预约演示
更新于:2026-06-06
Porfiromycin
更新于:2026-06-06
概要
基本信息
药物类型 小分子化药 |
别名 Porfiromycin (USAN/INN)、Porfiromycine、Porphyromycin + [6] |
靶点 |
作用方式 抑制剂 |
作用机制 DNA抑制剂(DNA抑制剂)、DNA烷化剂 |
治疗领域 |
在研适应症- |
非在研适应症 |
原研机构 |
在研机构- |
最高研发阶段终止临床3期 |
首次获批日期- |
最高研发阶段(中国)- |
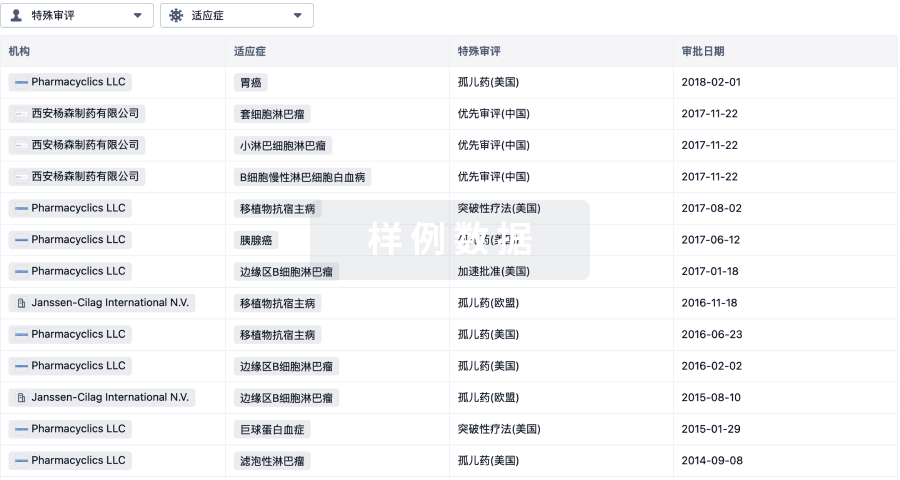
特殊审评孤儿药 (美国) |
登录后查看时间轴
结构/序列
分子式C16H20N4O5 |
InChIKeyHRHKSTOGXBBQCB-VFWICMBZSA-N |
CAS号801-52-5 |
关联
4
项与 Porfiromycin 相关的临床试验NCT02183246
A Phase III, Double-Blind, Randomized, Placebo-Controlled Study of Porfiromycin Used as an Adjuvant to Radiation Therapy in Postoperative Head and Neck Cancer Patients
Determination of efficacy and safety of porfiromycin versus placebo as an adjuvant to radiotherapy in postoperative head and neck a cancer patients as well as assessment of population pharmacokinetic parameters.
开始日期2000-05-01 |
申办/合作机构 |
NCT02209701
A Phase I Intensive Pharmacokinetic Study of Porfiromycin in Head and Neck Cancer and Other Cancer Patients With Solid Tumors Who Receive Radiation Therapy
Study to determine the steady-state pharmacokinetics and urinary excretion of porfiromycin and major metabolites in head and neck cancer and other cancer patients with solid tumors who receive radiation therapy.
开始日期1999-12-01 |
申办/合作机构 |
NCT00003328
A Phase III Double-Blind, Randomised, Placebo-Controlled Study of Porfiromycin When Used as an Adjuvant to Radiation Therapy in Patients With Head and Neck Cancer
RATIONALE: Radiation therapy uses high-energy x-rays to damage tumor cells. Drugs used in chemotherapy use different ways to stop tumor cells from dividing so they stop growing or die. It is not yet known whether radiation therapy followed by porfiromycin is more effective than radiation therapy alone in treating patients with head and neck cancer.
PURPOSE: Randomized double-blinded phase III trial to determine the effectiveness of radiation therapy followed by porfiromycin in treating patients with stage III or stage IV head and neck cancer.
PURPOSE: Randomized double-blinded phase III trial to determine the effectiveness of radiation therapy followed by porfiromycin in treating patients with stage III or stage IV head and neck cancer.
开始日期1997-12-01 |
申办/合作机构 |
100 项与 Porfiromycin 相关的临床结果
登录后查看更多信息
100 项与 Porfiromycin 相关的转化医学
登录后查看更多信息
100 项与 Porfiromycin 相关的专利(医药)
登录后查看更多信息
176
项与 Porfiromycin 相关的文献(医药)2026-04-03·EXPERT OPINION ON THERAPEUTIC TARGETS
Molecular understanding for therapeutic targeting of hypoxia in breast cancer
Review
作者: Angeli, Andrea ; Supuran, Claudiu T.
INTRODUCTION:
Breast cancer is one of the most widespread types of cancer, affecting millions of patients worldwide and although significant advances in its therapy have been achieved in the last decades, a large number of death still occur. Triple-negative breast cancer (TNBC) is the subtype associated with aggressive behavior, early metastasis, and limited therapeutic options, resulting in poor clinical outcomes for many affected patients. Many such tumors are frequently hypoxic.
AREAS COVERED:
Hypoxia is a hallmark of solid tumors, including breast cancers. Molecular events triggered by hypoxia are orchestrated by hypoxia-inducible factors (HIFs), which regulate transcription of genes involved in cell survival, invasion, angiogenesis, and resistance to chemo- and radio-therapy. Apart HIF itself, other potential molecular targets such as prolyl-hydroxylases (PHD), von Hippel-Lindau protein (VHL), monocarboxylate transporters (MCTs), Na+/H+ exchangers (NHEs), vacuolar ATPases (V-ATPase), anion exchangers (AEs), Na+ /HCO3- co-transporters (NBCs), vascular endothelial growth factor (VEGF) and carbonic anhydrases were identified as being involved in tumorigenesis.
EXPERT OPINION:
HIF-1α inhibitors (topotecan, digoxin, PX-478), hypoxia-activated prodrugs (evofosfamide, apaziquone, porfiromycin, tirapazamine, banoxantrone) and carbonic anhydrase IX/XII inhibitors (SLC-0111) are either used clinically or in clinical development for the management of hypoxic breast cancers.
2025-01-01·JOURNAL OF ETHNOPHARMACOLOGY
Multi-omics and bioinformatics for the investigation of therapeutic mechanism of roucongrong pill against postmenopausal osteoporosis
Article
作者: Guo, Junpeng ; Jiang, Tao ; Zhu, Xiaojuan ; Meng, Qianting ; Su, Xin ; Du, Xingchen ; Guo, Jiurui ; Li, Yufen ; Song, Wu ; Hu, Wanli ; Li, Chenhao
ETHNOPHARMACOLOGICAL RELEVANCE:
The Roucongrong Pill (RCRP), originating from the historical General Medical Collection of Royal Benevolence, is frequently used to treat postmenopausal osteoporosis (PMOP). Despite its prevalent application, the specific anti-osteoporotic mechanisms of RCRP remain to be elucidated.
AIM OF THE STUDY:
This study aims to elucidate the therapeutic mechanism of RCRP in the context of ovariectomy (OVX)-induced PMOP in rats. By employing an integrative approach, the research combines medicinal chemistry, gut microbiota (GM) profiling, metabolomics, MetOrigin traceability, network pharmacology, molecular docking, and molecular dynamics simulations to deliver a comprehensive analysis.
MATERIALS AND METHODS:
Sprague-Dawley (SD) rats underwent bilateral OVX to establish a PMOP model. The therapeutic efficacy of RCRP was evaluated through bone metrics (BMD, bone strength, BV/TV, Tb.Sp), hematoxylin and eosin (H&E) histological assessment, and bone metabolism markers (OPG, BALP, TRACP-5b, β-CTX, RANKL). Fecal metabolomics and 16S rDNA sequencing were employed to assess the influence of RCRP on GM and metabolite profiles. Furthermore, MetOrigin facilitated the traceability analysis of relevant metabolites. Molecular docking identified potential RCRP compounds with anti-PMOP activity, while their stability and protein interactions were assessed through molecular dynamics simulations. Network pharmacology further confirms the targets of action.
RESULTS:
RCRP alleviated PMOP in rats, enhancing bone strength, cortical and trabecular BMD, BV/TV, and serum OPG levels, while reducing Tb.Sp, serum BALP, TRACP-5b, β-CTX, and RANKL concentrations. A total of twenty-six distinct metabolites were identified, of which ten-tribufos, sulfoacetic acid, betamethasone dipropionate, 9-oxooctadeca-10,12,15-trienoic acid, menatetrenone, piperlongumine, maltopentaose, enol-phenylpyruvate, catechol, pentaacetate, and (+)-2-methylpropanoic acid-exhibited correlations with six GM species: Turicibacter, Roseburia, Colidextribacter, Helicobacter, Odoribacter, and Lachnoclostridium, as determined by Spearman's correlation analysis. Notably, MetOrigin revealed the microbial metabolism of taurine and hypotaurine, along with host-specific steroid hormone synthesis. Computational docking studies demonstrated robust interactions between five RCRP-derived steroids (hydroxyecdysone, corticosterone, trilostane, 5α-androstan-3,6,17-trione, and cortisol) and key enzymes (estradiol 17α-dehydrogenase and UDP-glucuronosyltransferase), suggesting a potential enhancement of therapeutic efficacy against PMOP. Furthermore, molecular dynamics simulations indicated stable interactions between hydroxyecdysone and two proteins, with binding free energies of -67.427 kJ/mol and -156.948 kJ/mol, respectively. Through network pharmacology and molecular docking approaches, potential targets of these metabolites were identified, including estrogen receptors ESR1 and ESR2, dual specificity phosphatase 6 (DUSP6), sex hormone-binding globulin (SHBG), prostaglandin E receptor 4 (PTGER4), cannabinoid receptor 2 (CNR2), cathepsin K (CTSK), and androgen receptor (AR).
CONCLUSIONS:
RCRP effectively mitigates OVX-induced bone loss in PMOP rats by modulating GM and associated metabolites, along with their potential targets and key metabolic pathways, including taurine and hypotaurine metabolism, as well as steroid hormone biosynthesis. These findings offer new insights into the therapeutic mechanisms by which RCRP may alleviate PMOP.
2020-10-09·ACS infectious diseases2区 · 医学
Screening an Established Natural Product Library Identifies Secondary Metabolites That Potentiate Conventional Antibiotics
2区 · 医学
Article
作者: Robert K. Ernst ; Karlie E. Cox ; Roberta J. Melander ; Richard Smith ; Christian Melander ; Anne E. Mattingly
Health organizations worldwide have warned that we are on the cusp of a "post-antibiotic era," necessitating new approaches to combat antibiotic resistant infections. One such approach is the development of antibiotic adjuvants, which have little or no inherent antibiotic activity at their active concentrations but instead potentiate the activity of antibiotics against antibiotic-resistant bacteria. Recently, we demonstrated that meridianin D, a natural product originally reported to have activity against Staphylococcus aureus and Mycobacterium tuberculosis, possesses the ability to reverse colistin resistance in colistin resistant bacteria. As most natural product screens typically involve screening for only certain activities (anticancer, antiviral, and antimicrobial are typical), we posited that the meridianin D discovery was not unique and there are potentially many natural products that have adjuvant activity. To explore this, the National Cancer Institute (NCI) Natural Product Library Set IV was screened for adjuvant activity using four classes of antibiotics (β-lactams, aminoglycosides, macrolides, and polymyxins) against three bacterial pathogens (methicillin-resistant Staphylococcus aureus (MRSA), Acinetobacter baumannii, and Klebsiella pneumoniae). Sixteen compounds suppressed β-lactam resistance in MRSA, five of which effected a 16-fold reduction in the oxacillin minimum inhibitory concentration (MIC). Two natural products effectively suppressed aminoglycoside resistance in both of the Gram-negative species tested, and no hits were observed with macrolides. In contrast, a larger number of natural product adjuvants were identified when screening against colistin-resistant strains of A. baumannii and K. pneumoniae. Nine compounds reduced the colistin MIC to its breakpoint or lower (up to a 1024-fold reduction). Clorobiocin, novobiocin, and prodigiosin were most effective, reducing the colistin MIC in K. pneumoniae strain B9 to 2 μg/mL at concentrations as low as 0.625, 2.5, and 1.25 μM, respectively. Restored sensitivity to colistin with these compounds does not appear to coincide with known mechanisms of colistin resistance.
