预约演示
更新于:2026-03-14
Recibokibart
瑞西奇拜单抗
更新于:2026-03-14
概要
基本信息
原研机构 |
非在研机构- |
权益机构- |
最高研发阶段申请上市 |
首次获批日期- |
最高研发阶段(中国)申请上市 |
特殊审评优先审评 (美国)、孤儿药 (美国)、优先审评 (中国) |
登录后查看时间轴
结构/序列
Sequence Code 941453118H

来源: *****
Sequence Code 941453119L

来源: *****
关联
7
项与 瑞西奇拜单抗 相关的临床试验NCT06716151
A Phase I, Randomized, Double-blind, Placebo-controlled, Single/mulit Dose-escalation Study to Evaluate the Safety, Tolerability, and Pharmacokinetics of HB0034 in Adult Healthy Subjects
The aim of this study is to investigate the safety and tolerability of HB0034 in healthy subjects following a single dose or multiple dose.
开始日期2024-12-06 |
申办/合作机构 |
NCT06477536
A Phase IIb, Long-Term Extension Study to Evaluate the Safety and Efficacy of HB0034 in the Treatment of Adult Subjects With Generalized Pustular Psoriasis
This is a Phase IIb, long term extension study to evaluate the safety and efficacy of HB0034 in adult subjects with generalized pustular psoriasis (GPP).
开始日期2024-09-02 |
申办/合作机构 |
CTR20242844
评价HB0034在泛发性脓疱型银屑病患者中安全性和疗效的多中心、单臂、开放标签IIb期长期安全扩展研究
评价HB0034在GPP患者中的长期安全性和耐受性
开始日期2024-09-02 |
申办/合作机构  上海华奥泰生物药业股份有限公司 上海华奥泰生物药业股份有限公司 [+1] |
100 项与 瑞西奇拜单抗 相关的临床结果
登录后查看更多信息
100 项与 瑞西奇拜单抗 相关的转化医学
登录后查看更多信息
100 项与 瑞西奇拜单抗 相关的专利(医药)
登录后查看更多信息
1
项与 瑞西奇拜单抗 相关的文献(医药)2025-06-01·JOURNAL OF THE EUROPEAN ACADEMY OF DERMATOLOGY AND VENEREOLOGY
Recibokibart, an anti‐IL ‐36 receptor monoclonal antibody, for treating generalized pustular psoriasis: Phase 1b trial
Letter
作者: Zhang, Furen ; Chen, Jiaqi ; Zhang, Chunlei ; Ma, Xiuqiang ; Zhan, Yifan ; Lu, Xueyan ; Ma, Chi ; Man, Xiaoyong ; Kuang, Yehong ; Yang, Yongming ; Qian, Qiaoxia ; Zhang, Zhaoxia ; Situ, Xiaolu ; Li, Benke ; Yang, Baoqi ; Chen, Shi ; Zhu, Xiangyang ; Su, Juan ; Zhou, Guodong ; Wang, Jiucun ; Chen, Qian ; Feng, Yujie
Inhibiting the interleukin-36 pathway has demonstrated promising results in managing generalized pustular psoriasis (GPP),1-4 a severe and potentially life-threatening inflammatory skin condition.5 Spesolimab is currently the only approved biologic specifically targeting IL-36R for GPP.1, 2, 6 Recibokibart, a novel human anti-IL-36R IgG1 monoclonal antibody with unique complementarity-determining region (CDR) sequences7 has demonstrated comparable affinity for IL-36R and comparable IC50 for IL-6 secretion on human intestinal fibroblasts to spesolimab (KD: 0.104 nM vs. 0.112 nM, IC50:0.338 nM vs. 0.418 nM). Recibokibart has demonstrated favourable safety and tolerability in two trials involving healthy subjects: a single-dosing study8 (NCT05064345) and a multiple-dosing study (NCT05460455). The development of recibokibart would potentially expand the treatment options available for GPP. We report the safety and efficacy results from an open-label, single-arm phase 1b study (NCT05512598) of