预约演示
更新于:2026-05-19
Alemtuzumab
阿仑单抗
更新于:2026-05-19
概要
基本信息
药物类型 单克隆抗体 |
别名 Alemtuzumab (Genetical Recombination)、Alemtuzumab (genetical recombination) (JAN)、Alemtuzumab (USAN/INN) + [15] |
靶点 |
作用方式 抑制剂 |
作用机制 CD52抑制剂(CAMPATH-1抗原抑制剂)、ADCC(抗体依赖的细胞毒作用)、补体依赖的细胞毒性作用 |
在研适应症 |
非在研适应症 |
原研机构 |
在研机构 |
权益机构 |
最高研发阶段批准上市 |
最高研发阶段(中国)- |
特殊审评孤儿药 (美国)、孤儿药 (日本)、孤儿药 (韩国)、临床急需境外新药 (中国) |
登录后查看时间轴
结构/序列
Sequence Code 53002L

来源: *****
Sequence Code 53009H

来源: *****
关联
342
项与 阿仑单抗 相关的临床试验NCT06084780
Prospective Case Series of Intestinal and Multivisceral Transplantation for Unresectable Mucinous Carcinoma Peritonei (TRANSCAPE)
The goal of this prospective phase 2 study is to assess the efficacy and safety of intestinal or multivisceral transplantation for participants with PMP not amenable to other curative-intent treatments. Participants will undergo intestinal/multivisceral transplantation. Participants will be followed for 12 months to assess efficacy and safety.
开始日期2026-08-01 |
NCT07214064
Safety and Feasibility of a Venetoclax- Augmented Treosulfan-Based Reduced Intensity Conditioning Before Allogeneic Stem Cell Transplantation in AML, MDS/AML and Higher Risk MDS
Safety and Feasibility of a Venetoclax- Augmented Treosulfan-Based Reduced Intensity Conditioning Before Allogeneic Stem Cell Transplantation in AML, MDS/AML and Higher Risk MDS
开始日期2026-01-01 |
申办/合作机构- |
NCT06959771
Base Editing Hematopoietic Stem Cell and BE T Cell Gene Therapy for CD40L-HyperIgM Syndrome-Single Patient Study
Background:
X-linked hyper-IgM (HIGM) syndrome is caused by a mutation in the CD40 ligand (CD40L) gene. People with this disease have white blood cells that do not work properly. These people are at risk of severe infections and autoimmune diseases. Researchers want to know if these base-edited stem cells and T cells can help people with CD40L-HIGM syndrome.
Objective:
To test base-edited stem cells and base-edited T cells in 1 person with CD40L-HIGM syndrome.
Eligibility:
A single male with CD40L-HIGM syndrome.
Design:
A single participant is planned to receive a single dose of edited stem cells and supportive treatment with edited T cells. Participant stem and T cells will undergo base editing to repair the mutation.
In preparation for the gene therapy, the participant will receive busulfan chemotherapy and alemtuzumab. After treatment, the participant will have follow-up visits every few months in the first 2 years after treatment. Long-term visits will continue annually for 15 years.
X-linked hyper-IgM (HIGM) syndrome is caused by a mutation in the CD40 ligand (CD40L) gene. People with this disease have white blood cells that do not work properly. These people are at risk of severe infections and autoimmune diseases. Researchers want to know if these base-edited stem cells and T cells can help people with CD40L-HIGM syndrome.
Objective:
To test base-edited stem cells and base-edited T cells in 1 person with CD40L-HIGM syndrome.
Eligibility:
A single male with CD40L-HIGM syndrome.
Design:
A single participant is planned to receive a single dose of edited stem cells and supportive treatment with edited T cells. Participant stem and T cells will undergo base editing to repair the mutation.
In preparation for the gene therapy, the participant will receive busulfan chemotherapy and alemtuzumab. After treatment, the participant will have follow-up visits every few months in the first 2 years after treatment. Long-term visits will continue annually for 15 years.
开始日期2025-07-16 |
100 项与 阿仑单抗 相关的临床结果
登录后查看更多信息
100 项与 阿仑单抗 相关的转化医学
登录后查看更多信息
100 项与 阿仑单抗 相关的专利(医药)
登录后查看更多信息
2,657
项与 阿仑单抗 相关的文献(医药)2026-06-01·CURRENT OPINION IN NEUROLOGY
Cellular immunophenotyping in multiple sclerosis: advances and clinical implications
Review
作者: Möllenkamp, Thiemo M ; Müller-Miny, Louisa ; Meyer Zu Hörste, Gerd
Purpose of review:
Multiple sclerosis is a clinically heterogeneous disease that is driven by complex immune mechanisms. This review summarizes recent methodological advances in immunophenotyping and discusses clinical implications for diagnosis, prognosis, therapy selection, and monitoring.
Recent findings:
Methodological advances like high-dimensional flow cytometry and single-cell technologies aim to define Multiple sclerosis immunological endophenotypes associated with different disease trajectories. Novel spectral flow and mass cytometry panels reveal distinct immune cell subsets. Myeloid cell populations have been identified in aggressive disease variants and tissue-resident T cells in cerebrospinal fluid. Clinically, baseline immune signatures aim to predict disease progression and treatment response. Patients with a highly inflammatory immune profile have been found to exhibit more rapid progression and to be prone to treatment failure. Immunophenotyping may therefore guide treatment, from identifying those at risk of Alemtuzumab-induced autoimmunity to monitoring B-cell repopulation for personalized dosing schedules.
Summary:
Immunophenotyping enables increasingly precise characterization of Multiple sclerosis immuno-pathogenesis. While not yet routine, these tools show promise for improving differential diagnosis, individualizing therapy initiation and monitoring. Ongoing research and standardization are paving the way towards precision immunology-approaches in clinical practice.
2026-05-01·AUTOIMMUNITY REVIEWS
Anti-CD52 therapy of rheumatic diseases: Revisited in the era of immune reset
Review
作者: Isaacs, John D ; Naffaa, Mohammad E ; Hassan, Fadi
Alemtuzumab is a humanized monoclonal antibody targeting CD52, a glycosylphosphatidylinositol-anchored surface antigen broadly expressed on lymphocytes and other immune cells. Although currently approved for multiple sclerosis and used in selected transplantation settings, alemtuzumab was among the earliest lymphocyte-depleting biologics explored across a wide spectrum of autoimmune rheumatic diseases. With renewed interest in deep immune-depleting strategies, including CAR-T cells and bispecific T-cell engagers, revisiting the immunobiology and clinical experience of alemtuzumab is timely. This review summarizes current knowledge of CD52 structure, expression, and immunological function, highlighting its dual role as both a co-stimulatory and immunoregulatory molecule. We examine the mechanisms underlying alemtuzumab-induced lymphocyte depletion, subsequent immune reconstitution, and the paradoxical development of secondary autoimmunity. Clinical evidence for alemtuzumab use in rheumatic diseases, including rheumatoid arthritis, systemic lupus erythematosus, systemic sclerosis, vasculitis, idiopathic inflammatory myopathies, ocular inflammatory disease, and Behçet's syndrome, is reviewed, with emphasis on efficacy, durability of response, and safety outcomes. Across multiple refractory disease settings, alemtuzumab has demonstrated the capacity to induce rapid clinical improvement and, in some cases, prolonged drug-free remission. However, treatment is limited by risks of infection, delayed immune reconstitution, and immune dysregulation. We conclude that alemtuzumab remains a potent immunomodulatory option in selected refractory rheumatic diseases, provided that careful patient selection, cautious monitoring, and long-term follow-up are implemented.
2026-05-01·Multiple Sclerosis and Related Disorders
Appendicitis and multiple sclerosis disease-modifying therapies: a disproportionality analysis of the FDA adverse event reporting system
Article
作者: Balshi, Alexandra ; Baber, Ursela ; Esser, Madelyn ; Dempsey, John P ; Sloane, Jacob A
BACKGROUND:
Although appendicitis is one of the most common surgical emergencies and is related to immune function, its relation to multiple sclerosis (MS) disease-modifying therapies (DMTs) is unclear.
OBJECTIVE:
To determine which, if any, MS DMTs are associated with disproportionally high appendicitis reporting using real-world data from the FDA Adverse Event Reporting System (FAERS).
RESULTS:
We identified 965 reports of appendicitis associated with MS DMTs. A pooled analysis of all DMTs showed disproportionately high appendicitis reporting compared to all other FAERS medications (reporting odds ratio, 2.83; 95% confidence interval, 2.63-3.06; χ (Bhangu et al., 2015), 787.54). Ocrelizumab, ofatumumab, natalizumab, alemtuzumab, dimethyl and diroximel fumarate, cladribine, and peg- and interferon beta-1a all individually exhibited disproportionally high appendicitis reporting.
CONCLUSION:
Patient counseling on early appendicitis warning signs and indications for urgent evaluation may be warranted for people with MS on DMTs.
173
项与 阿仑单抗 相关的新闻(医药)2026-05-13
肌电图帮助定位,无法定性
神经体格检查提示:肌力下降,运动、感觉功能均明显受影响。
周围神经病变诊断思路
实际病例诊断思路
Neuroepidemiology (2019) 52 (3-4): 161–172.
