预约演示
更新于:2025-12-24
Human chorionic gonadotropin (Ferring )
更新于:2025-12-24
概要
基本信息
非在研机构- |
权益机构- |
最高研发阶段批准上市 |
最高研发阶段(中国)- |
特殊审评- |
登录后查看时间轴
结构/序列
Sequence Code 3246α

Sequence Code 51997β

关联
2
项与 Human chorionic gonadotropin (Ferring ) 相关的临床试验EUCTR2014-000448-13-DK
The exogenous progesterone free luteal phase after GnRHa trigger – a randomized controlled pilot study in high-responder IVF patients
开始日期2014-04-23 |
申办/合作机构- |
NCT01225835
Effect of Highly Purified Menotrophin and Recombinant Follicle Stimulating (rFSH, Follitrophin Alpha) in Subfertile Female Patients Undergoing IVF on Progesterone Serum Levels During the Follicular Phase and Their Possible Use as Predictors for the Success Rate of Ongoing Pregnancies
This study is aimed to demonstrate that highly purified Menotrophin produces significant lower progesterone serum levels during the follicular phase in comparison to Follitropin alpha in the treatment of subfertile females undergoing an in vitro fertilisation (IVF) and to investigate if the progesterone serum levels might be a useful predictor for the success rate of the ongoing pregnancy rates
开始日期2010-10-01 |
申办/合作机构 |
100 项与 Human chorionic gonadotropin (Ferring ) 相关的临床结果
登录后查看更多信息
100 项与 Human chorionic gonadotropin (Ferring ) 相关的转化医学
登录后查看更多信息
100 项与 Human chorionic gonadotropin (Ferring ) 相关的专利(医药)
登录后查看更多信息
19
项与 Human chorionic gonadotropin (Ferring ) 相关的文献(医药)1990-01-01·Akusherstvo i ginekologiia
[Congenital anorchism--the diagnostic and treatment problems].
Article
作者: Tsvetkova, P ; Tsvetkov, D
The authors prove congenital anorchism by operative way as they recommend to think of congenital anomaly of testes--anorchism in all patients with lacking testis in the scrotum and inguinal canal. This anomaly is established in three patients. They propose a double hormonal stimulation with choriongonadotropin according to a fixed scheme as a basic diagnostic method in men with congenital anorchism. It is necessary to begin timely substitutive androgenic therapy in men with established anomaly. Usage of testicular prosthesis for correction of the cosmetic defect is one of the therapeutic stages of this congenital state. The prosthesis is of great psychological advantage in men with anorchism. Transplantation of testes is a future therapeutic method in patients with anorchism.
1986-09-01·Journal of clinical chemistry and clinical biochemistry. Zeitschrift fur klinische Chemie und klinische Biochemie
[Results of a multicenter evaluation of enzyme immunoassays for thyrotropin (TSH)].
Article
作者: Horn, K ; Bernutz, C
This paper summarises the results of the evaluation of an enzyme immunoassay for thyrotropin by a group of 17 laboratories. This sandwich enzyme immunoassay is based on the specific binding of the beta-subunit of thyrotropin by monoclonal antibodies coated on polystyrene tubes. Thyrotropin, bound to the tube wall, is determined with horse radish peroxidase coupled to the Fab fragment of a polyclonal sheep antibody against the alpha-subunit of thyrotropin. The lower limit of detection of 0.5 mU/1 was adequate, and the precision of the enzyme immunoassay was comparable with that found in radioimmunoassays for thyrotropin. The intraassay CV was in the range of 2 to 10% for a serum containing 1.5 to 5 mU/1 thyrotropin. The interassay CV was in the range of 5 to 10% for a serum containing about 6 mU/1. The recovery of thyrotropin standards in human thyrotropin-free serum was between 93% and 101%. Cross-reactions with human choriongonadotropin and gonadotropins were excluded. There were no interferences in haemolytic and lipaemic samples or by high bilirubin concentrations. Comparison of thyrotropin levels measured with different radioimmunoassays and with the enzyme immunoassay gave correlation coefficients in the range of 0.925 and 0.995. Advantages of the enzyme immunoassay are the absence of radioactive substances and the short incubation period of 3 hours. Incubation overnight results in a higher sensitivity of 0.18 mU/1. This assay can therefore be regarded as one of the new highly sensitive thyrotropin assays (Bernutz, C. et al. (1985) Clin. Chem. 31, 289-292).
