预约演示
更新于:2026-03-04

SparX Therapeutics, Inc.
更新于:2026-03-04
概览
标签
肿瘤
消化系统疾病
泌尿生殖系统疾病
双特异性抗体
单克隆抗体
恒定NKT疗法
疾病领域得分
一眼洞穿机构专注的疾病领域
暂无数据
技术平台
公司药物应用最多的技术
暂无数据
靶点
公司最常开发的靶点
暂无数据
| 排名前五的药物类型 | 数量 |
|---|---|
| 双特异性抗体 | 5 |
| 单克隆抗体 | 3 |
| 恒定NKT疗法 | 1 |
| CAR-NKT | 1 |
| 抗体 | 1 |
关联
11
项与 SparX Therapeutics, Inc. 相关的药物靶点 |
作用机制 CLDN18.2抑制剂 |
原研机构 |
在研适应症 |
最高研发阶段临床1期 |
首次获批国家/地区- |
首次获批日期- |
靶点 |
作用机制 CLDN18.2抑制剂 |
在研适应症 |
非在研适应症- |
最高研发阶段临床1期 |
首次获批国家/地区- |
首次获批日期- |
作用机制 LILRB2抑制剂 [+1] |
在研机构 |
非在研适应症- |
最高研发阶段临床1期 |
首次获批国家/地区- |
首次获批日期- |
2
项与 SparX Therapeutics, Inc. 相关的临床试验NCT06259552
A Phase 1, Open-label Study to Evaluate Safety, Tolerability, and Pharmacokinetics of an Anti-LILRB2 / PD-L1 Bispecific Antibody SPX- 303 in Patients With Solid Tumors
Part 1 of this study is an open-label, dose-escalation, and safety expansion study of an anti-LILRB2 / anti-PD-L1 bispecific antibody SPX- 303 in patients with solid tumors. Part 2 of this study is an indication-specific dose expansion study of SPX-303.
开始日期2024-03-20 |
申办/合作机构 |
NCT05231733
A Phase 1, Open-label Study to Evaluate Safety, Tolerability, Pharmacokinetics and Efficacy of an Anti-Claudin 18.2 Antibody SPX-101 in Patients With Advanced or Refractory Solid Tumors
A Phase 1, Open-label Study to Evaluate Safety, Tolerability, Pharmacokinetics and Efficacy of an anti-Claudin 18.2 Antibody SPX-101 in Patients with Advanced or Refractory Solid Tumors
开始日期2022-05-01 |
申办/合作机构 |
100 项与 SparX Therapeutics, Inc. 相关的临床结果
登录后查看更多信息
0 项与 SparX Therapeutics, Inc. 相关的专利(医药)
登录后查看更多信息
1
项与 SparX Therapeutics, Inc. 相关的文献(医药)Nature Communications
A citrullinated histone H3 monoclonal antibody for immune modulation in sepsis
Article
作者: Song, Yujing ; Zeng, Xindi ; Ma, Jichun ; Ma, Jianjie ; Tetz, Zoe ; Yu, Xin ; Zhao, Ting ; Li, Yongqing ; Alam, Hasan B ; Tian, Yuzi ; Tan, Tao ; Quan, Chao ; Dong, Tao ; Qin, Jingdong ; Go, Sophia ; Jin, Hua ; Zhu, Gui-Dong ; Li, Qingtian ; Shao, Liujiazi ; Lee, Kyung Eun ; Kurabayashi, Katsuo ; Stringer, Kathleen A ; Chen, Yuchen ; Zhou, Xinyu ; Williams, Brandon ; Ouyang, Wenlu
Citrullinated histone H3 (CitH3), released from immune cells during early sepsis, drives a vicious cycle of inflammation through excessive NETosis and pyroptosis, causing immune dysfunction and tissue damage. To regulate this process, we develop a humanized CitH3 monoclonal antibody (hCitH3-mAb) with high affinity and specificity to target this process. In murine models, hCitH3-mAb reduces cytokine production, mortality and acute lung injury (ALI) caused by LPS and Pseudomonas aeruginosa while enhancing bacteria phagocytosis in the lungs, spleen, and liver. Using pre-equilibrium digital ELISA (PEdELISA), we identify an optimal therapeutic window for hCitH3-mAb in sepsis-induced ALI. In parallel, we explore the molecular mechanism underlying CitH3-driven inflammation. We find that in macrophages, CitH3 activates Toll-like receptor 2 (TLR2), triggering Ca2+-dependent PAD2 auto-citrullination and nuclear translocation, amplifying CitH3 production via a harmful feedback loop. The hCitH3-mAb treatment effectively disrupts this cycle and restores macrophage function under septic conditions. Together, these findings highlight both the therapeutic potential of hCitH3-mAb and provide a deep mechanistic insight into the CitH3-PAD2 axis in sepsis, supporting its further development for treating immune-mediated diseases.