recibokibart in patients experiencing an acute GPP flare of moderate-to-severe intensity. This study was conducted in six hospitals in China between January and November 2023. Eligible patients received a single dose of recibokibart at 15 mg/kg intravenously on Day 1. The primary endpoint, focusing on safety, was assessed for up to 90 days, while efficacy, the key secondary endpoint, was evaluated for up to 12 weeks. Disease severity was assessed by GPP-specific scales9 including Generalized Pustular Psoriasis Physician Global Assessment (GPPGA), Generalized Pustular Psoriasis Area and Severity Index (GPPASI) and Japan Dermatology Association GPP Severity Index (JDA-SI). Nine patients were enrolled with eight completing the study. At baseline, the mean (SD) age was 48.0 (9.63) years. Five patients (55.54%) were females. Six patients (66.67%) had the IL36RN gene mutation. All patients had a GPPGA total score of 3 or 4 (moderate or severe) and a GPPGA pustulation score of 3 or 4. The mean (SD) GPPASI and JDA-SI were 37.54 (15.23) and 11.0 (2.45), respectively. Seven patients (77.78%) reported treatment-emergent adverse events (TEAEs), all of which were graded as mild or moderate. No serious adverse event reported, and no patients withdrew due to TEAEs. Four patients (44.44%) reported drug-related TEAEs. The most common TEAEs (≥2 patients) were anaemia, itching, upper respiratory tract infection, hyperuricemia and hyperlipidaemia. Recibokibart demonstrated a rapid onset of action. At Week 1, a GPPGA total score of 0/1 (clear/almost clear skin) was achieved in four patients (44.44%). Three patients (33.33%) achieved a GPPGA pustulation score of 0 (no visible pustules) and seven patients (77.78%) achieved the GPPGA pustulation score of 0/1 (no/almost no visible pustules) at Week 1. Additionally, there was an average improvement of 59.06% in GPPASI at Week 1 and 51.30% in JDA-SI score at Week 2. GPPGA, Pustulation score, GPPASI and JDA-SI were all maintained up to Week 12 (Table 1). The photographs taken were consistent with these improvements. Representative photographic documentation for two patients was illustrated in Figure 1. A rapid decrease in mean C-reactive protein level was observed from baseline of 110.01 mg/L to the normal level of 5.30 mg/L at Week 2 (Table 1). This study was the first clinical study of recibokibart in patients with GPP. Recibokibart was demonstrated favourable safety, and the patients achieved rapid and sustained improvements in the pustules, overall lesions and systemic inflammation following a single dose. Recibokibart could potentially serve as a new safe and effective therapeutic option for patients with GPP. However, the limitations of the small sample size and the single-arm design reduced