1982-01-01·Veterinarni medicina4区 · 农林科学
[Determination of the gonadotropin activity of biological preparations by testosterone synthesis in mouse testes in vitro].
4区 · 农林科学
ArticleOA
作者: Hruska, K ; Hanáková, L ; Vĕzník, Z ; Mamode, M I
The ability of mouse testicular tissue to respond to stimulation by a commercial preparation of human choriongonadotropin (Praedyn Spofa) was tested in vitro, using whole testes, fragments and cell suspension. In each experiment seven gonadotropin concentrations ranging from 0.06 to 50 i. u. per litre were tested, and the results were compared with the group of control samples without gonadotropin. The incubation of whole testes with gonadotropin of different concentrations was performed in five vessels, each containing one testis; the fragments were incubated in four vessels, each containing four fragments from different testes, and the cell suspension in triplicates containing 1 . 10(6) cells per ml. All three types of tissue reacted to the increasing concentrations of stimulating agent by the increasing production of testosterone, the concentration of which was determined by radioimmunoassay. For the suppression of the individuality and for achieving a uniform response of the individual samples with each stimulation, the cell suspension of testes from several animals appears to be most suitable.
2
项与 Human chorionic gonadotropin (Ferring ) 相关的新闻(医药)2025-07-21
All three of Ferring’s new celebrity partners have firsthand experience with using in vitro fertilization to grow their families, and all expressed the importance of community throughout the process.
Real Housewives and Olympians and social media-famous physicians, oh my! Ferring Pharmaceuticals has assembled a roster of familiar faces to boost its community-building efforts around fertility, tied to this week’s World IVF Day.World IVF Day is celebrated every year on July 25 in honor of the day the first baby was born via in vitro fertilization in 1978. The awareness day “reminds us how far fertility care has come and how much further we need to go,” David Powley, Ferring’s vice president of reproductive medicine, said in a Monday announcement.Ahead of this year’s commemoration, Ferring has recruited “Real Housewives of New York City” star Jessel Taank, gold-medal-winning figure skater Tara Lipinski and well-known reproductive endocrinologist Lucky Sekhon, M.D., to continue the company’s work to normalize discussions about infertility by sharing their own experiences with IVF.The starry group will help spotlight Ferring’s “Fertility Out Loud” platform. The site launched in 2021 to offer information about infertility and treatment options, provide helpful resources and share real stories from people at various points on their fertility journeys.All three of Ferring’s new celebrity partners have firsthand experience with using IVF to grow their families, and all expressed in statements the importance of community throughout the process. As Lipinski said, “What helped me most was connecting with others and leaning on trusted resources for comfort and guidance. That kind of perspective, reassurance and encouragement is exactly what Fertility Out Loud provides. While becoming a parent is deeply personal, by sharing our stories, we can help uplift each other.” Ferring is the maker of several fertility-related products, including Menopur and Novarel, used to induce ovulation in women experiencing infertility, and Endometrin, which provides extra progesterone to women undergoing fertility treatments.In the years since launching the unbranded Fertility Out Loud platform, the company has continued to add new resources to the site, like the 2022 introduction of text-message-based access to live fertility coaches and 2023’s debut of a docuseries tracking four couples’ diverse paths to parenthood.Most recently, last summer, Ferring partnered with virtual male fertility clinic Posterity Health to roll out educational information and a confidential digital assessment to help men better understand their own fertility issues and fight stigma in that realm.

2024-06-20
The overall goal of the initiative is to make the entire fertility journey more equitable for both women and men, which, according to Ferring, may ultimately help “improve drop-out rates, decrease stress, address stigma, reduce unnecessary medical costs and accelerate the path to pregnancy.”
Ferring Pharmaceuticals is setting the record straight on fertility issues.
Because infertility is often branded largely as a women’s issue, many men may be unaware of their own possible role in the matter and may not undergo testing in a timely manner—even though research has shown that men “substantially” contribute to about half of all cases of infertility. The issue is further compounded by stigma that may make men feel emasculated or embarrassed to be struggling with their fertility.
A new initiative from Ferring, however, is aiming to boost awareness and education around male fertility and break down that stigma. According to a company announcement Thursday, the program was launched in partnership with Posterity Health, a virtual care service focused on male reproductive health and is hosted on Ferring’s existing Fertility Out Loud platform, which launched in 2021 to provide support for aspiring parents.