9
项与 SparX Therapeutics, Inc. 相关的新闻(医药)2026-02-27
刚刚结束假期的调整与蓄力,我们便接连收到鹰谷合作伙伴们近期斩获的一系列“开门红”:从重磅商业化合作、大额融资落地,到多款创新药临床获批、全球首创技术实现出海授权——每一份喜报都印证了中国创新药研发的蓬勃活力。在研发数字化、AI化的浪潮中,鹰谷始终秉承“让研发有数据、有智慧、有未来,打造超级AI科学家”的理念,持续助力企业夯实研发数字基石,见证更多突破时刻。以下为近期鹰谷部分伙伴的成果速览:
先为达生物:携手辉瑞中国,加速偏向型GLP-1商业化进程(先为达生物使用鹰谷电子实验记录本InELN和科研项目管理系统InProject)
赜灵生物:完成近6亿元人民币C轮融资(赜灵生物使用鹰谷电子实验记录本InELN和化合物与样品注册管理系统InCMS)
达石药业:与Slate Medicines达成授权合作,携手推进PACAP抗体用于偏头痛防治(达石药业自2018年引入了鹰谷电子实验记录本InELN,至今已携手合作近9年)
羽冠生物:B群脑膜炎球菌OMV疫苗获批IND(羽冠生物使用鹰谷电子实验记录本InELN、化合物与样品注册管理系统InCMS和科研项目管理系统InProject)
云顶新耀:与麦科奥特达成MT1013独家商业化许可协议(云顶新耀使用鹰谷电子实验记录本InELN、库存管理系统InWMS、化合物与样品注册管理系统InCMS和科研项目管理系统InProject)
华森英诺:1类化药新药HSN002066C1片获批临床(华森英诺使用鹰谷电子实验记录本InELN)
注:排名不分先后
喜报1:先为达生物携手辉瑞中国,加速偏向型GLP-1商业化进程
2月24日,杭州先为达生物科技股份有限公司(以下简称“先为达生物”)与辉瑞中国宣布,双方就新一代偏向型GLP-1受体激动剂埃诺格鲁肽注射液(英文:Ecnoglutide injection,以下简称:埃诺格鲁肽)达成商业化战略合作协议。根据协议,辉瑞将获得该产品在中国大陆的独家商业化权益,迈出其全球代谢领域战略布局在中国的第一步;同时先为达生物为许可产品的药品上市许可持有人(MAH),负责许可产品的研发、注册、生产及供应。先为达生物将有权获得辉瑞支付的最高可达4.95亿美元的付款总额,包括首付款、注册及销售里程碑付款。
喜报2:赜灵生物完成近6亿元人民币C轮融资
1月12日,赜灵生物宣布完成近6亿元人民币C轮融资。本轮融资将用于加速推进赜灵生物两款处于3期注册性阶段的血液学/肿瘤学候选药物并拓展其他适应症的临床开发,同时启动多个免疫与炎症领域、中枢神经系统候选药物的国际临床试验。赜灵生物是一家临床后期阶段的生物技术公司,致力开发潜在“first-in-class”或”best-in-class”高度差异化小分子疗法,聚焦于血液系统疾病、肿瘤、中枢神经系统(CNS)及炎症╱免疫(I&I)等领域。
喜报3:达石药业与Slate Medicines达成授权合作,携手推进PACAP抗体用于偏头痛防治
达石药业(广东)有限公司(下称“达石药业”)近日宣布,已与美国新锐生物制药企业Slate Medicines, Inc.(下称“Slate Medicines”)达成独家授权合作,将公司自主研发的、潜在同类最佳的、靶向垂体腺苷酸环化酶激活多肽(PACAP)的单克隆抗体DS009(Slate Medicines命名为SLTE-1009)的全球(大中华区除外)临床开发及商业化权利独家许可给对方,用于偏头痛等头痛疾病的预防治疗。DS009成为我国首个“出海”的原研非阿片类生物镇痛药。
偏头痛全球患病率达14%,是严重危害人类健康的慢性神经血管性疾病。现有抗 CGRP 抗体药物对 30%~60% 的患者治疗无效,临床存在巨大未满足需求。作为达石药业在疼痛领域布局的核心研发管线之一,DS009是靶向PACAP的创新型单克隆抗体,其靶向的PACAP靶点独立于CGRP且经临床验证,可为对现有疗法应答不佳的全球数千万偏头痛患者提供新的治疗选择。该药物经蛋白工程改造延长半衰期,以支持皮下注射,提升患者用药便捷性与依从性。授权后,Slate Medicines将主导其大中华区以外的临床开发,预计于2026年中启动临床试验。
根据协议,达石药业将获得首付款、各阶段里程碑付款及全球销售额分级特许权使用费,同时保留DS009在大中华区的开发与商业化权利。此次合作成功标志着DS009迈入全球临床开发的快车道,也是公司在疼痛领域创新成果国际化的重要里程碑。
喜报4:羽冠生物B群脑膜炎球菌OMV疫苗获批IND
近日,上海羽冠生物技术有限公司(“羽冠生物”)宣布,公司自主研发的B群脑膜炎球菌OMV疫苗DX-104已于2月3日获得国家药品监督管理局药品审评中心(CDE)批准开展临床试验(IND)。
图片来源:CDE官网
这是国内首款获批进入临床开发的工程化OMV疫苗,本次获批也标志着羽冠生物自主搭建的工程化OMV技术平台完成从研发验证向临床转化的重要里程碑。此前,DX-104已在2026年1月获得伦理批件并完成澳大利亚临床试验备案(CTN),即将在澳大利亚启动一期临床研究,相关数据将用于支持其全球开发。
喜报5:云顶新耀与麦科奥特达成MT1013独家商业化许可协议
云顶新耀(HKEX 1952.HK)近日宣布与陕西麦科奥特医药科技股份有限公司(以下简称“麦科奥特”)签署独家商业化许可协议,获得MT1013在中国及亚太区(日本除外)的独家商业化授权。MT1013为全球首创的双靶点受体激动剂多肽,可同时靶向钙敏感受体(CaSR)及成骨生长肽(OGP)受体,开发主要用于治疗继发性甲状旁腺功能亢进症(SHPT)。此次战略合作将与云顶新耀现有肾科管线形成协同效应,强化产品布局,巩固麦科奥特在亚洲肾脏及自身免疫疾病领域的领导地位,并将产品覆盖从IgA肾病拓展至更广泛的慢性肾脏病领域。
根据协议,云顶新耀将向麦科奥特支付人民币2亿元首付款,以及最高不超过人民币10.40亿元的商业里程碑付款。中国III期临床研究正在进行中,相关临床开发费用将由麦科奥特承担。
喜报6:华森英诺1类化药新药HSN002066C1片获批临床
重庆华森英诺生物科技有限公司近日收到国家药品监督管理局核准签发的HSN002066C1片两个规格的《药物临床试验批准通知书》。HSN002066C1片为1.1类新药,适应症为晚期恶性实体瘤,它是华森英诺自主研发且完全享有自主知识产权的一种选择性聚二磷酸腺苷-核糖聚合酶7小分子抑制剂,具有较高的强效性和选择性,口服给药在小鼠中显示出较高的暴露量,并在不同肿瘤模型中展现出显著的肿瘤抑制活性。