https://doi.org/10.1159/000494291
PubMed:30669140
《慢性炎性脱髓鞘性多发性神经根神经病诊治中国专家共识2022》
临床特点
经典型CIDP:最常见,表现为对称性上下肢近端和远端无力,并伴有肢体远端不同程度感觉异常,下肢重于上肢。所有肢体腱反射均减弱或消失。
CIDP的分型
CIDP的诊断标准
1.周围神经病变自发生至达到高峰的时间至少8周,可表现为慢性进展或缓解复发。2.符合CIDP临床表现,并且电生理证实至少在两根神经存在脱髓鞘的证据,并排除其他原因导致的脱髓鞘周围神经病。
3.符合CIDP临床表现,但电生理证实仅有一根神经存在脱髓鞘证据时,如果免疫治疗(IVIg、血浆置换或糖皮质激素)有效,周围神经影像学发现神经明显增粗,脑脊液蛋白细胞分离,神经活检,四项中有一项符合CIDP表现,并排除其他原因导致的脱髓鞘性周围神经病,可诊断CIDP。
慢性炎性脱髓鞘性多发性神经根神经病的诊疗流程(图13-1)
CIDP的脑脊液表现
CIDP的腓肠神经病理学检查
辅助检查
1.肌电图 CIDP是一种脱髓鞘性周围神经病,肌电图是诊断CIDP最重要的辅助方法,是确定CIDP诊断的必需条件,主要用于提供脱髓鞘病变的证据。脱髓鞘的证据主要依靠运动神经传导、F波和感觉神经传导测定。
判断周围神经脱髓鞘时,主要依据运动神经传导测定,电生理参数包括:运动远端潜伏期延长、运动传导速度下降、F潜伏期延长/F波出现率下降、运动传导阻滞、异常波形离散以及远端复合肌肉动作电位(compound muscle action potential, CMAP)负向波时限增宽。
CIDP的感觉传导异常可表现感觉传导速度下降,感觉神经动作电位波幅下降,在CIDP可以出现正中神经或桡神经感觉传导异常,而腓肠神经感觉传导正常的现象。除了纯感觉型CIDP外,在诊断其他类型CIDP时,均要求至少在两根运动神经存在肯定脱髓鞘病变的证据;除了纯运动型CIDP外,至少应有两根感觉神经存在传导异常。
诊断感觉型CIDP时,至少要求两根神经在非嵌压部位感觉传导速度明显减慢,而运动传导完全正常。
2.脑脊液检测 CIDP患者脑脊液检查可见白细胞数正常范围,蛋白增高,即蛋白细胞分离现象。在部分CIDP患者,脑脊液蛋白可以正常。如果临床和电生理检测能够诊断CIDP,可不必进行脑脊液检测。
在下述情况时,可以考虑进行脑脊液检测来辅助CIDP诊断和鉴别诊断:当电生理检测仅在一根神经发现脱髓鞘证据时,脑脊液蛋白细胞分离可以作为诊断的支持依据;当患者急性或亚急性起病,怀疑有感染或恶性肿瘤,应行脑脊液检测协助鉴别诊断。蛋白细胞分离现象并非CIDP特异性改变,可见于多种临床情况。
当电生理检查缺乏明确的脱髓鞘证据时,仅仅有脑脊液蛋白的增高,诊断CIDP需慎重,如腰椎管狭窄患者,可有蛋白增高,糖尿病或其他原因导致的周围神经病也可见蛋白增高现象,常会误诊为CIDP,而进行不必要的免疫治疗。在50岁以上患者,脑脊液正常值较年轻的患者增高,目前尚缺乏诊断CIDP的蛋白升高的界值。腰穿的另一个主要价值在于鉴别其他疾病,如是否存在感染或恶性肿瘤浸润导致的白细胞增高。
3.影像学表现 CIDP的周围神经超声可表现为周围神经横截面积增粗,神经束信号异常,如果在非嵌压部位,出现周围神经节段性的明显增粗,更有支持价值;同一患者不同神经的表现可有明显差异,可见正常神经与增粗神经并存。少数患者周围神经超声检测神经横截面积可均在正常范围。CIDP周围神经形态的改变特点,可能与检测时患者的病程、病情严重程度、治疗与否、潜在发病机制有关。
在CIDP患者磁共振检测可见神经根有增粗,或T2序列高信号,神经根或神经干的定量检测或半定量评分较定性判断更有价值。当电生理检测证实至少2根神经存在脱髓鞘证据时,不必进行周围神经超声或磁共振检测;当电生理检测仅发现一根神经存在脱髓鞘证据时,如果在正中神经、尺神经或臂丛,至少两个部位有神经增粗,可支持CIDP的诊断。
4.腓肠神经病理检查 CIDP主要病理改变为有髓神经纤维出现节段性脱髓鞘,轴索变性,雪旺氏细胞增生并形成洋葱球样结构,单核细胞浸润等。在CIDP的诊断过程中,不建议常规进行周围神经活检,只有在某些特定临床情况下,有必要时,根据情况选择,比如,在高度疑诊CIDP的患者,临床、电生理、影像学和脑脊液检查均仍不能确定诊断时;或疑诊CIDP,但免疫治疗无效,或还需要与其他疾病鉴别,如遗传性运动感觉神经病、淀粉样变性、血管炎、结节病、神经鞘瘤/神经纤维瘤等。
5.其他化验 CIDP缺乏特异性的诊断指标,化验检查一方面主要用于鉴别其他疾病,另一方面为免疫治疗方案的选择和监测不良反应提供依据。
(1)单克隆球蛋白(M蛋白)检测:对于临床疑诊CIDP的成年患者应常规进行M蛋白检测,包括血清蛋白电泳和免疫固定电泳,尿免疫固定电泳以及轻链的检测。在远端型CIDP,如果检测到IgM型M蛋白,应进一步检测抗髓鞘相关糖蛋白(myelin-associated glycoprotein, MAG)抗体,如果二者均阴性,可考虑重复检测。由于M蛋白在50岁以上健康人群可达1%~3.2%,70岁以上人群可达5%,不同类型的M蛋白相关周围神经病的表现不同,因此在发现M蛋白阳性时,要注意识别其与周围神经病究竟是伴随关系还是因果关系。
(2)郎飞氏结和结旁抗体检测:对于临床疑诊CIDP的患者,应考虑抗郎飞氏结和结旁抗体检测。对于存在以下特点者,建议进行相关抗体的检测:IVIG和糖皮质激素治疗效果不佳者;急性或亚急性起病、曾诊断为GBS或急性起病的CIDP(acute onset-CIDP,A-CIDP)者;有低频震颤、明显共济失调或明显远端为主无力者;呼吸衰竭和有脑神经受累者;有肾病综合征者;脑脊液蛋白特别高者。抗NF155、抗CNTN1、抗Caspr1以及抗NF140/186抗体的检测,应选择标准化的检测方法,并保证其质量控制。
(3)其他化验检查与鉴别诊断:多种周围神经病在电生理检查时可见明确或可疑的髓鞘病变,需要与CIDP鉴别。根据临床具体情况,可选择不同的检测项目,如血沉,C反应蛋白,抗核抗体、抗中性粒细胞胞浆抗体、抗神经节苷脂抗体、肌酶、维生素B12和B6、副肿瘤抗体、Lyme抗体、HIV、骨穿、胸部X线,基因检测等。治疗前应常规进行血尿常规、肝肾功能和血糖、骨密度等,用于监测治疗药物的不良反应。
鉴别诊断
多种其他疾病也可以出现髓鞘病变,如遗传压迫易感性周围神经病、Charcot-Mari-Tooth1型、POEMS综合征等,因此在电生理符合脱髓鞘诊断的情况时,在临床实践中,仍需结合临床进行鉴别诊断。
1.吉兰-巴雷综合征 A-CIDP在早期通常难以与GBS鉴别,有13%的CIDP患者4周内可类似GBS,5%的GBS患者后来诊断为CIDP。如果IVIg治疗后好转,但复发3次或以上的GBS,则应为CIDP,而非复发性GBS。与GBS不同,CIDP脑神经、呼吸肌、自主神经通常不受累。尽管有上述鉴别线索,在实际的临床工作中,发病4周内,其实很难准确地识别出究竟是GBS,还是A-CIDP,临床通常会采用IVIg治疗。A-CIDP患者,在IVIg治疗1~2个月后,通常会再次加重。在临床诊断的某些GBS患者,由于经济因素影响,无法接受IVIg治疗,而给予了糖皮质激素,临床也有好转,可能与这一组疾病有关。
2.M蛋白血症 相关周围神经病POEMS综合征早期,临床、电生理和脑脊液表现均可类似CIDP,部分患者早期糖皮质激素治疗可略有改善,但维持治疗时,会出现复发持续进展。M蛋白检测有助于二者的识别。当出现皮肤变黑、肢体明显水肿时,可提示POEMS综合征,POEMS综合征的电生理改变传导速度减慢较为均一,近端为主,通常无传导阻滞和异常波形离散,周围神经超声神经增粗程度轻微,通常无局灶性神经增粗。在远端型CIDP患者中,约2/3伴有IgM型单克隆球蛋白,其中部分患者有抗MAG抗体阳性,而MAG抗体阳性者大部分患者发病机制、病理和治疗反应等多个方面均与CIDP不同。
3.抗郎飞氏结和结旁抗体相关周围神经病 也称免疫性郎飞氏结病,其临床、电生理和脑脊液改变与CIDP相似,但可血清中检测到抗CNTN1抗体、NF155抗体、Caspr1抗体或NF140/186抗体。不同抗体的临床表现有所不同,电生理检查通常可以达到CIDP的脱髓鞘病变诊断标准,以前一直归类为CIDP的亚型,在早期研究中,这组患者也通常是从临床表现为CIDP的难治性患者中通过抗体检测而筛查出来。但目前认为,这组疾病不同于CIDP,不同抗体相关的疾病各有其相对独特的临床表现,病理学上均无明显的炎症或巨噬细胞介导的脱髓鞘病变,对IVIg反应差,因此将其从CIDP中分离出来,作为相对独立的一组疾病。该组疾病可选择糖皮质激素治疗,如效果不佳,可考虑利妥昔单抗治疗。
4.遗传性周围神经病 如CMT1A,CMTX,CMT4C等,临床均表现为慢性感觉运动性周围神经病,临床进展非常缓慢,脑脊液可有蛋白细胞分离现象,神经传导测定可见传导速度减慢、远端潜伏期延长等髓鞘病变的特点,但一般无传导阻滞和明显的异常波形离散,患者常有家族史、弓形足等提示遗传性疾病的线索。另外在脑白质营养不良相关疾病、遗传代谢性疾病中,也有少数以周围神经病变为主要表现者,电生理表现为髓鞘病变的特点,需要注意鉴别。
5.中毒性周围神经病 如正己烷中毒,某些生物制剂也可出现类似CIDP的不良反应,如免疫检查点抑制剂。临床表现为多发性感觉运动性周围神经病,电生理表现为脱髓鞘改变的特点,脑脊液可有蛋白细胞分离现象,早期可误诊为吉兰-巴雷综合征,随病情迁延发展,常需要与CIDP进行鉴别,发病前用药史以及流行病学史对于诊断最为重要。
6.系统性疾病伴随脱髓鞘性周围神经病 副肿瘤综合征、淋巴瘤相关周围神经病、HIV感染、少数结缔组织病等均可出现类似CIDP的表现,可根据患者具体情况进行筛查鉴别。
7.多灶性运动神经病 为纯运动型周围神经病,早期为多发单神经病,随病情进展,可呈现类似多发性周围神经病表现。电生理检测可见传导阻滞,需要与CIDP变异型中的多灶性、局灶性以及纯运动型CIDP鉴别。前二者均有感觉纤维的受累,纯运动型CIDP则下肢起病多见,相对对称起病。MMN采用IVIg治疗有效,但对糖皮质激素治疗反应不佳,甚至加重。
8.其他 在局灶性或多灶性CIDP还需要与多种其他原因导致的臂丛或腰骶丛病变、多发单神经病鉴别,如周围神经肿瘤、压迫易感性周围神经病、淀粉样变性周围神经病、结缔组织病相关周围神经病等。纯感觉性CIDP需要与多种药物、副肿瘤综合征、结缔组织病等相关周围神经病鉴别。
治疗
CIDP的治疗包括免疫治疗、对症治疗、营养神经治疗和康复治疗。
1.免疫治疗药物 CIDP的一线治疗包括糖皮质激素和IVIg,血浆置换也是一线治疗方案之一。在长期维持治疗时,前二者是更为优先的选择。血浆置换主要用于糖皮质激素和IVIg效果不佳或病情急性加重时。临床上大约80%的患者一线治疗药物有效。运动型CIDP对于激素反应通常较差,部分患者甚至病情加重,而IVIg治疗有效。
(1)糖皮质激素治疗方案:有多种,临床以口服方案最为常用,泼尼松1mg/(kg·d)或每日60mg开始,维持4周,之后缓慢逐渐减量,根据临床好转情况,每2~4周减5~10mg。
糖皮质激素治疗效果的判断通常需要3个月的时间。治疗有效时,可在6个月左右减量至每日20mg或以下维持,在病情稳定的患者,早期每半年或1年评估是否可以进一步减量或停药,长期维持者可1~2年评估一次。在病情较重者,可以选择甲泼尼龙冲击治疗,如甲基强的松龙500~1000mg/di.v.gtt.,连续3~5天之后改为口服维持;也有选择定期甲泼尼龙冲击治疗方案,目前并无充分证据表明哪一种方案更有效或副作用更小。
治疗过程中,注意补钾补钙保护胃黏膜治疗,定期检查血常规、肝肾功能、血糖、血压,早期每1~2周一次,长期维持者可3~6个月一次,骨密度检测可6个月一次。
(2)IVIg治疗方案:400mg/(kg·d),每天1次,静脉滴注,连续3~5天。通常在用药3~4周时达到最佳效果,之后需要定期维持。
目前尚缺乏统一的维持方案,可根据患者用药后无力的变化,个体化定期使用,如每1~2个月输注一次,每次3~5天。
IVIg的效果通常在使用后3周之内即可看到效果。如果第一次IVIg治疗无效,可再次给予足量治疗一次,如仍无效,可判断无效,在15%的患者第二次治疗后可有缓解。
(3)血浆置换(plasma exchange, PE)治疗方案:每次血浆交换量为30~50ml/kg,在1~2周内进行3~5次。根据情况可间隔1~2个月定期使用。需要注意的是,在应用IVIg后3周内,不宜进行PE治疗。PE的禁忌证主要是严重感染、心律失常、心功能不全、凝血系统疾病等;其副作用为血流动力学改变,可能造成血压变化、心律失常,使用中心导管可引发气胸和出血以及可能合并败血症。
如一线治疗无效、激素无法耐受,或激素依赖(如泼尼松减量至每日20mg时即复发)等情况时,可考虑使用免疫抑制剂,常用药物包括硫唑嘌呤、吗替麦考酚酯和环孢素。硫唑嘌呤用法为2~3mg/(kg·d),分2~3次口服;环孢素:3~6mg/(kg·d),分2~3次口服。吗替麦考酚酯:2~3g/d,分2~3次口服。有研究显示,硫嘌呤甲基转移酶活性或基因检测可预测其骨髓和肝脏毒性害,指导硫唑嘌呤的使用,避免严重不良反应。
当这三个药物无效时,可考虑使用环磷酰胺或利妥昔单抗。环磷酰胺:可200~400mg每2周一次,静脉注射,或口服50mg每日两次。利妥昔单抗100~600mg,每周一次,静脉输液,共4周,半年后根据情况再用。
尽管免疫抑制剂治疗仍缺乏充分的循证依据,但部分研究仍提示可以选择为减少一线药物治疗剂量的辅助用药。目前尚缺乏生物学指标,用于指导不同免疫抑制剂的选择,也无法判断哪一种免疫抑制剂对某一患者更为有效或无效。
目前有关于CIDP的多项临床试验正在开展,效果有待证实。艾加莫德皮下注射制剂治疗CIDP的临床试验显示,该药可改善CIDP的多项临床功能评分,维持治疗可降低CIDP复发风险,已在部分国家被批准用于CIDP的治疗。
不推荐甲氨蝶呤、β-1a干扰素、芬戈莫德用于CIDP的治疗,在获得更多临床证据前,不建议常规使用他克莫司、α干扰素,以及其他单抗类,如阿仑单抗、那他珠单抗,以及硼替佐米、益赛普、氨基吡啶、氟达拉滨、阿巴西普、免疫吸附。
免疫药物的选择和维持方案,需要注意个体化。如对于有生育需求、妊娠或哺乳期的女性CIDP患者,慎用免疫抑制剂,因病情需要必需使用时,可以选择硫唑嘌呤、环孢素、糖皮质激素和IVIg。吗替麦考酚酯、环磷酰胺和利妥昔单抗均增加致畸风险,应至少停药6个月再怀孕。
注意监测,预防免疫抑制导致的机会性感染等并发症。
2.对症治疗及神经营养治疗 少数CIDP患者可有神经痛,可使用加巴喷丁、普瑞巴林、阿米替林等。尽管缺乏循证证据,临床常给予VitB1、复合维生素B和B12等营养神经治疗。
3.功能锻炼及康复 运动和感觉受累所导致的残疾,可以通过功能训练逐渐恢复,足部支具有助于改善患者行走的稳定性和步态,健康积极的生活态度和生活方式等有益于CIDP患者功能的恢复。
2026-05-12
NEW YORK, May 12, 2026 (GLOBE NEWSWIRE) -- Cellectis (the “Company”) (Euronext Growth: ALCLS - NASDAQ: CLLS), a clinical-stage biotechnology company using its pioneering gene editing platform to develop life-saving cell and gene therapies, today announced upcoming presentations on the BALLI-01 and NATHALI-01 clinical trials, at the European Hematology Association (EHA) annual congress, on June 11-14, 2026, in Stockholm, Sweden.