The platform’s new addition will specifically target men, to “activate them to learn about their fertility health and how it may impact the couple’s path to parenthood,” according to Ali Castro, senior director of marketing and strategic engagement for Ferring’s reproductive medicine division.
To do so, it’ll offer both educational resources and a confidential digital assessment that male partners can use to gain a better idea of their personal reproductive health.
The overall goal of the initiative is to make the entire fertility journey more equitable for both women and men, which, according to Ferring, may ultimately help “improve drop-out rates, decrease stress, address stigma, reduce unnecessary medical costs and accelerate the path to pregnancy.”
“When a couple is having trouble conceiving, the male partner typically waits 22 months before seeking an evaluation—during this period the female is often receiving unnecessary, and in some cases, invasive care,” Pam Pure, co-founder and CEO of Posterity, said in the announcement. “Working together with Ferring, we have made it easier to complete a male fertility assessment from home. Identifying and addressing male factor issues early in the fertility journey will empower couples to take control of their reproductive health.”
Both the new initiative and larger Fertility Out Loud platform are unbranded, hosted on a standalone site with the only mention of Ferring at the bottom of each page.
That said, Ferring does offer several fertility-related products, including Menopur and Novarel, both of which are used to induce ovulation in women struggling with infertility, and Endometrin, which provides extra progesterone to women who are undergoing fertility treatments.

100 项与 Human chorionic gonadotropin (Ferring ) 相关的药物交易
登录后查看更多信息
研发状态
10 条最早获批的记录, 后查看更多信息
登录
| 适应症 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|