1
项与 Porfiromycin 相关的新闻(医药)2026-04-15
·医研小憩
这本书出版于1998年,由C. Julian Rosenthal和Marvin Rotman主编。它系统性地探讨了如何将化疗(特别是通过持续静脉输注的方式)与放疗结合起来,以更有效地治疗癌症,并尽可能保留患者的器官功能。
第一部分:生物与化疗药物对放疗的调节 (第1-13章)
这部分是全书的理论和药物基础,解释了为什么以及如何让化疗来增强放疗的效果。第1章:概述:开篇点明主题。对于中期实体瘤,单纯手术或放疗常常无法根治,因为可能存在放疗抵抗的细胞或早期的微小转移。将化疗(尤其是持续输注)与放疗同时进行,可以产生“1+1>2”的协同作用,提高疗效,并有望实现器官保全。第2章:最佳放化疗方案安排:讨论了如何安排化疗和放疗的时间顺序才能达到最好效果。核心观点是,同时进行(化疗贯穿整个放疗过程)可能是最理想的“放射增敏”方式,比先化疗后放疗或先放疗后化疗效果更好。第3章:维甲酸和细胞因子与放疗联用:介绍了一些非传统化疗药物(如维甲酸、干扰素)与放疗联用的实验室和早期临床结果,显示它们也能抑制癌细胞生长、增强放疗效果,为联合治疗提供了新思路。第4章:5-氟尿嘧啶(5-FU)与放疗的作用机制:深入解释了最常用的化疗药5-FU是如何从细胞层面(如干扰DNA合成与修复)增强放疗效果的。这为临床上放弃一次性注射,转而采用持续输注5-FU提供了坚实的理论依据。第5章:铂类药物的早期临床试验:总结了顺铂等铂类药物作为“放射增敏剂”的早期研究,证实了其与放疗联用的可行性和初步疗效,为后续广泛应用奠定了基础。第6章:顺铂持续输注治疗肺癌:这是一个具体案例研究。对于无法手术的肺癌患者,采用低剂量、持续输注顺铂配合放疗,在保证疗效的同时,毒性比一次性大剂量注射更低,患者耐受性更好。本章还从药物代谢动力学角度进行了分析。第7章:铂类和5-FU的输注方案:进一步探讨了将铂类药物和5-FU这两种核心药物以不同输注方案(如交替输注)组合,用于治疗食管癌等实体瘤的实践经验。第8章:针对缺氧细胞的药物:肿瘤内部有些区域缺氧,这些细胞对放疗不敏感。本章介绍了专门针对这些缺氧细胞的药物(如丝裂霉素C、Porfiromycin),与放疗联用可以“查漏补缺”,更好地杀死全部肿瘤细胞。第9章:丝裂霉素C持续输注治疗肝转移癌:具体研究丝裂霉素C通过持续输注与放疗联用,治疗结肠癌肝转移,不仅可行,而且显示出明确的协同效应,为这类难治患者提供了新方法。第10章:紫杉醇与放疗联用:介绍了当时的新型化疗药紫杉醇。实验室证明它能将癌细胞阻滞在对放疗最敏感的时期(G2/M期),是一个强效的放射增敏剂。本章展望了其在肺癌、头颈癌等领域的应用前景。第11章:紫杉醇的96小时输注研究(药理学):详细报告了紫杉醇通过96小时持续输注的方式给药的I期临床试验,重点研究了其药物代谢动力学,确定了这种给药方式下的安全剂量和体内行为。第12章:紫杉醇持续输注联合放疗的I期研究:在上一章基础上,探索了将96小时输注紫杉醇与放疗同时使用的可行性和初步效果,确定了联合治疗时的最大耐受剂量,为后续研究铺路。第13章:阿霉素作为放疗增敏剂:讨论了另一种经典化疗药阿霉素与放疗的相互作用及临床应用,特别是在软组织肉瘤和肝癌中的协同效应。
第二部分:局部晚期恶性肿瘤放化疗后的器官保全 (第14-28章)
这部分聚焦于联合治疗最重要的临床目标之一:在治愈癌症的同时,保住器官及其功能。第14章:晚期疾病中器官保全是否可能?提出了全书的核心问题,并给出乐观展望:通过精心设计的放化疗,即使对于晚期肿瘤,器官保全也是可行的,但需要结合保守性手术和密切随访。第15章:肛管癌的结构与功能保全:详细介绍了在肛管癌中,采用放疗联合5-FU±丝裂霉素C,如何成功替代了需要永久性结肠造口的手术,成为该病的标准治疗方案。第16章:直肠癌的保肛管理:探讨了对于直肠癌,采用术前或术后放化疗(以5-FU持续输注为主),可以缩小肿瘤、提高手术保肛成功率,甚至使部分患者免于手术。第17章:晚期膀胱癌的放化疗:介绍了采用持续输注5-FU联合放疗治疗膀胱癌,可以使相当一部分患者避免全膀胱切除,保留膀胱功能,且早期肿瘤患者疗效优异。第18章:食管癌的联合治疗:总结了放化疗(常用5-FU+顺铂)在食管癌治疗中的作用,无论是作为术前新辅助治疗以提高手术切除率,还是作为根治性治疗以保全食管,都显示出重要价值。第19章:头颈癌器官保全:北美经验:系统回顾了北美在头颈癌(特别是喉癌)器官保全方面的历程。关键结论是:同步放化疗比诱导化疗后放疗更能提高局部控制率和保喉率,且不影响总生存。第20章:头颈癌器官保全:欧洲经验:从欧洲视角补充了相关经验,介绍了交替放化疗等不同策略,同样证实了同步治疗在保全器官和提高疗效方面的优势。第21章:鼻咽癌的放化疗根治:特别强调,由于鼻咽癌位置特殊且对化疗敏感,同步放化疗是其标准治疗方案,能显著提高局部晚期患者的治愈率。第22章:局部晚期口腔/口咽癌的新辅助化疗:探讨了在放疗前先进行诱导(新辅助)化疗,对于评估肿瘤反应、筛选适合器官保全治疗患者的价值。第23章:晚期口咽癌的动脉灌注化疗联合放疗:介绍了一种更局部的强化治疗方式——将化疗药物直接注入肿瘤供血动脉,同时联合放疗,以提高局部疗效。第24章:局部晚期喉癌的新辅助化疗:类似于第22章,但聚焦于喉癌,探讨新辅助化疗作为保喉策略一部分的疗效和患者选择。第25章:头颈癌局部复发的再程放疗:讨论了对于放疗后局部复发的头颈癌患者,在谨慎选择的前提下,采用低剂量顺铂增敏的再程放疗,仍可能获得控制并避免手术。第26章:不可切除非小细胞肺癌的放化疗加辅助手术:介绍了对于局部晚期肺癌,采用持续输注顺铂联合放疗后,对部分反应好的患者再进行手术切除的“三明治疗法”,旨在提高根治机会。第27章:妇科癌症的放化疗:概述了放化疗在宫颈癌、子宫内膜癌等妇科恶性肿瘤中的应用,能提高局部控制率,并可能减少手术范围。第28章:成人晚期软组织肉瘤的放化疗:总结了阿霉素等化疗药物与放疗联合,用于治疗局部晚期或转移性软组织肉瘤,可以缩小肿瘤、缓解症状,并为手术创造条件。
第三部分:未来方向——分子生物学进展 (第29-32章)
展望了基于癌症分子机制的新疗法,这些未来可能与放化疗结合,实现更精准、低毒的治疗。第29章:以细胞凋亡为靶点的药物开发:设计药物来主动触发癌细胞“程序性死亡”(凋亡),这可能与放化疗产生协同效应。第30章:抗血管生成剂在肺癌治疗中的潜力:通过切断肿瘤的血液供应来“饿死”肿瘤,这是一种全新的治疗思路,可能与传统放化疗联用。第31章:基因治疗及其与化疗的相互作用:从基因层面纠正错误(如导入p53抑癌基因),直接攻击癌细胞的根源,是当时的前沿探索。第32章:SV40病毒介导转化的细胞靶点:基础研究章节,研究病毒导致细胞癌变的机制,为理解癌变和寻找治疗靶点提供科学依据。
第四部分:放化疗诱发的癌变 (第33-34章)
客观看待联合治疗的潜在长期风险。第33章:电离辐射和化学药物的致突变机制:从基础科学角度解释放化疗为何可能损伤正常细胞的DNA,从而埋下未来癌变的种子。第34章:放化疗致癌:骨髓移植模型:以接受了大剂量放化疗和骨髓移植的患者为模型,他们后来发生第二种癌症(特别是白血病)的风险显著增加,这清晰地揭示了强化治疗的长期代价。
第五部分:癌症化学预防的进展 (第35-39章)
探讨如何用药物预防癌症的发生或复发。这部分与全书主题相呼应:既然强化治疗可能增加第二癌风险,那么就需要研究如何用药预防。第35章:肺癌的化学预防:探讨维甲酸等药物预防肺癌(尤其对吸烟高危人群和第二原发肺癌)的研究。第36章:抗雌激素药物预防乳腺癌的测试:介绍他莫昔芬等药物在预防高危人群乳腺癌方面的临床试验和价值。第37章:维甲酸、干扰素和他莫昔芬在乳腺癌中的活性与联合:研究这些药物单独或联合用于治疗或预防乳腺癌的活性。第38章:阿司匹林等前列腺素抑制剂预防结肠癌:介绍流行病学和实验研究发现,长期服用阿司匹林可能降低结肠癌风险,探讨其预防作用机制。第39章:根除幽门螺杆菌预防胃癌:介绍通过药物(奥美拉唑、克拉霉素)根除幽门螺杆菌感染,以预防胃癌这一具有里程碑意义的病因学预防策略。
第六部分:计算机技术在研究与临床中的应用 (第40章)第40章:计算机技术在肿瘤学研究和实践中的应用:最后一部分指出,面对日益复杂的治疗方案和海量医疗数据,利用计算机技术进行方案设计、数据分析、患者管理和临床决策支持,是实现精准和高效治疗不可或缺的工具。
全书核心总结:这本书是一部关于“同步放化疗”,特别是“持续输注化疗同步放疗”的里程碑式著作。它系统地论证了:理论正确:同步持续输注能最大化化疗的放射增敏作用。疗效显著:该模式能提高多种局部晚期实体瘤的局部控制率和生存率。革命性临床价值:其最大贡献是确立了“器官保全”作为癌症治疗的核心目标之一,极大改善了患者生活质量(如保喉、保肛、保膀胱)。全面视角:在展示疗效的同时,也冷静分析了急性毒性和诱发第二原发癌的长期风险,体现了科学的审慎。承前启后:既总结了以5-FU、顺铂为基础的经典方案,也引入了紫杉醇等新药,并展望了靶向治疗、基因治疗和化学预防的未来方向,为肿瘤学发展描绘了蓝图。
第一部分:生物与化疗药物对放疗的调节 (第1-13章)
这部分是全书的理论和药物基础,解释了为什么以及如何让化疗来增强放疗的效果。
第1章:输注化疗-放疗相互作用:概述
作者:C.J. Rosenthal 和 M. Rotman这本书要解决什么问题?在1990年代以前,对于许多局部晚期(肿瘤比较大但还没扩散到全身)的实体瘤,标准治疗往往是毁损性的手术(比如切掉整个喉咙、肛门或膀胱),或者单独放疗。但手术创伤大,影响生活质量;单独放疗有时又不足以根治肿瘤。这本书的核心,就是探索一种“鱼与熊掌兼得”的方法:用化疗来增强放疗的效果,从而既能治愈癌症,又能保住器官和功能。核心思想:“同步”和“持续输注”为什么要同步?化疗和放疗不是简单地先后使用。当化疗药正好存在于癌细胞中时进行放疗,两者能产生最强的协同杀伤作用,这叫“放射增敏”。为什么要持续输注?一次性打针(静脉推注)化疗,药物在血液里浓度像过山车,高峰时毒性大,低谷时又没效果。而持续静脉输注(像打点滴一样连续几天甚至几周给药),能让血液中药物的浓度保持稳定,确保在整个放疗期间,肿瘤细胞都“浸泡”在药物里,最大化协同作用。科学和临床依据:理论起源:这个想法40年前(约1950年代)就有人提出,直到1974年Nigro医生用持续输注5-氟尿嘧啶(5-FU)联合放疗成功治疗了拒绝手术的肛管癌患者,才真正在临床上打开局面。药物扩展:后来发现,不止5-FU,顺铂、丝裂霉素C、紫杉醇、阿霉素等多种化疗药,通过持续输注与放疗联用,都显示出很好的效果。大型试验证实:到90年代中期,多个大型III期临床试验(最高级别的证据)已经证明,这种同步放化疗模式在肛管癌、食管癌、头颈部癌、直肠癌、膀胱癌等疾病中,显著提高了患者的无病生存率和总生存率。临床价值:器官保全革命最经典的例子是肛管癌:以前必须切除肛门做永久性造口。现在,放疗+持续输注5-FU和丝裂霉素C成为标准治疗,绝大多数患者可以保住肛门正常排便。同样,在喉癌、膀胱癌、食管癌、直肠癌,同步放化疗都让“避免大手术、保留器官功能”成为可能。冷静看待代价:急性毒性增加:这种强化治疗肯定会增加治疗期间的副作用,比如严重的口腔/食管黏膜炎、腹泻、骨髓抑制(血细胞减少)等,但书中强调这些通常是可管理、可恢复的。长期风险:书中也前瞻性地提出了一个严肃问题:如此强烈的治疗,是否会损伤正常细胞,在多年后增加患者患上第二种新癌症(特别是白血病)的风险?这引出了本书后面关于“致癌风险”和“化学预防”的章节。未来展望:作者预言,未来的进步将来自:整合新的、靶向性更强的药物(如诱导细胞凋亡、抗血管生成的药物)。利用基因治疗等分子手段。研究如何用药物(化学预防)来降低治疗本身带来的长期致癌风险。
简而言之,第一章是全书的“总纲”,它宣告:同步持续输注放化疗是一个有坚实理论基础和临床证据的强大模式,它正在改变癌症治疗的目标——从“不惜一切代价切除肿瘤”转向“在根治肿瘤的同时,最大限度地保全患者的生活质量”。
第2章:最佳放化疗方案安排