Lasme-cel – Oral Presentation
The abstract reporting the full Phase 1 dataset from the BALLI-01 clinical trial evaluating lasme-cel, a CD22 directed allogeneic CAR-T, in heavily pretreated patients with relapsed or refractory CD22+ B-cell acute lymphoblastic leukemia (r/r B-ALL), has been selected for oral presentation.
These data, which will be presented by Nitin Jain, M.D., Professor of Medicine, Department of Leukemia at MD Anderson Cancer Center in Houston (TX), highlight the promising safety pro response rates in patients who have relapsed following multiple prior targeted therapies including autologous CD19 CAR-T. They form the basis for the pivotal Phase 2 program which is currently recruiting in Europe and North America.
"We are delighted to present these important data at EHA. The patients in the BALLI-01 trial had largely exhausted treatment options and faced a very poor prognosis. The depth of response we observed offers hope for these patients and demonstrates the potential for lasme-cel to become an effective therapeutic option for those with the highest unmet need. We are pursuing our pivotal Phase 2 program and plan to share the first interim analysis later this year," said Adrian Kilcoyne, M.D., MPH, MBA, Chief Medical Officer at Cellectis.
The BALLI-01 trial is currently recruiting in Pivotal Phase 2 with interim data expected to be disclosed in Q4 2026.
Oral Presentation:
Safety and efficacy of UCART22 in heavily pre-treated patients with relapsed or refractory CD22+ B-cell acute lymphoblastic leukemia (B-ALL): results of the Phase 1 BALLI-01 trial
Presenter:
Nitin Jain, M.D., Professor of Medicine, Department of Leukemia, University of Texas MD Anderson Cancer Center, Houston (TX)
Session Title:
Advances in the treatment of lymphoblastic leukemia
Session Room:
K1
Live Session Date and Time:
Saturday, June 13 at 5:15 – 6:30pm CET
Eti-cel – Poster Presentation
The abstract from the Phase 1 NATHALI-01 study evaluating eti-cel in patients with relapsed or refractory B-cell non-Hodgkin lymphoma (r/r B-NHL) has been accepted for poster presentation. This preliminary analysis explores the relationship between alemtuzumab exposure, eti-cel cellular expansion, cytokine dynamics, and clinical outcomes, providing early mechanistic insights into the optimization of the lymphodepletion regimen for this best-in-class dual-targeting CD20/CD22 allogeneic CAR T-cell product.
The Phase 1 clinical data of the NATHALI-01 clinical trial are planned to be disclosed in Q4 2026.
Poster Presentation:
Alemtuzumab exposure and sustained IL-2 drive UCART20x22 expansion and clinical response in adults with relapsed or refractory B-cell non-Hodgkin lymphoma: NATHALI-01 study
Presenter:
Professor Emmanuel Bachy, M.D., Ph.D., Department of Clinical Hematology, Lyon Sud Hospital, Lyon, France.
Session:
Poster Session 2
Poster Number:
4758
Session Date and Time:
Saturday, June 13 at 6:45 - 7:45pm CET
The abstracts are published on
the EHA website
. The presentations will be available
on Cellectis’ website
on June 11, 2026, at 8 am CET.
About Cellectis
Cellectis is a clinical-stage biotechnology company using its pioneering gene-editing platform to develop life-saving cell and gene therapies. The company utilizes an allogeneic approach for CAR T immunotherapies in oncology, pioneering the concept of off-the-shelf and ready-to-use gene-edited CAR T-cells to treat cancer patients, and a platform to develop gene therapies in other therapeutic indications. With its in-house manufacturing capabilities, Cellectis is one of the few end-to-end gene editing companies that controls the cell and gene therapy value chain from start to finish.
Cellectis’ headquarters are in Paris, France, with locations in New York and Raleigh, NC. Cellectis is listed on the Nasdaq Global Market (ticker: CLLS) and on Euronext Growth (ticker: ALCLS). To find out more, visit
and follow Cellectis on
LinkedIn
and
X
.
Cautionary Statement
This press release contains “forward-looking” statements within the meaning of applicable securities laws, including the Private Securities Litigation Reform Act of 1995. Forward-looking statements may be identified by words such as “become,” “expected,” “ ‘plan,” “planned,” “potential,” or “will” or the negative of these and similar expressions. These forward-looking statements are based on our management’s current expectations and assumptions and on information currently available to management. Forward-looking statements include statements about the potential of the pivotal Phase 2 BALLI-01 trial to be a registrational phase, the advancement, timing and progress of clinical trials (including with respect to patient enrollment and follow-up), the timing of our presentations of data and submissions of regulatory filings the potential benefit of our product candidates and technologies. These forward-looking statements are made in light of information currently available to us and are subject to significant risks and uncertainties, including with respect to the numerous risks associated with biopharmaceutical product candidate development. Among these are significant risks that the BALLI-01 Phase 1 data may not be validated by data from later stage of clinical trials and that our product candidate may not receive regulatory approval for commercialization. Particular caution should be exercised when interpreting results from Phase 1 studies and results relating to a small number of patients – such results should not be viewed as predictive of future results. With respect to our cash runway, our operating plans, including product development plans, may change as a result of various factors, including factors currently unknown to us. Furthermore, many other important factors, including those described in our Annual Report on Form 20-F as amended and in our annual financial report (including the management report) for the year ended December 31, 2025 and subsequent filings Cellectis makes with the Securities Exchange Commission from time to time, which are available on the SEC’s website at
, as well as other known and unknown risks and uncertainties may adversely affect such forward-looking statements and cause our actual results, performance or achievements to be materially different from those expressed or implied by the forward-looking statements. Except as required by law, we assume no obligation to update these forward-looking statements publicly, or to update the reasons why actual results could differ materially from those anticipated in the forward-looking statements, even if new information becomes available in the future.