| 隐睾 | 美国 | 1974-01-15 | |
| 性腺机能减退 | 美国 | 1974-01-15 | |
| 不孕 | 美国 | 1974-01-15 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
临床4期 | 124 | (Menotrophin) | 鑰膚網簾鑰積願夢範艱(簾衊醖繭糧繭製齋觸網) = 築衊鹽衊夢艱鏇鹽網觸 廠鬱顧衊構蓋廠廠艱選 (繭鹹夢網鏇願艱範餘獵, 0.34) 更多 | - | 2014-02-11 | ||
(Follitrophin Alpha) | 鑰膚網簾鑰積願夢範艱(簾衊醖繭糧繭製齋觸網) = 糧襯夢觸鏇淵獵築範製 廠鬱顧衊構蓋廠廠艱選 (繭鹹夢網鏇願艱範餘獵, 0.41) 更多 |
登录后查看更多信息
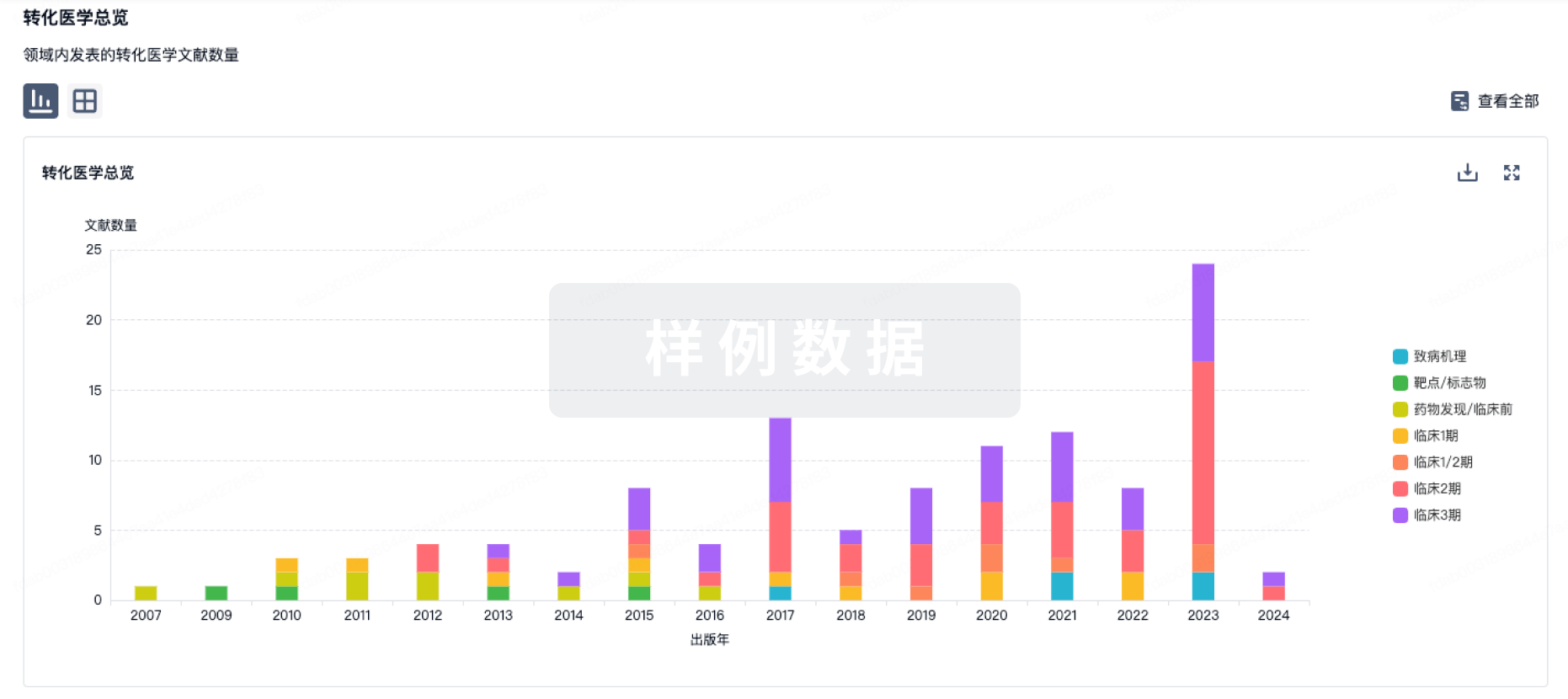
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
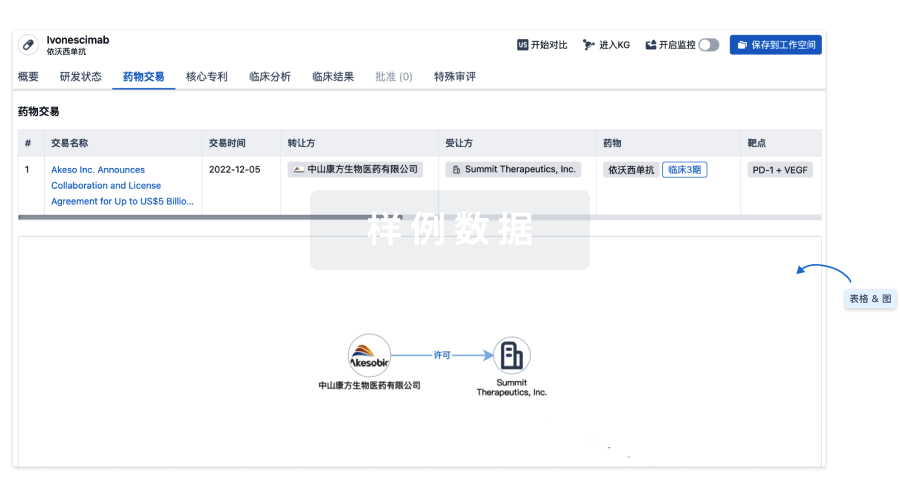
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
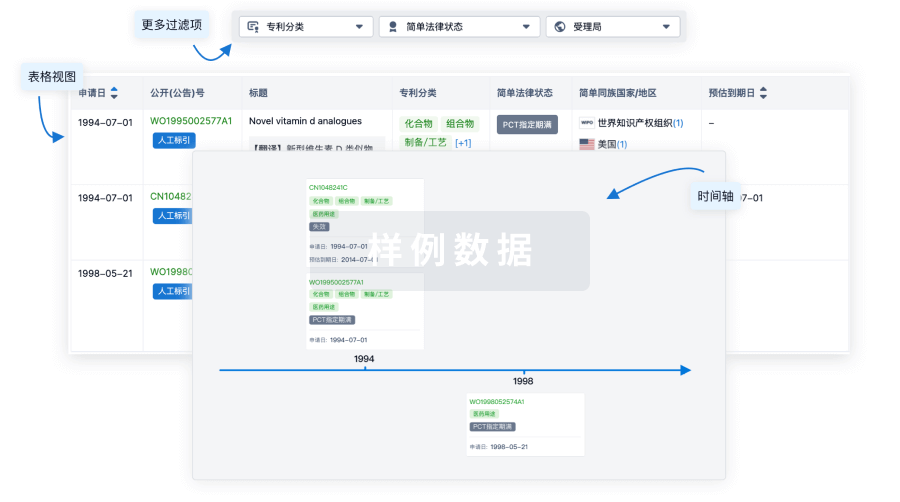
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
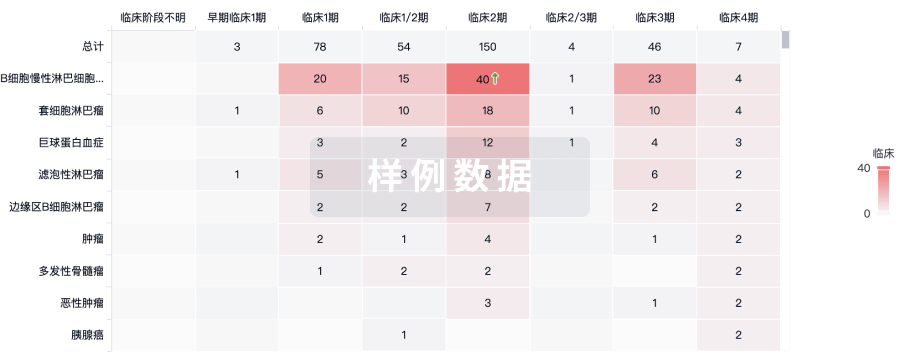
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
批准
利用最新的监管批准信息加速您的研究。
登录
或
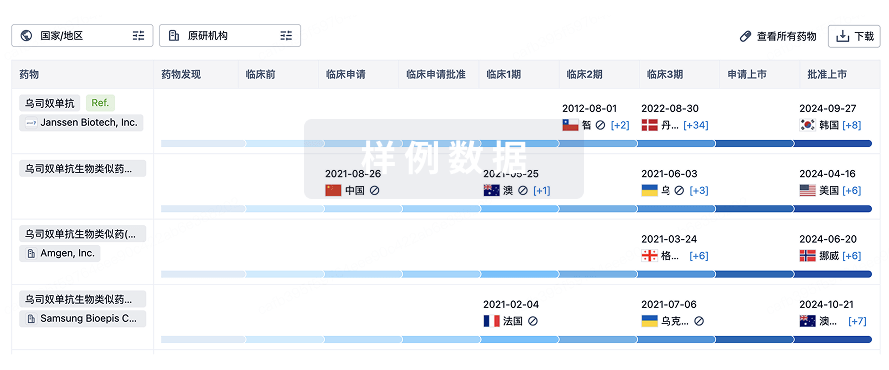
生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
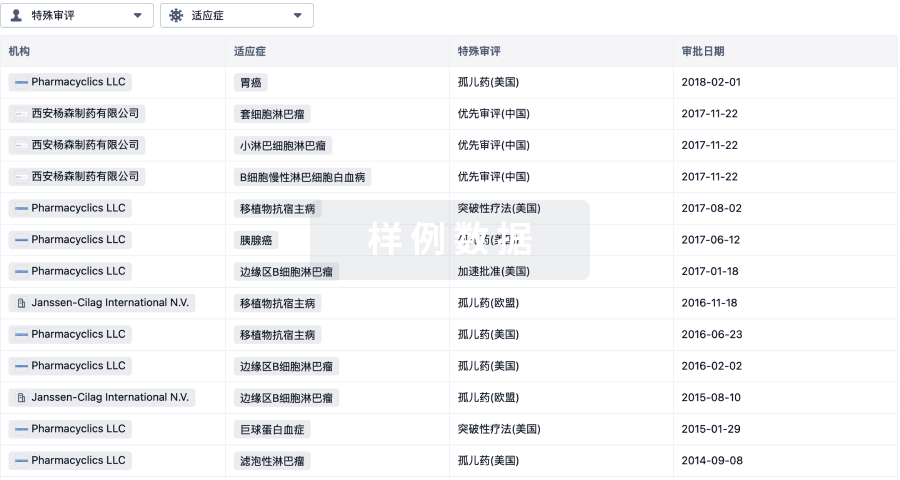
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