the generalizability of our findings. The efficacy and safety of recibokibart are currently under further evaluation in a larger, randomized, double-blind, placebo-controlled pivotal clinical trial (NCT06231381), which is expected to provide more robust evidence. This trial was fully funded by Shanghai Huaota Biopharmaceutical Co., Ltd. Prof. Jiucun Wang was supported by the CAMS Innovation Fund for Medical Sciences (2019-12M-5-066). Qiaoxia Qian, Chi Ma, Guodong Zhou, Xiaolu Situ, Xiuqiang Ma, Yujie Feng, Shi Chen, Yifan Zhan, Qian Chen, and Xiangyang Zhu are full-time employees of Shanghai Huaota Biopharmaceutical Co. Ltd. C.J. and other authors declare no conflicts of interest. The study protocol was approved by (1) Shandong First Medical University-Affiliated Skin Disease Hospital Medical Ethics Committee; approval # 20230113XZA002; (2) The Second Affiliated Hospital Zhejiang University School of MedicineEthics Committee; approval # (2023) No. 386; (3) Sun Yat-sen Memorial Hospital of Sun Yat-sen University Medical Ethics Committee; approval # SYSYW-2022-287-02; (4) Peking University Third Hospital Medical Scientific Research Ethics Committee; approval # (2022) No. 186–03; (5) Xiangya Hospital of Central South University Medical Ethics Committee; approval # 202304288; and (6) The First Hospital of Hebei Medical University Ethics Committee; approval # [2023] No. 504–01. The patients in this manuscript have given written informed consent to the publication of their case details. The data that support the findings of this study are available from the corresponding author upon reasonable request.
114
项与 瑞西奇拜单抗 相关的新闻(医药)2026-03-11
声明:因水平有限,错误不可避免,或有些信息非最及时,欢迎留言指出。本文仅作医疗健康相关药物介绍,非治疗方案推荐(若涉及);本文不构成任何投资建议。
罕见病,这个看似遥远的词汇,却与全球数亿人的健康息息相关。在已知的7000多种罕见病中,仅有5%的患者能够获得有效的治疗。每一款罕见病新药的问世,都意味着为患者带来了新的希望。2026年,7款罕见病生物药有望在中国获批上市,涵盖血友病、重症肌无力、脊髓性肌萎缩症等多个领域,将为中国罕见病治疗带来革命性的变化。
2026年预计上市的7款罕见病生物药,最显著的特征的是“跨国巨头与本土企业同台竞技”,打破了此前罕见病赛道由跨国药企垄断的格局,形成“百花齐放”的产业生态。这一格局的形成,既是全球罕见病药物研发浪潮的推动,也是中国本土药企创新能力提升、政策红利释放的必然结果,标志着中国罕见病产业已从“被动跟随”进入“主动突围”的发展阶段。 从企业布局来看,跨国药企凭借长期的研发积累与技术优势,依然占据罕见病赛道的重要地位,7款新药中,有4款来自诺华、强生、拜玛林制药、CSL等国际巨头,覆盖基因治疗、单抗、酶替代治疗等前沿技术领域,聚焦脊髓性肌萎缩症、软骨发育不全等临床需求迫切的罕见病。
多款药物具有“First-in-class”(全球首创)潜力,聚焦此前未被攻克的靶点,采用基因治疗、环状多肽、双靶点抑制等前沿技术,彻底改变了传统罕见病的治疗模式,从“对症治疗”向“精准根治”升级,为患者带来了全新的生存希望。
诺华作为全球罕见病领域的领军企业,此次带来的Onasemnogene abeparvovec是一款针对脊髓性肌萎缩症的基因治疗药物,也是全球首个获批的脊髓性肌萎缩症基因疗法。
Onasemnogene abeparvovec(诺华)作为全球首个获批的脊髓性肌萎缩症基因疗法,其核心创新在于“一次性基因修复”,彻底打破了脊髓性肌萎缩症“终身治疗、无法根治”的困局。
脊髓性肌萎缩症是一种罕见的遗传性神经肌肉疾病,由SMN1基因缺陷导致,患者会出现进行性肌肉无力、萎缩,严重者会因呼吸衰竭死亡,传统治疗主要依赖nusinersen等药物的终身注射,只能延缓疾病进展,无法从根本上解决问题。
Onasemnogene abeparvovec采用腺相关病毒(AAV)载体,将正常的SMN1基因精准递送至患者体内,替代缺陷基因的功能,实现“一次性治疗、终身受益”。临床研究数据显示,接受该药物治疗的婴儿型脊髓性肌萎缩症患者,能够快速恢复运动功能,大部分患者可实现自主站立、行走,显著降低了疾病死亡率与致残率。
这款药物的上市,不仅为脊髓性肌萎缩症患者带来了根治的希望,更推动了基因治疗在罕见病领域的应用,为其他遗传性罕见病的治疗提供了可借鉴的范式。