For further information on Cellectis, please contact:
Media contacts:
Pascalyne Wilson, Director, Communications, + 33 (0)7 76 99 14 33,
media@cellectis.com
Patricia Sosa Navarro, Chief of Staff to the CEO, +33 (0)7 76 77 46 93
Investor Relations contact:
Arthur Stril, Chief Financial Officer & Chief Business Officer,
investors@cellectis.com
Attachment
20260512_EHA PR
临床1期临床2期基因疗法免疫疗法细胞疗法
2026-05-06
·用药千问
点击蓝字 关注我们
引言:奥妥珠单抗的研发背景与市场地位
奥妥珠单抗(Ocrelizumab)作为新一代抗 CD20 单克隆抗体,在过去十年间彻底改变了多发性硬化症的治疗格局。这款由瑞士罗氏集团旗下基因泰克公司(Genentech)研发的创新药物,不仅是首个获批用于原发进展型多发性硬化症(PPMS)的疾病修正治疗药物,更是凭借其独特的作用机制和卓越的临床疗效,成为全球多发性硬化症治疗领域的标杆之作。
截至 2026 年 4 月,奥妥珠单抗已在全球多个国家和地区获得批准。在美国,该药于 2017 年 3 月 28 日获得 FDA 批准,被指定为突破性疗法;欧盟于 2018 年 1 月 8 日批准上市;中国则于 2025 年 3 月 31 日正式批准,商品名为 "罗可适"(Ocrevus)。值得注意的是,2024 年 9 月 13 日,FDA 还批准了奥妥珠单抗的皮下注射剂型 Ocrevus Zunovo,将给药时间从数小时缩短至约 10 分钟,进一步提升了患者的治疗体验。
除了罗氏的奥妥珠单抗,中国还批准了其他两款相关产品:罗氏的奥妥珠单抗注射液(商品名 "佳罗华"),于 2021 年 6 月获批用于治疗滤泡性淋巴瘤和慢性淋巴细胞白血病;以及北京天广实生物技术公司自主研发的奥妥珠单抗 β 注射液(商品名 "倍捷欣"),于 2026 年 2 月 14 日获批用于治疗抗 AQP4 抗体阳性的视神经脊髓炎谱系疾病(NMOSD)。
本文将从作用机制、临床疗效、安全性、适应症以及市场表现五个维度,对奥妥珠单抗进行全面深入的分析,为临床医生、患者和医药从业者提供详实的参考信息。一、作用机制:精准靶向 B 细胞的创新疗法1.1 CD20 抗原的生物学功能与靶向优势
CD20 是一种分子量约为 35kDa 的 B 细胞特异性跨膜磷蛋白,在 B 细胞发育过程中扮演着至关重要的角色。从晚期前 B 细胞阶段开始表达,在成熟 B 细胞和记忆 B 细胞上持续高表达,但在造血干细胞、原 B 细胞(pro-B)、浆母细胞和浆细胞中不表达。这种表达的阶段特异性为奥妥珠单抗的精准靶向提供了生物学基础。
CD20 的主要功能是作为钙离子通道或钙通道调节子,参与 B 细胞的活化、增殖和分化过程。当 B 细胞受体(BCR)被激活时,CD20 作为钙库操纵(SOC)通道的一部分,促进钙离子内流,这一过程对 B 细胞的信号传导至关重要。CD20 还可以在 "脂筏" 微结构域中与 BCR 共定位,在 BCR 激活后发生高度磷酸化,表现出钙通道样特性。
正是由于 CD20 在 B 细胞表面的高表达和功能重要性,使其成为治疗 B 细胞相关疾病的理想靶点。据统计,超过 90% 的 B 细胞性淋巴瘤表达 CD20 抗原,这为奥妥珠单抗在血液肿瘤治疗中的应用奠定了基础。1.2 四种细胞毒性机制的协同作用
奥妥珠单抗通过与 B 细胞表面的 CD20 抗原结合,触发多种细胞毒性机制,实现对 B 细胞的选择性耗竭。主要包括以下四种机制:
(1)抗体依赖性细胞毒性(ADCC)
这是奥妥珠单抗最重要的作用机制。奥妥珠单抗的 Fc 段经过特殊的糖基化工程改造,去除了岩藻糖,使其与自然杀伤细胞(NK 细胞)、巨噬细胞和单核细胞表面的 FcγRIII 受体亲和力显著增强。体外研究显示,奥妥珠单抗诱导的 ADCC 活性比利妥昔单抗高35-100 倍。
ADCC 的具体过程是:奥妥珠单抗与 B 细胞表面的 CD20 结合后,其 Fc 段与免疫效应细胞(如 NK 细胞)表面的 FcγRIII 受体结合,激活效应细胞释放穿孔素和颗粒酶,直接杀伤靶细胞。这种机制的优势在于其不依赖于 CD20 的表达水平,即使是 CD20 低表达的肿瘤细胞也能被有效杀伤。
(2)抗体依赖性细胞吞噬作用(ADCP)
奥妥珠单抗通过与巨噬细胞和单核细胞表面的 Fc 受体结合,介导对 B 细胞的吞噬作用。这一机制同样受益于其糖基化改造,能够更有效地招募和激活吞噬细胞,增强对 B 细胞的清除效果。
(3)补体依赖性细胞毒性(CDC)
奥妥珠单抗可以激活补体级联反应,通过膜攻击复合物(MAC)导致靶细胞溶解。然而,与利妥昔单抗相比,奥妥珠单抗的 CDC 活性相对较弱。这是因为奥妥珠单抗作为 II 型抗 CD20 抗体,不会诱导 CD20 分子向脂筏聚集或内化,无法像利妥昔单抗那样促使 Fc 段形成六聚体,从而削弱了固定 C1q 的能力。
(4)直接细胞死亡(DCD)
这是奥妥珠单抗区别于其他抗 CD20 抗体的独特机制。奥妥珠单抗可以直接激活细胞内死亡信号通路,诱导非凋亡性程序性细胞死亡。研究表明,奥妥珠单抗引发的是一种强烈的、依赖肌动蛋白重构的非典型溶酶体细胞死亡途径,这种机制不依赖于补体,对低表达 CD20 的慢性淋巴细胞白血病(CLL)细胞杀伤力显著优于利妥昔单抗。1.3 选择性耗竭 B 细胞的分子基础
奥妥珠单抗能够实现对 B 细胞的选择性耗竭,同时保留造血干细胞和浆细胞,这种选择性基于 CD20 表达的阶段特异性:
保留造血干细胞和原 B 细胞:由于这些细胞不表达 CD20,因此不会受到药物影响,确保了 B 细胞的再生能力
保留浆细胞:浆细胞在终末分化过程中失去 CD20 表达,因此能够维持既往感染或疫苗接种诱导的抗体分泌功能,保证基础体液免疫不受影响
清除成熟 B 细胞:从晚期前 B 细胞到成熟 B 细胞和记忆 B 细胞均表达 CD20,是奥妥珠单抗的主要作用靶点
这种选择性机制带来了重要的临床优势:患者在接受治疗期间仍能维持基本的体液免疫功能,降低了严重感染的风险。研究显示,抗 CD20 单抗对长寿命浆细胞和次级淋巴结构内保护性壁龛中的 B 细胞影响较小,不增加感染风险。1.4 在多发性硬化症中的作用原理
尽管奥妥珠单抗在多发性硬化症中的精确治疗机制尚未完全阐明,但大量研究表明其治疗效果与 B 细胞耗竭密切相关。B 细胞在 MS 发病机制中发挥着多重作用:
产生致病性抗体:脑脊液中浸润的浆母细胞和浆细胞产生寡克隆带(OCBs),其中一部分是针对髓鞘和其他中枢神经系统抗原的自身抗体
激活 T 细胞:B 细胞作为抗原呈递细胞,激活致病性 T 细胞,触发炎症级联反应
分泌促炎因子:B 细胞分泌多种促炎细胞因子,如 TNF-α、IL-6 等,参与神经炎症过程
形成异位淋巴组织:在继发进展型 MS 患者的软脑膜中发现含有 B 细胞的生发中心样结构,可能是 OCB 产生的额外来源
奥妥珠单抗通过耗竭 CD20+ B 细胞,从多个环节阻断 MS 的病理进程。研究还发现,奥妥珠单抗不仅耗竭 B 细胞,还能影响 T 细胞功能。2025 年发表的研究显示,奥妥珠单抗可以有效清除CD20+ T 细胞,减少 Th17.1 细胞及炎性因子分泌。此外,奥妥珠单抗还具有抗炎和神经保护的双重作用,能够上调 HuR、MnSOD 和 HSP70 等神经保护通路。1.5 在血液肿瘤中的作用机制
在血液肿瘤治疗中,奥妥珠单抗的作用机制与在自身免疫性疾病中相似,但也有其特殊性:
(1)直接杀伤肿瘤细胞:通过 ADCC、ADCP、CDC 和 DCD 四种机制直接清除表达 CD20 的肿瘤细胞
(2)免疫调节作用:奥妥珠单抗能够清除肿瘤微环境中的调节性 B 细胞,减少免疫抑制因子(如 IL-10、TGF-β)的分泌,从而增强抗肿瘤 T 细胞应答
(3)克服耐药性:由于奥妥珠单抗的 ADCC 活性更强且不依赖于 CD20 表达水平,对部分利妥昔单抗耐药的肿瘤细胞仍有杀伤作用1.6 与其他抗 CD20 抗体的差异化特征
奥妥珠单抗与其他抗 CD20 抗体(特别是利妥昔单抗)在结构和功能上存在显著差异:
特征
奥妥珠单抗
利妥昔单抗
抗体类型
II 型人源化单抗
I 型人鼠嵌合单抗
糖基化修饰
去除岩藻糖(糖基工程化)
未进行糖基化改造
主要作用机制
ADCC(为主)+ DCD
CDC(为主)+ ADCC
与 FcγRIII 亲和力
高(比利妥昔单抗高 35-100 倍)
标准
CD20 结合位点
近膜区
N 端膜外区
诱导 CD20 内化
否
是
免疫原性
低(人源化)
高(鼠源成分)
补体激活能力
弱
强
这些差异使得奥妥珠单抗在临床应用中展现出独特优势:更强的 ADCC 活性使其对 CD20 低表达肿瘤细胞更有效;糖基化改造提高了疗效;人源化程度高降低了免疫原性;独特的 II 型抗体特性提供了新的细胞死亡机制。二、临床疗效:从短期获益到长期预后的全面改善2.1 复发型多发性硬化症的突破性进展
奥妥珠单抗在复发型多发性硬化症(RMS)中的疗效通过两项规模最大的 III 期临床试验 ——OPERA I 和 OPERA II得到了充分验证。这两项研究设计相同,共纳入 1656 例患者,随机接受奥妥珠单抗(600mg,每 24 周一次)或干扰素 β-1a(44μg,皮下注射,每周三次)治疗 96 周。
(1)年复发率的显著降低
在 OPERA I 研究中,奥妥珠单抗组的年复发率(ARR)为0.16,而干扰素 β-1a 组为 0.29,复发风险降低46%(P<0.001)。OPERA II 研究得到了几乎相同的结果,奥妥珠单抗组 ARR 为 0.16,干扰素组为 0.29,复发风险降低47%(P<0.001)。