参考来源:先为达生物、医药观澜、恺思俱乐部、张通社、云顶新耀、谈医说药
关于鹰谷
让研发有数据、有智慧、有未来
上海鹰谷信息科技有限公司(Integle)成立于2013年,建立鹰谷科研智能管理平台,Scientific Intelligence Management System, SIMS,致力于为企业建立自己的科研知识库和AI生产力工具。以电子实验记录本为中心,提供电子实验记录本InELN、科研库存管理系统InWMS、化合物与样品注册管理InCMS、科研项目管理系统InProject、科研采购管理InPMS等科研数据管理系统,由科学家打造,拥有结构式编辑器InDraw、生物序列编辑器InSequence、文献结构化工具InPaper、科研AI大模型InAI等科研工具类软件。
经过10多年的迭代开发,掌握IUPAC中英文命名、化学结构高精度AI图像识别、质粒设计、引物设计等专业技术,实现国产替代,解决很多行业“卡脖子”问题。鹰谷SIMS平台全面接入DeepSeek,结合鹰谷知识图谱,AI直接生成周报、论文、专利、CTD申报资料等底稿,打造实验设计、专利写作、QA检查、申报注册等多种数字员工,助力企业拥有专属的“超级AI科学家”,从而显著提升100倍的研发效率。
服务团队大多数为来自世界五百强、北京大学、复旦大学、上海交通大学、浙江大学等化学、生物领域的科学家和工程师,做到真正理解客户需求,为客户的业务场景提供更专业的解决方案,具备30分钟快速反馈的响应机制,让客户更安心。
目前,鹰谷已经服务了700多家行业标杆客户(其中100多家上市企业),全面覆盖生物医药、化工、新材料、新能源、食品日化等研发领域,如华为、扬子江、倍特药业、和记黄埔、艾力斯、人福医药、迈瑞医疗、晶泰科技、英矽智能、法国娇韵诗、中科院上海神经科学研究所等企业或高校研究所。2019年率先实现了InELN软件出海美国,如美国ADARx Pharmaceuticals、美国Staidson Biopharma、美国SparX Therapeutics,并陆续进入韩国、新加坡、法国、德国、日本等多个国家。
鹰谷明星产品——电子实验记录本InELN,资深科学家主导设计,致力于将每一个功能做深做透且高度灵活,整合InDraw和InSequence,建立实验知识库。支持云端部署或本地私有部署。全面接入DeepSeek,帮助企业50人做出100人的业绩。
鹰谷核心工具软件——InDraw结构式编辑器,支持中文(全球首家)或英文的IUPAC命名,高精度(99.75%)AI化学结构式图像识别,大分子编辑器HELM,全同位素绘制,兼容ChemDraw。有网页端、客户端两种版本,InDraw绘制的结构图,已在国际顶级期刊上发表数百篇SCI论文。
鹰谷新品工具软件——InSequence序列编辑器,对标SnapGene,由鹰谷纯自主研发,可用于DNA/RNA/蛋白序列编辑。兼容GenBank、Addgene文件中的序列信息,能实现质粒设计、引物设计、特征与酶切位点展现等功能,支持千万数量级碱基处理。
鹰谷新品工具软件——InPaper文献结构化系统,基于AI研发的专利/论文数据挖掘工具,能自动提取PDF专利或论文数据,获得结构式、反应式和活性数据,可用于AI训练,帮助企业建立自己的文献数据库,实现全文搜索、结构式和反应式搜索。
//推荐阅读
鹰谷电子实验记录本 | 全面接入DeepSeek,人走经验带不走
不上电子实验记录本,CRO都要接不到订单了!
减少实验次数,不用DOE,用贝叶斯优化
2026-01-23
新年伊始,我们很高兴与您分享鹰谷合作伙伴在近期取得的丰硕成果:从重大授权首付款到成功挂牌港交所上市,从多款新药临床获批到全球首创智造系统发布,每一份捷报都印证了中国创新药研发的蓬勃活力与智慧前行。在研发数字化、AI化的浪潮中,鹰谷始终秉承“让研发有数据、有智慧、有未来,打造超级AI科学家”的理念,通过电子实验记录本InELN、科研AI大模型InAI等一体化解决方案,持续助力企业夯实研发数字基石。以下为近期鹰谷部分伙伴的成果速览:
硕迪生物:授权罗氏GLP-1专利,1亿美元首付款!(硕迪生物使用鹰谷电子实验记录本InELN和科研项目管理系统InProject)
英矽智能:挂牌港交所(英矽智能使用鹰谷电子实验记录本InELN和科研项目管理系统InProject)
映恩生物:ADAM9靶向ADC癌症新药获批临床(映恩生物使用鹰谷电子实验记录本InELN、库存管理系统InWMS和科研项目管理系统InProject)
和黄医药:索乐匹尼布片拟纳入优先审评(和黄医药使用鹰谷电子实验记录本InELN、化合物与样品注册管理系统InCMS和科研项目管理系统InProject)
翼思生物:新药IGS01获批开展临床试验(翼思生物使用鹰谷电子实验记录本InELN、化合物与样品注册管理系统InCMS和科研项目管理系统InProject)
睿智医药:联合华东师范大学发布全球首个ADC和核苷酸单体药物智造系统(睿智医药使用鹰谷电子实验记录本InELN和科研项目管理系统InProject)
注:排名不分先后
喜报1:1亿美元首付款!硕迪生物授权罗氏GLP-1专利
2025年12月30日,硕迪生物宣布其全资子公司Gasherbrum Bio与罗氏、基因泰克(共称GNE)达成非独占专利许可协议,成功获得1亿美元首付款。该协议解决了双方在GLP-1受体激动剂领域的潜在专利重叠问题,特别是针对基因泰克通过27亿美元收购Carmot Therapeutics获得的CT-996项目。
根据协议条款,基因泰克需在协议生效后30日内支付1亿美元不可退还首付款。Gasherbrum Bio还将按个位数低段比例,就CT-996产品各市场的净销售额收取专利许可费,直至相关专利保护期终止。值得注意的是,此次许可为非独占性质,意味着Gasherbrum Bio保有完全自主权:既可继续推进现有在研管线开发,也可就相同专利资产与其他第三方开展合作。
此次1亿美元现金注资为Gasherbrum Bio带来无稀释性资本,将专项用于支持其在GLP-1领域的临床研究。通过在不稀释核心资产的前提下构建专利许可收益新渠道,公司成功打造了"自主研发+专利货币化"的双轨价值体系,有效分散新药研发的固有风险。
喜报2:英矽智能挂牌港交所,AI制药引领年内最大港股Biotech IPO
12月30日,由生成式人工智能驱动的临床阶段生物医药科技公司英矽智能在港交所成功挂牌上市,股份代码:3696.HK,成为首家通过联交所主板上市规则8.05条上市的人工智能生物医药科技公司。本次首次公开募股(IPO)募集资金总额22.77亿港元,是年内募集资金最高的港股生物医药IPO。