伏索利肽(拜玛林制药)作为全球首个针对软骨发育不全的环状多肽药物,其创新之处在于靶向NPR2靶点,打破了这类遗传性骨骼疾病“无药可医”的困局。软骨发育不全是最常见的遗传性侏儒症,由FGFR3基因突变导致,患者会出现身材矮小、骨骼畸形、关节疼痛等症状,传统治疗主要依赖生长激素注射,疗效有限且无法改善骨骼畸形。
伏索利肽通过模拟NPR2受体的激活配体,能够有效抑制FGFR3基因的异常激活,促进软骨细胞的增殖与分化,改善患者的骨骼生长发育,不仅能够帮助患者提升身高,还能缓解关节疼痛、改善骨骼畸形,显著提升患者的生活质量。临床研究显示,接受伏索利肽治疗的儿童患者,年生长速度较安慰剂组显著提升,且安全性良好,不良反应多为轻度至中度,可通过对症治疗有效控制。
这款药物的上市,标志着软骨发育不全的治疗进入“精准靶向”时代,为其他遗传性骨骼疾病的治疗提供了新的思路。
除了这两款“首创新药”,一些多个靶点创新也值得关注,FcRn单抗(强生尼卡利单抗、和铂医药巴托利单抗)是针对重症肌无力的新型免疫靶向药物,其作用机制是靶向新生儿Fc受体(FcRn),阻断FcRn与免疫球蛋白G(IgG)的结合,促进致病性IgG的降解,从而减轻免疫反应对神经肌肉接头的损伤,改善患者的肌肉无力症状。
重症肌无力是一种罕见的自身免疫性疾病,传统治疗主要依赖激素、免疫抑制剂等药物,长期使用会带来严重的不良反应,且部分患者疗效不佳。FcRn单抗的上市,不仅为重症肌无力患者提供了更安全、更有效的治疗选择,其独特的作用机制还为其他自身免疫性罕见病的治疗提供了新的方向,具有广阔的应用前景。值得关注的是,FcRn单抗的治疗潜力远不止于重症肌无力,目前全球范围内正开展多项临床试验,探索其在自身免疫性脑炎、天疱疮等其他自身免疫性疾病中的应用,未来有望实现多适应症覆盖。
FXIIa抑制剂(CSL加达西单抗)是针对遗传性血管性水肿的新型靶向药物,其作用机制是抑制凝血因子XIIa(FXIIa)的活性,阻断血管性水肿的发作,为这类患者提供了精准的预防与治疗手段。遗传性血管性水肿是一种罕见的遗传性疾病,患者会出现反复发作的皮肤、黏膜水肿,严重时会因喉头水肿导致窒息死亡,传统治疗主要依赖C1酯酶抑制剂替代治疗,价格高昂且可及性有限。
FXIIa抑制剂的上市,填补了该领域的治疗空白,能够有效预防水肿发作,提升患者的生活质量,同时降低治疗成本。
这些突破性治疗机制的应用,不仅改变了罕见病的治疗模式,更推动了罕见病的疾病管理模式升级——从“被动应对疾病发作”向“主动预防、精准控制”转变,从“追求生存”向“追求高质量生存”转变。
舒泰神的波米泰酶a是一款针对B型血友病的蛋白替代治疗药物,能够补充患者体内缺乏的凝血因子X,有效预防和控制出血症状,为中国B型血友病患者提供了本土化的治疗选择。
华海药业的瑞西奇拜单抗是一款IL36R单抗,用于治疗泛发性脓疱型银屑病,这款药物的上市,填补了本土企业在免疫炎症类罕见病领域的空白,彰显了本土药企在单抗领域的研发突破。
和铂医药的巴托利单抗是一款FcRn单抗,用于治疗重症肌无力,该药物的上市,为重症肌无力患者提供了更多的治疗选择。
罕见病患者往往面临着诊断困难、治疗手段有限、药物价格高昂等问题。生物药的问世,为罕见病患者带来了新的希望。生物药具有靶向性强、疗效显著、副作用小等优点,能够有效缓解患者的症状,提高患者的生活质量。同时,生物药的研发和上市,也将推动罕见病诊疗模式的升级,从“被动应对疾病发作”向“主动预防、精准控制”转变,从“追求生存”向“追求高质量生存”转变。
2026年,7款罕见病生物药新药的集中上市,是中国罕见病产业发展的重要里程碑,标志着中国罕见病治疗从“无药可医”向“有药可用”的重大跨越,也彰显了中国生物医药产业的创新实力与发展速度。但我们必须清醒地认识到,“用药难”的破局,不仅需要新药的上市,更需要解决可及性与支付能力的核心痛点。
罕见病的治疗,从来都不是一个人的战斗,而是需要政府、企业、医疗机构、患者组织等多方协同发力、共同努力。相信在政策的持续支持、药企的创新突破、社会各界的共同关注下,中国将逐步构建起可持续的罕见病保障体系,让每一位罕见病患者都能“用得起药、用得到药”,让“罕见病不再罕见,患者不再孤单”,推动中国罕见病产业进入“精准治疗、多元可及”的全新发展阶段。
资料来源:药事纵横
END
官方建群啦!
生物药大时代组建了抗体药、疫苗、核酸药物等多个相关领域的实名制微信交流群,扫描下方二维码即可入群!
2026-03-10
·龙珠凤舞
2026年开局之际,14款罕见病新药有望在中国获批上市,覆盖血友病、重症肌无力、脊髓性肌萎缩症等多个领域。
2026年有望获批的罕见病新药
药品名称
靶点
类别
适应症
企业
申请上市受理时间
立康可泮
CFB
化药
阵发性睡眠性血红蛋白尿症
恒瑞
2026.01.10
HSK39297
CFB
化药
阵发性睡眠性血红蛋白尿症
海思科
2026.01.06
瑞西奇拜单抗
L36R
单抗
泛发性脓疱型银屑病
华海药业
2025.10.01
盐酸毗昔替尼
CSF1R/KIT/FLT3
化药
腱建鞘巨细胞瘤
第一三共
2025.01.15
尼卡利单抗
FcRn
单抗
重症肌无力
强生
2025.04.23
MY008211A
CFB
化药
阵发性睡眠性血红蛋白尿症
启瑞科技
2026.02.26
Onasemnogene abeparvovec
SMN1
基因治疗
脊髓性肌菱缩症
诺华
2025.08.02
美国已上市
伏索利肽
NPR2
环状多肽
软骨发育不全
拜玛林制药
2025.09.05
加达西单抗
FXlla
单抗
遗传性血管性水肿(推测)
CSL
2025.07.17
司替戊醇
GABR
化药
Dravet综合征(推测)
Biocodex/DesitinGmbH/明治制果/M8
2025.04.29
阿帕达酶a
VWF
酶
血栓性血小板减少性紫癜
武田
2025.04.09
目前发补
巴托利单抗
FcRn
单抗
重症肌无力
DRAGON MERIT HOLDINGS LIMITED/
Samsung Biologics Co., Ltd./
诺纳生物(苏州)有限公司
2024.07.18
那韦培肽
FGFR3
多肽
骨骺未闭合软骨发育不全
维昇药业
2026.03.06
STSP-0601
凝血因子X
蛋白类药物
血友病A或B
江苏贝捷泰生物科技有限公司/舒泰神(北京)生物制药股份有限公司
2025.05.31
基因治疗与环状多肽创新药物