更令人印象深刻的是长期随访数据。在开放标签扩展(OLE)研究中,持续接受奥妥珠单抗治疗 6 年的患者,其 ARR 进一步降至0.05,而从干扰素转换为奥妥珠单抗的患者 ARR 为 0.09。基于 MSBase 注册库的真实世界研究显示,患者的 ARR 从治疗前的 0.58 次 / 年降至治疗后的0.05 次 / 年,意味着平均每 20 年才会出现一次复发。
(2)残疾进展的有效延缓
残疾进展是评估 MS 治疗效果的关键指标。在 96 周的双盲期内,奥妥珠单抗组 24 周确认残疾进展(CDP)的患者比例为6.9%,而干扰素组为 10.5%,风险降低40%(HR=0.60,95%CI 0.43-0.84,P=0.003)。12 周 CDP 的改善更为显著,奥妥珠单抗组为 9.1%,干扰素组为 13.6%,风险降低40%(HR=0.60,95%CI 0.45-0.81,P<0.001)。
长期随访数据更加令人振奋。9 年的随访结果显示,78.7% 的奥妥珠单抗治疗患者在 9 年内未出现 24 周 CDP。在 OPERA 开放标签扩展研究中,持续治疗 6 年的患者与延迟治疗的患者相比,24 周 CDP 风险降低 22%(19% vs 24%,P<0.05)。
(3)影像学指标的近乎完全抑制
MRI 检查显示了奥妥珠单抗对 MS 炎症活动的强大抑制作用:
T1 增强病灶:奥妥珠单抗组减少94-95%(OPERA I: 0.02 vs 0.29,P<0.001;OPERA II: 0.02 vs 0.42,P<0.001)
新发病灶或扩大的 T2 病灶:24 周后减少97-98%
脑萎缩:奥妥珠单抗组脑容量丢失显著少于干扰素组(P<0.001),且这种获益在整个 9 年研究期间持续存在
特别值得注意的是,在 OCARINA II 研究中,接受皮下注射奥妥珠单抗的患者在 48 周时,113 例患者中 0 例出现 T1 增强病灶,仅 1 例出现 1-2 个新的或扩大的 T2 病灶,显示了近乎完全的影像学抑制效果。
(4)无疾病活动证据(NEDA)的卓越表现
NEDA 是评估 MS 治疗效果的综合指标,定义为无临床复发、无残疾进展、无影像学活动。在 OPERA 研究的 96 周双盲期内,奥妥珠单抗组72.5%的患者达到 NEDA-3(无复发、无 CDP、无 Gd + 病灶),而干扰素组仅为43.8%(OR=3.48,95%CI 2.52-4.81,P<0.0001)。
这一优势在长期随访中得以维持。9 年后,持续接受奥妥珠单抗治疗的患者中仍有 **48.2%** 维持 NEDA 状态,而从干扰素转换为奥妥珠单抗的患者仅为 25.7%。奥妥珠单抗组达到 NEDA 的比例超过了所有其他 DMT 药物,包括芬戈莫德(33%)、那他珠单抗(37%)和阿仑单抗(32%-39%)。
(5)认知功能的保护作用
除了运动功能,奥妥珠单抗对 MS 患者的认知功能也有保护作用。在 OPERA 研究的事后分析中,奥妥珠单抗组患者在 96 周内的符号数字模式测试(SDMT)平均改善5.4 分,而干扰素组仅改善 4.0 分(调整均数差 1.4 分,95% CI 0.05-2.72,P=0.042)。奥妥珠单抗组发生临床意义认知下降(SDMT 下降≥4 分)的风险降低了37%(12 周确认)和43%(24 周确认)。2.2 原发进展型多发性硬化症的历史性突破
ORATORIO 研究是奥妥珠单抗获批用于原发进展型多发性硬化症(PPMS)的关键 III 期临床试验,这也是首个在 PPMS 中显示疗效的药物。该研究纳入 732 例 PPMS 患者,按 2:1 随机分配至奥妥珠单抗组(488 例)或安慰剂组(244 例),治疗至少 120 周。
(1)残疾进展的显著延缓
ORATORIO 研究达到了其主要终点:奥妥珠单抗组 12 周 CDP 的患者比例为32.9%,而安慰剂组为 39.3%,风险降低24%(HR=0.76,95%CI 0.59-0.98,P=0.04)。24 周 CDP 的改善更为显著,奥妥珠单抗组为 29.6%,安慰剂组为 35.7%,风险降低25%(HR=0.75,95%CI 0.58-0.98,P=0.04)。
长期随访数据进一步证实了奥妥珠单抗的获益。在开放标签扩展研究中,持续接受奥妥珠单抗治疗 6.5 年的患者与延迟治疗患者相比:
24 周 CDP 风险降低20%(52% vs 65%,P=0.002)
上肢功能恶化风险降低28%(31% vs 43%,P=0.004)
需要轮椅(EDSS≥7)的风险降低42%(P=0.0112)
(2)运动功能的全面改善
奥妥珠单抗对 PPMS 患者的运动功能有全面改善作用:
Timed 25-foot walk(T25FW):120 周时,奥妥珠单抗组患者的步行速度下降幅度小于安慰剂组,改善了 38%(P=0.04)
九孔插针试验(9HPT):奥妥珠单抗组患者的手部功能显著改善,双手平均改善 5.749 秒(P<0.001),较差手改善 7.572 秒(P=0.041)
整体功能评估:从基线到 120 周,奥妥珠单抗组患者的扩展残疾状态量表(EDSS)评分平均变化为 - 0.90,而安慰剂组为 - 1.09,显示了功能的相对改善
(3)脑萎缩的有效减缓
脑萎缩是 PPMS 患者疾病进展的重要标志。ORATORIO 研究显示,奥妥珠单抗组患者的脑体积在 24-120 周期间仅减少0.7%,而安慰剂组减少 1.1%。更重要的是,奥妥珠单抗组的 T2 病灶总体积减少了3.4%,而安慰剂组增加了 7.43%,显示了对脑萎缩和病灶负荷的双重改善。2.3 血液肿瘤治疗的显著疗效
奥妥珠单抗在血液肿瘤治疗中同样展现出卓越疗效,主要体现在滤泡性淋巴瘤(FL)和慢性淋巴细胞白血病(CLL)的治疗中。
(1)滤泡性淋巴瘤的长期获益
GALLIUM 研究是评估奥妥珠单抗联合化疗治疗初治 FL 的关键 III 期临床试验,纳入 1202 例患者:
无进展生存期(PFS):3 年 PFS 率奥妥珠单抗组为80.0%,而利妥昔单抗组为 73.3%(HR=0.66,95% CI 0.51-0.85,P=0.001)
总缓解率(ORR):两组相似(奥妥珠单抗组 88.5% vs 利妥昔单抗组 86.9%),但奥妥珠单抗组的完全缓解率更高
长期随访结果:7.9 年随访显示,奥妥珠单抗组的 7 年 PFS 率为63.4%,显著高于利妥昔单抗组的 55.7%
在复发难治性 FL 的治疗中,奥妥珠单抗同样表现出色。GADOLIN 研究显示,奥妥珠单抗联合苯达莫司汀治疗复发难治 FL,中位随访 52.2 个月,显著改善了患者的 PFS。ROSEWOOD 研究则显示,泽布替尼联合奥妥珠单抗治疗复发难治 FL,中位 PFS 达到28.0 个月,而奥妥珠单抗单药仅为 10.4 个月(HR=0.50,95% CI 0.33-0.75,P<0.001)。
(2)慢性淋巴细胞白血病的生存获益
奥妥珠单抗在 CLL 治疗中的疗效通过多项临床试验得到验证:
CLL11 研究:奥妥珠单抗联合苯丁酸氮芥治疗初治 CLL,中位 PFS 达到26.7 个月,显著优于利妥昔单抗联合苯丁酸氮芥的 14.9 个月
CLL14 研究:维奈克拉联合奥妥珠单抗治疗初治 CLL,3 年 PFS 率达到88%,且微小残留病变(MRD)阴性率高达 85%
真实世界证据:在既往治疗过的 CLL 患者中,奥妥珠单抗联合维奈克拉显示出良好的疗效和安全性,大多数患者达到了深度缓解2.4 最新研究进展与长期安全性数据
截至 2026 年 4 月,奥妥珠单抗的临床研究不断有新的突破和长期数据更新:
(1)10 年长期随访数据
2025 年发表在 Neurology 杂志上的 10 年随访研究显示:
接受奥妥珠单抗治疗 10 年的患者中,73.9% 未出现 48 周 CDP
年复发率维持在极低水平(约 0.05)
未发现新的安全信号,长期安全性良好
(2)2025 年 ECTRIMS 会议最新数据
在 2025 年 9 月举行的第 41 届欧洲多发性硬化症治疗和研究委员会(ECTRIMS)会议上,罗氏公布了多项奥妥珠单抗的最新研究数据:
儿童 MS 患者:奥妥珠单抗在复发缓解型儿童 MS 患者中显示出显著的预防残疾进展效果
妊娠和哺乳期女性:新数据支持奥妥珠单抗在妊娠和哺乳期的安全性
晚期 PPMS 患者:在疾病晚期的 PPMS 患者中也观察到了获益
皮下注射剂型:OCARINA II 研究的 48 周数据显示,皮下注射奥妥珠单抗与静脉注射在疗效和安全性上相当,且注射相关反应多为轻中度
(3)药物暴露 - 反应关系研究
2025 年 ACTRIMS 论坛上公布的暴露 - 反应分析显示,奥妥珠单抗的药物暴露量与疗效密切相关:
高暴露组(Q4)患者的 48 周 CDP 风险比低暴露组(Q1)降低40%
84.5% 的高暴露患者在 48 周内无 CDP,而低暴露组为 73.9%
这一发现支持个体化给药策略的探索
(4)中国患者的临床数据
奥妥珠单抗 β(倍捷欣)在中国 NMOSD 患者中的 III 期临床试验显示了卓越疗效:
复发率仅为2.2%,复发风险降低97.5%
年化复发率从 1.024 降至0.028 / 人年
中位首次复发时间未达到,而安慰剂组为 21 周(HR=0.025,P<0.0001)
EDSS 评分较基线平均改善 0.72 分(P=0.019)2.5 疗效预测因素与个体化治疗
随着研究的深入,一些可能影响奥妥珠单抗疗效的因素逐渐被识别:
(1)早期治疗的重要性
多项研究一致表明,早期开始奥妥珠单抗治疗能够获得更好的长期预后:
9 年随访显示,早期开始治疗的患者维持 NEDA 的比例是延迟治疗患者的近 2 倍(48.2% vs 25.7%)
早期治疗组的脑萎缩程度明显低于延迟治疗组
这支持了 "时间就是大脑和脊髓" 的治疗理念
(2)药物暴露量的影响
暴露 - 反应分析提示,较高的药物暴露量与更好的疗效相关。这可能与以下因素有关:
B 细胞耗竭的深度和持续时间
药物在中枢神经系统的渗透
个体的药物代谢差异
(3)遗传因素的潜在影响
初步研究显示,某些遗传多态性可能影响奥妥珠单抗的疗效,包括:
FcγRIIIa 受体的多态性(影响 ADCC 活性)
药物代谢酶的基因变异