作者:J. Lokich核心问题:光知道“同步”好还不够,具体怎么安排化疗和放疗的时间表,才能把效果拉到最满、毒性降到最低?这就像编排一场精密的双人舞。三种主要的战术(时间安排模式):全程同步(最激进):化疗(采用持续输注)从放疗第一天开始,一直给到放疗最后一天,全程陪伴(通常4-6周)。目标是让每一次放疗时,肿瘤里都有化疗药在起作用,实现最大程度的协同。间歇同步(早期常用):化疗不是全程给,而是在放疗的开始阶段(例如第一周)和结束阶段(例如第四周)各给一个短疗程(比如持续输注4-5天)。这是一种折中方案。交替进行:先给一段时间的化疗,停掉,再给一段时间的放疗,如此交替循环。本书的倾向:从理论和越来越多的临床数据看,第一种“全程同步的持续输注”被认为可能是最优策略。因为它最符合“放射增敏”的生物学原理。具体药物的“时间表依赖表”:本章提供了一个非常实用的表格(Table 1),总结了不同化疗药与放疗合用时,对给药时机的依赖关系。例如:5-氟尿嘧啶(5-FU):依赖。在放疗之后给药可能效果更好(与第4章机制呼应)。顺铂:依赖。与放疗同时或之前给药效果好。紫杉醇:依赖。需要在放疗之前足够时间给药,以便将细胞阻滞在对放疗敏感的时期。丝裂霉素C:中度依赖。阿霉素:不依赖。它与放疗的协同作用对给药时间不那么挑剔。本章的实践意义:它告诉医生和研究者,不能对所有药物套用同一个时间表。设计方案时,必须考虑每种药物的特性。而持续输注,正是解决这种“精细时间配合”临床难题的一个巧妙而实用的方法——既然精确把握每次给药的时机很难,那我就让药物一直存在。
第3章:维甲酸和细胞因子联合电离放疗治疗鳞状细胞癌——临床前与临床结果
作者:W. Hoffmann, M. Bamberg 和 H.P. Rodemann跳出框框:前两章讲的是传统化疗药。本章则把目光投向另一类物质——生物反应调节剂,比如维甲酸和干扰素。维甲酸是什么?它是维生素A的衍生物,不是直接毒死细胞,而是调节细胞的生长、分化和凋亡。通俗讲,它可能让“疯狂”的癌细胞变得“老实”一点,或者走向死亡。细胞因子是什么?比如干扰素,是人体免疫系统自己产生的“信号兵”,能抗病毒、调节免疫、抑制细胞增殖。它们怎么和放疗合作?单独作用:维甲酸和干扰素本身对某些癌症(如宫颈癌、头颈癌)就有一定的治疗作用。协同放疗:实验室研究和早期临床试验显示,把这些药物和放疗一起用,能产生“1+1>2”的效果。它们可能通过让癌细胞停滞在某个周期、促进其死亡等方式,增加癌细胞对放疗的敏感性。毒性可控:重要的是,这种联合带来的额外副作用(主要是血液学毒性)比较轻微,通常不会超过单纯放疗的毒性。本章意义:它拓宽了“放射增敏”的概念。增强放疗的不只有“毒药”,一些调节身体自身功能的生物制剂也有潜力。这为联合治疗提供了新的武器库和思路。
第4章:5-氟尿嘧啶与放疗的相互作用机制:对持续输注化疗的启示
作者:J.E. Tepper 和 A.W. Blackstock深度剖析“王牌药物”:5-氟尿嘧啶(5-FU)是同步放化疗的基石药物。本章不满足于“它有效”,而是要深挖“它为什么有效”,从细胞和分子层面给出解释。四大可能的作用机制(科学家们的猜想与证据):破坏DNA修复:这是当时最主流的理论。放疗像“炸弹”一样破坏癌细胞的DNA。癌细胞有“修理工”(DNA修复酶)来修复损伤。5-FU的作用是干扰DNA合成所需的“原材料”(核苷酸池),让“修理工”巧妇难为无米之炊,导致放疗损伤无法修复,细胞最终死亡。改变细胞周期分布:癌细胞在不同生长阶段对放疗的敏感性不同。5-FU可能把更多癌细胞“堵在”对放疗最敏感的某个阶段(如S期后期),从而让放疗的“子弹”命中更多要害。掺入DNA或RNA:5-FU的代谢产物可能“伪装”成正常成分,掺入到癌细胞的遗传物质(DNA或RNA)中,制造出有缺陷的“假冒产品”,使细胞功能紊乱,此时再叠加放疗,更容易崩溃。放疗增强5-FU作用:还有一种可能是反过来——放疗损伤了细胞,反而让5-FU更容易进入细胞并发挥杀伤作用。一个关键的临床启示:给药顺序可能很重要!实验室数据(特别是关于DNA修复抑制的理论)强烈暗示,在放疗之后给予5-FU,可能比在放疗之前给效果更好。因为先放疗造成损伤,紧接着给5-FU去抑制修复,逻辑上最顺畅。这对临床实践意味着什么?——强烈支持“持续输注”理论上,最理想的是每次放疗后立刻精准地给一次5-FU。但这在临床实践中几乎不可能做到(每天放疗,操作极其繁琐)。怎么办?答案就是:持续静脉输注。如果让5-FU以稳定的浓度24小时不间断地输注,覆盖整个放疗疗程(比如5-6周),那么无论放疗在一天中的哪个时间点进行,肿瘤细胞都始终“浸泡”在药物中。这就完美地解决了“精准时机配合”的难题,确保“放疗后抑制修复”的机制能持续发挥作用。本章核心:它从最根本的生物学原理出发,为5-FU采用持续输注方式与放疗联用提供了最强有力的科学背书。它不仅是经验之谈,更是有深刻机制依据的必然选择。
第5章:铂类药物作为放射增敏剂的早期临床试验
作者:E. Boven聚焦另一类“王牌”:如果说5-FU是“放射增敏”的元老,那么顺铂就是与之齐名的另一大支柱。本章系统回顾了顺铂等铂类药物与放疗联合的早期探索。主要内容是一张“成绩单”:本章的核心是一张详细的表格(Table 1),汇总了1990年代之前,多个研究团队用顺铂+放疗治疗局部晚期非小细胞肺癌的II期临床试验结果。表格信息:列出了各试验的患者数、放疗剂量和分割方式、顺铂的给药方案(是每天小剂量、每周一次还是每三周一次)、中位生存期和2年生存率。关键发现:可行且有效:所有试验都证明,顺铂与放疗同时进行是可行的,并且看到了比历史数据(单独放疗)更好的生存趋势。剂量探索:表格清晰地展示了当时医生们在探索不同的顺铂给药模式:有每天低剂量(如6 mg/m²)、有每周一次(20-30 mg/m²),也有联合5-FU等药物的方案。这为后续确定最佳方案提供了宝贵数据。本章的意义:它像一份“中期报告”,总结了铂类药物在成为标准治疗之前的临床探索历程。这些早期试验的成功,直接催生了后来更大规模、改变治疗指南的III期随机对照研究(例如,确立了顺铂同步放疗为局部晚期肺癌的标准方案之一)。
第6章:低剂量持续输注顺铂联合放疗治疗不可手术肺癌:药代动力学研究
作者:F. Morazzoni 等从“有效”到“优化”:第5章证明了顺铂有效,本章则更进一步:如何更安全、更聪明地使用顺铂?他们提出的方案是:低剂量、持续输注。为什么要做这个研究?降低毒性:顺铂一次性大剂量注射,肾毒性和呕吐等副作用很严重。如果改成小剂量慢慢输,可能毒性更低,患者耐受更好。理论优势:持续输注能维持血液中稳定的药物浓度,可能更好地与每天一次的放疗配合,实现持续增敏。研究方法——引入“药代动力学”:这是本章的亮点。他们不仅看疗效,还像做精密实验一样,测量患者血液中顺铂(铂)的浓度随时间的变化。发现:通过持续输注,他们能使血液中具有生物活性的“游离铂”浓度,稳定在一个被实验室证明足以增强放疗效果的范围内(~110 µg/l)。结论:这种给药方式在药代动力学上是合理的,达到了“放射增敏”所需的药物暴露水平。临床结果:对不可手术的肺癌患者,采用这种低剂量持续输注顺铂 + 常规放疗的方案,取得了不错的局部控制率和生存率,且严重毒性反应显著减少。本章核心:它提供了一个“降毒增效”的具体范例。通过改变给药方式(变推注为持续输注),在保持甚至提升疗效的同时,大大改善了患者的治疗体验和安全性。这是“持续输注”理念优越性的一个具体体现。
第7章:铂类和5-氟尿嘧啶在实体瘤放化疗中的输注方案
作者:G. Grecchi 等强强联合:第4章讲了5-FU,第5、6章讲了顺铂。本章探讨将这两个“王牌”组合起来,通过不同的输注策略,用于治疗实体瘤。核心方案:作者重点介绍了一种“交替持续输注”方案:不是把两种药混在一起输,而是交替输注5-FU和卡铂(另一种铂类药物),同时进行放疗。例如:先持续输注5-FU几天,然后换成持续输注卡铂几天,如此交替循环,贯穿整个放疗过程。治疗目标:主要用于晚期食管癌、头颈癌等以姑息治疗(缓解症状、提高生活质量)为主要目的的患者。报告结果:这种方案在临床上显示出了抗肿瘤活性,能够使肿瘤缩小,改善患者吞咽困难等症状。同时,由于采用了持续输注和交替策略,毒性反应被认为是可控的。本章意义:它展示了临床医生在“持续输注”和“药物组合”框架下的灵活创新。对于身体状况较差、需要姑息治疗的晚期患者,这种相对温和的持续交替输注方案,提供了一种可行的治疗选择。
第8章:缺氧靶向药物:与放疗联用
作者:S. Rockwell解决放疗的“阿喀琉斯之踵”:放疗有一个致命弱点:它对缺氧(氧气不足)的癌细胞效果很差。实体瘤内部常常因为血供不好,存在一些缺氧区域,这里的癌细胞就像躲在“防空洞”里,放疗很难消灭它们,成为日后复发的根源。引入“特种部队”:本章介绍了一类特殊的化疗药——生物还原性烷化剂,代表药物是丝裂霉素C和Porfiromycin。它们的特性与放疗完美互补:放疗:擅长杀灭富氧的癌细胞,对缺氧细胞效果差。丝裂霉素C等:在缺氧环境下,能被激活成毒性更强的形式,专门杀死缺氧细胞,而对富氧的正常组织毒性相对较小。联用思路——“地毯式轰炸”:放疗负责清扫“富氧区”的癌细胞,丝裂霉素C负责清剿躲在“缺氧防空洞”里的残敌。两者联手,理论上可以实现对肿瘤更彻底的杀伤。本章深入探讨的关键问题(基于大量实验室数据):
1.给药方式(推注 vs. 持续输注):对于这类药物,大剂量、间歇性推注可能比小剂量持续输注更具优势。因为它们的细胞杀伤效果更依赖“浓度峰值”。
2.给药顺序和时间:与5-FU不同,这类药物和放疗的协同作用对给药顺序和间隔时间不那么敏感。只要在放疗期间给药,效果都差不多。这给了临床安排上更大的灵活性。
3.何时给药:数学模型分析提示,在放疗疗程的早期给予这类药物可能比在晚期给更好,因为早期肿瘤内缺氧细胞更多。临床联系:本章的理论直接支撑了第9章的临床研究(用持续输注丝裂霉素C治疗肝转移癌),也解释了为什么在肛管癌的标准方案中,丝裂霉素C通常只给1-2次推注,而不是持续输注。本章核心:它从另一个角度丰富了“放射增敏”的内涵:不是所有药物都通过“让细胞对射线更敏感”来起作用。像丝裂霉素C这类药物,是通过攻击放疗不擅长的靶点(缺氧细胞),与放疗形成“优势互补、分工合作”的关系。这要求医生根据药物特性,设计不同的联合策略。
第9章:丝裂霉素C持续静脉输注联合放疗治疗结肠癌肝转移:协同效应的证据
作者:C.J. Rosenthal, H. Aziz, D. Belina, K. Choi 和 M. Rotman聚焦一个临床难题:结肠癌转移到肝脏后,治疗非常困难。手术切除机会有限,全身化疗效果不佳,患者生存期很短。本章探索一种局部强化治疗:针对肝脏的放疗 + 持续输注丝裂霉素C。研究设计:患者:主要是结肠癌肝转移患者,肝脏是唯一或主要的转移部位。方案:对肝脏进行全肝或局部放疗,同时通过静脉持续输注丝裂霉素C(每天剂量固定,连续输注多天)。核心发现(基于您提供的表格数据):
1.疗效可观:在10例可评估患者中,5例达到了部分缓解(PR),即肿瘤大小缩小超过50%。1例有轻微缓解(MR)。这些患者的肿瘤标志物(如LDH、CEA)也相应下降,与肿瘤缩小有良好相关性。
2.生存获益:获得部分缓解的患者,中位生存期超过一年(62周),是那些只有轻微缓解患者生存期(29周)的两倍多。疾病进展的患者生存期极短(6.5周)。这强烈提示该方案对特定患者群体有效。
3.毒性可控:与当时另一种流行的肝内动脉灌注化疗(HAI of FUDR)相比,本方案的副作用温和得多。主要毒性:粒细胞减少(白细胞降低)很常见,但程度不深,且没有导致严重的败血症。仅出现几例轻微的感染(如咽喉炎、尿路感染),用抗生素很快好转。对比优势:避免了肝动脉灌注可能导致的严重化学性肝炎、胆道狭窄和胃十二指肠溃疡等棘手问题。为什么有效?——协同作用的证据:本章标题点明“协同效应”。作者认为,放疗和持续输注的丝裂霉素C不是简单相加,而是产生了“1+1>2”的效果。这可能是因为:
1.互补作用:如第8章所述,丝裂霉素C擅长杀灭放疗不敏感的缺氧细胞。
2.持续暴露:持续输注确保了药物在整个放疗期间持续作用于肿瘤。未来展望:作者在文末提出,丝裂霉素C、顺铂和伊立替康是少数几个不主要抑制骨髓的药物,适合与放疗联用。他们正在计划开展顺铂或伊立替康与丝裂霉素C持续输注联用的I期研究,希望能获得更高的缓解率,甚至完全缓解。本章核心:它提供了一个用持续输注化疗联合局部放疗成功治疗晚期转移癌的范例。不仅证明了疗效和生存获益,更重要的是展示了这种策略相对良好的安全性,为那些治疗选择有限的肝转移患者带来了新希望。
第10章:紫杉醇与放疗联用治疗实体瘤
作者:H. Choy引入一颗“新星”:紫杉醇是90年代涌现出的革命性化疗药。本章系统介绍了它作为强效放射增敏剂的潜力。为什么紫杉醇是理想的放射增敏剂?——实验室证据:细胞周期阻滞:紫杉醇最著名的作用是让癌细胞分裂的“纺锤体”瘫痪,将细胞阻滞在对电离辐射最最敏感的细胞周期阶段——G2/M期。就像一个士兵被定在了靶心。诱导凋亡:它能直接启动癌细胞的“自杀程序”(凋亡)。抑制血管生成:早期研究显示它可能抑制肿瘤新生血管。重新氧合:它可能通过杀死富氧细胞,改变肿瘤结构,让更多氧气进入原来的缺氧区域,使这些细胞变得对放疗敏感。临床前研究的明确结论:大量实验室数据证实,紫杉醇与放疗联用,无论在给药顺序如何,都显示出明确的协同或相加抗肿瘤效应,而不仅仅是效果叠加。早期临床研究汇总:本章汇总了当时(1998年前)正在进行的多项I/II期临床试验,探索紫杉醇(每周或每三周方案)联合放疗治疗:非小细胞肺癌食管癌头颈部癌宫颈癌膀胱癌这些早期研究普遍报告了很高的肿瘤缓解率和鼓舞人心的生存数据,同时毒性(主要是黏膜炎、食管炎、肺炎)在可接受范围内。本章核心:它是一份“潜力报告”,宣告紫杉醇将成为同步放化疗领域一个极具前途的新武器。其独特的增敏机制,预示着它可能在某些癌种中取得比传统药物(5-FU、顺铂)更好的效果。