英矽智能此次港股上市获得了香港本土及国际投资者的高度关注和积极参与。本次IPO由摩根士丹利、中金公司及广发证券担任联席保荐人,全球发行9469.05万股,其中香港公开发售占比10%,录得约1427.37倍超额认购,锁定认购资金逾3283.49亿港元,创下年内非18A港股医疗健康IPO香港公开发售认购金额之最;国际发售占比90%,录得26.27倍超额认购,创下年内非18A港股医疗健康IPO国际配售认购倍数之最。
在基石投资者方面,英矽智能引入包括礼来公司、腾讯、淡马锡、施罗德、瑞银、橡树资本、易方达、泰康人寿等在内的15家全球化基石投资者,阵容涵盖全球制药龙头、互联网巨头、国际主权基金与大型资管机构以及国内头部公募与险资。其中,礼来公司与腾讯首次认购生物医药企业基石投资,显示跨界产业头部公司对AI制药赛道的认可与信心;美国长线投资机构橡树资本年内首次以基石投资者身份重回港股Biotech市场,彰显其对香港资本市场及创新医药长期价值的持续看好。
喜报3:映恩生物ADAM9靶向ADC癌症新药在中国获批临床
1月15日,中国国家药监局药品审评中心(CDE)官网最新公示显示,映恩生物申报的1类新药注射用DB-1317获批临床,拟开发治疗晚期/转移性恶性实体瘤。根据映恩生物公开资料,这是一款ADAM9靶向抗体偶联药物(ADC)。该产品的全球1a/1b期临床研究此前已在澳大利亚开展,并获得美国FDA的新药临床试验(IND)批准。
图片来源:CDE官网
DB-1317是映恩生物依托自主研发的ADC技术平台DITAC开发的新一代ADC产品,载荷为拓扑异构酶I抑制剂。其靶点ADAM9在胃癌、结直肠癌和胰腺癌等多种消化道肿瘤中高表达,而在正常组织中低表达。临床前数据显示,DB-1317在胃癌和结直肠癌等多种消化道肿瘤模型中表现出显著的抗肿瘤活性,显示出广阔的临床转化潜力。
2025年9月,映恩生物宣布DB-1317全球1a/1b期临床研究已在澳大利亚完成首例受试者给药,全球临床研究同步启动。这项研究(NCT07141706)将在澳大利亚、美国和中国同步开展,旨在评估DB-1317单药在晚期实体瘤患者中的安全性、耐受性和初步疗效。本次该产品在中国获批临床,意味着其即将在中国启动临床研究。
喜报4:和黄医药的索乐匹尼布片拟纳入优先审评
1月8日,CDE官网显示,和黄医药的索乐匹尼布片拟纳入优先审评,适应症为既往接受过一线标准治疗(糖皮质激素、免疫球蛋白)无效或复发的成人原发慢性免疫性血小板减少症(ITP)。
图片来源:CDE官网
索乐匹尼布是一种新型、选择性的脾酪氨酸激酶(SYK) 抑制剂。Syk作为B细胞受体和Fc受体信号传导通路中的一个关键蛋白,是多种亚型的B细胞淋巴瘤及自身免疫疾病的成熟治疗靶点。Ib/Ⅱ期研究证实,索乐匹尼布用于治疗原发ITP患者具有良好的安全性和疗效,并在一项双盲、Ⅲ期ESLIM-01研究 (NCT05029635) 中得到进一步验证。ESLIM-01研究旨在评估索乐匹尼布长期治疗成人慢性原发ITP患者的疗效和安全性。2025年ASH上,和黄医药报道了该研究的最终分析结果。
除了免疫性血小板减少症外,和黄医药也在探索索乐匹尼布用于治疗温抗体性自身免疫性溶血性贫血和惰性非霍奇金淋巴瘤等适应症的效果。1月7日,和黄医药宣布索乐匹尼布用于治疗温抗体型自身免疫性溶血性贫血成人患者的ESLIM-02研究的III期注册阶段取得阳性顶线结果,已达到第5至24周治疗期间持久血红蛋白 (Hb) 应答这一主要终点。
喜报5:翼思生物治疗帕金森病的新药IGS01获批开展临床试验
2025年12月25日,翼思生物宣布其拥有全球权益,自主研发的口服小分子创新药物IGS01的I期临床试验申请,已获国家药品监督管理局(NMPA)批准。IGS01是由翼思生物医药(苏州)有限公司自主研发的第一款1类全新小分子创新药。
IGS01是一款拟用于治疗帕金森病异动症(LID)的高选择性M4毒蕈碱型乙酰胆碱受体正向变构调节剂(PAM)。LID发生率高,对帕金森病患者生活质量的影响显著。作为全球首个针对该适应症开展注册临床研究的M4 PAM类药物,IGS01通过增强内源性乙酰胆碱与M4受体的结合效能,上调M4受体功能,纠正LID核心病理机制中的突触可塑性异常。
临床前研究显示,IGS01在LID模型中表现出治疗潜力,并具备理想的药代动力学特性。值得关注的是,IGS01通过多个肝酶途径代谢,有望显著降低其在接受多种药物治疗的患者中发生药物相互作用的风险,有利于晚期帕金森患者的联合用药。此外,临床前数据提示IGS01不增加精神障碍风险,与LID标准药物疗法金刚烷胺相比具有安全性方面的潜在优势。
喜报6:睿智医药联合华东师范大学发布全球首个ADC和核苷酸单体药物智造系统
日前,睿智医药联合华东师范大学在浦东张江正式发布了全球首个适用于ADC(抗体药物偶联物)与核苷酸单体合成药物智造系统。这一创新成果有望推动医药产业向连续化、微型化、智能化全面升级,重塑药物研发与生产的整体范式,标志着我国在生物医药核心工艺装备领域实现自主可控,为中国创新药产业高质量发展持续注入新动能。
据悉,该系统直击药物研发中的“中试放大”瓶颈,将传统生产模式升级为连续、智能、精准的“桌面式”制造。ADC微流智造系统实现了对药物抗体比、游离毒素、聚合体等关键质量属性的毫秒级监测与精准控制,将传统需数周完成的工艺开发与优化工作,缩短至数天。核苷酸单体微流智造系统攻克了传统磷酰化工艺对剧毒催化剂与无水无氧苛刻条件的依赖,采用无催化剂、无碱参与的“智能微流”反应路径,从源头杜绝三废处理难题,实现了单体的全天候连续合成,解决了传统工艺因批次生产导致的质量波动问题。
参考来源:医药观澜、药渡、浦东国际人才港、药时代、英矽智能
关于鹰谷
让研发有数据、有智慧、有未来
上海鹰谷信息科技有限公司(Integle)成立于2013年,建立鹰谷科研智能管理平台,Scientific Intelligence Management System, SIMS,致力于为企业建立自己的科研知识库和AI生产力工具。以电子实验记录本为中心,提供电子实验记录本InELN、科研库存管理系统InWMS、化合物与样品注册管理InCMS、科研项目管理系统InProject、科研采购管理InPMS等科研数据管理系统,由科学家打造,拥有结构式编辑器InDraw、生物序列编辑器InSequence、文献结构化工具InPaper、科研AI大模型InAI等科研工具类软件。
