项与 INCLIVA 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年02月08日管线快照
管线布局中药物为当前组织机构及其子机构作为药物机构进行统计,早期临床1期并入临床1期,临床1/2期并入临床2期,临床2/3期并入临床3期
临床前
3
登录后查看更多信息
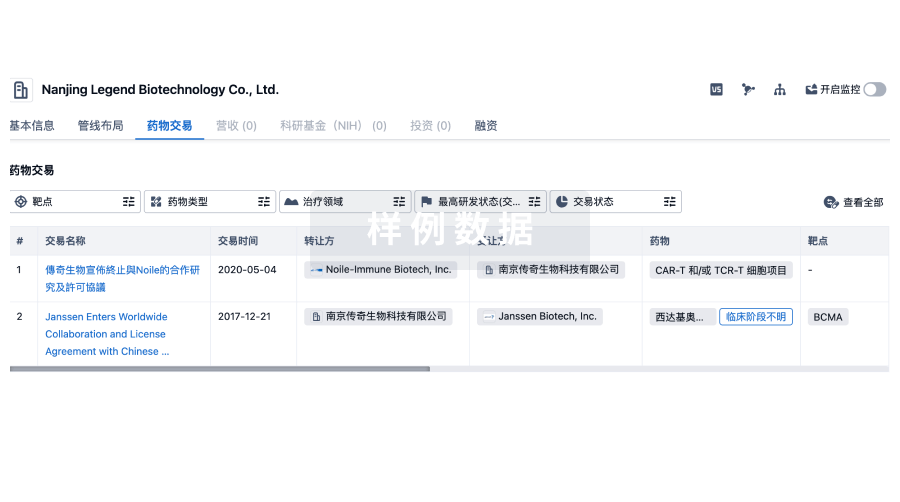
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
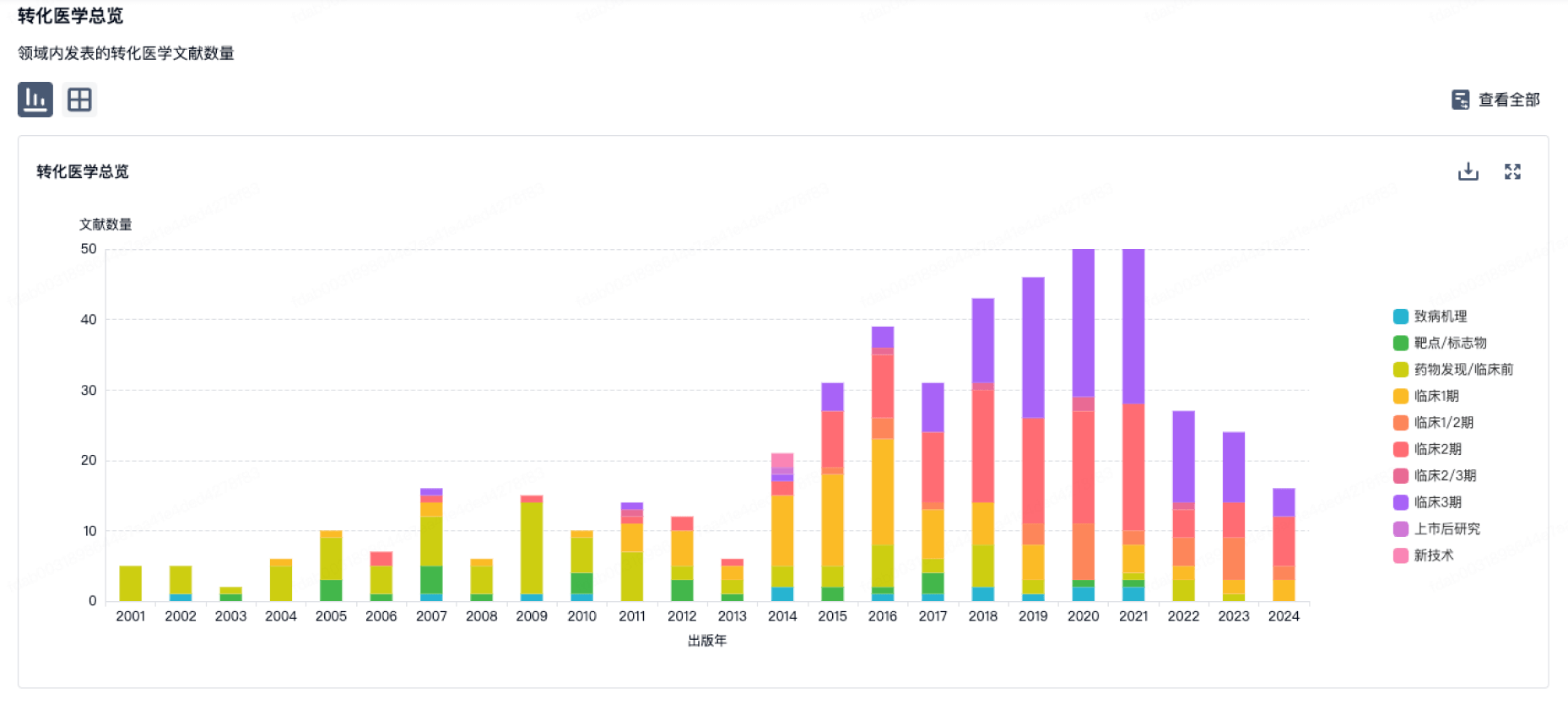
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