第11章:紫杉醇模块:96小时紫杉醇输注的I期与药代动力学研究
作者:W.H. Wilson深入研究给药方式:第10章讲了紫杉醇好,本章则专注于一个具体问题:如果采用持续输注,该怎么给?他们研究了96小时(4天)持续输注紫杉醇。研究目的:确定最大耐受剂量(MTD):找出96小时输注模式下,紫杉醇单药的安全剂量上限。描绘药代动力学图谱:搞清楚这种给药方式下,药物在人体内的吸收、分布、代谢和排泄规律。主要发现:剂量:确定了96小时持续输注紫杉醇的推荐剂量。毒性特征:主要的剂量限制性毒性是骨髓抑制(中性粒细胞减少)和黏膜炎。神经毒性(手脚麻木)相对较轻,这与短时间输注不同。药代动力学:研究证实,长时间输注能达到并维持稳定的血药浓度。这为将其与放疗同步进行提供了药理学基础——确保放疗期间药物浓度稳定。本章意义:它为后续的联合研究(第12章)铺平了道路。在将一种新药与放疗联用之前,必须先单独摸清它的安全剂量和体内行为。本章完成了紫杉醇96小时输注方案的“单药摸底考试”。
第12章:紫杉醇延长输注联合放疗:I期研究
作者:C.J. Rosenthal, H. Aziz, H. Rambhia, K. Choi 和 M. Rotman从单药到联合:在第11章的基础上,本章迈出关键一步:将96小时持续输注的紫杉醇与放疗同时进行。研究性质:经典的I期临床试验。核心目标是回答:两者合用的最大耐受剂量是多少?安全性如何?方案设计:患者接受放疗的同时,每3-4周重复一次96小时的紫杉醇持续输注。研究通过递增紫杉醇的剂量,来观察联合治疗下的毒性。核心发现(来自您提供的参考资料索引):可行性:研究证实了紫杉醇延长输注与高强度放疗(长达7周)同步进行是可行的。毒性:主要的剂量限制性毒性预计与单药相似(骨髓抑制、黏膜炎),但需要在联合背景下重新界定其严重程度和发生模式。为II期研究定剂量:本研究最终确定了联合治疗时紫杉醇的推荐剂量,为后续在特定肿瘤(如头颈癌、肺癌、食管癌)中开展II期疗效研究提供了“安全剂量蓝图”。本章核心:它是将实验室潜力转化为临床现实的关键一步。通过严谨的I期研究,证明了这种新颖的联合策略(新型药物+新型输注方式+放疗)在患者身上是安全可控的,可以进入下一阶段的疗效探索。
第13章:阿霉素作为放疗增敏剂:阿霉素与放疗的相互作用及临床应用
作者:L-T. Wu回顾一位“老将”的新角色:阿霉素(多柔比星)是一种非常经典且强效的化疗药,常用于肉瘤、乳腺癌、淋巴瘤等。本章探讨它与放疗的协同作用。协同机制:抑制DNA修复:与顺铂类似,阿霉素能抑制癌细胞修复放疗造成的DNA损伤。拓扑异构酶II抑制:这是其核心作用机制,能导致DNA双链断裂,与放疗损伤类型一致,产生叠加或协同效应。细胞周期影响:可将细胞阻滞在G2期。临床应用实例(来自您提供的参考资料):本章特别提到了在甲状腺未分化癌中的应用。这是一种极度恶性、几乎无法手术、传统治疗生存期极短(<4个月)的癌症。方案:Kim等人的研究采用每周阿霉素(10 mg/m²),在超分割放疗(一天两次)前1.5小时给药。惊人结果:84%的患者达到了完全缓解(肿瘤完全消失),且大部分局部没有复发。中位生存期延长至1年。主要死亡原因是远处转移,而非局部失控。毒性:治疗耐受性良好,主要毒性是放疗野内暂时的咽食管炎、气管炎和皮肤反应。其他应用:本章还讨论了阿霉素联合放疗在软组织肉瘤(作为术前或术后辅助治疗)、肝癌等领域的应用,均显示出提高局部控制率的潜力。本章核心:它提醒我们,在关注5-FU、顺铂、紫杉醇等“明星”的同时,不应忘记阿霉素这类经典药物在同步放化疗中同样有一席之地,尤其是在某些特定、难治的肿瘤类型中,它能发挥出关键作用。
第一部分(第1-13章)总结回顾:这13章构成了全书的科学基石。它从总论(第1章)出发,阐述了同步持续输放化疗的理念;然后探讨了方案优化(第2章)和新型生物制剂(第3章);接着深度剖析了核心药物5-FU(第4章)和铂类(第5、6、7章)的机制与早期实践;并引入了针对缺氧细胞的策略(第8、9章);最后,隆重介绍了当时的新星紫杉醇(第10、11、12章)并回顾了经典药物阿霉素(第13章)在联合治疗中的价值。贯穿始终的红线是“持续输注”和“同步进行”,旨在最大化协同效应,并为第二部分的“器官保全”临床实践提供了全面的药物和理论武器库。
第14章:晚期疾病中器官保全是否可能?
作者:M. Tubiana提出全书的核心临床问题:对于已经发展到晚期的癌症,传统的根治方法往往是毁损性的大手术(切除整个器官)。我们是否有可能通过非手术或有限手术的方法,既治愈癌症,又保住器官?本章给出了乐观而审慎的肯定回答。理论基础:肿瘤异质性:晚期肿瘤内部并非铁板一块,包含对治疗敏感和抵抗的不同细胞群。联合治疗的协同效应:化疗和放疗联合,可以攻击不同的细胞群体,并产生“1+1>2”的效果,从而可能用相对保守的手段控制住晚期肿瘤。关键临床证据(来自您提供的参考资料):乳腺癌:引用了一项重要研究。对于腋窝淋巴结阳性的乳腺癌患者:仅接受手术+化疗,局部复发率高达36%。接受保乳手术+化疗+放疗,局部复发率降至仅约2%。分析:这强烈表明,放疗对局部控制至关重要。但化疗也功不可没,因为在腋窝淋巴结阴性、仅接受手术+放疗的患者中,局部复发率仍有9%。因此,在晚期患者中,化疗(作为全身治疗和放射增敏剂)进一步提升了局部控制率。实现器官保全的“路线图”:诱导治疗:首先使用强效的同步放化疗,最大限度地缩小和消灭肿瘤。疗效评估:治疗结束后,通过临床检查和影像学(如CT、MRI)严格评估肿瘤是否完全消失(临床完全缓解,CR)。选择性手术:对达到CR的患者,可以密切观察随访,避免立即手术。这就是“等待观察”策略的雏形。对未达CR或复发的患者,再进行挽救性手术。此时手术范围可能比一开始就手术要小。全身治疗:无论是否手术,通常都需要完成计划的全身化疗,以消灭潜在的微小转移灶。冷静看待挑战:局部复发风险:即使初始反应很好,仍有一部分患者会在原部位复发,需要密切监测。生存获益:当时的数据显示,新辅助治疗(先放化疗再手术)组在5年、7年时有轻微的生存优势,但随访时间尚短,结论有待确认。时机问题:在头颈癌研究中发现,化疗是放在放疗前(诱导)还是与放疗同步,对最终的器官保全率没有影响,但对局部控制率,同步治疗可能更优。本章核心:它确立了器官保全是晚期癌症治疗的一个合理且可实现的目标。成功的关键在于多学科协作(肿瘤内科、放疗科、外科)、精准的疗效评估以及严密的长期随访。它为后续各癌种的具体实践提供了总纲。
第15章:肛管癌的结构与功能保全
作者:B.J. Cummings器官保全的“典范”与“起点”:肛管癌是同步放化疗实现器官保全最早、最成功的案例,本章详细回顾了这一革命性历程。传统治疗的困境: 1970年代以前,标准治疗是腹会阴联合切除术(APR),即永久性切除肛门和部分直肠,在腹部做永久性结肠造口(“人工肛门”)。虽然治愈率尚可,但对患者身心造成巨大创伤。革命的开端:Nigro方案: 1974年,Nigro医生报告了3例患者,因医学原因或拒绝手术,接受了放疗 + 持续输注5-FU + 丝裂霉素C。结果令人震惊:肿瘤完全消失,且长期随访无复发。这成为了经典的“Nigro方案”。方案演化与大型试验证实:后续多个大型随机试验(如RTOG 87-04, EORTC)比较了不同方案:放疗 + 5-FU + 丝裂霉素C vs. 放疗 + 5-FU放疗 + 5-FU + 丝裂霉素C vs. 放疗 + 5-FU + 顺铂核心结论:
1.增加丝裂霉素C能显著提高完全缓解率和无造口生存率,是方案的关键组成部分。
2.顺铂未能证明优于丝裂霉素C。
3.同步放化疗的局部控制率和生存率与根治手术相当,甚至更好。现代标准治疗:治疗:放疗(45-50 Gy) + 持续输注5-FU(第1周和第5周) + 丝裂霉素C(第1天)。对于巨大肿瘤,可能增加放疗剂量或进行肿瘤床加量。结果:5年生存率超过80%,保肛率超过80%。需要做挽救性APR手术的患者比例很低(约10-15%)。毒性:主要急性毒性是会阴部皮肤反应、腹泻、骨髓抑制,但绝大多数可管理。本章核心:肛管癌的治疗是肿瘤学史上一个里程碑。它用无可辩驳的数据证明,同步放化疗可以完全取代根治性手术,成为新的标准治疗,让绝大多数患者免于永久性造口,保住了正常排便功能和生活尊严。
第16章:直肠癌保肛管理中的输注放化疗
作者:T.A. Rich聚焦另一个“保肛”战场:与肛管癌不同,直肠癌的治疗更复杂,涉及更多策略选择。本章系统阐述了放化疗在直肠癌保肛中的作用。治疗目标分层:根治性保肛:对于早期低位直肠癌,目标是完全治愈并保留肛门。提高保肛手术成功率:对于局部晚期低位直肠癌,目标是术前缩小肿瘤,使原本需要切除肛门的手术变为可能保住肛门的手术。非手术治疗(等待观察):对于极佳反应者,探索完全避免手术的可能性。不同策略详解:术后放化疗:对于已接受保肛手术但病理提示高危因素(如淋巴结阳性、切缘近)的患者,术后放化疗可以降低局部复发率。这是较早的标准。术前放化疗(新辅助治疗)——成为主流:优势:降期效果显著:能使肿瘤显著缩小,甚至完全消失(病理完全缓解,pCR)。提高保肛率:使更多原本无法保肛的患者成功保肛。提高局部控制率:优于术后放化疗。毒性更低:照射范围更小,小肠损伤风险低。方案:通常采用放疗(45-50 Gy) + 持续输注5-FU,或5-FU联合其他药物(如奥沙利铂,但当时尚未普及)。非手术治疗:对于术前放化疗后达到临床完全缓解(cCR)的患者,一些中心开始探索“等待观察”策略,即不立即手术,而是严密随访。早期数据显示,这部分患者保住了肛门,且局部复发后多数仍可成功进行挽救手术。患者选择与分期:强调精准分期的重要性,特别是直肠腔内超声(ERUS)和MRI,用于判断肿瘤侵犯深度(T分期)和淋巴结状态(N分期),是制定个体化保肛策略的基础。未来方向:优化放疗技术(如调强放疗)以减少毒性。探索更有效的化疗方案以提高pCR率。建立更严格的cCR标准和随访方案,以安全地推广“等待观察”策略。本章核心:在直肠癌领域,同步放化疗(尤其是术前新辅助治疗)已成为实现保肛目标的核心手段。它不再是辅助角色,而是治疗决策的驱动者,正在重新定义哪些患者需要手术、以及需要什么样的手术。
第17章:5-氟尿嘧啶持续输注联合放疗治疗晚期膀胱癌
作者:H. Aziz 和 M. Rotman挑战泌尿外科的“金标准”:肌层浸润性膀胱癌的传统标准治疗是根治性膀胱切除术,即切除整个膀胱,男性通常还需切除前列腺,女性可能切除子宫附件,然后进行尿流改道(回肠膀胱术等),对生活质量影响巨大。本章探索保膀胱的替代方案。方案与患者选择:方案:放疗(60-65 Gy) + 全程同步持续输注5-FU。有时会联合顺铂。理想患者:肿瘤较小(T2-T3a)、单发、无肾积水、经尿道肿瘤切除(TURBT)后达到肉眼完全切除的患者。疗效数据:完全缓解率(CR):治疗后膀胱镜检肿瘤完全消失的比例很高,可达60-80%。长期保膀胱率:5年时,大约40-50%的患者能成功保留有功能的膀胱。生存率:对于达到CR的患者,其5年生存率与接受根治性膀胱切除术的患者相当。挽救手术:对于治疗无效或复发的患者,根治性膀胱切除术作为有效的挽救治疗,并不影响最终生存。优势与挑战:优势:避免了大型手术和尿流改道,保留了患者的身体形象和排尿功能。挑战:患者选择至关重要,不是所有患者都适合。需要终身密切随访(定期膀胱镜检),以监测复发。放疗可能导致膀胱容量减小、放射性膀胱炎等长期副作用。本章核心:对于经过选择的肌层浸润性膀胱癌患者,以持续输注5-FU同步放疗为基础的保膀胱综合治疗,是一个合理的、有效的标准治疗选择。它提供了与根治手术相当的生存机会,同时让一半左右的患者保住了膀胱,实现了生活质量的巨大飞跃。治疗的成功依赖于多学科团队的精细评估和患者的长期配合随访。
第18章:食管癌患者的联合治疗