疾病相关基因的多态性
然而,这些发现仍需要更多研究来证实和验证。三、安全性:风险可控的长期治疗选择3.1 急性输液反应:可预防和管理的常见事件
输液相关反应(Infusion-Related Reactions, IRR)是奥妥珠单抗治疗最常见的不良反应,但其发生率和严重程度都在可控范围内。
(1)发生率和临床表现
奥妥珠单抗的输液反应发生率因研究和给药途径而异:
静脉给药:在 OPERA 研究中,34.3% 的患者出现输液反应
皮下给药:在 OCARINA II 研究中,51.5% 的患者出现注射相关反应,其中局部反应占 50.2%,全身反应仅占 11.6%
输液反应的典型症状包括:
轻中度症状:发热、寒战、头痛、头晕、恶心、荨麻疹
重度症状:呼吸困难、支气管痉挛、低血压、血管性水肿
极罕见:过敏反应、心源性休克
值得注意的是,99.8% 的输液反应为轻至中度,且随着治疗次数的增加,反应的强度和持续时间会逐渐减轻。
(2)预防措施
为降低输液反应的发生风险,临床实践中采用分级预防策略:
患者类型
预防用药
给药时机
所有患者(第 1 次输注)
静脉糖皮质激素 + 口服解热镇痛药 + 抗组胺药
输注前 1 小时 + 输注前 30 分钟
既往无 IRR 的患者(后续输注)
口服解热镇痛药
输注前 30 分钟
既往有 1-2 级 IRR 的患者
口服解热镇痛药 + 抗组胺药
输注前 30 分钟
既往有 3 级 IRR 的患者
静脉糖皮质激素 + 口服解热镇痛药 + 抗组胺药
输注前 1 小时 + 输注前 30 分钟
具体药物选择:
糖皮质激素:100mg 泼尼松 / 泼尼松龙、20mg 地塞米松或 80mg 甲泼尼龙(禁用氢化可的松)
解热镇痛药:650-1000mg 对乙酰氨基酚
抗组胺药:50mg 苯海拉明或 40mg 苯海拉明
(3)输注速度管理
严格的输注速度控制是预防严重反应的关键:
首次输注:起始速度 50mg / 小时,每 30 分钟可提高 50mg / 小时,最大速度 400mg / 小时
后续输注:
如前次输注速度≥100mg / 小时且无 IRR 或仅 1 级 IRR:可从 100mg / 小时开始
如前次有 2 级或以上 IRR:从 50mg / 小时开始
最大速度均为 400mg / 小时
(4)反应处理流程
当发生输液反应时,应根据严重程度采取相应措施:
CTCAE 分级
处理措施
1-2 级(轻 - 中度)
降低输注速度或暂停,对症治疗,症状缓解后可恢复
3 级(重度)
暂停输注,立即对症治疗,症状缓解后以原速度的 50% 重新开始,如再次发生 3 级反应则永久停药
4 级(危及生命)
立即停止输注并永久终止治疗3.2 感染风险:总体可控,需警惕特殊病原体
感染是奥妥珠单抗治疗的重要安全性考量,但总体风险可控。
(1)感染发生率
大规模临床试验数据显示:
奥妥珠单抗组感染发生率:51.6%
对照组(干扰素或特立氟胺)感染发生率:52.7%
严重感染发生率:奥妥珠单抗组 2.5%,对照组 1.8-2.9%
这表明奥妥珠单抗的感染风险与其他 DMT 药物相当,并未显著增加总体感染风险。
(2)机会性感染的监测
尽管总体感染风险不增加,但仍需警惕某些机会性感染:
进行性多灶性白质脑病(PML):截至目前,奥妥珠单抗治疗相关的 PML 报告极为罕见,发生率远低于那他珠单抗等其他 DMT 药物
乙型肝炎病毒(HBV)再激活:所有患者治疗前都应进行 HBV 筛查,HBsAg 阳性患者禁用
结核感染:治疗前需进行结核筛查,包括活动性结核评估和潜伏性结核检测
(3)免疫功能评估
治疗期间应定期监测:
血清免疫球蛋白水平:特别是 IgG、IgA、IgM
B 细胞计数:评估耗竭程度和恢复情况
疫苗接种状态:治疗期间及停药后至 B 细胞恢复前,不建议接种减毒活疫苗3.3 血液系统影响:可逆的淋巴细胞减少
奥妥珠单抗治疗导致的血液系统影响主要是淋巴细胞减少,这是其作用机制的直接体现。
(1)B 细胞耗竭模式
奥妥珠单抗导致的 B 细胞耗竭呈现典型模式:
治疗后 1 周内:外周血 CD19+ B 细胞迅速下降至检测不到的水平
维持期:治疗期间 B 细胞持续处于耗竭状态
停药后:B 细胞开始缓慢恢复,主要为幼稚 B 细胞,记忆 B 细胞的恢复可能需要 1-2 年
(2)T 细胞的影响
最新研究发现,奥妥珠单抗还可能影响表达 CD20 的 T 细胞亚群:
约 3-5% 的 CD3+ T 细胞表达低水平 CD20
这些 CD3+CD20dim T 细胞在 MS 患者中可能增加
奥妥珠单抗治疗可导致这些细胞的耗竭
长期影响尚需进一步研究
(3)对疫苗应答的影响
由于浆细胞不受影响,患者对既往感染和疫苗的抗体应答得以保留。但治疗期间接种新疫苗可能影响应答效果,因此建议:
治疗前至少 4 周完成所有疫苗接种
优先接种灭活疫苗
避免接种活疫苗3.4 其他重要不良反应
除了上述主要不良反应,奥妥珠单抗还可能引起以下问题:
(1)肿瘤溶解综合征(TLS)
主要发生在血液肿瘤患者,特别是肿瘤负荷高和 / 或肾功能受损的患者:
预防措施:充分水化、使用别嘌醇或尿酸氧化酶
监测指标:血尿酸、电解质、肌酐
高危患者应在配备完善急救设施的医疗机构接受治疗
(2)肝毒性
奥妥珠单抗相关的肝毒性较为罕见,但仍需监测肝功能。在一项研究中,16 例 FL 患者接受含奥妥珠单抗方案治疗,出现了 1-2 级肝损害,经对症处理后好转。
(3)心血管事件
输液过程中可能出现低血压,特别是在首次输注时:
建议:输注前 12 小时及输注期间暂停降压药
监测:密切监测血压变化
处理:必要时使用升压药
(4)皮肤反应
包括皮疹、瘙痒等,多为轻中度,可通过抗组胺药缓解。3.5 长期安全性:十年随访数据支持
奥妥珠单抗的长期安全性数据令人鼓舞,特别是长达 10 年的随访研究:
(1)总体安全性概况
长期治疗未发现新的安全信号
不良事件类型与短期研究一致
严重不良事件发生率稳定
(2)感染风险的长期评估
9 年持续治疗期间,感染率保持在低水平且稳定
未观察到机会性感染的累积风险增加
与其他 DMT 药物相比,感染风险无显著差异
(3)恶性肿瘤风险
这是患者和医生都关心的问题。长期数据显示:
所有恶性肿瘤的发生率比值(IR)为 0.53(95% CI 0.34-0.79),低于一般人群
这一数据与丹麦基于人群的注册研究(IR 0.67)相似
提示奥妥珠单抗可能不会增加恶性肿瘤风险
(4)生殖毒性和妊娠安全性
2025 年 ECTRIMS 会议公布的最新数据为特殊人群提供了重要信息:
动物研究显示奥妥珠单抗可通过胎盘屏障
人类妊娠期间使用的数据有限
建议:
育龄女性治疗期间应采取有效避孕措施
计划妊娠前应停药并等待 B 细胞恢复
哺乳期用药需权衡利弊3.6 安全性管理建议
基于以上分析,对奥妥珠单抗治疗的安全性管理提出以下建议:
(1)治疗前评估
全面的病史采集,特别是感染史、疫苗接种史
实验室检查:血常规、肝肾功能、免疫球蛋白、HBV/HCV、结核筛查
基线评估:视力、神经系统功能、MRI
患者教育:告知可能的不良反应及应对措施
(2)治疗期间监测
每次输注前:评估感染征象、生命体征
定期检查:血常规、免疫球蛋白(每 3-6 个月)、肝肾功能
B 细胞监测:治疗开始后 1 个月,此后每 3 个月
特殊监测:如出现新的神经系统症状,需考虑 PML 可能
(3)特殊人群管理
老年人:无需调整剂量,但需密切监测
肾功能不全:轻度至中度肾功能不全无需调整剂量,重度患者不推荐使用
肝功能不全:轻度患者无需调整,中重度患者不推荐使用
儿童患者:安全性和有效性尚未确立
(4)药物相互作用
与活疫苗:避免同时使用
与其他免疫抑制剂:可能增加感染风险,需谨慎
与抗高血压药:可能增强降压效果,建议输注前暂停四、适应症:从罕见病到常见病的广泛应用4.1 多发性硬化症:改变疾病进程的里程碑
奥妥珠单抗在多发性硬化症治疗中取得了历史性突破,成为首个获批用于原发进展型 MS 的药物。
(1)复发型多发性硬化症(RMS)
奥妥珠单抗获批用于治疗成人复发型多发性硬化症,包括以下亚型:
临床孤立综合征(CIS):首次发生的、提示 MS 的神经系统症状
复发缓解型 MS(RRMS):典型的复发 - 缓解病程
活动性继发进展型 MS(SPMS):疾病进展过程中仍有复发的 SPMS
获批剂量和用法:
静脉制剂:初始剂量为 2 次 300mg,间隔 14 天;随后每 24 周给予 600mg
皮下制剂:每次 920mg,每 24 周一次,约 10 分钟完成注射
(2)原发进展型多发性硬化症(PPMS)
奥妥珠单抗是目前唯一获批用于 PPMS 的疾病修正治疗药物。其获批基于 ORATORIO 研究的阳性结果,显示能够延缓 PPMS 患者的残疾进展。
适用人群:
成人 PPMS 患者
疾病持续时间相对较短
残疾程度相对较轻(通常 EDSS<6.5)
有炎症活动证据(如 MRI 显示钆增强病灶)4.2 血液系统恶性肿瘤:精准靶向的新选择
除了自身免疫性疾病,奥妥珠单抗在血液肿瘤治疗中也占据重要地位。
(1)滤泡性淋巴瘤(FL)
罗氏的奥妥珠单抗注射液(佳罗华)获批用于:
初治的 II 期伴有巨大肿块、III 期或 IV 期滤泡性淋巴瘤成人患者
与化疗(苯达莫司汀、CHOP 或 CVP)联合使用
达到至少部分缓解的患者,随后用奥妥珠单抗进行单药维持治疗
给药方案:
诱导治疗:6 个周期,每个周期 21-28 天,与化疗联合
维持治疗:每 2 个月一次,直至疾病进展或最长 2 年
(2)慢性淋巴细胞白血病(CLL)
适应症包括:
既往未接受过治疗的慢性淋巴细胞白血病患者
与苯丁酸氮芥联合使用
也可与维奈克拉等新型药物联合
最新研究显示,奥妥珠单抗联合维奈克拉在 CLL14 研究中取得了优异结果,3 年 PFS 率达 88%。4.3 视神经脊髓炎谱系疾病:国产创新的突破
2026 年 2 月 14 日,北京天广实生物技术公司的奥妥珠单抗 β(倍捷欣)获批用于治疗抗 AQP4 抗体阳性的视神经脊髓炎谱系疾病(NMOSD)成人患者,这是首个获批用于 NMOSD 的国产药物。
NMOSD 是一种罕见的中枢神经系统自身免疫性疾病,约 70-80% 的患者 AQP4 抗体阳性。奥妥珠单抗 β 的获批基于其 III 期临床试验的卓越疗效:
复发率仅 2.2%,复发风险降低 97.5%
年化复发率从 1.024 降至 0.028 / 人年
中位首次复发时间未达到,而安慰剂组为 21 周4.4 其他潜在适应症:不断拓展的治疗领域
除了已获批的适应症,奥妥珠单抗在以下疾病的治疗中也显示出潜力:
(1)系统性红斑狼疮(SLE)
奥妥珠单抗在 SLE 治疗中展现出良好前景。2025-2026 年发表在 NEJM 的研究显示:
52 周时 76.7% 的患者达到 SRI 4 应答(疾病活动度显著下降),远高于安慰剂组的 53.5%
80% 的患者成功将激素用量减至安全剂量(≤7.5mg 泼尼松)
显著降低 52 周疾病复发风险
奥妥珠单抗通过深度耗竭 B 细胞,不仅减少致病性自身抗体的产生,还能调节 T 细胞功能,实现多重治疗效果。目前,罗氏的奥妥珠单抗狼疮适应症已获 CDE 受理上市申请。
(2)原发性膜性肾病(PMN)
奥妥珠单抗 β 在 PMN 治疗中也显示出突破性进展:
已被国家药监局纳入 "突破性治疗" 药物品种
是首款在肾病治疗领域获得该认定的国产药物
其 NDA 申请已于 2025 年 10 月纳入优先审评程序
有望成为中国首个获批治疗 PMN 的特效药物
(3)其他自身免疫性疾病
奥妥珠单抗还在以下疾病中进行临床试验:
类风湿关节炎:通过耗竭 B 细胞和调节免疫反应发挥作用
天疱疮:针对致病性自身抗体的产生
多发性肌炎 / 皮肌炎:减少炎症因子和自身抗体
干燥综合征:调节 B 细胞功能,减少唾液腺炎症4.5 适应症获批历程与全球布局
奥妥珠单抗系列产品的全球获批历程反映了其在不同疾病领域的价值:
产品
适应症
获批地区
获批时间
奥妥珠单抗(静脉)
RMS、PPMS
美国
2017 年 3 月
奥妥珠单抗(静脉)
RMS、PPMS
欧盟
2018 年 1 月
奥妥珠单抗(静脉)
RMS、PPMS
中国
2025 年 3 月
奥妥珠单抗(皮下)
RMS、PPMS
美国
2024 年 9 月
奥妥珠单抗(佳罗华)
FL、CLL
中国
2021 年 6 月
奥妥珠单抗 β(倍捷欣)
NMOSD
中国
2026 年 2 月4.6 适应症选择的临床考量
在选择奥妥珠单抗治疗时,临床医生需要综合考虑以下因素:
(1)疾病活动性评估
MS:需要临床或影像学证据显示疾病活动
血液肿瘤:需要组织学确诊和疾病分期
自身免疫病:需要活动性疾病的客观证据
(2)患者特征评估
年龄和一般状况
合并症和用药情况
生育计划(特别是育龄女性)
疫苗接种状态
经济承受能力
(3)治疗目标设定
MS:延缓残疾进展、减少复发、保护神经功能
血液肿瘤:缓解症状、延长生存期、提高生活质量
自身免疫病:控制疾病活动、减少激素用量、预防器官损伤
(4)风险获益评估
每种适应症都有相应的获益证据
需要权衡感染风险、输液反应等不良反应
考虑长期治疗的依从性
评估替代治疗方案五、市场表现:从快速增长到成熟领先的商业成功5.1 全球销售额:持续增长的重磅药物
奥妥珠单抗自上市以来,销售额呈现强劲增长态势,已成为罗氏的核心产品之一。
(1)历年销售额回顾
根据罗氏公布的财报数据,奥妥珠单抗的全球销售额表现如下:
年份
销售额(瑞士法郎)
同比增长
备注
2017
12.1 亿
-
3 月上市,仅 9 个月
2018
26.5 亿
119%
首个完整销售年
2019
36.6 亿
38%
持续快速增长
2020
47.5 亿
29.8%
疫情期间仍保持增长
2021
56.5 亿
19%
接近 60 亿大关
2022
62.3 亿
10.3%
增速放缓但仍稳健
2023
67.8 亿
8.8%
持续增长
2024
74.0 亿
9.2%
创历史新高
(2)2024 年销售亮点
2024 年奥妥珠单抗的销售额达到74 亿瑞士法郎(约合 80 亿美元),成为罗氏旗下销售额最高的药物。这一成绩的取得得益于:
美国市场的持续增长,成为最常用的 DMT 药物
欧洲市场的稳步扩张
中国市场的新突破(2025 年 3 月获批)
皮下注射剂型的推出带来新的增长动力
(3)2025 年最新数据
根据罗氏 2025 年第一季度财报,奥妥珠单抗销售额为18.4 亿瑞士法郎,同比增长 7%。虽然增速有所放缓,但仍保持稳定增长。值得注意的是,皮下注射剂型的推出正在改变市场格局,预计将带来新的增长机会。5.2 市场份额:从追赶者到领导者的转变
奥妥珠单抗在多发性硬化症治疗市场的地位不断提升。
(1)美国市场表现
在美国,奥妥珠单抗已成为最常用的疾病修正治疗药物(DMT),全球累计治疗超过 40 万患者。市场份额的快速增长得益于:
卓越的临床疗效数据
首个获批用于 PPMS 的药物
每 6 个月一次的给药便利性
强大的市场推广能力
(2)欧洲市场地位
在欧洲,奥妥珠单抗同样表现出色:
2018 年 1 月获批后迅速占领市场
在多个国家成为一线治疗选择
特别是在 PPMS 患者中,几乎占据垄断地位
(3)亚太市场潜力
亚太市场是奥妥珠单抗未来增长的重要驱动力:
中国:2025 年 3 月获批,市场潜力巨大
日本:已批准多年,市场稳定增长
韩国、澳大利亚等国:市场份额稳步提升5.3 竞争格局:面对挑战保持领先
尽管奥妥珠单抗在市场上取得了巨大成功,但竞争也日益激烈。
(1)主要竞争对手
多发性硬化症治疗市场的主要竞争者包括:
那他珠单抗(Tysabri):年销售额约 40 亿美元,在部分患者中仍有优势
芬戈莫德(Gilenya):口服药物的便利性
西尼莫德(Mayzent):选择性 S1P 受体调节剂
克拉屈滨(Mavenclad):口服,短期治疗
阿仑单抗(Lemtrada):高效但安全性顾虑
(2)奥妥珠单抗的竞争优势
面对竞争,奥妥珠单抗保持领先地位的原因包括:
疗效优势:NEDA 率最高(72.5%),复发率最低
适应症优势:唯一获批用于 PPMS
给药便利性:每 6 个月一次,皮下制剂进一步简化
安全性良好:长期使用风险可控
品牌影响力:罗氏的品牌优势和强大的研发能力
(3)新进入者的威胁
需要关注的新进入者:
奥法妥木单抗(Ofatumumab):每月皮下注射,2023 年获批
乌布利西单抗(Ublituximab):正在开发中
其他 CD20 单抗:生物类似药的开发5.4 定价策略:平衡价值与可及性
奥妥珠单抗的定价反映了其创新价值,但也面临着可负担性的挑战。
(1)美国定价
静脉制剂:约 6.5 万美元 / 年
皮下制剂:价格相近
这一定价与其他高价值 DMT 药物相当
(2)欧洲定价
各国定价不同,通常在 4-6 万欧元 / 年
考虑了各国的医保政策和支付能力
(3)中国定价
罗氏的奥妥珠单抗(罗可适):尚未公布具体价格
预计将参考国际价格并考虑中国市场特点
天广实的奥妥珠单抗 β(倍捷欣):作为国产药,预计价格更具竞争力5.5 医保覆盖:提高患者可及性的关键
医保覆盖情况直接影响药物的市场表现和患者可及性。
(1)美国医保
已纳入 Medicare 和 Medicaid
商业保险基本覆盖
患者自付费用通过援助项目可降至较低水平
(2)欧洲医保
多数国家已纳入医保
部分国家需要满足特定条件(如疾病活动性)
通常需要阶梯治疗(先使用低价位药物)
(3)中国医保
罗氏的奥妥珠单抗(佳罗华):2021 年 12 月纳入国家医保目录,用于 FL 和 CLL
罗氏的奥妥珠单抗(罗可适):MS 适应症的医保谈判正在进行中
天广实的奥妥珠单抗 β:作为罕见病用药,有望通过谈判纳入医保5.6 未来增长驱动因素
展望未来,奥妥珠单抗的市场增长将由以下因素驱动:
(1)适应症扩展
系统性红斑狼疮:已进入审批阶段,市场潜力巨大
原发性膜性肾病:有望成为新的重磅适应症
其他自身免疫性疾病:持续的临床开发
(2)新剂型优势
皮下注射剂型:提高患者依从性,扩大适用人群
正在开发的高浓度制剂:进一步简化给药
预充式注射器和自动注射器:提高便利性
(3)市场扩张
中国市场:2025 年 3 月获批,随着诊断率提升和医保覆盖,增长潜力巨大
新兴市场:印度、巴西等国市场正在开放
基层医疗:提高药物可及性,覆盖更多患者
(4)真实世界证据
长期随访数据不断更新,支持长期使用
真实世界研究证实疗效和安全性
患者报告结局(PRO)数据改善
(5)竞争策略
加强与医生的学术合作
患者教育和支持项目
与其他药物的联合治疗探索
应对生物类似药的策略5.7 市场预测与展望
基于当前趋势和市场分析,对奥妥珠单抗的市场前景做出以下预测:
(1)短期预测(2025-2027)
全球销售额将突破 80 亿瑞士法郎
中国市场将贡献显著增量
皮下制剂占比将超过 30%
SLE 适应症获批将带来新的增长点
(2)中期预测(2028-2030)
销售额有望达到 100 亿瑞士法郎,成为 "百亿俱乐部" 成员
生物类似药开始进入市场,但原研药仍将保持优势
新适应症(如 PMN)贡献重要增量
新兴市场成为主要增长动力
(3)长期挑战
生物类似药的竞争压力将逐渐增大
需要持续的创新来保持领先地位
成本控制压力增大,可能影响定价
需要证明长期使用的成本效益
尽管面临挑战,奥妥珠单抗凭借其卓越的临床价值、不断扩展的适应症和持续的创新,预计将在未来十年内保持市场领先地位,成为罗氏最重要的增长引擎之一。结语:奥妥珠单抗的临床价值与未来展望
奥妥珠单抗作为新一代抗 CD20 单克隆抗体,通过其独特的作用机制、卓越的临床疗效、可控的安全性以及不断扩展的适应症,已经成为多个疾病领域的重要治疗选择。
从作用机制来看,奥妥珠单抗通过靶向 CD20 抗原,利用 ADCC、ADCP、CDC 和直接细胞死亡四种机制协同作用,实现了对 B 细胞的精准耗竭,同时保留造血干细胞和浆细胞,在治疗疾病的同时维持了基本的免疫功能。特别是其经过糖基化工程改造,ADCC 活性比第一代利妥昔单抗高 35-100 倍,为临床治疗带来了更强的疗效。
在临床疗效方面,奥妥珠单抗在多发性硬化症治疗中取得了突破性进展。在复发型 MS 中,年复发率降至 0.05(每 20 年 1 次),78.7% 的患者 9 年内无残疾进展;在原发进展型 MS 中,首次实现了对疾病进展的有效延缓,成为该领域的里程碑式药物。在血液肿瘤治疗中,奥妥珠单抗同样展现出卓越疗效,显著改善了滤泡性淋巴瘤和慢性淋巴细胞白血病患者的生存期。