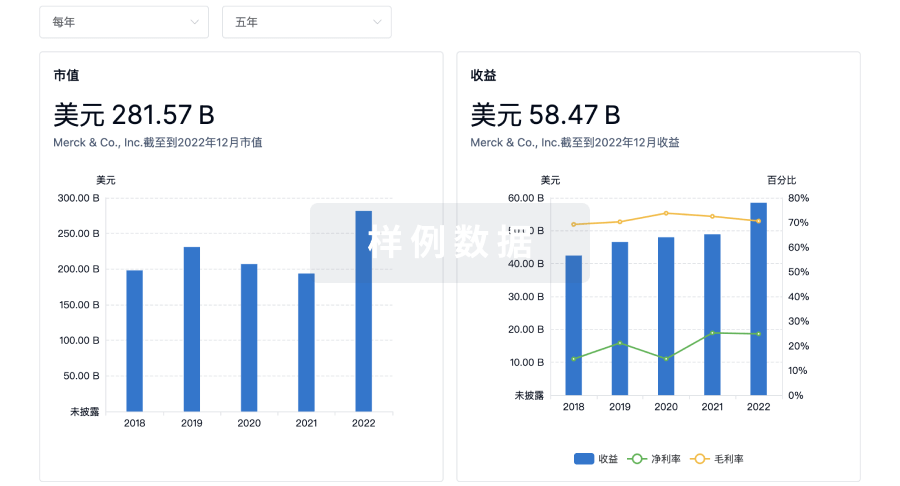
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
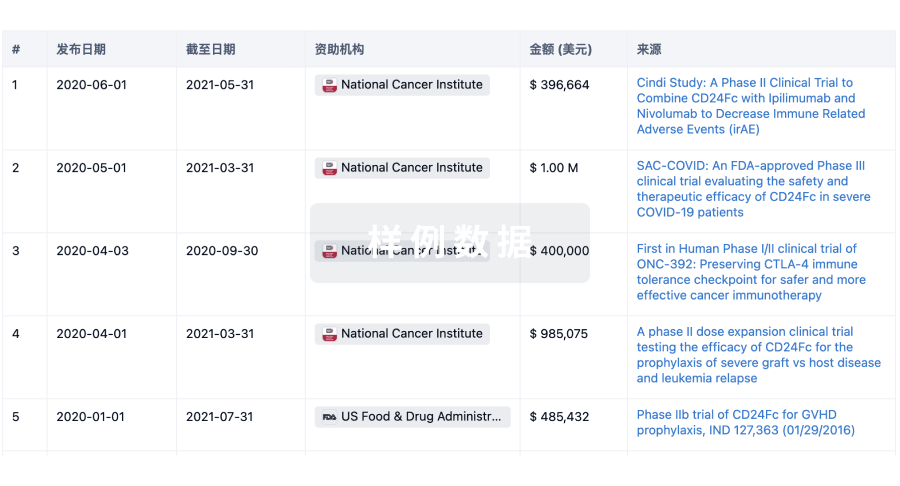
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
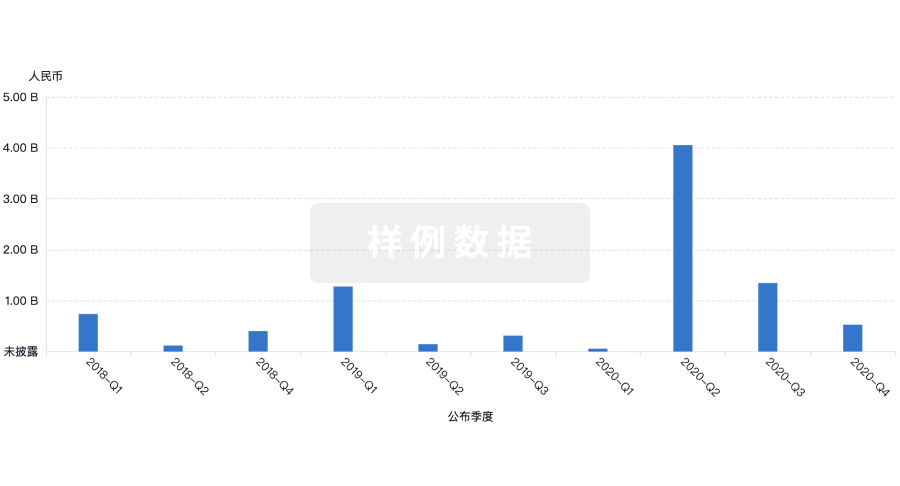
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
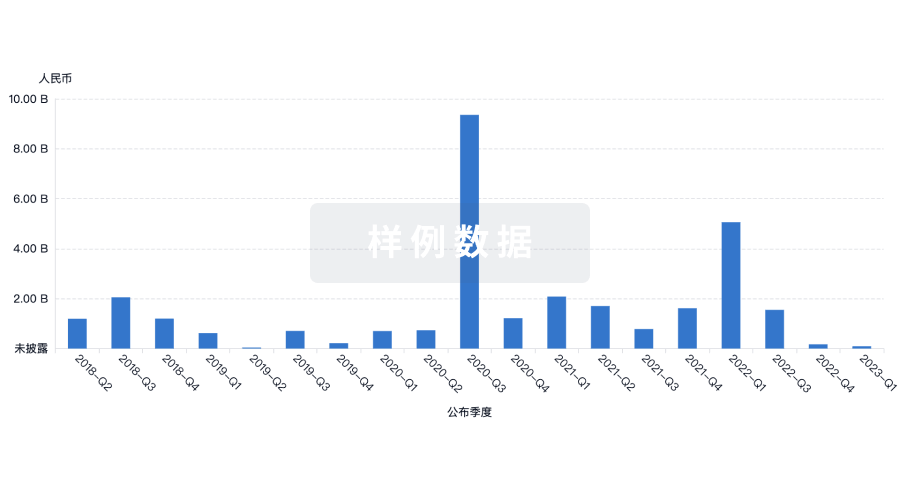
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