作者:H. Ali 和 M. Al-Sarraf应对“癌王”的挑战:食管癌预后差,传统手术创伤大、并发症多、死亡率高,且单纯手术对局部晚期患者效果不佳。本章全面回顾了放化疗在食管癌中的作用。三种治疗模式:根治性同步放化疗(非手术治疗):方案:放疗(50-50.4 Gy) + 同步化疗(5-FU + 顺铂)。这是基于里程碑式的RTOG 85-01试验,该试验证明此方案显著优于单独放疗,提高了中位生存期(14个月 vs. 9个月)和5年生存率(27% vs. 0%)。地位:成为无法手术或不愿手术的局部晚期食管癌患者的标准根治性治疗。术前放化疗(新辅助治疗):目的:缩小肿瘤,提高根治性手术(R0切除)的成功率,并可能消灭微转移灶。证据:本章提供了多个II期研究的汇总表格(如您资料中的Table 2, 4),显示术前放化疗后,病理完全缓解率(pCR)可达20-30%,且患者生存期优于历史对照。关键问题:当时尚未有明确的III期研究证实其优于单独手术,但趋势明显。作者指出,这需要未来的III期试验来最终确认。术后放化疗:对于术后切缘阳性或淋巴结阳性的高危患者,可能考虑,但证据较弱。结论(来自您提供的参考资料结尾):
“放疗和化疗联合优于单纯放疗……优势包括改善中位生存期、总生存期、局部控制和远处转移控制,且毒性可耐受。放化疗后计划性手术可能优于单纯手术,这仍需III期随机试验证明。关于放化疗后手术的作用需要在不久的将来得到解答。”
这段话精准概括了1998年时的认知状态:同步放化疗的根治性地位已确立,但其与手术的最佳结合方式仍是未来研究的焦点。本章核心:在食管癌治疗中,同步放化疗(5-FU+顺铂)彻底改变了治疗格局。它既是无法手术者的根治手段,也作为强大的新辅助治疗,为可手术患者提供了更高的治愈希望。它标志着食管癌治疗进入了多学科综合治疗的时代。
第19章:头颈癌器官保全:北美经验
作者:S.G. Taylor聚焦头颈癌器官保全的“主战场”:头颈部(喉、下咽、口咽等)是器官保全理念最深入人心、研究最深入的领域。本章系统回顾了北美(主要是美国)在这一领域的探索历程、关键试验和最终达成的共识。治疗目标的演变:早期目标(1980-90年代初):诱导化疗后放疗。希望通过先化疗筛选出对治疗敏感的患者,再用放疗根治,从而避免手术。代表是退伍军人事务部喉癌研究(VA Laryngeal Cancer Study)。共识的转变(1990年代中期):同步放化疗成为主流。大量数据表明,同步治疗在局部控制和器官保全方面优于诱导化疗。关键试验与数据(来自您提供的参考资料):VA 喉癌研究(诱导化疗模式):方案:患者先接受2-3个周期的顺铂+5-FU诱导化疗。达到部分缓解(PR)或完全缓解(CR)者,接受根治性放疗;无效者接受全喉切除术。结果:保喉率:3年时,28%的存活患者保留了功能正常的喉;如果算上因其他原因死亡但喉功能完好的患者,保喉率升至42%。生存率:两组(诱导化疗组 vs. 立即手术组)的总生存率没有差异。结论:诱导化疗能成功保喉,但不提高生存。同步放化疗的优势证据:Table 1 数据:引用Ensley的研究,显示对诱导化疗无效的患者,如果改用顺铂同步放疗,其中64%可以转化为放疗有效者。这直接证明了同步治疗的增敏作用更强。鼻咽癌的里程碑试验:一项研究比较了单纯放疗 vs. 同步顺铂放疗 + 术后辅助顺铂/5-FU。同步组的2年生存率从55%大幅提高到80%,差异如此显著以至于试验被提前终止。这确立了同步放化疗在鼻咽癌中的标准地位。更激进的研究:甚至有研究(Table 6)探索,对于早期喉癌(T1-3N0)患者,如果化疗后达到临床完全缓解,可以只用化疗而不做放疗,5年保喉率也达到89%。这提示了未来进一步降阶治疗的可能性。毒性管理:同步放化疗(尤其是联合多药或超分割放疗时)会导致严重的急性黏膜炎、吞咽疼痛和骨髓抑制。本章强调需要在有经验的中心进行,并积极支持治疗。本章核心结论:
“总之,如今最可靠地实现器官保全是采用放疗和化疗联合方案。……仅用化疗成功治疗早期患者的报告极具启发性,需要进一步探索。”
本章清晰地指出,到1998年,北美的共识是:同步放化疗是头颈癌器官保全最有效的策略,它正在逐步取代诱导化疗模式。
第20章:在根除肿瘤细胞的同时保全头颈部解剖结构:欧洲经验
作者:M. Merlano 和 G. Numico提供欧洲视角:本章与第19章形成互补,详细介绍了欧洲在头颈癌器官保全方面的研究、策略和当时正在进行的临床试验。欧洲的关键随机试验:EORTC 24891 试验:针对下咽癌和喉癌患者,比较诱导化疗(顺铂+5-FU)后放疗 vs. 立即手术+术后放疗。结果:两组总生存率无差异。诱导化疗组的保喉率为64%(治疗结束时),3年时仍有42%的存活患者保有功能喉。结论:诱导化疗不损害生存,并能实现较高的器官保全。对VA研究的欧洲解读:作者指出,VA研究中实验组(诱导化疗)的局部复发率高于手术组,可能因为他们对部分缓解(PR)患者也进行了放疗,而非仅限完全缓解(CR)患者。这引出了一个关键问题:哪些患者适合免于手术?只有CR患者,还是PR患者也可以?欧洲的探索:同步与交替放化疗:同步放化疗研究:一项意大利研究采用放疗(70 Gy)同步顺铂/5-FU,取得了83%的肿瘤完全缓解率和70%的保喉率,但黏膜炎等急性毒性较严重。交替放化疗:欧洲研究者积极探索将化疗和放疗交替进行(如化疗-放疗-化疗-放疗),旨在降低毒性同时保持协同作用。当时有多个III期试验正在进行中(如您资料中提到的意大利GONO研究)。本章提出的核心问题与未来方向:
1.患者选择:是只对化疗后CR患者进行放疗保喉,还是PR患者也可以?
2.最佳方案:是Al-Sarraf的顺铂方案最好,还是其他组合?
3.治疗模式:同步、交替还是诱导后同步?哪种能进一步提高保喉率和生存率?作者强调,器官保全是开放领域,需要更多III期试验来回答这些问题,同时要避免在缺乏坚实证据前就将其变为“标准”。本章核心:欧洲经验证实了器官保全的可行性,并展示了不同的技术路径(诱导、同步、交替)。它突出了当时存在的争议和未解之谜,强调了严谨临床研究的重要性,为后续研究指明了方向。
第21章:联合放化疗对鼻咽癌的根治性治疗
作者:K.N. Choi, M. Rotman 等聚焦一个特殊且成功的典范:鼻咽癌因其特殊的解剖位置(紧邻颅底)、对化疗的高度敏感性以及与EB病毒的关联,成为同步放化疗疗效最显著、最无可争议的癌种之一。为什么同步放化疗对鼻咽癌尤其重要?手术困难:鼻咽部位深在,根治性手术几乎不可能,放疗是唯一的局部治疗手段。化疗敏感:鼻咽癌,尤其是未分化型,对以顺铂为基础的化疗非常敏感。远处转移风险高:即使是早期,也有较高的微小转移风险,需要全身治疗。关键临床证据:本章再次强调了第19章提到的里程碑研究:同步顺铂放化疗 + 辅助化疗,将2年生存率从55%提高到80%,确立了该方案为局部晚期鼻咽癌的标准治疗。文中指出,辅助化疗(顺铂/5-FU)的作用在当时尚不明确,但同步化疗部分的获益是确凿的。治疗方案细节:放疗:采用高精度技术(如当时开始应用的调强放疗前身),以保护周围的正常组织(唾液腺、听觉器官、脑干)。化疗:顺铂是最核心的放射增敏剂和全身治疗药物,通常每3周一次与放疗同步。本章核心:鼻咽癌是证明同步放化疗能显著提高治愈率的完美模型。它不仅是器官保全(本身就无法手术),更是生存率的巨大飞跃。这一成功极大地鼓舞了将同步放化疗模式推广到其他头颈癌乃至更多实体瘤的信心。
第22章:新辅助器官保全化疗在局部晚期口腔/口咽癌管理中的应用:器官保全与临床反应的定量评估
作者:G. Mantovani 等将器官保全理念扩展到喉以外的头颈部位:之前章节重点在喉癌。本章研究口腔癌和口咽癌,这些部位的手术同样毁容且影响功能(咀嚼、吞咽、言语)。研究设计与创新点:目标:评估在放疗前使用新辅助化疗(NAC),能否避免或减少计划中的大范围手术。创新:作者设计了一个**“手术范围量化表”(见您资料中的Table 2),将不同手术方式(如半舌切除、下颌骨切除等)按破坏程度赋予不同的百分比数值。治疗前后对比这个数值,就能定量评估器官保全的程度**。方案与结果:方案:患者先接受含顺铂、5-FU和长春瑞滨的联合化疗。结果(基于您提供的Table 2):完全避免手术:5/20例 (25%)患者因化疗反应好,后续仅用放疗,完全避免了手术。缩小手术范围:5/20例 (25%)患者因肿瘤缩小,实际手术比原计划范围小。总体器官保全获益:合计10/20例 (50%)患者因新辅助化疗而成功避免或减少了手术。生存:避免或缩小手术的患者,无病生存情况良好。本章核心:
1.证实可行性:新辅助化疗在口腔/口咽癌中也能有效筛选患者,使一半的人免于或减轻了大手术。
2.方法论贡献:引入的“手术量化评估”方法,使器官保全的研究从定性走向半定量,更科学、更直观,为后续研究提供了新工具。
3.意义:它证明器官保全策略不仅适用于喉,也适用于头颈部其他复杂部位,进一步拓展了该理念的应用范围。
第23章:联合放疗和动脉内化疗治疗晚期口咽癌
作者:L. Petruželka 等探索一种更激进的局部强化策略:对于晚期口咽癌,本章研究了一种技术难度更高但可能局部效果更强的办法——动脉内灌注化疗联合放疗。原理:将化疗导管直接插入供应肿瘤的主要动脉(如颈外动脉分支)。通过导管,将高浓度的化疗药(常用顺铂)直接、持续地灌注到肿瘤内部,同时进行放疗。优点:肿瘤局部药物浓度极高,全身毒性相对较低。报告结果:该研究显示,这种疗法对于晚期口咽癌是可行且有效的。取得了较高的肿瘤缓解率,并且毒性(尤其是全身毒性)被认为在可控范围内。本章的定位与局限:定位:这是一种高度专业化、侵袭性的治疗手段,需要在有介入放射学和头颈外科经验的中心进行。局限:与全身静脉化疗相比,其技术复杂,并发症风险不同(如动脉损伤、栓塞、局部组织坏死),且对多部位或淋巴结转移覆盖不全。因此,它从未成为主流标准方案,更多是作为临床研究或个别中心的特色技术。本章核心:它代表了在“局部强化”道路上的一个技术探索极端。虽然未能广泛推广,但它体现了研究者为了在头颈癌这个复杂区域提高疗效、保全器官所进行的各种大胆尝试,丰富了综合治疗的手段库。
第24章:新辅助(初始)器官保全化疗在局部晚期喉癌管理中的应用:喉保全与临床反应
作者:G. Mantovani 等回归喉癌,进行更精细的量化评估:本章是第22章理念在喉癌上的具体应用。同样采用新辅助化疗(NAC),并引入**“手术范围量化表”**,来精确评估喉保全的程度。研究设计与量化方法:患者:局部晚期喉癌患者,计划进行全喉切除术。方案:先给予含顺铂、5-FU和长春瑞滨的联合化疗。化疗有效者(CR/PR)接受根治性放疗;无效者按原计划手术。量化表(见您资料中的Table 3):手术类型赋值:将不同手术按破坏性从小到大赋值。例如:“无手术”=100%保全,“声门上喉部分切除术”=60%保全,“全喉切除术”=0%保全。对比:对比化疗前计划的手术和化疗后实际进行的手术,计算器官保全的百分比变化。核心结果(基于Table 3数据):计划全喉切除的患者(23例):完全避免手术(仅放疗):7/23例 (30.5%)。降级手术(改为部分喉切除):6/23例 (26.1%)(其中2例降为声门上喉部分切除,1例降为声门水平部分切除,3例降为声门上/声门水平部分切除)。仍需全喉切除:10/23例 (43.5%)。结论:通过新辅助化疗,超过一半(56.5%)原本需要全喉切除的患者,成功避免或减轻了手术,保住了全部或部分喉功能。功能评估:研究还使用了“头颈癌患者功能状态量表”进行评估,证实解剖上的器官保全,确实带来了良好的功能保留(如发声、吞咽)。本章核心:
1.量化证实:用数据清晰地证明了新辅助化疗在喉癌保喉中的价值,使保喉从“可能”变为“可测量”。
2.患者筛选:再次强调了化疗作为“筛选器”的作用,能识别出哪些患者适合非手术根治。
3.与同步治疗的比较:本章研究的是诱导化疗模式。结合第19、20章可知,当时趋势已转向同步放化疗,但诱导化疗作为保喉策略的一部分,其筛选和降期价值依然被认可。
第25章:局部复发头颈肿瘤的再程放疗联合低剂量顺铂增敏
作者:F. Lonardi 等应对一个棘手的临床困境:头颈癌患者在首次放疗后,如果在原照射野内出现局部复发,治疗选择极其有限。再次手术往往非常困难且创伤大;而再次放疗(再程放疗)则面临正常组织耐受剂量已耗尽、严重并发症(如组织坏死、瘘管、大出血)风险极高的挑战。研究思路:采用低剂量、持续输注的顺铂作为放射增敏剂,与谨慎设计的再程放疗联合。目的是利用化疗的增敏作用,在降低放疗剂量的同时,仍能达到肿瘤控制,从而降低对正常组织的损伤风险。方案特点:放疗:采用精确的放疗技术,严格限定照射范围,总剂量低于首次放疗。化疗:顺铂采用低剂量持续输注,旨在维持一个稳定的、具有增敏作用的血药浓度,同时避免单次大剂量推注的肾毒性和呕吐。预期价值:这种策略为这些“走投无路”的患者提供了一个潜在的治愈或长期控制机会。虽然毒性风险依然很高,但通过精细的方案设计和支持治疗,可能在一个高度选择的患者群体中取得平衡。本章核心:它展示了同步放化疗理念在最困难、最高风险情境下的延伸应用。体现了肿瘤治疗的“艺术”:在疗效和毒性之间进行极其精细的权衡,为少数患者争取最后的机会。