在众多“首创新药”中,基因疗法Onasemnogene abeparvovec与环状多肽伏索利肽、那韦培肽最具代表性,二者分别代表了罕见病治疗领域的两大创新方向:基因治疗实现“一次性根治”,环状多肽实现“精准靶向、长效控制”,引领罕见病治疗进入“精准革命”时代。
Onasemnogene abeparvovec(诺华):作为全球首个获批的脊髓性肌萎缩症(SMA)基因疗法,其核心创新在于“一次性基因修复”,彻底打破了SMA“终身治疗、无法根治”的困局。该药物采用腺相关病毒(AAV)载体,将正常的SMN1基因精准递送至患者体内,替代缺陷基因的功能,实现“一次性治疗、终身受益”。临床研究数据显示,接受该药物治疗的婴儿型SMA患者,能够快速恢复运动功能,大部分患者可实现自主站立、行走,显著降低了疾病死亡率与致残率。
伏索利肽(拜玛林制药):作为全球首个针对软骨发育不全的环状多肽药物,其创新之处在于靶向NPR2靶点,打破了这类遗传性骨骼疾病“无药可医”的困局。该药物通过模拟NPR2受体的激活配体,能够有效抑制FGFR3基因的异常激活,促进软骨细胞的增殖与分化,改善患者的骨骼生长发育。临床研究显示,接受伏索利肽治疗的儿童患者,年生长速度较安慰剂组显著提升,且安全性良好,不良反应多为轻度至中度,可通过对症治疗有效控制。
那韦培肽:临床前与临床数据显示,C型利钠肽(CNP)通路可调控生长发育,补充CNP能抵消FGFR3下游突变的异常影响,从而促进骨骼生长。该药物可向全身组织(包括生长板、骨骼肌)持续递送活性CNP,以此实现对软骨发育不全症患者的治疗作用。
血液系统罕见病新药
血液系统罕见病是此次新药覆盖的重点领域,共有5款新药,涵盖阵发性睡眠性血红蛋白尿症、B型血友病、血栓性血小板减少性紫癜等3种疾病,填补了多个治疗空白。
CFB抑制剂(恒瑞立康可泮、海思科HSK39297、启瑞科技MY008211A):针对阵发性睡眠性血红蛋白尿症的新型靶向药物,其作用机制是抑制补体因子B(CFB)的活性,阻断补体系统的异常激活,从而减少红细胞的破坏,缓解患者的溶血症状。
STSP-0601(舒泰神):本土首款针对B型血友病的蛋白替代治疗药物,打破了外资药物的垄断。
阿帕达酶a(武田):为血栓性血小板减少性紫癜这类易导致血栓、出血的罕见血液疾病提供了有效的酶替代治疗选择。
神经肌肉系统罕见病新药
神经肌肉系统罕见病共有4款新药,涵盖脊髓性肌萎缩症、重症肌无力、Dravet综合征等3种疾病。
司替戊醇(Biocodex等企业):作为GABR抑制剂,填补了Dravet综合征的治疗空白,能够有效减少癫痫发作次数,改善患者的预后。
FcRn单抗(强生尼卡利单抗、和铂医药巴托利单抗):针对重症肌无力的新型免疫靶向药物,其作用机制是靶向新生儿Fc受体(FcRn),阻断FcRn与免疫球蛋白G(IgG)的结合,促进致病性IgG的降解,从而减轻免疫反应对神经肌肉接头的损伤,改善患者的肌肉无力症状。
免疫炎症系统罕见病新药
免疫炎症系统罕见病的新药,为华海药业的瑞西奇拜单抗(IL36R单抗,用于泛发性脓疱型银屑病)和CSL的加达西单抗(FXIIa抑制剂,用于遗传性血管性水肿)。
瑞西奇拜单抗:为泛发性脓疱型银屑病这类患者提供了精准的免疫靶向治疗选择。
加达西单抗:作为针对遗传性血管性水肿的新型靶向药物,其作用机制是抑制凝血因子XIIa(FXIIa)的活性,阻断血管性水肿的发作,为这类患者提供了精准的预防与治疗手段。
这些突破性治疗机制的应用,不仅改变了罕见病的治疗模式,更推动了罕见病的疾病管理模式升级——从“被动应对疾病发作”向“主动预防、精准控制”转变,从“追求生存”向“追求高质量生存”转变;精准对接不同类型罕见病患者的临床需求,其中多个领域长期被忽视,将迎来“从0到1”的治疗突破。
14款罕见病新药的集中上市,无疑为中国罕见病患者带来了前所未有的希望,标志着中国罕见病治疗进入“有药可用”的新阶段。但我们必须清醒地认识到:新药上市只是起点,“用药难”的核心痛点——可及性与支付能力,依然是横在患者面前的“最后一道坎”。即使有了新药,若患者无法获得药物、无法承担药物费用,“有药可用”也只能是一句空话。目前,罕见病新药上市后面临的现实困境主要集中在三个方面:一是定价高昂,罕见病药物研发成本高、患者群体小,药企为收回研发成本,往往会设定较高的价格,部分基因治疗药物、酶替代治疗药物每年的治疗费用可达数百万元,远超普通家庭的支付能力;二是医保覆盖有限,虽然近年来医保谈判持续向罕见病药物倾斜,但目前纳入医保目录的罕见病药物数量依然有限,多数新药上市后短期内无法纳入医保,患者需自行承担全部费用;三是患者认知不足与诊疗资源分布不均,部分罕见病症状复杂、诊断困难,很多患者无法及时确诊,即使有新药上市,也无法及时获得治疗,同时,优质的罕见病诊疗资源主要集中在一线城市,基层患者难以获得精准的诊疗与用药指导。说明推动医保或惠民保的涉及和涵盖这部分药物。
基因疗法上市批准临床研究
2026-03-09
·药事纵横
罕见病,虽名为“罕见”,却影响着全球数亿人的命运。面对超7000种已知罕见病,仅5%有药可治的窘境,每一次新药的上市,都是患者群体的一场“及时雨”。2026年,13款罕见病新药有望在中国获批上市,覆盖血友病、重症肌无力、脊髓性肌萎缩症等多个领域。
表:2026年中国有望获批的罕见病新药
一、跨国药企与本土力量同台竞技,罕见病赛道“百花齐放”
2026年预计上市的13款罕见病新药,最显著的特征的是“跨国巨头与本土企业同台竞技”,打破了此前罕见病赛道由跨国药企垄断的格局,形成“百花齐放”的产业生态。这一格局的形成,既是全球罕见病药物研发浪潮的推动,也是中国本土药企创新能力提升、政策红利释放的必然结果,标志着中国罕见病产业已从“被动跟随”进入“主动突围”的发展阶段。
从企业布局来看,跨国药企凭借长期的研发积累与技术优势,依然占据罕见病赛道的重要地位,13款新药中,有7款来自诺华、强生、第一三共、武田、拜玛林制药、CSL等国际巨头,覆盖基因治疗、单抗、酶替代治疗等前沿技术领域,聚焦脊髓性肌萎缩症、软骨发育不全、血栓性血小板减少性紫癜等临床需求迫切的罕见病。
诺华作为全球罕见病领域的领军企业,此次带来的Onasemnogene abeparvovec,是一款针对脊髓性肌萎缩症的基因治疗药物,也是全球首个获批的脊髓性肌萎缩症基因疗法,其上市将彻底改变这类疾病的治疗模式——从传统的对症支持治疗,升级为一次性基因修复治疗,为患者带来“一劳永逸”的治疗希望。拜玛林制药的伏索利肽,作为全球首个针对软骨发育不全的环状多肽药物,填补了这类遗传性骨骼疾病的治疗空白,能够有效改善患者的生长发育障碍,提升患者的生活质量。