经过10多年的迭代开发,掌握IUPAC中英文命名、化学结构高精度AI图像识别、质粒设计、引物设计等专业技术,实现国产替代,解决很多行业“卡脖子”问题。鹰谷SIMS平台全面接入DeepSeek,结合鹰谷知识图谱,AI直接生成周报、论文、专利、CTD申报资料等底稿,打造实验设计、专利写作、QA检查、申报注册等多种数字员工,助力企业拥有专属的“超级AI科学家”,从而显著提升100倍的研发效率。
服务团队大多数为来自世界五百强、北京大学、复旦大学、上海交通大学、浙江大学等化学、生物领域的科学家和工程师,做到真正理解客户需求,为客户的业务场景提供更专业的解决方案,具备30分钟快速反馈的响应机制,让客户更安心。
目前,鹰谷已经服务了700多家行业标杆客户(其中100多家上市企业),全面覆盖生物医药、化工、新材料、新能源、食品日化等研发领域,如华为、扬子江、倍特药业、和记黄埔、艾力斯、人福医药、迈瑞医疗、晶泰科技、英矽智能、法国娇韵诗、中科院上海神经科学研究所等企业或高校研究所。2019年率先实现了InELN软件出海美国,如美国ADARx Pharmaceuticals、美国Staidson Biopharma、美国SparX Therapeutics,并陆续进入韩国、新加坡、法国、德国、日本等多个国家。
鹰谷明星产品——电子实验记录本InELN,资深科学家主导设计,致力于将每一个功能做深做透且高度灵活,整合InDraw和InSequence,建立实验知识库。支持云端部署或本地私有部署。全面接入DeepSeek,帮助企业50人做出100人的业绩。
鹰谷核心工具软件——InDraw结构式编辑器,支持中文(全球首家)或英文的IUPAC命名,高精度(99.75%)AI化学结构式图像识别,大分子编辑器HELM,全同位素绘制,兼容ChemDraw。有网页端、客户端两种版本,InDraw绘制的结构图,已在国际顶级期刊上发表数百篇SCI论文。
鹰谷新品工具软件——InSequence序列编辑器,对标SnapGene,由鹰谷纯自主研发,可用于DNA/RNA/蛋白序列编辑。兼容GenBank、Addgene文件中的序列信息,能实现质粒设计、引物设计、特征与酶切位点展现等功能,支持千万数量级碱基处理。
鹰谷新品工具软件——InPaper文献结构化系统,基于AI研发的专利/论文数据挖掘工具,能自动提取PDF专利或论文数据,获得结构式、反应式和活性数据,可用于AI训练,帮助企业建立自己的文献数据库,实现全文搜索、结构式和反应式搜索。
//推荐阅读
鹰谷电子实验记录本 | 全面接入DeepSeek,人走经验带不走
新版InDraw怎么用?免费版能商用吗?(文末有福利)
喜报 | 鹰谷信息成功晋级第五届全国工业软件创新应用大赛决赛
2025-12-25
圣诞佳节,我们满怀喜悦地见证鹰谷伙伴们接连斩获捷报,从首仿突破到原创研发,从融资推进到临床获批,我们为每一份成果感到骄傲。在数字化、AI化的研发新时代,鹰谷始终秉承“让研发有数据、有智慧、有未来,打造超级AI科学家”的理念,致力于通过电子实验记录本InELN、研发数据平台等一体化解决方案,助力企业构建研发数字基础。我们愿继续与客户并肩同行,以数据驱动创新,以AI赋能研发。接下来,让我们快速一览鹰谷部分伙伴们的最新成果:
奥锐特药业:国产首仿雌二醇片/雌二醇地屈孕酮片复合包装获批上市(奥锐特药业使用鹰谷电子实验记录本InELN和科研项目管理系统InProject)
天境生物:与石药集团合作的依达格鲁肽α治疗肥胖适应症上市申请获NMPA受理(天境生物使用鹰谷电子实验记录本InELN和科研项目管理系统InProject)
人福医药:1类创新药HWS117注射液获批临床(人福医药使用鹰谷电子实验记录本InELN和科研项目管理系统InProject)
和誉医药:1类新药ABSK141临床试验申请获FDA和NMPA批准(和誉医药使用鹰谷电子实验记录本InELN、库存管理系统InWMS、化合物与样品注册管理系统InCMS、科研项目管理系统InProject)
安领科生物:完成近5000万美元A轮追加融资(安领科生物使用鹰谷电子实验记录本InELN和科研项目管理系统InProject)
元码智药:完成天使+轮融资(元码智药使用鹰谷电子实验记录本InELN)
注:排名不分先后
喜报1:奥锐特药业国产首仿雌二醇片/雌二醇地屈孕酮片复合包装获批上市
近日,国家药监局(NMPA)官网的一则公示:扬州奥锐特药业申报的4类仿制药——雌二醇片/雌二醇地屈孕酮片复合包装正式获批生产。这一长期由跨国巨头雅培(Abbott)独占的“6亿级”大品种,终于迎来了首位国产破局者。国内首仿+首家过评,奥锐特此役不仅拿下了入场券,更抢占了国产替代的制高点。
截图:NMPA官网
雌二醇片/雌二醇地屈孕酮片复合包装(原研商品名:芬吗通),由雌二醇片(红片)和雌二醇地屈孕酮片(黄片)组成,通过模拟女性自然的生理周期,为绝经后女性提供序贯的激素补充。数据显示,近年来该品种在全终端销售额稳健保持在6亿元以上,且稳居性激素及生殖系统调节剂(化药)TOP 10榜单。6亿大品种首仿的诞生,是奥锐特的一小步,却是国产妇科内分泌用药市场的一大步。它打破了进口药物的长期垄断,为中国女性提供了更具性价比的治疗选择。
喜报2:天境生物宣布与石药集团合作的依达格鲁肽α治疗肥胖适应症上市申请获NMPA受理
天境生物近期宣布,公司合作伙伴石药集团(01093.HK)旗下附属公司百克(山东)生物制药股份有限公司递交的依达格鲁肽a(efmedaglutidealfa,又称TJ103或TG103)用于超重或肥胖成人长期体重管理的新药上市申请(BLA)已获中国国家药品监督管理局(NMPA)正式受理。
依达格鲁肽a是一款重组人源GLP-1(胰高血糖素样肽-1)Fc融合蛋白注射液,每周给药一次。该产品可选择性激活GLP-1受体,通过抑制食欲、减少食物摄入等机制实现体重下降同时改善血糖及代谢指标,展现出优异的减重疗效和良好的安全性,有望为超重及肥胖患者提供新的治疗选择。
喜报3:人福医药1类创新药HWS117注射液获批临床
近日,人福医药获得国家药品监督管理局核准签发的HWS117注射液的《药物临床试验批准通知书》,批准开展临床试验,适应症为用于辅助生殖中的控制性卵巢刺激,促进多卵泡发育。
辅助生殖技术(ART)是女性不孕症的有效治疗手段,促卵泡激素(FSH)在ART中卵泡的发育和成熟过程中起着重要作用。长期以来,国内辅助生殖市场由短效FSH药物主导,然而短效FSH在人体内半衰期短,为了达到临床刺激阈值需要在生殖周期连续8-12天皮下注射给药,患者身体负担较重。HWS117注射液作为一款新型长效FSH药物,拟通过延长FSH在体内的半衰期,满足减少注射频率、提高治疗依从性的临床需求。