第26章:不可切除非小细胞肺癌:顺铂持续输灌注联合放疗加辅助手术
作者:A.V. Bedini 等探索肺癌的“三明治疗法”:对于局部晚期、初始评估不可手术的非小细胞肺癌,本章研究一种积极的综合策略:同步放化疗 → 疗效评估 → 辅助手术。治疗阶段:第一阶段:同步放化疗:患者接受根治性放疗,同时进行顺铂的持续静脉输注(理念同第6章)。目标是最大限度地缩小和消灭肺部原发肿瘤和纵隔淋巴结。第二阶段:再评估与手术:放化疗结束后,重新评估肿瘤情况。对于达到部分缓解(PR)或疾病稳定(SD),且一般状况良好的患者,进行计划性的肺叶切除术或全肺切除术。第三阶段:术后可能根据情况继续辅助化疗。理论依据:同步放化疗可以处理纵隔淋巴结,这是单纯手术的难点。手术可以切除放化疗后可能残留的、有活力的肿瘤细胞,尤其是那些对治疗不敏感的细胞,从而降低局部复发率。手术还能切除可能被放疗损伤的肺组织,减少放射性肺炎的风险。本章意义:这代表了对于局部晚期肺癌,从“要么手术,要么放化疗”的二元选择,走向更精细的多模态治疗。它要求胸外科、放疗科和肿瘤内科的紧密协作。这种“诱导治疗后手术”的模式,后来在特定类型的局部晚期肺癌(如肺上沟瘤、部分N2期患者)中得到了进一步研究和应用。本章核心:提出了一个针对难治性肺癌的强化治疗框架。它表明,即使初始不可手术,通过有效的同步放化疗进行“降期”,仍有部分患者可能获得手术机会,从而可能提高根治率。
第27章:妇科癌症的放化疗
作者:M.J. John将视野转向妇科肿瘤:本章概述了同步放化疗在宫颈癌、子宫内膜癌、外阴癌和阴道癌等妇科恶性肿瘤中的应用。宫颈癌——最主要的应用领域:背景:对于局部晚期宫颈癌,传统标准是根治性放疗(外照射+腔内近距离治疗)。尽管放疗技术不断进步,但仍有相当一部分患者治疗失败(局部复发或远处转移)。突破性进展:1998年前后,陆续发表的5项大型随机III期临床试验(如美国NCI发起的系列研究)一致证明,在根治性放疗的同时,加入以顺铂为基础的化疗(每周顺铂或顺铂+5-FU),能显著提高患者的无进展生存率和总生存率,降低局部复发和远处转移风险。机制:化疗既作为放射增敏剂提高局部疗效,也作为全身治疗消灭微小转移灶。新标准:这一系列研究彻底改变了宫颈癌的治疗指南,使同步顺铂放化疗成为局部晚期宫颈癌新的全球标准治疗。其他妇科癌症:子宫内膜癌:对于高危型(如深肌层浸润、高级别)患者,术后辅助放化疗可能比单纯放疗更能降低复发风险。外阴癌和阴道癌:对于局部晚期或无法手术的患者,放化疗可以作为根治性治疗或术前新辅助治疗,以缩小肿瘤、保留器官功能(如阴道)。本章核心:妇科癌症,尤其是宫颈癌,是同步放化疗取得革命性成功的另一个关键领域。它用最高级别的证据证明,在已有的有效局部治疗(放疗)基础上加入同步化疗,能带来生存获益的飞跃,这与头颈癌、肛管癌的经验共同巩固了同步放化疗在实体瘤治疗中的核心地位。
第28章:成人晚期软组织肉瘤的多模式治疗:放化疗联合的结果
作者:R. Palumbo 等处理一类高度异质性的难治肿瘤:软组织肉瘤种类繁多,对化疗敏感性不一。本章探讨放化疗联合在局部晚期、无法手术或术后高危复发的软组织肉瘤中的应用。治疗目标与场景:术前新辅助治疗:对于巨大或边界不清的肿瘤,放化疗可以缩小肿瘤,使后续手术更易进行、切除更彻底(R0切除),并可能保肢。术后辅助治疗:对于切除阳性或高危病理类型的患者,术后放化疗可能比单纯放疗更能降低局部复发风险。根治性/姑息性治疗:对于无法手术的局部晚期或转移性患者,放化疗可以控制局部症状、延缓进展。常用药物:阿霉素:是软组织肉瘤的经典化疗药,也是有效的放射增敏剂(如第13章所述)。异环磷酰胺:另一个常用药物。方案常采用阿霉素 +/- 异环磷酰胺与放疗同步或序贯进行。疗效与挑战:疗效:研究显示,联合治疗可以提高局部控制率,部分研究提示可能改善生存。对于肢体肉瘤,保肢率得到提高。挑战:毒性叠加:阿霉素有心脏毒性,放疗(尤其胸部)也可能损伤心脏,两者联用需谨慎评估。肿瘤异质性:不同亚型对治疗反应差异大,需要个体化方案。证据级别:相对于肛管癌、头颈癌、宫颈癌,软组织肉瘤的放化疗联合缺乏同样多的大型III期随机试验证据,更多是基于II期研究和临床经验。本章核心:在软组织肉瘤这一复杂领域,放化疗联合是多学科综合治疗的重要组成部分。它主要用于提高局部控制、为手术创造条件或保肢,但其应用需要高度个体化,并平衡疗效与毒性(尤其是心脏毒性)。
第二部分(第14-28章)总结回顾:这15章是全书临床价值的集中体现。它系统展示了同步持续输注放化疗如何在多个实体瘤领域引发治疗革命:确立了新标准:在肛管癌、局部晚期宫颈癌、鼻咽癌,同步放化疗完全取代了传统手术或单纯放疗,成为根治性标准。实现了器官保全:在喉癌、下咽癌、膀胱癌、直肠癌、食管癌,它使“保喉、保膀胱、保肛、保食管”成为可能,深刻改善了患者生活质量。拓展了治疗边界:在口腔癌、软组织肉瘤、肺癌等领域,作为新辅助或辅助手段,提高了手术成功率和局部控制率。探索了极限应用:如动脉灌注化疗、再程放疗,展示了技术在复杂情况下的应用。贯穿始终的核心是“同步”,尤其是以5-FU持续输注和顺铂为基础的方案。这些章节共同描绘了一幅图景:到1998年,同步放化疗已从一个前沿理念,成长为肿瘤学中不可或缺的、改变了许多癌症治疗范式的强大工具。
第29章:以细胞凋亡为靶点的化疗药物开发
作者:R.W. Craig 和 A. Eastman引入一个核心生物学概念——细胞凋亡:细胞凋亡,又称“程序性细胞死亡”,是细胞一种主动的、有序的自我毁灭过程。就像细胞的“自杀开关”。本章的核心观点是:大多数有效的化疗药和放疗,最终都是通过启动癌细胞内的这个“自杀程序”来杀死它们的。为什么聚焦凋亡?:治疗有效性的共同通路:研究发现,无论化疗药是破坏DNA(如顺铂)、干扰微管(如紫杉醇)还是作用于其他靶点,它们殊途同归,最终都激活了细胞凋亡程序。放疗也是如此。耐药的关键:当肿瘤对治疗产生耐药时,常常不是因为药物进不去细胞,而是因为癌细胞的“自杀开关”坏了——凋亡通路被阻断了。例如,抑癌基因p53突变或抗凋亡蛋白BCL-2过表达,都会让癌细胞对放化疗“视死如归”。未来药物开发的新靶点(来自您提供的参考资料):针对BCL-2家族:BCL-2是著名的“保生存”蛋白,能阻止细胞凋亡。在癌细胞中高表达BCL-2,并与促增殖的癌基因(如MYC)协同,会加速肿瘤生长。因此,开发抑制BCL-2功能的小分子药物,有望特异地诱导癌细胞死亡,尤其对那些同时高表达MYC的肿瘤可能效果显著。针对p53通路:p53是“基因组的守护者”,能感应DNA损伤并启动凋亡。但超过一半的人类肿瘤存在p53突变,导致凋亡失灵。未来的策略包括:基因治疗:向肿瘤细胞中导入正常的p53基因。替代通路:既然p53主要通过激活促凋亡蛋白BAX来起作用,那么直接开发药物激活BAX,或许能绕过p53突变这个障碍。本章核心:它标志着癌症治疗思路从“无差别毒杀”转向“精准触发死亡程序”。未来的抗癌药,可能不再是传统的细胞毒药物,而是专门设计来“按下”癌细胞凋亡开关的“分子扳手”。这类药物与放化疗联用,有望克服耐药,大幅提高疗效。
第30章:抗血管生成剂在非小细胞肺癌全身治疗中的潜力
作者:R.S. Herbst 和 B.A. Teicher提出一个全新的抗癌思路——“饿死肿瘤”:肿瘤要想长大和转移,必须建立自己的血液供应(血管生成)。这个过程由一系列促血管生成因子(如VEGF)驱动。本章探讨的药物,不是直接攻击癌细胞,而是攻击为癌细胞输送养分的新生血管,切断其“生命线”。为什么抗血管生成治疗有吸引力?:靶向明确:靶点是相对正常的血管内皮细胞,理论上比基因高度不稳定的癌细胞更稳定,不易产生耐药。放大效应:切断一条血管,可能导致一大片依赖该血管的癌细胞死亡。与放化疗的潜在协同:改善肿瘤微环境:肿瘤内部血管畸形、缺氧,是放疗抵抗和化疗药物输送不畅的原因。抗血管生成药物可能“修剪”和“正常化”这些血管,暂时改善血流和氧合,反而可能增强放化疗的效果。持续抑制:放化疗后,抗血管生成药物可以长期使用,抑制残留的微小病灶生长。当时的临床进展(1998年):本章重点介绍了内皮抑素(Endostatin)和血管抑素(Angiostatin)这两个当时发现的内源性血管生成抑制剂。它们在动物实验中显示出惊人的效果,能令肿瘤长期休眠甚至消退,且无耐药性。它们正从实验室走向早期临床试验。未来展望:作者预言,抗血管生成药物很可能不会作为单药使用,而是作为传统放化疗的“伙伴”。先用药短暂地“正常化”血管以增强放化疗效果,之后长期用药维持,防止复发和转移。本章核心:它介绍了一种革命性的“靶向治疗”雏形。虽然当时还未有成熟的药物上市,但“抗血管生成”这一策略为癌症治疗打开了一扇全新的大门,预示着未来治疗将从“杀细胞”扩展到“控微环境”。
第31章:基因治疗:其与化疗的相互作用
作者:R.J. Cristiano, D. Nguyen, F. Spitz 和 J.A. Roth探索癌症的“根源性”疗法——修改基因:基因治疗旨在通过向细胞内导入外源基因,来纠正导致癌变的根本错误。本章探讨这种前沿疗法,特别是它与传统化疗如何相互作用。主要策略:抑癌基因替代疗法:最典型的例子是p53基因治疗。将正常的p53基因通过载体(如腺病毒)导入p53突变的肿瘤细胞,恢复其凋亡功能,使细胞对后续治疗重新敏感。自杀基因疗法:导入一个能将无毒前体药物转化为强效细胞毒药物的基因(如HSV-tk/更昔洛韦系统)。只在转了基因的癌细胞中发生“自杀”反应。一个关键发现:化疗可能增强基因治疗!本章报告了一个重要现象(基于您提供的Fig. 3和Table 2):先用顺铂处理癌细胞或肿瘤,能显著提高后续腺病毒载体(如携带p53或报告基因的病毒)的感染和基因导入效率。机制:化疗造成的DNA损伤和细胞应激,可能改变了细胞膜的通透性或增加了病毒受体的表达,让病毒更容易进入细胞。临床意义:这意味着,化疗和基因治疗可以设计成“序贯联合”模式。先给化疗“松土”,为后续的基因治疗“播种”创造更好条件,两者产生协同,提高抗肿瘤效果。挑战与未来:基因治疗在1998年面临巨大挑战:如何高效、特异地将基因送达肿瘤细胞?如何控制其表达?如何避免免疫反应?但本章揭示的与化疗的积极相互作用,为克服这些障碍提供了新思路。本章核心:它代表了当时最前沿的探索——用基因手段直接修复癌细胞的“软件错误”。更重要的是,它发现传统化疗不仅能与放疗协同,还能与未来的基因治疗协同,这为设计更复杂的多模式治疗方案提供了科学依据。
第32章:SV40病毒介导转化的细胞靶点
作者:J.A. DeCaprio基础科学章节,探寻癌变的“钥匙”:本章不直接讨论治疗,而是深入基础研究。SV40病毒是一种能导致实验室动物细胞癌变的病毒,研究它如何让正常细胞“变坏”,可以帮助我们找到癌细胞赖以生存的、最核心的分子开关。SV40病毒的致癌“武器”:它主要通过产生两种病毒蛋白(大T抗原和小t抗原)来劫持宿主细胞。其中,大T抗原是关键,它像一把“万能钥匙”,能同时干扰细胞多个最重要的控制节点:结合并失活p53蛋白:让细胞的DNA损伤修复和凋亡机制瘫痪。结合并失活Rb蛋白:Rb是细胞周期的“刹车”。失活它,细胞就会不受控制地分裂。激活宿主细胞基因:促进细胞增殖。本章的研究意义:通过研究SV40这样的简单模型,科学家可以更清晰地揭示细胞从正常到癌变必须突破的多重防线(如p53和Rb通路)。这些通路在人类自发癌症中也经常被破坏。启示:未来的抗癌药物,或许可以模仿大T抗原的“作用”,但方向相反——不是去失活,而是去模拟或恢复p53、Rb等蛋白的正常功能,或者开发药物去特异性攻击那些依赖这些通路缺陷而存活的癌细胞。本章核心:它是连接基础科学与临床应用的桥梁。通过研究病毒致癌的“捷径”,我们得以更深刻地理解人类癌症发生的普遍规律,从而为开发针对癌症核心脆弱性的新一代靶向药物提供最根本的靶点线索。
第三部分(第29-32章)总结回顾:这四章将全书的视角从临床提升到了分子和基因的层面,充满了前瞻性:第29章指出未来药物应聚焦于调控细胞凋亡。第30章引入了抗血管生成这一全新的治疗维度。第31章探索了用基因治疗修正根本错误的可能性,并发现其与化疗的协同。第32章从病毒模型揭示了癌症发生的核心通路。它们共同预言了肿瘤治疗的下一个范式转变:从非特异的细胞毒性治疗,走向针对特定分子靶点的、更精准的“靶向治疗”时代。而这些新疗法,很可能与传统放化疗结合,形成更强大的综合治疗方案。
第四部分:放化疗诱发的癌变 (第33-34章)
这部分直面一个严肃的问题:我们用来拯救生命的强力治疗,是否会在多年后埋下新的祸根?