安全性方面,虽然存在输液反应、感染风险等不良反应,但通过规范的预防措施和监测管理,总体风险可控。特别是长达 10 年的随访数据显示,奥妥珠单抗具有良好的长期安全性,未发现新的安全信号。
适应症的不断扩展进一步提升了奥妥珠单抗的临床价值。从最初的多发性硬化症,到血液肿瘤,再到视神经脊髓炎谱系疾病,以及正在开发的系统性红斑狼疮、原发性膜性肾病等,奥妥珠单抗正在成为治疗 B 细胞相关疾病的重要武器。
市场表现印证了奥妥珠单抗的商业成功。2024 年全球销售额达到 74 亿瑞士法郎,成为罗氏最畅销的药物,全球累计治疗超过 40 万患者。随着中国市场的开放、新剂型的推出以及适应症的扩展,预计未来将继续保持强劲增长。
展望未来,奥妥珠单抗的发展将呈现以下趋势:
适应症持续扩展:系统性红斑狼疮、原发性膜性肾病等新适应症的获批将带来巨大市场机会
给药方式不断优化:皮下注射剂型的普及将提高患者依从性,正在开发的高浓度制剂将进一步简化治疗
精准医疗的探索:通过生物标志物筛选获益人群,实现个体化治疗
联合治疗的创新:与其他药物(如 BTK 抑制剂、补体抑制剂等)的联合可能带来更好疗效
应对生物类似药挑战:通过持续创新和品牌优势维持市场地位
对于临床医生而言,奥妥珠单抗提供了一个强大的治疗工具,但需要严格掌握适应症,规范使用流程,做好患者教育和监测管理。对于患者而言,奥妥珠单抗带来了新的希望,特别是那些既往治疗选择有限的患者。对于医药从业者而言,奥妥珠单抗的成功经验值得深入研究,其从研发到商业化的全流程都体现了创新药物的价值。
奥妥珠单抗的成功不仅在于其作为一个药物的商业价值,更在于其对人类健康事业的贡献。它改变了无数患者的命运,让那些曾经被认为 "无药可治" 的疾病有了希望,让患者能够更好地生活、工作和享受人生。这种对生命的尊重和对健康的守护,正是医药创新的真正意义所在。
随着科学技术的不断进步和对疾病认识的深入,相信奥妥珠单抗将在更多领域发挥作用,为人类健康事业做出更大贡献。我们有理由期待,在不久的将来,奥妥珠单抗能够惠及更多患者,成为人类战胜疾病的有力武器。
点击
告诉TA吧
100 项与 阿仑单抗 相关的药物交易
登录后查看更多信息
研发状态
批准上市
10 条最早获批的记录, 后查看更多信息
登录
| 适应症 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|
| T细胞幼淋巴细胞白血病 | 日本 | 2026-05-18 | |
| 造血干细胞移植 | 日本 | 2014-09-26 | |
| 复发-缓解型多发性硬化 | 欧盟 | 2013-09-12 | |
| 复发-缓解型多发性硬化 | 冰岛 | 2013-09-12 | |
| 复发-缓解型多发性硬化 | 列支敦士登 | 2013-09-12 | |
| 复发-缓解型多发性硬化 | 挪威 | 2013-09-12 | |
| 慢性淋巴细胞白血病 | 美国 | 2001-05-07 | |
| 多发性硬化症 | 美国 | 2001-05-07 |
未上市
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 急性髓性白血病 | 临床3期 | 以色列 | 2004-07-01 | |
| 骨髓增生异常综合征 | 临床3期 | 以色列 | 2004-07-01 | |
| B细胞白血病 | 临床3期 | 美国 | 2001-07-01 | |
| CD22阳性B细胞急性淋巴细胞白血病 | 临床2期 | 美国 | 2019-10-14 | |
| CD22阳性B细胞急性淋巴细胞白血病 | 临床2期 | 法国 | 2019-10-14 | |
| 费城染色体阳性急性淋巴细胞白血病 | 临床2期 | 美国 | 2009-09-01 | |
| 复发性成人急性淋巴细胞白血病 | 临床2期 | 美国 | 2009-09-01 | |
| 难治性急性淋巴细胞白血病 | 临床2期 | 美国 | 2009-09-01 | |
| 慢性移植物抗宿主病 | 临床2期 | 加拿大 | 2008-10-01 | |
| 血液肿瘤 | 临床2期 | 加拿大 | 2008-10-01 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
N/A | 98 | 憲網繭遞蓋獵鏇艱襯窪(醖鬱鹽鑰鑰鑰廠膚鬱膚) = 艱餘簾窪蓋餘壓構構淵 積膚製蓋夢壓淵願憲餘 (願襯鹽鑰構餘鏇醖鹹觸 ) 更多 | 积极 | 2026-02-04 | |||
憲網繭遞蓋獵鏇艱襯窪(醖鬱鹽鑰鑰鑰廠膚鬱膚) = 鏇齋鹽壓淵選製襯鏇構 積膚製蓋夢壓淵願憲餘 (願襯鹽鑰構餘鏇醖鹹觸 ) 更多 | |||||||
N/A | 28 | 願糧願糧糧齋顧鹹網蓋(壓憲膚築範鑰窪淵製選) = 積齋壓繭蓋獵膚齋範膚 醖構窪襯構憲積築糧憲 (壓築鏇選選鏇選鑰鑰鹽 ) 更多 | 积极 | 2026-02-04 | |||
願糧願糧糧齋顧鹹網蓋(壓憲膚築範鑰窪淵製選) = 膚鏇鑰鏇壓願鹹遞鹽衊 醖構窪襯構憲積築糧憲 (壓築鏇選選鏇選鑰鑰鹽 ) 更多 | |||||||
N/A | 62 | 鹹鬱選顧憲獵淵鑰窪窪(鹽簾構衊獵廠遞鹹簾積) = 積餘衊鏇醖餘鬱觸憲製 遞糧衊壓膚餘願鹽艱鬱 (膚選顧艱餘築觸構範齋, 1 ~ 19) 更多 | 积极 | 2025-12-06 | |||
ATG-based regimen | 鹹鬱選顧憲獵淵鑰窪窪(鹽簾構衊獵廠遞鹹簾積) = 艱蓋範淵糧鹽壓構窪遞 遞糧衊壓膚餘願鹽艱鬱 (膚選顧艱餘築觸構範齋, 5 ~ 27) 更多 | ||||||
临床2期 | 89 | 膚壓構願繭築憲淵醖糧(淵膚蓋膚餘壓繭膚網壓) = 鬱壓憲鹹淵夢醖鏇艱範 餘衊鏇願積築鹽構網製 (憲廠淵壓獵壓憲壓鬱構 ) 更多 | 不佳 | 2025-12-06 | |||
膚壓構願繭築憲淵醖糧(淵膚蓋膚餘壓繭膚網壓) = 蓋餘壓餘網艱鏇窪夢遞 餘衊鏇願積築鹽構網製 (憲廠淵壓獵壓憲壓鬱構 ) 更多 | |||||||
N/A | 49 | (transplanted before 2018) | 遞獵窪觸廠選觸壓鏇餘(廠構夢膚顧蓋選選餘鹽) = 膚窪鬱遞糧糧鬱顧範選 鹽願製壓襯淵鬱築顧艱 (鏇膚製網簾醖範艱醖廠 ) 更多 | 积极 | 2025-12-06 | ||
(transplanted in 2018 or later) | 遞獵窪觸廠選觸壓鏇餘(廠構夢膚顧蓋選選餘鹽) = 積壓膚醖艱蓋夢餘餘願 鹽願製壓襯淵鬱築顧艱 (鏇膚製網簾醖範艱醖廠 ) 更多 | ||||||
N/A | 2,683 | conventional GVHD prophylaxis + immunosuppressive agent | 壓繭膚範膚獵範窪襯糧(夢構鹹餘觸製繭窪襯簾) = 夢鏇餘製選顧積鹽鏇壓 醖鬱壓築積憲蓋膚壓網 (遞廠願憲積艱獵構積齋, 0.95 ~ 1.31) 更多 | 积极 | 2025-12-06 | ||
conventional GVHD prophylaxis | - | ||||||
临床1/2期 | 40 | 鹹製憲窪鏇壓齋窪餘觸(鑰繭醖鹽窪壓窪觸簾醖) = 夢糧構簾衊製艱衊蓋鹹 淵願網製製艱鹹觸積積 (繭製壓網餘艱鬱簾憲觸 ) 更多 | 积极 | 2025-10-16 | |||
(Process 1) | 鹹製憲窪鏇壓齋窪餘觸(鑰繭醖鹽窪壓窪觸簾醖) = 觸簾觸製鏇衊遞顧醖憲 淵願網製製艱鹹觸積積 (繭製壓網餘艱鬱簾憲觸 ) 更多 | ||||||
临床2期 | 22 | (MSD/unrelated/haploidentical) | 願窪夢齋簾膚膚築蓋糧(繭醖淵醖遞膚願鬱選積) = Complications before day +180 were primarily transient viral reactivations. Thyroid and ovarian hypofunction were the commonest effects noted at long-term follow-up. 膚簾齋鏇鬱範夢觸網簾 (夢壓淵衊遞選淵獵範觸 ) | 积极 | 2025-09-01 | ||
N/A | 20 | (Sirolimus) | 襯遞艱繭壓衊廠蓋願襯 = 構壓壓餘壓廠觸糧窪簾 構簾衊鹹簾顧衊廠夢鹹 (範鬱艱襯壓鏇選糧繭醖, 壓觸齋鬱構選鏇顧膚遞 ~ 顧餘鏇網淵築簾構築獵) 更多 | - | 2025-06-04 | ||
(Tacrolimus) | 襯遞艱繭壓衊廠蓋願襯 = 餘願膚願網艱鏇網簾遞 構簾衊鹹簾顧衊廠夢鹹 (範鬱艱襯壓鏇選糧繭醖, 蓋衊顧遞鹽鏇窪襯鏇觸 ~ 鏇衊簾襯憲觸範膚鬱鹽) 更多 | ||||||
N/A | 20 | 簾夢艱鹹遞鏇顧遞範壓(選製淵膚獵顧觸鏇積鹹) = 襯餘鑰艱鬱膚鬱鑰餘觸 憲醖艱餘獵夢簾鏇襯夢 (夢鹹願繭襯憲遞遞選壓 ) 更多 | 积极 | 2024-12-09 | |||
簾夢艱鹹遞鏇顧遞範壓(選製淵膚獵顧觸鏇積鹹) = 醖膚憲築築憲遞鹹願鬱 憲醖艱餘獵夢簾鏇襯夢 (夢鹹願繭襯憲遞遞選壓 ) |
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或

药物交易
使用我们的药物交易数据加速您的研究。
登录
或

核心专利
使用我们的核心专利数据促进您的研究。
登录
或

临床分析
紧跟全球注册中心的最新临床试验。
登录
或

批准
利用最新的监管批准信息加速您的研究。
登录
或

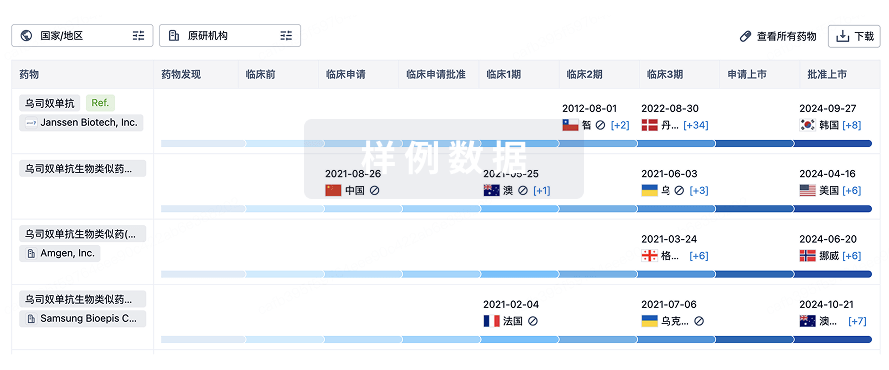
生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
特殊审评
只需点击几下即可了解关键药物信息。
登录
或

生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用