HWS117注射液临床试验申请的获批,将进一步丰富人福医药在辅助生殖领域的创新产品管线。人福医药将加快推进该品种的临床研究相关工作,为不孕症患者带来更高效、便捷的治疗选择。
喜报4:和誉医药1类新药ABSK141临床试验申请获FDA和NMPA批准
12月1日,上海和誉生物医药科技有限公司(以下简称“和誉医药”,港交所代码:02256)宣布,其在研的口服、高活性、高选择性小分子KRAS G12D抑制剂ABSK141用于治疗携带KRAS G12D突变的晚期实体瘤患者的新药临床试验(IND)申请已获得美国食品药品监督管理局(FDA)批准。12月18日,CDE 官网显示,和誉医药申报的1类新药 ABSK141片 获批临床。
截图来源:CDE官网
此次获批的是一项开放性I/II期临床研究,旨在评估ABSK141在携带KRAS G12D突变的晚期实体瘤患者中的安全性、耐受性、有效性和药代动力学特征。
KRAS是人类癌症中最常见的致癌驱动基因之一,其中G12D是最常见的突变亚型,广泛存在于胰腺导管腺癌(PDAC)、结直肠癌(CRC)及非小细胞肺癌(NSCLC)等多种实体瘤中。由于G12D突变导致蛋白构象发生独特改变,其药物靶向性开发长期面临极大挑战,目前尚无针对KRAS G12D突变的靶向疗法获批上市。
喜报5:安领科生物宣布完成近5000万美元A轮追加融资
12月16日,安领科生物 (Allink Biotherapeutics)宣布完成近5000万美元A轮追加融资。该公司致力于开发肿瘤及免疫领域的下一代ADC及多特异性抗体药物。本轮A轮扩展融资将助力加速推进公司两款核心管线的全球临床开发。其中,ALK201为一款靶向FGFR2b的ADC,已在多种肿瘤类型中展现出令人鼓舞的疗效信号及良好的安全性,旨在开发成为FGFR2b过表达实体瘤的基石疗法。同步推进的ALK202项目为一款EGFR/cMET双特异性ADC,其早期临床数据也初步验证了该产品在非小细胞肺癌治疗中的潜力。此外,该项目正在进一步扩展临床评估范围,覆盖更多由生物标志物定义的肿瘤类型及患者群体。
除了ADC疗法,安领科生物还正积极布局遮蔽型T细胞衔接器(Masked TCE)平台,旨在推动TCE疗法在实体瘤领域的创新性应用。在免疫及炎症疾病领域,安领科生物基于对致病机制的深刻理解,正在推进多个双/多特异性抗体项目。
喜报6:元码智药宣布完成天使+轮融资
12月15日,元码智药(Byterna Therapeutics)宣布完成天使+轮融资。本轮融资资金将用于加速推进环状mRNA(cmRNA)体内CAR-T管线BR101的IIT临床研究。元码智药成立于2023年,是一家以环状mRNA和靶向tLNP技术为核心的创新生物医药公司,聚焦于环状mRNA免疫治疗新药研发。基于环状mRNA化学修饰、体内T细胞靶向递送和环状mRNA CAR设计等技术,该公司研发了多条体内CAR-T管线,目前核心管线正快速推向临床研究。
参考来源:医药观澜、药闻天下、人福医药、天境生物TJBIO、摩熵医药
关于鹰谷
让研发有数据、有智慧、有未来
上海鹰谷信息科技有限公司(Integle)成立于2013年,建立鹰谷科研智能管理平台,Scientific Intelligence Management System, SIMS,致力于为企业建立自己的科研知识库和AI生产力工具。以电子实验记录本为中心,提供电子实验记录本InELN、科研库存管理系统InWMS、化合物与样品注册管理InCMS、科研项目管理系统InProject、科研采购管理InPMS等科研数据管理系统,由科学家打造,拥有结构式编辑器InDraw、生物序列编辑器InSequence、文献结构化工具InPaper、科研AI大模型InAI等科研工具类软件。
经过10多年的迭代开发,掌握IUPAC中英文命名、化学结构高精度AI图像识别、质粒设计、引物设计等专业技术,实现国产替代,解决很多行业“卡脖子”问题。鹰谷SIMS平台全面接入DeepSeek,结合鹰谷知识图谱,AI直接生成周报、论文、专利、CTD申报资料等底稿,打造实验设计、专利写作、QA检查、申报注册等多种数字员工,助力企业拥有专属的“超级AI科学家”,从而显著提升100倍的研发效率。
服务团队大多数为来自世界五百强、北京大学、复旦大学、上海交通大学、浙江大学等化学、生物领域的科学家和工程师,做到真正理解客户需求,为客户的业务场景提供更专业的解决方案,具备30分钟快速反馈的响应机制,让客户更安心。
目前,鹰谷已经服务了700多家行业标杆客户(其中100多家上市企业),全面覆盖生物医药、化工、新材料、新能源、食品日化等研发领域,如华为、扬子江、倍特药业、马应龙、和记黄埔、艾力斯、人福医药、迈瑞医疗、晶泰科技、英矽智能、法国娇韵诗、中科院上海神经科学研究所等企业或高校研究所。2019年率先实现了InELN软件出海美国,如美国ADARx Pharmaceuticals、美国Staidson Biopharma、美国SparX Therapeutics,并陆续进入韩国、新加坡、法国、德国、日本等多个国家。
鹰谷明星产品——电子实验记录本InELN,资深科学家主导设计,致力于将每一个功能做深做透且高度灵活,整合InDraw和InSequence,建立实验知识库。支持云端部署或本地私有部署。全面接入DeepSeek,帮助企业50人做出100人的业绩。
鹰谷核心工具软件——InDraw结构式编辑器,支持中文(全球首家)或英文的IUPAC命名,高精度(99.75%)AI化学结构式图像识别,大分子编辑器HELM,全同位素绘制,兼容ChemDraw。有网页端、客户端两种版本,InDraw绘制的结构图,已在国际顶级期刊上发表数百篇SCI论文。
鹰谷新品工具软件——InSequence序列编辑器,对标SnapGene,由鹰谷纯自主研发,可用于DNA/RNA/蛋白序列编辑。兼容GenBank、Addgene文件中的序列信息,能实现质粒设计、引物设计、特征与酶切位点展现等功能,支持千万数量级碱基处理。
鹰谷新品工具软件——InPaper文献结构化系统,基于AI研发的专利/论文数据挖掘工具,能自动提取PDF专利或论文数据,获得结构式、反应式和活性数据,可用于AI训练,帮助企业建立自己的文献数据库,实现全文搜索、结构式和反应式搜索。
//推荐阅读
鹰谷电子实验记录本 | 全面接入DeepSeek,人走经验带不走
颜值超越ChemDraw,实力相当强:InDraw 7.0携ADMET预测与3D大版本升级
全球首款新药上市、港交所上市 | 祝贺乐普生物、南大光电、先为达生物等7家鹰谷客户!