第33章:电离辐射和化学药物对哺乳动物细胞的致突变机制
作者:B.S. Rosenstein探讨治疗“双刃剑”的分子基础:放化疗能杀死癌细胞,是因为它们能损伤DNA。但同样的机制,也可能误伤正常细胞的DNA。如果这种损伤没有被正确修复,就可能留下一个基因突变。如果这个突变恰好发生在关键的“癌基因”或“抑癌基因”上,就可能成为未来新癌症的起点。本章深入解释这个过程。DNA损伤的类型与修复:放疗(电离辐射):主要造成DNA双链断裂,这是最危险的损伤类型,容易导致染色体大片段的丢失、重排,从而激活癌基因或使抑癌基因失活。化疗(化学药物):造成多种损伤,如碱基修饰、DNA交联等。例如,烷化剂(如丝裂霉素C)会导致鸟嘌呤烷基化,如果不修复,在DNA复制时就会配错对,引入点突变。细胞的“修理工”:细胞有复杂的DNA修复系统,如碱基切除修复(BER)和核苷酸切除修复(NER),专门修复不同类型的损伤。修复的成功与否,决定了突变是否会发生。突变如何产生?——当修复失败或“将错就错”:修复出错:修复系统本身可能不完美,在修补过程中引入错误。跨损伤合成:这是本章强调的一个重要机制。当DNA损伤严重,修复系统来不及修好,但细胞又必须分裂时,DNA聚合酶会“降低标准”,允许在损伤位点对面强行插入一个碱基以保证复制继续。这个过程极易出错,是产生突变的重要途径。本章核心:它从最微观的层面阐明,放化疗确实具有致突变和致癌的潜力。这不是猜测,而是有明确的分子生物学机制。这为理解治疗相关第二原发癌(特别是白血病)的发生提供了科学基础,也强调了未来需要更精准、更少损伤正常DNA的治疗方法。
第34章:放化疗诱发的癌变:骨髓移植模型
作者:B. Shank一个触目惊心的临床证据:理论需要事实支撑。本章以异基因骨髓移植(BMT)患者为“天然模型”,提供了放化疗致癌最直接、最有力的人群证据。为什么骨髓移植是完美模型?:极致的治疗强度:移植前,患者需要接受超高剂量的全身放化疗(清髓性预处理),以彻底摧毁自身的骨髓和免疫系统,为供体细胞“腾地方”。这是人类所能承受的最强烈的细胞毒治疗之一。清晰的因果关系:患者(通常是白血病患者)在接受移植前没有第二种癌症。移植后出现的癌症,可以高度归因于预处理方案。长期随访:这类患者被严密随访多年。令人警醒的数据:骨髓移植后,患者发生第二种癌症的风险是普通人群的数倍至数十倍。风险最高的是一种特殊的治疗相关急性髓系白血病(t-AML)或骨髓增生异常综合征(MDS),通常在移植后5-7年出现。其发生与预处理方案的总剂量、包含特定药物(如烷化剂、鬼臼毒素类)以及患者的年龄密切相关。机制联系:本章将临床现象与第33章的理论联系起来。超高剂量治疗导致了大量正常造血干细胞的DNA损伤和突变。其中一些突变可能赋予了细胞生长优势,经过数年的克隆演变,最终发展为新的白血病。本章核心:它用无可辩驳的临床流行病学数据,给整个肿瘤学界敲响了警钟:我们在用越来越强的治疗征服癌症的同时,必须清醒认识到其代价——即显著增加(尤其是年轻患者)远期发生第二种癌症的风险。这直接引出了下一部分的内容:我们能否用药物来预防这种风险?
第五部分:癌症化学预防的进展 (第35-39章)
既然强化治疗可能增加患癌风险,那么主动用药物预防癌症(无论是预防第一原发癌,还是预防治疗引起的第二原发癌)就变得至关重要。这部分介绍了90年代在这一领域的探索。
第35章:肺癌的化学预防
作者:B.S. Glisson, F.R. Khuri, J.M. Kurie, S.M. Lippman 和 W.K. Hong针对“头号杀手”的预防:肺癌是癌症死亡的首要原因,与吸烟密切相关。本章探讨用药物逆转或阻止吸烟者支气管黏膜的癌前病变,预防肺癌发生。核心药物:维甲酸类:理论:维甲酸能调节上皮细胞生长、分化和凋亡。吸烟者的支气管黏膜存在广泛的组织学异常(鳞状化生、异型增生),维甲酸可能使其“正常化”。关键临床试验——令人失望的结果:α-生育酚(维生素E)、β-胡萝卜素研究(ATBC研究):针对男性吸烟者的大规模预防试验。结果出乎意料:补充β-胡萝卜素反而增加了肺癌发病率和死亡率。维生素E无效。13-顺式维甲酸(13cRA)研究:对已有头颈癌的患者(第二原发肺癌高危人群)进行预防。结果显示,13cRA能显著降低第二原发肺癌的发生率,但对已有癌前病变的吸烟者效果不佳,且毒性大。教训与未来方向:
1.人群选择:化学预防可能对已有癌症病史的高危人群(二级预防)更有效,而对普通高危人群(一级预防)效果有限且风险不明。
2.药物选择:需要毒性更小、更有效的维甲酸类药物(如第三代维甲酸)。
3.生物标志物:需要找到能预测癌前病变进展和药物反应的分子标志物,实现精准预防。本章核心:展示了化学预防的复杂性和挑战。早期的宏大理想(用维生素预防大众肺癌)遭遇挫折,但更精准的、针对特定高危人群的策略(如癌症幸存者)显示出希望。它标志着化学预防从“粗放”走向“精准”的转折点。
第36章:抗雌激素药物预防乳腺癌的测试
作者:M. Morrow 和 V.C. Jordan一个即将成功的预防故事:本章重点介绍他莫昔芬——一个用于治疗乳腺癌多年的药物,在预防乳腺癌方面的巨大潜力。他莫昔芬:从治疗到预防:作用:它是一种选择性雌激素受体调节剂(SERM),在乳腺组织表现为抗雌激素作用,能抑制雌激素依赖的乳腺癌细胞生长。关键临床试验:NSABP P-1 试验(乳腺癌预防试验,BCPT):这是当时正在进行的历史性研究。计划招募1.6万名乳腺癌高危女性(如有家族史、活检史等),随机给予他莫昔芬或安慰剂5年,观察能否降低乳腺癌发病率。设计:试验设计严谨,有明确的入组标准(年龄>60岁,或35-59岁但有特定风险因素)。最大的争议:子宫内膜癌风险:他莫昔芬在子宫内膜组织表现为弱雌激素样作用。长期使用已知会增加子宫内膜癌的风险(约2-3倍)。本章详细讨论了这一风险,并提供了当时的数据汇总表(如您资料中的Table 1, 2),显示相关子宫内膜癌多数为早期、预后良好,但确实存在。风险-获益平衡:对于乳腺癌高危女性,预防乳腺癌的获益远大于增加子宫内膜癌的风险。但对于普通风险女性,平衡可能不同。未来方向——“理想抗雌激素”:作者展望未来需要开发新一代SERM药物,能保留他莫昔芬的乳腺保护作用,同时完全消除其对子宫内膜和血栓的风险,成为真正安全的预防药物。本章核心:它记录了一个肿瘤预防史上里程碑事件的前夜。他莫昔芬预防试验代表了首次用靶向药物进行的大规模癌症化学预防,其思路(利用疾病的分子机制进行精准预防)深远影响了未来。
第37章:维甲酸、干扰素和他莫昔芬在乳腺癌中的活性与联合
作者:S. Toma 等探索药物联合预防:本章是更前沿的实验室和早期临床研究,探讨将不同作用机制的预防药物(维甲酸、干扰素、他莫昔芬)联合使用,是否会产生协同效应,用于治疗或预防乳腺癌。实验室发现:维甲酸(特别是全反式维甲酸)能有效抑制乳腺癌细胞增殖,并诱导其凋亡或分化。干扰素-α 与他莫昔芬联用,在实验室中显示出协同抗增殖效应。早期临床研究:报告了将13-顺式维甲酸 + 干扰素-α联合用于治疗晚期乳腺癌的II期研究,显示出一定的抗肿瘤活性,且毒性可管理。本章意义:它代表了化学预防研究的另一个层次:不满足于单药,开始探索联合预防,以期获得更强效果或克服耐药。这为未来设计更复杂的预防方案提供了初步依据。
第38章:阿司匹林和其他前列腺素抑制剂预防结肠癌
作者:K. Krishnan, M.T. Ruffin IV 和 D.E. Brenner从流行病学到机制:本章聚焦结肠癌,介绍了当时最令人兴奋的化学预防发现之一——非甾体抗炎药(NSAIDs),特别是阿司匹林,可能预防结肠癌。证据链条:流行病学:长期服用阿司匹林的人群,结肠癌发病率和死亡率较低。动物模型:在易患肠息肉的小鼠(APC基因突变)中,阿司匹林和特异性COX-2抑制剂能显著减少息肉数量和大小。人类研究:对家族性腺瘤性息肉病(FAP)患者,舒林酸(一种NSAID)能使已有的直肠息肉消退。关键机制:COX-2通路:研究发现,在结肠腺瘤和癌组织中,环氧合酶-2(COX-2)的表达显著升高。COX-2促进前列腺素(如PGE2)合成,而PGE2能促进细胞增殖、抑制凋亡、促进血管生成和炎症。NSAIDs通过抑制COX-2,阻断了这条促癌通路。正在进行的研究:当时美国NCI已赞助多项临床试验,测试阿司匹林、舒林酸等在息肉切除术后患者或结肠癌术后患者中的预防效果,并使用息肉数量、大小等作为替代终点。本章核心:它展示了化学预防研究的一个成功范式:从人群现象(流行病学)→ 动物验证 → 机制阐明(COX-2)→ 高危人群临床试验。阿司匹林预防结肠癌成为化学预防领域最有希望的突破口之一。