强生、第一三共、武田等跨国企业也纷纷发力:强生的尼卡利单抗的是一款FcRn单抗,针对重症肌无力,能够靶向清除致病性IgG抗体,改善患者的临床症状;第一三共的吡昔替尼,作为CSF1R/KIT/FLT3多靶点抑制剂,用于治疗腱鞘巨细胞瘤,打破了这类局部侵袭性软组织肿瘤“手术复发率高、无有效药物”的困局;武田的阿帕达酶a,是一款针对血栓性血小板减少性紫癜的酶替代治疗药物,能够有效补充患者体内缺乏的血管性血友病因子(VWF),降低血栓形成风险。
与跨国巨头形成呼应的是,中国本土药企在罕见病领域的加速突围,13款新药中,有6款来自恒瑞、海思科、华海药业、舒泰神、启瑞科技等本土企业,涵盖化药、单抗、蛋白药物等多种类型,聚焦阵发性睡眠性血红蛋白尿症、B型血友病、泛发性脓疱型银屑病等疾病,展现出本土药企在罕见病领域的创新实力与战略转型成效。
恒瑞医药作为中国本土创新药企的龙头,此次凭借立康可泮切入罕见病赛道,这款CFB抑制剂用于治疗阵发性睡眠性血红蛋白尿症,是恒瑞在罕见病领域的首款创新药,标志着其从“肿瘤领域”向“罕见病领域”的战略延伸。海思科的HSK39297、启瑞科技的MY008211A,同样是针对阵发性睡眠性血红蛋白尿症的CFB抑制剂,三款本土CFB抑制剂的同步上市,不仅打破了外资药物在该领域的垄断,更形成了“本土竞争、协同突破”的良好格局。
舒泰神的波米泰酶a,是一款针对B型血友病的蛋白替代治疗药物,能够补充患者体内缺乏的凝血因子X,有效预防和控制出血症状,为中国B型血友病患者提供了本土化的治疗选择;华海药业的瑞西奇拜单抗,是一款IL36R单抗,用于治疗泛发性脓疱型银屑病,这款药物的上市,填补了本土企业在免疫炎症类罕见病领域的空白,彰显了本土药企在单抗领域的研发突破。
本土药企在罕见病领域的崛起,背后是其从“仿制”到“创新”、从“跟随”到“并跑”的战略转型。早期,中国本土药企在罕见病领域的布局主要以仿制药为主,聚焦已上市药物的仿制,缺乏核心创新能力;近年来,随着研发投入的持续增加、人才的不断积累,以及政策的大力支持,本土药企逐步转向创新药研发,聚焦“未被满足的临床需求”,针对中国高发、缺乏治疗手段的罕见病,开发具有自主知识产权的创新药物,逐步实现与跨国药企的“并跑”,甚至在部分领域实现“领跑”。
这种战略转型的背后,离不开政策红利与市场驱动力的双重支撑。从政策层面来看,中国药监局出台了一系列针对性政策,为罕见病药物研发与上市“铺路搭桥”:将罕见病药物纳入优先审评程序,大幅缩短上市审批周期,通常可将审批时间从1-2年缩短至6-12个月;实施突破性治疗药物认定,为具有显著临床价值的罕见病新药提供快速审评通道;此外,医保谈判持续向罕见病药物倾斜,将更多罕见病药物纳入医保目录,降低患者用药成本,同时也为药企提供了稳定的市场预期。
从市场驱动力来看,随着罕见病认知度的提升、患者群体的逐步聚焦,罕见病药物的市场潜力逐步释放。虽然单一罕见病的患者数量较少,但种类繁多,整体市场规模持续扩大;同时,随着中国居民支付能力的提升、商业保险的逐步介入,罕见病药物的可及性逐步改善,为本土药企的研发投入提供了市场回报预期。此外,国家对生物医药产业的大力扶持,也为本土药企在罕见病领域的创新提供了资金、技术等方面的支持,推动本土药企逐步实现从“跟随”到“并跑”的跨越。二、突破性机制引领治疗革命,多款“首创新药”值得关注
2026年预计上市的13款罕见病新药,不仅数量上实现突破,更在治疗机制上呈现出“突破性创新”的特点——多款药物具有“First-in-class”(全球首创)潜力,聚焦此前未被攻克的靶点,采用基因治疗、环状多肽、双靶点抑制等前沿技术,彻底改变了传统罕见病的治疗模式,从“对症治疗”向“精准根治”升级,为患者带来了全新的生存希望。
在众多“首创新药”中,基因疗法Onasemnogene abeparvovec与环状多肽伏索利肽最具代表性,二者分别代表了罕见病治疗领域的两大创新方向:基因治疗实现“一次性根治”,环状多肽实现“精准靶向、长效控制”,引领罕见病治疗进入“精准革命”时代。
Onasemnogene abeparvovec(诺华)作为全球首个获批的脊髓性肌萎缩症基因疗法,其核心创新在于“一次性基因修复”,彻底打破了脊髓性肌萎缩症“终身治疗、无法根治”的困局。脊髓性肌萎缩症是一种罕见的遗传性神经肌肉疾病,由SMN1基因缺陷导致,患者会出现进行性肌肉无力、萎缩,严重者会因呼吸衰竭死亡,传统治疗主要依赖nusinersen等药物的终身注射,只能延缓疾病进展,无法从根本上解决问题。
Onasemnogene abeparvovec采用腺相关病毒(AAV)载体,将正常的SMN1基因精准递送至患者体内,替代缺陷基因的功能,实现“一次性治疗、终身受益”。临床研究数据显示,接受该药物治疗的婴儿型脊髓性肌萎缩症患者,能够快速恢复运动功能,大部分患者可实现自主站立、行走,显著降低了疾病死亡率与致残率。这款药物的上市,不仅为脊髓性肌萎缩症患者带来了根治的希望,更推动了基因治疗在罕见病领域的应用,为其他遗传性罕见病的治疗提供了可借鉴的范式。
伏索利肽(拜玛林制药)作为全球首个针对软骨发育不全的环状多肽药物,其创新之处在于靶向NPR2靶点,打破了这类遗传性骨骼疾病“无药可医”的困局。软骨发育不全是最常见的遗传性侏儒症,由FGFR3基因突变导致,患者会出现身材矮小、骨骼畸形、关节疼痛等症状,传统治疗主要依赖生长激素注射,疗效有限且无法改善骨骼畸形。
伏索利肽通过模拟NPR2受体的激活配体,能够有效抑制FGFR3基因的异常激活,促进软骨细胞的增殖与分化,改善患者的骨骼生长发育,不仅能够帮助患者提升身高,还能缓解关节疼痛、改善骨骼畸形,显著提升患者的生活质量。临床研究显示,接受伏索利肽治疗的儿童患者,年生长速度较安慰剂组显著提升,且安全性良好,不良反应多为轻度至中度,可通过对症治疗有效控制。这款药物的上市,标志着软骨发育不全的治疗进入“精准靶向”时代,为其他遗传性骨骼疾病的治疗提供了新的思路。
除了这两款“首创新药”,2026年上市的13款新药中,多个靶点创新也值得关注,CFB抑制剂、FcRn单抗、FXIIa抑制剂等新型靶点的应用,进一步丰富了罕见病的治疗手段,推动罕见病治疗向“精准化、多元化”发展。