一致性评价引进/卖出上市批准
100 项与 SparX Therapeutics, Inc. 相关的药物交易
登录后查看更多信息
100 项与 SparX Therapeutics, Inc. 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2026年06月09日管线快照
管线布局中药物为当前组织机构及其子机构作为药物机构进行统计,早期临床1期并入临床1期,临床1/2期并入临床2期,临床2/3期并入临床3期
药物发现
1
7
临床前
临床1期
3
2
其他
登录后查看更多信息
当前项目
| 药物(靶点) | 适应症 | 全球最高研发状态 |
|---|---|---|
SPX-303 ( LILRB2 x PDL1 ) | 头颈部鳞状细胞癌 更多 | 临床1期 |
SPX-102 ( CLDN18.2 ) | 肿瘤 更多 | 临床1期 |
SPX-304 | 结肠癌 更多 | 临床前 |
ALA-105 ( CLDN18.2 ) | 肿瘤 更多 | 临床前 |
SPX-306 | 肿瘤 更多 | 临床前 |
登录后查看更多信息
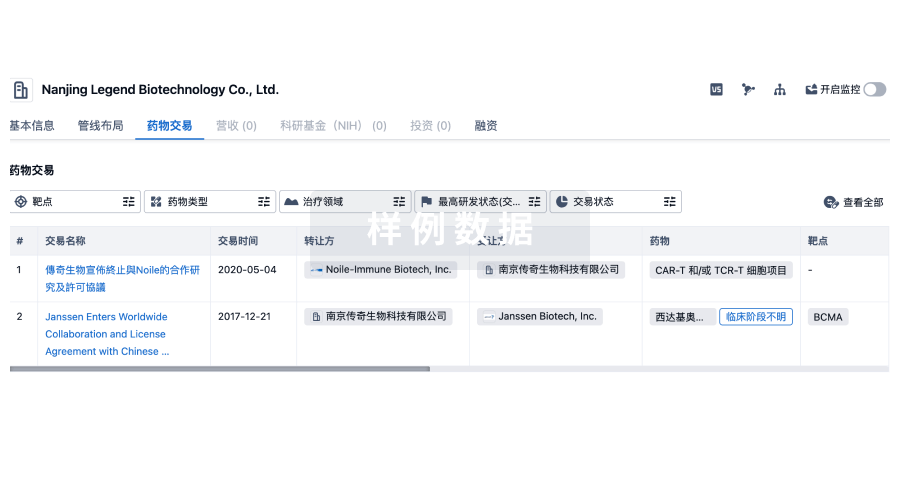