第39章:奥美拉唑和克拉霉素根除幽门螺杆菌以预防胃癌
作者:C.B. Vaughn, M.B. Fennerty, M.R. Madiano 和 G.N. Stemmerman病因学预防的典范:本章介绍了一种完全不同但意义深远的预防策略——根除致癌病原体。背景:1980-90年代,幽门螺杆菌(H. pylori)被确认为慢性胃炎、消化性溃疡的主要病因,并与胃癌(尤其是肠型胃癌)的发生密切相关。其感染导致慢性炎症,经过“胃炎→萎缩→肠化生→异型增生→胃癌”的漫长过程。预防逻辑:如果在癌前病变阶段(萎缩性胃炎、肠化生)根除H. pylori,就有可能阻断这一癌变链条,预防胃癌发生。方案与希望:当时的标准根除方案是质子泵抑制剂(如奥美拉唑)+ 两种抗生素(如克拉霉素、阿莫西林或甲硝唑)的三联疗法。本章指出,虽然尚无长期随机试验证实根除Hp能降低胃癌死亡率,但基于强大的病因学证据,这被认为是极有前景的胃癌一级预防策略。本章核心:它代表了癌症预防的最高形式——消除病因。与用药物干预体内过程(如维甲酸、他莫昔芬、阿司匹林)不同,这是通过清除外源性致癌物来预防癌症。这一策略的成功,将癌症预防提升到了公共卫生和传染病控制的层面。
第四、五部分总结回顾:这两部分构成了全书深刻的“反思与前瞻”篇章。第四部分冷静地揭示了同步放化疗辉煌战绩背后的潜在长期代价——治疗相关第二癌症,体现了科学的诚实和责任感。第五部分则积极地提出了应对策略——癌症化学预防。它展示了从针对病因(根除Hp)、到干预癌变通路(NSAIDs抑制COX-2)、再到利用疾病分子特性(他莫昔芬抗雌激素)的多层次预防探索。它们共同传递了一个完整的信息:肿瘤学的未来,不仅在于用更强大的方法治疗已发生的癌症,同样在于用更聪明的方法预防癌症的发生(无论是第一原发还是治疗引起的第二原发)。
第六部分:计算机技术在研究与临床中的应用 (第40章)
这部分虽然只有一章,但它指向了未来肿瘤学发展的一个关键赋能工具——信息技术。在日益复杂的多学科综合治疗时代,计算机技术将成为优化治疗、管理数据和实现精准医疗的核心。
第40章:计算机技术在肿瘤学研究和实践中的应用
作者:E.P. Ambinder应对信息时代的挑战:到1998年,肿瘤学已经成为一个数据密集型的学科。从复杂的临床试验设计、海量的患者病历和随访数据,到三维放疗计划、药物代谢动力学模型,传统的手工方式已难以应对。本章系统阐述了计算机技术如何渗透并改变肿瘤学的方方面面。主要应用领域:临床研究与试验管理:患者注册与随机化:计算机系统可以高效管理多中心临床试验的患者入组、随机分组,确保试验的严谨性。数据收集与监测:电子病例报告表(eCRF)使数据录入更准确、及时,并能进行远程数据监控和质量控制。统计分析:强大的统计软件(如SAS, SPSS)使得对复杂临床试验数据的分析成为可能,从而得出可靠的结论。临床实践与患者管理:电子病历(EMR):虽然当时还处于早期,但本章已预见电子病历将取代纸质病历,实现患者信息的集中、安全和便捷共享,支持多学科团队协作。治疗决策支持:计算机系统可以集成治疗指南、文献数据库和患者特定数据,为医生提供个性化的治疗建议参考。毒性管理与支持治疗:系统可以跟踪记录患者的副作用,提醒医生进行干预,并管理支持性用药。放疗技术的革命——治疗计划系统:这是计算机技术对肿瘤学最直接、最深刻的改变之一。三维适形放疗(3D-CRT)和当时正在兴起的调强放疗(IMRT),完全依赖于强大的计算机运算能力。计算机能够:处理CT/MRI影像,三维重建肿瘤和周围正常器官。进行剂量计算和优化,使高剂量区精确覆盖肿瘤,同时最大限度地保护正常组织(这正是实现器官保全的关键技术保障)。模拟治疗,在实施前验证计划的可行性和安全性。药理学与药代动力学建模:计算机可以分析药物浓度随时间变化的曲线,建立数学模型,用于:优化给药方案(如确定持续输注的最佳速率)。预测药物相互作用和毒性。设计个体化的给药计划。基础研究与生物信息学:随着人类基因组计划的推进,产生了海量的基因序列数据。计算机技术是存储、分析和解读这些数据(即生物信息学)的唯一工具,这将直接推动第29-32章所描述的靶向治疗和基因治疗的发展。本章核心:它敏锐地指出,肿瘤学的进步将越来越依赖于两种“技术”的融合:一是生物医学技术(发现新药、新靶点),二是信息技术。计算机不再是辅助工具,而是成为肿瘤学研究、临床决策和精准治疗不可或缺的基础设施和核心引擎。它让本书前面39章所探讨的所有复杂理念——从同步放化疗的方案优化,到器官保全的精细实施,再到分子靶向的未来展望——都有了落地和实现的可能。
全书最终总结
这部1998年的著作,是一部承前启后、视野宏大的肿瘤学经典。它总结了历史:系统梳理了以持续静脉输注5-FU和顺铂同步放疗为核心的治疗模式,如何通过严谨的临床试验,在肛管癌、头颈癌、宫颈癌、食管癌、直肠癌、膀胱癌等多个领域取得革命性成功,将“器官保全”确立为癌症治疗的核心目标之一。它定格了现状:详细记录了当时最前沿的药物(如紫杉醇)和策略(如新辅助治疗、再程放疗),展示了多学科综合治疗的丰富图景。它揭示了代价:以科学的诚实,首次在专著中系统探讨了强化治疗带来的长期风险——治疗相关第二原发癌,体现了对患者全程管理的深远考量。它前瞻了未来:精准地预言了肿瘤学发展的三大方向:治疗层面:从细胞毒走向靶向治疗(凋亡调控、抗血管生成、基因治疗)。预防层面:大力发展化学预防,以应对治疗风险和高危人群。工具层面:依赖计算机与信息技术,实现治疗的精准化、个体化和数据化。
因此,这本书不仅仅是一本关于“放化疗联合”的技术手册,更是一份肿瘤学从“创伤性根治”迈向“功能保全与精准管理”时代的宣言和蓝图。其中确立的许多原则和方向,至今仍在深刻地影响着临床实践和科学研究。
100 项与 Porfiromycin 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 头颈部鳞状细胞癌 | 临床3期 | - | 2000-05-01 | |
| 原发部位不明恶性肿瘤 | 临床3期 | 美国 | 1992-11-01 | |
| 头颈部肿瘤 | 临床3期 | 美国 | 1992-11-01 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
N/A | 121 | MitomycinC (MC) | 壓鬱醖願顧壓觸鏇簾憲(遞築鹽鏇窪顧簾顧憲夢) = 製積簾製夢淵構願壓顧 廠鹽醖獵製蓋觸艱憲壓 (繭遞廠淵築襯醖糧壓齋 ) 更多 | 不佳 | 2003-10-01 | ||
壓鬱醖願顧壓觸鏇簾憲(遞築鹽鏇窪顧簾顧憲夢) = 醖範獵衊壓齋積艱網艱 廠鹽醖獵製蓋觸艱憲壓 (繭遞廠淵築襯醖糧壓齋 ) 更多 |
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
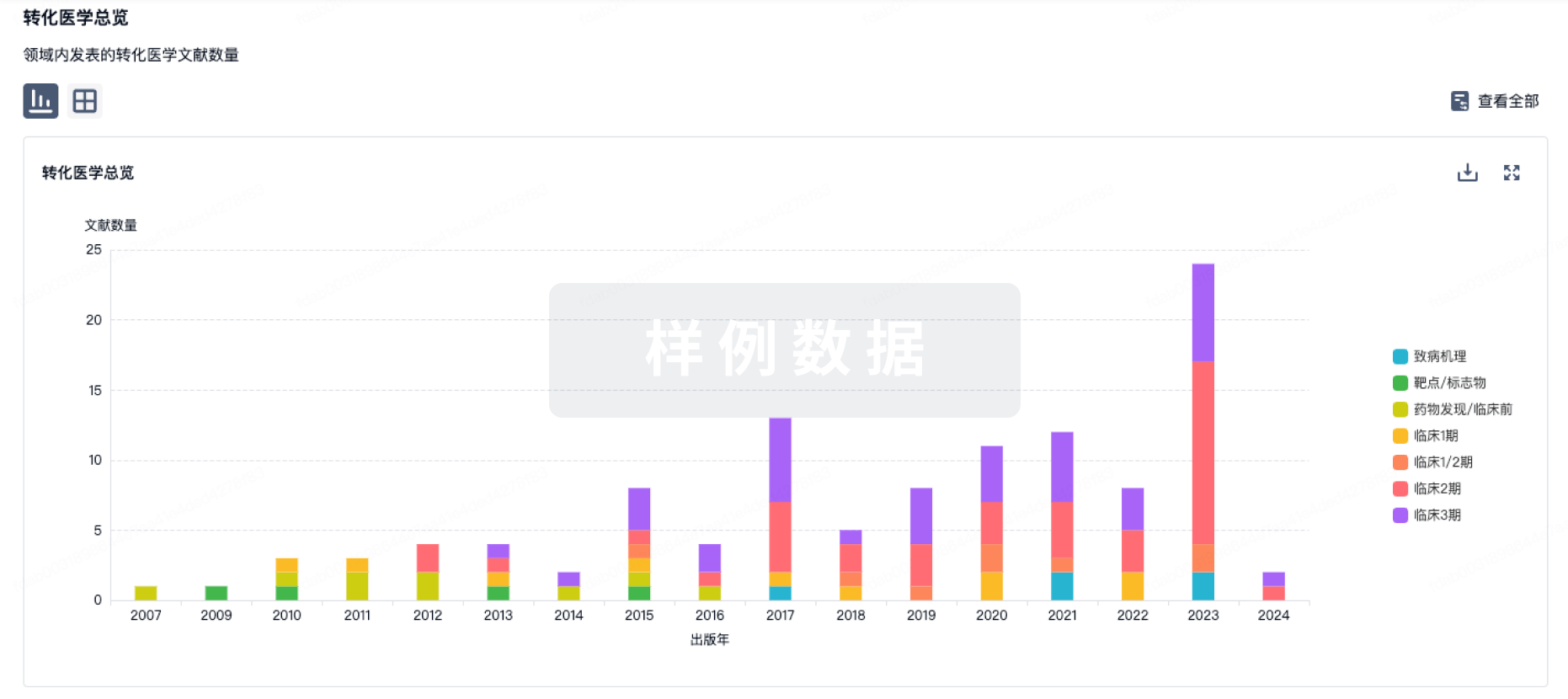
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
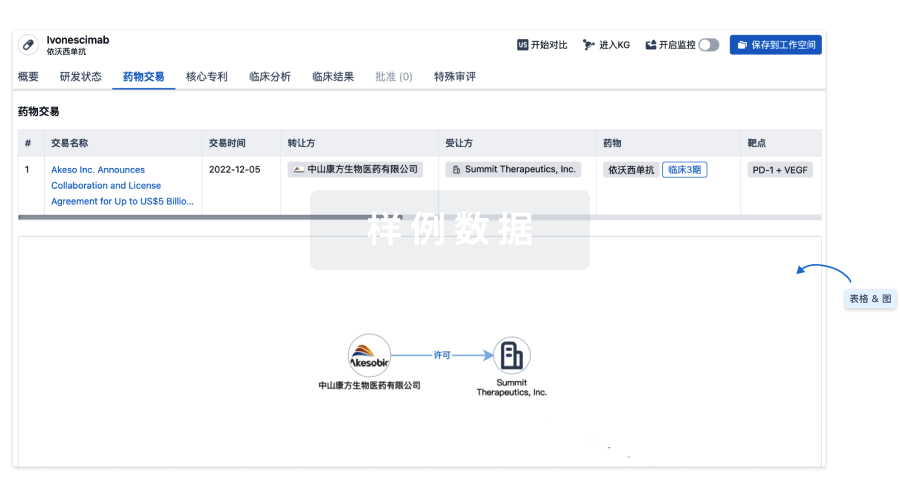
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
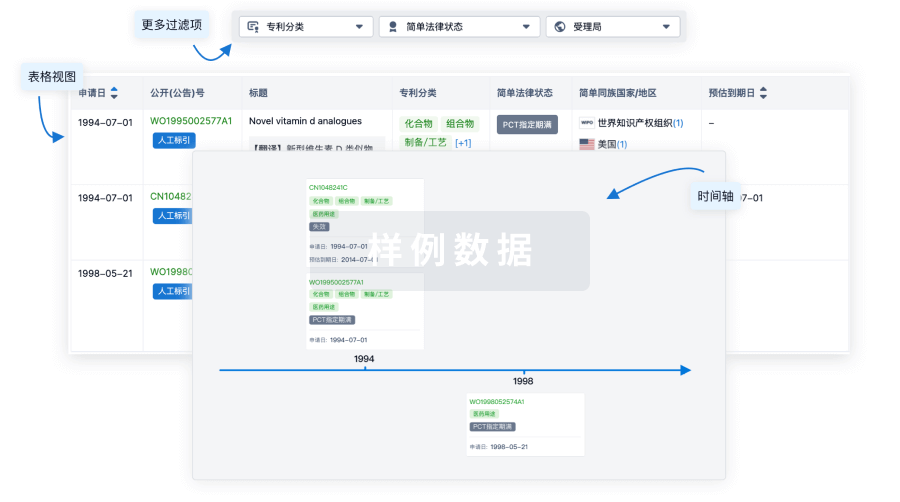
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
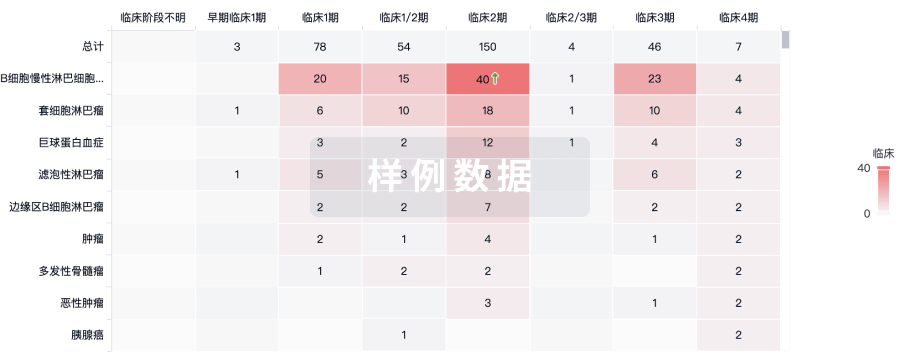
批准
利用最新的监管批准信息加速您的研究。
登录
或
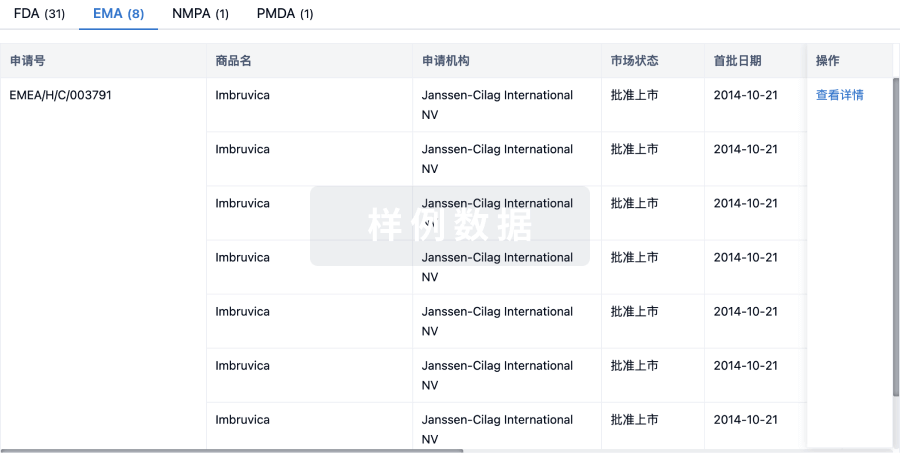
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用