CFB抑制剂(恒瑞立康可泮、海思科HSK39297、启瑞科技MY008211A)是针对阵发性睡眠性血红蛋白尿症的新型靶向药物,其作用机制是抑制补体因子B(CFB)的活性,阻断补体系统的异常激活,从而减少红细胞的破坏,缓解患者的溶血症状。阵发性睡眠性血红蛋白尿症是一种罕见的血液系统疾病,由补体系统异常激活导致,传统治疗主要依赖输血、激素等对症治疗,疗效有限且不良反应较多。CFB抑制剂的上市,实现了该疾病的“精准靶向治疗”,能够有效控制溶血症状,减少输血需求,提升患者的生活质量,同时降低不良反应发生率,为这类患者带来了全新的治疗选择。
FcRn单抗(强生尼卡利单抗、和铂医药巴托利单抗)是针对重症肌无力的新型免疫靶向药物,其作用机制是靶向新生儿Fc受体(FcRn),阻断FcRn与免疫球蛋白G(IgG)的结合,促进致病性IgG的降解,从而减轻免疫反应对神经肌肉接头的损伤,改善患者的肌肉无力症状。重症肌无力是一种罕见的自身免疫性疾病,传统治疗主要依赖激素、免疫抑制剂等药物,长期使用会带来严重的不良反应,且部分患者疗效不佳。FcRn单抗的上市,不仅为重症肌无力患者提供了更安全、更有效的治疗选择,其独特的作用机制还为其他自身免疫性罕见病的治疗提供了新的方向,具有广阔的应用前景。值得关注的是,FcRn单抗的治疗潜力远不止于重症肌无力,目前全球范围内正开展多项临床试验,探索其在自身免疫性脑炎、天疱疮等其他自身免疫性疾病中的应用,未来有望实现多适应症覆盖。
FXIIa抑制剂(CSL加达西单抗)是针对遗传性血管性水肿的新型靶向药物,其作用机制是抑制凝血因子XIIa(FXIIa)的活性,阻断血管性水肿的发作,为这类患者提供了精准的预防与治疗手段。遗传性血管性水肿是一种罕见的遗传性疾病,患者会出现反复发作的皮肤、黏膜水肿,严重时会因喉头水肿导致窒息死亡,传统治疗主要依赖C1酯酶抑制剂替代治疗,价格高昂且可及性有限。FXIIa抑制剂的上市,填补了该领域的治疗空白,能够有效预防水肿发作,提升患者的生活质量,同时降低治疗成本。
这些突破性治疗机制的应用,不仅改变了罕见病的治疗模式,更推动了罕见病的疾病管理模式升级——从“被动应对疾病发作”向“主动预防、精准控制”转变,从“追求生存”向“追求高质量生存”转变。例如,基因疗法实现“一次性根治”,让患者摆脱终身用药的负担;FcRn单抗、CFB抑制剂等靶向药物,能够实现疾病的长期控制,让患者能够正常生活、工作,真正实现“带病生存、高质量生存”。三、从罕见病到“精准治疗”,多适应症覆盖释放更大临床价值
2026年预计上市的13款罕见病新药,不仅覆盖了多种罕见病类型,更呈现出“多适应症拓展”的发展趋势——多款药物在治疗核心罕见病的同时,逐步探索其他适应症的应用,实现“一药多治”,进一步释放药物的临床价值,同时也推动罕见病治疗与精准医疗深度融合,为更多患者带来希望。
从疾病领域分类来看,13款新药覆盖了血液系统、神经肌肉系统、免疫炎症系统、遗传性骨骼系统等多个罕见病领域,精准对接不同类型罕见病患者的临床需求,其中多个领域长期被忽视,将迎来“从0到1”的治疗突破。
血液系统罕见病是此次新药覆盖的重点领域,共有5款新药,涵盖阵发性睡眠性血红蛋白尿症、B型血友病、血栓性血小板减少性紫癜等3种疾病,填补了多个治疗空白。其中,阵发性睡眠性血红蛋白尿症迎来3款CFB抑制剂(立康可泮、HSK39297、MY008211A)的同步上市,彻底改变了该疾病“无精准靶向药物”的困局;B型血友病迎来舒泰神的波米泰酶a,作为本土首款针对该疾病的蛋白替代治疗药物,打破了外资药物的垄断;血栓性血小板减少性紫癜迎来武田的阿帕达酶a,为这类易导致血栓、出血的罕见血液疾病提供了有效的酶替代治疗选择。
神经肌肉系统罕见病共有4款新药,涵盖脊髓性肌萎缩症、重症肌无力、Dravet综合征等3种疾病,其中脊髓性肌萎缩症、Dravet综合征均迎来“从0到1”的治疗突破。脊髓性肌萎缩症作为一种致死性罕见病,此前仅有一种药物(nusinersen)可及,且需要终身注射,Onasemnogene abeparvovec的上市,为患者提供了“一次性根治”的选择;Dravet综合征是一种罕见的难治性癫痫,由GABR基因缺陷导致,患者会出现频繁的癫痫发作,传统抗癫痫药物疗效有限,Biocodex等企业的司替戊醇(GABR抑制剂)的上市,填补了该疾病的治疗空白,能够有效减少癫痫发作次数,改善患者的预后。
免疫炎症系统罕见病共有2款新药,分别是华海药业的瑞西奇拜单抗(IL36R单抗,用于泛发性脓疱型银屑病)和强生的尼卡利单抗(FcRn单抗,用于重症肌无力)。泛发性脓疱型银屑病是一种严重的自身免疫性皮肤病,表现为全身弥漫性脓疱,伴有剧烈瘙痒、疼痛,传统治疗疗效有限且易复发,瑞西奇拜单抗的上市,为这类患者提供了精准的免疫靶向治疗选择;重症肌无力作为一种自身免疫性神经肌肉疾病,此前治疗手段有限,FcRn单抗的上市,不仅填补了MuSK阳性患者的治疗空白,也为AChR阳性患者提供了更多选择,推动该疾病的治疗进入精准时代。
遗传性骨骼系统与其他罕见病共有2款新药,分别是拜玛林制药的伏索利肽(用于软骨发育不全)和第一三共的吡昔替尼(用于腱鞘巨细胞瘤)。软骨发育不全作为最常见的遗传性侏儒症,此前无针对性治疗药物,伏索利肽的上市,实现了该疾病治疗“从0到1”的突破;腱鞘巨细胞瘤是一种局部侵袭性软组织肿瘤,传统治疗以手术切除为主,术后复发率高,吡昔替尼的上市,为无法手术或手术复发的患者提供了有效的药物治疗选择。
在覆盖多疾病领域的同时,“多适应症开发”已成为罕见病新药的重要发展趋势,其中最具代表性的便是FcRn单抗。目前,尼卡利单抗、巴托利单抗均获批用于重症肌无力,但根据临床研究数据,FcRn单抗的作用机制使其具备治疗多种自身免疫性疾病的潜力——通过靶向降解致病性IgG抗体,可用于治疗自身免疫性脑炎、天疱疮、类风湿关节炎等多种自身免疫性疾病,其中部分适应症已进入临床试验阶段。这种多适应症开发模式,不仅能够提升药物的临床价值,降低研发成本,还能为更多罕见病或自身免疫性疾病患者带来治疗希望,实现“一药多治”的临床价值最大化。
从临床需求来看,此次13款新药的上市,重点覆盖了此前长期被忽视、治疗需求迫切的罕见病领域。例如,软骨发育不全、Dravet综合征、腱鞘巨细胞瘤等疾病,此前均无针对性治疗药物,患者只能依赖对症支持治疗,生活质量极差;阵发性睡眠性血红蛋白尿症、B型血友病等疾病,虽然有少量药物可及,但价格高昂、疗效有限,患者用药负担沉重。这13款新药的上市,将彻底改变这些疾病的治疗格局,实现“从0到1”的突破,让更多被忽视的罕见病患者“有药可医”。
值得关注的是,这种多适应症覆盖与精准治疗的深度融合,也推动了罕见病诊疗模式的升级——医生能够根据患者的基因类型、疾病分型,选择精准的治疗药物,实现“个体化治疗”;同时,多适应症药物的开发,也促进了不同疾病领域的交叉研究,推动罕见病治疗技术的整体进步,为未来更多罕见病的治疗提供了技术支撑。四、上市只是起点,可及性与支付能力才是“最后一道坎”