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
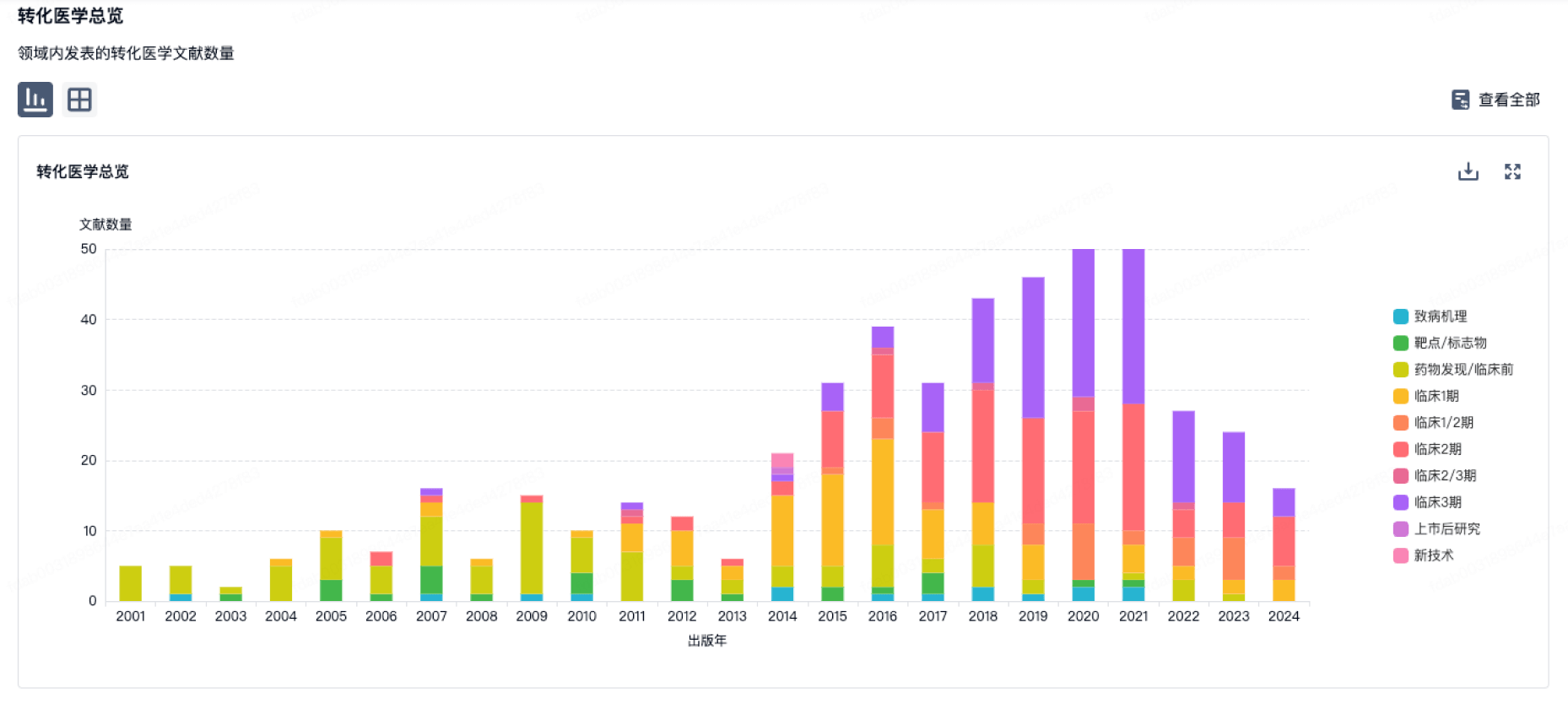
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
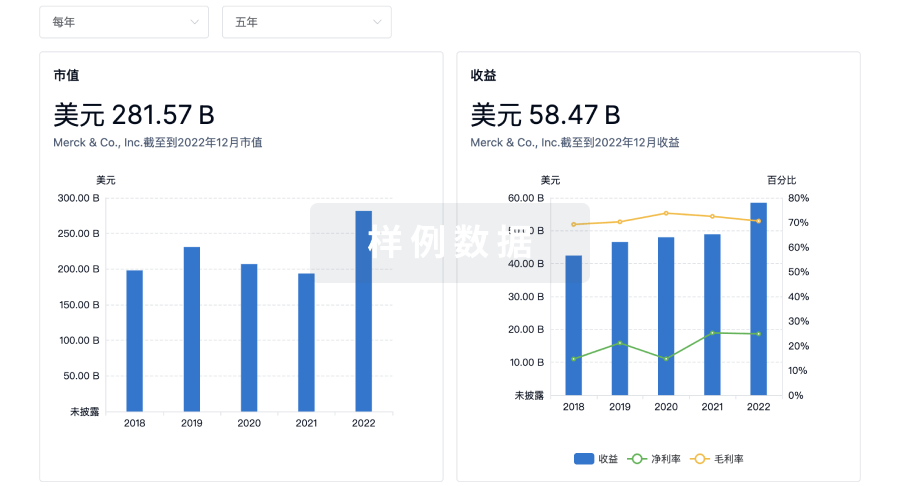
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
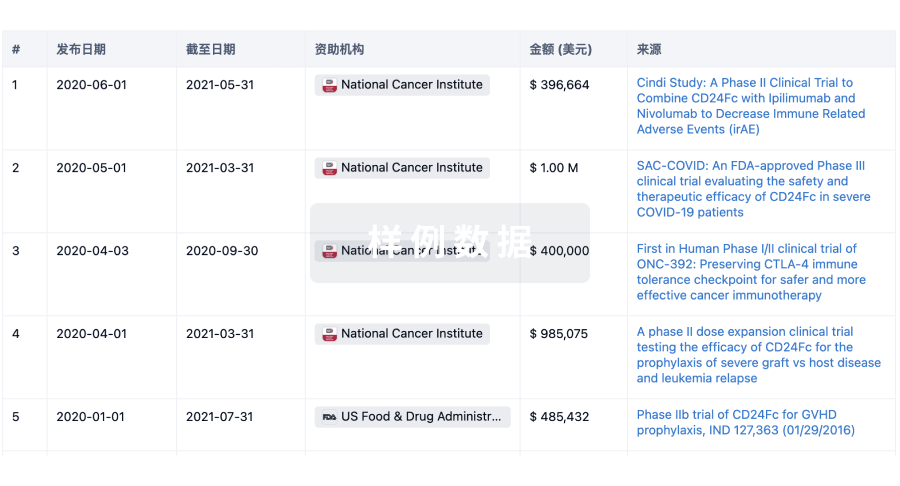
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
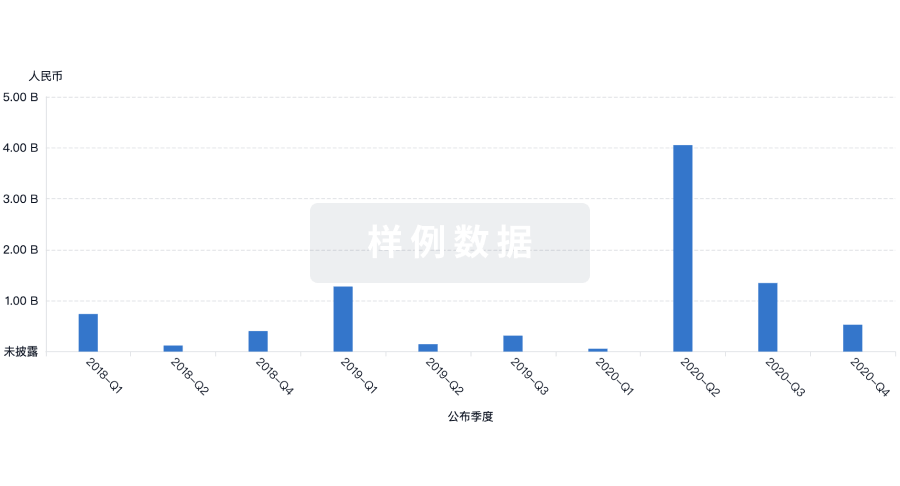
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
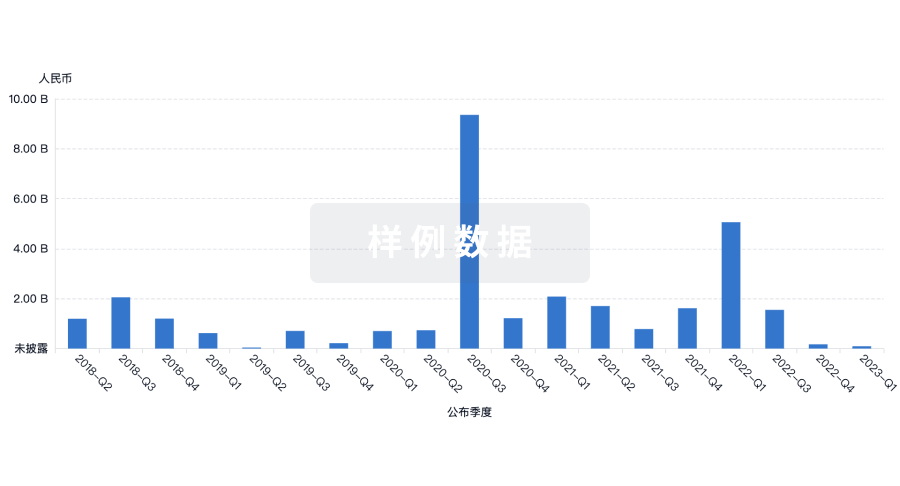
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用