预约演示
更新于:2025-05-07
Krukenberg Tumor
Krukenberg瘤
更新于:2025-05-07
基本信息
别名 Cancer metastatic to ovary、Carcinoma, Krukenberg、Krukenberg Carcinoma + [36] |
简介 Mucocellular carcinoma of the ovary, usually metastatic from the gastrointestinal tract, characterized by areas of mucoid degeneration and the presence of signet-ring-like cells. It accounts for 30%-40% of metastatic cancers to the ovaries and possibly 1%-2% of all malignant ovarian tumors. The lesions may not be discovered until the primary disease is advanced, and most patients die of their disease within a year. In some cases, a primary tumor is not found. (From Dorland, 27th ed; Holland et al., Cancer Medicine, 3d ed, p1685) |
关联
6
项与 Krukenberg瘤 相关的药物靶点 |
作用机制 微管蛋白抑制剂 |
在研机构 |
非在研适应症 |
最高研发阶段申请上市 |
首次获批国家/地区- |
首次获批日期1800-01-20 |
靶点 |
作用机制 fascin抑制剂 |
最高研发阶段临床1/2期 |
首次获批国家/地区- |
首次获批日期1800-01-20 |
作用机制 DNA嵌入剂 [+1] |
非在研适应症 |
最高研发阶段临床1/2期 |
首次获批国家/地区- |
首次获批日期1800-01-20 |
6
项与 Krukenberg瘤 相关的临床试验NCT06914687
Tirellizumab Combined With SOX and Hyperthermic Intraperitoneal Chemotherapy (HIPEC) in the Treatment of Peritoneal Metastatic Gastric/Gastroesophageal Junction Adenocarcinoma: A Single-arm, Phase II Clinical Trial (Solids-03)
For peritoneal metastatic gastric/gastroesophageal junction adenocarcinoma (cT3-4NanyM1), PD-1 antibody combined with chemotherapy and hyperthermic intraperitoneal chemotherapy (HIPEC) can downstage tumor stage, increase the conversion resection rate, and may improve the long-term survival. Tislelizumab, an anti-PD-1 antibody, has recently been proved in the first- and second-line standard treatment for advanced or metastatic gastric or gastro-oesophageal junction adenocarcinoma.In the subgroup analysis of RATIONALE-305 trial, tislelizumab also showed good efficacy in gastric/gastroesophageal junction adenocarcinoma patients with peritoneal metastasis. Combination of tirellizumab,SOX and HIPEC for peritoneal metastatic gastric/gastroesophageal junction adenocarcinoma could be a novel therapeutic strategy to increase response rate and therapeutic efficacy. This study is a monocenter, single-arm phase 2 clinical trial to evaluate tolerability, safety and efficacy of perioperative tirellizumab in combination with SOX and HIPEC in peritoneal metastatic gastric/gastroesophageal junction adenocarcinoma.
开始日期2025-03-30 |
申办/合作机构 |
NCT05143970
A Phase 1 First-In-Human Study of the Anti-CD73 IPH5301 Alone or in Combination With Chemotherapy and Trastuzumab in Patients With Advanced Solid Tumors
CHANCES-IPC 2021-008 is First In Human, Phase I, multicenter, European study evaluating an anti-CD73, IPH5301 in advanced and/or metastatic cancer.
The trial will be conducted in two parts, Part I- Dose escalation: This part aims to identify the maximum tolerated dose (MTD) of IPH5301 agent in monotherapy and recommended phase 2 dose (RP2D) for future trials, followed by a safety expansion study part cohort.
Part II- Expansion cohort: A total of 12 HER2+ cancer patients, respectively 6 breast cancer patients and 6 gastric cancer patients, is planned to be enrolled into the next expansion cohort to select a recommended dose of IPH5301 to be administered in combination with chemotherapy and trastuzumab for evaluation in future trials with selected advanced solid tumors.
The trial will be conducted in two parts, Part I- Dose escalation: This part aims to identify the maximum tolerated dose (MTD) of IPH5301 agent in monotherapy and recommended phase 2 dose (RP2D) for future trials, followed by a safety expansion study part cohort.
Part II- Expansion cohort: A total of 12 HER2+ cancer patients, respectively 6 breast cancer patients and 6 gastric cancer patients, is planned to be enrolled into the next expansion cohort to select a recommended dose of IPH5301 to be administered in combination with chemotherapy and trastuzumab for evaluation in future trials with selected advanced solid tumors.
开始日期2022-01-21 |
申办/合作机构 |
NCT05001282
Dose Escalation and Expansion Clinical Study to Evaluate the Safety and Efficacy of ELU001 in Subjects Who Have Advanced, Recurrent or Refractory FRα Overexpressing Tumors
This study, ELU- FRα-1, was focused on adult subjects who have advanced, recurrent or refractory folate receptor alpha (FRα) overexpressing tumors considered to be topoisomerase 1 inhibitor-sensitive based on scientific literature, and, in the opinion of the Investigator, have no other meaningful life-prolonging therapy options available.
开始日期2021-09-13 |
申办/合作机构 |
100 项与 Krukenberg瘤 相关的临床结果
登录后查看更多信息
100 项与 Krukenberg瘤 相关的转化医学
登录后查看更多信息
0 项与 Krukenberg瘤 相关的专利(医药)
登录后查看更多信息
1,096
项与 Krukenberg瘤 相关的文献(医药)2025-05-01·European Journal of Surgical Oncology
Efficacy and safety of subtotal pelvic peritonectomy for colorectal cancer patients with peritoneal metastasis confined to the pelvic cavity
Article
作者: Tang, Jinghua ; Pan, Zhizhong ; Xiao, Binyi ; Liao, Leen ; Ding, Peirong ; Jiang, Wu ; Han, Kai ; Kong, Lingheng ; Zheng, Muxu ; Sui, Qiaoqi
2025-04-01·Radiology Case Reports
Krukenberg tumor secondary to gallbladder adenocarcinoma: A case report
Article
作者: Ibenyahya, Abderrahmane ; Bazi, Imane ; Saalaoui, Abir ; Wakrim, Soukaina ; Bigi, Soufiane ; Chahbi, Zakaria ; Adnor, Said ; Elagouri, Hajar
2025-04-01·Radiology Case Reports
Unexpected encounters: The surprising link between ovarian cancer and axillary lymphadenopathy
Article
作者: Guglielmi, Giuseppe ; Carpagnano, Francesca Anna ; Balbino, Marina ; Montatore, Manuela ; Masino, Federica
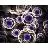
分析
对领域进行一次全面的分析。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用