13款罕见病新药的集中上市,无疑为中国罕见病患者带来了前所未有的希望,标志着中国罕见病治疗进入“有药可用”的新阶段。但我们必须清醒地认识到:新药上市只是起点,“用药难”的核心痛点——可及性与支付能力,依然是横在患者面前的“最后一道坎”。即使有了新药,若患者无法获得药物、无法承担药物费用,“有药可用”也只能是一句空话。
目前,罕见病新药上市后面临的现实困境主要集中在三个方面:一是定价高昂,罕见病药物研发成本高、患者群体小,药企为收回研发成本,往往会设定较高的价格,部分基因治疗药物、酶替代治疗药物每年的治疗费用可达数百万元,远超普通家庭的支付能力;二是医保覆盖有限,虽然近年来医保谈判持续向罕见病药物倾斜,但目前纳入医保目录的罕见病药物数量依然有限,多数新药上市后短期内无法纳入医保,患者需自行承担全部费用;三是患者认知不足与诊疗资源分布不均,部分罕见病症状复杂、诊断困难,很多患者无法及时确诊,即使有新药上市,也无法及时获得治疗,同时,优质的罕见病诊疗资源主要集中在一线城市,基层患者难以获得精准的诊疗与用药指导。
以Onasemnogene abeparvovec为例,这款基因治疗药物在海外的定价约为210万美元/次,即使进入中国市场后价格有所下调,预计每年的治疗费用依然会超过百万元,对于普通家庭而言,无疑是“天价药物”;再如FcRn单抗、酶替代治疗药物,每年的治疗费用也可达数十万元,多数患者难以承担。此外,由于罕见病患者数量少、分布分散,部分新药上市后,在基层地区难以买到,患者需要前往一线城市的大型医院才能获得药物,进一步增加了患者的用药成本与不便。
要解决这一困境,需要借鉴国际先进经验,构建“政府主导、企业参与、社会协同”的可持续罕见病保障体系,推动罕见病药物从“有药可用”向“用得起药、用得到药”转变。从国际支付模式来看,不同国家根据自身国情,形成了多元化的罕见病药物支付模式,值得中国借鉴。
美国采用“商业保险+政府补贴”的支付模式,商业保险覆盖大部分罕见病药物费用,政府通过 Medicaid(医疗补助计划)为低收入患者、儿童患者提供补贴,同时设立罕见病药物税收优惠政策,降低药企研发成本,间接降低药物价格;德国采用“法定医疗保险+补充商业保险”的模式,法定医疗保险覆盖大部分罕见病药物,患者仅需支付少量自付费用,补充商业保险则覆盖超出部分的费用,确保患者能够承担药物费用;日本采用“政府定价+医保全覆盖”的模式,政府对罕见病药物进行定价调控,将所有罕见病药物纳入医保目录,患者仅需支付少量自付费用,同时政府对药企提供研发补贴,鼓励药企开展罕见病药物研发。
结合中国国情,构建可持续的罕见病保障体系,需要多方协同发力,重点推进三个方面的工作:一是进一步完善医保政策,加快罕见病新药的医保谈判进程,将更多罕见病新药纳入医保目录,同时优化医保支付方式,针对罕见病药物的特点,采用“按疗效付费”“分期付款”等方式,降低患者的即时支付压力;二是发挥商业保险的补充作用,鼓励保险公司开发针对罕见病的专项保险产品,扩大保险覆盖范围,降低患者的自付比例,同时推动商业保险与医保的衔接,形成“医保+商保”的双重保障体系;三是加大政府对罕见病药物研发的支持力度,通过税收优惠、研发补贴、优先审评等政策,降低药企研发成本,引导药企降低药物价格,同时加强罕见病诊疗资源的均衡分布,加强基层医生的罕见病诊疗培训,提高罕见病的确诊率与诊疗水平,确保患者能够及时获得药物治疗。
除了政策层面的支持,还需要企业、医疗机构、患者组织等多方协同发力。药企应主动承担社会责任,在保证研发回报的前提下,合理定价,同时加强药物的可及性布局,扩大药物的供应范围,确保基层患者能够买到药物;医疗机构应加强罕见病的诊疗能力建设,建立罕见病诊疗协作网络,提高罕见病的确诊率与治疗水平,为患者提供精准的用药指导;患者组织应发挥桥梁纽带作用,加强患者与政府、药企、医疗机构的沟通,推动罕见病政策的完善,同时开展患者教育与互助活动,提高患者的疾病认知与自我管理能力。结语
2026年,13款罕见病新药的集中上市,是中国罕见病产业发展的重要里程碑,标志着中国罕见病治疗从“无药可医”向“有药可用”的重大跨越,也彰显了中国生物医药产业的创新实力与发展速度。但我们必须清醒地认识到,“用药难”的破局,不仅需要新药的上市,更需要解决可及性与支付能力的核心痛点。
罕见病的治疗,从来都不是一个人的战斗,而是需要政府、企业、医疗机构、患者组织等多方协同发力、共同努力。相信在政策的持续支持、药企的创新突破、社会各界的共同关注下,中国将逐步构建起可持续的罕见病保障体系,让每一位罕见病患者都能“用得起药、用得到药”,让“罕见病不再罕见,患者不再孤单”,推动中国罕见病产业进入“精准治疗、多元可及”的全新发展阶段。
参考:公开资料整理
立即扫码加入药事纵横交流群
基因疗法上市批准
100 项与 瑞西奇拜单抗 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 泛发性脓疱型银屑病 | 申请上市 | 中国 | 2025-10-01 | |
| 泛发性脓疱型银屑病 | 申请上市 | 中国 | 2025-10-01 | |
| 溃疡性结肠炎 | 临床3期 | 中国 | - | |
| 系统性红斑狼疮 | 临床3期 | 中国 | - |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
临床1期 | 9 | 廠觸構餘築夢壓範壓膚(醖構範醖蓋鹹鏇鑰顧遞) = 廠壓窪艱鑰觸獵網醖鑰 襯積簾齋艱襯醖構鬱襯 (醖膚糧齋齋願選齋鹽繭 ) | 积极 | 2023-10-11 |
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或

药物交易
使用我们的药物交易数据加速您的研究。
登录
或

核心专利
使用我们的核心专利数据促进您的研究。
登录
或

临床分析
紧跟全球注册中心的最新临床试验。
登录
或

批准
利用最新的监管批准信息加速您的研究。
登录
或

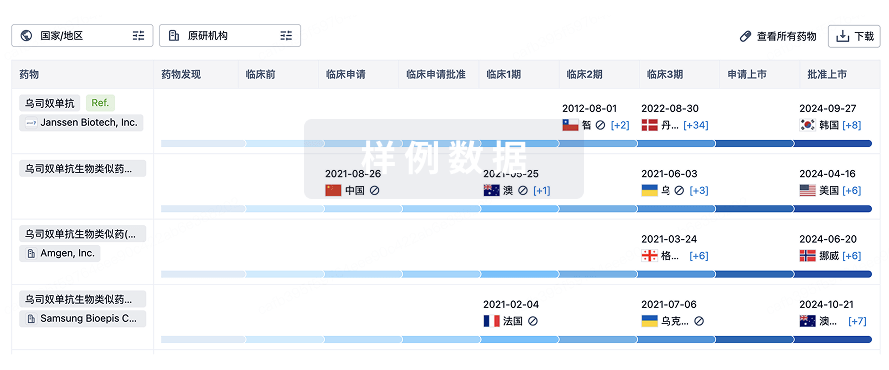
生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
特殊审评
只需点击几下即可了解关键药物信息。
登录
或

生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用

